4 results
Transition to Psychosis in Individuals at Clinical High Risk: Meta-analysis
- G. Salazar De Pablo, J. Radua, I. Bonoldi, V. Arienty, F. Besana, A. Cabras, A. Catalan, P. Fusar-Poli
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S367
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Estimating the current likelihood of transitioning from a clinical high risk for psychosis (CHR-P) to psychosis holds paramount importance for preventive care and applied research.
ObjectivesOur aim was to quantitatively examine the consistency and magnitude of transition risk to psychosis in individuals at CHR-P.
MethodsThis meta-analysis is compliant with Preferred Reporting Items for Systematic Reviews and Meta-analyses (PRISMA) and Meta-analysis of Observational Studies in Epidemiology (MOOSE) reporting guidelines. PubMed and Web of Science databases were searched for longitudinal studies reporting transition risks in individuals at CHR-P.
Primary effect size was cumulative risk of transition to psychosis at 0.5, 1, 1.5, 2, 2.5, 3, 4, and more than 4 years’ follow-up, estimated using the numbers of individuals at CHR-P transitioning to psychosis at each time point. Random-effects meta-analysis were conducted.
ResultsA total of 130 studies and 9222 individuals at CHR-P were included. The mean (SD) age was 20.3 (4.4) years, and 5100 individuals (55.3%) were male.
The cumulative transition risk was 9% (95% CI = 7-10% k = 37; n = 6485) at 0.5 years, 15% (95% CI = 13-16%; k = 53; n = 7907) at 1 year, 20% (95% CI = 17%-22%; k = 30; n = 5488) at 1.5 years, 19% (95% CI = 17-22%; k = 44; n = 7351) at 2 years, 25% (95% CI, 21-29%) at 2.5 years, 25% (95% CI = 22-29%; k = 29; n = 4029) at 3 years, 27% (95% CI = 23-30%; k = 16; n = 2926) at 4 years, and 28% (95% CI = 20-37%; k = 14; n = 2301) at more than 4 years.
Meta-regressions showed that a lower proportion of female individuals (β = -0.02; 95% CI, -0.04 to -0.01) and a higher proportion of brief limited intermittent psychotic symptoms (β = 0.02; 95% CI, 0.01-0.03) were associated with an increase in transition risk. Other predictors were not statistically significant (p > 0.05).
Heterogeneity across the studies was high (I2 range, 77.91% to 95.73%).
ConclusionsIn this meta-analysis, 25% of individuals at CHR-P developed psychosis within 3 years. Transition risk continued increasing in the long term. Extended clinical monitoring and preventive care may be beneficial in this patient population.
Disclosure of InterestNone Declared
Relationship between elimination disorders and internalizing-externalizing problems in children: A systematic review and meta-analysis
- C. Aymerich, B. Pedruzo, M. Pacho, M. Laborda, J. Herrero, M. Bordenave, G. Salazar de Pablo, E. Sesma, A. Fernandez-Rivas, A. Catalan, M. Á. González-Torres
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S328-S330
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Elimination disorders (ED) include enuresis, defined as wetting from 5 years, and encopresis, defined as soiling from 4 years onwards after organic causes are excluded. They are highly prevalent in childhood and often associated with clinically relevant comorbid psychological disorders. However, no systematic review or meta-analysis examines their co-occurrence with internalizing and externalizing problems in children.
ObjectivesThe aim of this study is to determine if, and to what extent, children with ED show higher internalizing and externalizing problems than their healthy peers.
MethodsA multistep literature search was performed from database inception until May 1st, 2022. PRISMA/MOOSE-compliant systematic review (PROSPERO: CRD42022303555) were used to identify studies reporting on internalizing and/or externalizing symptoms in children with an ED and a healthy control (HC) group. First, a systematic review was provided. Second, where data allowed for it, a quantitative meta-analysis using random effects model was conducted to analyze the differences between the ED and the HC groups for internalizing and externalizing symptoms. Effect size was standardized mean difference. Meta-regression analyses were conducted to examine the effect of sex, age, and study quality. Funnel plots were used to detect a publication bias. Where found, the trim and fill method was used to correct it.
Results36 articles were included, 32 of them reporting on enuresis (n=3244; mean age=9.4; SD=3.4; 43.84% female) and 7 of them on encopresis (n=214; mean age=8.6; SD=2.3; 36.24% female) [Image 1]. The ED group presented significantly lower self-concept (ES:0.42; 95%CI: [0.08;9.76]; p=0.017) and higher symptom scores for thought problems (ES:-0.26; 95%CI: [-0.43;-0.09]; p=0.003), externalizing symptoms (ES:-0.20; 95%CI: [-0.37;-0.03]; p=0.020), attention problems (ES:-0.37; 95%CI: [-0.51;-0.22]; p=0.0001), aggressive behaviour (ES:-0.33; 95%CI: [-0.62;-0.04]; p=0.025) and social problems (ES: 0.39; 95%CI: [-0.58;-0.21]; p=0.0001) [Image 2]. Significant publication biases were found across several of the studied domains [Image 3]. No significant effect of sex, age or quality of the study score was found.
Image:
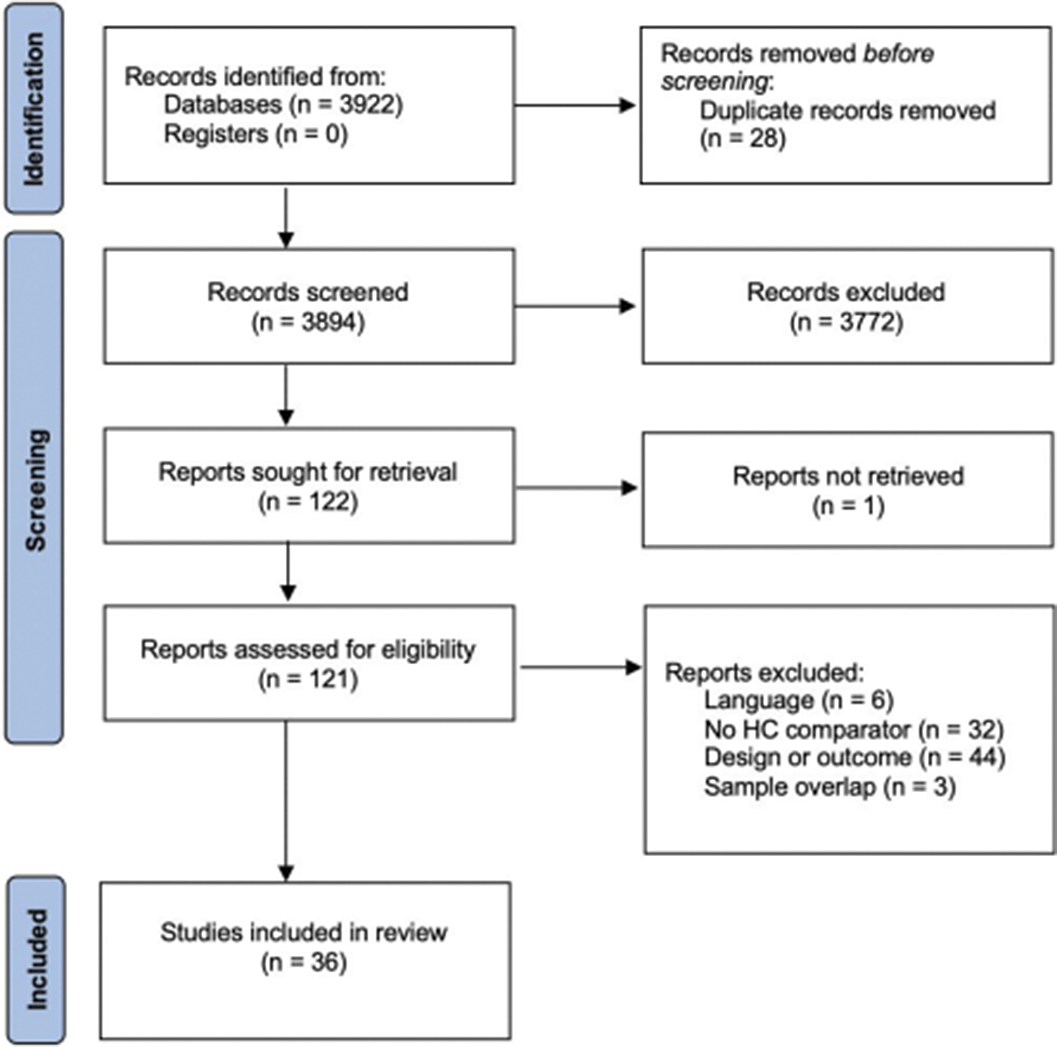
Image 2:
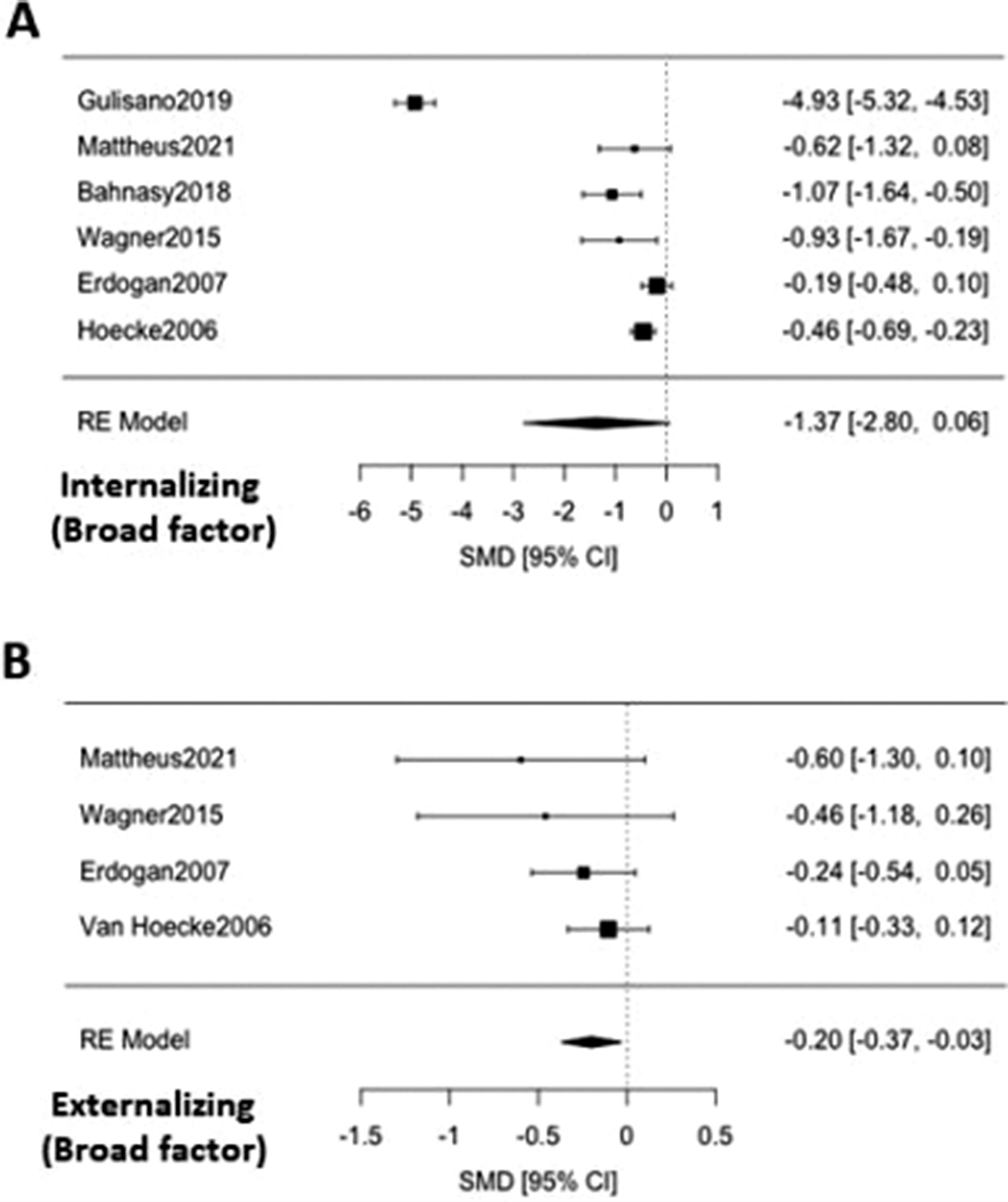
Image 3:
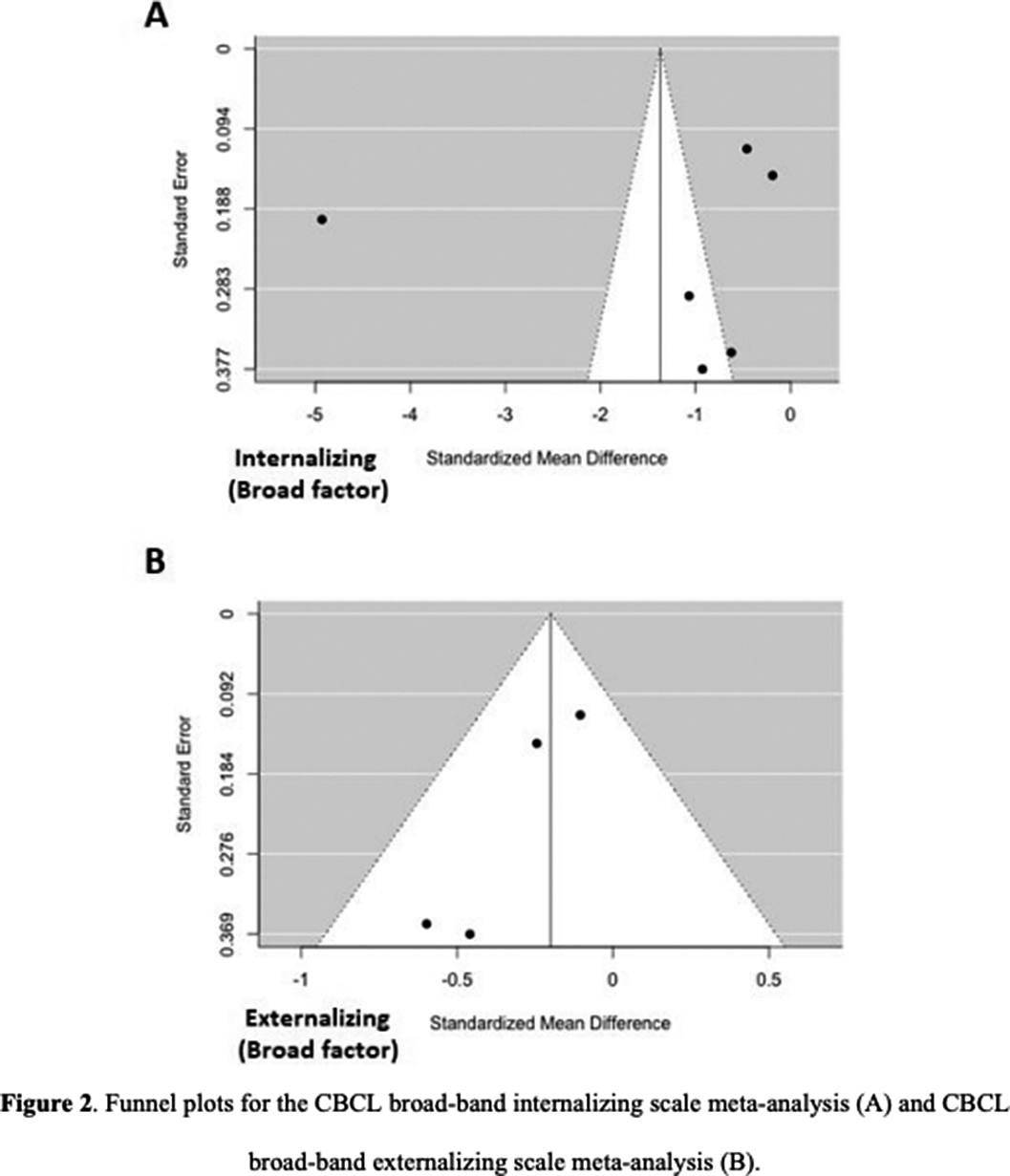 Conclusions
ConclusionsChildren with an elimination disorder may have significant internalizing and externalizing problems, as well as impaired self-concept. It is recommendable to screen for them in children with ED and provide interventions as appropriate.
Disclosure of InterestNone Declared
Catatonia in autism spectrum disorders: A systematic review and meta-analysis
- J. Vaquerizo-Serrano, G. Salazar De Pablo, J. Singh, P. Santosh
-
- Journal:
- European Psychiatry / Volume 65 / Issue 1 / 2022
- Published online by Cambridge University Press:
- 15 December 2021, e4
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
Catatonic features can appear in autism spectrum disorders (ASDs). There can be overlap in symptoms across catatonia and ASD. The overall aim of this review is to provide evidence for the presence of catatonic features in subjects with ASD.
MethodsA systematic literature search using the Web of Science database from inception to July 10, 2021 was conducted following PRISMA, MOOSE guidelines and the PROSPERO protocol. (CRD42021248615). Twelve studies with information about catatonia and ASD were reviewed. Data from a subset was used to conduct meta-analyses of the presence of catatonia in ASD.
ResultsThe systematic review included 12 studies, seven of which were used for the meta-analysis, comprising 969 individuals. The mean age was 21.25 (7.5) years. Two studies (16.6%) included only children and adolescents. A total of 70–100% were males. Our meta-analysis showed that 10.4% (5.8–18.0 95%CI) of individuals with ASD have catatonia. Motor disturbances were common in ASD subjects with catatonia. No differences were found in comorbidity. Several treatments have been used in ASD with catatonic features, including benzodiazepines, antipsychotics, and electroconvulsive therapy (ECT). The findings of the systematic review showed that ECT might help manage catatonic symptoms.
ConclusionsDifferent features of catatonia can exist in individuals with ASD and core symptoms of catatonia are reported in ASD. Longitudinal and longer-term studies are required to understand the relationship between catatonia and ASD, and the response of catatonic symptoms to treatment.
Clinical outcomes in brief psychotic episodes: a systematic review and meta-analysis
- U. Provenzani, G. Salazar de Pablo, M. Arribas, F. Pillmann, P. Fusar-Poli
-
- Journal:
- Epidemiology and Psychiatric Sciences / Volume 30 / 2021
- Published online by Cambridge University Press:
- 04 November 2021, e71
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Aims
Patients with brief psychotic episodes (BPE) have variable and fluctuating clinical outcomes which challenge psychiatric care. Our meta-analysis aims at providing a comprehensive summary of several clinical outcomes in this patient group.
MethodsA multistep systematic PRISMA/MOOSE-compliant literature search was performed for articles published from inception until 1st March 2021. Web of Science database was searched, complemented by manual search of original articles reporting relevant outcomes (psychotic recurrence, prospective diagnostic change or stability, remission, quality of life, functional status, mortality and their predictors) for patients diagnosed with acute and transient psychotic disorders (ATPD), brief psychotic disorders (BPD), brief intermittent psychotic symptoms (BIPS) and brief limited intermittent psychotic symptoms (BLIPS). Random-effects methods and Q-statistics were employed, quality assessment with Newcastle-Ottawa Scale, assessment of heterogeneity with I2 index, sensitivity analyses (acute polymorphic psychotic disorders, APPD) and multiple meta-regressions, assessment of publication bias with funnel plot, Egger's test and meta-regression (psychotic recurrence and sample size).
ResultsA total of 91 independent articles (n = 94 samples) encompassed 37 ATPD, 24 BPD, 19 BLIPS and 14 BIPS samples, totalling 15 729 individuals (mean age: 30.89 ± 7.33 years, mean female ratio: 60%, 59% conducted in Europe). Meta-analytical risk of psychotic recurrence for all BPE increased from 15% (95% confidence interval (CI) 12–18) at 6 months, 25% (95% CI 22–30) at 12 months, 30% (95% CI 27–33) at 24 months and 33% (95% CI 30–37) at ⩾36 months follow-up, with no differences between ATPD, BPD, BLIPS and BIPS after 2 years of follow-up. Across all BPE, meta-analytical proportion of prospective diagnostic stability (average follow-up 47 months) was 49% (95% CI 42–56); meta-analytical proportion of diagnostic change (average follow-up 47 months) to schizophrenia spectrum psychoses was 19% (95% CI 16–23), affective spectrum psychoses 5% (95% CI 3–7), other psychotic disorders 7% (95% CI 5–9) and other (non-psychotic) mental disorders 14% (95% CI 11–17). Prospective diagnostic change within APPD without symptoms of schizophrenia was 34% (95% CI 24–46) at a mean follow-up of 51 months: 18% (95% CI 11–30) for schizophrenia spectrum psychoses and 17% (95% CI 10–26) for other (non-psychotic) mental disorders. Meta-analytical proportion of baseline employment was 48% (95% CI 38–58), whereas there were not enough data to explore the other outcomes. Heterogeneity was high; female ratio and study quality were negatively and positively associated with risk of psychotic recurrence, respectively. There were no consistent factor predicting clinical outcomes.
ConclusionsShort-lived psychotic episodes are associated with a high risk of psychotic recurrences, in particular schizophrenia spectrum disorders. Other clinical outcomes remain relatively underinvestigated. There are no consistent prognostic/predictive factors.






