5 results
General intelligence in adult patients with early- and adult-onset schizophrenia
- T. Calkova, L. Mørch-Johnsen, R. Elle Smelror, K. Nordbø Jørgensen, S. Cervenka, K. Collste, A. Vaskinn, A. Margrethe Myhre, O. A. Andreassen, T. Ueland, I. Agartz, D. Andreou
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S490-S491
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Early-onset schizophrenia (EOS) is a relatively uncommon disorder with psychotic symptoms emerging before 18 years of age. Although still under debate, EOS may be a more severe disorder relative to adult-onset schizophrenia (AOS), with worse prognosis. Cognitive deficits are a core feature of schizophrenia, accounting for a large part of the detrimental effect of the disorder and may reflect underlying neurodevelopmental disturbances. Some but not all previous studies show that the magnitude of cognitive deficits, including intelligence quotient (IQ), in patients with schizophrenia is dependent on the age of onset.
ObjectivesWe aimed to assess IQ in adult patients with EOS and AOS, and healthy controls. We hypothesized that patients with EOS would show lower IQ than those with AOS, and both patient groups lower IQ than HC.
MethodsWe included 136 adult patients with EOS (mean age: 24.7 (7.7) years, mean duration of illness: 9.3 (8.5) years, 50% women), 382 patients with AOS (mean age: 32.4 (9.5) years, mean duration of illness: 5.7 (6.6) years, 40.1% women) and 896 adult healthy controls (mean age: 33.2 (9.2) years, 47.1% women). We assessed current IQ with the Wechsler Abbreviated Scale of Intelligence (WASI) which yielded verbal (VIQ), performance (PIQ) and full-scale IQ (FIQ) scores. In a post-hoc analysis, we estimated premorbid IQ using the National Adult Reading Test (NART). We applied analyses of covariance (ANCOVAs) to investigate the putative differences in IQ scores and IQ change between patients with EOS, patients with AOS and healthy controls.
ResultsIn sex-, and age-adjusted models, FIQ and PIQ, but not VIQ, were significantly lower in EOS than in AOS (p=0.03, p<0.001 and p=0.428, respectively) (Image). Patients with EOS had fewer years of education than patients with AOS (p<0.001); the PIQ but not the FIQ difference between EOS and AOS remained significant after adjustment for education years (p=0.016 and p=0.333, respectively). Both patient groups had significantly lower IQ scores than healthy controls (Image). Further, patients with EOS and patients with AOS did not significantly differ in estimated premorbid IQ (109 and 110 units, respectively, p=0.092), whereas patients with EOS had a significantly larger estimated IQ decline after the disease onset compared to patients with AOS (12 and 9 units decline, respectively, p=0.015).
Image:
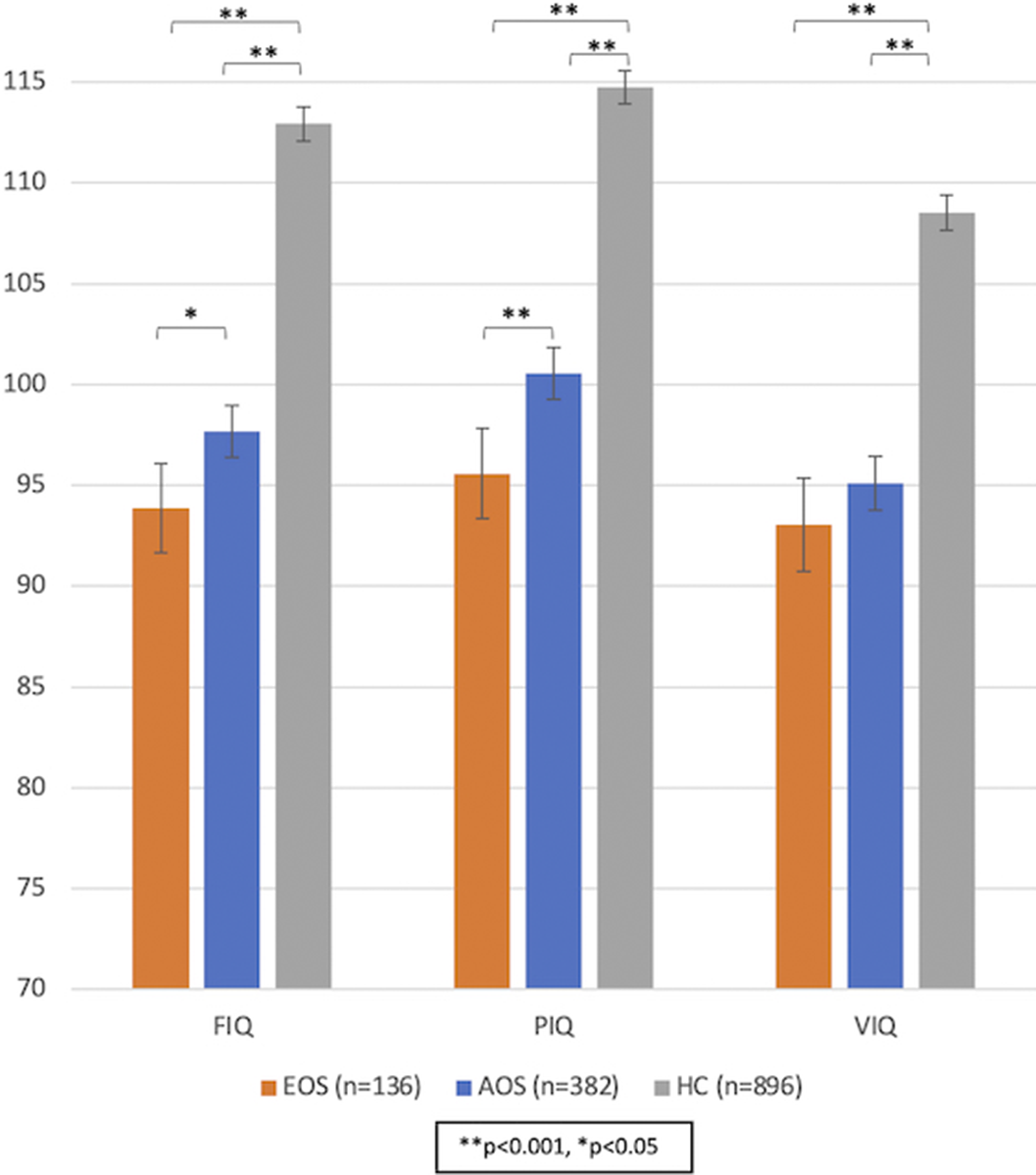 Conclusions
ConclusionsOur findings show that adult patients with EOS have significantly lower PIQ and FIQ scores, and significantly larger IQ decline after the disease onset, but not lower premorbid IQ, compared to patients with AOS. The adolescent onset of psychotic symptoms is linked, as expected, to fewer total years of education, which appears to explain the lower FIQ but only partially the lower PIQ in EOS, which may thereby be linked to the disorder per se.
Disclosure of InterestT. Calkova: None Declared, L. Mørch-Johnsen: None Declared, R. Elle Smelror: None Declared, K. Nordbø Jørgensen: None Declared, S. Cervenka: None Declared, K. Collste: None Declared, A. Vaskinn: None Declared, A. Margrethe Myhre: None Declared, O. A. Andreassen Consultant of: HealthLytix, Speakers bureau of: Lundbeck and Sunovion, T. Ueland: None Declared, I. Agartz: None Declared, D. Andreou: None Declared
Auditory Cortex Characteristics in Early Onset Psychosis and its Associations with Auditory Hallucinations: A Structural MRI Study
- R.E. Smelror, V. Lonning, L. Mørch-Johnsen, S. Nerland, T. Gurholt, I. Agartz
-
- Journal:
- European Psychiatry / Volume 41 / Issue S1 / April 2017
- Published online by Cambridge University Press:
- 23 March 2020, p. S59
-
- Article
-
- You have access Access
- Export citation
-
Introduction
Smaller auditory cortex volume in schizophrenia patients with auditory hallucinations (AH) may be a result of reduced cortical surface area and/or cortical thickness. A neuro–imaging study from our group demonstrated that adult schizophrenia spectrum patients with AH had significantly thinner cortex in the left side Heschl's gyrus (HG), compared to patients without AH, and healthy controls (HC).
ObjectivesThis study aims to investigate if adolescents with early-onset psychosis (EOP) and AH demonstrate thinner cortices in HG, as found in Mørch-Johnsen et al. in 2016, compared to EOP patients without AH, and HC.
MethodsEOP patients (schizophrenia spectrum, psychotic disorder not otherwise specified) (n = 29) underwent MRI. Mean volume, cortical thickness and surface area in auditory cortex regions (HG, superior temporal gyrus [STG]) were compared between patients with AH (n = 20) and without AH (n = 9), measured with item P3 from the Positive And Negative Syndrome Scale (PANSS), and 48 HC.
ResultsPreliminary results show no significant differences between patients with and without AH and HC in mean volume, cortical thickness, or surface area in HG or STG. There were no significant side differences across hemispheres for these structures.
ConclusionsAH in EOP were not related to smaller volume, thinner cortex or reduced surface area in auditory cortex regions. To overcome the limitation of having a relatively small sample size, the sample will be expanded with other EOP cohorts. Investigations into HG structure variation in relation to AH in EOP will also be conducted.
Disclosure of interestThe authors have not supplied their declaration of competing interest.
Prefrontal cortical thinning links to negative symptoms in schizophrenia via the ENIGMA consortium
- E. Walton, D. P. Hibar, T. G. M. van Erp, S. G. Potkin, R. Roiz-Santiañez, B. Crespo-Facorro, P. Suarez-Pinilla, N. E. M. van Haren, S. M. C. de Zwarte, R. S. Kahn, W. Cahn, N. T. Doan, K. N. Jørgensen, T. P. Gurholt, I. Agartz, O. A. Andreassen, L. T. Westlye, I. Melle, A. O. Berg, L. Morch-Johnsen, A. Færden, L. Flyckt, H. Fatouros-Bergman, Karolinska Schizophrenia Project Consortium (KaSP), E. G. Jönsson, R. Hashimoto, H. Yamamori, M. Fukunaga, N. Jahanshad, P. De Rossi, F. Piras, N. Banaj, G. Spalletta, R. E. Gur, R. C. Gur, D. H. Wolf, T. D. Satterthwaite, L. M. Beard, I. E. Sommer, S. Koops, O. Gruber, A. Richter, B. Krämer, S. Kelly, G. Donohoe, C. McDonald, D. M. Cannon, A. Corvin, M. Gill, A. Di Giorgio, A. Bertolino, S. Lawrie, T. Nickson, H. C. Whalley, E. Neilson, V. D. Calhoun, P. M. Thompson, J. A. Turner, S. Ehrlich
-
- Journal:
- Psychological Medicine / Volume 48 / Issue 1 / January 2018
- Published online by Cambridge University Press:
- 26 May 2017, pp. 82-94
-
- Article
- Export citation
-
Background
Our understanding of the complex relationship between schizophrenia symptomatology and etiological factors can be improved by studying brain-based correlates of schizophrenia. Research showed that impairments in value processing and executive functioning, which have been associated with prefrontal brain areas [particularly the medial orbitofrontal cortex (MOFC)], are linked to negative symptoms. Here we tested the hypothesis that MOFC thickness is associated with negative symptom severity.
MethodsThis study included 1985 individuals with schizophrenia from 17 research groups around the world contributing to the ENIGMA Schizophrenia Working Group. Cortical thickness values were obtained from T1-weighted structural brain scans using FreeSurfer. A meta-analysis across sites was conducted over effect sizes from a model predicting cortical thickness by negative symptom score (harmonized Scale for the Assessment of Negative Symptoms or Positive and Negative Syndrome Scale scores).
ResultsMeta-analytical results showed that left, but not right, MOFC thickness was significantly associated with negative symptom severity (βstd = −0.075; p = 0.019) after accounting for age, gender, and site. This effect remained significant (p = 0.036) in a model including overall illness severity. Covarying for duration of illness, age of onset, antipsychotic medication or handedness weakened the association of negative symptoms with left MOFC thickness. As part of a secondary analysis including 10 other prefrontal regions further associations in the left lateral orbitofrontal gyrus and pars opercularis emerged.
ConclusionsUsing an unusually large cohort and a meta-analytical approach, our findings point towards a link between prefrontal thinning and negative symptom severity in schizophrenia. This finding provides further insight into the relationship between structural brain abnormalities and negative symptoms in schizophrenia.
Alcohol use is associated with thinner cerebral cortex and larger ventricles in schizophrenia, bipolar disorder and healthy controls
- E. H. Lange, S. Nerland, K. N. Jørgensen, L. Mørch-Johnsen, R. Nesvåg, C. B. Hartberg, U. K. Haukvik, K. Osnes, I. Melle, O. A. Andreassen, I. Agartz
-
- Journal:
- Psychological Medicine / Volume 47 / Issue 4 / March 2017
- Published online by Cambridge University Press:
- 10 November 2016, pp. 655-668
-
- Article
- Export citation
-
Background
Excessive alcohol use is associated with brain damage but less is known about brain effects from moderate alcohol use. Previous findings indicate that patients with severe mental illness, particularly schizophrenia, are vulnerable to alcohol-related brain damage. We investigated the association between levels of alcohol consumption and cortical and subcortical brain structures in schizophrenia and bipolar disorder patients and healthy controls, and investigated for group differences for this association.
Method1.5 T structural magnetic resonance images were acquired of 609 alcohol-using participants (165 schizophrenia patients, 172 bipolar disorder patients, 272 healthy controls), mean (s.d.) age 34.2 (9.9) years, 52% men. Past year alcohol use was assessed with the Alcohol Use Disorder Identification Test – Consumption part (AUDIT-C). General linear models were used to investigate associations between AUDIT-C score and cortical thickness, surface area, and total brain and subcortical volumes.
ResultsIncreasing AUDIT-C score was linearly associated with thinner cortex in medial and dorsolateral frontal and parieto-occipital regions, and with larger left lateral ventricle volume. There was no significant interaction between AUDIT-C score and diagnostic group. The findings remained significant after controlling for substance use disorders, antipsychotic medication and illness severity.
ConclusionThe results show a dose-dependent relationship between alcohol use and thinner cortex and ventricular expansion. The findings are present also at lower levels of alcohol consumption and do not differ between schizophrenia or bipolar disorder patients compared to healthy controls. Our results do not support previous findings of increased vulnerability for alcohol-related brain damage in severe mental illness.
Increased MRI-based cortical grey/white-matter contrast in sensory and motor regions in schizophrenia and bipolar disorder
- K. N. Jørgensen, S. Nerland, L. B. Norbom, N. T. Doan, R. Nesvåg, L. Mørch-Johnsen, U. K. Haukvik, I. Melle, O. A. Andreassen, L. T. Westlye, I. Agartz
-
- Journal:
- Psychological Medicine / Volume 46 / Issue 9 / July 2016
- Published online by Cambridge University Press:
- 06 April 2016, pp. 1971-1985
-
- Article
- Export citation
-
Background
Schizophrenia and bipolar disorder share genetic risk factors and one possible illness mechanism is abnormal myelination. T1-weighted magnetic resonance imaging (MRI) tissue intensities are sensitive to myelin content. Therefore, the contrast between grey- and white-matter intensities may reflect myelination along the cortical surface.
MethodMRI images were obtained from patients with schizophrenia (n = 214), bipolar disorder (n = 185), and healthy controls (n = 278) and processed in FreeSurfer. The grey/white-matter contrast was computed at each vertex as the difference between average grey-matter intensity (sampled 0–60% into the cortical ribbon) and average white-matter intensity (sampled 0–1.5 mm into subcortical white matter), normalized by their average. Group differences were tested using linear models covarying for age and sex.
ResultsPatients with schizophrenia had increased contrast compared to controls bilaterally in the post- and precentral gyri, the transverse temporal gyri and posterior insulae, and in parieto-occipital regions. In bipolar disorder, increased contrast was primarily localized in the left precentral gyrus. There were no significant differences between schizophrenia and bipolar disorder. Findings of increased contrast remained after adjusting for cortical area, thickness, and gyrification. We found no association with antipsychotic medication dose.
ConclusionsIncreased contrast was found in highly myelinated low-level sensory and motor regions in schizophrenia, and to a lesser extent in bipolar disorder. We propose that these findings indicate reduced intracortical myelin. In accordance with the corollary discharge hypothesis, this could cause disinhibition of sensory input, resulting in distorted perceptual processing leading to the characteristic positive symptoms of schizophrenia.




