26 results
Impact of discontinuation of contact precautions on surveillance- and whole genome sequencing-defined methicillin-resistant Staphylococcus aureus healthcare-associated infections
- Sharon Karunakaran, Lora Lee Pless, Ashley M. Ayres, Carl Ciccone, Joseph Penzelik, Alexander J. Sundermann, Elise M. Martin, Marissa P. Griffith, Kady Waggle, Jacob C. Hodges, Lee H. Harrison, Graham M. Snyder
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue 1 / 2024
- Published online by Cambridge University Press:
- 04 June 2024, e97
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Objective:
Prior studies evaluating the impact of discontinuation of contact precautions (DcCP) on methicillin-resistant Staphylococcus aureus (MRSA) outcomes have characterized all healthcare-associated infections (HAIs) rather than those likely preventable by contact precautions. We aimed to analyze the impact of DcCP on the rate of MRSA HAI including transmission events identified through whole genome sequencing (WGS) surveillance.
Design:Quasi experimental interrupted time series.
Setting:Acute care medical center.
Participants:Inpatients.
Methods:The effect of DcCP (use of gowns and gloves) for encounters among patients with MRSA carriage was evaluated using time series analysis of MRSA HAI rates from January 2019 through December 2022, compared to WGS-defined attributable transmission events before and after DcCP in December 2020.
Results:The MRSA HAI rate was 4.22/10,000 patient days before and 2.98/10,000 patient days after DcCP (incidence rate ratio [IRR] 0.71 [95% confidence interval 0.56–0.89]) with a significant immediate decrease (P = .001). There were 7 WGS-defined attributable transmission events before and 11 events after DcCP (incident rate ratio 0.90 [95% confidence interval 0.30–2.55]).
Conclusions:DcCP did not result in an increase in MRSA HAI or, in WGS-defined attributable transmission events. Comprehensive analyses of the effect of transmission prevention measures should include outcomes specifically measuring transmission-associated HAI.
Implementing nasal povidone-iodine decolonization to reduce infections in hemodialysis units: a qualitative assessment
- Kimberly C. Dukes, Stacey Hockett Sherlock, AM Racila, Loreen A. Herwaldt, Jesse Jacob, Anitha Vijayan, Joseph Kellogg, David Pegues, Pam C. Tolomeo, Jason Cobb, Mony Fraer, Susan C. Bleasdale, Melissa A. Ward, Brenna Lindsey, Marin L. Schweizer
-
- Journal:
- Infection Control & Hospital Epidemiology , First View
- Published online by Cambridge University Press:
- 23 May 2024, pp. 1-6
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background:
A substantial proportion of patients undergoing hemodialysis carry Staphylococcus aureus in their noses, and carriers are at increased risk of S. aureus bloodstream infections. Our pragmatic clinical trial implemented nasal povidone-iodine (PVI) decolonization for the prevention of bloodstream infections in the novel setting of hemodialysis units.
Objective:We aimed to identify pragmatic strategies for implementing PVI decolonization among patients in outpatient hemodialysis units.
Design:Qualitative descriptive study.
Setting:Outpatient hemodialysis units affiliated with five US academic medical centers. Units varied in size, patient demographics, and geographic location.
Interviewees:Sixty-six interviewees including nurses, hemodialysis technicians, research coordinators, and other personnel.
Methods:We conducted interviews with personnel affiliated with all five academic medical centers and conducted thematic analysis of transcripts.
Results:Hemodialysis units had varied success with patient recruitment, but interviewees reported that patients and healthcare personnel (HCP) found PVI decolonization acceptable and feasible. Leadership support, HCP engagement, and tailored patient-focused tools or strategies facilitated patient engagement and PVI implementation. Interviewees reported both patients and HCP sometimes underestimated patients’ infection risks and experienced infection-prevention fatigue. Other HCP barriers included limited staffing and poor staff engagement. Patient barriers included high health burdens, language barriers, memory issues, and lack of social support.
Conclusion:Our qualitative study suggests that PVI decolonization would be acceptable to patients and clinical personnel, and implementation is feasible for outpatient hemodialysis units. Hemodialysis units could facilitate implementation by engaging unit leaders, patients and personnel, and developing education for patients about their infection risk.
319 Development and Validation of an Artificial Intelligence Model to Accurately Predict Spinopelvic Parameters
- Part of
- Edward S Harake, Joseph R. Linzey, Cheng Jiang, Jaes C. Jones, Rushikesh Joshi, Mark Zaki, Zachary Wilseck, Jacob Joseph, Todd Hollon, Siri Sahib S. Khalsa, Paul Park
-
- Journal:
- Journal of Clinical and Translational Science / Volume 8 / Issue s1 / April 2024
- Published online by Cambridge University Press:
- 03 April 2024, p. 98
-
- Article
-
- You have access Access
- Open access
- Export citation
-
OBJECTIVES/GOALS: The correction of spinopelvic parameters is associated with better outcomes in patients with adult spinal deformity (ASD). This study presents a novel artificial intelligence (AI) tool that automatically predicts spinopelvic parameters from spine x-rays with high accuracy and without need for any manual entry. METHODS/STUDY POPULATION: The AI model was trained/validated on 761 sagittal whole-spine x-rays to predict the following parameters: Sagittal Vertical Axis (SVA), Pelvic Tilt (PT), Pelvic Incidence (PI), Sacral Slope (SS), Lumbar Lordosis (LL), T1-Pelvic Angle (T1PA), and L1-Pelvic Angle (L1PA). A separate test set of 40 x-rays was labeled by 4 reviewers including fellowship-trained spine surgeons and a neuroradiologist. Median errors relative to the most senior reviewer were calculated to determine model accuracy on test and cropped-test (i.e. lumbosacral) images. Intraclass correlation coefficients (ICC) were used to assess inter-rater reliability RESULTS/ANTICIPATED RESULTS: The AI model exhibited the following median (IQR) parameter errors: SVA[2.1mm (8.5mm), p=0.97], PT [1.5° (1.4°), p=0.52], PI[2.3° (2.4°), p=0.27], SS[1.7° (2.2°), p=0.64], LL [2.6° (4.0°), p=0.89], T1PA [1.3° (1.1°), p=0.41], and L1PA [1.3° (1.2°), p=0.51]. The parameter errors on cropped lumbosacral images were: LL[2.9° (2.6°), p=0.80] and SS[1.9° (2.2°), p=0.78]. The AI model exhibited excellent reliability at all parameters in both whole-spine (ICC: 0.92-1.0) and lumbosacral x-rays: (ICC: 0.92-0.93). DISCUSSION/SIGNIFICANCE: Our AI model accurately predicts spinopelvic parameters with excellent reliability comparable to fellowship-trained spine surgeons and neuroradiologists. Utilization of predictive AI tools in spine-imaging can substantially aid in patient selection and surgical planning.
The fragility index: how robust are the outcomes of head and neck cancer randomised, controlled trials?
- Neeraj V Suresh, Beatrice C Go, Christian G Fritz, Jacob Harris, Vinayak Ahluwalia, Katherine Xu, Joseph Lu, Karthik Rajasekaran
-
- Journal:
- The Journal of Laryngology & Otology / Volume 138 / Issue 4 / April 2024
- Published online by Cambridge University Press:
- 05 October 2023, pp. 451-456
- Print publication:
- April 2024
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
The fragility index represents the minimum number of patients required to convert an outcome from statistically significant to insignificant. This report assesses the fragility index of head and neck cancer randomised, controlled trials.
MethodsStudies were extracted from PubMed/Medline, Scopus, Embase and Cochrane databases.
ResultsOverall, 123 randomised, controlled trials were included. The sample size and fragility index medians (interquartile ranges) were 103 (56–213) and 2 (0–5), respectively. The fragility index exceeded the number of patients lost to follow up in 42.3 per cent (n = 52) of studies. A higher fragility index correlated with higher sample size (r = 0.514, p < 0.001), number of events (r = 0.449, p < 0.001) and statistical significance via p-value (r = −0.367, p < 0.001).
ConclusionHead and neck cancer randomised, controlled trials demonstrated low fragility index values, in which statistically significant results could be nullified by altering the outcomes of just two patients, on average. Future head and neck oncology randomised, controlled trials should report the fragility index in order to provide insight into statistical robustness.
Epidemiology of extended-spectrum β-lactamase–producing Enterobacterales in five US sites participating in the Emerging Infections Program, 2017
- Nadezhda Duffy, Maria Karlsson, Hannah E. Reses, Davina Campbell, Jonathan Daniels, Richard A. Stanton, Sarah J. Janelle, Kyle Schutz, Wendy Bamberg, Paulina A. Rebolledo, Chris Bower, Rebekah Blakney, Jesse T. Jacob, Erin C. Phipps, Kristina G. Flores, Ghinwa Dumyati, Hannah Kopin, Rebecca Tsay, Marion A. Kainer, Daniel Muleta, Benji Byrd-Warner, Julian E. Grass, Joseph D. Lutgring, J. Kamile Rasheed, Christopher A. Elkins, Shelley S. Magill, Isaac See
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 43 / Issue 11 / November 2022
- Published online by Cambridge University Press:
- 14 February 2022, pp. 1586-1594
- Print publication:
- November 2022
-
- Article
- Export citation
-
Objective
The incidence of infections from extended-spectrum β-lactamase (ESBL)–producing Enterobacterales (ESBL-E) is increasing in the United States. We describe the epidemiology of ESBL-E at 5 Emerging Infections Program (EIP) sites.
MethodsDuring October–December 2017, we piloted active laboratory- and population-based (New York, New Mexico, Tennessee) or sentinel (Colorado, Georgia) ESBL-E surveillance. An incident case was the first isolation from normally sterile body sites or urine of Escherichia coli or Klebsiella pneumoniae/oxytoca resistant to ≥1 extended-spectrum cephalosporin and nonresistant to all carbapenems tested at a clinical laboratory from a surveillance area resident in a 30-day period. Demographic and clinical data were obtained from medical records. The Centers for Disease Control and Prevention (CDC) performed reference antimicrobial susceptibility testing and whole-genome sequencing on a convenience sample of case isolates.
ResultsWe identified 884 incident cases. The estimated annual incidence in sites conducting population-based surveillance was 199.7 per 100,000 population. Overall, 800 isolates (96%) were from urine, and 790 (89%) were E. coli. Also, 393 cases (47%) were community-associated. Among 136 isolates (15%) tested at the CDC, 122 (90%) met the surveillance definition phenotype; 114 (93%) of 122 were shown to be ESBL producers by clavulanate testing. In total, 111 (97%) of confirmed ESBL producers harbored a blaCTX-M gene. Among ESBL-producing E. coli isolates, 52 (54%) were ST131; 44% of these cases were community associated.
ConclusionsThe burden of ESBL-E was high across surveillance sites, with nearly half of cases acquired in the community. EIP has implemented ongoing ESBL-E surveillance to inform prevention efforts, particularly in the community and to watch for the emergence of new ESBL-E strains.
Support with extracorporeal membrane oxygenation for over 1 year duration as a bridge to cardiac transplantation: a case report and review of the literature
- Part of
- Seth C. Shanefield, Daniel Knewitz, Joseph Philip, F. Jay Fricker, Kevin Sullivan, Circe Laucerica, Jeffrey P. Jacobs, Giles J. Peek, Mark S. Bleiweis
-
- Journal:
- Cardiology in the Young / Volume 31 / Issue 9 / September 2021
- Published online by Cambridge University Press:
- 20 September 2021, pp. 1495-1497
-
- Article
- Export citation
-
We present the case of a 13-year-old male with a complex congenital cardiac history who was supported with extracorporeal membrane oxygenation for 394 days while awaiting cardiac transplantation. The patient underwent successful cardiac transplantation after 394 days of support with veno-arterial extracorporeal membrane oxygenation and is currently alive 2 years after cardiac transplantation. We believe that this case represents the longest period of time that a patient has been supported with extracorporeal membrane oxygenation as a bridge to cardiac transplantation.
We also review the literature associated with prolonged support with extracorporeal membrane oxygenation. This case report documents many of the challenges associated with prolonged support with extracorporeal membrane oxygenation, including polymicrobial bacterial and fungal infections, as well as renal dysfunction. It is possible to successfully bridge a patient to cardiac transplantation with prolonged support with extracorporeal membrane oxygenation of over 1 year; however, multidisciplinary collaboration is critical.
Takayasu’s arteritis presenting as acute myocardial infarction: case series and review of literature
- Laura Wilson, Arun Chandran, James C. Fudge, Diego Moguillansky, Akaluck Thatayatikom, Joseph Philip, Jeffrey P. Jacobs, Mark Bleiweis, Melissa Elder, Dipankar Gupta
-
- Journal:
- Cardiology in the Young / Volume 31 / Issue 11 / November 2021
- Published online by Cambridge University Press:
- 21 May 2021, pp. 1866-1869
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
This series describes three adolescent females who presented with chest pain and ventricular dysfunction related to acute coronary ischemia secondary to Takayasu’s arteritis with varied courses of disease progression leading to a diverse range of therapies including cardiac transplantation. While Takayasu’s arteritis is rare in childhood, it should be strongly considered in any adolescent female presenting with systemic inflammation and chest pain consistent with myocardial infarction. A high index of suspicion can lead to early detection and aggressive management of the underlying vasculitis reducing associated morbidity and mortality. The purpose of this report is to describe the challenges in the clinical diagnosis and management of Takayasu’s arteritis with myocardial infarction. We also seek to enhance awareness about unique presentations of Takayasu’s arteritis within the paediatric community.
Unconventional Care at a Convention Center: An Overview of Patient Focused Care at a COVID-19 Alternative Care Site in New Orleans
- Meghan Maslanka, John C. Carlson, Estaban Gershanik, Yanti Turang, Jacob Hurwitz, Michelle Warren, Joseph Kanter
-
- Journal:
- Disaster Medicine and Public Health Preparedness / Volume 16 / Issue 6 / December 2022
- Published online by Cambridge University Press:
- 03 May 2021, pp. 2612-2618
-
- Article
- Export citation
-
In March 2020, the State of Louisiana opened an alternative care site at the New Orleans Convention Center, known as the Medical Monitoring Station (MMS). The facility was designed, constructed, and staffed to serve a population with basic medical needs as they recovered from COVID-19. As the MMS prepared to open, local hospitals indicated a greater need for assistance with patients requiring a higher acuity of care and populations unable to be discharged due to infection risks. In response to this, the capabilities of the facility were altered to accommodate primarily elderly patients, with significant comorbidities, requiring extensive care. This manuscript presents the demographics of the first 250 patients seen at the MMS, and describes the most critical policies/protocols, interventions, and resources that proved successful in adjusting to effectively serve its population.
The impact of tandem redundant/sky-based calibration in MWA Phase II data analysis
- Part of
- Zheng Zhang, Jonathan C. Pober, Wenyang Li, Bryna J. Hazelton, Miguel F. Morales, Cathryn M. Trott, Christopher H. Jordan, Ronniy C. Joseph, Adam Beardsley, Nichole Barry, Ruby Byrne, Steven J. Tingay, Aman Chokshi, Kenji Hasegawa, Daniel C. Jacobs, Adam Lanman, Jack L. B. Line, Christene Lynch, Benjamin McKinley, Daniel A. Mitchell, Steven Murray, Bart Pindor, Mahsa Rahimi, Keitaro Takahashi, Randall B. Wayth, Rachel L. Webster, Michael Wilensky, Shintaro Yoshiura, Qian Zheng
-
- Journal:
- Publications of the Astronomical Society of Australia / Volume 37 / 2020
- Published online by Cambridge University Press:
- 04 November 2020, e045
-
- Article
-
- You have access Access
- HTML
- Export citation
-
Precise instrumental calibration is of crucial importance to 21-cm cosmology experiments. The Murchison Widefield Array’s (MWA) Phase II compact configuration offers us opportunities for both redundant calibration and sky-based calibration algorithms; using the two in tandem is a potential approach to mitigate calibration errors caused by inaccurate sky models. The MWA Epoch of Reionization (EoR) experiment targets three patches of the sky (dubbed EoR0, EoR1, and EoR2) with deep observations. Previous work in Li et al. (2018) and (2019) studied the effect of tandem calibration on the EoR0 field and found that it yielded no significant improvement in the power spectrum (PS) over sky-based calibration alone. In this work, we apply similar techniques to the EoR1 field and find a distinct result: the improvements in the PS from tandem calibration are significant. To understand this result, we analyse both the calibration solutions themselves and the effects on the PS over three nights of EoR1 observations. We conclude that the presence of the bright radio galaxy Fornax A in EoR1 degrades the performance of sky-based calibration, which in turn enables redundant calibration to have a larger impact. These results suggest that redundant calibration can indeed mitigate some level of model incompleteness error.
Evaluation of Discrepancies in Carbapenem Minimum Inhibitory Concentrations Obtained at Clinical Laboratories Compared to a Public Health Laboratory
- Julian E. Grass, Shelley S. Magill, Isaac See, Uzma Ansari, Lucy E. Wilson, Elisabeth Vaeth, Paula Snippes Vagnone, Brittany Pattee, Jesse T. Jacob, Georgia Emerging Infections Program, Chris Bower, Atlanta Veterans Affairs Medical Center, Foundation for Atlanta Veterans Education and Research, Sarah W. Satola, Sarah J. Janelle, Kyle Schutz, Rebecca Tsay, Marion A. Kainer, Daniel Muleta, P. Maureen Cassidy, Vivian H. Leung, Meghan Maloney, Erin C. Phipps, New Mexico Emerging Infections Program, Kristina G. Flores, New Mexico Emerging Infections Program, Erin Epson, Joelle Nadle, Maria Karlsson, Joseph D. Lutgring
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s474-s476
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Automated testing instruments (ATIs) are commonly used by clinical microbiology laboratories to perform antimicrobial susceptibility testing (AST), whereas public health laboratories may use established reference methods such as broth microdilution (BMD). We investigated discrepancies in carbapenem minimum inhibitory concentrations (MICs) among Enterobacteriaceae tested by clinical laboratory ATIs and by reference BMD at the CDC. Methods: During 2016–2018, we conducted laboratory- and population-based surveillance for carbapenem-resistant Enterobacteriaceae (CRE) through the CDC Emerging Infections Program (EIP) sites (10 sites by 2018). We defined an incident case as the first isolation of Enterobacter spp (E. cloacae complex or E. aerogenes), Escherichia coli, Klebsiella pneumoniae, K. oxytoca, or K. variicola resistant to doripenem, ertapenem, imipenem, or meropenem from normally sterile sites or urine identified from a resident of the EIP catchment area in a 30-day period. Cases had isolates that were determined to be carbapenem-resistant by clinical laboratory ATI MICs (MicroScan, BD Phoenix, or VITEK 2) or by other methods, using current Clinical and Laboratory Standards Institute (CLSI) criteria. A convenience sample of these isolates was tested by reference BMD at the CDC according to CLSI guidelines. Results: Overall, 1,787 isolates from 112 clinical laboratories were tested by BMD at the CDC. Of these, clinical laboratory ATI MIC results were available for 1,638 (91.7%); 855 (52.2%) from 71 clinical laboratories did not confirm as CRE at the CDC. Nonconfirming isolates were tested on either a MicroScan (235 of 462; 50.9%), BD Phoenix (249 of 411; 60.6%), or VITEK 2 (371 of 765; 48.5%). Lack of confirmation was most common among E. coli (62.2% of E. coli isolates tested) and Enterobacter spp (61.4% of Enterobacter isolates tested) (Fig. 1A), and among isolates testing resistant to ertapenem by the clinical laboratory ATI (52.1%, Fig. 1B). Of the 1,388 isolates resistant to ertapenem in the clinical laboratory, 1,006 (72.5%) were resistant only to ertapenem. Of the 855 nonconfirming isolates, 638 (74.6%) were resistant only to ertapenem based on clinical laboratory ATI MICs. Conclusions: Nonconfirming isolates were widespread across laboratories and ATIs. Lack of confirmation was most common among E. coli and Enterobacter spp. Among nonconfirming isolates, most were resistant only to ertapenem. These findings may suggest that ATIs overcall resistance to ertapenem or that isolate transport and storage conditions affect ertapenem resistance. Further investigation into this lack of confirmation is needed, and CRE case identification in public health surveillance may need to account for this phenomenon.
Funding: None
Disclosures: None
Whole-Genome Sequencing Reveals Diversity of Carbapenem-Resistant Pseudomonas aeruginosa Collected Through the Emerging Infections Program
- Richard Stanton, Jonathan Daniels, Erin Breaker, Davina Campbell, Joseph Lutgring, Maria Karlsson, Kyle Schutz, Jesse Jacob, Lucy Wilson, Elisabeth Vaeth, Linda Li, Ruth Lynfield, Erin C. Phipps, Emily Hancock, Ghinwa Dumyati, Rebecca Tsay, P. Maureen Cassidy, Jacquelyn Mounsey, Julian Grass, Maroya Walters, Alison Halpin
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s513-s514
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Carbapenem-resistant Pseudomonas aeruginosa (CRPA) is a frequent cause of healthcare-associated infections (HAIs). The CDC Emerging Infections Program (EIP) conducted population and laboratory-based surveillance of CRPA in selected areas in 8 states from August 1, 2016, through July 31, 2018. We aimed to describe the molecular epidemiology and mechanisms of resistance of CRPA isolates collected through this surveillance. Methods: We defined a case as the first isolate of P. aeruginosa resistant to imipenem, meropenem, or doripenem from the lower respiratory tract, urine, wounds, or normally sterile sites identified from a resident of the EIP catchment area in a 30-day period; EIP sites submitted a systematic random sample of isolates to CDC for further characterization. Of 1,021 CRPA clinical isolates submitted, 707 have been sequenced to date using an Illumina MiSeq. Sequenced genomes were classified using the 7-gene multilocus sequence typing (MLST) scheme, and a core genome MLST (cgMLST) scheme was used to determine phylogeny. Antimicrobial resistance genes were identified using publicly available databases, and chromosomal mechanisms of carbapenem resistance were determined using previously validated genetic markers. Results: There were 189 sequence types (STs) among the 707 sequenced genomes (Fig. 1). The most frequently occurring were high-risk clones ST235 (8.5%) and ST298 (4.7%), which were found across all EIP sites. Carbapenemase genes were identified in 5 (<1%) isolates. Overall, 95.6% of the isolates had chromosomal mutations associated with carbapenem resistance: 93.2% had porinD-associated mutations that decrease membrane permeability to the drugs; 24.8% had mutations associated with overexpression of the multidrug efflux pump MexAB-OprM; and 22.9% had mutations associated with overexpression of the endogenous β-lactamase ampC. More than 1 such chromosomal resistance mutation type was present in 37.8% of the isolates. Conclusions: The diversity of the sequence types demonstrates that HAIs caused by CRPA can arise from a variety of strains and that high-risk clones are broadly disseminated across the EIP sites but are a minority of CRPA strains overall. Carbapenem resistance in P. aeruginosa was predominantly driven by chromosomal mutations rather than acquired mechanisms (ie, carbapenemases). The diversity of the CRPA isolates and the lack of carbapenemase genes suggest that this ubiquitous pathogen can readily evolve chromosomal resistance mechanisms, but unlike carbapenemases, these cannot be easily spread through horizontal transfer.
Funding: None
Disclosures: None
Science with the Murchison Widefield Array: Phase I results and Phase II opportunities – Corrigendum
- A. P. Beardsley, M. Johnston-Hollitt, C. M. Trott, J. C. Pober, J. Morgan, D. Oberoi, D. L. Kaplan, C. R. Lynch, G. E. Anderson, P. I. McCauley, S. Croft, C. W. James, O. I. Wong, C. D. Tremblay, R. P. Norris, I. H. Cairns, C. J. Lonsdale, P. J. Hancock, B. M. Gaensler, N. D. R. Bhat, W. Li, N. Hurley-Walker, J. R. Callingham, N. Seymour, S. Yoshiura, R. C. Joseph, K. Takahashi, M. Sokolowski, J. C. A. Miller-Jones, J. V. Chauhan, I. Bojičić, M. D. Filipović, D. Leahy, H. Su, W. W. Tian, S. J. McSweeney, B. W. Meyers, S. Kitaeff, T. Vernstrom, G. Gürkan, G. Heald, M. Xue, C. J. Riseley, S. W. Duchesne, J. D. Bowman, D. C. Jacobs, B. Crosse, D. Emrich, T. M. O. Franzen, L. Horsley, D. Kenney, M. F. Morales, D. Pallot, K. Steele, S. J. Tingay, M. Walker, R. B. Wayth, A. Williams, C. Wu
-
- Journal:
- Publications of the Astronomical Society of Australia / Volume 37 / 2020
- Published online by Cambridge University Press:
- 23 March 2020, e014
-
- Article
-
- You have access Access
- HTML
- Export citation
Science with the Murchison Widefield Array: Phase I results and Phase II opportunities
- A. P. Beardsley, M. Johnston-Hollitt, C. M. Trott, J. C. Pober, J. Morgan, D. Oberoi, D. L. Kaplan, C. R. Lynch, G. E. Anderson, P. I. McCauley, S. Croft, C. W. James, O. I. Wong, C. D. Tremblay, R. P. Norris, I. H. Cairns, C. J. Lonsdale, P. J. Hancock, B. M. Gaensler, N. D. R. Bhat, W. Li, N. Hurley-Walker, J. R. Callingham, N. Seymour, S. Yoshiura, R. C. Joseph, K. Takahashi, M. Sokolowski, J. C. A. Miller-Jones, J. V. Chauhan, I. Bojičić, M. D. Filipović, D. Leahy, H. Su, W. W. Tian, S. J. McSweeney, B. W. Meyers, S. Kitaeff, T. Vernstrom, G. Gürkan, G. Heald, M. Xue, C. J. Riseley, S. W. Duchesne, J. D. Bowman, D. C. Jacobs, B. Crosse, D. Emrich, T. M. O. Franzen, L. Horsley, D. Kenney, M. F. Morales, D. Pallot, K. Steele, S. J. Tingay, M. Walker, R. B. Wayth, A. Williams, C. Wu
-
- Journal:
- Publications of the Astronomical Society of Australia / Volume 36 / 2019
- Published online by Cambridge University Press:
- 13 December 2019, e050
-
- Article
-
- You have access Access
- HTML
- Export citation
-
The Murchison Widefield Array (MWA) is an open access telescope dedicated to studying the low-frequency (80–300 MHz) southern sky. Since beginning operations in mid-2013, the MWA has opened a new observational window in the southern hemisphere enabling many science areas. The driving science objectives of the original design were to observe 21 cm radiation from the Epoch of Reionisation (EoR), explore the radio time domain, perform Galactic and extragalactic surveys, and monitor solar, heliospheric, and ionospheric phenomena. All together
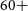 $60+$
programs recorded 20 000 h producing 146 papers to date. In 2016, the telescope underwent a major upgrade resulting in alternating compact and extended configurations. Other upgrades, including digital back-ends and a rapid-response triggering system, have been developed since the original array was commissioned. In this paper, we review the major results from the prior operation of the MWA and then discuss the new science paths enabled by the improved capabilities. We group these science opportunities by the four original science themes but also include ideas for directions outside these categories.
$60+$
programs recorded 20 000 h producing 146 papers to date. In 2016, the telescope underwent a major upgrade resulting in alternating compact and extended configurations. Other upgrades, including digital back-ends and a rapid-response triggering system, have been developed since the original array was commissioned. In this paper, we review the major results from the prior operation of the MWA and then discuss the new science paths enabled by the improved capabilities. We group these science opportunities by the four original science themes but also include ideas for directions outside these categories.
Preservation and Recognition of Middle and Early Pleistocene Loess in the Driftless Area, Wisconsin
- Peter M. Jacobs, James C. Knox, Joseph A. Mason
-
- Journal:
- Quaternary Research / Volume 47 / Issue 2 / March 1997
- Published online by Cambridge University Press:
- 20 January 2017, pp. 147-154
-
- Article
- Export citation
-
An exceptional stratigraphic and pedologic record of Pleistocene environmental conditions occurs at the Kieler Site in the Driftless Area of southwestern Wisconsin. Peoria, Roxana, Loveland, and pre-Loveland loesses overlie weathered bedrock residuum. The pre-Loveland unit previously has been included as part of the residuum at other Driftless Area sites. Early and middle Pleistocene loesses in the Mississippi Valley are normally absent at most localities. Rather than nondeposition, we suggest the apparent absence of pre-Illinoian loess units is due in part to erosion, but also to weathering that renders loesses unrecognizable so they are classified as “residuum.”
Summary of the 2015 International Paediatric Heart Failure Summit of Johns Hopkins All Children’s Heart Institute
- Jeffrey P. Jacobs, James A. Quintessenza, Tom R. Karl, Alfred Asante-Korang, Allen D. Everett, Susan B. Collins, Genaro A. Ramirez-Correa, Kristin M. Burns, Mitchell Cohen, Steven D. Colan, John M. Costello, Kevin P. Daly, Rodney C. G. Franklin, Charles D. Fraser, Kevin D. Hill, James C. Huhta, Sunjay Kaushal, Yuk M. Law, Steven E. Lipshultz, Anne M. Murphy, Sara K. Pasquali, Mark R. Payne, Joseph Rossano, Girish Shirali, Stephanie M. Ware, Mingguo Xu, Marshall L. Jacobs
-
- Journal:
- Cardiology in the Young / Volume 25 / Issue S2 / August 2015
- Published online by Cambridge University Press:
- 17 September 2015, pp. 8-30
-
- Article
- Export citation
-
In the United States alone, ∼14,000 children are hospitalised annually with acute heart failure. The science and art of caring for these patients continues to evolve. The International Pediatric Heart Failure Summit of Johns Hopkins All Children’s Heart Institute was held on February 4 and 5, 2015. The 2015 International Pediatric Heart Failure Summit of Johns Hopkins All Children’s Heart Institute was funded through the Andrews/Daicoff Cardiovascular Program Endowment, a philanthropic collaboration between All Children’s Hospital and the Morsani College of Medicine at the University of South Florida (USF). Sponsored by All Children’s Hospital Andrews/Daicoff Cardiovascular Program, the International Pediatric Heart Failure Summit assembled leaders in clinical and scientific disciplines related to paediatric heart failure and created a multi-disciplinary “think-tank”. The purpose of this manuscript is to summarise the lessons from the 2015 International Pediatric Heart Failure Summit of Johns Hopkins All Children’s Heart Institute, to describe the “state of the art” of the treatment of paediatric cardiac failure, and to discuss future directions for research in the domain of paediatric cardiac failure.
Contributors
-
- By Mitchell Aboulafia, Frederick Adams, Marilyn McCord Adams, Robert M. Adams, Laird Addis, James W. Allard, David Allison, William P. Alston, Karl Ameriks, C. Anthony Anderson, David Leech Anderson, Lanier Anderson, Roger Ariew, David Armstrong, Denis G. Arnold, E. J. Ashworth, Margaret Atherton, Robin Attfield, Bruce Aune, Edward Wilson Averill, Jody Azzouni, Kent Bach, Andrew Bailey, Lynne Rudder Baker, Thomas R. Baldwin, Jon Barwise, George Bealer, William Bechtel, Lawrence C. Becker, Mark A. Bedau, Ernst Behler, José A. Benardete, Ermanno Bencivenga, Jan Berg, Michael Bergmann, Robert L. Bernasconi, Sven Bernecker, Bernard Berofsky, Rod Bertolet, Charles J. Beyer, Christian Beyer, Joseph Bien, Joseph Bien, Peg Birmingham, Ivan Boh, James Bohman, Daniel Bonevac, Laurence BonJour, William J. Bouwsma, Raymond D. Bradley, Myles Brand, Richard B. Brandt, Michael E. Bratman, Stephen E. Braude, Daniel Breazeale, Angela Breitenbach, Jason Bridges, David O. Brink, Gordon G. Brittan, Justin Broackes, Dan W. Brock, Aaron Bronfman, Jeffrey E. Brower, Bartosz Brozek, Anthony Brueckner, Jeffrey Bub, Lara Buchak, Otavio Bueno, Ann E. Bumpus, Robert W. Burch, John Burgess, Arthur W. Burks, Panayot Butchvarov, Robert E. Butts, Marina Bykova, Patrick Byrne, David Carr, Noël Carroll, Edward S. Casey, Victor Caston, Victor Caston, Albert Casullo, Robert L. Causey, Alan K. L. Chan, Ruth Chang, Deen K. Chatterjee, Andrew Chignell, Roderick M. Chisholm, Kelly J. Clark, E. J. Coffman, Robin Collins, Brian P. Copenhaver, John Corcoran, John Cottingham, Roger Crisp, Frederick J. Crosson, Antonio S. Cua, Phillip D. Cummins, Martin Curd, Adam Cureton, Andrew Cutrofello, Stephen Darwall, Paul Sheldon Davies, Wayne A. Davis, Timothy Joseph Day, Claudio de Almeida, Mario De Caro, Mario De Caro, John Deigh, C. F. Delaney, Daniel C. Dennett, Michael R. DePaul, Michael Detlefsen, Daniel Trent Devereux, Philip E. Devine, John M. Dillon, Martin C. Dillon, Robert DiSalle, Mary Domski, Alan Donagan, Paul Draper, Fred Dretske, Mircea Dumitru, Wilhelm Dupré, Gerald Dworkin, John Earman, Ellery Eells, Catherine Z. Elgin, Berent Enç, Ronald P. Endicott, Edward Erwin, John Etchemendy, C. Stephen Evans, Susan L. Feagin, Solomon Feferman, Richard Feldman, Arthur Fine, Maurice A. Finocchiaro, William FitzPatrick, Richard E. Flathman, Gvozden Flego, Richard Foley, Graeme Forbes, Rainer Forst, Malcolm R. Forster, Daniel Fouke, Patrick Francken, Samuel Freeman, Elizabeth Fricker, Miranda Fricker, Michael Friedman, Michael Fuerstein, Richard A. Fumerton, Alan Gabbey, Pieranna Garavaso, Daniel Garber, Jorge L. A. Garcia, Robert K. Garcia, Don Garrett, Philip Gasper, Gerald Gaus, Berys Gaut, Bernard Gert, Roger F. Gibson, Cody Gilmore, Carl Ginet, Alan H. Goldman, Alvin I. Goldman, Alfonso Gömez-Lobo, Lenn E. Goodman, Robert M. Gordon, Stefan Gosepath, Jorge J. E. Gracia, Daniel W. Graham, George A. Graham, Peter J. Graham, Richard E. Grandy, I. Grattan-Guinness, John Greco, Philip T. Grier, Nicholas Griffin, Nicholas Griffin, David A. Griffiths, Paul J. Griffiths, Stephen R. Grimm, Charles L. Griswold, Charles B. Guignon, Pete A. Y. Gunter, Dimitri Gutas, Gary Gutting, Paul Guyer, Kwame Gyekye, Oscar A. Haac, Raul Hakli, Raul Hakli, Michael Hallett, Edward C. Halper, Jean Hampton, R. James Hankinson, K. R. Hanley, Russell Hardin, Robert M. Harnish, William Harper, David Harrah, Kevin Hart, Ali Hasan, William Hasker, John Haugeland, Roger Hausheer, William Heald, Peter Heath, Richard Heck, John F. Heil, Vincent F. Hendricks, Stephen Hetherington, Francis Heylighen, Kathleen Marie Higgins, Risto Hilpinen, Harold T. Hodes, Joshua Hoffman, Alan Holland, Robert L. Holmes, Richard Holton, Brad W. Hooker, Terence E. Horgan, Tamara Horowitz, Paul Horwich, Vittorio Hösle, Paul Hoβfeld, Daniel Howard-Snyder, Frances Howard-Snyder, Anne Hudson, Deal W. Hudson, Carl A. Huffman, David L. Hull, Patricia Huntington, Thomas Hurka, Paul Hurley, Rosalind Hursthouse, Guillermo Hurtado, Ronald E. Hustwit, Sarah Hutton, Jonathan Jenkins Ichikawa, Harry A. Ide, David Ingram, Philip J. Ivanhoe, Alfred L. Ivry, Frank Jackson, Dale Jacquette, Joseph Jedwab, Richard Jeffrey, David Alan Johnson, Edward Johnson, Mark D. Jordan, Richard Joyce, Hwa Yol Jung, Robert Hillary Kane, Tomis Kapitan, Jacquelyn Ann K. Kegley, James A. Keller, Ralph Kennedy, Sergei Khoruzhii, Jaegwon Kim, Yersu Kim, Nathan L. King, Patricia Kitcher, Peter D. Klein, E. D. Klemke, Virginia Klenk, George L. Kline, Christian Klotz, Simo Knuuttila, Joseph J. Kockelmans, Konstantin Kolenda, Sebastian Tomasz Kołodziejczyk, Isaac Kramnick, Richard Kraut, Fred Kroon, Manfred Kuehn, Steven T. Kuhn, Henry E. Kyburg, John Lachs, Jennifer Lackey, Stephen E. Lahey, Andrea Lavazza, Thomas H. Leahey, Joo Heung Lee, Keith Lehrer, Dorothy Leland, Noah M. Lemos, Ernest LePore, Sarah-Jane Leslie, Isaac Levi, Andrew Levine, Alan E. Lewis, Daniel E. Little, Shu-hsien Liu, Shu-hsien Liu, Alan K. L. Chan, Brian Loar, Lawrence B. Lombard, John Longeway, Dominic McIver Lopes, Michael J. Loux, E. J. Lowe, Steven Luper, Eugene C. Luschei, William G. Lycan, David Lyons, David Macarthur, Danielle Macbeth, Scott MacDonald, Jacob L. Mackey, Louis H. Mackey, Penelope Mackie, Edward H. Madden, Penelope Maddy, G. B. Madison, Bernd Magnus, Pekka Mäkelä, Rudolf A. Makkreel, David Manley, William E. Mann (W.E.M.), Vladimir Marchenkov, Peter Markie, Jean-Pierre Marquis, Ausonio Marras, Mike W. Martin, A. P. Martinich, William L. McBride, David McCabe, Storrs McCall, Hugh J. McCann, Robert N. McCauley, John J. McDermott, Sarah McGrath, Ralph McInerny, Daniel J. McKaughan, Thomas McKay, Michael McKinsey, Brian P. McLaughlin, Ernan McMullin, Anthonie Meijers, Jack W. Meiland, William Jason Melanson, Alfred R. Mele, Joseph R. Mendola, Christopher Menzel, Michael J. Meyer, Christian B. Miller, David W. Miller, Peter Millican, Robert N. Minor, Phillip Mitsis, James A. Montmarquet, Michael S. Moore, Tim Moore, Benjamin Morison, Donald R. Morrison, Stephen J. Morse, Paul K. Moser, Alexander P. D. Mourelatos, Ian Mueller, James Bernard Murphy, Mark C. Murphy, Steven Nadler, Jan Narveson, Alan Nelson, Jerome Neu, Samuel Newlands, Kai Nielsen, Ilkka Niiniluoto, Carlos G. Noreña, Calvin G. Normore, David Fate Norton, Nikolaj Nottelmann, Donald Nute, David S. Oderberg, Steve Odin, Michael O’Rourke, Willard G. Oxtoby, Heinz Paetzold, George S. Pappas, Anthony J. Parel, Lydia Patton, R. P. Peerenboom, Francis Jeffry Pelletier, Adriaan T. Peperzak, Derk Pereboom, Jaroslav Peregrin, Glen Pettigrove, Philip Pettit, Edmund L. Pincoffs, Andrew Pinsent, Robert B. Pippin, Alvin Plantinga, Louis P. Pojman, Richard H. Popkin, John F. Post, Carl J. Posy, William J. Prior, Richard Purtill, Michael Quante, Philip L. Quinn, Philip L. Quinn, Elizabeth S. Radcliffe, Diana Raffman, Gerard Raulet, Stephen L. Read, Andrews Reath, Andrew Reisner, Nicholas Rescher, Henry S. Richardson, Robert C. Richardson, Thomas Ricketts, Wayne D. Riggs, Mark Roberts, Robert C. Roberts, Luke Robinson, Alexander Rosenberg, Gary Rosenkranz, Bernice Glatzer Rosenthal, Adina L. Roskies, William L. Rowe, T. M. Rudavsky, Michael Ruse, Bruce Russell, Lilly-Marlene Russow, Dan Ryder, R. M. Sainsbury, Joseph Salerno, Nathan Salmon, Wesley C. Salmon, Constantine Sandis, David H. Sanford, Marco Santambrogio, David Sapire, Ruth A. Saunders, Geoffrey Sayre-McCord, Charles Sayward, James P. Scanlan, Richard Schacht, Tamar Schapiro, Frederick F. Schmitt, Jerome B. Schneewind, Calvin O. Schrag, Alan D. Schrift, George F. Schumm, Jean-Loup Seban, David N. Sedley, Kenneth Seeskin, Krister Segerberg, Charlene Haddock Seigfried, Dennis M. Senchuk, James F. Sennett, William Lad Sessions, Stewart Shapiro, Tommie Shelby, Donald W. Sherburne, Christopher Shields, Roger A. Shiner, Sydney Shoemaker, Robert K. Shope, Kwong-loi Shun, Wilfried Sieg, A. John Simmons, Robert L. Simon, Marcus G. Singer, Georgette Sinkler, Walter Sinnott-Armstrong, Matti T. Sintonen, Lawrence Sklar, Brian Skyrms, Robert C. Sleigh, Michael Anthony Slote, Hans Sluga, Barry Smith, Michael Smith, Robin Smith, Robert Sokolowski, Robert C. Solomon, Marta Soniewicka, Philip Soper, Ernest Sosa, Nicholas Southwood, Paul Vincent Spade, T. L. S. Sprigge, Eric O. Springsted, George J. Stack, Rebecca Stangl, Jason Stanley, Florian Steinberger, Sören Stenlund, Christopher Stephens, James P. Sterba, Josef Stern, Matthias Steup, M. A. Stewart, Leopold Stubenberg, Edith Dudley Sulla, Frederick Suppe, Jere Paul Surber, David George Sussman, Sigrún Svavarsdóttir, Zeno G. Swijtink, Richard Swinburne, Charles C. Taliaferro, Robert B. Talisse, John Tasioulas, Paul Teller, Larry S. Temkin, Mark Textor, H. S. Thayer, Peter Thielke, Alan Thomas, Amie L. Thomasson, Katherine Thomson-Jones, Joshua C. Thurow, Vzalerie Tiberius, Terrence N. Tice, Paul Tidman, Mark C. Timmons, William Tolhurst, James E. Tomberlin, Rosemarie Tong, Lawrence Torcello, Kelly Trogdon, J. D. Trout, Robert E. Tully, Raimo Tuomela, John Turri, Martin M. Tweedale, Thomas Uebel, Jennifer Uleman, James Van Cleve, Harry van der Linden, Peter van Inwagen, Bryan W. Van Norden, René van Woudenberg, Donald Phillip Verene, Samantha Vice, Thomas Vinci, Donald Wayne Viney, Barbara Von Eckardt, Peter B. M. Vranas, Steven J. Wagner, William J. Wainwright, Paul E. Walker, Robert E. Wall, Craig Walton, Douglas Walton, Eric Watkins, Richard A. Watson, Michael V. Wedin, Rudolph H. Weingartner, Paul Weirich, Paul J. Weithman, Carl Wellman, Howard Wettstein, Samuel C. Wheeler, Stephen A. White, Jennifer Whiting, Edward R. Wierenga, Michael Williams, Fred Wilson, W. Kent Wilson, Kenneth P. Winkler, John F. Wippel, Jan Woleński, Allan B. Wolter, Nicholas P. Wolterstorff, Rega Wood, W. Jay Wood, Paul Woodruff, Alison Wylie, Gideon Yaffe, Takashi Yagisawa, Yutaka Yamamoto, Keith E. Yandell, Xiaomei Yang, Dean Zimmerman, Günter Zoller, Catherine Zuckert, Michael Zuckert, Jack A. Zupko (J.A.Z.)
- Edited by Robert Audi, University of Notre Dame, Indiana
-
- Book:
- The Cambridge Dictionary of Philosophy
- Published online:
- 05 August 2015
- Print publication:
- 27 April 2015, pp ix-xxx
-
- Chapter
- Export citation
Contributors
-
- By Stefan Bechtold, Barton Beebe, Lionel Bently, Graeme B. Dinwoodie, Stacey L. Dogan, Rochelle C. Dreyfuss, Séverine Dusollier, Susy Frankel, Jeanne C. Fromer, Dev S. Gangjee, Daniel Gervais, Jane C. Ginsburg, C. Scott Hemphill, Robin Jacob, Annette Kur, David Lefranc, Joseph P. Liu, Justine Pila, Carol M. Rose, Ted Sichelman, Katherine J. Strandburg, Jeannie Suk, Rebecca Tushnet, Silke von Lewinski
- Edited by Rochelle Cooper Dreyfuss, New York University, Jane C. Ginsburg, Columbia University, New York
-
- Book:
- Intellectual Property at the Edge
- Published online:
- 05 May 2014
- Print publication:
- 19 June 2014, pp x-xvi
-
- Chapter
- Export citation
Contributors
-
- By Syed S. Ali, Nathan Allen, John E. Arbo, Elizabeth Arrington, Ani Aydin, Kenneth R. L. Bernard, Amy Caggiula, Nolan Caldwell, Jennifer L. Carey, Jennifer Carnell, Jayaram Chelluri, Michael N. Cocchi, Cristal Cristia, Vishal Demla, Bram Dolcourt, Andrew Eyre, Shawn Fagan, Brandy Ferguson, Sarah Fisher, Jonathan Friedstat, Brian C. Geyer, Brandon Godbout, Jeremy Gonda, Jeremy Goverman, Ashley L. Greiner, Casey Grover, Carla Haack, Abigail Hankin, John W. Hardin, Katrina L. Harper, Gregory Hayward, Stephen Hendriksen, Daniel Herbert-Cohen, Nadine Himelfarb, Calvin E. Hwang, Jacob D. Isserman, Joshua Jauregui, Joshua W. Joseph, Elena Kapilevich, Feras H. Khan, Sarvotham Kini, Karen A. Kinnaman, Ruth Lamm, Calvin Lee, Jarone Lee, Charles Lei, John Lemos, Daniel J. Lepp, Elisabeth Lessenich, Brandon Maughan, Julie Mayglothling, Kevin McConnell, Laura Medford-Davis, Kamal Medlej, Heather Meissen, Payal Modi, Joel Moll, Jolene H. Nakao, Matthew Nicholls, Lindsay Oelze, Carolyn Maher Overman, Viral Patel, Timothy C. Peck, Jeffrey Pepin, Candace Pettigrew, Byron Pitts, Zubaid Rafique, Chanu Rhee, Jonathan C. Roberts, Daniel Rolston, Steven C. Rougas, Benjamin Schnapp, Kathryn A. Seal, Raghu Seethala, Todd A. Seigel, Navdeep Sekhon, Kaushal Shah, Robert L. Sherwin, Kirill Shishlov, Ashley Shreves, Sebastian Siadecki, Jeffrey N. Siegelman, Liza Gonen Smith, Ted Stettner, Marie Carmelle Tabuteau, Joseph E. Tonna, N. Seth Trueger, Chad Van Ginkel, Bina Vasantharam, Graham Walker, Susan Wilcox, Sandra J. Williams, Matthew L. Wong, Nelson Wong, Samantha Wood, John Woodruff, Benjamin Zabar
- Edited by Kaushal Shah, Jarone Lee, Kamal Medlej, American University of Beirut, Scott D. Weingart
-
- Book:
- Practical Emergency Resuscitation and Critical Care
- Published online:
- 05 November 2013
- Print publication:
- 24 October 2013, pp xi-xx
-
- Chapter
- Export citation
Contributors
-
- By Basem Abdelmalak, Joseph Abdelmalak, Alaa A. Abd-Elsayed, David L. Adams, Eric E. Adelman, Maged Argalious, Endrit Bala, Gene H. Barnett, Sheron Beltran, Andrew Bielaczyc, William Bingaman, James M. Blum, Alina Bodas, Vera Borzova, Richard Bowers, Adam Brown, Chad M. Brummett, Alexandra S. Bullough, James F. Burke, Juan P. Cata, Neeraj Chaudhary, Michael J. Claybon, Miguel Cruz, Milind Deogaonkar, Vikram Dhawan, Thomas Didier, D. John Doyle, Zeyd Ebrahim, Hesham Elsharkawy, Wael Ali Sakr Esa, Ehab Farag, Ryen D. Fons, Joseph J. Gemmete, Matt Giles, Phil Gillen, Goodarz Golmirzaie, Marcos Gomes, Lisa Grilly, Maged Guirguis, David W. Healy, Heather Hervey-Jumper, Shawn L. Hervey-Jumper, Paul E. Hilliard, Samuel A. Irefin, George K. Istaphanous, Teresa L. Jacobs, Ellen Janke, Greta Jo, James W. Jones, Rami Karroum, Allen Keebler, Stephen J. Kimatian, Colleen G. Koch, Robert Scott Kriss, Andrea Kurz, Jia Lin, Michael D. Maile, Negmeldeen F. Mamoun, Mariel Manlapaz, Edward Manno, Donn Marciniak, Piyush Mathur, Nicholas F. Marko, Matthew Martin, George A. Mashour, Marco Maurtua, Scott T. McCardle, Julie McClelland, Uma Menon, Paul S. Moor, Laurel E. Moore, Ruairi Moulding, Dileep R. Nair, Todd Nelson, Julie Niezgoda, Edward Noguera, Jerome O’Hara, Aditya S. Pandey, Mauricio Perilla, Paul Picton, Marc J. Popovich, J. Javier Provencio, Venkatakrishna Rajajee, Mohit Rastogi, Stacy Ritzman, Lauryn R. Rochlen, Leif Saager, Vivek Sabharwal, Oren Sagher, Kenneth Saliba, Milad Sharifpour, Lesli E. Skolarus, Paul Smythe, Wolf H. Stapelfeldt, William R. Stetler, Peter Stiles, Vijay Tarnal, Khoi D. Than, B. Gregory Thompson, Alparslan Turan, Christopher R. Turner, Justin Upp, Sumeet Vadera, Jennifer Vance, Anthony C. Wang, Robert J. Weil, Marnie B. Welch, Karen K. Wilkins, Erin S. Williams, George N. Youssef, Asma Zakaria, Sherif S. Zaky, Andrew Zura
- Edited by George A. Mashour, Ehab Farag
-
- Book:
- Case Studies in Neuroanesthesia and Neurocritical Care
- Published online:
- 03 May 2011
- Print publication:
- 03 February 2011, pp x-xvi
-
- Chapter
- Export citation
Contributors
-
- By Shamsuddin Akhtar, Greg Albert, Sidney Allison, Muhammad Anwar, Haruo Arita, Amanda Barker, Mary Hanna Bekhit, Jeanna Blitz, Tyson Bolinske, David Burbulys, Asokumar Buvanendran, Gregory Cain, Keith A. Candiotti, Daniel B. Carr, Derek Chalmers, John Charney, Rex Cheng, Roger Chou, Keun Sam Chung, Anna Clebone, Frederick Conlin, Susan Dabu-Bondoc, Tiffany Denepitiya-Balicki, Jeanette Derdemezi, Anahat Kaur Dhillon, Ho Dzung, Juan Jose Egas, Stephen M. Eskaros, Zhuang T. Fang, Claudia R. Fernandez Robles, Victor A. Filadora, Ellen Flanagan, Dan Froicu, Allison Gandey, Nehal Gatha, Boris Gelman, Christopher Gharibo, Muhammad K. Ghori, Brian Ginsberg, Michael E. Goldberg, Jeff Gudin, Thomas Halaszynski, Martin Hale, Dorothea Hall, Craig T. Hartrick, Justin Hata, Lars E. Helgeson, Joe C. Hong, Richard W. Hong, Balazs Horvath, Eric S. Hsu, Gabriel Jacobs, Jonathan S. Jahr, Rongjie Jaing, Inderjeet Singh Julka, Zeev N. Kain, Clinton Kakazu, Kianusch Kiai, Mary Keyes, Michael M. Kim, Peter G. Lacouture, Ryan Lanier, Vivian K. Lee, Mark J. Lema, Oscar A. de Leon-Casasola, Imanuel Lerman, Philip Levin, Steven Levin, JinLei Li, Eric C. Lin, Sharon Lin, David A. Lindley, Ana M. Lobo, Marisa Lomanto, Mirjana Lovrincevic, Brenda C. McClain, Tariq Malik, Jure Marijic, Joseph Marino, Laura Mechtler, Alan Miller, Carly Miller, Amit Mirchandani, Sukanya Mitra, Fleurise Montecillo, James M. Moore, Debra E. Morrison, Philip F. Morway, Carsten Nadjat-Haiem, Hamid Nourmand, Dana Oprea, Sunil J. Panchal, Edward J. Park, Kathleen Ji Park, Kellie Park, Parisa Partownavid, Akta Patel, Bijal Patel, Komal D. Patel, Neesa Patel, Swati Patel, Paul M. Peloso, Danielle Perret, Anthony DePlato, Marjorie Podraza Stiegler, Despina Psillides, Mamatha Punjala, Johan Raeder, Siamak Rahman, Aziz M. Razzuk, Maggy G. Riad, Kristin L. Richards, R. Todd Rinnier, Ian W. Rodger, Joseph Rosa, Abraham Rosenbaum, Alireza Sadoughi, Veena Salgar, Leslie Schechter, Michael Seneca, Yasser F. Shaheen, James H. Shull, Elizabeth Sinatra, Raymond S. Sinatra, Neil Singla, Neil Sinha, Denis V. Snegovskikh, Dmitri Souzdalnitski, Julie Sramcik, Zoreh Steffens, Alexander Timchenko, Vadim Tokhner, Marc C. Torjman, Co T. Truong, Nalini Vadivelu, Ashley Vaughn, Anjali Vira, Eugene R. Viscusi, Dajie Wang, Shu-ming Wang, J. Michael Watkins-Pitchford, Steven J. Weisman, Ira Whitten, Bryan S. Williams, Jeremy M. Wong, Thomas Wong, Christopher Wray, Yaw Wu, Anthony T. Yarussi, Laurie Yonemoto, Bita H. Zadeh, Jill Zafar, Martha Zegarra, Keren Ziv
- Edited by Raymond S. Sinatra, Jonathan S. Jahr, University of California, Los Angeles, School of Medicine, J. Michael Watkins-Pitchford
-
- Book:
- The Essence of Analgesia and Analgesics
- Published online:
- 06 December 2010
- Print publication:
- 14 October 2010, pp xi-xviii
-
- Chapter
- Export citation