4 results
Relevance of RSV in hospitalized adults and the need for continued testing
- Katherine Miller, Arnold Monto, H. Keipp Talbot, Manjusha Gaglani, Tresa McNeal, Fernanda Silveira, Richard Zimmerman, Donald Middleton, Shekhar Ghamande, Kempapura Murthy, Lindsay Kim, Jill Ferdinands, Manish Patel, Emily Martin
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, p. s62
-
- Article
-
- You have access Access
- Open access
- Export citation
-
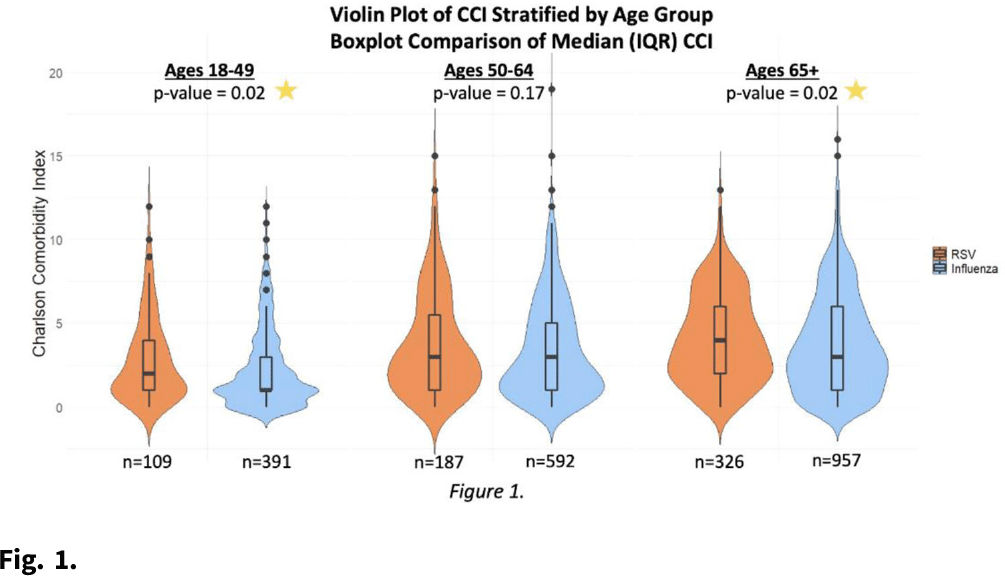
Background: RSV is underrecognized in hospitalized adults. A better understanding of RSV in this population could help prioritize targeted viral-testing resources. Hospitalization and in-hospital outcomes are widely accepted as markers of clinical severity with respect to acute respiratory illness (ARI). We compared characteristics and clinical outcomes between adults hospitalized with ARI from October 2016 through May 2019. Methods: All hospitalized adults (≥ 18 years) who met a standardized case definition of ARI were prospectively enrolled across 3 respiratory seasons from 9 hospitals participating in the US Hospitalized Adult Influenza Vaccine Effectiveness Network (HAIVEN). Demographic data were collected during enrollment interviews, and electronic medical records (EMRs) were reviewed to extract comorbidity data. Throat and nasal swabs collected at enrollment were tested for ARI pathogens using real-time PCR assays at respective HAIVEN research laboratory sites. Characteristics and clinical outcomes of participants were compared using χ2 or nonparametric tests where appropriate. Multivariable logistic regression models were used to test associations between infection status, characteristics, and clinical outcomes, adjusting for age, sex, race, Charlson comorbidity index (CCI), body mass index (BMI), site, season, and days to admission. Results: In total, 10,311 adults were included, 22.3% (n = 2,300) were aged 18–49 years, 33.2% (n = 3,423) were aged 50–64 years, and 44.5% (n = 4,588) were aged ≥65 years. Moreover, 6% of adults tested positive for RSV (n = 622), 18.8% positive for influenza (n = 1,940), and 75.1% negative for both (n = 7,749). Obesity and age ≥65 years were significantly associated with RSV detection when compared with participants negative for both RSV and influenza. Patients aged 18–49 years and ≥65 years with RSV had significantly higher median CCI scores compared to patients with influenza (Fig. 1.). The proportion of adults with CHF or COPD was significantly (p-value Conclusions: Severe RSV illness may differ from severe influenza illness, and those infected with RSV may have different characteristics than those infected with influenza. Hospitalized adults with RSV infection were more likely to have underlying cardiopulmonary comorbidities and higher CCI scores as well as experience an extended length of hospital stay and need for mechanical ventilation. These data highlight the importance of retaining testing for RSV in older adults hospitalized with ARI.
Funding: None
Disclosures: None
Economic Evaluation of Standing Order Programs for Pneumococcal Vaccination of Hospitalized Elderly Patients
- Donald B. Middleton, Chyongchiou J. Lin, Kenneth J. Smith, Richard K. Zimmerman, Mary Patricia Nowalk, Mark S. Roberts, Dwight E. Fox
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 29 / Issue 5 / May 2008
- Published online by Cambridge University Press:
- 02 January 2015, pp. 385-394
- Print publication:
- May 2008
-
- Article
- Export citation
-
Background.
Standing order programs (SOPs), which allow for vaccination without an individual physician order, are the most effective mechanism to achieve high vaccination rates. Among the suggested settings for the utilization of SOPs are hospital inpatient units, because they provide care for those most likely to benefit from vaccination. The cost-effectiveness of this approach for elderly hospitalized persons is unknown. The purpose of this study was to estimate the cost-effectiveness of SOPs for pneumococcal polysaccharide vaccine (PPV) vaccination for patients 65 years of age or older in 2 types of hospital.
Methods.In 2004, a 1,094-bed tertiary care hospital implemented a pharmacy-based SOP for PPV, and a 225-bed community hospital implemented a nursing-based SOP for PPV. Newly admitted patients 65 years of age or older were screened for PPV eligibility and then offered PPV. Vaccination rates before and after initiation of SOPs in the United States, incidence rates of invasive pneumococcal disease in the United States, and US economic data were the bases of the cost-effectiveness analyses. One-way and multivariate sensitivity analyses were conducted.
Results.PPV vaccination rates increased 30.5% in the tertiary care hospital and 15.3% in the community hospital. In the base-case cost-effectiveness analysis, using a societal perspective, we found that both pharmacy-based and nursing-based SOPs cost less than $10,000 per quality-adjusted life-year gained, with program costs (pharmacy-based SOPs cost $4.16 per patient screened, and nursing-based SOPs cost $4.60 per patient screened) and vaccine costs ($18.33 per dose) partially offset by potential savings from cases of invasive pneumococcal disease avoided ($12,436 per case). Sensitivity analyses showed SOPs for PPV vaccination to be cost-effective, compared with PPV vaccination without SOPs, unless the improvement in vaccination rate was less than 8%.
Conclusion.SOPs do increase PPV vaccination rates in hospitalized elderly patients and are economically favorable, compared with PPV vaccination rates without SOPs.
Overcoming Barriers to Establishing an Inpatient Vaccination Program for Pneumococcus Using Standing Orders
- Donald B. Middleton, Dwight E. Fox, Mary Patricia Nowalk, Susan J. Skledar, Denise R. Sokos, Richard K. Zimmerman, Kelly A. Ervin, Chyongchiou J. Lin
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 26 / Issue 11 / November 2005
- Published online by Cambridge University Press:
- 21 June 2016, pp. 874-881
- Print publication:
- November 2005
-
- Article
- Export citation
-
Objectives:
To identify and classify barriers to establishing a standing orders program (SOP) for adult pneumococcal vaccination in acute care inpatient facilities and to provide recommendations for overcoming these roadblocks. Vaccination rates in hospitals with SOPs are generally higher than those in hospitals that require individual physician orders. The array of solutions drawn from our experience in different hospital settings should permit many types of facilities to anticipate and overcome barriers, allowing a smoother transition from initiation to successful implementation of an inpatient pneumococcal vaccination SOP.
Design:Descriptive study of barriers and solutions encountered during implementation of a pneumococcal vaccination SOP in three hospitals of the University of Pittsburgh Medical Center Health System (UPMC) and in the scientific literature.
Setting:As of 2004, two UPMC tertiary-care hospitals and one UPMC community hospital had incorporated SOPs into existing physician order-driven programs for inpatient vaccination with pneumococcal polysaccharide vaccine.
Results:Barriers were identified at each step of implementation and categorized as patient related, provider related, or institutional. Based on a process of continual review and revision of our programs in response to encountered barriers, steps were taken to overcome these impediments.
Conclusions:A strong commitment by key individuals in the facility's administration including a physician champion; ongoing, persistent efforts to educate and train staff; and close monitoring of the vaccination rate were essential for successful implementation of a SOP for pneumococcal vaccination of eligible inpatients. Legal statutes and evaluations of external hospital-rating associations regarding the effectiveness of the vaccination program were major motivating factors in its success.
Increasing Pneumococcal Vaccination Rates Among Hospitalized Patients
- Mary Patricia Nowalk, Donald B. Middleton, Richard K. Zimmerman, Mary M. Hess, Susan J. Skledar, Marjorie A. Jacobs
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 24 / Issue 7 / July 2003
- Published online by Cambridge University Press:
- 02 January 2015, pp. 526-531
- Print publication:
- July 2003
-
- Article
- Export citation
-
Objective:
To increase the proportion of inpatients vaccinated against pneumococcal infection.
Design:Pre- and post-intervention study.
Setting:University medical center–affiliated, suburban community teaching hospital.
Patients:Unvaccinated inpatients 65 years and older and those 2 to 64 years old who had chronic medical conditions predisposing them to invasive pneumococcal infection.
Intervention:The nursing staff screened newly admitted patients for eligibility based on age, diagnosis, or medications from a computer-generated admissions list and placed a pre-printed order form for the pneumococcal polysaccharide vaccine (PPV) on the charts of eligible patients. Following the physician's order, the nursing staff administered the PPV and recorded it. Ongoing quality improvements including admission vaccination screening and computer-based record keeping were initiated to identify unvaccinated eligible patients and track vaccination status.
Results:Efforts resulted in rates of in-hospital vaccination ranging from 3.1% to 7.9% (mean, 5.2% ± 1.7% [standard deviation]) and significant improvements in the assessment of previous vaccination status, reaching 54% of eligible patients after 1 year. Ascertainment of a previous vaccination increased significantly following the initiation of the use of admission forms that specifically assessed vaccination status and a system to permanently record vaccination status in an electronic medical record (P < .05).
Conclusion:Concerted efforts using electronic medical records significantly improved the assessment and documentation of inpatient vaccination status. Greater improvement of the rates of in-hospital vaccination will require healthcare system–wide efforts such as a standing order policy for vaccinating all eligible patients. Standing orders for inpatient immunization supported by effective assessment and tracking systems have the potential to raise vaccination rates to the goals of Healthy People 2010 (Infect Control Hosp Epidemiol 2003;24:526-531)




