3 results
Choroid plexus volume as a proxy of neuroinflammation in depression
- B. Bravi, E. Melloni, L. Servidio, E. Agnoletto, M. Paolini, S. Poletti, C. Lorenzi, C. Colombo, F. Benedetti
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S244-S245
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Choroid plexus (CP) is a physiological barrier, producing cerebrospinal fluid (CSF), neurotrophic, and inflammatory factors. It’s also involved in the neuro-immune axis, facilitating the interplay between central and peripheral inflammation, allowing trafficking of immune cells. Coherently, CP enlargement has been found in psychiatric diseases characterized by inflammatory signature. Although CP volume correlates with central microglia activation in major depressive disorder (MDD), it’s never been directly associated with peripheral markers in mood disorders.
ObjectivesExamine CP volume in mood disorders and healthy controls (HC) in relation to clinical features and peripheral inflammatory markers.
MethodsCP volume was extracted with FreeSurfer in 72 HC and 152 age- and sex-matched depressed patients: 79 BD and 73 MDD. Plasma analytes in patients were collected through immunoassay technology (Bioplex). We tested for the effect of age by group on CP volume. Then we focused on the interaction between illness duration and diagnosis in predicting CP volume. After testing the effect of specific analytes by diagnosis, we calculated moderated moderation models (SPSS, PROCESS) setting each analyte as independent variable, CP volume as predicted variable and illness duration and diagnosis as moderators. We get the effects’ significance with the likelihood ratio statistic, always controlling for age, sex, and intracranial volume.
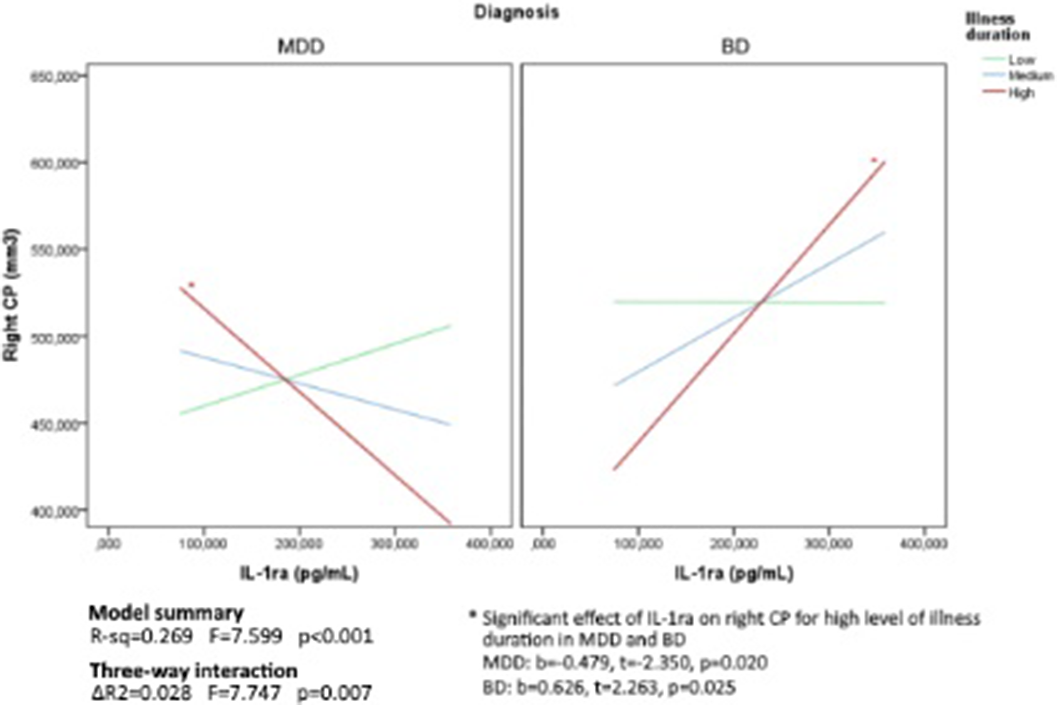
ResultsPatients were comparable in illness duration and severity. CP volume is differentially distributed through groups (right: p=0.04; left: p<0.01), with higher volumes in the clinical groups. Age by group significantly predict right CP volume (p=0.01). Also, duration of illness differently predicts right CP volume in MDD and BD (p=0.03) (Figure1). Then, given the significant interaction effect of IL13 (p=0.02) and IL1ra (p=0.01) in predicting right CP, we run the moderated moderation model. Longer illness duration has an effect in strengthening the opposite predicting value of IL1ra (ΔR2=0.03, p<0.01) on right CP volume in MDD and BD (Figure2).
Image:

Image 2:
 Conclusions
ConclusionsOur findings propose CP as a proxy of inflammation in depression, being significantly predicted by peripheral immune markers in MDD and BD. In particular, the signature of inflammation in depression, could represent the neurotoxic load of the disease over the illness, with a worse effect in BD, with possible disruption of brain barriers permeability and an opposite effect of tightening and central segregation in MDD. Further analyses are needed to better elucidate this neurobiological mechanisms across mood disorders.
Disclosure of InterestNone Declared
Mega-analysis of association between obesity and cortical morphology in bipolar disorders: ENIGMA study in 2832 participants
- Sean R. McWhinney, Christoph Abé, Martin Alda, Francesco Benedetti, Erlend Bøen, Caterina del Mar Bonnin, Tiana Borgers, Katharina Brosch, Erick J. Canales-Rodríguez, Dara M. Cannon, Udo Dannlowski, Ana M. Diaz-Zuluaga, Lorielle M.F. Dietze, Torbjørn Elvsåshagen, Lisa T. Eyler, Janice M. Fullerton, Jose M. Goikolea, Janik Goltermann, Dominik Grotegerd, Bartholomeus C. M. Haarman, Tim Hahn, Fleur M. Howells, Martin Ingvar, Neda Jahanshad, Tilo T. J. Kircher, Axel Krug, Rayus T. Kuplicki, Mikael Landén, Hannah Lemke, Benny Liberg, Carlos Lopez-Jaramillo, Ulrik F. Malt, Fiona M. Martyn, Elena Mazza, Colm McDonald, Genevieve McPhilemy, Sandra Meier, Susanne Meinert, Tina Meller, Elisa M. T. Melloni, Philip B. Mitchell, Leila Nabulsi, Igor Nenadic, Nils Opel, Roel A. Ophoff, Bronwyn J. Overs, Julia-Katharina Pfarr, Julian A. Pineda-Zapata, Edith Pomarol-Clotet, Joaquim Raduà, Jonathan Repple, Maike Richter, Kai G. Ringwald, Gloria Roberts, Alex Ross, Raymond Salvador, Jonathan Savitz, Simon Schmitt, Peter R. Schofield, Kang Sim, Dan J. Stein, Frederike Stein, Henk S. Temmingh, Katharina Thiel, Sophia I. Thomopoulos, Neeltje E. M. van Haren, Cristian Vargas, Eduard Vieta, Annabel Vreeker, Lena Waltemate, Lakshmi N. Yatham, Christopher R. K. Ching, Ole A. Andreassen, Paul M. Thompson, Tomas Hajek, for the ENIGMA Bipolar Disorder Working Group
-
- Journal:
- Psychological Medicine / Volume 53 / Issue 14 / October 2023
- Published online by Cambridge University Press:
- 27 February 2023, pp. 6743-6753
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background:
Obesity is highly prevalent and disabling, especially in individuals with severe mental illness including bipolar disorders (BD). The brain is a target organ for both obesity and BD. Yet, we do not understand how cortical brain alterations in BD and obesity interact.
Methods:We obtained body mass index (BMI) and MRI-derived regional cortical thickness, surface area from 1231 BD and 1601 control individuals from 13 countries within the ENIGMA-BD Working Group. We jointly modeled the statistical effects of BD and BMI on brain structure using mixed effects and tested for interaction and mediation. We also investigated the impact of medications on the BMI-related associations.
Results:BMI and BD additively impacted the structure of many of the same brain regions. Both BMI and BD were negatively associated with cortical thickness, but not surface area. In most regions the number of jointly used psychiatric medication classes remained associated with lower cortical thickness when controlling for BMI. In a single region, fusiform gyrus, about a third of the negative association between number of jointly used psychiatric medications and cortical thickness was mediated by association between the number of medications and higher BMI.
Conclusions:We confirmed consistent associations between higher BMI and lower cortical thickness, but not surface area, across the cerebral mantle, in regions which were also associated with BD. Higher BMI in people with BD indicated more pronounced brain alterations. BMI is important for understanding the neuroanatomical changes in BD and the effects of psychiatric medications on the brain.
List of contributors
-
- By H. Elliott Albers, Reut Avinun, Karen L. Bales, Jorge A. Barraza, Michael T. Bowen, Sunny K. Boyd, Heather K. Caldwell, Elena Choleris, Amy E. Clipperton-Allen, Bruce S. Cushing, Monica B. Dhakar, Riccardo Dore, Richard P. Ebstein, Craig F. Ferris, Sara M. Freeman, James L. Goodson, Joshua J. Green, Haruhiro Higashida, Eric Hollander, Salomon Israel, Martin Kavaliers, Keith M. Kendrick, Ariel Knafo, Yoav Litvin, Olga Lopatina, David Mankuta, Iain S. McGregor, Richard H. Melloni, Inga D. Neumann, Jerome H. Pagani, Cort A. Pedersen, Donald W. Pfaff, Anna Phan, Benjamin J. Ragen, Amina Sarwat, Idan Shalev, Erica L. Stevenson, Bonnie Taylor, Richmond R. Thompson, Florina Uzefovsky, Erwin H. van den Burg, James C. Walton, Scott R. Wersinger, Nurit Yirmiya, Larry J. Young, W. Scott Young, Paul J. Zak
- Edited by Elena Choleris, University of Guelph, Ontario, Donald W. Pfaff, Rockefeller University, New York, Martin Kavaliers, University of Western Ontario
-
- Book:
- Oxytocin, Vasopressin and Related Peptides in the Regulation of Behavior
- Published online:
- 05 April 2013
- Print publication:
- 11 April 2013, pp xi-xiv
-
- Chapter
- Export citation





