6 results
Caring for Bierzo: A plan for improving motivation for health workers from Mental Health
- J. M. Pelayo-Terán, Y. Zapico-Merayo, S. Vega-García, M. E. García-Llamas, Z. Gutiérrez-Hervás, A. Castro-Bayón
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S309-S310
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Motivation is an essential determinant of performance, particularly for those working in difficult conditions, such as the conditions facing many health workers. The relationship between motivation and performance is influenced by the health workers’ organizational environment and social context. Many intrinsic and extrinsic factors may influence the impulse to head for and maintain and effort to achieve the objectives of the organization these may include acknowledgements, status and incentives, but also auto efficacy perception, personal growth, welfare and physical and mental health.
In the last years and particularly during COVID-19 pandemic health organizations have suffered a crisis of lack of motivation and high turnover rates in health professional, particularly among highly specialized professions.
Objectivesto develop a quality program to promote mental health and motivation, detect risk of mental disorders and improve communication skills in the health workers of the Health Area of El Bierzo (GASBI).
MethodsA committee with four members form the psychiatry and mental health service, two from the Quality and Security Unit and 1 from the Occupational Risk Prevention Service analyzed the GASBI with a SWOT-CAME matrix analysis. Actions to be implemented were ordered with a Hanlon method score according to a representative sample of the employees of GASBI.
ResultsThe CAME matrix recommended an offensive strategy, given a number of strengths and the opportunities for an administration sensible to new paradigms. The program proposed included 6 main lines (evaluation, access to mental health consultation, prevention of suicide behavior, resilience group, communication and relation groups and a group of actions to improve motivation and prevent burnout called “10 actions to dream together”, displayed in figures 1 and 2. The Hanlon classified suicide behaviour as the highest priority (score: 16,25 points), mental disorders the second (score: 13.75), then fatigue (13 p), burnout and resilience (12p) and the less prioritary was motivation (7 points). The project was displayed in a canvas business model (figure 3)
Image:
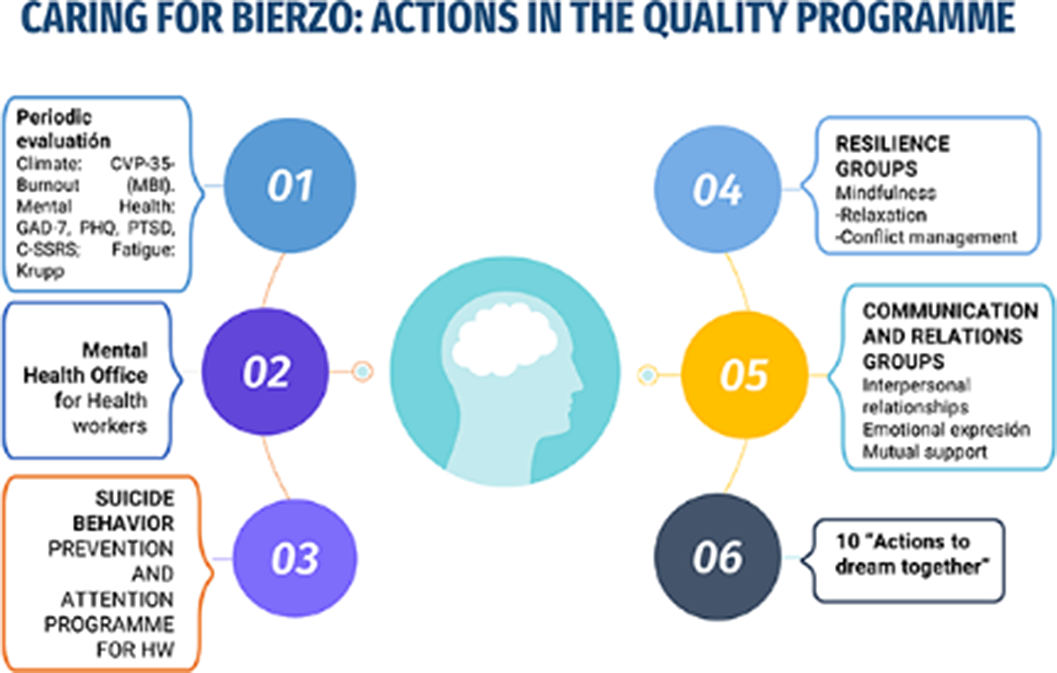
Image 2:

Image 3:
 Conclusions
ConclusionsMental health, fatigue, burnout and motivation of health workers is a complex problem that affect health organizations and quality of services. Mental Health service have an important role in the promotion of wellbeing and prevent burnout in the health system.
Disclosure of InterestNone Declared
Establishing priorities for a Mental Health strategy in Castilla y Leon: The cohesion of professionals and society
- J. M. Pelayo-Terán, Y. Zapico-Merayo, A. M. Saez Aguado, R. Villa Carcedo, Á. Álvaro Prieto
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S540-S541
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The reform of mental health care is a key health policy target. Mental health care provision in Spain is designed with national and regional strategies that stablish the objectives to develop. The Castilla y Leon regional strategy 2022-2026 aim to stabilsh the priorities for objectives and actions with stakeholders from th eregional society.
ObjectivesTo evaluate priorities in the implementation of a Mental Health strategy with the consensus of professionals and society.
MethodsAn initial consensus was achieved with the regional health goverment and local mental health representatives, considering the 2022-2026 national strategy and other mental health plans from nearby regions. Lines in the strategy included transversal lines (part of all the mental health scope) and action lines (priorities focused in one relevant field)
Priorities were stablished by different representatives from mental health and other healthcare professionals, social and educational stakeholders, scientific societies, people with mental health disorders and families. After agreeing to participate in the process, they had to answer an online survey. For each line, they have to score from 0 to 10.
Results500 subjects participated (44% Healthcare workers, 5.8% education or social services, 3.8% Justice, 8,6% workers for associations, 14% Mental Health Care users). All the lines were highly appreciated (mean score >7). Within the transversal lines, the highest score was for the Humanization line (8.81±1.43) and the lowest for the Digitalization line (7.18±1.92). In the Action Lines, the highest score was for Suicide (9.03±11.5) and the lowest for Elder people (8.04±1.94).
Prevention line had higher scores by Education, Justice, Associations and Healthcare professionals and the lowest was for users (F: 2.754; p=0.012). In the Digitalization line the higher scores were in the health professionals and scientific societies and the lowest in the users (F:4.665; p<0.001). In the research, innovation and Training line, the higher scores were for professionals, societies and users and the lowest in the education and justice groups. The only differences found in the Action lines was for the Addiction line, with higher scores for societies, social services, professionals and users and lower in Associations and Justice (F:2.219; p=0,040)
Image:
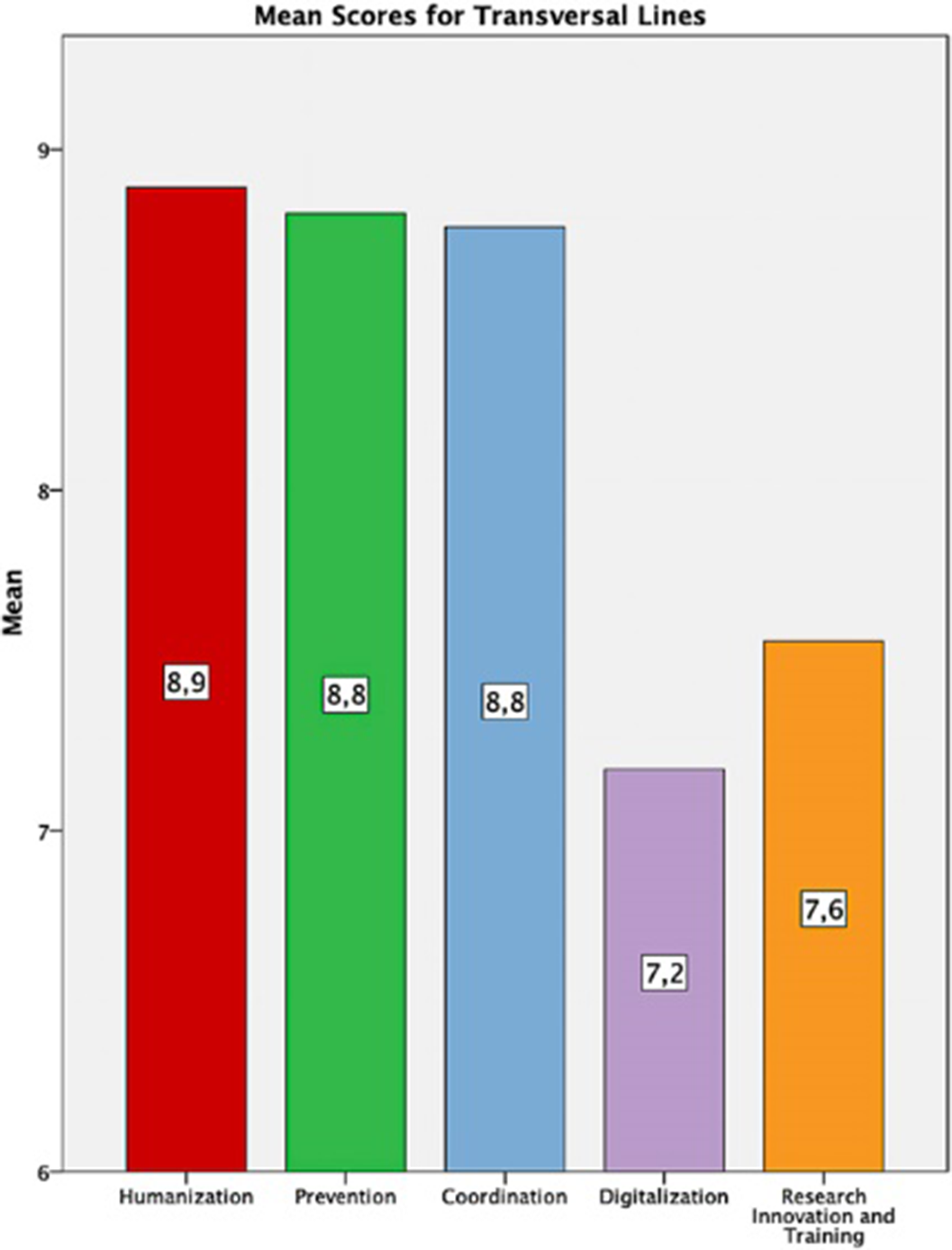
Image 2:
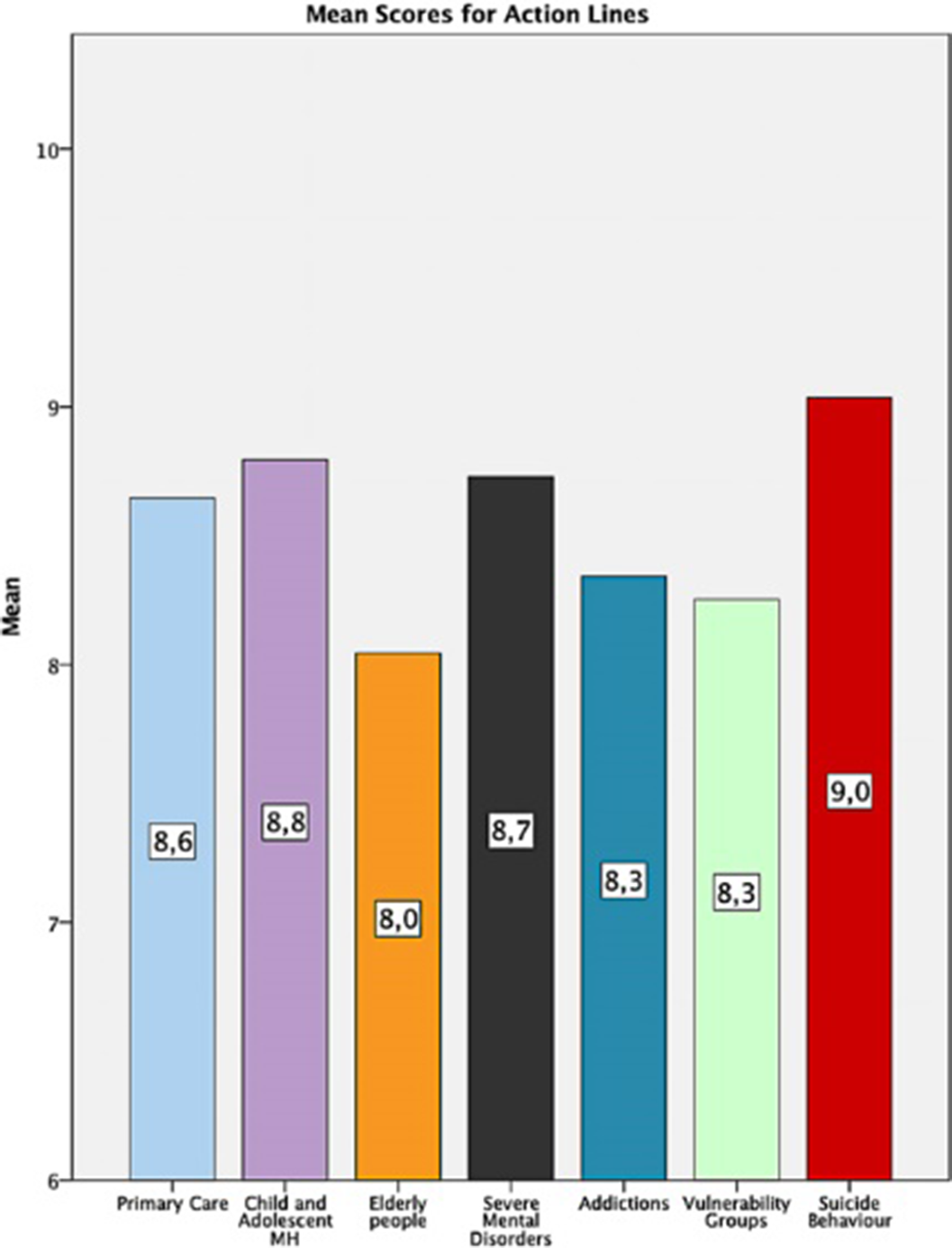 Conclusions
ConclusionsHighest transversal priority for the MH Strategy was Humanization of Mental Health Services, and the most critical action was Suicide prevention. Professionals, Scientific societies and Users considered more important research, innovation and training compared with other society groups, whereas the less important areas for the users were digitalization and prevention users. These priorities will help to design the implementation and schedule for the lines of the Mental Health Strategy in Castilla y León.
Disclosure of InterestNone Declared
A social consensus to prioritize humanization strategies for Mental Health in Castilla y León
- J. M. Pelayo-Terán, Y. Zapico-Merayo, S. Vega-García, M. E. García-Llamas, Z. Gutiérrez-Hervás, A. Sáez-Aguado, M. R. Villa-Carcedo, A. Álvaro-Prieto
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S908-S909
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Humanization in Mental Health is a concept that treat to conceal in the last decades the quality, efficiency and safety of care of complex diseases and conditions with individual values, needs and preferences and involves the patient and society in the decision-making priority.
Objectivesto stablish and evaluate the priorities of different groups of interest in the development of a new humanization plan for mental health
MethodsDuring 2022 a Humanization plan for the Spanish region of Castilla y Leon (2.400.000 habs) was developed with a Delphi model. Participants included 36 stakeholders including mental health services, administration, social services, associations, patients and families. They stablished 32 objectives distributed in 7 strategic lines: 1. “People First” (Rights, Autonomy and Information); 2. “From People to Services” (Participation of users in mental heal services); 3. “Person-Centered-Assistance” 4. “Processes sensible to change” (reduction of coercion); 5. “Human ambient” (Improvement of units, psychosocial interventions). 6. Innovation, training and climate (not evaluated here). 7. “People without marks” (battle against stigma).
Priorities in the lines were stablished by representatives from mental health and other healthcare professionals, social and educational stakeholders, scientific societies, patients and families. After agreeing to participate in the process, they had to answer an online survey. For each line, they have to score it from 0 to 10.
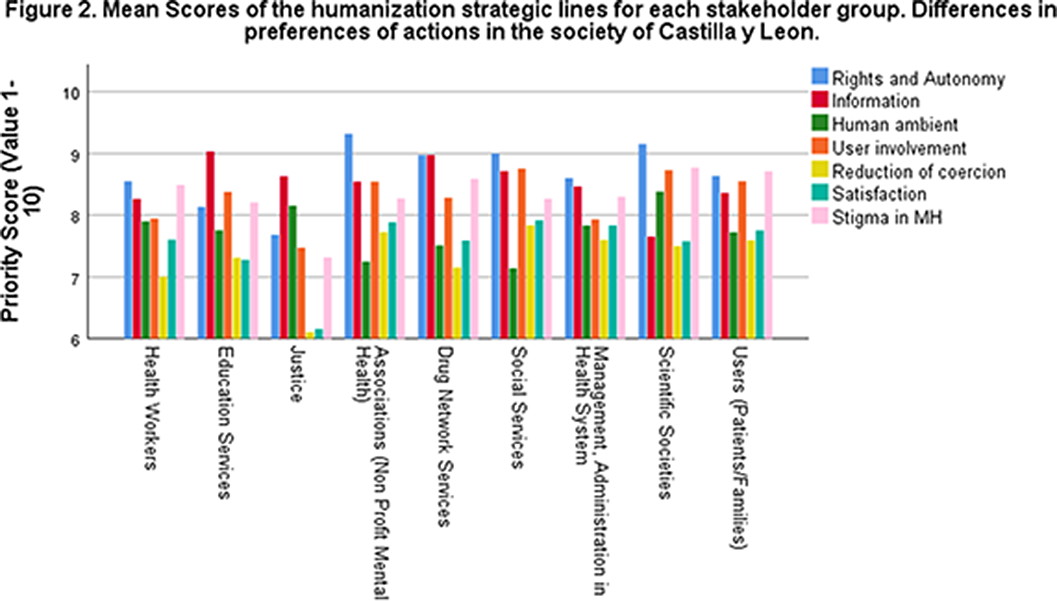
Results500 subjects participated (38.6% Healthcare workers, 14% Mental Health Care users, 9.8% Social Services, 8.8% Associations, 7.8% Drug Services 6% Management of Health System, 5.8% Education Services, 3.8 Justice). Humanization was the most appreciated plan within the mental health plan 2022-2026 in Castilla y Leon (8.81±1.43).
The Highest priority score was given to the Rights (8.68 + 1.54), Information (8.44 + 1.60) and Stigma (8.43 + 1.89) lines and the lowest were the evaluation of satisfaction (7.62 + 1.90) and Reduction of Coercion (7.29 + 2.12). Differences were found between groups. Scores in Rights and Autonomy (F:3.474; p<0.001) were highest in the Associations (9.32 +1.01) and lowest in the Justice group (7.68 + 1.67). In the information line the highest score (F:2.431; p=0,014) was in the Education Services (9.03 +0,94) compared to Scientific Societies (7,65 + 2,13). Highest score for Participation of Users (F:2,968; p=0,003) was in Social Services (8.76 +1.48) compared to Justice (7.47 +1.95). There were differences in the coercion reduction line (F:2.165; p=0,029) but no pairwise differences were found
Image:
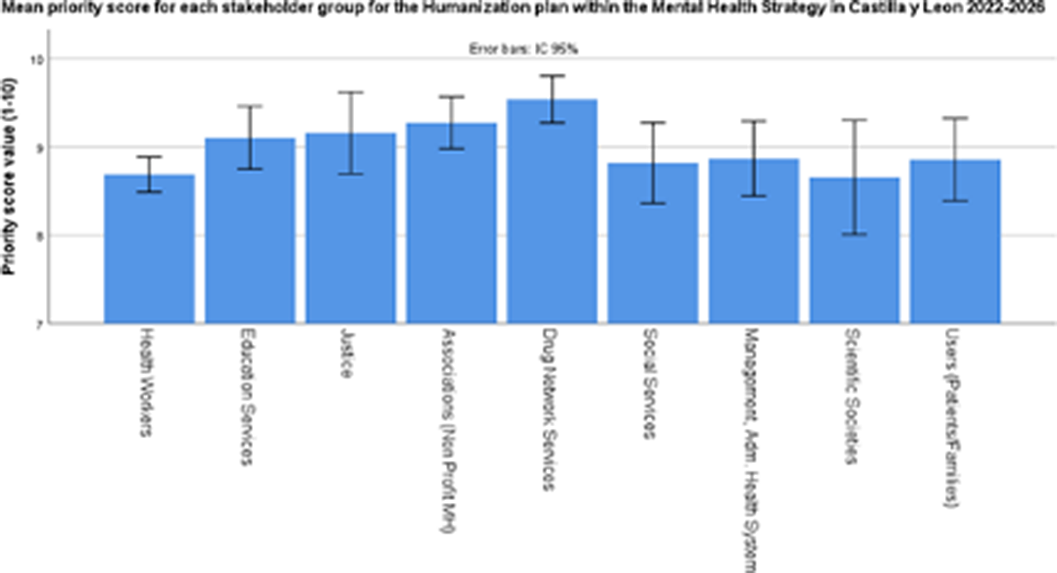
Image 2:
 Conclusions
ConclusionsHumanization approaches are well appreciated by different stakeholders. Priorities in our region start with rights, information and integration and mental health users in the health system and society
Disclosure of InterestNone Declared
Changes in psychiatric emergencies during COVID-19 pandemic lockdown in El Bierzo (Spain)
- Y. Zapico-Merayo, J.M. Pelayo-Terán, S. Vega-García, M.E. Garcia Llamas, R. Landera-Rodríguez, A. Espandian
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S256
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The interest have focused in the effects of COVID-19 in mental symptoms. However, the pandemic and restrictions such as the lockdown decreed in Spain limited access to resources and lead to a change in assistance organization.
Objectivesto compare the incidence and characteristics of psychiatric emergencies during the Spanish 2020 Lockdown with the same period in 2019
MethodsAll the emergencies attended the the emergency room (Hospital El Bierzo) From 01/02/2019 to 30/06/2019 and those from 01/02/2020 to 30/06/2020 were analysed by two senior psychiatrists. Cases were selected if attended by any psychiatric reason. The cases were evalueated identifying ICD-10 diagnosis (according to clinical records and best criteria matching), sociodemographics, factors associated to the emergency and resolution.
Results23360 cases were attended in 2019 (799 psychiatric), 14907 (578) in 2020. That means a 36.19% of reduction in general emergencies and 27.66% in psychiatric emergencies (psychiatric emergencies proportion increased form 3.42% to 4.03%). The reduction started the week just before the lockdown declaration, minimal records coincided with the highest COVID-19 incidence and the recovery starts in early june for psychiatric and late June for general emergencies (figure 1). A decrease of 62.79% of anxiety cases and 45.9% of depresion was observed with no incresaes in any diagnosis. A slight increase in suicide attempts (two cases) was observed.
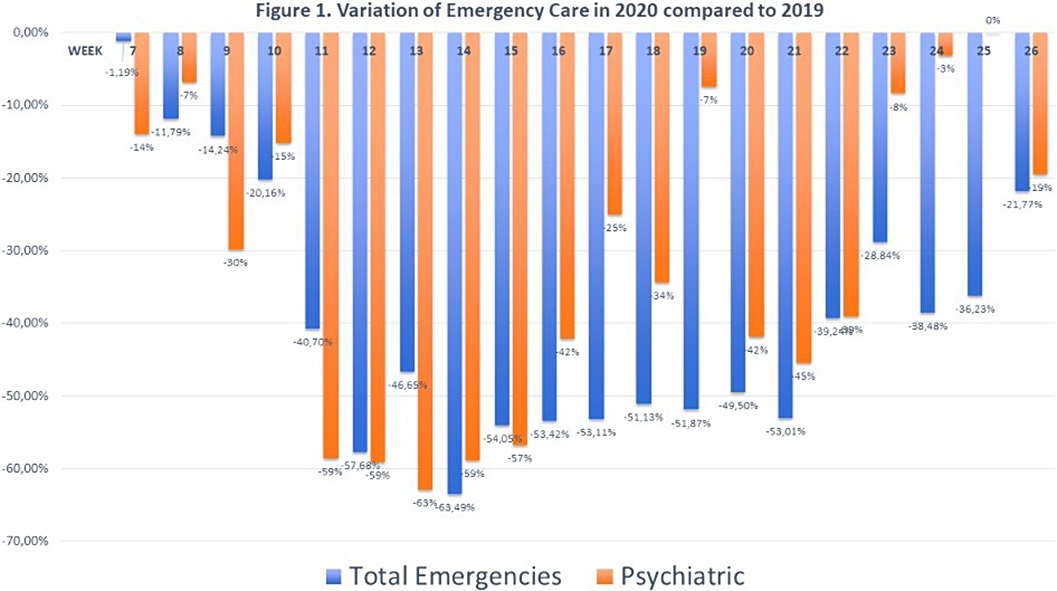 Conclusions
ConclusionsThe lockdown seem to decrease psychiatric emergency care. Only suicidability was maintained/increased during the period. Psychiatry services must be aware of the risk of unattended inicidence that may cause an increase of cases after the lockdown.
DisclosureNo significant relationships.
Clozapine Toxicity in the Setting of COVID-19: A case of differential diagnosis
- J.M. Pelayo-Terán, Y. Zapico-Merayo, S. Vega-García
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S510
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Together with agranulocytosis, fever and immflamatory manifestations are clozapine side effects to be monitorized during initial treatment. In the context of COVID-19 pandemic, implied mechanisms, and symptomatology should be carefully controlled.
ObjectivesTo analyze the clinical analytic and inflammatory chracterisctics the resembles and differenciates clozapine immune response and SARS-CoV-2 infection. To describe a case of clozapine induced fever and pneumonitis during COVID-19 pandemic.
MethodsA case of clozapine-induced pneumonitis during COVID-19 pandemic is described.- A mini-review of clozapine inflamamtory effects, induced-pneumonitis and SARS-CoV-2 was performed.
ResultsA 33 year old afrolatin male started treatment with clozapine up to 250 mg daily. He developed fever and respiratory symptoms in the 11th day of treatment. The exploration revealed pulmonary sounds decreased and 91% basal saturation, making the probable causes viral infection (local incidence of SARS-CoV-2 >800/100000hab), nosocomial bacterial infection or pulmonary thromboembolism. The patient was isolated due to probable COVID-19. Blood tests showed leucocytosis (13400/mcL), Lymphocytopenia (11.8%), high PCR (14.4mg/dL), Ferritine (506.9ng/mL), Fibrinigen (663.83 mg/dL), D-Dimer (1.61mg/dL), and Interleukin-9 /25.8pg/mL). The angioTC revealed a pleural efusion and ground glass infiltrates (figure1). Only after 2 weeks eosinophilia was discovered (88/mcL) After 2 negative consecutieve PCRs for SARS-CoV-2, no imrovement with ampirical antibiotics and all infectious pannels negative, we started decreasing clozapine with improvement of the symptoms and resolution after suspending clozapine completely.
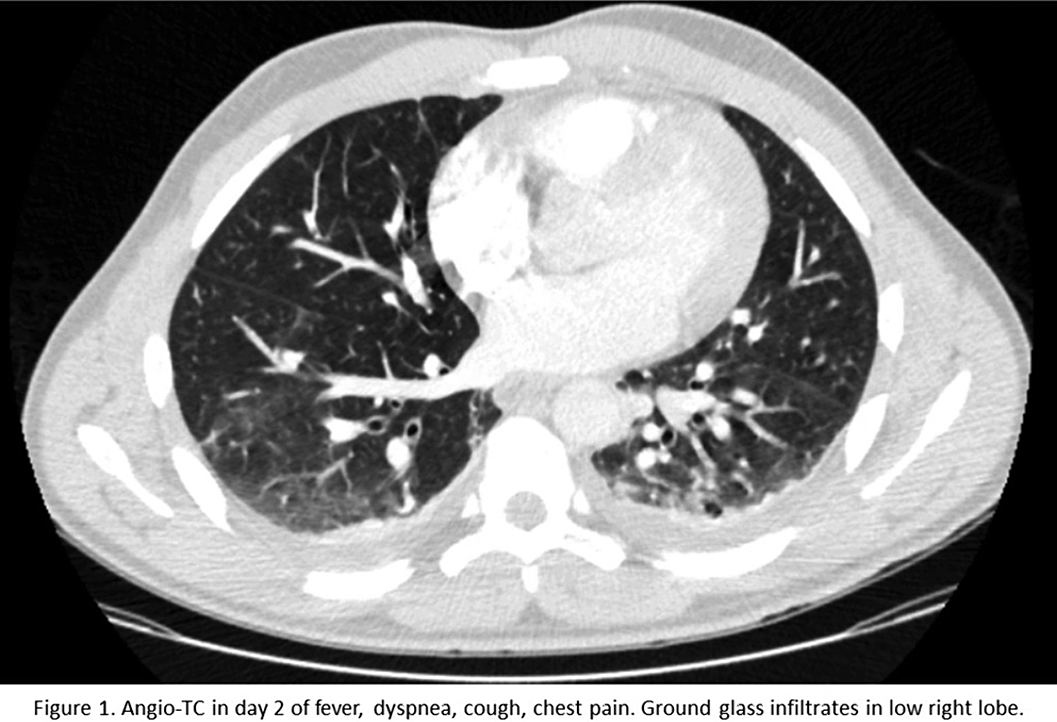 Conclusions
ConclusionsClozapine may induce a generalize inflammatory response mediated by interleukin-6. Patients treated with clozapine may exhibit fever and rarely, insterstitial lung inflammation. The expression of induced pneumonitis resembles viral infections, particularly SARS-CoV-2
DisclosureNo significant relationships.
Factors associated to stigma in mental health workers of Castilla y Leon. The role of burnout and work motivation
- J.M. Pelayo-Terán, Y. Zapico-Merayo, M.E. Garcia Llamas, S. Vega-García, C. López-Zapico, M.R. Villa-Carcedo, Á. Álvaro-Prieto
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S689-S690
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Stigma is one of the most important barriers to help-seeking, treating maintenance and recovery for people suffering mental disorders. These attitudes, when present in mental health workers, may have a negative effect on the quality of health care.
Objectivesto evaluate the levels of stigma in a representative sample of mental health workers and to explore potential modifiable factors associated to stigma attitudes.
MethodsAn online survey was conducted on the mental health workers of Castilla y León (Spain, 2409164 habs) while projecting the 2022 Mental Health Humanization plan in order to asses educational skills, burnout (Maschlach MBI), Professional Quiality of life (CVP-35) and Stigma attitudes (Mental Illness: Cinician’s Attitudes Scales, MICA4) together with sociodemographic and work position variables.
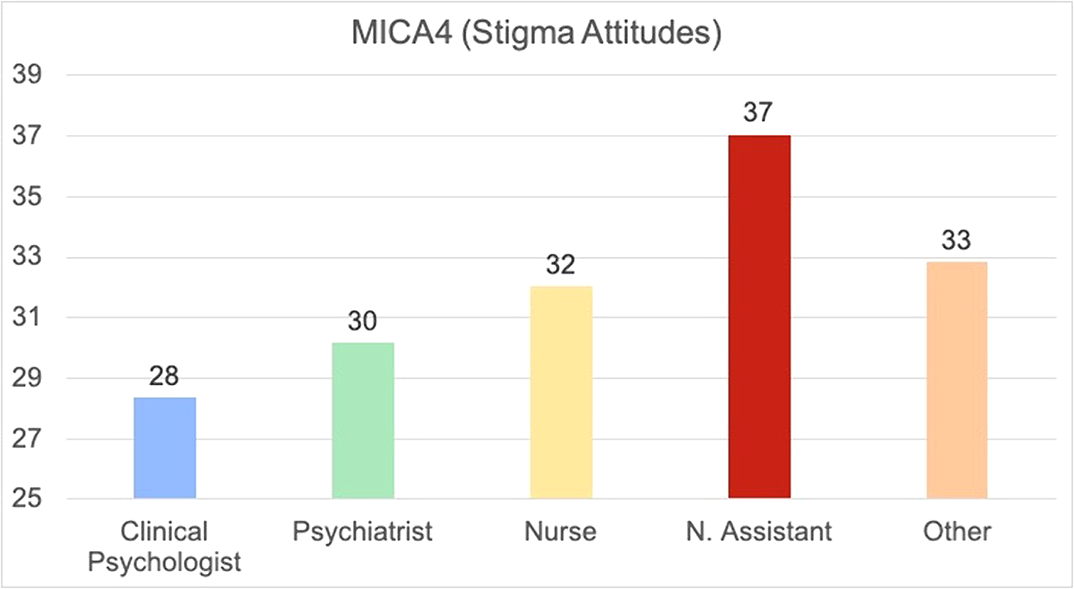
Results193 workers completed completed the survey. Stigma Attitude values of the sample were low (MICA4: 31.71; SD:7.3) and burnout were low or medium (medium Emotional Exhaustion: 19.22; SD8.89; low Depersonalization: 4.91; SD:3.61; Medium Personal Accomplishment: 34,17; 6.3). In the linear regression (R2=0.249; F:11,527; p<0,001), a lower Stigma was predicted by psychologist (Beta:0,207; p=0,003) or psychiatrist position (Beta:0,204; 0,005), Self-efficacy assessed by the item “I am qualified” in the CVP-35 (Beta:-10,144; p=0,023), and a higher stigma was predicted by nurse assistant position (Beta: -0.230; p=0.001), Depersonalization Burnout dimension (Beta:0,351; p<0,001) and years of service (Beta:0.148; p=0,023)
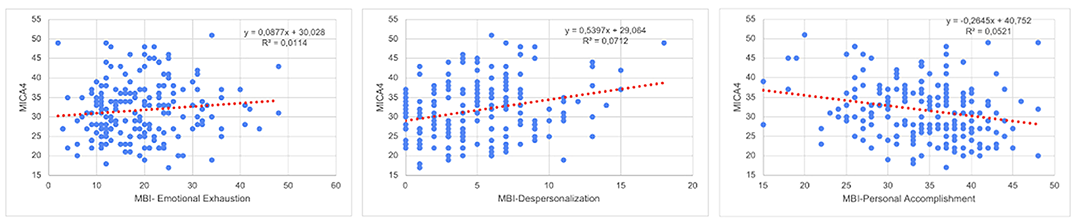
 Conclusions
ConclusionsSome groups of mental workers are more vulnerable to develop stigma attitudes. These, may be increased by fatigue and burnout. Future interventions should determine if reducing burnout and increasing capacitation may be effective in stigma eradication
DisclosureNo significant relationships.














