Introduction
Research concerning older lesbian, gay, bisexual and trans (LGBT) people is an expanding field (see Fredriksen-Goldsen et al. Reference Fredriksen-Goldsen and Muraco2010; Ward, Rivers and Sutherland Reference Ward, Rivers and Sutherland2012). Much of this research considers the health and social care needs of older LGBT people (Addis et al. Reference Addis, Davies, Greene, MacBride-Stewart and Shepherd2009; Ward Rivers and Sutherland Reference Ward, Rivers and Sutherland2012). However, the distinct needs of older LGBT individuals remain neglected within mainstream care policies and practice (Concannon Reference Concannon2009; Hafford-Letchfield Reference Hafford-Letchfield2008; Ward, Rivers and Sutherland Reference Ward, Rivers and Sutherland2012). Although much of our analysis focuses on issues that are common to older LGBT care home residents, we acknowledge that whilst LG and B constitute expressions of sexuality, trans is an umbrella term that encompasses a range of expressions of gender from how individuals identify and present through to gender re-assignment following surgery and/or medical intervention. Indeed trans can involve those who describe as ‘gender fluid’, ‘gender-queer’, or even not definable or reducible to a gender (but defined by some other preferred quality/attribute). It also needs acknowledging that the range of sexualities is also available to trans individuals. For example, it is possible to identify as a gay, bisexual, heterosexual or sexually fluid transman.
There is also little research addressing cultural sensitivity within care environments that LGBT people may need to access. Institutional and historical barriers (Moran et al. Reference Moran, Skeggs, Tyrer and Korteen2004) may mean the oldest generations of LGBT people are reluctant to disclose their sexuality or gender identity (Witten Reference Witten2008). Despite significant social and legal changes, older LGBT people are likely to manage their personal networks in ways that minimise vulnerability to discrimination and stigma (Almack, Seymour and Bellamy Reference Almack, Seymour and Bellamy2010). Moving into care involves additional challenges to identity for older LGBT individuals adjusting to new relationships with fellow residents and care staff (Willis et al. Reference Willis, Maegusuku-Hewett, Raithby and Miles2016).
In light of the concerns just described, the research on which this article is based was motivated by three concerns. First, comparatively little research has been done in the United Kingdom (UK) addressing practitioners’ perspectives on meeting the distinct needs of old(er) LGBT people living in care homes. A study in Wales exploring the provision of inclusive care for older LGB adults in residential and nursing environments is a notable exception (see Willis et al. Reference Willis, Maegusuku-Hewett, Raithby and Miles2016). Second, we wanted to explore how well-equipped, in an era of greater tolerance towards sexual difference and non-normative genders, care homes and their staff are in terms of the attitudes, knowledge, skills and the support measures required to enable them to meet the needs of LGBT residents. Third, we wanted to provide information that could help staff and homes take practical steps to advance the inclusion of LGBT residents.
To address the above knowledge gaps, we discuss the results of a survey comprising 187 care home staff in England (conducted Autumn 2013) who responded to a questionnaire designed to elicit attitudes, knowledge and practices apropos LGBT residents. On the basis of the results, we advance three inter-related arguments. First, whilst employees’ attitudes generally indicate a positive disposition towards LGBT residents, this is not matched by staff ability to recognise such individuals and knowledge of the issues and policies affecting LGBT residents/people (see also Concannon Reference Concannon2009). Statements such as, ‘We don't have any at the moment’ and ‘I/we treat them all the same’ were common refrains in responses to the more open-ended items in our survey. Such statements indicate the regulatory force of heteronormativity (a form of discourse that assumes heterosexuality as the norm) and cisgenderism (thinking that assumes that people (should) comply with the gender into which they were born/socialised), both of which can deny LGBT residents’ identities. Second, failure to recognise LGBT residents’ distinct health and social care needs means that they may be subject to a uniform service, which presumes a heterosexual past and cisgender status and is thus likely to reinforce inequality and exacerbate invisibility. Equal treatment is not merely a perceived absence of discrimination in ‘treating everyone the same’. It also requires, inter alia, proactive measures to address unconscious assumptions and habitual behaviours (Almack and National Council for Palliative Care Organization (NCPC) 2016; NCPC 2012), which may make LGBT people feel less inclined to approach, use or feel comfortable in care home environments. Third, it appears that LGBT residents are obliged to depend largely on the goodwill, knowledge and professional reflection of individual staff to meet their distinct care and personal needs. Indeed, we make several observations concerning a form of reflexivity that is practised by care staff professing faith that enables them to manage religious antipathy to LGBT status. However, goodwill and reflexivity are necessary but not sufficient conditions for more collective forms of good practice required to secure equality of outcomes. Failure to convert staff goodwill into strategically informed practice is more likely to prevent inclusion and risks compromising human rights that concern avoidance of degrading treatment and discrimination and enabling freedom of self-expression and association.
Context: older people, residents and care homes
Theories of ageing are well documented (see Johnson, Bengtson and Coleman Reference Johnson, Bengtson and Coleman2005) and are beyond the scope of this article. However, given the nature of our enquiry, we are concerned with longevity. Longevity is increasing globally but especially in resource-rich countries, with the majority of deaths, unsurprisingly, occurring over the age of 65 and mortality rates highest among those aged over 85 (Holloway and Taplin Reference Holloway and Taplin2013). Estimating the size and demographic trends of the ageing LGBT population is difficult. There are no official British/UK statistics on LGBT individuals of any age group. A commonly used estimate is that 5–7 per cent of the population identifies as LGBT (see Aspinall Reference Aspinall2009). On this basis, there are likely to be between 520,000 and 728,000 people, aged 65 and over, who are LGBT (using the UK 2011 Census figures). Such demographic shifts signal an older, more dependent population. Those requiring long-term care are not a homogeneous group and the demand for long-term care provided in care homes is increasing (Select Committee on Public Service and Demographic Change 2013).
In the UK, of the 10.3 million people aged 65 or over, 4.5 per cent of these individuals (still more than 500,000 people) were accommodated in a communal home (Office for National Statistics (ONS) 2014). This official category could accommodate anyone who is living in a non-familial shared home but consists mainly of those accommodated in aged care facilities.
Individuals aged 85 and over (ONS 2013) represent 58 per cent of the population in care homes accommodating older people (ONS 2014). Nearly one in ten men and one in five women (20 per cent) aged 85 or over live in a communal establishment (ONS 2011) where female residents outnumber male residents by a ratio of nearly 3:1 (ONS 2014).
The UK care sector accommodating older people consists of various provisions that include ‘informal’ care at home by significant others, domiciliary care from local authorities (often self-funded following means-testing) and residential, nursing and mixed residential and nursing homes (see National Health Service (NHS) 2015). Whilst residential care homes cater largely for infirm people with considerable autonomy but needing some support with everyday physical activities, nursing homes usually accommodate individuals with more complex needs resulting from more severe limitations on physical and cognitive capacities (NHS 2015). The Social Care Act 2008 requires nursing homes to ensure that a registered nurse is on duty at all times. Mixed homes, largely in the private or voluntary-owned sector, have emerged in response to diverse and changing needs (Help the Aged 2007) and could prevent the fatal consequences of transferring residents to a nursing home if/when frailty, morbidity and dependency increase.
Moreover, aged care is largely privatised with 350,000 (70 per cent) of the 500,000 beds available in the UK being located in for-profit homes (Laing Reference Laing2014). Whilst some residents remain entitled to NHS services (and the NHS both provides and purchases services in care homes), it has been calculated that 45 per cent of individuals accommodated in residential care and 48 per cent of individuals in nursing homes for older people fund entirely their own placements (Care Quality Commission 2012). Such placements are commonly funded from the sale of assets over the £21,000 threshold set by the British Government in 2006. Even those individuals whose places are funded by the local authority may be required to make some contribution to their care or a top-up fee levied by an independent or private home over what the local authority will pay. The local authority has to step in when individuals’ private resources fall beneath the £21,000 threshold (Miller, Bunnin and Rayner Reference Miller, Bunnin and Rayner2013). It is likely that most LGBT individuals, many of whom will not have borne the expense of child-rearing, could be paying for/towards their care.
The influence of organisational cultures, their relationship to the quality of care and residents’ experiences of this is increasingly acknowledged but to date little research has focused on this matter (Killett et al. Reference Killett, Burns, Kelly and Brooker2016). Killett et al. highlight the need to investigate how the ethos of a care home culture (e.g. provision of person-centred care) and unconscious assumptions and behaviour interact to inform practice. There appears, however, to be little published research investigating the relationship between person-centred care and equality-led approaches. Existing work tends to treat residents as a homogenous group, rarely mentions LGBT individuals and supports anecdotal evidence concerning their invisibility. There is evidence that LGBT people have additional concerns about care home environments (Almack, Moss and Smith Reference Almack, Moss, Smith, Fish and Karban2015; Stein, Beckerman and Sherman Reference Stein, Beckerman and Sherman2010), anticipating that staff and residents could be hostile, ignore specific needs, deny identity, and effectively reinforce LGBT exclusion and oppression (Hafford-Letchfield Reference Hafford-Letchfield2008).
Meeting the needs of older LGBT care home residents – ageism, heteronormativity and cisgenderism: the literature
Whilst we did not have the resources to carry out a full systematic review nor did we find one in existence, nonetheless, we are aware that there is scant published literature pertaining to the issues of older LGBT individuals’ experiences in care homes. Thus, our aim was solely to provide a contextual background drawing on a body of research related to the health and social care needs of older LGBT people. However, the past 20 years have witnessed a decisive shift in official and public attitudes towards sexual difference and gender plurality in Britain (see Weeks Reference Weeks2007). Most notably, legislative advances include protection against discrimination of LGBT individuals in the Equalities Act 2010 (which also outlaws age discrimination) and the Marriage (Same-sex Couples) Act 2013, which extended civil marriage to lesbian and gay citizens. Despite these gains in rights and tolerance (albeit short of full equality and parity of esteem), care settings may still not recognise concerns unique to older LGBT people.
In general terms, older people's sexuality tends to be made invisible. Ageist and heteronormative and/or cisgenderist assumptions combine to render LGBT individuals doubly/triply invisible as old and post-sexual, though still marked as different (Westwood Reference Westwood2015). Individuals identifying as trans might be misrecognised as cisgender (misgendered) and, even if recognised, could be treated as a problem category (Witten and Whittle Reference Witten and Whittle2004). LGBT residents have spoken of living in fear and the necessity of ‘selective concealment’ of their identities (not always successful) from residents and staff (Westwood Reference Westwood2015). Such thinking likely reflects the operation of heteronormativity or homophobia/biphobia – fear and ignorance of sexual difference that can animate hostility, prejudice and discrimination. Such neglect in relation to trans individuals is likely the result of transphobia associated with cisgenderist discourse. Such discourses have been adduced to explain LGBT individuals’ underuse of end-of-life care services (Almack and NCPC Reference Almack2016; Almack, Moss and Smith Reference Almack, Moss, Smith, Fish and Karban2015; Stein and Almack Reference Stein, Almack, Ward, Rivers and Sutherland2012).
However, more sensitive care for LGBT residents could be provided by ensuring that decisions concerning sexuality and its expression are led by residents’ expressed needs rather than staff anxieties (Simpson et al. Reference Simpson, Horne, Brown, Brown Wilson, Dickinson and Torkington2015). As discussed later, more inclusive care would also involve acknowledging LGBT individuals as integral to the home as a diverse community and culture, e.g. in terms of images in publicity materials, reading materials made available and maintaining links with LGBT community contacts/organisations (see Hafford-Letchfield Reference Hafford-Letchfield2008; Help the Aged 2007).
The small but growing body of research has highlighted various forms of LGBT invisibility in aged-care facilities (see Bell et al. Reference Bell, Bern-Klug and Kramer2010; Bellamy and Gott Reference Bellamy and Gott2013; Hughes, Harold and Boyer Reference Hughes, Harold and Boyer2011; Johnson et al. Reference Johnson, Jackson, Arnette and Koffman2005; Knochel, Quam and Croghan Reference Knochel, Quam and Croghan2011; Neville et al. Reference Neville, Adams, Bellamy, Boyd and George2014; Phillips and Marks Reference Phillips and Marks2008; Sullivan Reference Sullivan2014; Westwood Reference Westwood2015; Willis et al. Reference Willis, Maegusuku-Hewett, Raithby and Miles2016). This work highlights the importance of: recognising diversity and needs (resulting from combined influences of gender, sexuality, class and race); avoidance of stereotyping; and enabling choices and the fulfilment of rights and desires. This research has also identified how service providers fall back on the notion of ‘treating everyone the same’. Two consequences of such an approach, however well-meaning, are that it perpetuates heterosexism (Knochel, Quam and Croghan Reference Knochel, Quam and Croghan2011) and limits service development that would ensure culturally sensitive, safe and inclusive provision (Phillips and Marks Reference Phillips and Marks2008).
Being unaware of LGBT service users was also a common finding in this body of research, which contributes to or exacerbates loneliness, isolation and exclusion (Fredriksen-Goldsen and Muraco Reference Fredriksen-Goldsen and Muraco2010; Hughes, Harold and Boyer Reference Hughes, Harold and Boyer2011; Willis et al. Reference Willis, Maegusuku-Hewett, Raithby and Miles2016). Service providers’ reluctance to ask questions about sexual and gender identification can also exacerbate the invisibility and silencing of LGBT residents (Johnson et al. Reference Johnson, Jackson, Arnette and Koffman2005). Phillips and Marks (Reference Phillips and Marks2008) have observed that information recorded on intake commonly frames ‘sexuality’ in heteronormative ways and focuses on physical/biological ‘problems’ associated with ageing rather than on sexual/gender needs and identities. Participants in the study by Willis et al. (Reference Willis, Maegusuku-Hewett, Raithby and Miles2016) feared having to conceal their identity in such circumstances to protect themselves from discrimination and hostility from staff and residents (see also Stein and Almack Reference Stein, Almack, Ward, Rivers and Sutherland2012). The forms of discrimination just described are compounded by experience of ageing that is likely to have included a history of marginalisation (Fredriksen-Goldsen and Muraco Reference Fredriksen-Goldsen and Muraco2010), which heightens LGBT people's vulnerability to being ostracised. In light of the above-mentioned constraints, it is unsurprising that older LGBT residents describe care homes as alienating (Phillips and Marks Reference Phillips and Marks2008) and being taken into care registers as a major fear of older LGBT individuals (Almack, Moss and Smith Reference Almack, Moss, Smith, Fish and Karban2015; Croucher Reference Croucher2008) and those not so old (Johnson et al. Reference Johnson, Jackson, Arnette and Koffman2005).
By way of solution to some of the problems identified above, a study by Tolley and Ranzijn (Reference Tolley and Ranzijn2006) recommends staff development measures that include ‘exposure to non-heterosexual people’ and training designed to develop knowledge about the diversity and realities of LGBT lives and initiatives to help staff to challenge heteronormativity. Within England, there are pockets of good practice and initiatives that offer practical guidance on meeting needs, e.g. Suffolk County Council and Suffolk LGB&T Network (2012). At a national level, the Care Quality Commission (CQC; the government agency that inspects care standards) has produced guidance for inspectors in relation to ‘sexual orientation’ (CQC 2008). In a review of end-of-life care, the CQC (2016) has brought to the attention of service providers the need to avoid poorer-quality care by marginalised groups (e.g. concerning ethnicity, disability, sexuality, gender difference) because providers do not always understand or fully consider their needs.
Finally, in this section, we note some useful resources from the voluntary sector that offer care environments practical ways of addressing LGBT inclusion. One example is a resource pack for professionals supporting older LGB care home residents, which provides a checklist on good practice at individual and organisational levels (Knocker Reference Knocker2006). A survey-based report commissioned by UK-based campaigning organisation, Stonewall, highlighted the existence of goodwill amongst care staff (across the range of residential and domiciliary provision) keen to deliver the best possible service to LGBT people. However, this report identified limited understanding of LGBT health issues (Somerville Reference Somerville2012). This story of goodwill undercut by lack of knowledge is a major theme in our discussion below.
The study: research design and respondents
This section explains the research methods, sampling and recruitment strategy, ethical approach and method of data analysis used in the research. Using a non-randomised survey, we obtained 187 responses to a questionnaire completed by staff who managed and/or delivered care in homes accommodating older people.
The questionnaire consisted of 30 questions on attitudes, knowledge/policies and practices concerning LGBT residents and 58 items in all given that several questions were broken down into various sub-questions/themes. Complete non-responses (refusals to participate because they ‘treat residents the same’) from within the homes visited were low and appeared to be motivated more by avoiding LGBT issues rather than because of language difficulties. The lowest response rate to an item was 89 per cent to a question about whether ‘LGBT issues are discussed openly’ in the home. Lower response rates tended to occur either towards the end of a lengthy questionnaire and/or came in response to sub-themes that were part of a set of questions (e.g. on care home inclusivity measures). Response rates were also slightly lower for more controversial questions, e.g. whether religious belief affected acceptance of LGBT individuals. It is worth noting that whilst religious belief could be an explanatory variable in discriminatory attitudes towards LGBT residents, later discussion – on how professional duty could override antipathy – indicates ambivalence. Thus, our conclusions in this respect are tentative and we consider that this particular issue requires specific study.
The questionnaire was posted online by Care England. Care England is the leading representative (voluntary) body for independent residential care services that comprises single and national (corporate) providers who manage over 7,000 care services. Whilst we cannot know how many providers saw the link/survey, 89 completed questionnaires online indicate a lower response rate and thus further caution concerning validity and reliability of the results (see, however, the discussion below on the limits of the method). However, to avoid a mono-sample mainly of managers/more senior staff (who may not work so closely with residents), seven care homes (smaller, medium and large) were visited in the East Midlands and North-West regions to solicit the views of diverse staff, especially those providing direct care or support. This yielded 98 responses (figure derived from the lead researcher's field notes) as given in Table 1.
Table 1. Breakdown of responses from care homes visited

Notes: N = 93. 1. Local authority maintained.
Staff completed the questionnaire on the premises independently in work time. Incentives to participate announced by the lead researcher were that: the subject is under-researched; the survey was tacitly endorsed by Care England; and a plain-English summary of findings would be provided to participating homes and Care England for dissemination.
All homes were referred to us through the professional networks of the second author and ranged from smaller/modest-sized homes (no more than 40 residents) to medium-sized (of up to 80 residents) residents and larger care homes of 80 plus residents. Respondents from within the seven care homes (which yielded between three and 25 respondents and a subtotal of 101) were self-selecting. Staff from the homes visited represented 49.7 per cent of respondents and online responses (mainly from service managers) accounted for 50.3 per cent of such. During care home visits, the first author outlined the study at staff briefings and all members of staff in attendance were given the option to complete a questionnaire. Very few staff declined to take part: in one care home, one maintenance man declined without offering a reason; and in another home, two older female care staff declined, citing their personal policy of ‘treating residents all the same’.
The limitations of the survey method, which emphasises discovery of factual knowledge to answer ‘what’ type questions, have been well documented. They concern its lack of suitability for accessing data to answer ‘why’ questions that concern the detail of individual reasoning, motive, and ambivalences in thought and practice (Bryman Reference Bryman2012; Cicourel Reference Cicourel1964). However, in-depth investigation of a small number of informants was not our purpose. The survey method was chosen because it is a relatively quick and economical way of generating data from a large number of geographically dispersed respondents (Rattray and Jones Reference Rattray and Jones2007). The questionnaire yielded much data about a lot of people in a short period. Completing the questionnaires individually minimised the potential for biasing respondents’ views by dint of researcher presence or intervention (Rattray and Jones Reference Rattray and Jones2007), though advice on the rationale of a question was given on rare occasions when participants asked for clarification.
As the sample is non-probabilistic, claims concerning the findings are cautious. To compensate for such limitations, we added a purposive element to the sampling strategy (care home visits) which was designed to include significant dimensions of variation among employees. Indeed, given the range of occupations provided in the survey, our sampling frame approximates a maximum variation sample (Patton Reference Patton2005). This means that the data are at least indicative rather than representative of broader trends (Bryman Reference Bryman2003). Rather than being generalisable, findings may be ‘transferable’ to similar contexts (Lincoln and Guba Reference Lincoln and Guba1985). In terms of our ethical approach, the voluntary and anonymous nature of the study was highlighted on the questionnaire and during site visits. Whilst maintaining a critical stance, we have deliberately avoided representing respondents as intrinsically intolerant and acknowledge that less favourable views towards LGBT individuals continue to be influenced by forms of social organisation and thought, often religious in nature (Valentine and Waite Reference Valentine and Waite2012) and inflected by generation (Edmunds and Turner Reference Edmunds and Turner2002). In response to some open-ended questions, several respondents opined that the questionnaire presumed a bias in favour of acceptance of those thought to represent non-normative genders and sexualities. Whilst we make no apology for such a stance, the questionnaire was worded to accommodate diverse views without implied judgement.
Although the data are non-probabilistic, our analysis seeks to add nuance and rigour beyond simple percentages. We therefore conducted cross-tabulations, which indicate associations between explanatory variables. Our analysis foregrounds: the more significant associations (e.g. between religion and acceptance of non-normative genders and sexualities); where variables indicate surprisingly little difference in acceptance (e.g. age and the need for specific training on LGBT issues); and apparently counter-intuitive findings (e.g. wish for specific training by those of faith and confidence in LGBT knowledge among older, religious and male respondents).
The respondents
Gender
The gender profile in our sample (Table 2) closely resembles the national profile of care-sector staff where females represent 83 per cent of the care workforce as identified by Hussein et al. (Reference Hussein, Manthorpe, Stevens, Rapaport, Martineau and Harris2009). This study is based on a random sample drawn from the National Minimum Dataset in Social Care, an online database with information on 25,000 care establishments and 700,000 care workers in England.
Table 2. Respondents by gender, age, job, ethnicity, religious belief and sexual identification
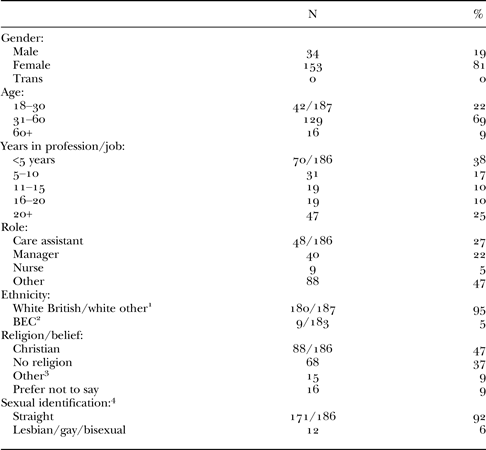
Notes: 1. Irish, Kurdish, Polish, Romanian and American. 2. Refers to black and ethnic community individuals and includes dual heritage, Asian-British (i.e. ‘Pakistani’ and ‘Sri Lankan’), Black and Black-British. 3. Buddhist, Muslim, Jewish and spiritual. 4. The wording to describe this was very similar to the categories used by the National Survey of Sexual Attitudes and Lifestyles (card NN; NATSAL 3) but we separated out gay and lesbian and added ‘prefer not to say’. If the response was ‘Other’, the respondent was asked to specify the preferred identity label.
Age and length of experience in the care sector
Age was chosen as a variable given that recent research has shown that younger people will have grown up in a less ‘homohysteric’ era which could impact upon their attitudes to non-normative genders and sexualities (Anderson Reference Anderson2009). The age groups deployed reflect early adulthood (18–30), middle adulthood/mid-career (31–60) and late career/approaching ‘retirement’ (61+). Respondents ranged from 18 to 70+ and resemble the randomised sample of Hussein et al. (Reference Hussein, Manthorpe, Stevens, Rapaport, Martineau and Harris2009), which had a median age of 42. The sample is distinctly middle-aged given that the largest category (just under a third of respondents) was aged 41–50 and 58 per cent of respondents were aged 41–60. Although staff with five or more years of experience of working in the care sector constituted a majority of respondents at 62 per cent, the sample reflected a mixture of those relatively new to the job and those with considerable experience.
Roles and types of care home
The biggest category in response to an item on respondent roles was ‘Other’, which comprised nearly half of the sample. This diverse group included decorators, maintenance, kitchen, ‘marketing’, ‘training’, ‘customer service’ and administrative staff. When combined, the ‘Other’ and ‘Care assistant’ categories, accounted for nearly three-quarters of respondents. Such staff are likely to have more day-to-day interaction with residents. The types of care homes are explained above in the ‘Context’ section, though ‘nursing homes’ were slightly more prominent than ‘residential care’ homes by a margin of 5% (44% versus 39%, respectively). The remaining respondents (18%) working in ‘other’ establishments largely indicated working in mixed ‘nursing and residential care’.
Ethnicity
The majority of respondents (95%) identified as ‘white British’/‘white other’. All other ethnic categories comprised 13 respondents (5%). Black and ethnic community (BEC) individuals appear significantly under-represented in our sample given that they have been estimated to constitute nearly of one-fifth of the care-sector workforce (Hussein et al. Reference Hussein, Manthorpe, Stevens, Rapaport, Martineau and Harris2009). The small number of BEC respondent limits ability to draw conclusions about associations between ethnicity and attitudes, knowledge and practices.
Religion
Just over half of respondents (55%) professed some religious belief with the majority (47% of those responding to the item), identifying as ‘Christian’. Those selecting ‘no religion’ represented 37 per cent of responses. Such figures are considerably higher than those in the 2011 Census where 25 per cent of the population of England identified as having no religion (Office for National Statistics (ONS) 2012).
Sexual identification
The majority of respondents (92 per cent) identified as heterosexual and the remainder as lesbian, gay or bisexual. This is consistent with figures from the National Study of Sexual Attitudes and Lifestyles (NATSAL) (Mercer et al. Reference Mercer, Tanton, Prah, Erens, Sonnenberg, Clifton and Johnson2013), which indicate that 7 per cent of the population identifies as ‘homosexual’, though the latter figure does not include those identifying as bisexual, trans, ‘queer’ or ‘fluid’. The small number of LGBT respondents limits drawing of conclusions about associations between these individuals and their responses.
Results
This section describes data generated on: attitudes towards; knowledge about LGBT individuals and issues affecting them; and policies and practices affecting provision. When we refer to ‘respondents’ in the results and discussion sections, we are referring to the number of respondents to each item, given varying response rates.
Attitudes to LGBT residents
To elicit employees’ attitudes, questions asked about: embarrassment about talking about LGBT issues; whether same-sex relationships were considered ‘wrong’ (immoral); sexual expression and sexual activity by residents; and whether respondents considered specific training on LGBT issues necessary.
Most significantly, more than four-fifths of respondents agreed that they would not feel embarrassed to talk about LGBT issues and 83 per cent of those who responded to the item rejected the proposition that same-sex relationships ‘are wrong’ (Figure 1). This figure exceeds NATSAL figures (Mercer et al. Reference Mercer, Tanton, Prah, Erens, Sonnenberg, Clifton and Johnson2013), which showed that 48 per cent of men and 66 per cent of women aged 16–44 considered same-sex relations ‘not at all wrong’.

Figure 1. Attitudes towards sexuality per se and lesbian, gay, bisexual and trans (LGBT) issues (e.g. signalling openness to address sexual and gender differences).
Further, and contrary to extant literature (Simpson et al. Reference Simpson, Horne, Brown, Brown Wilson, Dickinson and Torkington2015), nearly four-fifths recognised residents, regardless of their identification, as sexual beings and nearly two-thirds of respondents believed that residents could be ‘sexually active’. Moreover, nearly two-thirds of respondents agreed that staff should receive specific training on the needs of LGBT people, though a significant minority (22 per cent) either felt neutral (registering ‘neither agree nor disagree’) or were unsure (choosing ‘don't know’) in relation to this item.
Desire for specific LGBT training by gender, age and role
In terms of needs for training on LGBT-related issues, there was little difference by gender with slightly more females at 66 per cent answering in the affirmative compared with 61 per cent of males. The desire for training did though increase with age, with 68 per cent of those responding aged 31–60 answering in the affirmative compared with 56 per cent of responses from the 18–30 category. Just over 70 per cent of responses from managers (which included nurses) and two-thirds of ‘other’ staff (mixed group of maintenance and administrative staff) appeared keener for such training than the 58 per cent of care assistants who responded likewise. There was slightly more need for training indicated by 68 per cent of religious respondents which compared with 61 per cent of responses from non-religious individuals. Nonetheless, different indications emerge when the responses are cross-tabulated with respondent differences concerning gender, religious belief and age.
Gender difference and age and same-sex relations as wrong
Male respondents appeared more likely than female ones to express uncertainty or disapproval concerning same-sex relations as morally wrong. Whilst a third of male respondents answered thus, only 12 per cent of female employees did so. Significantly, nearly 90 per cent of those responding to this item from the young adulthood age–bracket (18–30) disagreed with the statement that same-sex relations are wrong, which slightly eclipsed the 84 per cent of those in middle-adulthood (31–60) who disagreed with the idea that same-sex relations are morally wrong. The likelihood of holding negative attitudes increases more markedly in the run-up to retirement age group (61+). In this latter group, 38 per cent of respondents agreed with the proposition that same-sex relations are wrong but still just short of two-thirds of this oldest age group disagreed with the proposition.
Knowledge of LGBT individuals, legislation and policies
Whilst attitudes appeared generally positive, knowledge of actual LGBT individuals and the issues affecting them seems somewhat less well-developed (see Somerville Reference Somerville2012). Just over two-thirds of responses (67%) indicated that a resident had never disclosed their sexual or gender difference to the respondent (see Willis et al. Reference Willis, Maegusuku-Hewett, Raithby and Miles2016). Indeed, 59 per cent of responses registered being unaware of any LGBT residents in their present workplace and only 7 per cent of those responding reported that a resident had disclosed their bisexual or trans status to the care worker. Indeed, staff reported much greater awareness of staff who were LGBT, as 70 per cent of those responding indicated awareness of such colleagues.
Sufficient knowledge of issues affecting LGB and trans residents
More than 70 per cent of respondents considered that they had sufficient knowledge generally of issues affecting LGB individuals, though fewer declared having sufficient knowledge of issues related to trans individuals by a margin of 10 per cent (61%). Whilst a minority reported having insufficient knowledge of LGB (7%) and trans residents (just over one in ten respondents), when responses signalling not knowing or uncertainty were combined, they represent significant minorities of 27 and 36 per cent, respectively.
Cross-tabulations by gender, age, role, type of home and religion with knowledge indicate high levels of confidence in knowledge of LGBT-related issues. We make five particular observations here. First, gender difference appeared of little consequence as 70 per cent of males and 69 per cent of females considered they had sufficient knowledge of LGB-related issues and 78 and 74 per cent, respectively, reported this in relation to trans-related issues. Second, the two older groups expressed (perhaps counter-intuitively) slightly more confidence in their knowledge of trans than LGB issues (though the middle age-bracket did so in relation to the two other age-groups apropos LGB knowledge). Third, care assistants considered themselves the least and managers the most knowledgeable of the three age-groups in relation to LGBT issues. Fourth, those who were in the late career stage and/or religious expressed (again counter-intuitively) slightly more confidence in their knowledge of LGBT issues than younger and non-religious respondents. Fifth, policy knowledge appeared highest in mixed residential/nursing homes at just over 41 per cent – almost double that in nursing homes where levels of awareness registered as the lowest – though awareness levels were generally low anyway (Figure 2). It is also worth noting that negligible differences in knowledge were reported by religious and atheist participants.
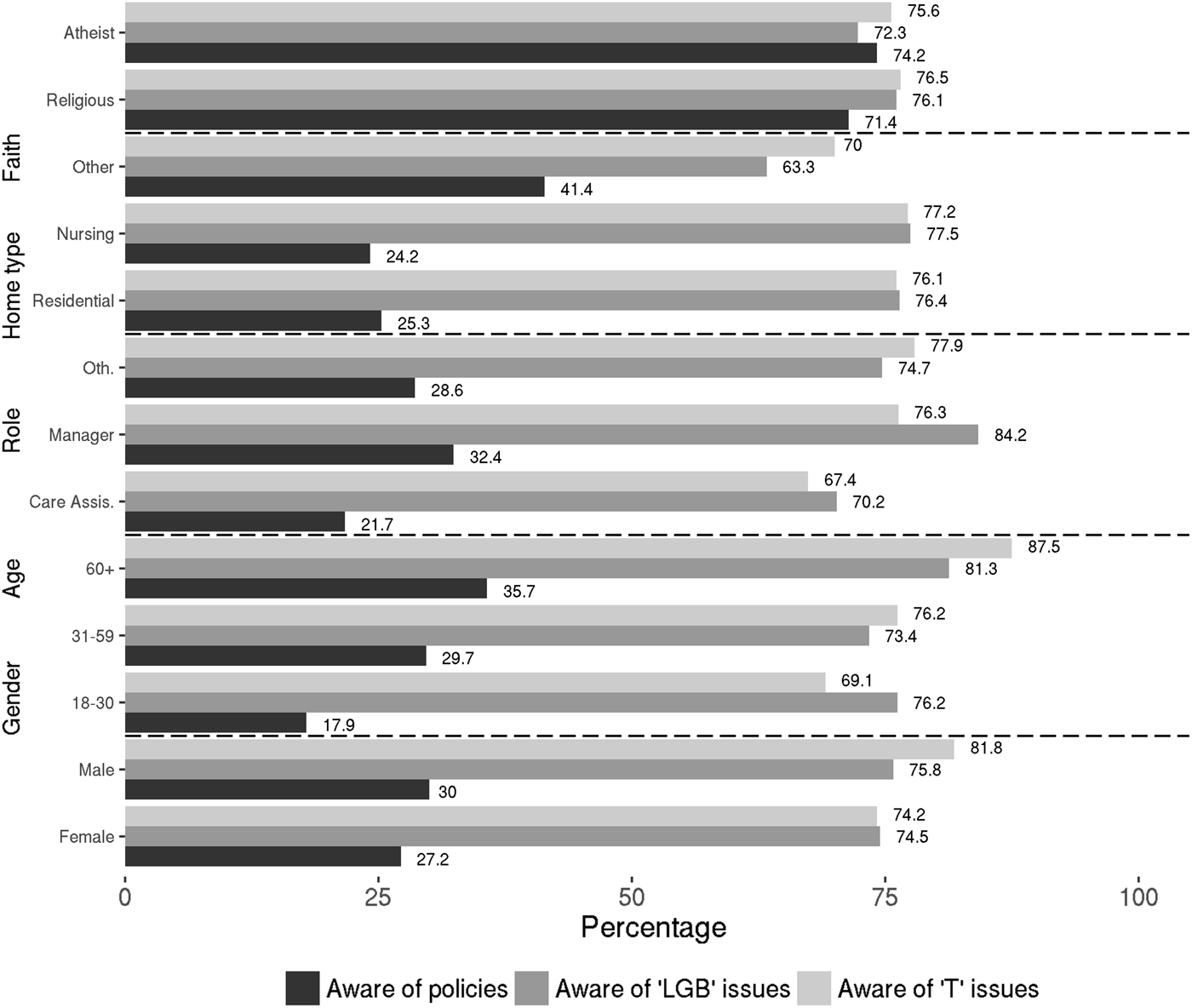
Figure 2. Awareness of equality policies and lesbian, gay, bisexual (LGB) and trans (T) issues by belief system, gender, age/time served, job role and type of home.
Moreover, in relation to an item on knowledge of laws affecting LGBT residents, only 17 per cent of respondents volunteered information. Fourteen respondents, or 44 per cent of this sub-set, cited The Equality Act 2010 and some of these also cited the Human Rights Act 1998, particularly in relation to the right to privacy. A few respondents cited the Protection of Vulnerable Adults list (a government register containing details of individuals disbarred from working with vulnerable people). However another 15 responses (59 per cent of the sub-set) vaguely referred to ‘equality and diversity law’, ‘sexual and gender discrimination’, ‘equality and diversity’, ‘equal rights’ and ‘equal opportunities’. Vaguer still, eight respondents (a quarter of the sub set) cited ‘internal policies’, ‘staff and clinical policies’, ‘management guidelines’, ‘disciplinary procedures’ and ‘acceptance of all’.
Individual and institutional practices: training and inclusion measures
This sub-section examines: individual practices, i.e. the reported effects of religious belief on professional practice concerning LGBT residents; and respondents’ views on collective/institutional practices (i.e. training and organisational measures) intended to support inclusion.
Significantly, in response to a question about religious belief and attitudes, about one-fifth of Christian respondents expressed disapproval of same-sex relations compared with 14 per cent of non-believers; a relatively narrow margin of 6 per cent difference. Moreover, 68 per cent of respondents disagreed that their religious belief would affect their ability to accept LGBT residents, though a significant minority, nearly a third of respondents, appeared uncertain. Yet, the majority response to an item about whether respondents would have to suppress religious belief to enable them to work with LGBT residents suggests a more divided response, where the majority response at 38 per cent were ‘unsure/didn't know’. Indeed, one care assistant declared during a brief discussion with the Principal Investigator that her professionalism and recognition of the essential humanity of vulnerable residents would override religious antipathy, which was echoed in several responses to open-ended items. This kind of negotiated response compared with just over a quarter of respondents of who expressed agreement with such a proposition and 35 per cent who disagreed.
The majority of respondents to this item reported that LGBT-specific training had not been provided in their current workplace, which contrasts with the number reporting experience of training in other areas of cultural sensitivity (Table 3). Similarly, a majority indicated uncertainty or denial (i.e. those who selected ‘No’) in relation to a question about whether their current workplace routinely provides staff with training designed to sensitise them to LGBT residents and related issues. Further, 56 per cent of respondents were either unsure or considered such training unnecessary (37%), though a significant minority (44%) wanted more training on LGBT issues. This could either reflect the positive attitudes reported earlier or the mantra of treating residents ‘all the same’. There needs to be caution when interpreting data on training and, indeed, on inclusion measures. As we did not request details of care homes’ policies, we cannot measure staff perception against benchmarks set by the homes. However, such disappointing responses indicate that dissemination of such policies could be improved.
Table 3. Training

Note: LGBT: lesbian, gay, bisexual and trans.
LGBT-related training experienced by age, role, religion and type of home
Reported experience of LGBT-specific training events was highest among the mid-career/middle age-bracket (31–60) with nearly 16 per cent of those in this category responding as against just over 14 per cent for the late career/oldest age-bracket (61+) and just under 5 per cent for those in the 18–30 age bracket. Further, 35 and 40 per cent, respectively, of the youngest and middle age-brackets reported that their workplaces had provided some LGBT-related equality training compared with just over 57 per cent of those responding in the oldest age category. Care assistants appeared least likely to report experience of LGBT-specific training, at just over 6 per cent compared with around 16 per cent of managers and ‘Other’ employees. Individuals in the two latter categories were more likely to report that their home had provided some LGBT-related training at 39 and 45 per cent, respectively, compared with just over 30 per cent of care assistants. Those professing religion (43%) were more likely than atheists (33%) to report that their care home had provided some such training. Significantly, nursing home employees were more likely to report having attended LGBT-specific training at nearly 27 per cent as against just over 9 and 11 per cent of residents and ‘Other’/mixed homes, which might reflect that nursing homes accommodate more vulnerable residents. Nevertheless, staff who were employed in residential homes were more likely to report that their home had provided at least some LGBT-related training (commonly part of generic equality training). Forty five per cent of such staff reported this which compared with 36 and 39 per cent of residential and ‘Other’ homes, respectively.
In response to a question concerning need for further LGBT-related training, cross-tabulations indicated mainly differences by gender and job role: 62 per cent of females considered further training on LGBT issues necessary as against 36 per cent of males. Managers (who generally registered greater confidence in their knowledge of such issues), appeared keener for additional training and accounted for just over half of such responses (54%) compared with around 40 per cent of responses from care assistants and those occupying ‘Other’ roles.
Immediately striking in Figure 3 are the low numbers able to report positively on a range of practices designed to promote inclusion. With regard to measures to encourage residents to talk about LGBT issues, just over a quarter of the responses considered that this was the case, though one-fifth of responses expressed disagreement. Similar figures resulted in relation to talking about LGBT issues generally. Nearly a third of responses indicated agreement but those who were unsure about or disagreed with the statement represented just over 70 per cent of responses. Only 8 per cent of respondents reported links between their home and a LGBT organisation and just over a third of respondents to the item answered in the negative. Besides, less than one in ten respondents answered in the affirmative to a question about whether their home provided LGBT-related literature (leaflets and magazines). In response to an item ‘home uses images that show LGBT people in publicity material (e.g. leaflets)’ that could portray recognisable symbols of difference (rainbow flag), 5 per cent of respondents thought that their care home used such images. This, however, differed across type of care home, with 98 per cent of respondents based in nursing homes answering ‘no’ or unsure as against 71 per cent of respondents based in residential homes. Furthermore, in response to a question asking if their care home uses appropriate language concerning self-identification on assessment forms, fewer than half of responses indicated that this was the case and 58 per cent were either unsure or answered in the negative.
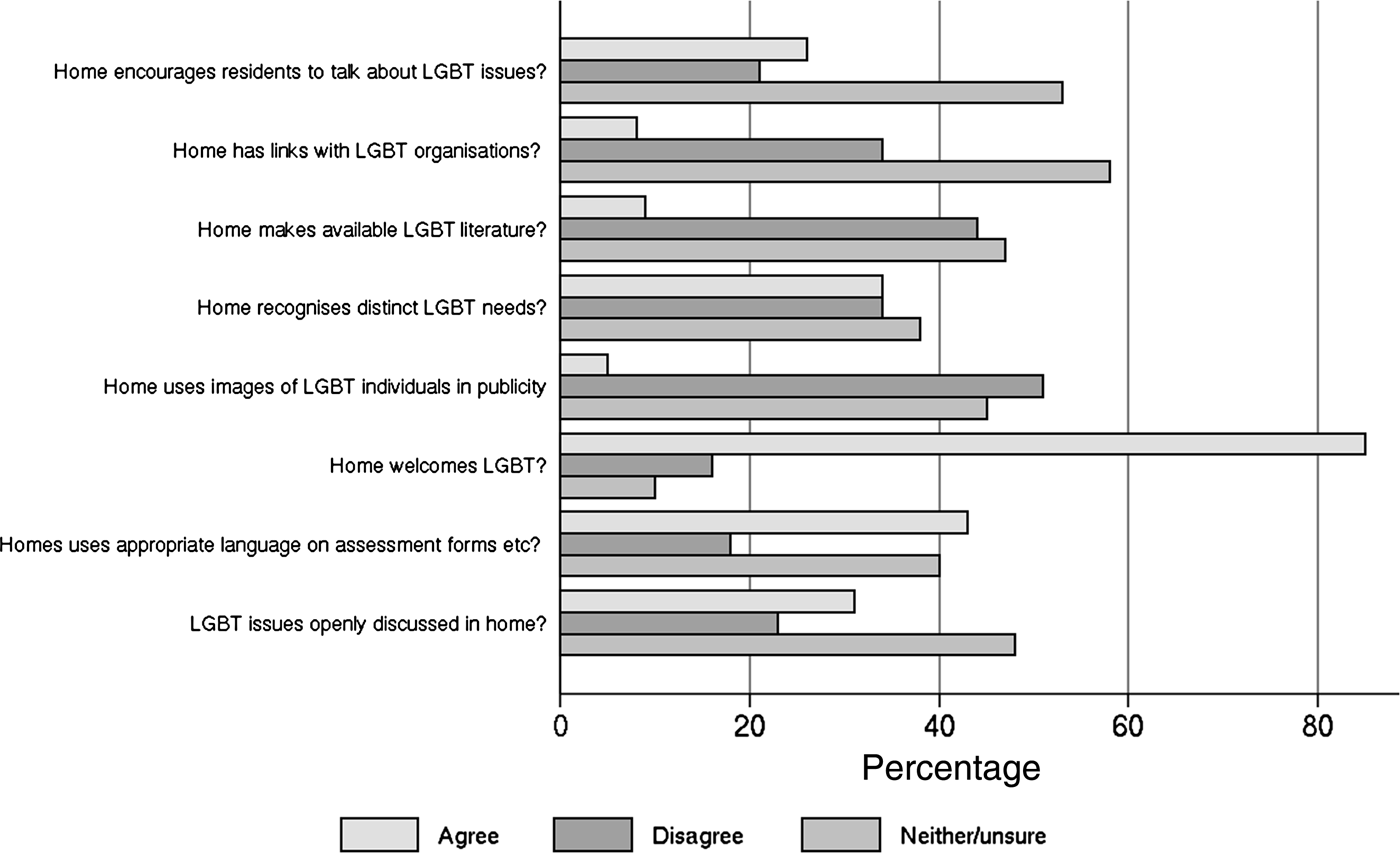
Figure 3. Respondents views of homes’ inclusion measures.
Answers to the item on whether a ‘care home recognises the distinct needs of LGBT residents’ differed markedly according to type of home, where 50 per cent of those employed in nursing homes were more likely to answer in the affirmative compared with 54 and 64 per cent of respondents in residential and mixed homes, respectively. Wider differences were also apparent in relation to age, where 46 per cent of the 18–30 age group answered in the affirmative to this item compared with nearly four-fifths of the middle age group and two-thirds of the oldest group. In terms of religious status, 55 per cent of non-believers compared with 73 per cent of Christians and 69 per cent of ‘other’ faiths answered in the affirmative. As regards role, 57 per cent of care assistants answered in the affirmative to the item in question compared with 76 per cent of managers and 67 per cent of those occupying other roles.
Somewhat more encouragingly, in Figure 4 a clear majority (over four-fifths of respondents) considered that that their care home welcomes LGBT residents. However, this appears more contested when we combine the number of respondents who either disagreed or who were unsure that LGBT residents had distinct needs. Such respondents represented nearly three-quarters of those who answered.
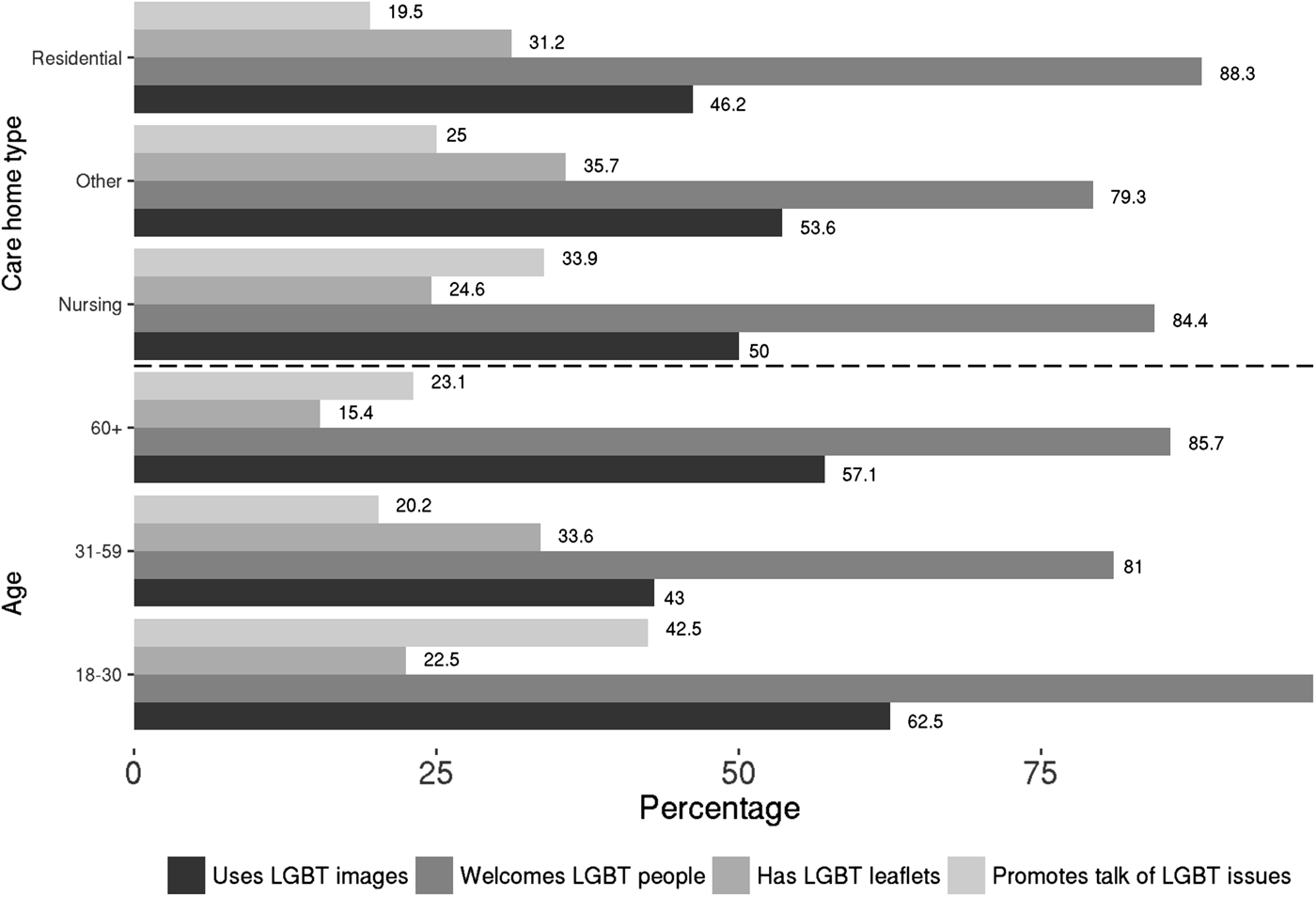
Figure 4. Presence of inclusion measures by age and type of home.
In terms of age differences, it appears that the youngest age group is more likely to express positive perceptions in relation to the measures/practices. In particular, this age group is considerably more likely to consider that their home welcomes LGBT individuals and encourages residents to talk about LGBT-related issues. Also of note is that there are only marginal differences between the reported inclusion practices between the three types of home: the most significant being that employees in residential homes appear somewhat more likely than those in the two other types of home to report that their workplace encourages residents to acknowledge LGBT-related issues.
Discussion
This section highlights key themes within the data described. It discusses the theoretical and practical implications of staff's attitudes, knowledge and practices, and links them to broader themes and issues concerning the partial reflexivity of individual staff and organisations.
Attitudes: reflexivity and tolerance within limits
A clear majority of respondents felt comfortable talking about LGBT-related issues and disagreed with the proposition that same-sex relations are ‘morally wrong’. This suggests qualified support for theorising concerning greater tolerance of non-normative sexualities and genders. For Giddens (Reference Giddens1992), greater acceptance of sexual difference is integral to a complex ‘late modernity’ that has seen the erosion of old traditions and thus obliged self-reflection on identities, relations and lived experience. This process of ‘reflexivity in a de-traditionalised’ society is thought to have led to changes in sexual mores, which has also been supported by shifts since about the 1960s in culture (mainly via secularisation of society), the law and an increasingly globalised socio-economic order. For instance, we can now integrate images (about ageing, etc.) from various cultures into our lives via digital technology. The ‘remoralisation’ of social, political and erotic-relational lives that Giddens invokes, he believes, has encouraged increased sexual exploration and equality in close relationships generally. Indeed, not only is there greater toleration of diverse genders and sexualities but also, Giddens argues, lesbian and gay people are ‘trailblazers’ for ‘new experiments in intimacy’ based on negotiated equality.
Whilst much of Giddens’ argument applies implicitly to younger generations and those of a secular persuasion, his analysis overlooks the reflexive capacities being developed by some individuals (younger and older) embracing a form of traditionalism. Indeed, our data indicate a significant correlation between strong religious beliefs and reluctance to accept sexual and transgender difference, which Dorsen (Reference Dorsen2012) found applicable to nursing staff in Canada. Yet, there are signs that the largely middle-aged population surveyed in this study has accommodated to the times when we consider the high levels of recognition of the value of LGBT-related training. Although cross-tabulated data indicated that younger staff and those professing no religion (more accustomed to narratives of tolerance), were considerably less likely to object to non-normative sexualities and genders, a significant minority of older and religious staff reflexively seek rather than shun LGBT-related training opportunities. Such opportunities could offer help to individuals concerned to manage the contradictions between personal conviction or feelings and professional duty. Whilst individuals cleave to the traditionalism represented by religious faith, nonetheless, a significant minority of them appear to be engaging in reflexive (and sometimes difficult) dialogues or forms of negotiation between established and newer strands of thought. Indeed, Yip (Reference Yip2005) has noted a growing claim among individuals of faith concerning the right to choose how they practise their religion. This might represent individualisation of religious thought and practice where people draw on and develop narrative resources to them to articulate their own complex morality.
Indeed, it appears that individuals of faith can develop particular humanistic ‘strategies of co-existence’ (Valentine and Waite Reference Valentine and Waite2012: 481) that help assuage tensions between faith and the wish to act respectfully towards LGBT individuals as fellow human beings. Such strategies include compartmentalisation of thoughts and feelings in the everyday where complex, intersectional identities prioritise a pragmatic ‘ethic of care’ and the reality of ‘what is’ over theology and ‘what ought to be’ (Valentine and Waite Reference Valentine and Waite2012: 490). As reflected in this study, individuals can distinguish between their abstract religious beliefs about sexual and gender difference and the (convivial) human qualities of vulnerable LGBT individuals needing support. The narrow margin of disapproval of LGBT individuals between religious and non-religious respondents (6% higher in the former category) indicates further support for the conclusions just presented. It also suggests the persistence of subconscious religious influences or even of secular forms of homophobia among a significant minority of non-believers.
There are other limits to Giddensian theorising concerning reflexivity, which, in turn, indicate limits to theories that almost universalise the idea of more inclusive and emotionally literate (youthful) hetero-masculinities (see Anderson Reference Anderson2009). Just as significant as any difficulties stemming from faith was an apparent gender-inflected limit to tolerance when we consider that male respondents were considerably more likely than female ones to object morally to same-sex relations, yet men felt no less secure in claiming knowledge about LGBT-related concerns. In contrast to Giddens’ thinking described above, such a caveat indicates support for arguments concerning the persistence of dominant forms of masculinity that are achieved by covert, subtle distancing of the self from non-normative expressions of sexuality and gender coded as ‘feminine’ (Connell and Messerschmidt Reference Connell and Messerschmidt2005). In effect, we steer a course between the theorising of Giddens and that of Connell and Messerschmidt in acknowledging like the former that there have been clear gains in tolerance towards LGBT people in a relatively short time in the UK. Simultaneously, the above caveats concerning age, religion and masculinity indicate more a form of tolerance (a power asymmetry nonetheless), than a fuller, mutual and more equal understanding across differences (McGhee Reference McGhee2008). Indeed, social proximity and opportunities for familiarisation by no means guarantee the socio-cultural transformations needed for inclusion and can instead engender defensiveness, reinforce boundary-maintenance and entrench hostility (Amin Reference Amin2002). Whilst tolerance represents an improvement on a deeply homo-/bi-/transphobic past, we contend that substantive equality, sexual and erotic democracy and inclusion remain distant prospects (Simpson Reference Simpson2015).
Knowledge
The levels of confidence expressed by respondents concerning their general knowledge of LGBT issues are prima facie encouraging. Declarations of sufficient knowledge are quite likely a function of/associated with attitudes predisposing openness to learning about LGBT lives, cultures and the political issues affecting them. Again, this gives credence to the notion of reflexive societies where individuals are prepared to discuss more openly such issues within and courtesy of various media and in their personal life where they explore and share knowledge of gender and sexual differences in more thoughtful, less judgemental or prurient ways. Levels of knowledge about more specific LGBT-related policy issues, however, appear much less advanced. For instance, 79 per cent of those responding either answered in the negative or were unsure of any monitoring of civil partnerships/equal marriage in their workplace; 76 per cent disagreed or were unsure about whether their workplace monitored trans identity; and 72 per cent answered in the same way to items concerning monitoring of sexual identity and whether the law was integrated into the home's policy.
It is also significant that only a third of respondents were able to report that a resident had disclosed their gay or lesbian identity and only 7 per cent reported thus in relation to trans residents. The above data not only resonate with several comments in response to open-ended questions expressing that ‘We don't have any/many at the moment’ but also offer support for research highlighting how LGB (and no doubt trans) individuals ‘continue to live in fear and hide their identities’ in care spaces (Westwood Reference Westwood2015).
However, striking within our data and standing in need of explanation are the contradictory findings indicating that a significant minority of older staff and/or professing Christianity in particular seem more confident in their knowledge of general and specific LGBT-related concerns (see, however, the sub-section on ‘Policies and practices’ below). The nature of the survey does not allow in-depth exploration of these contradictions but, we would reason, based on qualitative comments from care assistants in our dataset and from our knowledge of existing scholarship, that this is attributable to a humanistic professionalism itself redolent of the ‘strategies of co-existence’ identified by Valentine and Waite (Reference Valentine and Waite2012). This situation could also reflect the epistemic and emotional resources accrued through the ageing process (Heaphy Reference Heaphy2007; Simpson Reference Simpson2015). Nevertheless, even if we ascribe the above-identified problems to negligible dissemination of knowledge at individual or institutional levels, such instances offer further support for the view that they represent tolerance rather than the thorough understanding that is a prerequisite for equality and inclusion.
Policies and practices
As indicated in the description of the study results, responses to items concerning institutional practices that would support the inclusion of LGBT residents were the least encouraging. This was particularly evident in relation to responses to questions about staff training where only 5 per cent of those responding from the 18–30 age bracket and 6 per cent of responses from care assistants reported that their current workplace had provided a distinct LGBT-focused training experience. That only a minority considered any further specific LGBT-related training necessary could either reflect the view that residents are ‘treated all the same’ or ‘we don't have any/many’ (identified in Knochel, Quam and Croghan Reference Knochel, Quam and Croghan2011 and Fredriksen-Goldsen et al. Reference Fredriksen-Goldsen, Hoy-Ellis, Goldsen, Emlet and Hooyman2014), but also suggests a lack of awareness of the need for ongoing training. Again, a gender difference stands in need of explanation when we consider that 62 per cent of female staff (who largely occupied direct care roles) responding to this item answered in the affirmative as against 36 per cent of responses from their male counterparts. We contend that this reflects hegemonic gender ideology (as noted earlier), which encourages men to feel more confident about the objective validity of their knowledge and expertise (Rose Reference Rose1993). Additionally, denial of the necessity of dedicated, strategic, developmental LGBT training not only risks homogenising people with a range of needs. It also risks reinforcing the view that once-and-for-all (or, at best, occasional training) is sufficient to impart the knowledge and skills required to meet needs resulting from dynamic, intersecting differences within and between LGBT individuals.
We have already noted that 85 per cent of respondents felt that their workplace welcomes LGBT individuals but this appears to be undercut by responses to other items. In turn, this contradiction reflects uncertainty about whether homes implemented measures recognising the distinct character of LGBT individuals’ needs. Such uncertainty is bolstered by findings that very few respondents considered that their care home deployed appropriate images in publicity materials, had links with LGBT community groups, or encouraged residents and other stakeholders to discuss related issues. Altogether, such responses indicate a lack of institutional support and commitment to fostering inclusion over time. If individuals, including some people of faith, are making considerable efforts to act reflexively, this is not being underpinned by a complementary organisational/collective reflexivity. Such findings indicate further support for the view that the needs of residents thought to represent non-normative expressions of gender and sexuality are effectively erased from policy and institutional practice (Fredriksen-Goldsen et al. Reference Fredriksen-Goldsen, Hoy-Ellis, Goldsen, Emlet and Hooyman2014; Hafford-Letchfield Reference Hafford-Letchfield2008). The above points reinforce our argument that individualised (as opposed to institutional) reflexivity, as theorised by Giddens, is only part of the story and does not account for the subtle workings of heteronormative and cisgender discourses that entertain toleration based on partial knowledge and understanding but, again, fall significantly short of genuine equality and inclusion.
Concluding thoughts
The headline message is that there is some encouraging good practice, though considerable room for improvement. Whilst there is much individual goodwill and elements of reflexivity among staff, there is also considerable uncertainty and lack of awareness about the existence of internal policies and a small degree of resistance to more egalitarian thought and practice. It is though noteworthy and encouraging that some religious staff reflexively overrode their antipathy by drawing on a more humanistic professionalism that involves a strong sense of the basic human dignity of individuals needing care. This issue should be addressed if not exploited within training and staff development.
Whilst attitudes were generally favourable, knowledge of LGBT individuals and issues relating to them was somewhat less well-developed. Approaches to equality could involve treating residents ‘all the same’ but this risks undercutting equality and reinforcing exclusion. Consequently, LGBT residents may be misrecognised as heterosexual (or asexual), cisgender or rendered invisible and further marginalised. This was partly counterbalanced by reflexive commentary in response to questions about how staff reacted to residents’ LGBT status and an encouraging general awareness that LGBT residents are covered by equality laws and internal policies.
There are more grounds for concern at the level of practice. Care home staff may not be so well supported in terms of training and therefore may be struggling (reflexively) alone to meet needs. The lack of a complementary organisational reflexivity was evident in the lack of strategic monitoring of the numbers of LGBT residents or efforts to work with residents to normalise sexual/gender difference. Care homes rarely made available LGBT-related literature or liaised with local LGBT support organisations. In sum, LGBT service users may have to depend more on the individualised knowledge and goodwill of staff rather than collective practice at a systemic level. As hinted in our discussion, and following more recent critical work on ageing sexuality, this could involve the creation of opportunities at periodic intervals for staff, residents and their significant others as part of an inclusive community, to reflect collectively on ingrained homo-/bi-/transphobia and consider how to manage this process (Phillips and Marks Reference Phillips and Marks2008; Westwood Reference Westwood2012). Such critical reflection, which is integral to professionalism and ethical behaviour, should also consider how non-normative sexualities and genders enmesh with other forms of difference including class and race, etc. (Hafford-Letchfield Reference Hafford-Letchfield2008; Westwood Reference Westwood2012). This would require that managers take a lead on disseminating knowledge concerning law, policy, knowledge and good practice. With this in mind, we have already provided a plain-English report of key findings to study participants and English Care. We intend to disseminate this article and the shorter plain-English version variously among academic networks, professional organisations (including trade unions and employers organisations), and voluntary sector and governmental agencies such the Alzheimer's Society, Dementia Care, the CQC and the Department of Health.
Further, we acknowledge that attitudes towards LGBT people are catching up with equality legislation (Anderson Reference Anderson2009). This may result in increased demands for person-centred care that is fully inclusive for LGBT people and needs addressing now. However, in certain ways as identified, awareness and knowledge of LGBT residents in care homes remains rudimentary and a step-by-step approach is required to improve this situation and to challenge heteronormativity over time. Care homes could, individually or in groups, appoint ‘diversity champions’ to work with managers to ensure that policies, promotional and information literature, and materials represent all LGBT people (and other groups); and to identify links that could be made with local LGBT groups. Although resources are limited, face-to-face training is a priority if staff are to work towards ensuring a community where LGBT residents can express themselves and not hide their sexual and/or gender identity. Indeed, much more could be done to raise awareness and campaign for person-centred care for older LGBT people via the Care Home Parliamentary Network. Also, homes need to review how they measure up to the CQC's care home reviewing processes to ensure that assessments of how they address diversity and equality transcend the tokenism of a tick-box exercise.
The general goodwill of staff needs acknowledging but this needs converting into concrete, strategic practice at the home and broader policy levels to advance inclusivity. Finally, the time is ripe to promote a bigger societal conversation on sexual and gender difference in aged care facilities. Failing to addresses the challenges and initiatives we have described is to risk perpetuating all manner of injustices against older LGBT residents/individuals.
Acknowledgements
We should like to thank the Editor and reviewers who have helped sharpen the focus of the end-product. Sincere thanks are also extended to Professor Martin Green, Chief Executive, English Care for supporting dissemination of the survey, the participating care homes and all those who took the time to complete the survey. Thanks are also extended to The National End of Life Care Programme (Department of Health) and The School of Health Sciences (internal grant), University of Nottingham for funding the research on which this article is based. KA held the funding and designed and piloted the survey. PS was Research Fellow who undertook the care home visits with a view to further completions of the survey. PW undertook statistical analysis. PS, KA and PW were all involved in analysis and writing of the paper. There are no conflicts of interest.











