4 results
Characterization of carbapenem-resistant gram-negative bacteria collected in the Sentinel Surveillance Program, 2018–2019
- Lori Spicer, Davina Campbell, J. Kristie Johnson, Cynthia Longo, Thomas Balbuena, Thomas Ewing, Maria Karlsson, J. Kamile Rasheed, Christopher Elkins, Amy Gargis, Joseph Lutgring
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, p. s52
-
- Article
-
- You have access Access
- Open access
- Export citation
-
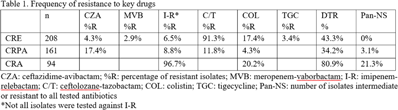
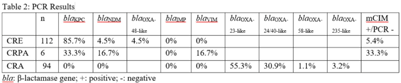
Background: Carbapenem resistance in gram-negative organisms is an important public health problem. The CDC conducted Sentinel surveillance in 2018–2019 to characterize these organisms from 9 facilities in 9 different states. Methods: Carbapenem-resistant Enterobacterales (CRE), Pseudomonas aeruginosa (CRPA), and Acinetobacter spp (CRA) obtained from clinical samples of patients in acute-care or long-term care facilities were submitted to the CDC. Identification was confirmed using matrix-assisted laser desorption ionization time-of-flight (MALDI-TOF), and antimicrobial susceptibility testing (AST) was performed via broth microdilution for 27 antibiotics. All confirmed CRE and CRPA were tested for carbapenemase production (CP) using the modified carbapenem inactivation method (mCIM). The isolates that were mCIM-positive were assessed by real-time PCR for presence of blaKPC, blaNDM, blaVIM, and blaIMP. CP-CRE were also assessed for blaOXA-48-like. All confirmed CRA were tested for the same genes as CRPA and blaOXA-23–like, blaOXA-24/40-like, blaOXA-58–like, and blaOXA-235–like genes. Difficult-to-treat resistance (DTR) was defined as resistance to all β-lactams (excluding newer β-lactam combination agents) and quinolones tested. Results: The CDC confirmed 208 CRE, 161 CRPA, and 94 CRA. Table 1 summarizes AST results for a selection of drugs. We identified 112 (53.8%) mCIM-positive CRE and 6 (3.7%) mCIM-positive CRPA. The PCR results are summarized in Table 2. One mCIM-positive and PCR-negative isolate was positive in a metallo-β-lactamase screen. Conclusions: Resistance among CRE and CRPA to newer β-lactam combination agents was detected. Options for treating CRA are limited. Of 112 CP-CRE, 85.7% harbored blaKPC; CP-CRPA were rare (3.7%); and most CRA harbored blaOXA-23-like (55.3%) or blaOXA-24/40-like (30.9%). Whole-genome sequencing is planned to better understand gene variants, sequence types, and additional resistance markers present among the isolates.
Funding: None
Disclosures: None
Trimethoprim-Sulfamethoxazole Resistance Patterns Among Methicillin-Resistant Staphylococcus aureus, 2012–2018
- D. Cal Ham, Lucy Fike, Tara Fulton, Nychie Dotson, Rebecca Perlmutter, Ericka Kalp, Joseph Lutgring, Amy Gargis, Alison Laufer-Halpin, Alexander Kallen, Maroya Walters
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, p. s418
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Trimethoprim-sulfamethoxazole is commonly used for the treatment of noninvasive methicillin-resistant Staphylococcus aureus (MRSA) infections. Following a report from 2 facilities of increased trimethoprim-sulfamethoxazole resistance among MRSA infections, we assessed changes in resistance nationally and by state. Methods: We reviewed antibiotic susceptibility testing (AST) data for trimethoprim-sulfamethoxazole among S. aureus isolates associated with surgical site infections (SSIs), central-line–associated bloodstream infections (CLABSIs), and catheter-associated urinary tract infections (CAUTIs) from acute-care hospitals reported to the NHSN Device and Procedure Module from 2012 to 2018. We compared the pooled mean percentage of isolates nonsusceptible to trimethoprim-sulfamethoxazole in 2012 and 2018, stratified by MRSA and methicillin-sensitive Staphylococcus aureus (MSSA). Among MRSA isolates, we compared the percentage nonsusceptible to trimethoprim-sulfamethoxazole by healthcare-associated infection (HAI) type and state in 2012 and 2018. States with ≥20 MRSA isolates with AST reported each year were included in the state-level analysis. Results: Overall, 36,587 MRSA isolates and 46,824 MSSA isolates were reported from 2012 to 2018. Moreover, >80% of MRSA and MSSA isolates had trimethoprim-sulfamethoxazole AST reported each year. Nationally, the percentage of trimethoprim-sulfamethoxazole nonsusceptible among MRSA isolates was 3.9% in 2012 compared to 6.5% in 2018 (P < .001), but it was unchanged among MSSA isolates during the same period (1.1% in 2012 vs 1.4% in 2018; P = .08). Among MRSA surgical site infections (SSIs), the proportion of trimethoprim-sulfamethoxazole nonsusceptible isolates was 3.1% in 2012 versus 6.1% in 2018 (P < .001) but did not change significantly for CLABSIs or CAUTIs (Fig. 1). Among the 32 states that met the inclusion criteria, there were no significant decreases, whereas 4 (12.5%) showed significant increases in the percentage of MRSA that were trimethoprim-sulfamethoxazole nonsusceptible in 2018 compared to 2012: New Jersey (2.4% in 2012 vs 19.3% in 2018; P <.001); Florida (9.1% in 2012 vs 22.4% in 2018; P < .001); Maryland (0.0% in 2012 vs 10.9% in 2018; P < .01); and Pennsylvania (1.7% in 2012 vs 6.5% in 2018; P < .001). Conclusions: Nationally, there was a modest but significant increase in the percentage of MRSA HAI isolates nonsusceptible to trimethoprim-sulfamethoxazole in 2018 compared to 2012; however, 3 of 4 states with significant increases in nonsusceptibility had substantial, potentially clinically relevant increases (>10%). Ongoing characterization of MRSA isolates from Florida and New Jersey may provide insight into the underlying cause of these shifting patterns in trimethoprim-sulfamethoxazole resistance among MRSA. Healthcare personnel should select appropriate antibiotic regimens based on local resistance patterns, should monitor patients for treatment failure, and should report changes in resistance to the appropriate public health department.
Funding: None
Disclosures: None
Molecular Typing of Invasive Staphylococcus aureus from the Emerging Infections Program (EIP) Using Whole-Genome Sequencing
- Davina Campbell, Gillian McAllister, Kelly Jackson, Isaac See, Alison Halpin, Joseph Lutgring, Erin Epson, Susan Petit, Susan Ray, William Schaffner, Ghinwa Dumyati, Thomas Ewing, Michelle Adamczyk, Amy Gargis
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s71-s72
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: The CDC has performed surveillance for invasive Staphylococcus aureus (iSA) infections through the Emerging Infections Program (EIP) since 2004. SCCmec and spa typing for clonal complex (CC) assignment and genomic markers have been used to characterize isolates. In 2019, whole-genome sequencing (WGS) of isolates began, allowing for high-resolution assessment of genomic diversity. Here, we evaluate the reliability of SCCmec typing, spa typing, and CC assignment using WGS data compared to traditional methods to ensure that backwards compatibility is maintained. Methods:S. aureus isolates were obtained from a convenience sample of iSA cases reported through the EIP surveillance system. Overall, 78 iSA isolates with diverse spa repeat patterns, CCs, SCCmec types, and antimicrobial susceptibility profiles were sequenced (MiSeq, Illumina). Real-time PCR and Sanger sequencing were used as the SCCmec and spa typing reference methods, respectively. spa-MLST mapping (Ridom SpaServer) served as the reference method for CC assignment. WGS assembly and multilocus sequence typing (MLST) were performed using the CDC QuAISAR-H pipeline. WGS-based MLST CCs were assigned using eBURST and SCCmec types using SCCmecFinder. spa types were assigned from WGS assemblies using BioNumerics. For isolate subtyping, previously published and validated canonical single-nucleotide polymorphisms (canSNPs) as well as the presence of the Panton-Valentine leukocidin (PVL) toxin and arginine catabolic mobile element (ACME) virulence factor were assessed for all genome assemblies. Results: All isolates were assigned WGS-based spa types, which were 100% concordant (78 of 78) with Sanger-based spa typing. SCCmecFinder assigned 91% of isolates (71 of 78) SCCmec types, which were 100% concordant with reference method results. Also, 7 isolates had multiple cassettes predicted or an incomplete SCCmec region assembly. Using WGS data, 96% (75 of 78) of isolates were assigned CCs; 3 isolates had unknown sequence types that were single-locus variants of established sequence types. Overall, 70 isolates had CCs assigned by the reference method; 100% (70 of 70) concordance was observed with WGS-based CCs. Analysis of canSNPs placed 42% (33 of 78) of isolates into CC8, with 17 (52%) of these isolates classified as USA300. PVL and ACME were not accurate markers for inferring the USA300 subtype as 24% (4 of 17) of isolates did not contain these markers. Conclusions:S. aureus CCs, SCCmec, and spa types can be reliably determined using WGS. Incorporation of canSNP analysis represents a more efficient method for CC8 assignment than the use of genomic markers alone. WGS allows for the replacement of multiple typing methods for increased laboratory efficiency, while maintaining backward compatibility with historical typing nomenclature.
Funding: None
Disclosures: None
Antimicrobial Nonsusceptibility Among Invasive MRSA USA300 Strains by Healthcare Exposure, Three Sites, 2005–2016
- Kelly Jackson, Runa Gokhale, Davina Campbell, Amy Gargis, Susan Ray, Ruth Lynfield, William Schaffner, Joseph Lutgring, Isaac See
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s120-s121
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Incidence of community-associated (CA) and healthcare-associated, community-onset (HACO) USA300 methicillin-resistant Staphylococcus aureus (MRSA) bloodstream infections has remained unchanged in recent years. Traditionally considered a CA strain, USA300 is increasingly associated with healthcare settings. We examined whether antimicrobial nonsusceptibility among USA300 strains could distinguish epidemiologic class (community vs hospital), and whether divergences in susceptibility were occurring over time. Methods: We used data on invasive MRSA infections from active, population, and laboratory-based surveillance during 2005–2016 from 11 counties in 3 states. Invasive cases were defined as MRSA isolation from a normally sterile site in a surveillance area resident. Cases were considered hospital-onset (HO) if the culture was obtained >3 days after hospitalization and HACO if ≥1 of the following risk factors was present: hospitalization, surgery, dialysis, or residence in a long-term care facility in the past year; or central vascular catheter ≤2 days before culture. Otherwise, cases were considered CA. Sites submitted a convenience sample of clinical MRSA isolates for molecular typing and antimicrobial susceptibility testing. Molecular typing was performed by pulsed-field gel electrophoresis until 2008, when typing was inferred using a validated algorithm based on molecular characteristics. Reference broth microdilution was performed for 8 antimicrobials and interpreted based on CLSI interpretive criteria. We compared USA300 nonsusceptibility for HO and CA isolates. For antimicrobials with >5% nonsusceptibility and for which HO isolates had greater nonsusceptibility than CA isolates, we compared nonsusceptibility for HACO and CA and analyzed annual trends in nonsusceptibility within each epidemiologic class (ie, CA, HACO, and HO) using linear regression. Results: Of 17,947 MRSA cases during 2005–2016, isolates were available for 6,685 (37%), and 2,120 were USA300 (34% CA, 52% HACO, 14% HO). HO isolates had more nonsusceptibility than CA isolates to gentamicin (2.2% vs 0.6%; P = .03), levofloxacin (47.8% vs 39.7%; P = .02), rifampin (3.7 vs 1.1%; P = .01), and trimethoprim-sulfamethoxazole (3.4% vs 0.6%; P = .04). HACO isolates also had more nonsusceptibility than CA isolates to levofloxacin (50.9% vs 39.7%; P < .01). Levofloxacin nonsusceptibility increased during 2005–2016 for HACO and CA isolates (P < .01), but not among HO isolates (P = .36) (Fig. 1). Conclusions: Overall, nonsusceptibility across drugs cannot distinguish USA300 isolates causing HO versus CA disease. Although HO isolates had higher levofloxacin nonsusceptibility than CA and HACO isolates early on, USA300 MRSA HACO isolates now have levofloxacin nonsusceptibility most similar to that of HO isolates. Further study could help to explore whether increases in fluoroquinolone nonsusceptibility among CA and HACO cases may be contributing to the persistence of USA300 strains.
Disclosures: None
Funding: None





