2 results
A cross-sectional descriptive study to assess the impact of the “open door” policy on patient satisfaction
- M. Campillo, J. Marti, L. Rius, S. Garcia Fernandez, M. Olivero, G. Sanchez Tomico, G. Brusco-Passalaqua, E. Pechuan, T. Vates, R. Sanchez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S910
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Since the beginning of the modern psychiatry the acute units have established a “locked door” policy. Some studies show that this condition may increase patient’s discomfort and affect the perception of health quality of care (Boyer L, 2009, Eur Psychiatry Dec;24(8):540-9). Lately, several European countries such as Germany, Switzerland and Spain are starting to implement the “open-door” policy but its impact on patient’s satisfaction is still unknown (Hochstrasser, L, Frontiers in Psychiatry, 9(57). https://doi.org/10.3389/fpsyt.2018.00057) .
ObjectivesTo help characterize the advantages of the “open-door” policy implemented in an acute inpatient psychiatric unit in order to assess the patient’s view of it.
MethodsThis is a descriptive observational study carried out at an inpatient psychiatric unit. Data were collected after the implementation of the open door policy on June 2019, assessing the patient satisfaction of 31 subjects who completed the SATISPSY-22 scale at the time of discharge. Results are described using the average and its standard deviation.
ResultsResults show scores in all items above 50 points, being the care team and the quality of care the most valued ones with 82 and 79 points respectively. The overall score is above 65 points (Fig. 1).
Image:
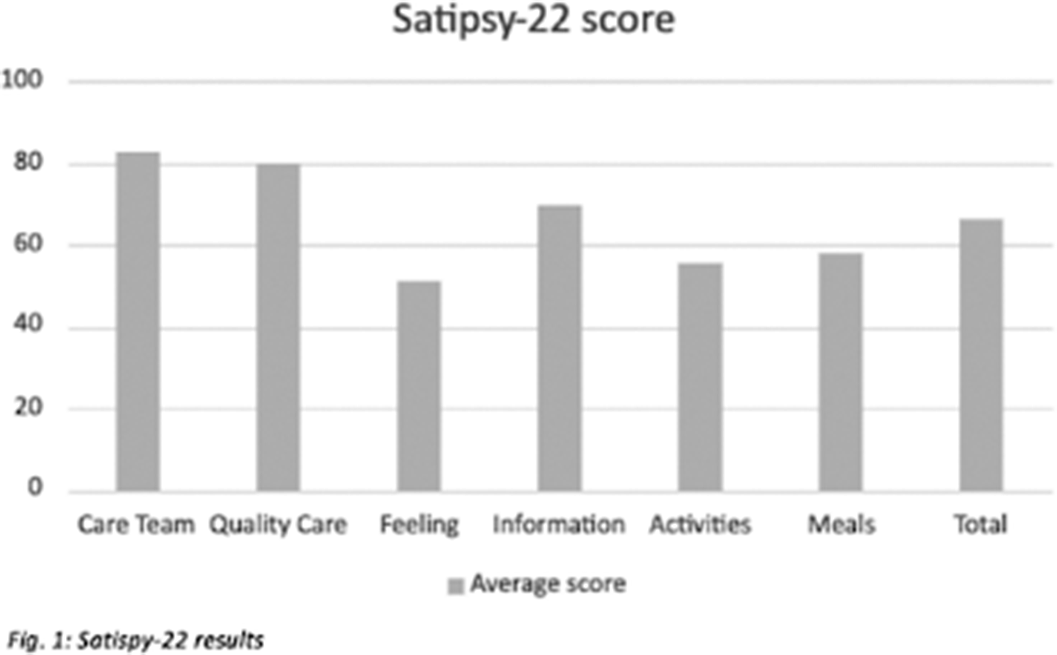 Conclusions
ConclusionsIn line with previous studies, our data suggests that the main impact of the “open-door” policy implementation is on patients’ perception of the care, being Quality of care and satisfaction with the Staff the items with highest scores. This could be explained by patients trusting more in the Care team, which would help enhance the therapeutic relationship improving therapeutic adherence, treatment adequacy and the outcome. Nevertheless, the Feeling related to hospitalisation was found to be the item with the lowest score. This could mean strategies should focus on improving patient’s insight regarding their clinical state and their need to be admitted. Our study supports the hypothesis that open-door policy in acute psychiatric units is seen positively by patients and that further research should be carried.
Disclosure of InterestNone Declared
Music therapy in psychiatric units: evaluating its effectiveness
- M. Campillo, T. Vates, A. Pratdesava, M. Vallve, A. Casals, J. Ortega Vallve, R. Sanchez Gonzalez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S902-S903
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Research shows the benefits of music therapy for various mental health conditions, including depression, trauma, and schizophrenia. Music acts as a medium for processing emotions, trauma, and grief.
Playing instruments can encourage emotional expression, socialization and exploration of various therapeutic themes (i.e. conflict, communication, grief, etc.).
Group music therapy, measured by questionnaires and described in qualitative interviews, improved quality of life and self-esteem for people with severe mental illness (SMI).Group singing and song writing provide creative options for social connections. Music therapy should be considered as a component of holistic care for people with SMI. Jungup Lee, Thyer BA. May 2013Journal of Human Behaviour in the Social Environment 23(5):597-609
ObjectivesMusic therapy sessions are held in our hospital for people admitted to short-term hospitalization units and to psychosocial rehabilitation units. The goal of the sessions is to create a connection space, promote people’s confidence in their own resources for their recovery, and evoke valuable experiences and memories. Sometimes musicians from the community have been present in the sessions, contributing to overcoming the stigma towards mental illness.
MethodsWe describe self-assessment of people admitted to psychiatric units after attending music therapy sessions. People from brief hospitalization unit filled out a survey, after each session, voluntarily, about their emotional state at the beginning of the session and after it. People from rehabilitation units, voluntarily filled the SRS V.3.0. 2002-Miller. Duncan & Johnson escale.The SRS was designed for use by clinicians to assess the therapeutic alliance during therapy (Duncan BL et al. The Session Rating Scale: Preliminary Psychometric Properties of a “Working” Alliance Measure JBT 3(1) 3-12 12/14/04 3:53 PM Page 3).
Results23 sessions took place for each unit. 39 patients from brief hospitalization, 22 women and 17 men, attended the sessions. 15 had a diagnosis of schizophrenia and related disorders, 13 were affective disorders, and 11 others diagnosis. All of them liked the participation either fully or partially. 76% men and 77% women felt better after, none of them reported to feel worse. 82% men and 86% women replied they would repeat the session.
Patients from rehabilitation units were 7 women and 10 men. 14 had a schizophrenia related disorder and 3 had bipolar disorder. All items on the scale were scored above 9 over 10, (I felt heard, understood, and respected/ We worked on and talked about what I wanted to work on and talk about/ The therapist’s approach is a good fit for me) with an overall score of 9,62 over 10 (Overall, today’s session was right for me).
ConclusionsMusic therapy sessions achieve benefits on an emotional level in any of the diagnoses, improving alliance with care teams, who value sessions as normalizing spaces, helping to overcome stigma.
Disclosure of InterestNone Declared




