As part of the Canadian Journal of Emergency Medicine (CJEM) developing social media strategy,Reference Thoma, Mohindra and Artz 1 we are collaborating with the Skeptics’ Guide to Emergency Medicine (SGEM) to summarize and critically appraise the current emergency medicine literature using evidence-based medicine principles. In the Hot Off the Press (HOP) series, we select original research manuscripts published in CJEM to be summarized and critically appraised on the SGEM website/podcastReference Milne 2 and discussed by the study authors and the online EM community. A similar collaboration is underway between the SGEM and Academic Emergency Medicine. What follows is a summary of the selected article and the immediate post-publication critical appraisal from the SGEM podcast, as well as an overview of the subsequent discussion from the SGEM blog and other social media. Through this series, we hope to enhance the value, accessibility, and application of important, clinically relevant EM research. In this, the fifth SGEM HOP hosted collaboratively with CJEM, we discuss Racine et al.’s paper describing delayed complications and functional outcomes of isolated sternal fractures after emergency department discharge.Reference Racine, Émond and Audette-Côté 3
BACKGROUND
Sternal fractures can result from significant blunt thoracic trauma, especially affecting belted drivers in motor vehicle collisions, with a reported incidence of 0.33% of trauma patients and 3.7% of patients admitted after a motor vehicle collision.Reference Recinos, Inaba and Dubose 4 , Reference Yeh, Hwabejire and Demoya 5 Poor outcomes associated with sternal fractures correlate with severity and the number of other injuries,Reference Yeh, Hwabejire and Demoya 5 and there is some literature supporting emergency department discharge of patients with isolated sternal fractures.Reference Khoriati, Rajakulasingam and Shah 6 , Reference Kouritas, Zisis and Vahlas 7 However, these fractures can result in delayed complications and poor functional outcomes.Reference Misthos, Kakaris and Sepsas 8 , Reference Émond, Sirois and Guimont 9
ARTICLE SUMMARY
Racine et al.Reference Racine, Émond and Audette-Côté 3 conducted a prospective cohort observational study in four university-affiliated hospitals in Montreal and Quebec City, Quebec. They compared delayed complications of sternal fractures with other minor thoracic traumatic injuries in those discharged directly from the emergency department. The study took place from 2006 to 2010, and their analysis was a preplanned sub-analysis of a larger project.
The population studied was patients age 16 years and over who sought care within 3 days of injury and were diagnosed with either isolated sternal fracture or other minor thoracic injury, defined as chest abrasion, chest contusion, or rib fracture. Patients with hemothorax, pneumothorax, lung contusion, or any significant cerebral, thoracic, abdominal, or extremity injury were excluded, as were those who were unable to complete follow-up. Patients received standard care as decided by their treating physician and were given follow-up medical evaluations at 7 and 14 days post-injury. At the postdischarge follow-up, their pain severity was recorded, they were clinically examined, and a chest X-ray was performed. Delayed complications included a hemothorax, pneumothorax, atelectasis, and lung contusion. Research nurses performed 30- and 90-day telephone interviews to assess pain severity, functional status, and complications.
The primary end points were delayed hemothorax, as identified by a blinded radiologist on chest X-ray, and functional status at 30 and 90 days, as assessed using the Medical Outcome Short-Form Health Survey (SF-12). Secondary end points included aggregated scores of the physical health summary (PHS) and mental health summary (MHS) from the SF-12, role limitations, physical functioning, and overall body pain.
KEY RESULTS
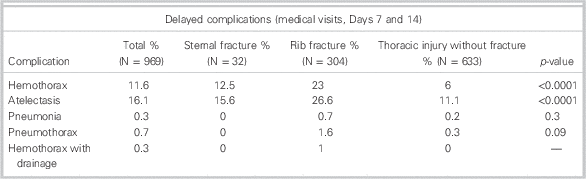
The authors concluded that delayed hemothorax and atelectasis were both more common in rib fracture than in sternal fracture (Table 1). However, physical disability was greater after sternal fracture (average score 30.2 v. 35.2 and 39.2 in the other groups out of a possible 47), and more patients with sternal fracture had persistent disability at the end of the follow-up period. The mean physical functioning scores were lower, role limitations were greater, and overall body pain was significantly higher in the sternal fracture group.
Table 1 Delayed complications of thoracic injuries
QUALITY ASSESSMENT – SUMMARY OF THE SGEM POST-PUBLICATION CRITIQUE
The study by Racine et al. was a large, prospective cohort comparing delayed complications and functional outcomes after sternal fracture and other minor thoracic trauma. This was a sub-analysis of a larger study, but one which was preplanned and with clearly defined end points. The inclusion and exclusion criteria were appropriate, and the number lost to follow-up at 30 and 60 days was within acceptable ranges for prospective cohort trials.Reference Kristman, Manno and Côté 10 The functional outcomes and pain scales were patient-centred outcomes that strengthened the analysis. Nevertheless, this study has several limitations.
One of the major limitations of trauma research is the inability to accurately assess pre-injury status. In this study, pre-injury functional status and pain could have elucidated the impact of thoracic injuries through a change in functional status, strengthening the analysis. With a prospective design, this could have been assessed at the first data collection moment as a retrospection on pre-injury status, which, although not as reliable as an assessment that actually preceded the injury in time, it could have been a close proxy that would reduce potential bias from baseline differences in functional status and pain.
The existence of hemothorax was implied by the surrogate marker of a pleural effusion on the follow-up chest X-ray. Although it may be reasonable to assume in an otherwise healthy patient that such a finding post-thoracic injury represents a hemothorax, in their population, approximately 25% of each group had at least one (unspecified) comorbidity, some of which could potentially cause pleural effusion. A confirmatory test, such as pleurocentesis, ultrasound, or computed tomography (CT), would have strengthened the assertion that the fluid collections seen were hemothoraces.
Diagnostic methods for thoracic injury may have introduced bias into this study. It is not stated how many patients received chest CT scans and how many were evaluated with X-ray only. A chest CT has substantially better sensitivity for diagnosing rib fractures, and many may have been missed using only X-ray, resulting in systematic group misallocation.
The clinical importance of delayed complications was not measured using a standard instrument. Interventions were at the discretion of the treating physicians, without any guidance or protocols as to standards of care. This may have introduced a large degree of variability in clinicians’ practice, although it is unclear whether this would systematically favour intervention in one group over another. Physicians were also not blinded to the nature of the thoracic injury, and physician perception of injury severity or familiarity with the management of late complications could have influenced decisions of whether to treat. It is notable that sternal fracture was much rarer than rib fracture, so there is a strong possibility that physician familiarity with post-injury management may have differed significantly between those groups. The number of interventions was very low, and the absolute number of hemothoraces identified in each group differed substantially, complicating the interpretation of this outcome.
Although a large number of patients were included in the study, a very small percentage of the total actually presented with isolated sternal fracture (32, or 0.03%). Given that this was the injury of interest, a larger number of cases would be needed for a more robust assessment of the rate of delayed complications.
The study groups were not equivalent in their demographic characteristics in ways that are likely unavoidable in this type of research. The authors accounted for this by adjusting variables for age and sex, which is appropriate given the differences. There was also substantial loss to follow-up at 90 days, which was worse in the sternal fracture group (50%) than the other two groups (80% followed up). Also, although those lost to follow-up were similar in terms of demographics, the loss of these datapoints makes the 90-day data less reliable.
SGEM TAKE-TO-WORK POINTS
Sternal fractures are rare injuries and, when found in isolation, are associated with significant functional limitations and pain in the months following injury. However, delayed clinical complications of sternal fractures are rare, and this study supports discharge of these patients after the initial emergency department evaluation. The results of this study are difficult to interpret given the rarity of studied outcomes, differences in the populations, and the influence of clinician decisions in management. Despite the limitations, it is noteworthy that Racine et al.’s work is the largest prospective study to date on isolated sternal fracture.
METHODS OF THE SOCIAL MEDIA RESPONSE ANALYSIS
The blog post and podcast were launched on September 21, 2016, and the social media discussion continued for one week until September 28, 2016. Listeners and viewers were invited to comment on the article through the podcast audio, the blog post text, and on Twitter and Facebook.
The social media responses found in the SGEM blog comments, the SGEM Facebook page, and on Twitter (directed at using the #SGEMHOP hashtag) between September 21 and 28, 2016, were reviewed by the authorship team. HL compiled and reviewed all social media commentary and conducted a thematic analysis of tweets and posts related to the SGEM podcast and blog post. The qualitative framework approach used is described in Table 2.Reference Wu, Thompson and Aroian 11 - Reference Burnard, Gill and Stewart 17
Table 2 Framework approach for thematic analysis – methods

Multiple metrics of dissemination were further tracked by the SGEM HOP team for analysis. Blog post page views were monitored using the Jetpack plugin by Wordpress.com (available at: https://wordpress.org/plugins/jetpack/). Facebook “reach” analytics were provided by Facebook and represented the number of users who saw the original SGEM Facebook post on their own newsfeeds. 18 Twitter impressions (the number of users whose newsfeeds contained a tweet featuring the #SGEMHOP hashtag) were tracked using Symplur, a software program that monitors health–care-related Twitter conversations.Reference Symplur 19 Tweets not containing the hashtag were not tracked by Symplur. The number of impressions was calculated by taking the number of tweets per Twitter user using the #SGEMHOP hashtag and multiplying it by the number of followers of each participant. The Altmetric score, a proprietary, standardized tool that tracks the disseminative impact of research articles in social media forums (e.g., Facebook, Twitter) and on blogs, podcasts, and news outlets 20 - Reference Warren, Raison and Dasgupta 22 , was also used. The Altmetrics of the featured article by Racine et al.Reference Racine, Émond and Audette-Côté 3 were compared to all other articles published in CJEM and all published research analysed by Altmetric. 20
RESULTS OF THE SOCIAL MEDIA RESPONSE
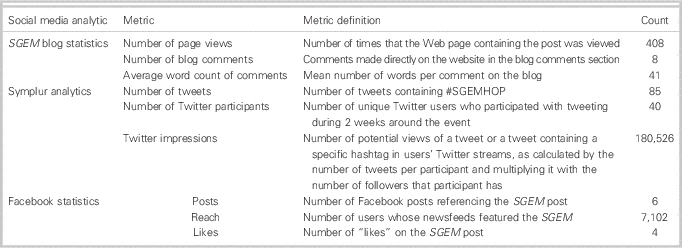
Table 3 provides details on the social media reach of Racine et al.’s articleReference Racine, Émond and Audette-Côté 3 during the SGEM HOP campaign. During the 1-week period following the podcast release, #SGEMHOP was used in 85 tweets by 40 individual users, resulting in 180,526 Twitter impressions. Sixteen of these tweets were from the study’s authors or CJEM personnel. The online discussion at the SGEM blog and through Twitter remained active for 14 days following release of the podcast. The article by Racine et al. received an Altmetric score of 44, placing it as the 9th highest of ranked CJEM publications and in the 97th percentile and in the top 5% of all research outputs scored. Prior scores for SGEM HOP featured that articles were in the 41-71 range.
Table 3 Aggregate analytic data of social media platform discussions following the SGEM blog posting
ONLINE DISCUSSION SUMMARY
The discourse around this article was conducted entirely on the SGEM blog, with the link disseminated through Twitter and Facebook. Eight comments were submitted to the blog from five original contributors, including feedback from the study’s primary author Samuel Racine.Reference Racine, Émond and Audette-Côté 3 A few themes arose from the discussion, including uncertainty about the clinical relevance of end points, general comments about study methodology limitations, and the perception of good external validity among commenters (Table 4).
Table 4 Framework approach for thematic analysis – results

Issues of clinical relevance arose, including Kirsty Challen’s comment that “[I] think we tend to be more worried about blunt cardiac injury with sternal fractures.” However, several individuals felt these results were consistent with their clinical practice and that of other physicians in their institutions, such as “Thoracic” Rick’s assertion that “the results are consistent with our own experience. Sternal fractures rarely require operative repair…(or) any additional interventions.”
Comments about study methodology were nonspecific. Anand Swaminathan commented, “Although there are some key limitations in the data as you raise…”; Thoracic Rick pointed out the “small numbers and numerous biases,” but these were elucidated in the podcast, and commenters did not add further to this topic.
The Twitter and Facebook response to the SGEM podcast and blog consisted solely of reposts of its URL. There was no exchange of ideas relating to the article on the Twitter or Facebook platforms.
It is difficult to speculate the reason for limited social media discussion of this particular article and critical analysis, because prior SGEM posts have generated more response. The content of the posts made suggests that the topic is of interest but rarely encountered, so perhaps the majority of the readers had a paucity of professional experience upon which to comment. The article also presented a fairly high quality of evidence for the general trauma literature, and the depth of the critical analysis by SGEM may have adequately addressed the majority of potential comments by readers. The conclusions of the study also seemed to support the practice of those who responded, and if those responses are to be taken as representative of the opinions of other readers, perhaps the article was not controversial enough to generate vigorous discussion.
LIMITATIONS OF SOCIAL MEDIA ANALYSIS
The study of social media engagement is inherently limited by several factors. In this instance, small numbers did not allow for a robust analysis, and nonspecific remarks did not generate a great deal of discussion. These analyses are confounded by selection bias, because the online community self-selects to comment and tends to represent a small subset of emergency physicians who engage heavily in free open access medical education (FOAMed) activities. The opinions of the wider audience may consistently differ from this group, in particular, a generational effect is likely evidence between the comfortable computer and Internet users and those who consume journal materials in print form (although there is not yet literature addressing this topic).
Social media analytic scores offer the ability to quantify article dissemination but lack context about the quality of resultant discussion.Reference Eysenbach 23 - Reference Fox, Gurary and Ryan 25 This is evidenced by a closer review of the #SGEMHOP hashtag, which only included directions to view the blog and did not offer material contribution to the discussion.
Although here we have summarized the social media discourse and original paper, it behooves the reader to conduct an independent critical evaluation of the primary source and its social media feedback.
CONCLUSION
Racine et al.’s paperReference Racine, Émond and Audette-Côté 3 elucidates the delayed complications and functional outcomes of isolated sternal fractures relative to other minor thoracic injuries, with some caveats regarding methodology and loss to follow-up. The SGEM blog post and podcast offered a readily digestible summary of the article, drawing attention to key limitations in methodology. The online distribution of the article and blog post and podcast resulted in a conversation that affirmed the external validity of the study results while continuing to question the methodology and clinical relevance of the chosen outcomes. This type of online engagement by academic experts and authors of primary literature is instrumental in increasing the general awareness of primary literature among emergency physicians, improving the critical appraisal of findings, and helping with interpretation of research to enhance its applicability in clinical practice.
Keywords: sternal fracture, trauma, thoracic trauma, chest trauma, discharge, FOAMed, EBM, evidence based medicine, social media
Competing interests: None declared.








