2 results
Differential diagnosis of late onset psychotic symptoms. A case report.
- J. Sánchez Rodríguez, S. Puyal González, M. Paz Otero, E. Lozano Bori, A. García Recio
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1063
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We present the case of a sixty-seven-year-old woman who is examined for the first time in the emergency room because of a nine-month clinical picture that involves psychotic symptoms. The patient exhibits persecutory delusions that started after she shared some private information on social media. These symptoms also entail emotional distress and behavioral disturbances. She has never experienced hallucinations, but she does present delusional interpretations of the environment. Her clinical history reveals abnormalities of premorbid personality, including paranoid and immature features.
Objectives(1) We will be carrying out a differential diagnosis of late onset psychotic symptoms. We will as well be exploring the concept of Paraphrenia and analyzing its differential features in order to stablish the most suitable diagnosis for the case.
(2) The relationship between abnormalities in premorbid personality and psychotic symptoms will be covered, reviewing the available literature on this matter, and relating it to the patient’s symptomatology.
MethodsA review of the patient’s clinical history will be carried out, considering her biography, the testimony of her family and the complementary tests performed during the hospitalization period.
A bibliographic review of the available scientific literature will also be developed involving disorders that could explain psychotic symptoms in the elderly, as well as the term Paraphrenia, which describes specific features in a psychotic episode but is not included in the diagnostic manuals.
Results(1) The symptomatology that our patient exhibits may be considered atypical given the late stage of its onset and its specific features.
(2) The case could be explained under the category of Delusional Disorder. From a psychopathological point or view, it could also fit under de diagnosis of Paraphrenia as described by Ravindran et al.
(3) Pathological personality traits were assessed in premorbid personality which included paranoid and immature features.
ConclusionsIt could be useful to review the concept of the “paranoid spectrum” as proposed by some authors regarding some patient’s psychotic symptoms that don’t exactly fit any of the nowadays diagnostic categories. “Paraphrenia” could be understood as a distinct clinical entity for patients who show psychotic disorders but keep affective warmth and lack though deterioration and grossly disorganized behavior.
Most patients with late life paranoid psychoses have abnormal premorbid personalities, most usually of schizoid or paranoid type. There’s a decent amount of consensus in viewing the premorbid personality as having been abnormal as an early marker of impending psychosis.
Reformulating the way we approach diagnosis of psychotic symptoms of late onset could help us identify vulnerable patients on a premorbid stage and better classify and understand atypical entities.
Disclosure of InterestNone Declared
Cyclothymia, bipolar disorder and multiple sclerosis: A case report
- M. D. P. Paz Otero, E. Lozano Bori, J. Sánchez Rodríguez, S. Puyal González, M. Fernández Fariña, F. Mayor Sanabria, A. Francos Ajona
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S703-S704
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We present the case of a 49-year-old woman who was diagnosed with multiple sclerosis at the age of 19 and suffers from an affective disorder that has been evolving for years. This condition, for which she has been followed by psychiatry and psychology for more than ten years, consists of alternating periods of hypomania lasting weeks and phases in which frank depressive symptomatology predominates, with no phases of euthymia in between and with a predominance of severe deterioration of her functionality at both poles.
Objectives(1) We will review the term cyclothymia and explore the concept of “cyclothymic temperament” advocated by some authors, in order to be able to understand the dimension of the present case and reformulate its approach.
(2) The relationship between multiple sclerosis and bipolar spectrum disorders will be covered, reviewing the current knowledge in this regard and relating it to the patient’s symptomatology.
MethodsA review of the patient’s clinical history will be carried out, taking into account her life history, the complementary tests performed as well as the multiple therapeutic approaches tried over the last few years.
Likewise, a bibliographic review of the available scientific literature will be carried out in relation to the diagnosis of cyclothymia or bipolar disorder type II, the controversial term “cyclothymic temperament”, and the relationship that these diagnoses have with the diagnosis of Multiple Sclerosis.
Results(1) Our patient could fit into what many authors define as a cyclothymic temperament, fulfilling, in certain episodes, the criteria that the manuals propose for bipolar disorder type II.
(2) 2.1 The prevalence of bipolar affective disorder in MS is approximately twice as high as in the general population (rates of 0.3-2.4%). 2.2 Patients with MS have higher scores in cyclothymic and hyperthymic temperament than the control group. 2.3 Certain drugs generally used in BD also seem to have a beneficial effect on MS.
Image:
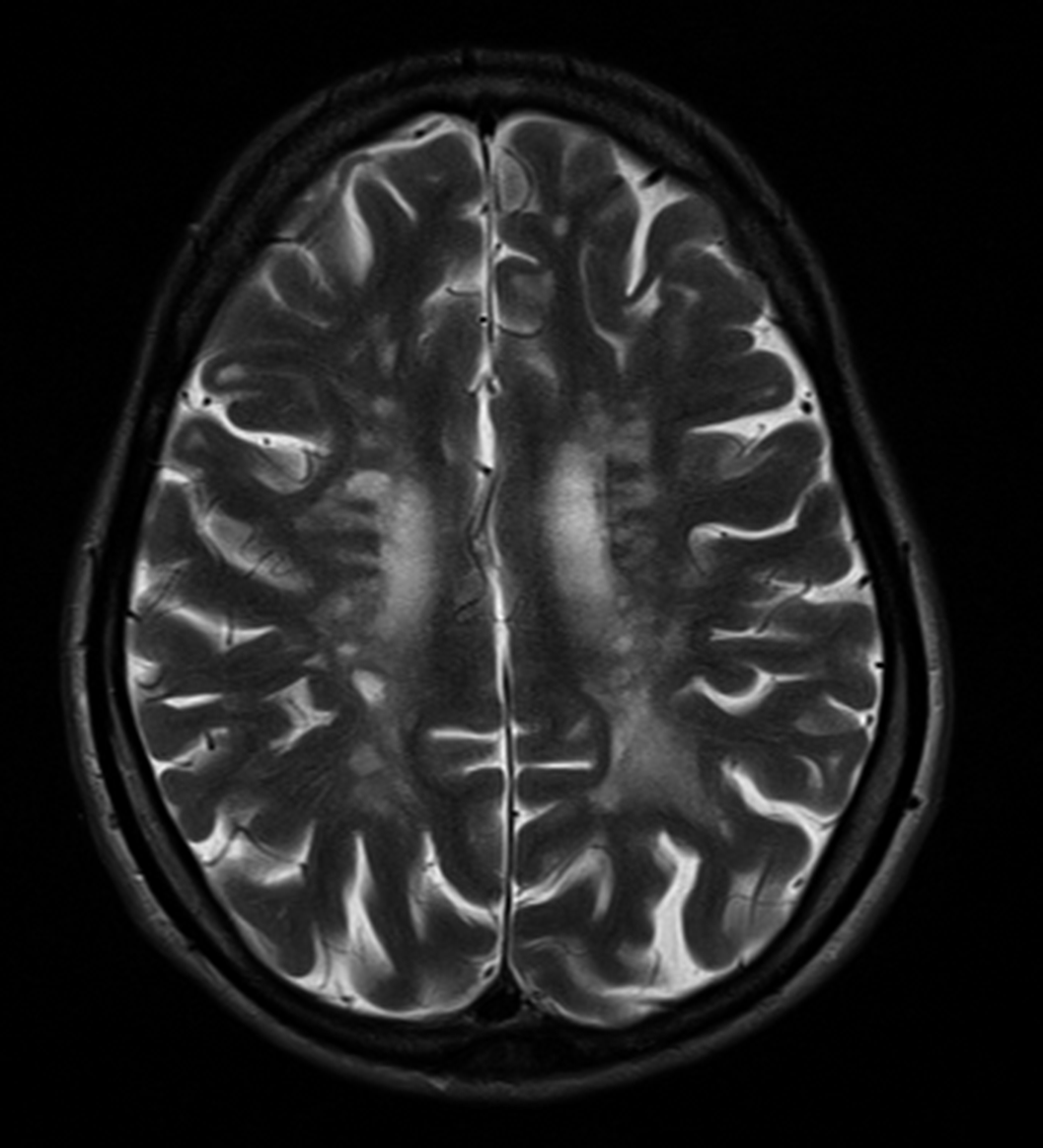
Image 2:
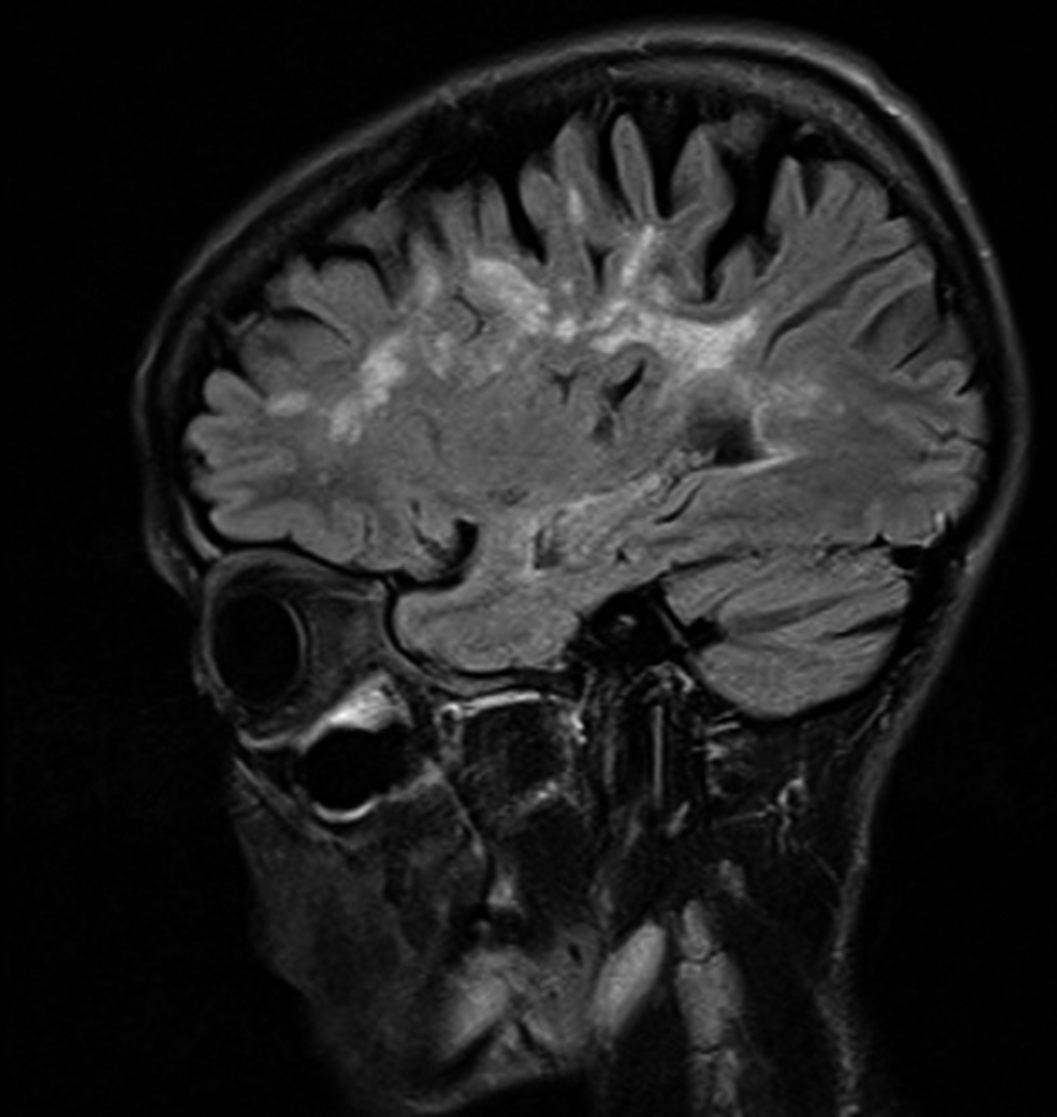 Conclusions
ConclusionsThe reformulation of the concept of cyclothymia would allow us to recognize in our patient a basic temperament of long evolution that would be the substrate on which different factors have subsequently influenced, such as antidepressant drugs or multiple sclerosis. In addition, it is necessary to know the association between BD and MS, in order to be able to offer an adequate treatment, contemplating some pharmacological options such as Lithium or some Atypical Antipsychotics, given the beneficial effect both for the affective disorder and for the neurological process.
Disclosure of InterestNone Declared





