2 results
Relevance of RSV in hospitalized adults and the need for continued testing
- Katherine Miller, Arnold Monto, H. Keipp Talbot, Manjusha Gaglani, Tresa McNeal, Fernanda Silveira, Richard Zimmerman, Donald Middleton, Shekhar Ghamande, Kempapura Murthy, Lindsay Kim, Jill Ferdinands, Manish Patel, Emily Martin
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, p. s62
-
- Article
-
- You have access Access
- Open access
- Export citation
-
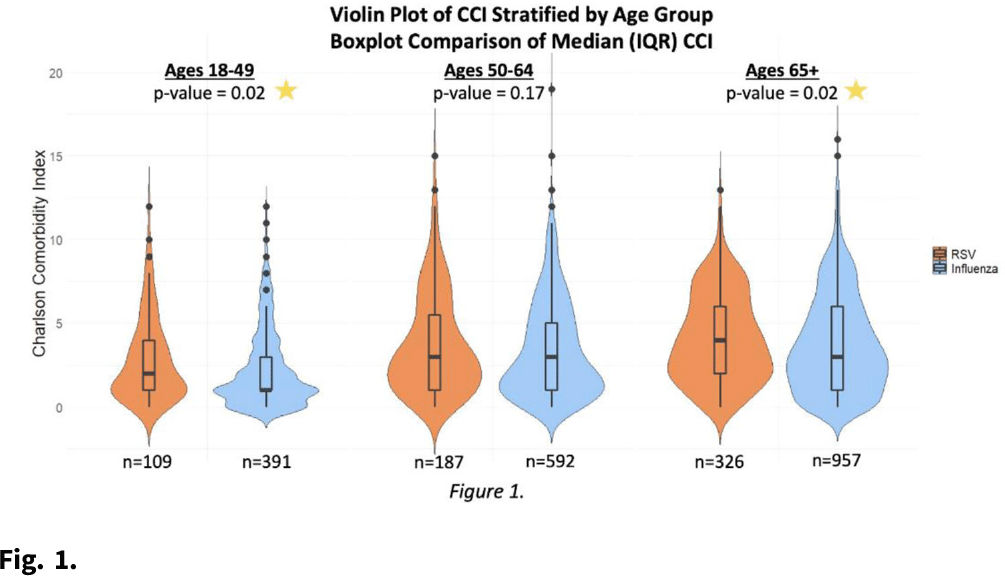
Background: RSV is underrecognized in hospitalized adults. A better understanding of RSV in this population could help prioritize targeted viral-testing resources. Hospitalization and in-hospital outcomes are widely accepted as markers of clinical severity with respect to acute respiratory illness (ARI). We compared characteristics and clinical outcomes between adults hospitalized with ARI from October 2016 through May 2019. Methods: All hospitalized adults (≥ 18 years) who met a standardized case definition of ARI were prospectively enrolled across 3 respiratory seasons from 9 hospitals participating in the US Hospitalized Adult Influenza Vaccine Effectiveness Network (HAIVEN). Demographic data were collected during enrollment interviews, and electronic medical records (EMRs) were reviewed to extract comorbidity data. Throat and nasal swabs collected at enrollment were tested for ARI pathogens using real-time PCR assays at respective HAIVEN research laboratory sites. Characteristics and clinical outcomes of participants were compared using χ2 or nonparametric tests where appropriate. Multivariable logistic regression models were used to test associations between infection status, characteristics, and clinical outcomes, adjusting for age, sex, race, Charlson comorbidity index (CCI), body mass index (BMI), site, season, and days to admission. Results: In total, 10,311 adults were included, 22.3% (n = 2,300) were aged 18–49 years, 33.2% (n = 3,423) were aged 50–64 years, and 44.5% (n = 4,588) were aged ≥65 years. Moreover, 6% of adults tested positive for RSV (n = 622), 18.8% positive for influenza (n = 1,940), and 75.1% negative for both (n = 7,749). Obesity and age ≥65 years were significantly associated with RSV detection when compared with participants negative for both RSV and influenza. Patients aged 18–49 years and ≥65 years with RSV had significantly higher median CCI scores compared to patients with influenza (Fig. 1.). The proportion of adults with CHF or COPD was significantly (p-value Conclusions: Severe RSV illness may differ from severe influenza illness, and those infected with RSV may have different characteristics than those infected with influenza. Hospitalized adults with RSV infection were more likely to have underlying cardiopulmonary comorbidities and higher CCI scores as well as experience an extended length of hospital stay and need for mechanical ventilation. These data highlight the importance of retaining testing for RSV in older adults hospitalized with ARI.
Funding: None
Disclosures: None
3258 The Relationship Between the Severity of Influenza-Related Illness and Timing of Seasonal Influenza Vaccination in Hospitalized Patients with Influenza
- Julia Haston, Shikha Garg, Angela Campbell, Jill Ferdinands, Monica Farley, Evan Anderson
-
- Journal:
- Journal of Clinical and Translational Science / Volume 3 / Issue s1 / March 2019
- Published online by Cambridge University Press:
- 26 March 2019, pp. 56-57
-
- Article
-
- You have access Access
- Open access
- Export citation
-
OBJECTIVES/SPECIFIC AIMS: The overall goal of this project is to determine whether timing of seasonal influenza vaccination affects the severity of illness in vaccinated individuals who are hospitalized with influenza. This will be assessed with the following aims: 1. To determine whether differences in demographic and clinical characteristics exist among patients with short duration between seasonal influenza vaccination and influenza-related hospitalization and those with longer duration. 2. To determine whether time between seasonal influenza vaccination and hospitalization is associated with the duration of influenza-related hospitalization. 3. To determine whether time between seasonal influenza vaccination and hospitalization is associated with the rate of influenza-related ICU admission among patients hospitalized with influenza. 4. To determine whether time between seasonal influenza vaccination and hospitalization is associated with the rate of influenza-related death among adults hospitalized with influenza. METHODS/STUDY POPULATION: The Influenza Hospitalization Surveillance Network (FluSurv-NET) is a surveillance platform of influenza-related hospitalizations through the CDC Emerging Infections Program (EIP). FluSurv-NET conducts active surveillance for influenza-related hospitalizations of both children and adults in selected counties in California, Colorado, Connecticut, Georgia, Maryland, Michigan, Minnesota, Ohio, Oregon, New Mexico, New York, Tennessee, and Utah with a total catchment population of over 27 million people (~9% of the US population). Using this platform, we will retrospectively evaluate four influenza seasons using FluSurv-NET data to look at the timing of influenza vaccination and severity of illness among patients with influenza-related hospitalization. We will conduct a multivariate analysis to assess for differences in severe outcomes including duration of hospitalization, ICU admission, and death among patients with varying lengths of time between influenza vaccination and influenza-related hospitalization. Separate analyses will be performed among different age groups and influenza type/subtypes, as well as specific seasons as a surrogate for most common circulating strain. RESULTS/ANTICIPATED RESULTS: We hypothesize that patients with chronic medical conditions and those at the extremes of age will have a longer duration between vaccination and hospitalization as they are more likely to get vaccinated earlier. We also hypothesize that patients with longer duration between seasonal influenza vaccination and hospitalization will have a longer duration of hospitalization and a higher rate of other severe outcomes (e.g., ICU admission, death). Such data would suggest that immune protection wanes during the influenza season. DISCUSSION/SIGNIFICANCE OF IMPACT: Limited data suggest that vaccine-induced influenza immunity may wane during the influenza season. It is not known whether the impact of influenza vaccination upon severity of disease might wane with increasing time between vaccination and influenza infection. In contrast to many previous studies evaluating vaccine effectiveness which have assessed medically-attended influenza illness as a primary outcome, our dataset is a large cohort of hospitalized patients which allows us to assess rare yet critical outcomes such as ICU admission and death. This study will also have a substantially larger amount of pediatric data than previous studies, which will provide the opportunity to determine whether timing of vaccination affects children and adults differently. Improving our understanding of whether influenza vaccine-induced protection might wane over time could ultimately impact U.S. influenza vaccination policy resulting in decreased morbidity and mortality attributed to influenza each season.




