32 results
Substance use amongst adult patients admitted to an irish acute mental health unit
- A. Duggan, N. Murray, S. Buckley, G. Lalevic
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S566
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Comorbid substance misuse in mental illness presents a significant challenge to mental health services. It may lead to higher rates of relapse, hospital admissions and poorer treatment outcomes. Up to 47% of inpatients in Irish mental health units may experience substance misuse. Despite the Irish government’s ‘Vision for Change’ policy (2006), access to specialised services remains variable.
ObjectivesEvaluate: -prevalence of substance misuse at an Irish mental health unit. -quality and detail of the recorded substance misuse history. -access to specialised services for patients experiencing substance misuse.
MethodsA retrospective chart review of inpatients in a mental health unit over 12 months, was completed. Information recorded included: demographic details, diagnosis, substance use history; access to substance misuse services. Microsoft Excel was utilised for data input and analysis.
Results267 patients were admitted over twelve months. Substance misuse was the primary diagnosis of 6% and the secondary diagnosis of 67%. 46% of patients reported current substance misuse, 52% reported historical substance misuse. Frequency and quantity of use was documented in 65% and 48% of cases respectively. 4% of patients with a substance misuse history were in current contact with addiction services.
ConclusionsAlthough 46% of patients reported substance misuse, only 4% were in contact with specialised addiction services. This highlights a significant unmet need. There was variability in the quality of the recorded substance misuse history. In order to fully understand comorbid substance misuse, this be addressed. The addition of a more formatted substance misuse section, to admission proformas, may help to alleviate this issue.
S08-01 - Cochrane Reviews of Pharmacological and Psychological Interventions for Antisocial Personality Disorder (ASPD)
- B. Vollm, S. Gibbon, N. Khalifa, C. Duggan, J. Stoffers, N. Huband, M. Ferriter, K. Lieb
-
- Journal:
- European Psychiatry / Volume 25 / Issue S1 / 2010
- Published online by Cambridge University Press:
- 17 April 2020, 25-E90
-
- Article
-
- You have access Access
- Export citation
-
Introduction
ASPD has a prevalence of 2-3% in the general population but rates in prison have been reported as 50% to 75%. ASPD is associated with significant psychiatric and medical comorbidity, high offending rates, poor psychosocial adaptation and premature death. Outcomes are poor. There is little consensus regarding the most effective intervention for the condition.
Aims and objectivesTo conduct systematic literature reviews to identify randomised controlled trials for either pharmacological or psychological interventions for ASPD.
MethodsSystematic literature reviews (Cochrane reviews).
ResultsFor the review on psychological interventions only 11 studies could be included with a total of 411 participants, but only five reported data separately for the subgroup of ASPD. Nine of the studies looked at participants with substance misuse problems who also suffered from ASPD. Only three types of interventions were effective (contingency management, CBT and a specific programme for those convicted for driving whilst intoxicated). These interventions showed positive results for substance misuse related outcomes but not for any others behaviours or symptoms. For the pharmacological review 10 studies were identified, anticonvulsants were the most commonly used drugs with some evidence of effectiveness on aggression, however, study quality was poor.
ConclusionsDespite the considerable personal and societal consequences of ASPD, very little research is carried out with regards to interventions in this patient group and subsequently the evidence base to support any interventions is extremely limited.
Pharmacotherapy in patients with cluster a personality disorders
- B.A. Völlm, S. Farooq, M. Ferriter, H. Jones, N. Smailagic, N. Khalifa, N. Huband, S. Gibbon, J. Stoffers, C. Duggan, K. Lieb
-
- Journal:
- European Psychiatry / Volume 26 / Issue S2 / March 2011
- Published online by Cambridge University Press:
- 16 April 2020, p. 2107
-
- Article
-
- You have access Access
- Export citation
-
Background
Among the 10 categories of personality disorders (PDs), interventions for antisocial and borderline personality disorder are best studied. However, the remaining PDs also pose major problems in everyday health care settings. People affected often additionally present with Axis-I disorders such as substance-related, mood or anxiety disorders, and are among those most difficult to treat. Cluster A PDs (paranoid, schizoid, schizotypal) are of particular significance as some authors argue that they may be part of a continuum of mental disorders and be considered as sub-syndrome of schizophrenia
MethodsIn the context of Cochrane Collaboration reviews for Cluster A, B and C PDs, exhaustive literature searches were completed to identify the current RCT evidence for PD treatments. Retrievals were assessed and evaluated by two reviewers independently and trials for Cluster A PD were identified.
ResultsOnly very few (under five) RCTs specifically for Cluster A PDs were identified. Some studies reported on mixed PD samples but it was not always possible to extract data specifically for Cluster A disorders. Participants mostly also suffered from Axis-I disorders. Reported outcomes also focus on Axis-I disorder outcomes or general measures such as overall functioning rather than specific PD symptoms.
ConclusionsThe current evidence for psychpathological treatment of Cluster A PD is sparse and does not allow for distinct treatment recommendations. Symptom-driven treatment regimes as suggested by several guidelines are not supported by current evidence.
1659 – The Development Of a Case Formulation Training Package For Probation Staff
- S. Brown, L. Hedges, G. Patel, C. Duggan, B. Vollm
-
- Journal:
- European Psychiatry / Volume 28 / Issue S1 / 2013
- Published online by Cambridge University Press:
- 15 April 2020, 28-E936
-
- Article
-
- You have access Access
- Export citation
-
Introduction
A recent UK Government initiative has sought to address the management of personality disordered (PD) offenders, aiming to improve public protection by reducing reoffending whilst simultaneously improving the psychological health of offenders with PD. Case formulation (CF) is given primacy here as it enhances offender management through a psychologically informed approach and informs pathway planning through Criminal Justice System or NHS services. Probation services are given an important role in formulating cases as part of the new strategy.
ObjectivesDevelop a consensus amongst professionals as to what makes a good Case Formulation (CF). Investigate whether probation services can be taught CF skills, and to enhance these skills.
AimsDevelop a case formulation training package for probation staff and evaluate the training.
MethodThe training package was informed by the results of a Delphi survey amongst professionals, and focus groups with probation staff, offenders and carers of individuals with PD.
ResultsThere was consensus that CF allows for collaboration between client and therapist, helps with complexity through organisation of case notes and has utility in treatment planning. Themes highlighted for effective CF included background, trauma, offending, risk and current lifestyle. The theoretical model gaining most support was a CBT model. The assessment of formulations was identified as challenging.
The CF training package is currently being evaluated and findings will be presented at the conference, alongside outcomes of all phases of the research.
ConclusionsCF has the potential to enhance treatment planning. Its suitability for probation staff will be discussed.
P072: Comparing met vs. unmet palliative care needs in patients with end-stage conditions presenting to two Canadian emergency departments
- M. Garrido Clua, M. Kruhlak, S. Kirkland, C. Villa-Roel, A. Elwi, B. O'Neill, A. Brisebois, S. Duggan, B. Rowe
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 21 / Issue S1 / May 2019
- Published online by Cambridge University Press:
- 02 May 2019, p. S89
- Print publication:
- May 2019
-
- Article
-
- You have access Access
- Export citation
-
Introduction: Patients with end-stage conditions require integrated physical, spiritual, psychological and social care. Despite efforts to provide comprehensive community care, those with severe symptoms often present to emergency departments (EDs) with palliative care (PC) needs. The objective of this study was to identify patients with end-stage diagnoses presenting to EDs, and to document and compare their PC needs. Methods: A four-month prospective cohort study was conducted in two Canadian EDs. Using a modified PC screening tool, volunteer emergency physicians identified adult patients with end-stage illnesses and documented their PC needs. This tool has the ability to classify patients as having met vs. unmet PC needs based on the documentation of risk factors. Research assistants documented demographic information, severity at presentation (Canadian Triage and Acuity Scale {CTAS}), disposition and revisits from an electronic repository. Bivariate comparisons between patients with met vs. unmet PC needs were completed. Results: Overall, 663 patients were enrolled, of which 78% (n = 518/663) were identified as having unmet PC needs according to the screening tool. Cancer was the most prevalent condition in each group (43% unmet needs, 37% met needs). There was no significant difference between the two groups in terms of age, sex or CTAS score. The unmet PC needs group was more likely to be admitted (68% vs. 50%; p = 0.0001) when compared to patients with PC needs assessed as being met. No significant difference was noted in terms of time to physician assessment or ED length of stay. The two groups did not significantly differ in the proportion of return visits within 30 days (34% vs. 32%) or the average number of return visits (3 vs. 2 visits). A higher proportion of patients with unmet PC needs made at least one visit to the ED in the 6 months prior to their index visit compared to patients with met PC needs (74% vs. 51%, p < 0.001); yet, the average number of ED visits was similar between the groups (3 visits). Conclusion: This study revealed that patients with end-stage diagnoses, especially cancer, commonly have unmet PC needs. They are also more likely to present to the ED and to require hospitalization than patients in whom PC needs have been met. Further investigations into their clinical profile and health care utilization may clarify the impact of their unmet PC needs on the healthcare system.
MP08: The frequency of emergency departments visits for patients with end-of-life conditions: a call for action
- S. Kirkland, M. Kruhlak, M. Garrido Clua, C. Villa-Roel, S. Couperthwaite, A. Brisebois, A. Elwi, B. O'Neil, S. Duggan, B. Rowe
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 21 / Issue S1 / May 2019
- Published online by Cambridge University Press:
- 02 May 2019, pp. S44-S45
- Print publication:
- May 2019
-
- Article
-
- You have access Access
- Export citation
-
Introduction: An increasing number of patients with end-stage diseases present to emergency departments (EDs) for physical, spiritual, psychological and social care. The objective of this study was to identify patients with end-stage diseases with palliative care (PC) needs and document their frequency of ED visits. Methods: This prospective cohort study was conducted in two Canadian EDs. Using a modified palliative care screening tool, volunteer ED physicians were asked to identify adult patients with end-stage, chronic conditions including cancer, chronic obstructive pulmonary disease (COPD), chronic kidney disease (CKD), heart failure (HF), cirrhosis, dementia and/or progressive central nervous system (PCNS) disease. Demographic data were collected from these tools and data regarding patients’ visits in both the 6 months prior to and 30 days following their index visits were collected from the ED Information System. Bivariate analyses were completed using Student's t and chi-square test. Results: A total of 663 patients with end-stage illness were identified; 338 (51%) were female and the median age was 76 (IQR: 63, 85). Cancer was the most common presentation (41%), followed by dementia (23%), COPD (16%), HF (9%), CKD (9%), PCNS disease (9%) and cirrhosis (7%). These patients made a total of 1277 visits in the 6 months prior to and 288 in the 30 days following the index visit. Patients presenting to the EDs with cancer (p = 0.001), cirrhosis (p = 0.005) and CKD (p = 0.03) were more likely to visit an ED in the 6 months prior to their index visit. In contrast, patients presenting with dementia (p < 0.0001) and PCNS disease (p = 0.02) were significantly less likely to present to an ED in the 6 months prior to their index visit. Patients presenting with cirrhosis or CKD had the highest average number of ED visits in the 6 months prior to their index visit (cirrhosis: 4.59 visits, SD: 3.8, p < 0.0001; CKD: 4.39 visits, SD: 3.8, p = 0.0001). Of these patients, those presenting with end-stage cirrhosis were significantly more likely to make a return visit to an ED within 30 days after their index visit (p = 0.014). Conclusion: Cancer is the most common condition for patients with end-stage, chronic illnesses in these EDs. Those presenting with cirrhosis or CKD are at a significantly higher risk of repeat visits to the EDs. This study has identified potential deficits in care and can serve as a baseline for future intervention studies.
2450 Delirium and catatonia: Age matters
- Jo E. Wilson, Richard Carlson, Maria C. Duggan, Pratik Pandharipande, Timothy D. Girard, Li Wang, Jennifer L. Thompson, Rameela Chandrasekhar, Andrew Francis, Stephen E. Nicolson, Robert S. Dittus, Stephan Heckers, E. W. Ely
-
- Journal:
- Journal of Clinical and Translational Science / Volume 2 / Issue S1 / June 2018
- Published online by Cambridge University Press:
- 21 November 2018, p. 39
-
- Article
-
- You have access Access
- Open access
- Export citation
-
OBJECTIVES/SPECIFIC AIMS: Background: Delirium is a well described form of acute brain organ dysfunction characterized by decreased or increased movement, changes in attention and concentration as well as perceptual disturbances (i.e., hallucinations) and delusions. Catatonia, a neuropsychiatric syndrome traditionally described in patients with severe psychiatric illness, can present as phenotypically similar to delirium and is characterized by increased, decreased and/or abnormal movements, staring, rigidity, and mutism. Delirium and catatonia can co-occur in the setting of medical illness, but no studies have explored this relationship by age. Our objective was to assess whether advancing age and the presence of catatonia are associated with delirium. METHODS/STUDY POPULATION: Methods: We prospectively enrolled critically ill patients at a single institution who were on a ventilator or in shock and evaluated them daily for delirium using the Confusion Assessment for the ICU and for catatonia using the Bush Francis Catatonia Rating Scale. Measures of association (OR) were assessed with a simple logistic regression model with catatonia as the independent variable and delirium as the dependent variable. Effect measure modification by age was assessed using a Likelihood ratio test. RESULTS/ANTICIPATED RESULTS: Results: We enrolled 136 medical and surgical critically ill patients with 452 matched (concomitant) delirium and catatonia assessments. Median age was 59 years (IQR: 52–68). In our cohort of 136 patients, 58 patients (43%) had delirium only, 4 (3%) had catatonia only, 42 (31%) had both delirium and catatonia, and 32 (24%) had neither. Age was significantly associated with prevalent delirium (i.e., increasing age associated with decreased risk for delirium) (p=0.04) after adjusting for catatonia severity. Catatonia was significantly associated with prevalent delirium (p<0.0001) after adjusting for age. Peak delirium risk was for patients aged 55 years with 3 or more catatonic signs, who had 53.4 times the odds of delirium (95% CI: 16.06, 176.75) than those with no catatonic signs. Patients 70 years and older with 3 or more catatonia features had half this risk. DISCUSSION/SIGNIFICANCE OF IMPACT: Conclusions: Catatonia is significantly associated with prevalent delirium even after controlling for age. These data support an inverted U-shape risk of delirium after adjusting for catatonia. This relationship and its clinical ramifications need to be examined in a larger sample, including patients with dementia. Additionally, we need to assess which acute brain syndrome (delirium or catatonia) develops first.
Tlapallite, a new mineral from Moctezuma, Sonora, Mexico
- S. A. Williams, Marjorie Duggan
-
- Journal:
- Mineralogical Magazine / Volume 42 / Issue 322 / June 1978
- Published online by Cambridge University Press:
- 05 July 2018, pp. 183-186
-
- Article
- Export citation
-
Tlapallite is a new mineral found in 1972 at the Bambollita (La Oriental) mine near Moctezuma, Sonora. Also recently found in old specimens from Tombstone, Arizona. Data for type (Mexican) material: Colour viridian green RHS-128A with pale streak, H = 3, Dcalc = 5·05 g/cm3. Crystals monoclinic, class unknown. Indexing based on Ito method gave a cell: a = 11·97 Å, b = 9·11, c = 15·66, β = 90 ° 36′. Strongest lines: 11·972 Å (10), 2·985 (10), 3·540 (6), 5·946 (5), 2·887 (5), 4·731 (4), 3·372 (4), 3·282 (4). Similar data obtain for Tombstone. Chemical analysis for type material yielded the formula H6Ca2Cu3(SO4)(TeO3)4,TeO6 with Te4+:Te6+ = 4:1. However, analysis of the Tombstone material indicates a more general formula H6(Ca, Pb)2(Cu, Zn)3(SO4) (TeO3)4,TeO6. The better data from this material indicate Z = 4, Dcalc = 5·465 vs Dmeas = 5·38. Characterized by extreme birefringence, α = 1·815, β = γ = 1·960; for Tombstone α = 1·955, β = γ = 2·115.
Named from the Nahua word tlapalli, meaning paint, in allusion to its mode of occurrence at the type locality.
Ruizite, a new silicate mineral from Christmas, Arizona
- S. A. Williams, M. Duggan
-
- Journal:
- Mineralogical Magazine / Volume 41 / Issue 320 / December 1977
- Published online by Cambridge University Press:
- 05 July 2018, pp. 429-432
-
- Article
- Export citation
-
Ruizite is a new mineral found in the mesogene calc-silicate assemblage at the Christmas mine, Gila County, Arizona. Occurs with kinoite, apophyllite, smectite, and junitoite. Colour is orange inclining to brown with pale streak, H = 5, Sp. Gr. meas. = 2·9. Crystals monoclinic 2/m, elongate on [010]; a = 11·95 Å, b = 6·17, c = 9·03, β = 91° 22½′. Probable space group P21/c with Z = 4 giving Dcalc = 2·997. Strongest lines are 11·951 Å(10), 4·190 (7), 3·116 (6), 5·092 (5), 3·644 (4), 2·951 (4), 2·591 (4), 2·132 (4). Indices are α = 1·663, β = 1·715 ‖ [010], γ = 1·734, 44° to [001] in obtuse β; 2Vα = 60·2°; inclined dispersion p > v strong. Twinned on {100}. Analysis by wet methods gave CaO = 20·57%, Mn2O3 = 23·42, SiO2 = 39·14, H2O = 16·0 leading to
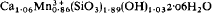 or CaMn3+ (SiO3)2(OH). 2H2O.
or CaMn3+ (SiO3)2(OH). 2H2O.Named for its discoverer, Joe Ana Ruiz of Mammoth, Arizona
Maternal dietary vitamin D intakes during the first trimester of pregnancy
- S. Cawley, K. Duggan, L. Mullaney, D. McCartney, M.J. Turner
-
- Journal:
- Proceedings of the Nutrition Society / Volume 75 / Issue OCE3 / 2016
- Published online by Cambridge University Press:
- 24 November 2016, E187
-
- Article
-
- You have access Access
- HTML
- Export citation
Maternal dietary vitamin B12 intakes during the first trimester of pregnancy
- K. Duggan, S. Cawley, L. Mullaney, D. McCartney, M.J. Turner
-
- Journal:
- Proceedings of the Nutrition Society / Volume 75 / Issue OCE3 / 2016
- Published online by Cambridge University Press:
- 24 November 2016, E241
-
- Article
-
- You have access Access
- HTML
- Export citation
Interstage somatic growth in children with hypoplastic left heart syndrome after initial palliation with the hybrid procedure
- Fiona T. S. Chan, Hannah R. Bellsham-Revell, Hannah Duggan, John M. Simpson, Tony Hulse, Aaron J. Bell
-
- Journal:
- Cardiology in the Young / Volume 27 / Issue 1 / January 2017
- Published online by Cambridge University Press:
- 08 April 2016, pp. 131-138
-
- Article
- Export citation
-
Introduction
The hybrid procedure is one mode of initial palliation for hypoplastic left heart syndrome. Subsequently, patients proceed with either the “three-stage” pathway – comprehensive second stage followed by Fontan completion – or the “four-stage” pathway – Norwood procedure, hemi-Fontan, or Fontan completion. In this study, we describe somatic growth patterns observed in the hybrid groups and a comparison primary Norwood group.
MethodsA retrospective analysis of patients who have undergone hybrid procedure and Fontan completion was performed. Weight-for-age and height-for-age z-scores were recorded at each operation.
ResultsWe identified 13 hybrid patients – eight in the three-stage pathway and five in the four-stage pathway – and 49 Norwood patients. Weight: three stage: weight decreased from hybrid procedure to comprehensive second stage (−0.4±1.3 versus −2.3±1.4, p<0.01) and then increased to Fontan completion (−0.4±1.5 versus −0.6±1.4, p<0.01); four stage: weight decreased from hybrid procedure to Norwood (−2.0±1.4 versus −3.3±0.9, p=0.06), then stabilised to hemi-Fontan. Weight increased from hemi-Fontan to Fontan completion (−2.7±0.6 versus −1.0±0.7, p=0.01); primary Norwood group: weight decreased from Norwood to hemi-Fontan (p<0.001) and then increased to Fontan completion (p<0.001). Height: height declined from hybrid procedure to Fontan completion in the three-stage group. In the four-stage group, height decreased from hybrid to hemi-Fontan, and then increased to Fontan completion. The Norwood group decreased in height from Norwood to hemi-Fontan, followed by an increase to Fontan completion.
ConclusionIn this study, we show that patients undergoing the hybrid procedure have poor weight gain before superior cavopulmonary connection, before returning to baseline by Fontan completion. This study identifies key periods to target poor somatic growth, a risk factor of morbidity and worse neurodevelopmental outcomes.
Multiplexed TEM Specimen Preparation and Analysis of Plasmonic Nanoparticles
- Sėan K. Mulligan, Jeffrey A. Speir, Ivan Razinkov, Anchi Cheng, John Crum, Tilak Jain, Erika Duggan, Er Liu, John P. Nolan, Bridget Carragher, Clinton S. Potter
-
- Journal:
- Microscopy and Microanalysis / Volume 21 / Issue 4 / August 2015
- Published online by Cambridge University Press:
- 30 July 2015, pp. 1017-1025
- Print publication:
- August 2015
-
- Article
- Export citation
-
We describe a system for rapidly screening hundreds of nanoparticle samples using transmission electron microscopy (TEM). The system uses a liquid handling robot to place up to 96 individual samples onto a single standard TEM grid at separate locations. The grid is then transferred into the TEM and automated software is used to acquire multiscale images of each sample. The images are then analyzed to extract metrics on the size, shape, and morphology of the nanoparticles. The system has been used to characterize plasmonically active nanomaterials.
Contributors
-
- By Marcus P. Adams, Robert Bolton, Sanjay Chandrasekharan, Elijah Chudnoff, Edward T. Cokely, William Duggan, Adam Feltz, Roger Giner-Sorolla, Barbara S. Held, Jonathan Jenkins Ichikawa, Chad Kidd, Tara-Marie Linné, Peter Machamer, Farzad Mahootian, Heath Massey, William Meehan, Lisa M. Osbeck, Claude Panaccio, Daniel N. Robinson, Peter Slezak, Thomas Sturm, Paul Thagard
- Edited by Lisa M. Osbeck, University of West Georgia, Barbara S. Held, Bowdoin College, Maine
-
- Book:
- Rational Intuition
- Published online:
- 05 September 2014
- Print publication:
- 25 August 2014, pp vii-viii
-
- Chapter
- Export citation
Typhon: Multiplexed TEM Sample Preparation
- Sean Mulligan, Tilak Jain, Erika Duggan, Er Liu, Jeffrey A. Speir, Anchi Cheng, John Nolan, Bridget Carragher, Clinton S. Potter
-
- Journal:
- Microscopy and Microanalysis / Volume 20 / Issue S3 / August 2014
- Published online by Cambridge University Press:
- 27 August 2014, pp. 1158-1159
- Print publication:
- August 2014
-
- Article
-
- You have access Access
- Export citation
Variation at 8q24 and 9p24 and Risk of Epithelial Ovarian Cancer
- Kristin L. White, Thomas A. Sellers, Brooke L. Fridley, Robert A. Vierkant, Catherine M. Phelan, Ya-Yu Tsai, Kimberly R. Kalli, Andrew Berchuck, Edwin S. Iversen, Jr, Lynn C. Hartmann, Mark Liebow, Sebastian Armasu, Zachary Fredericksen, Melissa C. Larson, David Duggan, Fergus J. Couch, Joellen M. Schildkraut, Julie M. Cunningham, Ellen L. Goode
-
- Journal:
- Twin Research and Human Genetics / Volume 13 / Issue 1 / February 2010
- Published online by Cambridge University Press:
- 21 February 2012, pp. 43-56
-
- Article
-
- You have access Access
- Export citation
-
The chromosome 8q24 region (specifically, 8q24.21.a) is known to harbor variants associated with risk of breast, colorectal, prostate, and bladder cancers. In 2008, variants rs10505477 and rs6983267 in this region were associated with increased risk of invasive ovarian cancer (p < 0.01); however, three subsequent ovarian cancer reports of 8q24 variants were null. Here, we used a multi-site case-control study of 940 ovarian cancer cases and 1,041 controls to evaluate associations between these and other single-nucleotide polymorphisms (SNPs) in this 8q24 region, as well as in the 9p24 colorectal cancer associated-region (specifically, 9p24.1.b). A total of 35 SNPs from previous reports and additional tagging SNPs were assessed using an Illumina GoldenGate array and analyzed using logistic regression models, adjusting for population structure and other potential confounders. We observed no association between genotypes and risk of ovarian cancer considering all cases, invasive cases, or invasive serous cases. For example, at 8q24 SNPs rs10505477 and rs6983267, analyses yielded per-allele invasive cancer odds ratios of 0.95 (95% confidence interval (CI) 0.82–1.09, p trend 0.46) and 0.97 (95% CI 0.84–1.12, p trend 0.69), respectively. Analyses using an approach identical to that of the first positive 8q24 report also yielded no association with risk of ovarian cancer. In the 9p24 region, no SNPs were associated with risk of ovarian cancer overall or with invasive or invasive serous disease (all p values > 0.10). These results indicate that the SNPs studied here are not related to risk of this gynecologic malignancy and that the site-specific nature of 8q24.21.a associations may not include ovarian cancer.
Relationship of exclusive breast-feeding to infections and growth of Tanzanian children born to HIV-infected women
- Ramadhani S Mwiru, Donna Spiegelman, Christopher Duggan, Karen Peterson, Enju Liu, Gernard Msamanga, Said Aboud, Wafaie W Fawzi
-
- Journal:
- Public Health Nutrition / Volume 14 / Issue 7 / 09 June 2011
- Published online by Cambridge University Press:
- 16 February 2011, pp. 1251-1258
-
- Article
-
- You have access Access
- HTML
- Export citation
-
Objective
We examined the relationships between exclusive breast-feeding and the risks of respiratory, diarrhoea and nutritional morbidities during the first 2 years of life among children born to women infected with HIV-1.
DesignWe prospectively determined the incidence of respiratory illnesses, diarrhoea, fever, hospitalizations, outpatient visits and nutritional morbidities. Generalized estimating equations were used to estimate the relative risks for morbidity episodes and Cox proportional hazards models to estimate the incidence rate ratios of nutritional morbidities.
SettingDar es Salaam, Tanzania.
SubjectsThe sample consisted of 666 children born to HIV-infected women.
ResultsThe 666 children were followed for 2 years. Exclusive breast-feeding was associated with lower risk for cough (rate ratio (RR) = 0·49, 95 % CI 0·41, 0·60, P < 0·0001), cough and fever (RR = 0·44, 95 % CI 0·32, 0·60, P < 0·0001) and cough and difficulty breathing or refusal to feed (RR = 0·31, 95 % CI 0·18, 0·55, P < 0·0001). Exclusive breast-feeding was also associated with lower risk of acute diarrhoea, watery diarrhoea, dysentery, fever and outpatient visits during the first 6 months of life, but showed no effect at 6–24 months of life. Exclusive breast-feeding did not significantly reduce the risks of nutritional morbidities during the first 2 years of life.
ConclusionsExclusive breast-feeding is strongly associated with reductions in the risk of respiratory and diarrhoea morbidities during the first 6 months of life among children born to HIV-infected women.
Contributors
-
- By Rose Teteki Abbey, K. C. Abraham, David Tuesday Adamo, LeRoy H. Aden, Efrain Agosto, Victor Aguilan, Gillian T. W. Ahlgren, Charanjit Kaur AjitSingh, Dorothy B E A Akoto, Giuseppe Alberigo, Daniel E. Albrecht, Ruth Albrecht, Daniel O. Aleshire, Urs Altermatt, Anand Amaladass, Michael Amaladoss, James N. Amanze, Lesley G. Anderson, Thomas C. Anderson, Victor Anderson, Hope S. Antone, María Pilar Aquino, Paula Arai, Victorio Araya Guillén, S. Wesley Ariarajah, Ellen T. Armour, Brett Gregory Armstrong, Atsuhiro Asano, Naim Stifan Ateek, Mahmoud Ayoub, John Alembillah Azumah, Mercedes L. García Bachmann, Irena Backus, J. Wayne Baker, Mieke Bal, Lewis V. Baldwin, William Barbieri, António Barbosa da Silva, David Basinger, Bolaji Olukemi Bateye, Oswald Bayer, Daniel H. Bays, Rosalie Beck, Nancy Elizabeth Bedford, Guy-Thomas Bedouelle, Chorbishop Seely Beggiani, Wolfgang Behringer, Christopher M. Bellitto, Byard Bennett, Harold V. Bennett, Teresa Berger, Miguel A. Bernad, Henley Bernard, Alan E. Bernstein, Jon L. Berquist, Johannes Beutler, Ana María Bidegain, Matthew P. Binkewicz, Jennifer Bird, Joseph Blenkinsopp, Dmytro Bondarenko, Paulo Bonfatti, Riet en Pim Bons-Storm, Jessica A. Boon, Marcus J. Borg, Mark Bosco, Peter C. Bouteneff, François Bovon, William D. Bowman, Paul S. Boyer, David Brakke, Richard E. Brantley, Marcus Braybrooke, Ian Breward, Ênio José da Costa Brito, Jewel Spears Brooker, Johannes Brosseder, Nicholas Canfield Read Brown, Robert F. Brown, Pamela K. Brubaker, Walter Brueggemann, Bishop Colin O. Buchanan, Stanley M. Burgess, Amy Nelson Burnett, J. Patout Burns, David B. Burrell, David Buttrick, James P. Byrd, Lavinia Byrne, Gerado Caetano, Marcos Caldas, Alkiviadis Calivas, William J. Callahan, Salvatore Calomino, Euan K. Cameron, William S. Campbell, Marcelo Ayres Camurça, Daniel F. Caner, Paul E. Capetz, Carlos F. Cardoza-Orlandi, Patrick W. Carey, Barbara Carvill, Hal Cauthron, Subhadra Mitra Channa, Mark D. Chapman, James H. Charlesworth, Kenneth R. Chase, Chen Zemin, Luciano Chianeque, Philip Chia Phin Yin, Francisca H. Chimhanda, Daniel Chiquete, John T. Chirban, Soobin Choi, Robert Choquette, Mita Choudhury, Gerald Christianson, John Chryssavgis, Sejong Chun, Esther Chung-Kim, Charles M. A. Clark, Elizabeth A. Clark, Sathianathan Clarke, Fred Cloud, John B. Cobb, W. Owen Cole, John A Coleman, John J. Collins, Sylvia Collins-Mayo, Paul K. Conkin, Beth A. Conklin, Sean Connolly, Demetrios J. Constantelos, Michael A. Conway, Paula M. Cooey, Austin Cooper, Michael L. Cooper-White, Pamela Cooper-White, L. William Countryman, Sérgio Coutinho, Pamela Couture, Shannon Craigo-Snell, James L. Crenshaw, David Crowner, Humberto Horacio Cucchetti, Lawrence S. Cunningham, Elizabeth Mason Currier, Emmanuel Cutrone, Mary L. Daniel, David D. Daniels, Robert Darden, Rolf Darge, Isaiah Dau, Jeffry C. Davis, Jane Dawson, Valentin Dedji, John W. de Gruchy, Paul DeHart, Wendy J. Deichmann Edwards, Miguel A. De La Torre, George E. Demacopoulos, Thomas de Mayo, Leah DeVun, Beatriz de Vasconcellos Dias, Dennis C. Dickerson, John M. Dillon, Luis Miguel Donatello, Igor Dorfmann-Lazarev, Susanna Drake, Jonathan A. Draper, N. Dreher Martin, Otto Dreydoppel, Angelyn Dries, A. J. Droge, Francis X. D'Sa, Marilyn Dunn, Nicole Wilkinson Duran, Rifaat Ebied, Mark J. Edwards, William H. Edwards, Leonard H. Ehrlich, Nancy L. Eiesland, Martin Elbel, J. Harold Ellens, Stephen Ellingson, Marvin M. Ellison, Robert Ellsberg, Jean Bethke Elshtain, Eldon Jay Epp, Peter C. Erb, Tassilo Erhardt, Maria Erling, Noel Leo Erskine, Gillian R. Evans, Virginia Fabella, Michael A. Fahey, Edward Farley, Margaret A. Farley, Wendy Farley, Robert Fastiggi, Seena Fazel, Duncan S. Ferguson, Helwar Figueroa, Paul Corby Finney, Kyriaki Karidoyanes FitzGerald, Thomas E. FitzGerald, John R. Fitzmier, Marie Therese Flanagan, Sabina Flanagan, Claude Flipo, Ronald B. Flowers, Carole Fontaine, David Ford, Mary Ford, Stephanie A. Ford, Jim Forest, William Franke, Robert M. Franklin, Ruth Franzén, Edward H. Friedman, Samuel Frouisou, Lorelei F. Fuchs, Jojo M. Fung, Inger Furseth, Richard R. Gaillardetz, Brandon Gallaher, China Galland, Mark Galli, Ismael García, Tharscisse Gatwa, Jean-Marie Gaudeul, Luis María Gavilanes del Castillo, Pavel L. Gavrilyuk, Volney P. Gay, Metropolitan Athanasios Geevargis, Kondothra M. George, Mary Gerhart, Simon Gikandi, Maurice Gilbert, Michael J. Gillgannon, Verónica Giménez Beliveau, Terryl Givens, Beth Glazier-McDonald, Philip Gleason, Menghun Goh, Brian Golding, Bishop Hilario M. Gomez, Michelle A. Gonzalez, Donald K. Gorrell, Roy Gottfried, Tamara Grdzelidze, Joel B. Green, Niels Henrik Gregersen, Cristina Grenholm, Herbert Griffiths, Eric W. Gritsch, Erich S. Gruen, Christoffer H. Grundmann, Paul H. Gundani, Jon P. Gunnemann, Petre Guran, Vidar L. Haanes, Jeremiah M. Hackett, Getatchew Haile, Douglas John Hall, Nicholas Hammond, Daphne Hampson, Jehu J. Hanciles, Barry Hankins, Jennifer Haraguchi, Stanley S. Harakas, Anthony John Harding, Conrad L. Harkins, J. William Harmless, Marjory Harper, Amir Harrak, Joel F. Harrington, Mark W. Harris, Susan Ashbrook Harvey, Van A. Harvey, R. Chris Hassel, Jione Havea, Daniel Hawk, Diana L. Hayes, Leslie Hayes, Priscilla Hayner, S. Mark Heim, Simo Heininen, Richard P. Heitzenrater, Eila Helander, David Hempton, Scott H. Hendrix, Jan-Olav Henriksen, Gina Hens-Piazza, Carter Heyward, Nicholas J. Higham, David Hilliard, Norman A. Hjelm, Peter C. Hodgson, Arthur Holder, M. Jan Holton, Dwight N. Hopkins, Ronnie Po-chia Hsia, Po-Ho Huang, James Hudnut-Beumler, Jennifer S. Hughes, Leonard M. Hummel, Mary E. Hunt, Laennec Hurbon, Mark Hutchinson, Susan E. Hylen, Mary Beth Ingham, H. Larry Ingle, Dale T. Irvin, Jon Isaak, Paul John Isaak, Ada María Isasi-Díaz, Hans Raun Iversen, Margaret C. Jacob, Arthur James, Maria Jansdotter-Samuelsson, David Jasper, Werner G. Jeanrond, Renée Jeffery, David Lyle Jeffrey, Theodore W. Jennings, David H. Jensen, Robin Margaret Jensen, David Jobling, Dale A. Johnson, Elizabeth A. Johnson, Maxwell E. Johnson, Sarah Johnson, Mark D. Johnston, F. Stanley Jones, James William Jones, John R. Jones, Alissa Jones Nelson, Inge Jonsson, Jan Joosten, Elizabeth Judd, Mulambya Peggy Kabonde, Robert Kaggwa, Sylvester Kahakwa, Isaac Kalimi, Ogbu U. Kalu, Eunice Kamaara, Wayne C. Kannaday, Musimbi Kanyoro, Veli-Matti Kärkkäinen, Frank Kaufmann, Léon Nguapitshi Kayongo, Richard Kearney, Alice A. Keefe, Ralph Keen, Catherine Keller, Anthony J. Kelly, Karen Kennelly, Kathi Lynn Kern, Fergus Kerr, Edward Kessler, George Kilcourse, Heup Young Kim, Kim Sung-Hae, Kim Yong-Bock, Kim Yung Suk, Richard King, Thomas M. King, Robert M. Kingdon, Ross Kinsler, Hans G. Kippenberg, Cheryl A. Kirk-Duggan, Clifton Kirkpatrick, Leonid Kishkovsky, Nadieszda Kizenko, Jeffrey Klaiber, Hans-Josef Klauck, Sidney Knight, Samuel Kobia, Robert Kolb, Karla Ann Koll, Heikki Kotila, Donald Kraybill, Philip D. W. Krey, Yves Krumenacker, Jeffrey Kah-Jin Kuan, Simanga R. Kumalo, Peter Kuzmic, Simon Shui-Man Kwan, Kwok Pui-lan, André LaCocque, Stephen E. Lahey, John Tsz Pang Lai, Emiel Lamberts, Armando Lampe, Craig Lampe, Beverly J. Lanzetta, Eve LaPlante, Lizette Larson-Miller, Ariel Bybee Laughton, Leonard Lawlor, Bentley Layton, Robin A. Leaver, Karen Lebacqz, Archie Chi Chung Lee, Marilyn J. Legge, Hervé LeGrand, D. L. LeMahieu, Raymond Lemieux, Bill J. Leonard, Ellen M. Leonard, Outi Leppä, Jean Lesaulnier, Nantawan Boonprasat Lewis, Henrietta Leyser, Alexei Lidov, Bernard Lightman, Paul Chang-Ha Lim, Carter Lindberg, Mark R. Lindsay, James R. Linville, James C. Livingston, Ann Loades, David Loades, Jean-Claude Loba-Mkole, Lo Lung Kwong, Wati Longchar, Eleazar López, David W. Lotz, Andrew Louth, Robin W. Lovin, William Luis, Frank D. Macchia, Diarmaid N. J. MacCulloch, Kirk R. MacGregor, Marjory A. MacLean, Donald MacLeod, Tomas S. Maddela, Inge Mager, Laurenti Magesa, David G. Maillu, Fortunato Mallimaci, Philip Mamalakis, Kä Mana, Ukachukwu Chris Manus, Herbert Robinson Marbury, Reuel Norman Marigza, Jacqueline Mariña, Antti Marjanen, Luiz C. L. Marques, Madipoane Masenya (ngwan'a Mphahlele), Caleb J. D. Maskell, Steve Mason, Thomas Massaro, Fernando Matamoros Ponce, András Máté-Tóth, Odair Pedroso Mateus, Dinis Matsolo, Fumitaka Matsuoka, John D'Arcy May, Yelena Mazour-Matusevich, Theodore Mbazumutima, John S. McClure, Christian McConnell, Lee Martin McDonald, Gary B. McGee, Thomas McGowan, Alister E. McGrath, Richard J. McGregor, John A. McGuckin, Maud Burnett McInerney, Elsie Anne McKee, Mary B. McKinley, James F. McMillan, Ernan McMullin, Kathleen E. McVey, M. Douglas Meeks, Monica Jyotsna Melanchthon, Ilie Melniciuc-Puica, Everett Mendoza, Raymond A. Mentzer, William W. Menzies, Ina Merdjanova, Franziska Metzger, Constant J. Mews, Marvin Meyer, Carol Meyers, Vasile Mihoc, Gunner Bjerg Mikkelsen, Maria Inêz de Castro Millen, Clyde Lee Miller, Bonnie J. Miller-McLemore, Alexander Mirkovic, Paul Misner, Nozomu Miyahira, R. W. L. Moberly, Gerald Moede, Aloo Osotsi Mojola, Sunanda Mongia, Rebeca Montemayor, James Moore, Roger E. Moore, Craig E. Morrison O.Carm, Jeffry H. Morrison, Keith Morrison, Wilson J. Moses, Tefetso Henry Mothibe, Mokgethi Motlhabi, Fulata Moyo, Henry Mugabe, Jesse Ndwiga Kanyua Mugambi, Peggy Mulambya-Kabonde, Robert Bruce Mullin, Pamela Mullins Reaves, Saskia Murk Jansen, Heleen L. Murre-Van den Berg, Augustine Musopole, Isaac M. T. Mwase, Philomena Mwaura, Cecilia Nahnfeldt, Anne Nasimiyu Wasike, Carmiña Navia Velasco, Thulani Ndlazi, Alexander Negrov, James B. Nelson, David G. Newcombe, Carol Newsom, Helen J. Nicholson, George W. E. Nickelsburg, Tatyana Nikolskaya, Damayanthi M. A. Niles, Bertil Nilsson, Nyambura Njoroge, Fidelis Nkomazana, Mary Beth Norton, Christian Nottmeier, Sonene Nyawo, Anthère Nzabatsinda, Edward T. Oakes, Gerald O'Collins, Daniel O'Connell, David W. Odell-Scott, Mercy Amba Oduyoye, Kathleen O'Grady, Oyeronke Olajubu, Thomas O'Loughlin, Dennis T. Olson, J. Steven O'Malley, Cephas N. Omenyo, Muriel Orevillo-Montenegro, César Augusto Ornellas Ramos, Agbonkhianmeghe E. Orobator, Kenan B. Osborne, Carolyn Osiek, Javier Otaola Montagne, Douglas F. Ottati, Anna May Say Pa, Irina Paert, Jerry G. Pankhurst, Aristotle Papanikolaou, Samuele F. Pardini, Stefano Parenti, Peter Paris, Sung Bae Park, Cristián G. Parker, Raquel Pastor, Joseph Pathrapankal, Daniel Patte, W. Brown Patterson, Clive Pearson, Keith F. Pecklers, Nancy Cardoso Pereira, David Horace Perkins, Pheme Perkins, Edward N. Peters, Rebecca Todd Peters, Bishop Yeznik Petrossian, Raymond Pfister, Peter C. Phan, Isabel Apawo Phiri, William S. F. Pickering, Derrick G. Pitard, William Elvis Plata, Zlatko Plese, John Plummer, James Newton Poling, Ronald Popivchak, Andrew Porter, Ute Possekel, James M. Powell, Enos Das Pradhan, Devadasan Premnath, Jaime Adrían Prieto Valladares, Anne Primavesi, Randall Prior, María Alicia Puente Lutteroth, Eduardo Guzmão Quadros, Albert Rabil, Laurent William Ramambason, Apolonio M. Ranche, Vololona Randriamanantena Andriamitandrina, Lawrence R. Rast, Paul L. Redditt, Adele Reinhartz, Rolf Rendtorff, Pål Repstad, James N. Rhodes, John K. Riches, Joerg Rieger, Sharon H. Ringe, Sandra Rios, Tyler Roberts, David M. Robinson, James M. Robinson, Joanne Maguire Robinson, Richard A. H. Robinson, Roy R. Robson, Jack B. Rogers, Maria Roginska, Sidney Rooy, Rev. Garnett Roper, Maria José Fontelas Rosado-Nunes, Andrew C. Ross, Stefan Rossbach, François Rossier, John D. Roth, John K. Roth, Phillip Rothwell, Richard E. Rubenstein, Rosemary Radford Ruether, Markku Ruotsila, John E. Rybolt, Risto Saarinen, John Saillant, Juan Sanchez, Wagner Lopes Sanchez, Hugo N. Santos, Gerhard Sauter, Gloria L. Schaab, Sandra M. Schneiders, Quentin J. Schultze, Fernando F. Segovia, Turid Karlsen Seim, Carsten Selch Jensen, Alan P. F. Sell, Frank C. Senn, Kent Davis Sensenig, Damían Setton, Bal Krishna Sharma, Carolyn J. Sharp, Thomas Sheehan, N. Gerald Shenk, Christian Sheppard, Charles Sherlock, Tabona Shoko, Walter B. Shurden, Marguerite Shuster, B. Mark Sietsema, Batara Sihombing, Neil Silberman, Clodomiro Siller, Samuel Silva-Gotay, Heikki Silvet, John K. Simmons, Hagith Sivan, James C. Skedros, Abraham Smith, Ashley A. Smith, Ted A. Smith, Daud Soesilo, Pia Søltoft, Choan-Seng (C. S.) Song, Kathryn Spink, Bryan Spinks, Eric O. Springsted, Nicolas Standaert, Brian Stanley, Glen H. Stassen, Karel Steenbrink, Stephen J. Stein, Andrea Sterk, Gregory E. Sterling, Columba Stewart, Jacques Stewart, Robert B. Stewart, Cynthia Stokes Brown, Ken Stone, Anne Stott, Elizabeth Stuart, Monya Stubbs, Marjorie Hewitt Suchocki, David Kwang-sun Suh, Scott W. Sunquist, Keith Suter, Douglas Sweeney, Charles H. Talbert, Shawqi N. Talia, Elsa Tamez, Joseph B. Tamney, Jonathan Y. Tan, Yak-Hwee Tan, Kathryn Tanner, Feiya Tao, Elizabeth S. Tapia, Aquiline Tarimo, Claire Taylor, Mark Lewis Taylor, Bishop Abba Samuel Wolde Tekestebirhan, Eugene TeSelle, M. Thomas Thangaraj, David R. Thomas, Andrew Thornley, Scott Thumma, Marcelo Timotheo da Costa, George E. “Tink” Tinker, Ola Tjørhom, Karen Jo Torjesen, Iain R. Torrance, Fernando Torres-Londoño, Archbishop Demetrios [Trakatellis], Marit Trelstad, Christine Trevett, Phyllis Trible, Johannes Tromp, Paul Turner, Robert G. Tuttle, Archbishop Desmond Tutu, Peter Tyler, Anders Tyrberg, Justin Ukpong, Javier Ulloa, Camillus Umoh, Kristi Upson-Saia, Martina Urban, Monica Uribe, Elochukwu Eugene Uzukwu, Richard Vaggione, Gabriel Vahanian, Paul Valliere, T. J. Van Bavel, Steven Vanderputten, Peter Van der Veer, Huub Van de Sandt, Louis Van Tongeren, Luke A. Veronis, Noel Villalba, Ramón Vinke, Tim Vivian, David Voas, Elena Volkova, Katharina von Kellenbach, Elina Vuola, Timothy Wadkins, Elaine M. Wainwright, Randi Jones Walker, Dewey D. Wallace, Jerry Walls, Michael J. Walsh, Philip Walters, Janet Walton, Jonathan L. Walton, Wang Xiaochao, Patricia A. Ward, David Harrington Watt, Herold D. Weiss, Laurence L. Welborn, Sharon D. Welch, Timothy Wengert, Traci C. West, Merold Westphal, David Wetherell, Barbara Wheeler, Carolinne White, Jean-Paul Wiest, Frans Wijsen, Terry L. Wilder, Felix Wilfred, Rebecca Wilkin, Daniel H. Williams, D. Newell Williams, Michael A. Williams, Vincent L. Wimbush, Gabriele Winkler, Anders Winroth, Lauri Emílio Wirth, James A. Wiseman, Ebba Witt-Brattström, Teofil Wojciechowski, John Wolffe, Kenman L. Wong, Wong Wai Ching, Linda Woodhead, Wendy M. Wright, Rose Wu, Keith E. Yandell, Gale A. Yee, Viktor Yelensky, Yeo Khiok-Khng, Gustav K. K. Yeung, Angela Yiu, Amos Yong, Yong Ting Jin, You Bin, Youhanna Nessim Youssef, Eliana Yunes, Robert Michael Zaller, Valarie H. Ziegler, Barbara Brown Zikmund, Joyce Ann Zimmerman, Aurora Zlotnik, Zhuo Xinping
- Edited by Daniel Patte, Vanderbilt University, Tennessee
-
- Book:
- The Cambridge Dictionary of Christianity
- Published online:
- 05 August 2012
- Print publication:
- 20 September 2010, pp xi-xliv
-
- Chapter
- Export citation
Does recurrent depression lead to a change in neuroticism?
- Conor F. Duggan, Pak Sham, Alan S. Lee, Robin M. Murray
-
- Journal:
- Psychological Medicine / Volume 21 / Issue 4 / November 1991
- Published online by Cambridge University Press:
- 09 July 2009, pp. 985-990
-
- Article
- Export citation
-
The hypothesis that recurrent or chronic depressive illness produces a long-term change in neuroticism was examined in a sample (N = 34) from a consecutive series of 89 depressed patients admitted to the Maudsley Hospital in 1965/6. The Eysenck Personality Inventory (EPI) was administered at the time of the index illness both when the patients were depressed and on recovery, and then again at follow-up 18 years later. The change in the neuroticism (N) score over the 18-year-period was compared in good and poor outcome groups defined variously by a global rating of outcome, frequency of episodes, extent of subsequent hospitalization and the presence or absence of subsequent chronicity. The mean N score for the sample as a whole did not change significantly over the 18 years, and no differential change in the N score was observed between any of the good and poor outcome groups. Thus, the hypothesis was not supported.
Dysfunctional attitudes in depressed and recovered depressed patients and their first-degree relatives
- M. J. Power, C. F. Duggan, A. S. Lee, R. M. Murray
-
- Journal:
- Psychological Medicine / Volume 25 / Issue 1 / January 1995
- Published online by Cambridge University Press:
- 09 July 2009, pp. 87-93
-
- Article
- Export citation
-
A series of depressed probands and their first-degree relatives were categorized as follows: (a) currently depressed; (b) recovered depressed; and (c) never-ill relatives. Their scores on a subscaled version of the Dysfunctional Attitude Scale (the DAS-24) were compared. The DAS total scores mirrored previous findings in that the total scores for recovered individuals returned to normal or near-normal levels. However, the dependency subscale scores remained elevated for the recovered depressed group. It is proposed that these results support the conclusion that self-report measures of cognitive vulnerability should focus on specific rather than global effects, if progress is to be made in the search for true vulnerability factors.




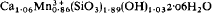 or CaMn
or CaMn