3 results
How COVID-19 spread varied by resident length of stay and resident–staff transmission pathways over time in US nursing homes
- Jessica Healy, Prabasaj Paul, Brajendra Singh, Nimalie Stone, Kara Jacobs Slifka, Rachel Slayton
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, p. s111
-
- Article
-
- You have access Access
- Open access
- Export citation
-
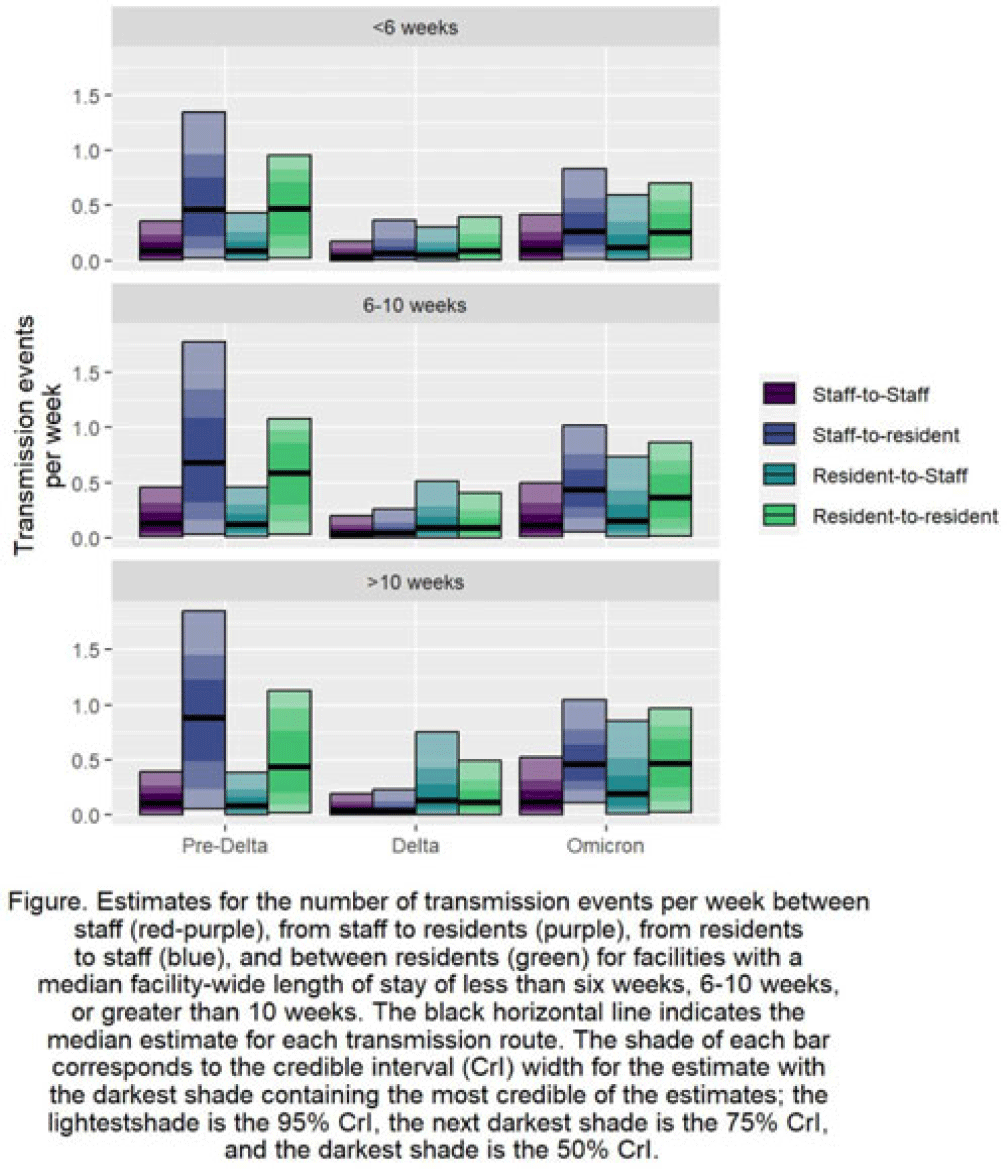
Background: Pathogen transmission among staff and residents in nursing homes can vary depending on their interactions and by the amount of time a resident receives care in the facility. Understanding the relative differences in transmission rates between and among staff and residents can identify the pathways that contributed most to the spread of SARS-CoV-2 in US nursing homes. Further exploring relative differences by categorizing facilities by residents’ lengths of stay can identify priority categories for intervention. Methods: Using US National Healthcare Safety Network (NHSN) surveillance data on resident and staff cases, vaccination, and resident deaths during June 2020–June 2022, we estimated SARS-CoV-2 transmission among and between residents and staff. We used a Bayesian inversion of a susceptible–exposed–infected–removed–virus–death (SEIRVD) compartmental model to produce the estimates. The facilities were divided into those with median length of stay (LOS) among the residents of 10 weeks. Additional inputs included the incidence and vaccination levels of the county where each facility was located. For the compartmental model, all data were averaged to form a representative facility for each category. Transmission was estimated separately for 3 periods: (1) June 2020–March 2021 as before the SARS-CoV-2 delta variant, (2) April 2021—October 2021 during SARS-CoV-2 delta variant dominance, and (3) November 2021—June 2022 during the prevalence of the SARS-CoV-2 omicron variant. Results: Regardless of facility category, transmission was highest from staff to residents or resident to resident (Fig.). These estimates of transmission were highest during the pre–SARS-CoV-2 delta variant phase. Transmission in that phase was highest in the facilities with LOS >10 weeks from staff to residents at 0.88 per week (95% credible interval [CrI], 0.06–1.85), in the facilities with LOS 6–10 weeks from staff to residents at 0.68 per week (95% CrI, 0.03–1.78), and in the facilities with LOS <6 weeks between residents at 0.47 per week (95% CrI, 0.02–0.95). Conclusions: Staff-to-resident or resident-to-resident transmission were the dominant pathways of spread of SARS-CoV-2 across the periods or the facility categories. Facilities with LOS 6 weeks or longer had higher median transmission estimates across the periods and transmission routes compared to facilities with LOS less than 6 weeks, implying that when prioritization of intervention resources is needed, facilities caring for populations with longer stays could be prioritized.
Disclosures: None
Targeted gown and glove use to prevent Staphylococcus aureus acquisition in community-based nursing homes: A pilot study
- Alison D. Lydecker, Patience A. Osei, Lisa Pineles, J. Kristie Johnson, Jacquelyn Meisel, O. Colin Stine, Laurence Magder, Ayse P. Gurses, Joan Hebden, Cagla Oruc, Lona Mody, Kara Jacobs Slifka, Nimalie D. Stone, Mary-Claire Roghmann
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 42 / Issue 4 / April 2021
- Published online by Cambridge University Press:
- 20 October 2020, pp. 448-454
- Print publication:
- April 2021
-
- Article
- Export citation
-
Objective:
To test the feasibility of targeted gown and glove use by healthcare personnel caring for high-risk nursing-home residents to prevent Staphylococcus aureus acquisition in short-stay residents.
Design:Uncontrolled clinical trial.
Setting:This study was conducted in 2 community-based nursing homes in Maryland.
Participants:The study included 322 residents on mixed short- and long-stay units.
Methods:During a 2-month baseline period, all residents had nose and inguinal fold swabs taken to estimate S. aureus acquisition. The intervention was iteratively developed using a participatory human factors engineering approach. During a 2-month intervention period, healthcare personnel wore gowns and gloves for high-risk care activities while caring for residents with wounds or medical devices, and S. aureus acquisition was measured again. Whole-genome sequencing was used to assess whether the acquisition represented resident-to-resident transmission.
Results:Among short-stay residents, the methicillin-resistant S. aureus acquisition rate decreased from 11.9% during the baseline period to 3.6% during the intervention period (odds ratio [OR], 0.28; 95% CI, 0.08–0.92; P = .026). The methicillin-susceptible S. aureus acquisition rate went from 9.1% during the baseline period to 4.0% during the intervention period (OR, 0.41; 95% CI, 0.12–1.42; P = .15). The S. aureus resident-to-resident transmission rate decreased from 5.9% during the baseline period to 0.8% during the intervention period.
Conclusions:Targeted gown and glove use by healthcare personnel for high-risk care activities while caring for residents with wounds or medical devices, regardless of their S. aureus colonization status, is feasible and potentially decreases S. aureus acquisition and transmission in short-stay community-based nursing-home residents.
Transmission of Carbapenemase-Producing Hypervirulent Klebsiella pneumoniae in Georgia, 2018–2019
- Jeanne Negley, Elizabeth Smith, Maroya Walters, Tonia Parrott, Richard Stanton, David Ham, Jacobs Slifka Kara, Patricia Kopp, Mary Connelly, Gebre Tiga, Gillian McAllister, Alison Halpin, Cherie Drenzek
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s414-s415
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: In April 2019, the Georgia Department of Public Health (DPH) initiated whole-genome sequencing (WGS) on NDM-producing Enterobacteriaceae identified since January 2018. The WGS data analyzed at CDC identified related Klebsiella pneumoniae isolates with hypervirulence markers from 2 patients. Carbapenemase-producing hypervirulent K. pneumoniae (CP-hvKP) are rarely reported in the United States, but they can to cause serious, highly resistant, invasive infections. We conducted an investigation to identify cases and prevent spread. Methods: We defined a case as NDM-producing K. pneumoniae with ≥4 hypervirulence markers identified by WGS, isolated from any specimen source from a Georgia patient. We reviewed the case patient’s medical history to identify potentially affected facilities. We also performed PCR-based colonization screening and retrospective and prospective laboratory-based surveillance. Finally, we assessed facility infection control practices. Results: Overall, 7 cases from 3 case patients (A, B, and C) were identified (Fig. 1). The index case specimen was collected from case-patient A at ventilator-capable skilled nursing facility 1 (vSNF1) in May 2018. Case-patient A had been hospitalized for 1 month in India before transfer to the United States. Case-patient B’s initial isolate was collected in January 2019 on admission to vSNF2 from a critical access hospital (CAH). The CAH laboratory retrospectively identified case-patient C, who overlapped with case-patient B at the CAH in October 2018. The CAH and the vSNF2 are geographically distant from vSNF1. Case-patients B and C had no known epidemiologic links to case-patient A. Colonization screening occurred at vSNF1 in May 2018, following detection of NDM-producing K. pneumoniae from case-patient A ∼1 year before determining that the isolate carried hypervirulence markers. Among 30 residents screened, 1 had NDM and several had other carbapenemases. Subsequent screening did not identify additional NDM. Colonization screening of 112 vSNF2 residents and 13 CAH patients in 2019 did not reveal additional case patients; case-patient B resided at vSNF2 at the time of screening and remained colonized. At all 3 facilities, the DPH assessed infection control practices, issued recommendations to resolve lapses, and monitored implementation. The DPH sequenced all 27 Georgia NDM–K. pneumoniae isolates identified since January 2018; all were different multilocus sequence types from the CP-hvKP isolates, and none possessed hypervirulence markers. Conclusions: We hypothesize that CP-hvKP was imported by a patient hospitalized in India and spread to 3 Georgia facilities in 2 distinct geographic regions through indirect patient transfers. Although a response to contain NDM at vSNF1 in 2018 likely limited CP-hvKP transmission, WGS identified hvKP and established the relatedness of isolates from distinct regions, thereby directing the DPH’s additional containment activities to halt transmission.
Funding: None
Disclosures: None




