2 results
The prevalence of abnormal spirometry in children with CHD
- Geena Y. Zhou, Daniel Cerrone, Katherine Lewinter, Imran Masood, Jon Detterich, Sasha Singh, Payal Shah, Thomas Keens, Arash Sabati, Roberta Kato
-
- Journal:
- Cardiology in the Young / Volume 33 / Issue 12 / December 2023
- Published online by Cambridge University Press:
- 31 March 2023, pp. 2548-2552
-
- Article
- Export citation
-
Background:
The burden of pulmonary disease in children with CHD remains under-recognised. Studies have examined children with single ventricle and two ventricle heart disease and documented a decreased forced vital capacity. Our study sought to further explore the pulmonary function of children with CHD.
Methods:A retrospective review was performed of spirometry in CHD patients over a 3-year period. Spirometry data were corrected for size, age, and gender and analysed using z-scores.
Results:The spirometry of 260 patients was analysed. About 31% had single ventricle (n = 80, 13.6 years (interquartile range 11.5-16.8)) and 69% had two ventricle circulation (n = 180, 14.4 years (interquartile range 12.0-17.3)). Single ventricle patients were found to have a lower median forced vital capacity z-score compared to two ventricle patients (p = 0.0133). The prevalence of an abnormal forced vital capacity was 41% in single ventricle patients and 29% in two ventricle patients. Two ventricle patients with tetralogy of Fallot and truncus arteriosus had similar low forced vital capacity comparable to single ventricle patients. The number of cardiac surgeries predicted an abnormal forced vital capacity in two ventricle patients except tetralogy of Fallot patients.
Conclusion:Pulmonary morbidity in patients with CHD is common with a decreased forced vital capacity noted in single ventricle and two ventricle patients. Forced vital capacity is lower in patients with single ventricle circulation; however, two ventricle patients with tetralogy of Fallot or truncus arteriosus have similar lung function in comparison to the single ventricle group. The number of surgical interventions was predictive of forced vital capacity z-score in some but not all two ventricle patients and not predictive in single ventricle patients suggesting a multifactorial to pulmonary disease in children with CHD.
Optimizing COVID-19 Symptom Screening in the Pediatric Population
- Geena Zhou, Prachi Singh, Emily R. Perito, Naomi Bardach, Nicole Penwill, William Burrough, Ann Cheung, Margaret Nguyen, Shalini Mittal, Grace Cheng, Mia-Ashley Spad
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue S1 / July 2021
- Published online by Cambridge University Press:
- 29 July 2021, pp. s55-s56
-
- Article
-
- You have access Access
- Open access
- Export citation
-
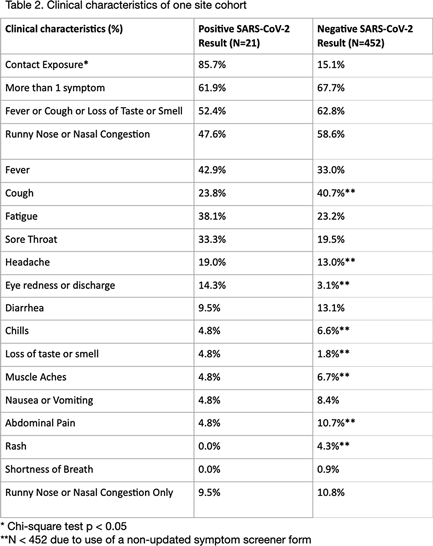
Background: Research analyzing COVID-19 symptom screening has primarily focused on adult patients. In efforts to safely reopen schools, symptom screeners are being widely utilized. However, pediatric-specific outpatient data on which symptom combinations best identify children with COVID-19 are lacking. Such data could refine school symptom screening by improving screener sensitivity and specificity. In this study, we assessed the frequency of symptoms and symptom combinations in children tested for SARS-CoV-2 in outpatient settings. We aim to contribute to the optimization of pediatric COVID-19 screening questionnaires, to ultimately minimize both COVID-19 transmission in schools and missed school days. Methods: We conducted a retrospective analysis of outpatient symptoms screens, SARS-CoV-2 test results, and demographics of children (≤18 years) tested for SARS-CoV-2 between March 30 and November 30, 2020, at 3 UCSF-affiliated COVID-19 outpatient screening clinics in northern California. Those with incomplete symptom screens, >7 days between symptom documentation and test, and invalid test results were excluded. Results: Of 473 children tested at 1 site, 21 children had positive SARs-CoV-2 results and 452 children had negative results (4.4% positivity rate). Moreover, 85.7% of SARS-CoV-2–positive children had a known exposure to COVID-19 (Table 1). Of SARS-CoV-2–positive children, 61.9% had >1 symptom. Also, 52.4% of SARS-CoV-2–positive children had at least 1 symptom (fever, cough, or loss of taste or smell) versus 62.8% of SARS-CoV-2–negative children (Table 2). Runny nose or nasal congestion was the most frequently reported symptom in the SARS-CoV-2–positive group (47.6%) as well as the SARS-CoV-2–negative group (58.6%). Also, 14.3% of SARS-CoV-2–positive children had eye redness or discharge versus 3.1% of SARS-CoV-2–negative children. Isolated runny nose presented in 10.8% of SARS-CoV-2–negative versus 9.5% of SARS-CoV-2–positive children. All children with isolated diarrhea (n = 5), isolated headache (n = 3), and isolated rash (n = 2) tested negative. Preliminary symptom data based on 176 children from a second site showed that 9.9% of symptomatic children had a positive test result. Conclusions: Runny nose or nasal congestion was the most frequently reported symptom in all children tested for SARS-CoV-2. However, isolated runny nose or nasal congestion identified 2 cases of COVID-19 in our cohort. Eye redness or discharge may be an important symptom to screen for COVID-19 in children. Further research with a larger number of positive cases is needed to make conclusions about improving efficiency and efficacy of symptom screeners for COVID-19 in children.
Funding: No
Disclosures: None
Table 1. 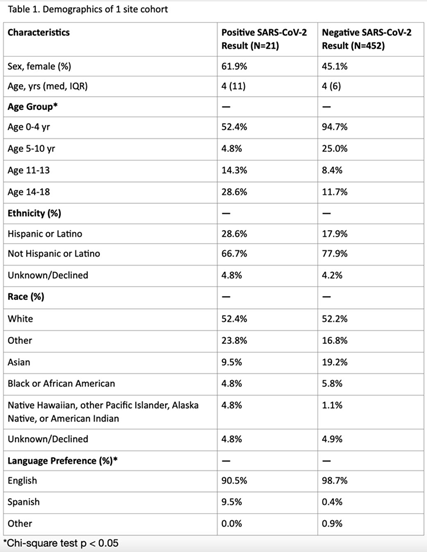
Table 2.