7 results
55 Psychometric Properties of the Verbal Series Attention Test: Preliminary Findings
- Stephen R McCauley, Michele K York, Adriana M Strutt, Jennifer M Stinson, Samantha K Henry, Victoria A Windham, Victoria Armendariz, Melany Land, Kevin D Nguyen
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 733-734
-
- Article
-
- You have access Access
- Export citation
-
Objective:
To investigate the latent factor structure and construct validity of the Verbal Series Attention Test (VSAT) across clinical patient populations.
Participants and Methods:Participants included a consecutive series of clinical patients presenting with a primary memory complaint. Each patient underwent a comprehensive neuropsychological assessment and provided informed consent to allow their clinical data to be used for research. Groups formed included 1) No Neurocognitive Disorder [NoND, N=262, mean age=68.8, mean education=16.2, mean MMSE=28.3], 2) Mild Neurocognitive Disorder [MildND, N=337, mean age=72.3, mean education=15.4, mean MMSE=28.7], and 3)
Major Neurocognitive Disorder [MajorND, N=524, mean age=76.5, mean education=14.5, mean MMSE=19.0] with etiologies including suspected Alzheimer’s disease and/or vascular pathology. Latent factors were investigated using exploratory factor analysis (EFA).
Results:EFA was conducted using SAS 9.4 software and the promax (oblique) rotation to reveal the latent factors of the eight timed items of the VSAT in each of the three clinical groups. The structure was essentially identical in all three groups with two primary factors consistently emerging identified as 1-Complex Attention and 2-Simple Attention. Each factor had four items loading with a correlation range of > 0.37 x < 0.92. The internal consistency (Cronbach’s alpha) for the VSAT total score in each group was excellent (NoND a=0.83, MildND a=0.81, and MajorND a=0.84). To investigate construct validity, the VSAT items were entered into factor analysis with measures of attention and executive function (i.e., Digit Span [forward, backward, sequence], Trail Making Test A & B, semantic fluency (animals), Controlled Oral Word Association Test [COWAT, FAS]). All three patient groups were combined (N=950) given the VSAT’s consistent factor structure. Using the same EFA procedure as before, two main factors emerged with the VSAT Complex Attention variables loading on a general complex attention/working memory factor including Trails B, semantic fluency, and Digit Span subtests. The VSAT Simple Attention items loaded on a general attention factor with the VSAT Simple Attention variables and Trails A. COWAT did not load significantly on either factor.
Conclusions:The latent factor structure of the VSAT was consistent across patient populations with excellent internal consistency in each clinical group. The Complex and Simple Attention factors of the VSAT loaded on factors with similar variables identifying the anticipated latent factor structure demonstrating the construct validity of the VSAT across a wide spectrum of cognitive impairment in patients with primary memory complaints ranging from NoND to MajorND. This supports the use of the VSAT in patients across neurocognitive severity. Future studies will further explore additional psychometric properties of this instrument.
36 Disparities in General Mental Status Between Lower and Higher SES Ethnically Diverse Older Adults
- Donna M. Talavari, Samantha K. Henry, Jennifer M. Stinson, Victoria Armendariz, Victoria Windham, Adriana M. Strutt
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 448-449
-
- Article
-
- You have access Access
- Export citation
-
Objective:
To investigate differences in performance on a widely used cognitive screener between community-dwelling older adults from two disparate socioeconomic groups.
Participants and Methods:Participants were part of a larger study of cognitive screening in healthy older adults. The total sample (N=79, 69.6% female, 19% White/Caucasian, 12.7% Asian, 43% Latino/a, 25.3% Black/African-American) consisted of community-dwelling adults (Mage=73.1 years [SD=7.2] and Meducation=14.3 years [SD=2.6]) who were initially recruited via social media, flyers, and general community announcements. A lack of ethnic minority participants resulted in a two-year commitment to reach communities of color via visits and provision of health literacy to local religious and community programs. Continuous contact with leaders/gatekeepers helped establish research study credibility and forge a stronger sense of trust among ethnically diverse participants in the greater Houston, TX, area. Testing was initially conducted at the clinical study site. Due to low participation rates among people of color, greater effort was placed on tailored strategies to overcome economic and time constraints (i.e., schedule/time conflicts, lack of transportation, inability to pay for parking). To fit the priorities and needs of the participants, testing was also conducted at their homes (25.3%) and nearby religious and community centers (22.8%). Participants identifying as Latino/a or Black were predominantly recruited and tested at their local community center (as requested by gatekeepers/participants) to increase access to the study, in contrast to Caucasian participants. Median income estimates were used to stratify participants by socioeconomic status (SES) based on zip codes into low SES (L-SES) or high SES (H-SES) groups.
Results:Participants from the L-SES group had significantly lower total scores on the MoCA than their H-SES counterparts, t(77J=2.837, p=0.003, g=0.696. The average MoCA total score for participants from the L-SES group was 2.64 points lower. The observed differences in MoCA total score when stratifying by ethnicity may be attributable to differences in education level and SES, which are known risk factors for cognitive impairment and will be further examined upon recruitment completion.
Conclusions:Studies have found that ethnically diverse older adults not only encounter more barriers to accessing quality health care but also experience disparities in brain health research. Communities of color comprise a sizeable portion of our older adults but have been traditionally underrepresented in clinical research, limiting the generalizability of research findings to clinical treatment. Socioeconomic deprivation has been identified as one of several barriers to research engagement for people of color, placing ethnic communities at increased risk for under- or misdiagnosis and limited access to medical intervention. Preliminary findings have implications for the recruitment of ethnically diverse groups in clinical research. Given the growing racial and ethnic diversity among the United States population, we must do our due diligence to increase understanding of participation and recruitment barriers for racial/ethnic individuals. Tailored community outreach and engagement strategies may be effective in improving the inclusion of ethnically diverse populations and facilitating recruitment and retention in clinical research studies.
75 Mood and Quality of Life after Responsive Neurostimulation (RNS) in Epilepsy Patients
- Stephanie Santiago Mejias, Zulfi Haneef, Adriana M. Strutt, Michele K. York, Stephen R. McCauley, Samantha K. Henry, Jennifer M. Stinson
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 480-481
-
- Article
-
- You have access Access
- Export citation
-
Objective:
Poor mood and quality of life is common among patients with medically intractable seizures. Many of these patients are not candidates for seizure focus resection and continue to receive standard medical care. Responsive neurostimulation (RNS) has been an effective approach to reduce seizure frequency for nonsurgical candidates. Previous research using RNS clinical trial participants has demonstrated improved mood and quality of life when patients received RNS-implantation earlier in their medically resistant epilepsy work-up (Loring et al., 2021). We aimed to describe the level of depression and quality of life in adults with medical resistant epilepsy, treated with RNS, presenting to an outpatient clinic.
Participants and Methods:This pilot study was conducted among 11 adult epilepsy patients treated with RNS at the epilepsy specialty clinic at Baylor College of Medicine. Ages of participants ranged from 18-56 (M=32.01, SD=12.37) with a mean education of 12.43 (SD=0.85). The majority of the participants identified as White (White=72.2%; Hispanic/Latino/a=14.3%, Other=7.1%). We also present pre- and post-RNS preliminary results of a subset of 4 patients for whom pre and post implantation data was available. Depression symptoms were assessed through the Beck Depression Inventory, 2nd Edition (BDI-II) and quality of life was determined using the Quality of Life in Epilepsy (QoLiE-31).
Results:Patients reported minimal symptoms of depression (M=5.45, SD=4.03) and good overall quality of life (M=71.18, SD=14.83) after RNS. Participants’ scores on their overall quality of life ranged from 50 to 95 (100=better quality of life). The QoLiE-31 showed high scores on emotional wellbeing (M=69.45, SD=14.56) and cognitive functioning (M=65.36, SD=16.66) domains. Post-hoc analysis revealed a significant difference in the cognitive functioning domain of QoLiE-31 before (M=44.75, SD=12.58) and after (M=51.0, SD=11.58) RNS implantation(t(3)=-3.78, p=0.016. Additionally, overall QoLiE score approached statistical significance when comparing pre-RNS (M=44.75 SD=9.29) to post-RNS (M=49.75 SD=11.62; t(3)=-2.01, p = 0.069). No significant differences were evident on seizure worry, energy/fatigue, medication effects, and social functioning domains of QoLiE-31 before and after RNS treatment.
Conclusions:These pilot study results suggest low levels of depression with this population post-RNS implantation. Additionally, there is preliminary evidence to suggest improved patient-rated cognitive functioning and overall quality of life. While this is a small study population, the results have important implications for patients with intractable epilepsy, even with those form who surgical resection may not be possible. Future studies with large enough samples to examine moderating and mediating factors to mood and quality of life changes post-RNS will be important.
Exploring the needs of children and caregivers to inform design of an artificial intelligence-enhanced social robot in the pediatric emergency department
- Fareha Nishat, Summer Hudson, Prabdeep Panesar, Samina Ali, Sasha Litwin, Frauke Zeller, Patricia Candelaria, Mary Ellen Foster, Jennifer Stinson
-
- Journal:
- Journal of Clinical and Translational Science / Volume 7 / Issue 1 / 2023
- Published online by Cambridge University Press:
- 24 August 2023, e191
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background & Objective:
Socially assistive robots (SARs) are a promising tool to manage children’s pain and distress related to medical procedures, but current options lack autonomous adaptability. The aim of this study was to understand children’s and caregivers' perceptions surrounding the use of an artificial intelligence (AI)-enhanced SAR to provide personalized procedural support to children during intravenous insertion (IVI) to inform the design of such a system following a user-centric approach.
Methods:This study presents a descriptive qualitative needs assessment of children and caregivers. Data were collected via semi-structured individual interviews and focus groups. Participants were recruited from two Canadian pediatric emergency departments (EDs) between April 2021 and January 2022.
Results:Eleven caregivers and 19 children completed 27 individual interviews and one focus group. Three main themes were identified: A. Experience in the clinical setting, B. Acceptance of and concerns surrounding SARs, and C. Features that support child engagement with SARs. Most participants expressed comfort with robot technology, however, concerns were raised about sharing personal information, photographing/videotaping, and the possibility of technical failure. Suggestions for feature enhancements included increasing movement to engage a child’s attention and tailoring language to developmental age. To enhance the overall ED experience, participants also identified a role for the SAR in the waiting room.
Conclusion:Artificial intelligence-enhanced SARs were perceived by children and caregivers as a promising tool for distraction during IVIs and to enhance the overall ED experience. Insights collected will be used to inform the design of an AI-enhanced SAR.
Mixed-methods process evaluation of a respiratory-culture diagnostic stewardship intervention
- Kathleen Chiotos, Deanna Marshall, Katherine Kellom, Jennifer Whittaker, Heather Wolfe, Charlotte Woods-Hill, Hannah Stinson, Garrett Keim, Jennifer Blumenthal, Joseph Piccione, Giyoung Lee, Guy Sydney, Jeffrey Gerber
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 2 / February 2023
- Published online by Cambridge University Press:
- 03 January 2023, pp. 191-199
- Print publication:
- February 2023
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Objective:
To conduct a process evaluation of a respiratory culture diagnostic stewardship intervention.
Design:Mixed-methods study.
Setting:Tertiary-care pediatric intensive care unit (PICU).
Participants:Critical care, infectious diseases, and pulmonary attending physicians and fellows; PICU nurse practitioners and hospitalist physicians; pediatric residents; and PICU nurses and respiratory therapists.
Methods:This mixed-methods study was conducted concurrently with a diagnostic stewardship intervention to reduce the inappropriate collection of respiratory cultures in mechanically ventilated children. We quantified baseline respiratory culture utilization and indications for ordering using quantitative methods. Semistructured interviews informed by these data and the Consolidated Framework for Implementation Research (CFIR) were then performed, recorded, transcribed, and coded to identify salient themes. Finally, themes identified in these interviews were used to create a cross-sectional survey.
Results:The number of cultures collected per day of service varied between attending physicians (range, 2.2–27 cultures per 100 days). In total, 14 interviews were performed, and 87 clinicians completed the survey (response rate, 47%) and 77 nurses or respiratory therapists completed the survey (response rate, 17%). Clinicians varied in their stated practices regarding culture ordering, and these differences both clustered by specialty and were associated with perceived utility of the respiratory culture. Furthermore, group “default” practices, fear, and hierarchy were drivers of culture orders. Barriers to standardization included fear of a missed diagnosis and tension between practice standardization and individual decision making.
Conclusions:We identified significant variation in utilization and perceptions of respiratory cultures as well as several key barriers to implementation of this diagnostic test stewardship intervention.
Indications for and Utility of Tracheal Aspirate Cultures for the Diagnosis of VAI
- Kathleen Chiotos, Giyoung Lee, Guy Sydney, Heather Wolfe, Jennifer Blumenthal, Hannah Stinson, Julie Harab, Danielle Traynor, Joseph Piccione, Ashlee Doll, Garrett Keim, Charlotte Woods-Hill, Megan Jennings, Rebecca Harris, Jeffrey Gerber, Aaditya Dudhia, Nancy McGowan, Jennalyn Burke
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue S1 / July 2021
- Published online by Cambridge University Press:
- 29 July 2021, pp. s60-s61
-
- Article
-
- You have access Access
- Open access
- Export citation
-
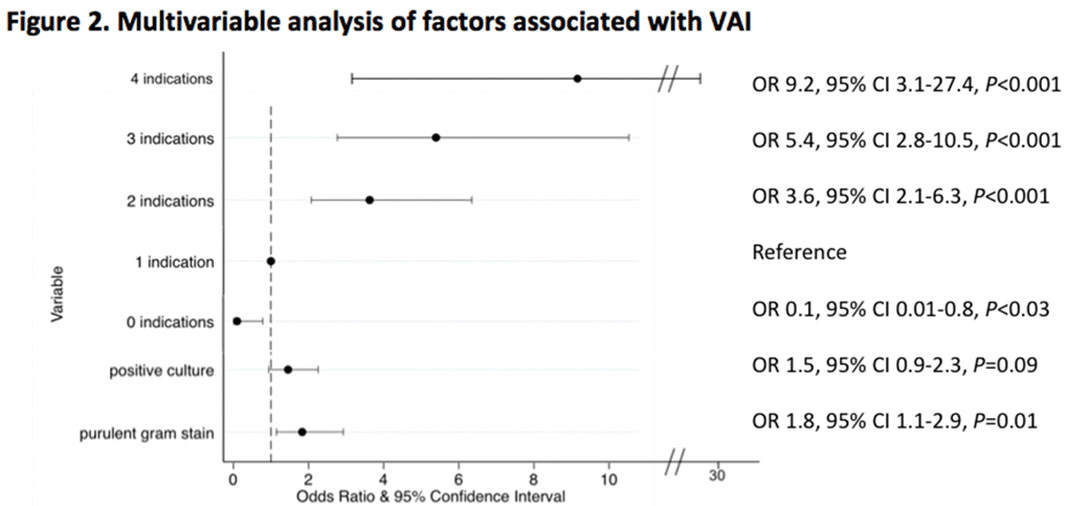
Background: Tracheal aspirate bacterial cultures are routinely collected in mechanically ventilated children for the evaluation of ventilator-associated infections (VAIs). However, frequent bacterial colonization of endotracheal and tracheostomy tubes contribute to the marginal performance characteristics of the test for diagnosing VAI. Published literature characterizing drivers of culture collection and the predictive value of positive cultures are limited. Methods: This single-center, retrospective cohort study included children admitted to the pediatric intensive care unit who were receiving mechanical ventilation for at least 48 hours and had 1 or more semiquantitative tracheal aspirate cultures collected between September 1, 2019, and August 31, 2020. Indications for culture collection were determined through medical record review and included fever, hypothermia, tracheal secretion changes, radiographic pneumonia, increased oxygen requirement, and/or increased positive end-expiratory pressure (PEEP). A positive culture was defined as moderate or heavy growth of a noncommensal bacterial organism. A purulent Gram stain was defined as detection of moderate or many white blood cells. Diagnosis of VAI was based on treating-clinician documentation and was ascertained through medical record review. Logistic regression accounting for clustering by patient was performed to estimate the association between indications for culture collection and (1) culture positivity, (2) purulent Gram stain, and (3) diagnosis of VAI. Results: In total, 625 tracheal aspirate cultures were performed in 261 unique patients. Common indications for culture collection included isolated fever or hypothermia (n = 124, 20%), fever with an increase in oxygen requirement or PEEP (n = 71, 11%), isolated increase in oxygen requirement or PEEP (n = 67, 11%), or isolated secretion change (n = 54, 9%) (Figure 1). Overall, 230 cultures (37%) were positive and 218 (35%) Gram stains were purulent. There were no associations between culture indications and a positive culture. Presence of isolated fever was negatively associated with a purulent Gram stain (odds ratio [OR], 0.49; 95% CI, 0.30–0.81; P = .005); otherwise, there were no associations between indication and purulent Gram stain. Finally, in a multivariable model, odds of VAI diagnosis increased with both the number of indications for culture collection and purulent Gram stain, but not with positive culture (Figure 2). Conclusions: Number and type of clinical signs were not associated with tracheal aspirate culture positivity or purulence on Gram stain, but they were associated with a clinical diagnosis of VAI. These findings suggest that positive tracheal aspirate cultures may not aid clinicians in the diagnosis of VAI, and they highlight the opportunity for improved diagnostic stewardship.
Funding: No
Disclosures: None
Figure 1.
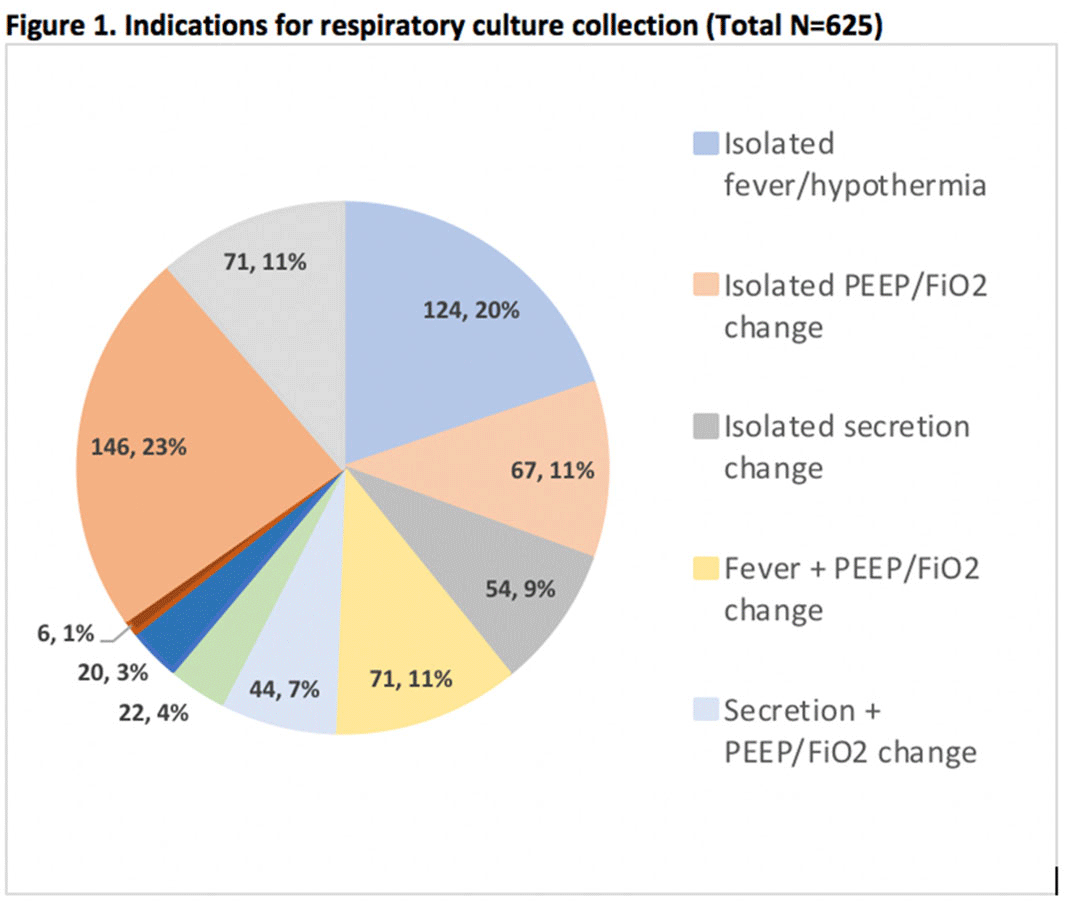
Figure 2.
How does peer similarity influence adult children caregivers' perceptions of support from peers? A mixed-method study
- MARINA BASTAWROUS WASILEWSKI, JENNIFER N. STINSON, FIONA WEBSTER, JILL I. CAMERON
-
- Journal:
- Ageing & Society / Volume 38 / Issue 11 / November 2018
- Published online by Cambridge University Press:
- 15 June 2017, pp. 2280-2303
- Print publication:
- November 2018
-
- Article
- Export citation
-
Due to the growing elderly population, adult children care-givers (ACCs) are increasingly providing complex care for one or both elderly parents. Social support from similar peers can mitigate care-giving-related health declines. To date, ‘peer similarity’ amongst care-givers has been predominantly investigated in the context of peer-matching interventions. However, because peer similarity is especially influential in ‘naturally occurring’ support networks, care-givers' everyday peer support engagement warrants further attention. Our goal was to explore care-givers' everyday peer support engagement and the influence of peer similarity on support perceptions. We employed a mixed-method design using Web-based surveys and in-depth qualitative interviews. The quantitative data were analysed using a hierarchical multiple while qualitative data were thematically analysed. Seventy-one ACCs completed the online questionnaire and 15 participated in a telephone interview. Peer similarity was positively and significantly associated with perceived support (β = 0.469, p < 0.0005) and explained 18.5 per cent of the additional variance. ACCs' narratives suggested the most important aspect of similarity was ‘shared care-giving experience’ as it optimised the support received from peers, and also enhanced the quality of the relationship. In conclusion, both data-sets underscored that peer similarity importantly influences support perceptions. The importance of ‘shared care-giving experience’ suggests that a more comprehensive understanding of this concept is needed to optimise peer-matching endeavours. Peer similarity's influence on relationship quality should also be explored.





