11 results
Susceptibility results discrepancy analysis between NHSN antimicrobial resistance (AR) Option and NEDSS Base System in Tennessee, July 2020–December 2021
- Carol Davis, Youssoufou Ouedraogo, Christopher Evans, Christopher Wilson
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, p. s104
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: The NHSN Antimicrobial Resistance (AR) Option is an important avenue for acute-care hospitals to electronically report facilitywide antibiogram data. The NEDSS Base System (NBS) is the statewide surveillance system for mandatory reporting of all carbapenem-resistant Enterobacteriaceae (CRE) cases. The state health department (SHD) validated CRE case data reported through the AR Option to assess completeness and accuracy. Methods: NHSN AR Option data from July 2020–December 2021 for 24 facilities were validated by comparing reported CRE and susceptibility results to CRE isolates reported via the NBS. Isolates were matched based on specimen date, sex, birth month and day, pathogen, and specimen source. NHSN susceptibility results were dichotomized as “not resistant” and “resistant” to match the NBS results. Susceptibility discordance (differing proportions of resistant isolates) of matched pairs were evaluated using the McNemar exact test in SAS version 9.4 software. Results: The SHD identified 270 CRE cases from the NHSN and 1,254 unique CRE isolates from the NBS. Of the NHSN events, 72 (26.67%) were matched to the NBS. Among matched isolates, discordance was significant for doripenem (0 resistant isolates in the NHSN vs 13 in the NBS; P < .001) and imipenem (5 resistant isolates in the NHSN vs 23 in the NBS; P < .0001). Discordance was not significant for ertapenem nor meropenem. Sensitivity analyses maximized the match rate at 30.74% (83 matches) when NBS isolates from unknown sources were included and matching factors were specimen date and date of birth ± 1 day, and pathogen. Among all 6,325 CRE isolates in NBS, 290 (4.58%) did not have a specimen source provided. Of all 47,348 NHSN events, 7,624 (16.10%) had impossible patient birthdays. Conclusions: Many NHSN isolates could not be matched to NBS due to either isolates being missing from NBS or to data differences across the systems. This mismatch highlights the need for data validation and standardization at the point of entry for both systems. Discordant susceptibility outcomes raise concerns about using the NHSN as a method for facility and regional antibiogram data.
Disclosures: None
Susceptibility results discrepancy analysis between NHSN Antibiotic Resistance (AR) Option and laboratory instrument data
- Youssoufou Ouedraogo, Christopher Evans, Daniel Muleta, Christopher Wilson
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, p. s66
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: The NHSN Antibiotic Resistance (AR) Option can serve as a useful tool for tracking antibiotic-resistant infections and can aid in the development of inpatient antibiograms. We recently described the frequency of antibiotic suppression in NHSN AR Option data. In this analysis, we describe the effects of suppression on practical uses of the NHSN AR Option, specifically selected agent antibiogram development, and detection of reportable conditions. Methods: Antibiotic susceptibility data were collected from the NHSN AR Option and commercial automated antimicrobial susceptibility testing instruments (cASTI) from 3 hospital networks. Data were obtained from January 1, 2017, to December 31, 2018. The clinical susceptibility data for third-generation cephalosporins and carbapenems against carbapenem-resistant Enterobacterales (CRE), Pseudomonas aeruginosa, and Acinetobacter baumannii were included. Susceptibility results were defined as suppressed when susceptibility results were observed from the laboratory instrument but not from NHSN data. For the overall percentage susceptibility estimation, isolates with <30 susceptibility results were excluded. Percentage susceptibility of NHSN results were compared to their counterparts from cASTI. Results: Of the 852 matched isolates in the primary analysis, 804 had at least 1 suppressed result. Of the 804 isolates, 16.9% were P. aeruginosa, 67.3% by E. coli, and 11.1% by Klebsiella spp. The following pathogen–drug combinations had no difference observed in the percentage susceptible between the 2 systems: ceftazidime tested against P. aeruginosa, ceftriaxone tested against Klebsiella spp, ertapenem tested against Klebsiella spp, imipenem tested against E. coli and P. aeruginosa, and meropenem tested against P. aeruginosa. Significant differences were observed for the following drugs tested against E. coli: ceftazidime (11.1%), cefotaxime (8.6%), and ceftriaxone (8.3%). In the NHSN AR Option, the following isolates showed suppressed results related to their phenotypic case definition: 17 (3%) CRE isolates, 7 (28%) carbapenem-resistant Acinetobacter baumannii (CRAB) isolates, 511 (93.2%) extended spectrum β-lactamase (ESBL) isolates, and 94 (66.7%) carbapenem-resistant Pseudomonas aeruginosa (CRPA) isolates. Conclusions: For select isolates, notably E. coli, we observed a large difference in the percentage of susceptible isolates reported into the NHSN AR Option compared to the cASTI data. This difference significantly limits the ability of the AR Option to create valid antibiograms for select pathogen–drug combinations. Moreover, significant numbers of CRAB, ESBL, and CRPA isolates would not be identified from NHSN AR Option because of suppression. This finding warrants the need for antimicrobial stewardship teams to regularly assess the impact of selective reporting in identifying pathogens of public health importance.
Funding: None
Disclosures: None
Effect of the COVID-19 pandemic on Tennessee hospital antibiotic use
- Youssoufou Ouedraogo, Christopher Evans, Daniel Muleta, Christopher Wilson
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, p. s20
-
- Article
-
- You have access Access
- Open access
- Export citation
-
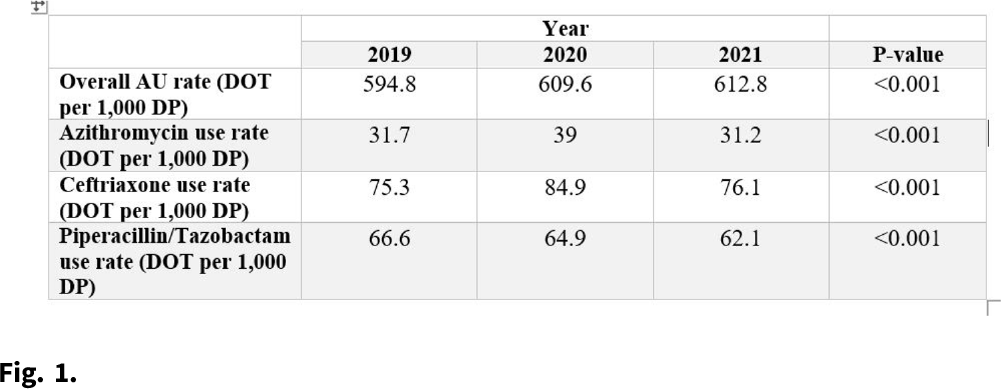
Background: On March 5, 2020, the Tennessee Department of Health (TDH) announced the first case of COVID-19 in the state. Since then, hospitals have been overwhelmed by the spike in respiratory infections. Several studies have attempted to describe the impact of the pandemic on antibiotic prescriptions. The NHSN Antimicrobial Use Option offers a platform for hospitals to report their antibiotic usage. The TDH has established access to hospital antibiotic usage data statewide through an existing NHSN user group. We compared the change in the volume of inpatient antibiotic prescriptions before and during the pandemic. Methods: An ecological study was conducted from January 2019 to December 2021. Aggregated facility-level data from the NHSN Antimicrobial Use Option were used to describe antibacterial use among Tennessee hospitals. Data from facilities that had reported at least 1 month of data during the study period were included in this study. The antimicrobial use rate was calculated by dividing the antimicrobial days of therapy (DOT) by the number of 1,000 days present. Overall antimicrobial use rates as well as specific antimicrobial use rates for azithromycin, ceftriaxone, and piperacillin–tazobactam were compared across years. Results: In total, 55 hospitals reported at least 1 month of data into the NHSN Antimicrobial Use Option during the study period. These hospitals had a median bed size of 140 (range, 12–689). Conclusions: We observed a modest increase in overall antibiotic use during the COVID-19 pandemic in Tennessee facilities. This trend appeared to be primarily attributed to agents used for community-acquired respiratory infections, such as azithromycin and ceftriaxone, earlier in the pandemic. However, both of these agents have fallen to prepandemic use levels during 2021. The fact that overall use increased in 2021 suggests that other agents not analyzed may have contributed to this effect. Further analysis may help determine which agents are responsible for this increase in 2021.
Funding: None
Disclosures: None
Determining the effect of COVID-19 on antibiotic use in long-term care facilities across Tennessee
- Cullen Adre, Youssoufou Ouedraogo, Christopher Evans, Christopher Wilson
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, pp. s21-s22
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Nationally, a decrease in total antibiotic use in nursing homes during the COVID-19 pandemic was observed with an increase in select agents used for respiratory infections. Currently there is minimal data on antibiotic use in long-term care facilities (LTCFs) in Tennessee. To address this issue, the Tennessee Department of Health (TDH) developed a monthly point-prevalence survey of antibiotic use. Utilizing this tool, we sought to determine the effect the pandemic had on antibiotic use in Tennessee LTCFs. Method: We developed a REDCap questionnaire to collect information on selected antibiotics administered in Tennessee LTCFs. Antibiotic use percentage was determined by dividing the number of residents who received an antibiotic on the day of survey by facilities’ average censuses. Data were divided into a prepandemic period (January 2019–February 2020) and a period during the pandemic (March 2020–December 2021). Antibiotic prescriptions were grouped into 4 classes according to their most common uses: Clostridium difficile infections, urinary tract infections, skin and soft-tissue infections (SSTIs), and respiratory infections. Average percentage of residents on antibiotics were compared between study periods. Results: In total, 37 facilities participated in the survey during the prepandemic period and 32 facilities participated during the pandemic period; 14 participated during both periods. The average percentage of residents on antimicrobials before the pandemic was 16.3%, which decreased to 11.5% during the pandemic period (P = .04). During the prepandemic period, 40.2% of antibiotics prescribed were in the common for SSTI category and 38.3% were in the common for respiratory infections category (P = .01); during the pandemic period, 64.3% of antibiotics prescribed were in the common for SSTI category and 45.8% were in the common for respiratory infections category (P = .01). The 3 most prescribed antibiotics in the prepandemic period were amoxicillin (148 prescriptions), doxycycline (140 prescriptions), and levofloxacin (135 prescriptions). The 3 most prescribed antibiotics during the pandemic were doxycycline (141 prescriptions), levofloxacin (125 prescriptions), and trimethoprim–sulfamethoxazole (115 prescriptions). Conclusions: Survey results revealed that antibiotic prescriptions commonly used for respiratory infections increased 7.5% during the pandemic study period. Additionally, the average percentage of residents on antimicrobials fell 4.8% during this period. Both statistics reflect what has been seen nationally with a decrease in antibiotic use with an increase in respiratory antibiotics. This could be due to multiple factors including decreased reporting, a change in healthcare delivery during the pandemic, and facilities seeing an increase of respiratory tract infections. These data will be used to guide future TDH antibiotic stewardship efforts in the long-term care setting.
Funding: None
Disclosures: None
Effects of antibiotic suppression on three healthcare systems’ National Healthcare Safety Network Antibiotic Resistance Option data
- Christopher D. Evans, Matthew D. Estes, Youssoufou Ouedraogo, Daniel Muleta, Marion A. Kainer, Pamela P. Talley
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue 1 / 2021
- Published online by Cambridge University Press:
- 10 November 2021, e47
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Objective:
The National Healthcare Safety Network (NHSN) Antibiotic Resistance (AR) Option is a valuable tool that can be used by acute-care hospitals to track and report antibiotic resistance rate data. Selective and cascading reporting results in suppressed antibiotic susceptibility results and has the potential to adversely affect what data are submitted into the NHSN AR Option. We describe the effects of antibiotic suppression on NHSN AR Option data.
Methods:NHSN AR Option data were collected from 14 hospitals reporting into an existing NHSN user group from January 1, 2017, to December 31, 2018, and linked to commercial automated antimicrobial susceptibility testing instruments (cASTI) that were submitted as part of unrelated Tennessee Emerging Infections Program surveillance projects. A susceptibility result was defined as suppressed if the result was not found in the NHSN AR Option data but was reported in the cASTI data. Susceptibility results found in both data sets were described as released. Proportions of suppressed and released results were compared using the Pearson χ2 and Fisher exact tests.
Results:In total, 852 matched isolates with 3,859 unique susceptibilities were available for analysis. At least 1 suppressed antibiotic susceptibility result was available for 726 (85.2%) of the isolates. Of the 3,859 susceptibility results, 1,936 (50.2%) suppressed antibiotic susceptibility results were not reported into the NHSN AR option when compared to the cASTI data.
Conclusion:The effect of antibiotic suppression described in this article has significant implications for the ability of the NHSN AR Option to accurately reflect antibiotic resistance rates.
Determining Core Element Achievement in Long-Term Care Facilities Across Tennessee
- Cullen Adre, Youssoufou Ouedraogo, Christopher David Evans, Amelia Keaton, Marion Kainer
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, p. s89
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: In 2017, a new antimicrobial stewardship standard was established by the Joint Commission that requires long-term care facilities (LTCFs) to have an antimicrobial stewardship program (ASP) based on current scientific literature. The Tennessee Department of Health (TDH) team sought to ascertain the current state of ASPs across Tennessee and to assist programs with implementation strategies. Utilizing a Centers for Medicaid and Medicare Services’ Civil Monetary Penalties grant, the TDH purchased copies of the National Quality Partners Playbook for Antibiotic Stewardship in Post-Acute and Long-Term Care to provide to LTCFs as incentive to complete a survey that would evaluate their current adoption of core elements. Methods: A self-administered questionnaire on ASP practices was developed and distributed to LCTFs. This survey expanded upon questions from the NHSN 2018 LTCF annual survey. These questions pertained to actionable items facilities are taking to achieve core elements. Achievement of the CDC’s 7 core elements of ASPs was determined based upon a combination of 1 or more responses to the survey questions. The percentage of LTCFs achieving each ASP core element at the regional and statewide level was determined. We also calculated the percentage of LTCFs that achieved all 7 elements versus 5 or more core elements. The analyses and visualizations were performed using SAS 9.4 and Tableau software. Results: Currently, 88 of 316 licensed LTCF facilities in Tennessee have participated in the survey. All regions were represented by EMS region. Based on the results of our survey, 100% of participating facilities have achieved at least 5 core elements, and 78% of participating facilities have achieved all 7 core elements. The core element with the lowest achievement was Accountability at 89%, and reporting and action had the highest achievement (100%). Conclusions: Early results suggest that LTCFs across Tennessee have active ASPs with strong core element achievement. However, we received responses from only 27% of licensed LTCFs. Minimal data are available regarding the current state of LTCF ASPs in Tennessee, and data will continue to be collected and analyzed. Participation may be limited to those already actively engaged in public health efforts, including antimicrobial stewardship. LTCFs that have participated in the initial evaluation will be surveyed at 6 months and 12 months after receipt of playbooks to evaluate their ASP progression and NQP Playbook utilization.
Funding: None
Disclosures: None
Determining Antibiotic Use in Long-Term Care Facilities Across Tennessee
- Cullen Adre, Youssoufou Ouedraogo, Christopher David Evans, Amelia Keaton, Marion Kainer
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s185-s186
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Antibiotic stewardship is an area of great concern in long-term care facilities nationwide. The CDC promotes 7 core elements of antimicrobial stewardship. Based on information obtained from the Infection Control Assessment and Response (ICAR) Program, the 2 core elements most infrequently achieved by LTCFs are tracking and reporting. Currently, minimal data are available on antibiotic use (AU) in LTCFs in Tennessee. To address both issues, the Tennessee Department of Health (TDH) developed a monthly antibiotic use (AU) point-prevalence (PP) survey to provide LTCFs with a free tool to both track and report their AU and to gather data on how LTCFs are using antibiotics. Methods: We used REDCap to create a questionnaire to collect information on selected antibiotics administered in Tennessee LTCFs. This self-administered survey was promoted through the TDH monthly antimicrobial stewardship and infection control (ASIC) call as well as at various conferences and speaking engagements across the state. Antimicrobial stewardship leads for each facility were targeted. Antibiotics were grouped into 4 classes according to their indications: C. difficile infections, urinary tract infections, skin and soft-tissue infections (SSTIs) and respiratory infections. We determined AU percentage by dividing the number of days of therapy for a drug by a facility’s average census. Individualized reports are provided to each participating facility on a quarterly basis. Results: Currently, 16 facilities have participated in the survey. Overall, 40.7% of antibiotics prescribed were in the common for SSTI category and 39.3% were common for respiratory infections. The top 33 most commonly prescribed antibiotics were amoxicillin (156 days of therapy [DOT]), nitrofurantoin (92 DOT), and levofloxacin (88 DOT). The average percentage of residents on antimicrobials on the day of survey was 12.3%; within this group, 57% of antibiotics were initiated in the LTCF, whereas 43% were present upon admission. Conclusions: Early results from the TDH AU PP survey revealed that drugs commonly used for SSTIs and respiratory infection were the most common antibiotic prescriptions and a potential area of focus for TDH’s antimicrobial stewardship efforts. None of the 3 most frequently prescribed antibiotics, however, fall under the SSTI indication, despite SSTI being the most commonly prescribed indication based on the survey’s evaluation metrics. This finding could be related to the larger number of antibiotics that fall under the SSTI indication. Preliminary data are being used to guide the direction of TDH’s future ASIC calls to better suit disease states, which have room for improvement.
Funding: None
Disclosures: None
Effects of Susceptibility Result Suppression on National Healthcare Safety Network Antibiotic Resistance Option Data
- Matthew Estes, Youssoufou Ouedraogo, Christopher David Evans, Daniel Muleta, Cullen Adre, Amelia Keaton, Marion Kainer
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s33-s34
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: The National Healthcare Safety Network’s (NHSN) Antibiotic Resistance (AR) Option offers hospitals a way to report antibiotic resistance data from their facility’s laboratory information system and create facility-specific antibiograms. Suppression of select antibiotic susceptibility results may be used by antibiotic stewardship teams to prevent unnecessary use of broad-spectrum therapies by not making those susceptibilities available to providers. To be of use, antibiograms should offer a complete picture of antibiotic resistance. We wanted to understand the impact of data suppression. Methods: A retrospective cross-sectional study was conducted including data from 2017 and 2018. The clinical susceptibility data for cefotaxime, ceftriaxone, ceftazidime, ertapenem, imipenem, and meropenem against carbapenem-resistant Enterobacteriaceae (CRE), Pseudomonas aeruginosa (CRPA), Acinetobacter baumannii (CRAB), and extended-spectrum β-lactamase–producing Enterobacteriaceae (ESBL) were collected from commercial antimicrobial susceptibility testing instruments (cASTI) in 3 Tennessee healthcare networks that also report to the NHSN AR Option. These data were linked to the NHSN data using 4 keys: date of birth, isolate collection date, pathogen, and specimen source. An isolate was defined as suppressed when susceptibility results were observed from the cASTI but not in NHSN. The proportions of suppressed results were calculated and stratified by genus, facility, and antibiotic. Results: Overall, 1,009 isolates were matched between the NHSN AR data and the laboratory test results. Of these, 4.1% were CRAB, 23.3% were CRPA, and 72.6% were Enterobacteriaceae. In total, 4,948 susceptibility results were available from cASTIs. Suppressed results in NHSN data were observed in 918 isolates (91.0%) and accounted for 2,797 results (56.6%). Of the 817 isolates tested against imipenem, 18.7% were found to be suppressed. Moreover, 100%, 57.9%, and 8.6% of imipenem tests against CRAB, CRPA, and Enterobacteriaceae, respectively, were suppressed. Of the suppressed results, 38.3%, 3.6%, and 58.1% were susceptible, intermediate, and resistant respectively. Of the 363 isolates tested against meropenem, 48.2% were found to be suppressed. In addition, 12.2%, 53.0%, and 52.2% of meropenem tests against CRAB, CRPA, and Enterobacteriaceae, respectively, were suppressed. Of the suppressed results, 47.4%, 11.4%, and 41.1% were susceptible, intermediate, and resistant, respectively. Conclusions: A large proportion of isolates had at least 1 analyzed antibiotic suppressed within the NHSN AR Option. It will be important to develop and implement strategies to ensure that nonsuppressed data are available to be reported to the NHSN AR module.
Funding: None
Disclosures: None
Population-based assessment of patient and provider characteristics influencing pediatric outpatient antibiotic use in a high antibiotic-prescribing state
- Sophie E. Katz, Milner Staub, Youssoufou Ouedraogo, Christopher D. Evans, Marion A. Kainer, Marie R. Griffin, Ritu Banerjee
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue 3 / March 2020
- Published online by Cambridge University Press:
- 15 January 2020, pp. 331-336
- Print publication:
- March 2020
-
- Article
- Export citation
-
Objective:
To identify patient and provider characteristics associated with high-volume antibiotic prescribing for children in Tennessee, a state with high antibiotic utilization.
Design:Cross-sectional, retrospective analysis of pediatric (aged <20 years) outpatient antibiotic prescriptions in Tennessee using the 2016 IQVIA Xponent (formerly QuintilesIMS) database.
Methods:Patient and provider characteristics, including county of prescription fill, rural versus urban county classification, patient age group, provider type (nurse practitioner, physician assistant, physician, or dentist), physician specialty, and physician years of practice were analyzed.
Results:Tennessee providers wrote 1,940,011 pediatric outpatient antibiotic prescriptions yielding an antibiotic prescribing rate of 1,165 per 1,000 population, 50% higher than the national pediatric antibiotic prescribing rate. Mean antibiotic prescribing rates varied greatly by county (range, 39–2,482 prescriptions per 1,000 population). Physicians wrote the greatest number of antibiotic prescriptions (1,043,030 prescriptions, 54%) of which 56% were written by general pediatricians. Pediatricians graduating from medical school prior to 2000 were significantly more likely than those graduating after 2000 to be high antibiotic prescribers. Overall, 360 providers (1.7% of the 21,798 total providers in this dataset) were responsible for nearly 25% of both overall and broad-spectrum antibiotic prescriptions; 20% of these providers practiced in a single county.
Conclusions:Fewer than 2% of providers account for 25% of pediatric antibiotic prescriptions. High antibiotic prescribing for children in Tennessee is associated with specific patient and provider characteristics that can be used to design stewardship interventions targeted to the highest prescribing providers in specific counties and specialties.
Analysis of a high-prescribing state’s 2016 outpatient antibiotic prescriptions: Implications for outpatient antimicrobial stewardship interventions
- Milner B. Staub, Youssoufou Ouedraogo, Christopher D. Evans, Sophie E. Katz, Pamela P. Talley, Marion A. Kainer, George E. Nelson
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue 2 / February 2020
- Published online by Cambridge University Press:
- 22 November 2019, pp. 135-142
- Print publication:
- February 2020
-
- Article
- Export citation
-
Objective:
To identify prescriber characteristics that predict antibiotic high-prescribing behavior to inform statewide antimicrobial stewardship interventions.
Design:Retrospective analysis of 2016 IQVIA Xponent, formerly QuintilesIMS, outpatient retail pharmacy oral antibiotic prescriptions in Tennessee.
Setting:Statewide retail pharmacies filling outpatient antibiotic prescriptions.
Participants:Prescribers who wrote at least 1 antibiotic prescription filled at a retail pharmacy in Tennessee in 2016.
Methods:Multivariable logistic regression, including prescriber gender, birth decade, specialty, and practice location, and patient gender and age group, to determine the association with high prescribing.
Results:In 2016, 7,949,816 outpatient oral antibiotic prescriptions were filled in Tennessee: 1,195 prescriptions per 1,000 total population. Moreover, 50% of Tennessee’s outpatient oral antibiotic prescriptions were written by 9.3% of prescribers. Specific specialties and prescriber types were associated with high prescribing: urology (odds ratio [OR], 3.249; 95% confidence interval [CI], 3.208–3.289), nurse practitioners (OR, 2.675; 95% CI, 2.658–2.692), dermatologists (OR, 2.396; 95% CI, 2.365–2.428), physician assistants (OR, 2.382; 95% CI, 2.364–2.400), and pediatric physicians (OR, 2.340; 95% CI, 2.320–2.361). Prescribers born in the 1960s were most likely to be high prescribers (OR, 2.574; 95% CI, 2.532–2.618). Prescribers in rural areas were more likely than prescribers in all other practice locations to be high prescribers. High prescribers were more likely to prescribe broader-spectrum antibiotics (P < .001).
Conclusions:Targeting high prescribers, independent of specialty, degree, practice location, age, or gender, may be the best strategy for implementing cost-conscious, effective outpatient antimicrobial stewardship interventions. More information about high prescribers, such as patient volumes, clinical scope, and specific barriers to intervention, is needed.
Annual population dynamics of mango fruit flies (Diptera: Tephritidae) in West Africa: socio-economic aspects, host phenology and implications for management
- Jean-François Vayssières, Antonio Sinzogan, Appolinaire Adandonon, Jean-Yves Rey, Elhadj Oumar Dieng, Koumandian Camara, Morodian Sangaré, Sylvain Ouedraogo, N’klo Hala, Adama Sidibé, Youssouf Keita, Guy Gogovor, Sam Korie, Ousmane Coulibaly, Cinthia Kikissagbé, Alliance Tossou, Max Billah, Koffi Biney, Oswald Nobime, Paterne Diatta, Robert N’Dépo, Moussa Noussourou, Lanciné Traoré, Symphorien Saizonou, Manuele Tamo
-
- Article
- Export citation
-
Introduction. Losses in West African commercial mango orchards due to fruit fly infestations have exceeded 50% by the middle of the crop season since 2005, resulting in considerable income loss for the growers. Materials and methods. In 2009, weekly monitoring of adult fruit fly species of economic significance was carried out in eight West African countries at 12 sites across five agro-ecological zones: (i) Humid Forest, (ii) Guinean savanna, (iii) Southern Sudan, (iv) Northern Sudan, and (v) Sahelian. Trapping was performed using methyl eugenol and terpinyl acetate in 288 Tephri-traps, targeting Bactrocera invadens and Ceratitis cosyra. Results. The data showed that B. invadens was present throughout the year in the Forest zone, abundant for 7 months, with a peak in May at the end of the mango season, C. cosyra being totally absent. In the Guinean savanna zone, B. invadens was abundant for 6-7 months, with a peak at the beginning of June coinciding with the season, with a few C. cosyra. In the Southern Sudan zone, B. invadens was abundant for 6 months, with a peak in mid-June during the season, C. cosyra peaking in April. In the Northern Sudan zone, B. invadens was abundant for 5 months, with a peak at the end of June at the end of the season, C. cosyra peaking in May. In the Sahelian zone, B. invadens was abundant for 4 months, peaking in August during the season, C. cosyra peaking just before. These preliminary results showed that the exotic species, B. invadens, was present at high levels [mean peak of 378 flies per trap per day (FTD)] in all agro-ecological zones, while the native species, C. cosyra, preferred the drier zones of West Africa, with lower population levels (mean peak of 77 FTD). Conclusion. Detection trapping of male flies with parapheromones is a useful indicator of field population levels and could be used to deploy control measures (IPM package) in a timely manner when the Economic Injury Level is reached. Control strategies for these quarantine mango fruit fly species are discussed with respect to agro-ecological zones and the phenological stages of the mango tree.




