8 results
338 Diffusion Basis Spectrum Imaging (DBSI) Prognosticates Outcomes for Cervical Spondylotic Myelopathy after Surgery
- Justin Zhang, Saad Javeed, Jacob K. Greenberg, Dinal Jayasekera, Christopher F. Dibble, Jacob Blum, Rachel Jakes, Peng Sun, Sheng-Kwei Song, Wilson Z. Ray
-
- Journal:
- Journal of Clinical and Translational Science / Volume 6 / Issue s1 / April 2022
- Published online by Cambridge University Press:
- 19 April 2022, p. 62
-
- Article
-
- You have access Access
- Open access
- Export citation
-
OBJECTIVES/GOALS: Diffusion basis spectrum imaging (DBSI) allows for detailed evaluation of white matter microstructural changes present in cervical spondylotic myelopathy (CSM). Our goal is to utilize multidimensional clinical and quantitative imaging data to characterize disease severity and predict long-term outcomes in CSM patients undergoing surgery. METHODS/STUDY POPULATION: A single-center prospective cohort study enrolled fifty CSM patients who underwent surgical decompression and twenty healthy controls from 2018-2021. All patients underwent diffusion tensor imaging (DTI), DBSI, and complete clinical evaluations at baseline and 2-years follow-up. Primary outcome measures were the modified Japanese Orthopedic Association score (mild [mJOA 15-17], moderate [mJOA 12-14], severe [mJOA 0-11]) and SF-36 Physical and Mental Component Summaries (PCS and MCS). At 2-years follow-up, improvement was assessed via established MCID thresholds. A supervised machine learning classification model was used to predict treatment outcomes. The highest-performing algorithm was a linear support vector machine. Leave-one-out cross-validation was utilized to test model performance. RESULTS/ANTICIPATED RESULTS: A total of 70 patients – 20 controls, 25 mild, and 25 moderate/severe CSM patients – were enrolled. Baseline clinical and DTI/DBSI measures were significantly different between groups. DBSI Axial and Radial Diffusivity were significantly correlated with baseline mJOA and mJOA recovery, respectively (r=-0.33, p<0.01; r=-0.36, p=0.02). When predicting baseline disease severity (mJOA classification), DTI metrics alone performed with 38.7% accuracy (AUC: 72.2), compared to 95.2% accuracy (AUC: 98.9) with DBSI metrics alone. When predicting improvement after surgery (change in mJOA), clinical variables alone performed with 33.3% accuracy (AUC: 0.40). When combining DTI or DBSI parameters with key clinical covariates, model accuracy improved to 66.7% (AUC: 0.65) and 88.1% (AUC: 0.95) accuracy, respectively. DISCUSSION/SIGNIFICANCE: DBSI metrics correlate with baseline disease severity and outcome measures at 2-years follow-up. Our results suggest that DBSI may serve as a valid non-invasive imaging biomarker for CSM disease severity and potential for postoperative improvement.
Association of Antibiotic Duration and Outcomes among NICU Infants with Invasive Staphylococcus aureus Infections
- Areej Bukhari, Ibukunoluwa Akinboyo, Kanecia Zimmerman, Danny Benjamin, Veeral Tolia, Rachel Greenberg
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue S1 / July 2021
- Published online by Cambridge University Press:
- 29 July 2021, pp. s27-s28
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background:Staphylococcus aureus is the second-leading cause of late-onset sepsis among infants in US neonatal intensive care units (NICUs). Management of S. aureus bacteremia and meningitis in infants varies widely due to the lack of standardized guidelines. We examined the association between initial antibiotic duration and recurrent S. aureus infection or death among NICU infants with S. aureus bacteremia and/or meningitis. Methods: We conducted a retrospective cohort study of infants in Pediatrix Medical Group NICUs from 1997 to 2018 with first episode of S. aureus bacteremia and/or meningitis, identified as having at least 1 blood or cerebrospinal fluid (CSF) culture growing only S. aureus at any point during their NICU stay. Excluded infants were those not started on antistaphylococcal therapy within 2 days of positive culture, those with had endocarditis or osteomyelitis, or those who died or were discharged during or up to 1 day after antibiotic cessation. Antibiotic cessation was defined as last day of antibiotic given if followed by at least 3 days without antibiotics. Multivariable logistic regression was used to analyze the association between antibiotic duration categorized as <14 or ≥14 days) and recurrent SA infection (within 12 weeks of antibiotic cessation, prior to hospital discharge), or death (within 7 days of antibiotic cessation and at discharge). Results: Of 4,086 infants included, 3,991 (98%) had S. aureus bacteremia only and 95 (2%) had meningitis ± bacteremia. Of those with bacteremia only, 2,017 (50.5%), and 17 (18%) of those with meningitis received <14 days antibiotics (Figure 1). Longer antibiotic duration was associated with lower gestational age, methicillin-resistance, severe illness and bacteremia duration of ≥4 days (Table 1). There was a significant association between <14 days antibiotics and recurrent infection (p = 0.04) and 7-day mortality (p = 0.02) in the meningitis cohort. Infants with SA bacteremia who received ≥14 days antibiotics had reduced odds of recurrent SA infection (OR 0.24, 95% CI 0.18-0.32) and death (OR 0.33, 95% CI 0.25-0.44), adjusting for post-natal age, gestational age, sex, methicillin-resistance, severe illness and duration of bacteremia (Table 2). Conclusions: In the largest study thus far examining antibiotic duration among hospitalized infants with S. aureus bacteremia and/or meningitis, ≥14 days antibiotics was associated with decreased odds of recurrent infection or death. Further studies are needed to define the optimal treatment duration and identify clinical factors distinguishing infants able to safely receive a shorter antibiotic duration.
Funding: No
Disclosures: None
Figure 1.
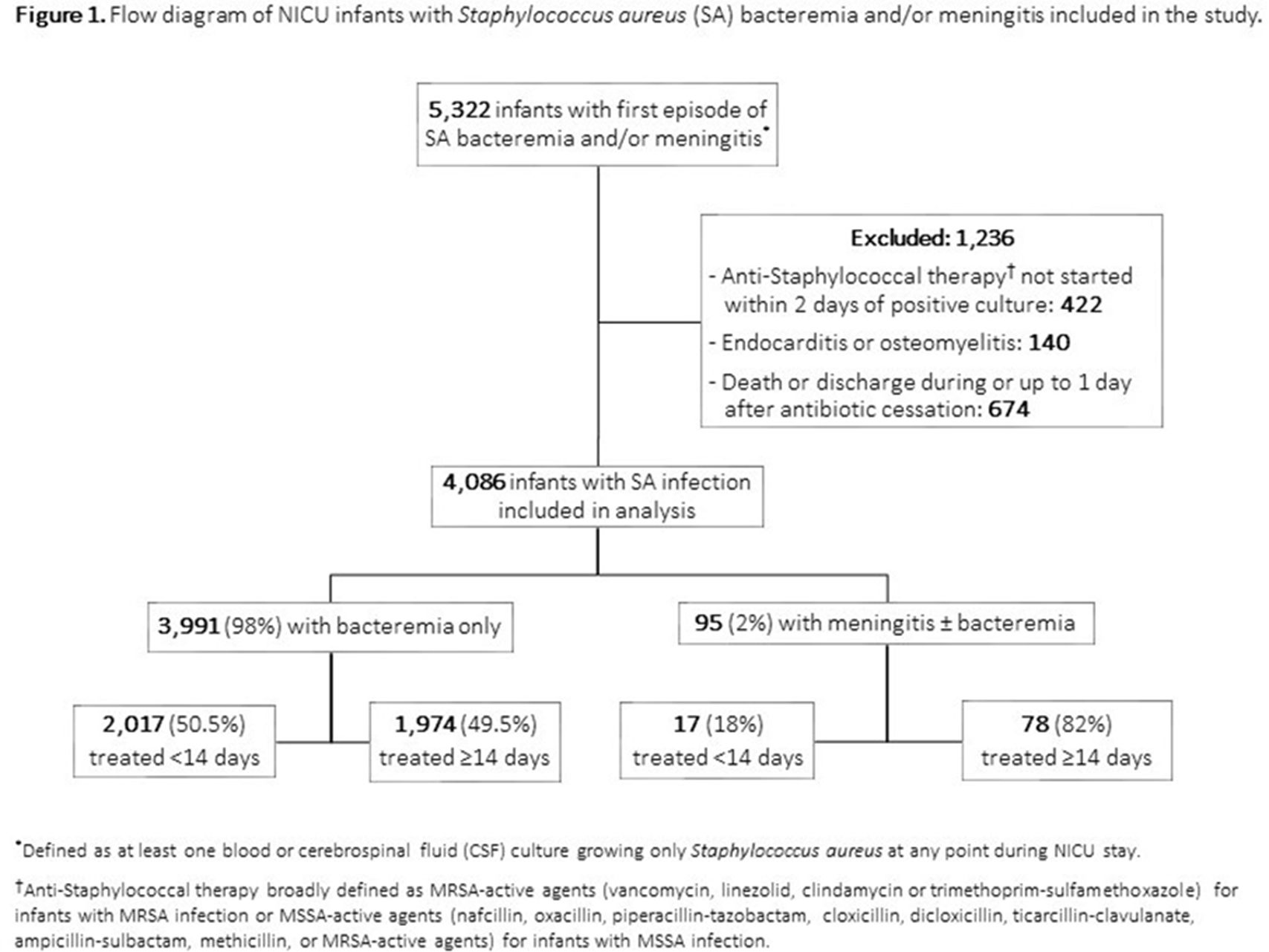
Table 1. 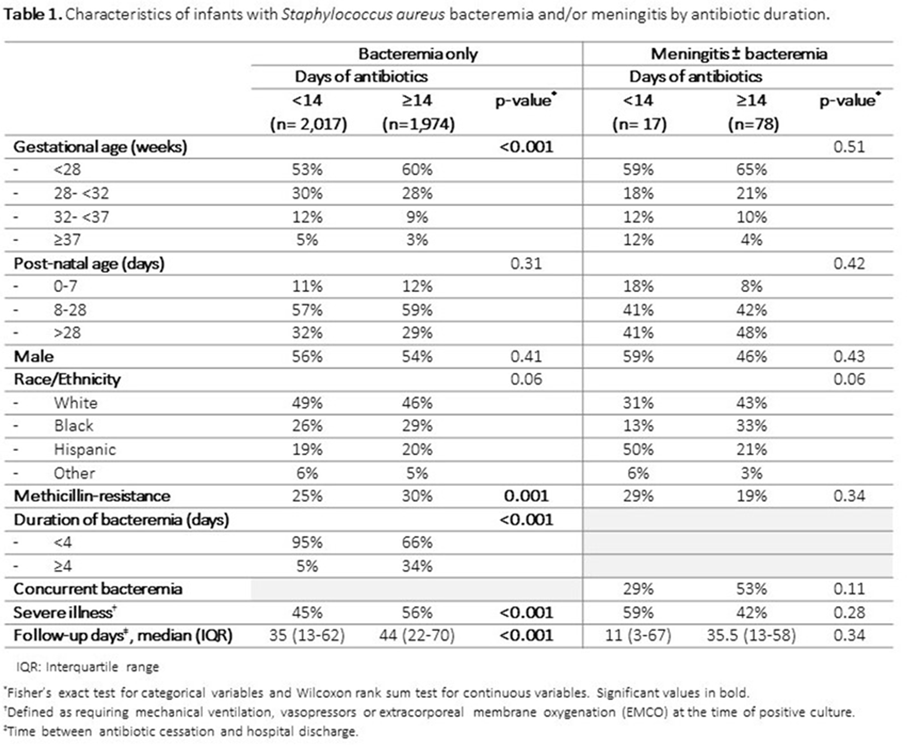
Table 2. 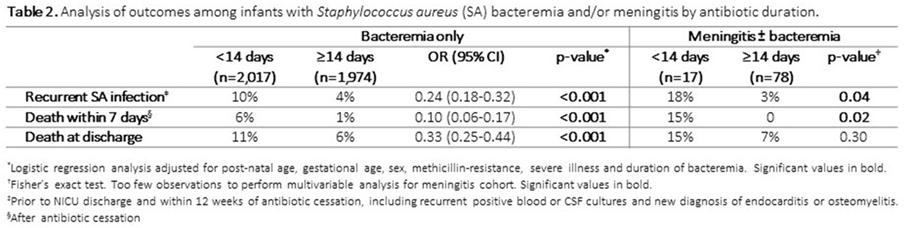
Response of the trial innovation network to the COVID-19 pandemic
- Rachel G. Greenberg, Lori Poole, Daniel E. Ford, Daniel Hanley, Harry P. Selker, Karen Lane, J. Michael Dean, Jeri Burr, Paul Harris, Consuelo H. Wilkins, Gordon Bernard, Terri Edwards, Daniel K. Benjamin, Jr
-
- Journal:
- Journal of Clinical and Translational Science / Volume 5 / Issue 1 / 2021
- Published online by Cambridge University Press:
- 20 April 2021, e100
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Introduction:
The COVID-19 pandemic prompted the development and implementation of hundreds of clinical trials across the USA. The Trial Innovation Network (TIN), funded by the National Center for Advancing Translational Sciences, was an established clinical research network that pivoted to respond to the pandemic.
Methods:The TIN’s three Trial Innovation Centers, Recruitment Innovation Center, and 66 Clinical and Translational Science Award Hub institutions, collaborated to adapt to the pandemic’s rapidly changing landscape, playing central roles in the planning and execution of pivotal studies addressing COVID-19. Our objective was to summarize the results of these collaborations and lessons learned.
Results:The TIN provided 29 COVID-related consults between March 2020 and December 2020, including 6 trial participation expressions of interest and 8 community engagement studios from the Recruitment Innovation Center. Key lessons learned from these experiences include the benefits of leveraging an established infrastructure, innovations surrounding remote research activities, data harmonization and central safety reviews, and early community engagement and involvement.
Conclusions:Our experience highlighted the benefits and challenges of a multi-institutional approach to clinical research during a pandemic.
Association between early echocardiography, therapy for patent ductus arteriosus, and outcomes in very low birth weight infants
- Jan Hau Lee, Rachel G. Greenberg, Bin H. Quek, Reese H. Clark, Matthew M. Laughon, P. Brian Smith, Christoph P. Hornik
-
- Journal:
- Cardiology in the Young / Volume 27 / Issue 9 / November 2017
- Published online by Cambridge University Press:
- 19 June 2017, pp. 1732-1739
-
- Article
- Export citation
-
Background
In very low birth weight infants, persistence of a patent ductus arteriosus results in morbidity and mortality. Therapies to close the ductus are effective, but clinical outcomes may depend on the accuracy of diagnosis and the timing of administration. The objective of the present study was to characterise the association between early echocardiography, therapy for patent ductus arteriosus, and outcomes in very low birth weight infants.
MethodsThis retrospective cohort study used electronic health record data on inborn infants of gestational age ⩽28 weeks and birth weight <1500 g who were discharged after day of life 7 from 362 neonatal ICU from 1997 to 2013. The primary outcome was death between day of life 7 and discharge. Secondary outcomes included bronchopulmonary dysplasia, necrotising enterocolitis, and grade 3 or 4 intraventricular haemorrhage.
ResultsThis study included a total of 48,551 infants with a median gestational age of 27 weeks (interquartile range 25, 28) and birth weight 870 g (706, 1050). Early echocardiography – that is, performed during days of life 2 to 6 – was performed in 15,971/48,551 (33%) infants, and patent ductus arteriosus was diagnosed in 31,712/48,551 (65%). The diagnosis was more common in infants who had undergone early echocardiography (14,549/15,971 [91%] versus 17,163/32,580 [53%], p<0.001). In multivariable analysis, early echocardiography was not associated with reduced mortality (odds ratio 0.97, 95% CI 0.89–1.05). Results were similar in the subset of infants who received therapy for patent ductus arteriosus (odds ratio 1.01, 95% CI 0.90–1.15).
ConclusionsEarly echocardiography was associated with an increased diagnosis of patent ductus arteriosus, but not with decreased mortality.
Antihypertensive drug exposure in premature infants from 1997 to 2013
- Srikanth Ravisankar, Devon Kuehn, Reese H. Clark, Rachel G. Greenberg, P. Brian Smith, Christoph P. Hornik
-
- Journal:
- Cardiology in the Young / Volume 27 / Issue 5 / July 2017
- Published online by Cambridge University Press:
- 17 October 2016, pp. 905-911
-
- Article
- Export citation
-
Background
Systemic hypertension is increasingly recognised in premature infants. There is limited evidence regarding treatment, and most published treatment recommendations are based solely on expert opinions.
MethodsWe identified all infants born ⩽32 weeks of gestation and ⩽1500 g birth weight discharged from one of 348 neonatal ICUs managed by the Pediatrix Medical Group between 1997 and 2013. We defined antihypertensive drugs as vasodilators, angiotensin-converting enzyme inhibitors, β receptor blockers, calcium channel blockers, and central α2 receptor agonists. We compared characteristics between infants who were treated with at least one antihypertensive drug during their initial hospitalisation and infants who were not prescribed antihypertensive drugs using Wilcoxon’s ranked sum test or Pearson’s χ2-test.
ResultsWe identified 2504/119,360 (2.1%) infants who required at least one antihypertensive drug. The median postnatal age of first exposure was 48 days (25th, 75th percentile 15, 86), and the median length of therapy was 6 days (1, 16). Hydralazine was the most commonly prescribed antihypertensive with 1280/2504 (51.1%) treated infants exposed to the drug. More than two antihypertensive drugs were administered in 582/2504 (23.2%) infants, and 199/2097 (9.5%) of the treated infants were discharged home on antihypertensive therapy. Infants who received antihypertensive drugs were of lower gestational age (p<0.001) and birth weight (p<0.001) compared with infants not prescribed antihypertensive drugs.
ConclusionsOur study is the largest to describe current antihypertensive drug exposure in a cohort of exclusively premature infants born ⩽32 weeks of gestation. We found wide variations in practice for treating hypertension in premature infants.
Use of vitamin D supplements during infancy in an international feeding trial
- Eveliina Lehtonen, Anne Ormisson, Anita Nucci, David Cuthbertson, Susa Sorkio, Mila Hyytinen, Kirsi Alahuhta, Carol Berseth, Marja Salonen, Shayne Taback, Margaret Franciscus, Teba González-Frutos, Tuuli E Korhonen, Margaret L Lawson, Dorothy J Becker, Jeffrey P Krischer, Mikael Knip, Suvi M Virtanen, , Thomas Mandrup-Poulsen, Elias Arjas, Åke Lernmark, Barbara Schmidt, Jeffrey P. Krischer, Hans K. Åkerblom, Mila Hyytinen, Mikael Knip, Katriina Koski, Matti Koski, Eeva Pajakkala, Marja Salonen, David Cuthbertson, Jeffrey P. Krischer, Linda Shanker, Brenda Bradley, Hans-Michael Dosch, John Dupré, William Fraser, Margaret Lawson, Jeffrey L. Mahon, Mathew Sermer, Shayne P. Taback, Dorothy Becker, Margaret Franciscus, Anita Nucci, Jerry Palmer, Minna Pekkala, Suvi M. Virtanen, Jacki Catteau, Neville Howard, Patricia Crock, Maria Craig, Cheril L. Clarson, Lynda Bere, David Thompson, Daniel Metzger, Colleen Marshall, Jennifer Kwan, David K. Stephure, Daniele Pacaud, Wendy Schwarz, Rose Girgis, Marilyn Thompson, Shayne P. Taback, Daniel Catte, Margaret L. Lawson, Brenda Bradley, Denis Daneman, Mathew Sermer, Mary-Jean Martin, Valérie Morin, Lyne Frenette, Suzanne Ferland, Susan Sanderson, Kathy Heath, Céline Huot, Monique Gonthier, Maryse Thibeault, Laurent Legault, Diane Laforte, Elizabeth A. Cummings, Karen Scott, Tracey Bridger, Cheryl Crummell, Robyn Houlden, Adriana Breen, George Carson, Sheila Kelly, Koravangattu Sankaran, Marie Penner, Richard A. White, Nancy King, James Popkin, Laurie Robson, Eva Al Taji, Irena Aldhoon, Pavla Mendlova, Jan Vavrinec, Jan Vosahlo, Ludmila Brazdova, Jitrenka Venhacova, Petra Venhacova, Adam Cipra, Zdenka Tomsikova, Petra Krckova, Pavla Gogelova, Ülle Einberg, Mall-Anne Riikjärv, Anne Ormisson, Vallo Tillmann, Päivi Kleemola, Anna Parkkola, Heli Suomalainen, Anna-Liisa Järvenpää, Anu-Maaria Hämälainen, Hannu Haavisto, Sirpa Tenhola, Pentti Lautala, Pia Salonen, Susanna Aspholm, Heli Siljander, Carita Holm, Samuli Ylitalo, Raisa Lounamaa, Anja Nuuja, Timo Talvitie, Kaija Lindström, Hanna Huopio, Jouni Pesola, Riitta Veijola, Päivi Tapanainen, Abram Alar, Paavo Korpela, Marja-Liisa Käär, Taina Mustila, Ritva Virransalo, Päivi Nykänen, Bärbel Aschemeier, Thomas Danne, Olga Kordonouri, Dóra Krikovszky, László Madácsy, Yeganeh Manon Khazrai, Ernesto Maddaloni, Paolo Pozzilli, Carla Mannu, Marco Songini, Carine de Beaufort, Ulrike Schierloh, Jan Bruining, Margriet Bisschoff, Aleksander Basiak, Renata Wasikowa, Marta Ciechanowska, Grazyna Deja, Przemyslawa Jarosz-Chobot, Agnieszka Szadkowska, Katarzyna Cypryk, Malgorzata Zawodniak-Szalapska, Luis Castano, Teba Gonzalez Frutos, Mirentxu Oyarzabal, Manuel Serrano-Ríos, María Teresa Martínez-Larrad, Federico Gustavo Hawkins, Dolores Rodriguez Arnau, Johnny Ludvigsson, Malgorzata Smolinska Konefal, Ragnar Hanas, Bengt Lindblad, Nils-Osten Nilsson, Hans Fors, Maria Nordwall, Agne Lindh, Hans Edenwall, Jan Aman, Calle Johansson, Margrit Gadient, Eugen Schoenle, Dorothy Becker, Ashi Daftary, Margaret Franciscus, Carol Gilmour, Jerry Palmer, Rachel Taculad, Marilyn Tanner-Blasiar, Neil White, Uday Devaskar, Heather Horowitz, Lisa Rogers, Roxana Colon, Teresa Frazer, Jose Torres, Robin Goland, Ellen Greenberg, Maudene Nelson, Holly Schachner, Barney Softness, Jorma Ilonen, Massimo Trucco, Lynn Nichol, Erkki Savilahti, Taina Härkönen, Mikael Knip, Outi Vaarala, Kristiina Luopajärvi, Hans-Michael Dosch
-
- Journal:
- Public Health Nutrition / Volume 17 / Issue 4 / April 2014
- Published online by Cambridge University Press:
- 24 June 2013, pp. 810-822
-
- Article
-
- You have access Access
- HTML
- Export citation
-
Objective
To examine the use of vitamin D supplements during infancy among the participants in an international infant feeding trial.
DesignLongitudinal study.
SettingInformation about vitamin D supplementation was collected through a validated FFQ at the age of 2 weeks and monthly between the ages of 1 month and 6 months.
SubjectsInfants (n 2159) with a biological family member affected by type 1 diabetes and with increased human leucocyte antigen-conferred susceptibility to type 1 diabetes from twelve European countries, the USA, Canada and Australia.
ResultsDaily use of vitamin D supplements was common during the first 6 months of life in Northern and Central Europe (>80 % of the infants), with somewhat lower rates observed in Southern Europe (>60 %). In Canada, vitamin D supplementation was more common among exclusively breast-fed than other infants (e.g. 71 % v. 44 % at 6 months of age). Less than 2 % of infants in the USA and Australia received any vitamin D supplementation. Higher gestational age, older maternal age and longer maternal education were study-wide associated with greater use of vitamin D supplements.
ConclusionsMost of the infants received vitamin D supplements during the first 6 months of life in the European countries, whereas in Canada only half and in the USA and Australia very few were given supplementation.
Laurie Ellinghausen. Labor and Writing in Early Modern England, 1567–1667. Aldershot, and Burlington, VT: Ashgate, 2008. Pp. 166. $99.95 (cloth).
- Rachel Greenberg
-
- Journal:
- Journal of British Studies / Volume 49 / Issue 3 / July 2010
- Published online by Cambridge University Press:
- 21 December 2012, pp. 690-691
- Print publication:
- July 2010
-
- Article
- Export citation
Contributors
-
- By Jennifer Alvarez, Ananda B. Amstadter, Metin Başoğlu, David M. Benedek, Charles C. Benight, George A. Bonanno, Evelyn J. Bromet, Richard A. Bryant, Barbara Lopes Cardozo, M. L. Somchai Chakkraband, Claude Chemtob, Roman Cieslak, Lauren M. Conoscenti, Joan M. Cook, Judith Cukor, Carla Kmett Danielson, JoAnn Difede, Charles DiMaggio, Anja J.E. Dirkzwager, Cristiane S. Duarte, Jon D. Elhai, Diane L. Elmore, Yael L.E. Errera, Julian D. Ford, Carol S. Fullerton, Sandro Galea, Freya Goodhew, Neil Greenberg, Lindsay Greene, Linda Grievink, Michael J. Gruber, Sumati Gupta, Johan M. Havenaar, Alesia O. Hawkins, Clare Henn-Haase, Kimberly Eaton Hoagwood, Christina W. Hoven, Sabra S. Inslicht, Krzysztof Kaniasty, Ronald C. Kessler, Rachel Kimerling, Richard V. King, Rolf J. Kleber, Jessica Mass Levitt, Brett T. Litz, Maria Livanou, Katelyn P. Mack, Paula Madrid, Shira Maguen, Paul Maguire, Donald J. Mandell, Charles R. Marmar, Andrea R. Maxwell, Shannon E. McCaslin, Alexander C. McFarlane, Thomas J. Metzler, Summer Nelson, Yuval Neria, Elana Newman, Thomas C. Neylan, Fran H. Norris, Carol S. North, Lawrence A. Palinkas, Benjaporn Panyayong, Maria Petukhova, Betty Pfefferbaum, Marleen Radigan, Beverley Raphael, James Rodriguez, G. James Rubin, Kenneth J. Ruggiero, Ebru Şalcıoğlu, Nancy A. Sampson, Arieh Y. Shalev, Bruce Shapiro, Laura M. Stough, Prawate Tantipiwatanaskul, Warunee Thienkrua, Phebe Tucker, J. Blake Turner, Robert J. Ursano, Bellis van den Berg, Peter G. van der Velden, Frits van Griensven, Miranda Van Hooff, Edward Waldrep, Philip S. Wang, Simon Wessely, Leslie H. Wind, C. Joris Yzermans, Heidi M. Zinzow
- Edited by Yuval Neria, Columbia University, New York, Sandro Galea, University of Michigan, Ann Arbor, Fran H. Norris
-
- Book:
- Mental Health and Disasters
- Published online:
- 07 May 2010
- Print publication:
- 20 July 2009, pp xi-xvi
-
- Chapter
- Export citation






