2 results
Congruence between International Classification of Disease, Tenth Revision (ICD-10) code and written documentation for outpatient encounters with antibiotic prescriptions
- Charles Oertli, Milner Owens Staub, Sophie Katz
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, p. s39
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Antimicrobial stewardship programs (ASPs) often rely on International Classification of Diseases, Tenth Revision (ICD-10) codes to assess antibiotic appropriateness for provider feedback. Concordance between encounter ICD-10 codes and documented indication for antibiotics based on manual chart review varies greatly (74%–95%) in the inpatient setting. Data on concordance between documented indication and ICD-10 code in the outpatient setting are scarce. Methods: We conducted a retrospective cohort study of 650 randomly selected outpatient encounters with antibiotic prescriptions from walk-in and retail clinics between July 15 and September 15, 2021, at Vanderbilt University Medical Center. We performed chart review to compare documented antibiotic indication to the 3 most frequent encounter-associated ICD-10 codes. Also, 12 encounters were excluded due to insufficient available written documentation. The 95% CI for proportion of encounters with concordant antibiotic indications was calculated using Stata version 15.1 software. Results: Of the 638 antibiotic prescriptions with written documentation available for chart review, 204 (32%) were for amoxicillin, 102 (16%) were for amoxicillin-clavulanate, 61 (10%) were for cefdinir, and 56 (9%) were for azithromycin. Overall, 540 (84.6%; 95% CI, 81.6%–87.4%) of 638 encounters had concordant antibiotic indication based on documentation in the note and associated ICD-10 for the encounter. Of the 540 encounters with concordant ICD-10 and documented indications, 348 (64%), 130 (24%), and 35 (6%) were listed as the first, second, and third ICD-10 codes, respectively. An additional 27 (5%) had a concordant ICD-10 code listed beyond the third position. In total, 125 (19.6%) of 638 encounters did not have the intended antibiotic indication as documented in the note in the 3 most frequent encounter-associated ICD-10 codes (whether a lower position or incongruent ICD-10 code with documentation). Of those 125 encounters, 42 (34%) had a documented diagnosis of strep pharyngitis, 16 (13%) had a documented diagnosis of skin or soft-tissue infection, 11 (9%) had a documented diagnosis of urinary tract infection, and 11 (9%) had a documented diagnosis of acute otitis media. Conclusions: Our data suggest that outpatient antimicrobial prescriptions correlate relatively well with encounter ICD-10 codes. However, most ASP prescribing goals aim to reduce inappropriate prescribing to 10% or fewer of prescriptions based on indication. Therefore, providers may not trust individual prescribing feedback that is based on data that is only correct 85% of the time. For ASPs to accurately assess prescribing and provide trusted, meaningful recommendations and specific feedback to individual prescribers, more reliable and valid data are needed. We intend to evaluate whether requiring outpatient antibiotic indications on prescriptions increases data reliability and validity.
Disclosures: None
Veteran Satisfaction for Upper Respiratory-Tract Infection (URI) Visits Is Not Associated with Antibiotic Receipt But Is Associated with Antibiotic Expectation
- Milner Owens Staub, Rachael Pellegrino, Morgan Johnson, Erin Gettler, Christianne Roumie, Robert Dittus, Todd Hulgan
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue S1 / July 2021
- Published online by Cambridge University Press:
- 29 July 2021, p. s33
-
- Article
-
- You have access Access
- Open access
- Export citation
-
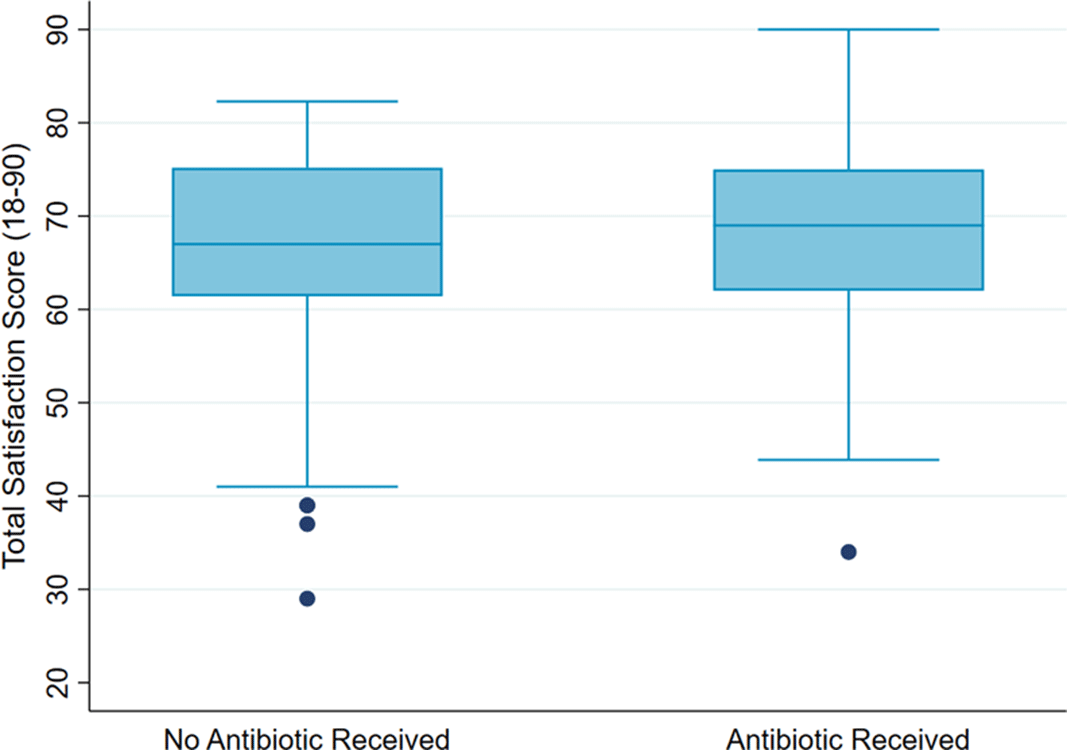
Background: Antibiotics are not recommended but are often prescribed for upper respiratory-tract infections (URIs). Prescribers cite patient expectation as a driver of inappropriate antibiotic prescribing; prior literature has demonstrated higher satisfaction scores in patients who receive antibiotics compared to those who do not. We assessed whether veteran satisfaction at URI visits was associated with antibiotic receipt or with reported expectation for antibiotics. Methods: We surveyed veterans with documented URI encounters in the Veterans’ Affairs Tennessee Valley Healthcare System between January 1, 2018, and December 31, 2019. Patients not evaluated in person, with documented dementia, or who died prior to the study start date were excluded. Veterans were asked to recall their URI visit and to complete the Patient Safety Questionnaire (PSQ)-18 (Rand Corporation) and questions assessing antibiotic expectations. The PSQ-18, an 18-item survey that assesses patient satisfaction, uses a 5-point Likert scale (ie, strongly disagree, disagree, uncertain, agree, strongly agree), yielding a composite score of 18–90. Higher scores represent more satisfaction with care. Demographic and visit-specific information were extracted via chart review. We used multivariable linear regression to assess differences in composite PSQ-18 satisfaction scores between those who did and did not receive an antibiotic, adjusted for patient and visit characteristics, and to assess differences in satisfaction scores for those who did and did not report expecting antibiotics, adjusted for antibiotic receipt. Results: We identified 1,435 patients seen for URI at 17 sites. After exclusions, 1,343 veterans were eligible for chart abstraction. After excluding 42 responders who responded after study close or returned blank surveys, the final analytic cohort included 432 (32.2%) of 1,343 responders; 225 (52.1%) received an antibiotic and 207 (47.9%) did not. Mean total satisfaction for veterans who received an antibiotic was 67.8 (SD, ±9.4) compared to 66.7 (SD, ±9.7) for those who did not (Figure 1). Increased total satisfaction was not significantly associated with antibiotic receipt (0.65; 95% CI, −2.0 to 3.3). Most veterans (72.0%) disagreed that visit satisfaction depended on antibiotic receipt. However, only 30.8% reported that they would not expect an antibiotic for URI visits. A significant reduction in total satisfaction (−4.1; 95% CI, −6.3 to −1.9) was associated with expecting compared to not expecting an antibiotic. Conclusions: Our findings suggest that prescribing an antibiotic is not associated with increased veteran satisfaction for URI visits but is associated with expecting an antibiotic. Future work will evaluate methods to change veteran antibiotic expectations.
Funding: No
Disclosures: None
Figure 1.