2 results
From contact coverage to effective coverage of community care for patients with severe mental disorders: a real-world investigation from Italy. Methodology and results from the QUADIM project
- M. Monzio Compagnoni, G. Corrao, A. Barbato, B. D’Avanzo, T. Di Fiandra, F. Carle, L. Ferrara, V. D. Tozzi, A. Gaddini, A. Saponaro, S. Scondotto, D. Chisholm, A. Lora
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S66-S67
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The evaluation of healthcare pathways must be considered of fundamental importance. The quality of care provided to patients with severe mental disorders (SMD) does not correspond to the standards set by the recommendations. Therefore, measures such as the real coverage rate of psychiatric patients’ needs (contact coverage), by comparing epidemiological prevalence rates and the number of patients receiving adequate care, could be a valuable resource for implementing the transition to community mental health. However, simple assessment and reporting of rates of contact with mental healthcare potentially overestimate the full expected health benefits of services. Therefore, in addition to monitor the coverage rate achieved by the services, the evaluation of the effectiveness of the care provided (effective coverage) [De Silva et al. Int J Epidemiol 2014;43(2):341–53] is also of relevant importance.
ObjectivesTo measure the gap between contact and effective coverage of mental healthcare, i.e., the effectiveness of interventions provided by services for the treatment of SMD in preventing an exacerbation of psychiatric symptoms.
MethodsData were retrieved from Healthcare Utilization databases of four Italian Regions (Lombardy, Emilia-Romagna, Lazio, Sicily). 45,761 newly taken-in-care cases of depression, schizophrenia, bipolar, and personality disorder were included. A variant of the self-controlled case series method was used to estimate the incidence rate ratio (IRR) for the relationship between exposure (use of different types of mental healthcare such as pharmacotherapy, generic contacts with the outpatient service, psychosocial interventions, and psychotherapies) and relapse episodes (mental illness emergency hospital admissions).
Results11,500 relapses occurred. Relapse risk was reduced (Figure) during periods covered by (i) psychotherapy for patients with depression (IRR 0.67; 95% CI, 0.49 to 0.91) and bipolar disorder (0.64; 0.29 to 0.99); (ii) psychosocial interventions for those with depression (0.74; 0.56 to 0.98), schizophrenia (0.83; 0.68 to 0.99) and bipolar disorder (0.55; 0.36 to 0.84), (iii) pharmacotherapy for those with schizophrenia (0.58; 0.49 to 0.69), and bipolar disorder (0.59; 0.44 to 0.78). Coverage with generic mental healthcare, in the absence of psychosocial/psychotherapeutic interventions, did not affect the risk of relapse.
Image:
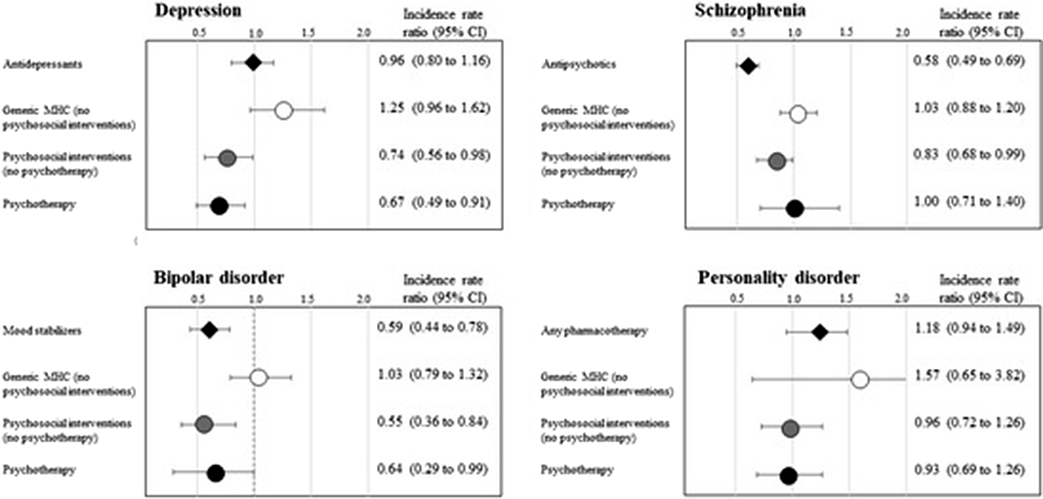 Conclusions
ConclusionsPsychosocial interventions, psychotherapies and specific pharmacotherapies can be considered particularly effective in treating patients with bipolar, depressive, and schizophrenic disorders. This study ascertained the gap between utilization of mental healthcare and effective coverage, showing that real-world data can represent a useful resource to monitor mental healthcare paths and to assess the effectiveness of a mental health system.
Disclosure of InterestNone Declared
The quality of mental health care delivered to patients with schizophrenic disorder in the Italian mental health system. The QUADIM project A multi-regional Italian investigation based on healthcare utilization databases
- M. Monzio Compagnoni, G. Corrao, L. Allevi, A. Barbato, B. D’Avanzo, F. Carle, A. Saponaro, A. Gaddini, S. Scondotto, L. Ferrara, V. D. Tozzi, T. Di Fiandra, A. Lora
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S486
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The 1978 Italian reform of psychiatric services initiated the closure of psychiatric hospitals encouraging the development of community mental health. However, there is wide variability across regions in the amount of resources devoted to community-based psychiatric care, and the range of services provided still is cause of concern.
ObjectivesTo evaluate the quality of mental health care delivered to patients with schizophrenia and related disorders taken-in-care by mental health services in four Italian regions (Lombardy, Emilia-Romagna, Lazio, Sicily).
MethodsThirty-one clinical indicators concerning accessibility, appropriateness, continuity, and safety were defined and estimated using healthcare utilization (HCU) databases, containing data on mental health treatments, hospital admissions, outpatient interventions, lab tests and drug prescriptions.
ResultsA total of 70,586 prevalent patients with schizophrenia treated in 2015 were identified, of whom 1,752 were newly taken-in-care. For most patients community care was accessible and moderately intensive. However, care pathways were not implemented based on a structured assessment and only half of the patients received psychosocial treatments. One patient out of ten had access to psychological interventions and psychoeducation. Activities specifically addressed to families involved a third of prevalent patients and less than half of new patients. One patient out of six was admitted to a community residential facility, and one out of ten to a general hospital psychiatric ward (GHPW); higher values were identified in new cases. In general hospitals, one-fifth of the admissions were followed by readmission within 30 days of discharge. For two- thirds of patients continuity of community care was met, and six times out of ten a discharge from a GHPW was followed by an outpatient contact within two weeks. For cases newly taken-in-care the continuity of community care was uncommon, while the readiness of outpatient contacts after discharge was slightly more frequent. Most of the patients received antipsychotic medication, but their adherence to long-term treatment was low. Antipsychotic polytherapy was frequent and the control of metabolic side effects was poor. The variability between regions was high and consistent.
ConclusionsThe Italian mental health system could be improved by increasing the accessibility to psychosocial interventions, improving the quality of care for newly taken-in-care patients, focusing on somatic health and mortality, and reducing regional variability. Clinical indicators demonstrate the strengths and weaknesses of the mental health system in these regions, and, as HCU databases, they could be useful tools in the routine assessment of mental healthcare quality at regional and national levels.
Disclosure of InterestNone Declared




