4 results
Disruptions to essential health services in Kenya during the COVID-19 pandemic – February 2020–May 2021
- Matthew Hudson, Carolyn Herzig, Godfrey Woelk, Evelyn Wesangula, Rhoderick Machekano, Rose Masaba, Benjamin Park, Elizabeth Bancroft
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, pp. s49-s50
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: The COVID-19 pandemic disrupted essential health services (EHS) delivery worldwide; however, there are limited data for healthcare facility (HCF)–level EHS disruptions in low- and middle-income countries. We surveyed HCFs in 3 counties in Kenya to understand the extent of and reasons for EHS disruptions occurring during February 2020–May 2021. Methods: We included 3 counties in Kenya with high burden of COVID-19 at the time of study initiation. Stratified sampling of HCFs occurred by HCF level. HCF administrators were interviewed to collect information on types of EHS disruptions that occurred and reasons for disruptions, including those related to infection prevention and control (IPC). Analyses included descriptive statistics with proportions for categorical variables and median with interquartile range (IQR) for continuous variables. Results: In total, 59 HCFs in Kenya provided complete data. All 59 HCFs (100%) reported EHS disruptions due to COVID-19. Among all HCFs, limiting patient volumes was the most common disruption reported (97%), while 56% of HCFs reduced staffing of EHS and 52% suspended EHS. Median duration of disruptions ranged from 7 weeks (IQR, 0–15) for inpatient ward closures to 25 weeks (IQR, 14–37) for limiting patient volumes accessing EHS. Among HCFs that reported disruptions, the most cited reason (ie, 95% of HCFs) was fewer patients receiving services. The most common IPC-related reason for disruption was diversion of resources to accommodate physical distancing measures (76%) followed by COVID-19 outbreaks among patients or staff (34%); staff shortages due to COVID-19 illness (25%) or perceived infection risk (19%); and lack of adequate personal protective equipment (20%). Conclusions: Most HCFs reported disruptions to EHS during the pandemic, including many that were related to IPC. Some disruptions may be mitigated by strengthening IPC infrastructure and practices, including protecting healthcare personnel to prevent staffing shortages.
Funding: None
Disclosures: None
Readiness assessment: Implications for COVID-19 infection prevention and control (IPC) preparedness in health facilities
- Evelyn Wesangula, Veronica Kamau, Felister Kiberenge, Emmanuel Tanui, Susan Githii, Linus Ndegwa, George Owiso, Irungu Kamau, Jennifer Njuhigu
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, pp. s79-s80
-
- Article
-
- You have access Access
- Open access
- Export citation
-
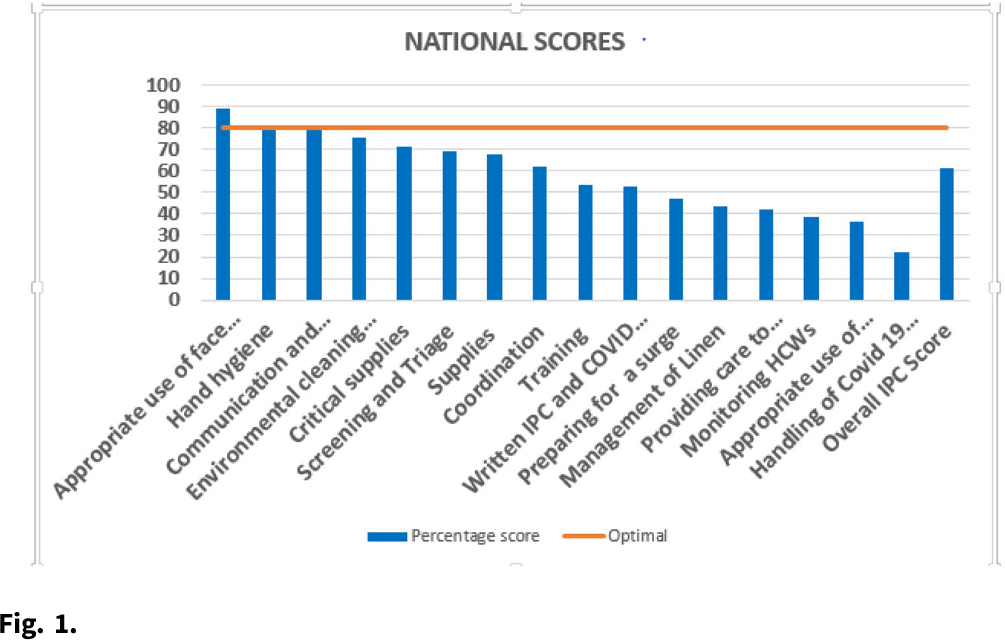
Background: Monitoring uptake of infection prevention and control (IPC) interventions is critical for the targeted and rational use of limited resources. A national facility readiness assessment conducted in August 2020 provided key information for targeted interventions to strengthen priority IPC areas. We assessed the level of COVID-19 preparedness in the facilities, identified priority COVID-19 IPC gaps, and generated a baseline report to further guide IPC investments at all levels. Methods: The Kenya Ministry of Health in collaboration with the CDC and International Training and Education Center for Health adapted a WHO Facility Readiness Assessment tool to include COVID-19–specific areas. In August 2020, data were collected using tablets through an Android-based electronic platform and were analyzed using descriptive statistics. Assessments were conducted in public, private, and faith-based health facilities nationally after 4 months of preparedness and investment in the healthcare system. Results: We assessed 684 facilities of the targeted 844 (81%). Overall facility readiness in Kenya was rated above average (61%), and the performance score significantly increased with the Kenya Essential Package for Health level, with level 5 and 6 facilities scoring an average of 83% and 79% respectively. Of the assessed facilities, 82% had an appointed IPC coordinator. Only 14% of the facilities had all the required guidelines, policies, and the appropriate COVID-19 case definitions. 67% of the facilities had updated supply inventories for past week. Only 50% of the facilities had adequate supplies of N95 masks. The assessment revealed that 52% of healthcare facilities had trained their healthcare workforce; morticians were the least trained (only 17% of facilities). Moreover, 41% of the facilities had clear work plans for monitoring healthcare workers exposures to COVID-19, but only 33% of the facilities had policies on the management of infected healthcare workers. Conclusions: The findings provided critical information for stakeholders at all levels to be used for policy decisions, to prioritize key intervention areas in leadership and governance of facility IPC programs, for guideline development, and for capacity building and targeted investment in IPC to improve COVID-19 facility preparedness.
Funding: None
Disclosures: None
Point-Prevalence Surveys of Antibiotic Use at Three Large Public Hospitals in Kenya
- Sylvia Omulo, Margaret Oluka, Loice Ombajo, Eric Osoro, Rosaline Kinuthia, Anastasia Guantai, Linus Ndegwa, Jennifer Verani, Sylvia Opanga, Evelyn Wesangula, Jarred Nyakiba, Jones Makori, Charles Kwobah, Wilson Sugut, Hanako Osuka, M. Kariuki Njenga, Douglas Call, Guy H. Palmer, Daniel VanderEnde, Ulzii-Oshikh Luvsansharav
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s353-s354
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Antibiotics are the most prescribed medicines worldwide, accounting for 20%–30% of total drug expenditures in most settings. Antimicrobial stewardship activities can provide guidance for the most appropriate antibiotic use. Objective: In an effort to generate baseline data to guide antimicrobial stewardship recommendations, we conducted point-prevalence surveys at 3 hospitals in Kenya. Methods: Sites included referral hospitals located in Nairobi (2,000 beds), Eldoret (900 beds) and Mombasa (700 beds). [Results are presented in this order.] Hospital administrators, heads of infection prevention and control units, and laboratory department heads were interviewed about ongoing antimicrobial stewardship activities, existing infection prevention and control programs, and microbiology diagnostic capacities. Patient-level data were collected by a clinical or medical officer and a pharmacist. A subset of randomly selected, consenting hospital patients was enrolled, and data were abstracted from their medical records, treatment sheets, and nursing notes using a modified WHO point-prevalence survey form. Results: Overall, 1,071 consenting patients were surveyed from the 3 hospitals (n = 579, n = 263, and n = 229, respectively) of whom >60% were aged >18 years and 53% were female. Overall, 489 of 1,071 of patients (46%) received ≥1 antibiotic, of whom 254 of 489 (52%) received 1 antibiotic, 201 of 489 (41%) received 2 antibiotics, 31 of 489 (6%) received 3 antibiotics, and 3 of 489 (1%) received 4 antibiotics. Antibiotic use was higher among those aged <5 years: 150 of 244 (62%) compared with older individuals (337 of 822, 41%). Amoxicillin/clavulanate was the most commonly used antibiotic (66 of 387, 17%) at the largest hospital (in Nairobi) whereas ceftriaxone was the most common at the other 2 facilities: 57 of 184 (31%) in Eldoret and 55 of 190 (29%) in Mombasa. Metronidazole was the next most commonly prescribed antibiotic (15%–19%). Meropenem was the only carbapenem reported: 22 of 387 patients (6%) in Nairobi, 2 of 190 patients (1%) in Eldoret, and 8 of 184 patients (4%) in Mombasa. Stop dates or review dates were not indicated for 106 of 390 patients (27%) in Nairobi, 75 of 190 patients (40%) in Eldoret, and 113 of 184 patients (72%) in Mombasa receiving antibiotics. Of 761 antibiotic prescriptions, 45% had a least 1 missed dose. Culture and antibiotic susceptibility tests were limited to 50 of 246 patients (20%) in Nairobi, 17 of 124 patients (14%) in Eldoret, and 23 of 119 patients (19%) in Mombasa who received antibiotics. The largest hospital had an administratively recognized antimicrobial stewardship committee. Conclusions: The prevalence of antibiotic use found by our study was 46%, generally lower than the rates reported in 3 similar studies from other African countries, which ranged from 56% to 65%. However, these survey findings indicate that ample opportunities exist for improving antimicrobial stewardship efforts in Kenya considering the high usage of empiric therapy and low microbiologic diagnostic utilization.
Funding: None
Disclosures: None
Improvement of Infection Prevention and Control Practices Using Quality Improvement Approach in Two Model Hospitals in Kenya
- Loyce Kihungi, Mary Ndinda, Samantha Dolan, Evelyn Wesangula, Linus Ndegwa, George Owiso, John Lynch, Lauren Frisbie, Peter Rabinowitz
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s286-s287
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Little is known about how best to implement infection prevention and control programs in low-resource settings. The quality improvement approach using plan-do-study-act (PDSA) cycles provides a framework for data-driven infection prevention and control implementation. We used quality improvement techniques and training to improve infection prevention and control practices in 2 model hospitals in Kenya. Methods: The 2 hospitals were chosen by the Kenya Ministry of Health for capacity building on infection prevention and control. At each site, the project team (the University of Washington International Training for Education and Training in Health, Ministry of Health, and Centers for Disease Control) conducted infection prevention and control training to infection prevention and control committee members. Infection prevention and control quality improvement activities were introduced in a staggered manner, focusing on hand hygiene and waste management practices. For hand hygiene, the project team’s technical assistance focused on facility hand hygiene infrastructure, hand hygiene practice adherence, hand hygiene supply quantification, and monitoring and evaluation using WHO hand hygiene audit tools. Waste management technical assistance focused on availability of policy, guidelines, equipment and supplies, waste segregation, waste quantification, and monitoring and evaluation using a data collection tool customized based on previously published tools. Regular interactive video conference sessions between the project team and the sites that included didactic sessions and sharing of data provided ongoing mentorship and feedback on quality improvement implementation, data interpretation, and data use. Results: Hand hygiene data collection began in April 2018. In hospital A, hand hygiene compliance increased from a baseline of 3% to 51% over 9 months. In Hospital B, hand hygiene compliance rates increased from 23% at baseline to 44% after 9 months. Waste management data collection began in November 2018. At hospital A, waste segregation compliance scores increased from 73% at baseline to 80% over 6 months, whereas hospital B, waste segregation compliance went from 44% to 80% over 6 months. Conclusions: A quality improvement approach appears to be a feasible means of infection prevention and control program strengthening in low resource settings.
Funding: None
Disclosures: None




