2 results
A Cluster of Coronavirus Disease 2019 (COVID-19) Cases on an Inpatient Hospital Unit Involving Multiple Modes of Transmission
- Kelsey Witherspoon, Michael Haden, Justin Smyer, Jennifer Flaherty, Heather Smith, Nora Colburn, Christina Liscynesky, James Allen, Shandra Day
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue S1 / July 2021
- Published online by Cambridge University Press:
- 29 July 2021, pp. s2-s3
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: The Ohio State University Wexner Medical Center identified a cluster of coronavirus disease 2019 (COVID-19) cases on an inpatient geriatric stroke care unit involving both patients and staff. The period of suspected severe acute respiratory coronavirus virus 2 (SARS-CoV-2) transmission and exposure on the unit was December 20, 2020, to January 1, 2021, with some patients and staff developing symptoms and testing positive within the 14 days thereafter. Methods: An epidemiologic investigation was conducted via chart review, staff interviews, and contact tracing to identify potential patient and staff linkages. All staff who worked on the unit were offered testing regardless of the presence of symptoms as well as all patients admitted during the outbreak period. Results: In total, 6 patients likely acquired COVID-19 in the hospital (HCA). An additional 6 patients admitted to the unit during the outbreak period subsequently tested positive but had other possible exposures outside the hospital (Fig. 1). One patient failed to undergo COVID-19 testing on admission but tested positive early in the cluster and is suspected to have contributed to patient to employee transmission. Moreover, 32 employees who worked on the unit in some capacity during this period tested positive, many of whom became symptomatic during their shifts. In addition, 18 employees elected for asymptomatic testing with 3 testing positive; these were included in the total. Some staff also identified potential community exposures. Additionally, staff reported an employee who was working while symptomatic with inconsistent mask use (index employee) early in the outbreak period. The index employee likely contributed to employee transmission but had no direct patient contact. Our epidemiologic investigation ultimately identified 12 employees felt to be linked to transmission based on significant, direct patient care provided to the patients within the outbreak period (Fig. 1). In addition, 3 employees had an exposure outside the hospital indicating likely community transmission. Conclusions: Transmission was felt to be multidirectional and included employee-to-employee, employee-to-patient, and patient-to-employee transmission in the setting of widespread community transmission. Interventions to stop transmission included widespread staff testing, staff auditing regarding temperature and symptom monitoring, and re-education on infection prevention practices. Particular focus was placed on appropriate PPE use including masking and eye protection, hand hygiene, and cleaning and disinfection practices throughout the unit. SARS-CoV-2 admission testing and limited visitation remain important strategies to minimize transmission in the hospital.
Figure 1.
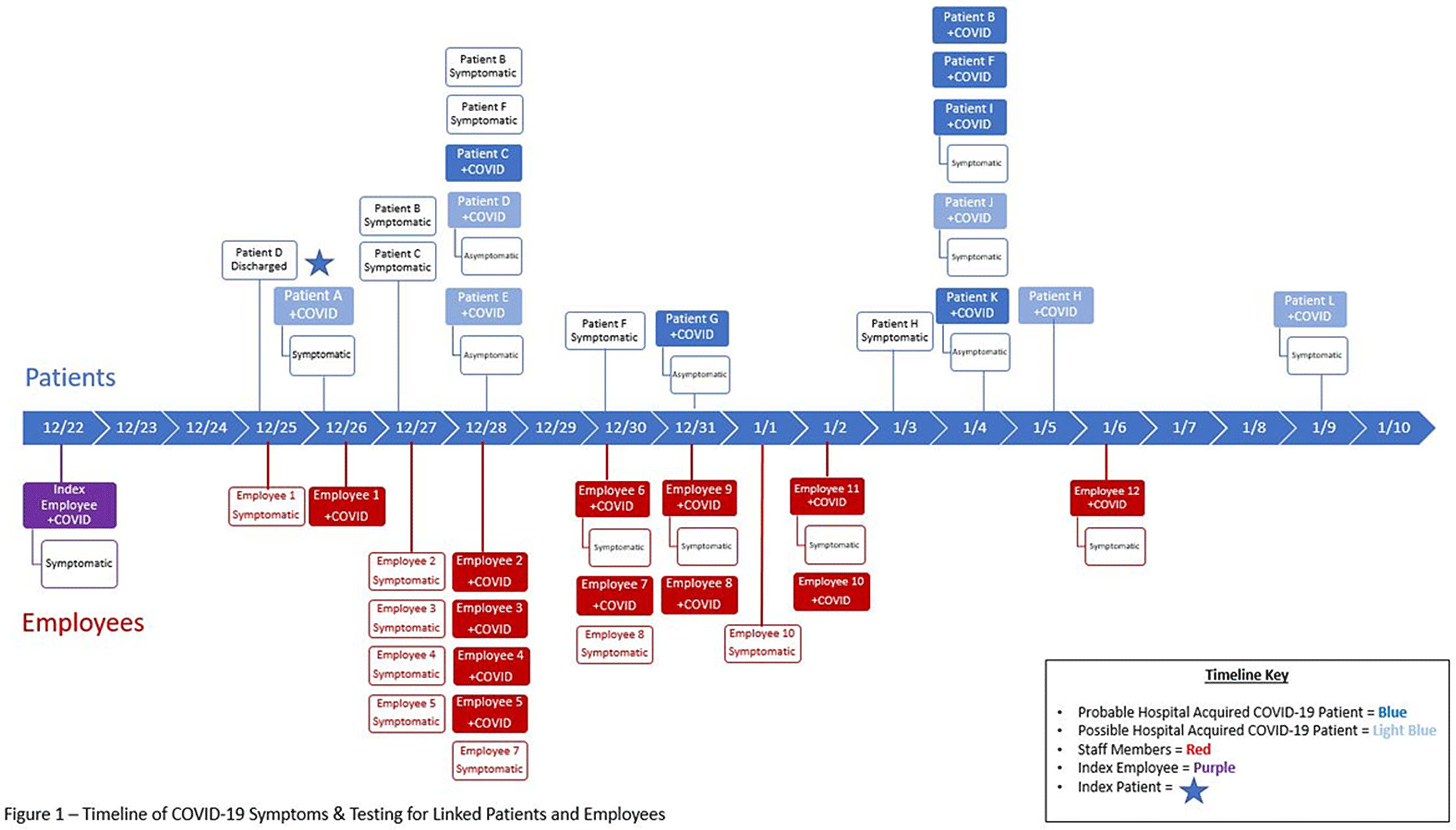
Funding: No
Disclosures: None
Transmission of COVID-19 on an Inpatient Hospital Prison Unit
- Kelsey Witherspoon, Manisha Shah, Justin Smyer, Nora Colburn, Christina Liscynesky, Courtney Hebert, Shandra Day
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue S1 / July 2021
- Published online by Cambridge University Press:
- 29 July 2021, p. s47
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Prison populations have been disproportionally affected by COVID-19, partly due to challenges related to social distancing. Data on viral transmission dynamics in inpatient prison units remain limited. The Ohio State University Wexner Medical Center (OSUWMC) has a 24-bed inpatient prison unit in collaboration with the Ohio Department of Rehabilitations and Corrections (ODRC). The unit has 5 shared rooms holding 4 patients each and 4 single-patient rooms. Several cases of inpatient transmission of COVID-19 were identified on the inpatient prison unit. Methods: An IRB-approved retrospective chart review was conducted to evaluate inpatient transmission dynamics of hospital-acquired (HCA) COVID-19. All ODRC patients admitted from March 1 to April 24, 2020, were included. Patients assigned to the prison unit during their hospital stay were evaluated for potential HCA COVID-19, defined as a positive SARS-CoV-2 test ≥4 days after admission. Patient characteristics, testing data, symptoms, aerosol-generating procedures (AGPs), and room assignments were reviewed. Healthcare workers (HCWs) and correction officers (COs) working on the unit who tested positive during this period were identified. Results: In total, 142 ODRC patients were admitted during the study period and 89% had a positive SARS-CoV-2 testing prior to or during admission. Also, 61 patients (43%) were assigned to the prison unit. Moreover, 8 patients on the unit met potential HCA COVID-19 definition with 7 linked to 3 distinct clusters. Also, 7 COs had COVID-19 (outside hospital exposure) and 5 HCWs acquired COVID-19 from patient exposure on the unit. In cluster 1, 4 patients admitted to the same room developed HCA COVID-19. A symptomatic index patient not tested on admission given an atypical presentation required CPAP and frequent nebulizer treatments. In cluster 2, 1 patient from cluster 1 was transferred to another room. The new roommate subsequently developed HCA COVID-19. In cluster 3, a symptomatic correctional officer was assigned to 2 patients in a shared room; the patients later developed HCA COVID-19. Conclusions: Three patient clusters of HCA COVID-19 on a prison unit were identified. Aerosol transmission potentially played a role in cluster 1. Inpatient transmission within the unit prompted updated guidance for ODRC admissions, including universal SARS-CoV-2 admission testing, excluding patients requiring AGPs from shared rooms, and preemptive isolation for patients from an ODRC facility experiencing a COVID-19 surge. Universal testing was quickly expanded to all inpatient admissions. HCWs and COs were also linked to inpatient transmission, highlighting the importance of strict infection control practices for patient populations who cannot socially distance.
Funding: No
Disclosures: None




