2 results
Integrated safety analysis of phase 3 studies for investigational microbiome therapeutic, SER-109, in recurrent CDI
- Matthew Sims, Charles Berenson, Stuart Cohen, Elaine Wang, Elizabeth Hohmann, Richard Nathan, Alberto Odio, Paul Cook, Kelly Brady, David Lombardi, Asli Memisoglu, Ananya De, Brooke Hasson, Bret Lashner, Louis Korman, Doria Grimard, Juan Carlos Moises Gutierrez, Barbara McGovern, Lisa Von Moltke
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s44-s45
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Clostridioides difficile infection (CDI) often recurs in patients aged ≥65 years and those with comorbidities. Clinical trials often exclude patients with history of immunosuppression, malignancy, renal insufficiency, or other comorbidities. In a phase 3 trial (ECOSPOR III), SER-109 was superior to placebo in reducing recurrent CDI (rCDI) risk at week 8 and was well tolerated. We report integrated safety data for SER-109 in a broad patient population through week 24 from phase 3 studies: ECOSPOR III and ECOSPOR IV. Methods: ECOSPOR III was a double-blind, placebo-controlled trial conducted in participants with ≥2 CDI recurrences randomized 1:1 to placebo or SER-109. ECOSPOR IV was an open-label, single-arm study conducted in 263 patients with rCDI enrolled in 2 cohorts: (1) rollover participants from ECOSPOR III with on-study recurrence and (2) participants with ≥1 CDI recurrence, inclusive of the current episode. In both studies, the investigational product was administered as 4 oral capsules over 3 days. Treatment-emergent adverse events (TEAEs) were collected through week 8; serious TEAEs and TEAEs of special interest (ie, bacteremia, abscess, meningitis) were collected through week 24. Results: In total, 349 participants received SER-109 in ECOSPOR III and/or ECOSPOR IV (mean age 64.2; 68.8% female). Chronic diseases included cardiac disease (31.2%), immunocompromised or immunosuppressed (21.2%), diabetes (18.9% ), and renal impairment or failure (13.2%). Overall, 221 (63.3%) of 349 participants who received SER-109 experienced TEAEs through week 24. Most were mild to moderate and gastrointestinal. The most common (>5% of participants) treatment related TEAEs were flatulence, abdominal pain and distension, decreased appetite, constipation, nausea, fatigue, and diarrhea. No participants experienced a treatment-related TEAE leading to study withdrawal. Invasive infections were observed in 28 participants (8%); those with identified pathogens were unrelated to SER-109 species, and all were deemed unrelated to treatment by the investigators. There were 11 deaths (3.2%) and 48 participants (13.8%) with serious TEAEs, none of which were deemed treatment related. There were no clinically important differences in the safety profile across subgroups of sex, race, prior antibiotic regimen, or number of CDI recurrences. No safety signals were observed in participants with renal impairment or failure, diabetes, cardiac disease, or immunocompromised or immunosuppressed individuals. Conclusions: In this integrated analysis of phase 3 trials, SER-109, an investigational microbiome therapeutic, was well tolerated in this vulnerable patient population with prevalent comorbidities. No infections, nor those with identified pathogens, were attributed to SER-109 or product species. This safety profile might be expected because this purified product is composed of spore-forming Firmicutes normally abundant in the healthy microbiome.
Financial support: This study was funded by Seres Therapeutics.
Disclosures: None
Healthcare resource utilization in a phase 3 trial of SER-109 in patients with recurrent Clostridioides difficile infection
- Stuart Cohen, Thomas Louie, Charles Berenson, Alpesh Amin, David Lombardi, Sissi Pham, Shirley Huang, Elaine Wang, Brooke Hasson, Barbara McGovern, Lisa Von Moltke
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, p. s73
-
- Article
-
- You have access Access
- Open access
- Export citation
-
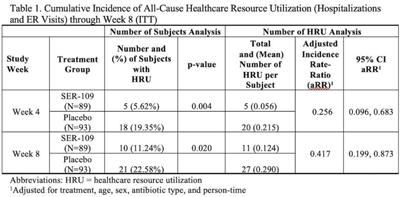
Background: The estimated economic cost of Clostridioides difficile infection (CDI) is $5.4 billion annually, primarily attributed to acute-care costs. We previously reported data from ECOSPOR III that SER-109, an investigational oral microbiome therapeutic, was superior to placebo in reducing recurrent CDI (rCDI) in adults at 8 weeks after treatment, with a 68% relative risk reduction. Adults with rCDI have more hospitalizations and emergency room (ER) visits (defined herein as healthcare resource utilization, HRU) compared to those without recurrence. Thus, we evaluated incidence of HRU. Methods: Adults with rCDI (≥3 episodes in 12 months) were screened at 56 US and Canadian sites and were randomized 1:1 to SER-109 (4 capsules × 3 days) or placebo following resolution of CDI with standard-of-care CDI antibiotics. The primary end point was rCDI at 8 weeks. Exploratory end points included cumulative incidence of hospitalizations through 24 weeks after treatment. Here, we report cumulative incidence of all-cause HRU through 8 weeks after treatment. Results: In total, 281 patients were screened and 182 were randomized (59.9% female; mean age 65.5 years; 98.9% outpatient). Overall, 31 patients (17%) had 38 hospitalizations or ER visits through week 8 (11 events in 10 SER-109 patients and 27 events in 21 placebo patients) (Table 1). The cumulative incidence of HRU was lower in SER-109–treated patients compared to placebo at both weeks 4 and 8 with most events (65.8%) recorded within 4 weeks after treatment. The adjusted HRU incidence rate (by person time, age, sex, and antibiotic use) was also lower in SER-109–treated patients compared to placebo at weeks 4 and 8 (0.256 [95% CI, 0.096–0.683] versus 0.417 [95% CI, 0.199–0.873], respectively). Conclusions: SER-109–treated patients had less HRU compared to placebo patients through 8 weeks after treatment in this mostly outpatient population. These data suggest a potential benefit of SER-109 in reducing HRU, thus lowering the healthcare burden of rCDI.
Funding: Seres Therapeutics
Disclosures: None