Patient navigation is an emerging phenomenon of interest in health care as an approach to provide effective care coordination and enhanced patient satisfaction (Calhoun et al., Reference Calhoun, Whitley, Esparza, Ness, Greene and Garcia2010). A major recommendation from the Parliamentary Committee on Palliative and Compassionate Care is that navigators are needed to guide individuals with advanced illness and their families through the complexities of the health care system (Parliamentary Committee on Palliative and Compassionate Care, 2011). In particular, there is a critical need to have skilled navigators in rural settings. For rural older persons, the realities of dying and death include isolation, lack of services, the necessity of commuting for care, and high levels of caregiver burden (Castleden, Crooks, Schuurman, & Hanlon, Reference Castleden, Crooks, Schuurman and Hanlon2010; Crooks & Schuurman, Reference Crooks and Schuurman2008; Duggleby et al., Reference Duggleby, Penz, Goodridge, Wilson, Leipert and Berry2010, Reference Duggleby, Penz, Leipert, Wilson, Goodridge and Williams2011; Goodridge & Duggleby, Reference Goodridge and Duggleby2010; Lockie, Bottorff, Robinson, & Pesut, Reference Lockie, Bottorff, Robinson and Pesut2010; McKee, Kelley, Guirguis-Younger, MacLean, & Nadin, Reference McKee, Kelley, Guirguis-Younger, MacLean and Nadin2010; Robinson, Pesut, & Bottorff, Reference Robinson, Pesut and Bottorff2010; Robinson et al., Reference Robinson, Pesut, Bottorff, Mowry, Broughton and Fyles2009; Wilson, Truman, et al., Reference Wilson, Truman, Thomas, Fainsinger, Kovacs-Burns and Frogatt2009). Palliative care services are lacking in rural Canada and, along with a lack of other health care services, have caused inequities in access to services in rural communities that are not experienced in urban areas (Robinson et al., Reference Robinson, Pesut and Bottorff2010).
Although several models of navigation exist in the literature (Case, Reference Case2011; Fillion et al., Reference Fillion, Cook, Veillette, Aubin, de Serres and Rainville2012; Pedersen & Hack, Reference Pedersen and Hack2011), they were developed for cancer care, not palliative care, and they do not appear to reflect the unique issues of rural older adults with advanced illness. Rural and urban comparisons are difficult because of the diversity of rural contexts (Keating, Reference Keating2008). However, in studying rural contexts there appear to be some commonalities that suggest there are unique issues for a person with advanced illness. For example, McKee et al. (Reference McKee, Kelley, Guirguis-Younger, MacLean and Nadin2010) suggested that in rural contexts, when a person is dying, the entire community is affected, and care for the dying person is an expression of reciprocity that characterizes rural community life. Thus, the conceptualization and subsequent development of navigation competencies specific to the care of older persons living in rural areas with advanced illness is an important step to improve older persons’ quality of life.
In this article, we describe a four-phased Delphi process conducted with experts in rural aging, rural palliative care, and navigation, as well as with community stakeholders, to develop navigation competencies specifically oriented to the care of older persons with advanced illness and their families living in rural areas.
Background
The focus of the navigation competencies literature has been on cancer care. In cancer care, the goal of patient navigation is to address cancer health disparities by eliminating barriers to diagnosis, treatment, and services for vulnerable populations who have limited or difficult access to health care resources (Calhoun et al., Reference Calhoun, Whitley, Esparza, Ness, Greene and Garcia2010). The term navigator has been applied to any type of service that assists individuals in overcoming obstacles from screening to treatment, and in coping with challenges during survivorship (Wells et al., Reference Wells, Battaglia, Dudley, Greene, Calhoun and Mandelblatt2008). One of the major challenges in the literature is the lack of a generally accepted definition for patient navigation and very little consensus on the actual roles and responsibilities of navigators (Wilcox & Bruce, Reference Wilcox and Bruce2010). The literature also uses the terms patient navigation program and patient navigator interchangeably. In the Canadian health care system, navigators have been called case managers, clinical coordinators, cancer support nurses, follow-up nurses, breast specialists, breast cancer coordinators, and patient navigators (Fillion et al., Reference Fillion, Cook, Veillette, Aubin, de Serres and Rainville2012).
The Canadian Partnerships Against Cancer (CPAC) (2012) and the National Case Management Network (NCMN) (2012) have developed definitions of navigation and related competencies. CPAC (2012) has defined navigation as “a system of services and resources that are mobilized based on the immediacy and severity of patients’ needs. It is a proactive, intentional process of collaborating with a person and his or her family to provide guidance as they negotiate cancer care” (p. 6). The focus of the CPAC navigation definition and resulting competencies have been on patient needs and cancer care. Accordingly, this definition and resulting competencies may not be applicable to rural palliative care for multiple reasons. For example, palliative care utilizes a family-centred approach (Canadian Hospice Palliative Care Association, 2013a), so care is provided to both the family and patient. Although the CPAC definition does include the family, the competencies clearly have a patient focus for cancer treatment. Navigation competencies are needed that also include screening and access to services to support for family members.
The CPAC navigation definition and competencies have a focus on cancer care. Palliative care services include many chronic conditions, not only cancer, and traditionally exceed conventional definitions of health care to include social, psychological, and spiritual care (Canadian Hospice Palliative Care Association, 2013b). Additionally, cancer care emphasizes treatment whereas the palliative approach emphasizes quality of life as a goal (World Health Organization, 2013). Consequently, navigation competencies in cancer care will have a significantly different focus than those needed in rural palliative care.
Rural Canada has very few health care services in general (Robinson et al., Reference Robinson, Pesut, Bottorff, Mowry, Broughton and Fyles2009), so navigation specific to this population should include accessing other community resources (in addition to health), and informal services. The NCMN (2012) has viewed navigation as helping clients to navigate the health and social care system by working with their networks to identify and address barriers. The NCMN identifies two key case management navigation competencies: (a) anticipate, identify, and help remove barriers to holistic care; and (b) facilitate safe and effective connections to services across settings. This definition recognizes the importance of the social care system and networks in addressing barriers to care, which is more reflective of rural aging. However, it does not address important concepts in rural aging described by Keating, Swindle, and Fletcher (Reference Keating, Swindle and Fletcher2011) such as aging well, and the contributions that older adults make to their family, friends, and community. A definition and competencies of navigation for the care of older adults residing in rural areas are needed that reflect important rural aging concepts and perspectives. The purpose of this project was to develop health care provider competencies specific to the care of older persons with advanced illness living in rural areas.
Method
There were two main stages in the development of the navigation competencies: a discussion paper and a four-phased Delphi process. The first stage involved writing a discussion paper on rural aging and rural palliative care based on a literature review (described in more detail later). This paper identified important considerations in the development of the competencies. From this discussion paper, the research team developed a conceptual definition of navigation and identified its purpose and goals.
Delphi Process
The second stage was a four-phased Delphi process suggested by Linstone and Turoff (Reference Linstone and Turoff2002) to develop the competencies.
Participants
The research team identified potential members of an international expert panel of researchers, knowledge users, and community stakeholders based on the inclusion criteria. The inclusion criteria for the expert panel were persons who had experience or expertise in rural palliative care, rural aging, or navigation. Team members sent the names and contact information of potential panel members to the Principal Investigator (PI). The PI then contacted potential panel members via email to determine if they were willing to participate in the process. They were provided with information about the purpose of the project and the Delphi process procedures. A return email agreeing to participate served as consent for the study. Thirty researchers, health care professionals, and community stakeholders were approached, and all agreed to participate.
Data Collection
In the first phase of the Delphi process, panel members were sent an email with a copy of the discussion paper and were asked to identify possible competencies for each of the navigation dimensions identified in the discussion paper. Their answers were then collated by the PI and her research coordinator and categorized into general areas of competencies (GACs). In the second phase, panel members were contacted via email and asked to rank all the specific competencies in each GAC in order of importance. The top five ranking competencies were then retained. In the third phase, panel members were asked via email to evaluate the competencies for importance of inclusion using a consensus tool. Competencies had to receive a 75 per cent consensus from expert panel members to be retained. A competency was removed if it ranked lower than the 75 per cent threshold.
The fourth phase of the Delphi process was a face-to-face meeting with 24 of the expert panel’s members involved in the first three phases of the Delphi process, including decision makers, knowledge users, researchers, and rural community members. Six panel members were unable to attend. The goal of the fourth phase was to achieve consensus around a preliminary set of navigation competencies for the care of older rural adults with advanced illness and their families. Two facilitators who were experts in a process of developing competencies guided the process. They utilized a process entitled “Developing a Curriculum (DACUM)” (Norton, Reference Norton1997) whereby expert practitioners are assembled to consider a job, vocation, role, or courses of studies in their field. In this case, the DACUM process was used to describe the navigation skills necessary for the care of older rural adults with advanced illness and their families.
Results
Stage 1: Discussion Paper
In order to define navigation and identify challenges and issues to consider for the care of older rural adults, we completed a discussion paper on aging, rural palliative care and navigation. The full discussion paper can be viewed at www.nurs.ualberta.ca/livingwithhope. Considerations for navigation competencies identified in the discussion paper included the following: (a) finding the “best fit” for the older person and their environment (Keating, Reference Keating2008; Keating, Eales, & Phillips, Reference Keating, Eales and Phillips2013; Keating, Swindle, & Fletcher, Reference Keating, Swindle and Fletcher2011); (b) filling the need to foster independence (Duggleby et al., Reference Duggleby, Penz, Leipert, Wilson, Goodridge and Williams2011; Pesut, McLeod, Hole, & Dalhuisen, Reference Pesut, McLeod, Hole and Dalhuisen2012; Wilson, Fillion, Thomas, Justice, Bhardwaj, et al., Reference Wilson, Fillion, Thomas, Justice, Bhardwaj and Viellette2009); (c) fostering community connections (Crooks & Schuurman, Reference Crooks and Schuurman2008; Duggleby et al., Reference Duggleby, Penz, Leipert, Wilson, Goodridge and Williams2011; McKee et al., Reference McKee, Kelley, Guirguis-Younger, MacLean and Nadin2010; Robinson et al., Reference Robinson, Pesut and Bottorff2010; Wilson, Fillion, Thomas, Justice, Veillette, et al., Reference Wilson, Fillion, Thomas, Justice, Veillette and Bhardwaj2009); (d) accessing both formal and informal services (Kelley, Reference Kelley2007; Robinson et al, Reference Robinson, Pesut, Bottorff, Mowry, Broughton and Fyles2009); (e) applying a family-centric approach (Canadian Hospice Palliative Care Association, 2012; Duggleby et al., Reference Duggleby, Penz, Goodridge, Wilson, Leipert and Berry2010, Reference Duggleby, Penz, Leipert, Wilson, Goodridge and Williams2011; Robinson, Pesut, & Bottorff, Reference Robinson, Pesut and Bottorff2012); and (f) focusing on the palliative approach with quality of life as a goal (Canadian Hospice Palliative Care Association, 2013b).
“Best fit” is a concept that reflects the diversity of rural communities, older persons, and their interactions with the environment (Keating et al., Reference Keating, Eales and Phillips2013). Although people are continuously interacting with the physical and social contexts in which they live, they are not passive recipients (Keating, Reference Keating2008). Instead, older adults, through their responses to their contexts, and at times through purposeful interactions, change the contexts in which they live. For example, an older adult may decide to participate in a social activity and as a result expand their network. Thus, older adults interact with their environment in ways that are critical to their health and well-being (Keating, Reference Keating2008). With the diversity of older adults and their communities, it is important to consider both the best fit between the needs of the older adults in a given community and the community resources available to them (Keating et al., Reference Keating, Eales and Phillips2013).
Rural persons’ connection to their communities and their need for independence were found to be equally and highly valued by rural populations (Duggleby et al., Reference Duggleby, Penz, Leipert, Wilson, Goodridge and Williams2011). For example, in an ethnographic study, Wilson et al. (Reference Wilson, Fillion, Thomas, Justice, Bhardwaj and Viellette2009a) found that a good rural death was defined against the backdrop of rural community values in terms of independence and community connections. Accordingly, fostering community connections and helping older persons maintain independence as much as possible were viewed as important aspects of navigation.
Another consideration for the navigation competencies was the use of a family-centred and palliative approach. The palliative approach views patient/family (family-centred approach) as the unit of care with the goal of optimizing quality of life for both the patient and family. As well, it reflects a shift from specialist-led models to a generalist multidisciplinary approach (Canadian Hospice Palliative Care Association, 2013b). There is a debate in the literature, particularly among rural physicians, about whether palliative care should be delivered through a specialist or a generalist model in rural settings (Robinson et al., Reference Robinson, Pesut and Bottorff2010). The lack of physicians in many rural areas in Canada also means there are few palliative care specialists (Kaasalainen et al., Reference Kaasalainen, Brazil, Williams, Wilson, Willison and Marshall2012). There is also a debate in the literature as to whether the primary responsibility for palliative care should rest on formal specialists, or it should be a fundamental part of all primary care. The Canadian Hospice Palliative Care Association (2013b) suggests that a palliative approach that integrates the palliative ideals into primary care will increase the access to some palliative care services in Canada.
In working together to write the discussion paper, our research team developed the definition of rural navigation as a framework to guide the development of the competencies. Rural navigation is working in collaboration with patients, families, and communities (a) to negotiate the best fit between the needs of older rural persons, their families and communities, and available resources; (b) to improve access to needed informal and formal services and resources at the end of life (including death) and bereavement; (c) to promote quality of life; (d) to support independence; and (e) to facilitate community connections utilizing a family-centric, culturally safe, palliative approach.
The principles underpinning this conceptual definition were then translated into proposed goals of navigation which included (a) promoting an optimal quality of life (physical, emotional, psychological, relational, financial, existential, and spiritual), (b) fostering independence, and (c) facilitating community connections. These goals are also congruent with the rural aging literature that identified an important rural lens through which to view rural navigation: quality of life, independence, and social connections (Keating et al., Reference Keating, Swindle and Fletcher2011).
Stage 2: Delphi Results
In the first phase of the Delphi process, the participants brainstormed 66 competencies which were then grouped into five general area competencies (GACs). These GACs were as follows: (a) provide patient/family screening, (b) advocate for patient/family, (c) facilitate community connections, (d) coordinate access to services and resources, and (e) promote active engagement. Associated with each GAC were more-specific competencies. Panel members were asked to rank all the specific competencies in each GAC in order of importance (phase two). The top ranked 5 in each GAC were then sent to the expert panel members for phase three (25 competencies).
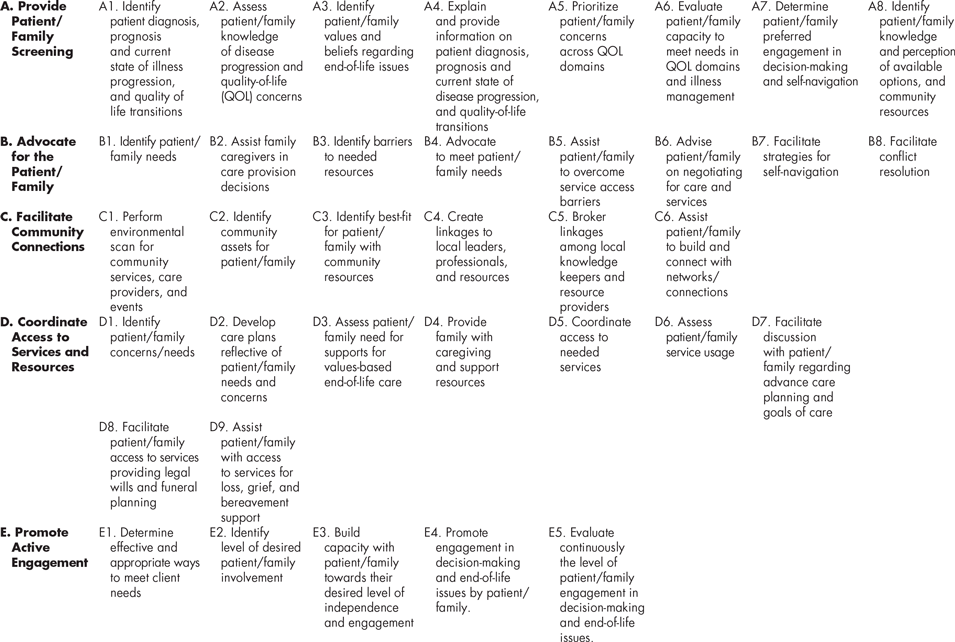
In phase three, we evaluated the competencies for importance of inclusion. Only one competency was removed during this process, as it ranked below the 75 per cent inclusion criterion resulting in 24 specific competencies. The competency that was removed was “encourage development of family/friend/community resource-based plans with minimal dependence upon professional support”. It was not considered to be important to be included as there was another similar competency. In phase four at the face-to-face consensus meeting, both the general area and the specific competencies were reviewed once more with the addition of 12 more specific competencies. Consensus of the competencies that are important for rural navigation of older persons was achieved. These competencies are called “Navigation Competencies for Rural Older Adults (NCROA)” (Table 1) which included a contextual statement and definitions as well as five GACs and 36 specific navigation competencies. The contextual statement was as follows: The competencies reflect a family-centric approach, in that they are focused on the patient and family. Provision of navigation services commences when an older adult is deemed palliative (see definition below) and extends through bereavement.
Table 1: Navigation Competencies for Rural Older Adults (NCROA)

Definitions
(1) Patient refers to older adults with advanced illness whether they are at home, in a long-term care or an acute care facility.
(2) Quality of life domains include these: physical, emotional, psychological, relational, financial, existential, and spiritual.
(3) Services for older adults may include these: psychosocial, emotional, spiritual, and physical supports to enable desired level of independence.
(4) Generalist health care providers are professionals who have training and provide palliative care, but are not considered specialists in palliative care.
(5) Family is defined broadly as relatives, friends, and neighbors.
(6) Palliative is defined as a person whose health care provider would not be surprised if they were to die in the next 6–12 months.
Table 1 presents the NCROA consisting of five GACs (A-E) which are not listed in order of importance or sequence. These GACs (a) provide patient/family screening, (b) advocate for the patient/family, (c) facilitate community connections, (d) coordinate access to services and resources, and (e) promote active engagement. Within each GAC are five to nine specific competencies that further delineate and describe the GACs. Figure 1 is a visual representation of the five GACs and their integration into the conceptual definition of navigation for older rural adults with advanced illness and their family. Quality-of-life priorities guide the navigation competencies which, within a context of best fit and the palliative approach, results in connecting older adults and their families with resources. The goal of navigation is optimal quality of life, independence, and community connections.

Figure 1: Navigation model representing the five general areas of competencies (GACs) and the conceptual definition of navigation for older rural adults with advanced illness and their families
Discussion
The NCROA conceptual definition and competencies, developed through the two stages of a discussion paper and a four-phased Delphi process, reflects the values of independence, quality of life, and community connections, along with a family-centric and palliative approach. As a result, it differed significantly from the definitions and competences developed by the Canadian Partnerships Against Cancer (CPAC; 2012) and the National Case Management Network (NCMN; 2011). For example, the importance of independence resulted in a GAC entitled “promoting active engagement” and a specific competency under the “advocate for the patient/family” category of facilitating strategies for self-navigation. Facilitating self-navigation is similar to the NCMN competencies that include coaching clients and social networks to self-navigate the health and social systems. The CPAC competencies focus on self-management of the disease and not self-navigation of the health care and social systems. In contrast, the NCROA guidelines include promoting active engagement of the patient and family by building their capacity to meet (a) their desired levels of independence and engagement in achieving their quality-of-life goals, and (b) promoting engagement in decision-making.
Another significant difference among NCROA competencies and those of CPAC and NCMN is the goal of improving quality of life of older rural persons and their families with advanced illnesses. For example, in all three areas (NCROA, CPAC, and NCMN) screening and or assessment is mentioned. The focus of the screening/assessment is usually on unmet needs, and on knowledge and assessment of the progression of disease. However, NCROA also includes the assessment of patient and family quality-of-life concerns. Moreover, information provided by the navigator does include information about the disease, but also about possible transitions in quality of life. The navigator also works with the patient/family to prioritize their quality-of-life needs.
Another unique GAC is entitled “facilitating community connections”. The specific competencies within this GAC focus not only on finding community resources, but also on how to work with the patient/family to connect and or reconnect with the community. Although there is potential for the competencies to apply to both urban and rural areas, this competency in particular reflects the possible requirement for a different approach in a rural community for older persons and their families. For example, staying connected with the community has been found to be very important to rural older persons and their families (Duggleby et al., Reference Duggleby, Penz, Leipert, Wilson, Goodridge and Williams2011; Keating et al., Reference Keating, Eales and Phillips2013).
Throughout NCROA, there is evidence of a family-centred approach. There is, for example, assessment of patient/family values and beliefs, knowledge of diagnosis and disease progression, and quality-of-life transitions. Navigators need to have the knowledge and skills to screen, advocate, and coordinate access to resources and services and to facilitate community connections for families of older rural persons with advanced illnesses. The health of rural family caregivers of persons with advanced illness has been found to be poor (Duggleby et al., Reference Duggleby, Williams, Holtslander, Thomas, Cooper and Hallstrom2014; Robinson et al., Reference Robinson, Pesut and Bottorff2010), so is naturally of concern to health care providers and policy makers. Moreover, a family-centric approach is also in keeping with the palliative approach as outlined by the Canadian Hospice Palliative Care Association (2013a) report on family caregiving.
The palliative approach is also evident throughout NCROA. For example, under the GAC “coordinate access to services and resources”, there are specific competencies in relation to accessing services for loss, grief, and bereavement support, legal wills, and funeral planning, as well as for advanced care planning and goals of care. The focus on quality of life throughout the competencies also reflects the palliative approach.
Limitations
There are limitations to the approach we used to develop NCROA. The first is that the discussion paper was not a systematic review of research studies in the area but an integrative review of research and policy papers. The purpose of the discussion paper was to identify issues, rather than to identify gaps in knowledge, regarding the areas of rural aging, rural palliative care, and navigation. As well, although we reviewed navigation programs in the literature, the focus of the discussion paper was the specific competencies that have been developed and validated in Canada. A final limitation is that the NCROA conceptual definition and resulting competencies are a reflection of the expert panel and require further validation.
Conclusion
The discussion paper provided the basis for the NCROA navigation framework and definition, which guided the development of navigation competencies for caring for rural older adults and their families with advanced illness. In addition, the Delphi process was successful in bringing together experts in rural aging, rural palliative care, and navigation, along with health care providers and community partners, to inform the development of the competencies. Without this initial ground-breaking work, the competencies would not have reflected the current and critical knowledge of rural aging, rural communities, rural palliative care, and navigation. Future research is needed to validate and evaluate the competencies.
The navigation competencies were specifically designed to help health care providers in assisting rural older palliative patients and their families in ways that honour and respect rural communities and values. Ultimately, these navigation competencies represent a commitment to achieving equity of care for rural older adults and their families with advanced illness. The process we used to develop the conceptual understanding of navigation in this population and the resultant competencies may be of use in the development of navigation competencies for other populations.