INTRODUCTION
The use of filtration and disinfection to make clean water widely available has been recognized as one of the greatest US public health achievements of the 20th century [1, 2], and is credited with an estimated 50% of the reduction in mortality in major cities and nearly two-thirds of the decrease in child mortality observed in the early 1900s [Reference Cutler and Miller3]. Although classic drinking water-associated diseases such as cholera and typhoid fever have become rare, water usage in the USA has become more complex; waterborne disease is now associated with recreational, industrial, healthcare, agricultural, and medical uses. As a result, although transmission patterns have changed, waterborne illness remains a public health problem in the USA.
The magnitude of waterborne disease in the USA is thought to be substantial but is not well quantified. Almost 1400 outbreaks have been reported to the Centers for Disease Control and Prevention (CDC) since the current surveillance system was created in 1971 [Reference Yoder4, Reference Yoder5]. Estimates of gastrointestinal illness caused by drinking water from public water systems fall between 4 and 33 million annual US cases [Reference Messner6, Reference Colford7], but no overall estimate of the total burden from all water pathways exists. A more complete accounting would include illness from recreational water exposures, industrial exposure, and the built environment. Aerosolized mists generated in hospital and other building cooling and water distribution systems can contain pathogens such as Legionella [Reference Diederen8] and non-tuberculous mycobacteria (NTM) [Reference Falkinham9, Reference Thomson10]. Thus, Legionnaires' disease and NTM infections are serious illnesses primarily transmitted by water although the transmission pathway differs from that of gastrointestinal infections spread through drinking water. The burden of illness due to swimming and other recreational water exposure also appears extensive. Swimmers at southern California beaches were estimated to have experienced 689 000–4 003 000 gastrointestinal illness episodes and 693 000 respiratory illness episodes associated with contaminated water annually [Reference Brinks11], while the chlorine-tolerant parasite Cryptosporidium is estimated to cause 740 000 cases of diarrhoeal illness each year [Reference Scallan12].
A more precise quantification of the costs of US waterborne disease would be useful in prioritizing waterborne disease prevention activities and allocating limited resources, and is a key building block for determining the overall burden of waterborne disease in the USA. To begin to quantify the costs of waterborne diseases, the hospitalization costs of specific waterborne infections were estimated. This study summarizes data from three large health insurance claims databases to estimate the inpatient and outpatient cost per episode of selected waterborne diseases in the privately insured, Medicare-, and Medicaid-eligible populations and gives a national estimate of the total hospitalization costs. In a landscape of diminishing public health resources, these estimates are necessary components of any plan developed by policy-makers working to prioritize waterborne disease prevention efforts.
METHODS
Data sources for cost estimates
This analysis used data from the Marketscan® 2006 and 2007 Commercial Claims, Medicare Supplemental, and 2004 and 2005 Multi-State Medicaid databases from Thomson Reuters, the two most recent years of each database that were available at CDC. The commercial and Medicare databases contain anonymized medical and pharmaceutical insurance claim information for over 20 million employees, dependants, and retirees enrolled in primary or Medicare Supplemental insurance coverage through employers across the USA. The Medicaid database contains anonymized medical and prescription drug claims for seven million people enrolled in Medicaid programmes in eight states.
Inclusion criteria
All inpatients and outpatients in the databases whose record included an eligible diagnosis for five infections or syndromes considered to be primarily (over 50%) transmitted by water were included: International Classification of Diseases, Ninth Revision, Clinical Modification (ICD-9-CM) codes 007.1 for giardiasis, 007.4 for cryptosporidiosis, 482.84 for Legionnaires' disease, 380.10, 380.12, and 380.14 for acute or malignant otitis externa, and 031.0–031.9 for non-tuberculous pulmonary mycobacterial infection. NTM infections were further subdivided into pulmonary (031.0) and disseminated (031.2) infections. Hospitalizations and outpatient visits with ICD-9-CM code 031.0 were classified as pulmonary NTM infections and hospitalizations and visits with code 031.2 were classified as disseminated NTM infections. Because chronic otitis externa (particularly chronic otitis externa associated with suppurative otitis media) may be less likely to be waterborne, only acute (380.10 and 380.12) and malignant (380.14) otitis externa codes were included. Furthermore, for otitis externa hospitalizations, only cases with a primary diagnosis of otitis externa and no concurrent diagnosis of otitis media were included. For otitis externa outpatient visits, visits with a first or second diagnosis of otitis externa and no concurrent diagnosis of otitis media were included. Five infections or syndromes considered to be partially (<50%) transmitted by water were also included: ICD-9-CM codes 008.43 for campylobacteriosis, 003 for salmonellosis, 004 for shigellosis, 283.11 for haemolytic uraemic syndrome (HUS), and 130 for toxoplasmosis. Outpatient visits associated with an inpatient admission within 7 days were excluded from the outpatient set and included with inpatient costs.
Cost-per-case estimates
Using the Marketscan databases, the cost paid by the insurer, the out-of-pocket cost, and the sum of total payments from any source for each hospital or outpatient visit was calculated. Cost estimates included payments for prescription medication. The insurer cost for Medicare, Medicaid, and privately insured patients is the total amount paid by the insurer to the healthcare provider and excludes out-of-pocket payments (deductibles, co-payments, or co-insurance). The sum of total payments from any source is the sum of insurer payments and out-of-pocket payments. Because all enrollees in the Marketscan Medicare Supplemental database have a Medicare Supplemental insurance plan through their employer, payments from three sources (Medicare, the employer-provided supplemental plan, and out-of-pocket payments) are reported. To avoid calculating cost estimates based on a very small sample, cost estimates were not calculated for any disease with less than five patients from any payment source. Any hospitalized patient with a diagnosis code included in the list of immunocompromising conditions in the Prevention Quality Indicators Technical Specifications published by the Agency for Health Research and Quality was considered to be immunocompromised [13]. Because only two diagnosis codes were reported for outpatients, immune status was not determined. All costs were adjusted to 2007 US dollars using the Medical Care Consumer Price Index (Bureau of Labor Statistics, US Department of Labor).
National hospitalization cost estimates
To begin to quantify total waterborne disease costs, an estimate of the annual national cost of hospitalization for each disease was calculated. Because no single national surveillance system for the diseases included in this analysis exists, multiple sources were used to estimate the total cost of hospitalizations per year for each disease. The total number of hospitalizations per year for each disease was obtained from published estimates. For giardiasis, cryptosporidiosis, campylobacteriosis, salmonellosis, shigellosis, and toxoplasmosis, the estimates of Scallan et al. were used [Reference Scallan12]. For Legionnaires' disease, the midpoint (13 000 hospitalizations per year) of the range (8000–18 000) estimated by Marston et al. was used [Reference Marston14]. For otitis externa, NTM infections, and HUS, the 2006 and 2007 Healthcare Utilization Project Nationwide Inpatient Sample (NIS) was used. The NIS was also used to estimate the distribution of payers (commercial, Medicare, Medicaid, uninsured, other) for each diagnosis. The NIS is the largest all-payer database of US hospital inpatient stays. To obtain the average cost per case for all payers, the cost per case for each payer was multiplied by the corresponding proportion of payers in the NIS. The commercially insured cost per case was used for uninsured cases and cases with others types of insurance (e.g. Tricare, the military health plan).
RESULTS
This analysis included 3684 hospitalizations and 341 157 outpatient visits. Among primarily waterborne diseases, cryptosporidiosis (24%) and NTM infections (21%) had the highest proportion of immunocompromised patients; hospitalized patients with NTM infections (10·5 days) and Legionnaire's disease (10·2 days) had the longest average length of stay. The average length of hospitalization for giardiasis and otitis externa was 3 days; length of stay for cryptosporidiosis was more than twice as long (6·5 days).
Among diseases partially transmitted by water, HUS (24%) and toxoplasmosis (44%) had the highest proportion of immunocompromised patients. Average length of hospitalization for the diarrhoeal diseases campylobacteriosis, salmonellosis, and shigellosis was 4 days, while the average length of stay was greater for toxoplasmosis and HUS, infections with systemic effects (10 and 13 days, respectively).
Both hospitalization and outpatient costs per case varied by disease and by payer (Table 1). The majority of outpatient visits were for otitis externa (334 201 visits, average cost per visit $192). The most expensive primarily waterborne disease per outpatient visit was pulmonary NTM infection ($1649 per visit, commercially insured patients); the most expensive partially waterborne disease was HUS ($2591).
Table 1. Estimates of the cost (in US$) of illness per episode for selected waterborne diseases in the USA, by type of insurance
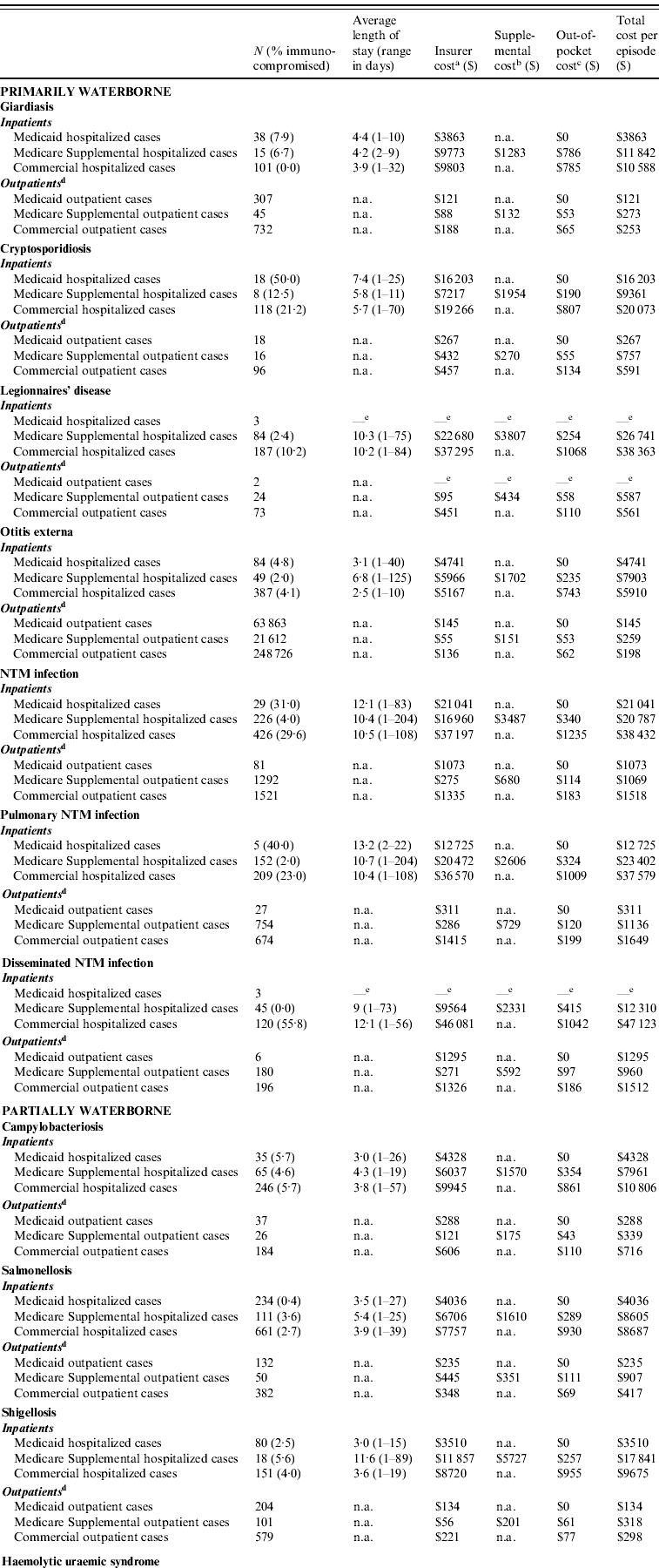
NTM, Non-tuberculous mycobacteria; n.a., not applicable.
Data sources: Marketscan 2004–2005 Multistate Medicaid and 2006–2007 Medicare Supplemental and Commercial Claims databases. All costs in 2007 US dollars.
a Insurer cost: total amount paid by the insurer to the healthcare provider.
b Supplemental cost: for Medicare enrollees, this amount includes payments from the employer-provided supplemental plan. All patients in the Marketscan Medicare Supplemental database are enrolled in an employer-provided supplemental plan. For persons without a supplemental plan, this would most likely represent an out-of-pocket cost.
c Out-of-pocket cost: total amount paid by the insured person, including deductibles, co-payments, and co-insurance.
d Outpatient visits associated with an inpatient admission within 7 days were excluded from the outpatient set and included with inpatient costs.
e Costs were not reported for groups of <5 cases.
Over 40 000 hospitalizations for primarily waterborne diseases were estimated to occur annually (Table 2). Legionnaires' disease ($33 366) and NTMs ($25 985) had the highest cost per episode of primarily waterborne diseases. The cost of hospitalization for cryptosporidiosis was nearly twice the cost of giardiasis or otitis externa. Nationally, insurers paid an estimated $434 million in hospitalization claims annually for Legionnaires' disease alone. Over $250 million in annual hospitalization costs for Medicare patients were due to Legionnaires' disease and pulmonary NTM infection, two diseases that disproportionately affect the elderly. Among partially waterborne diseases, hospitalization for HUS ($51 261) and toxoplasmosis ($44 705) were the most costly. Average hospitalization costs for campylobacteriosis ($8915), salmonellosis ($7687), and shigellosis ($8721) were lower.
Table 2. Estimates of the annual prevalence and total cost (in US$) of hospitalizations for selected waterborne diseases in the USA
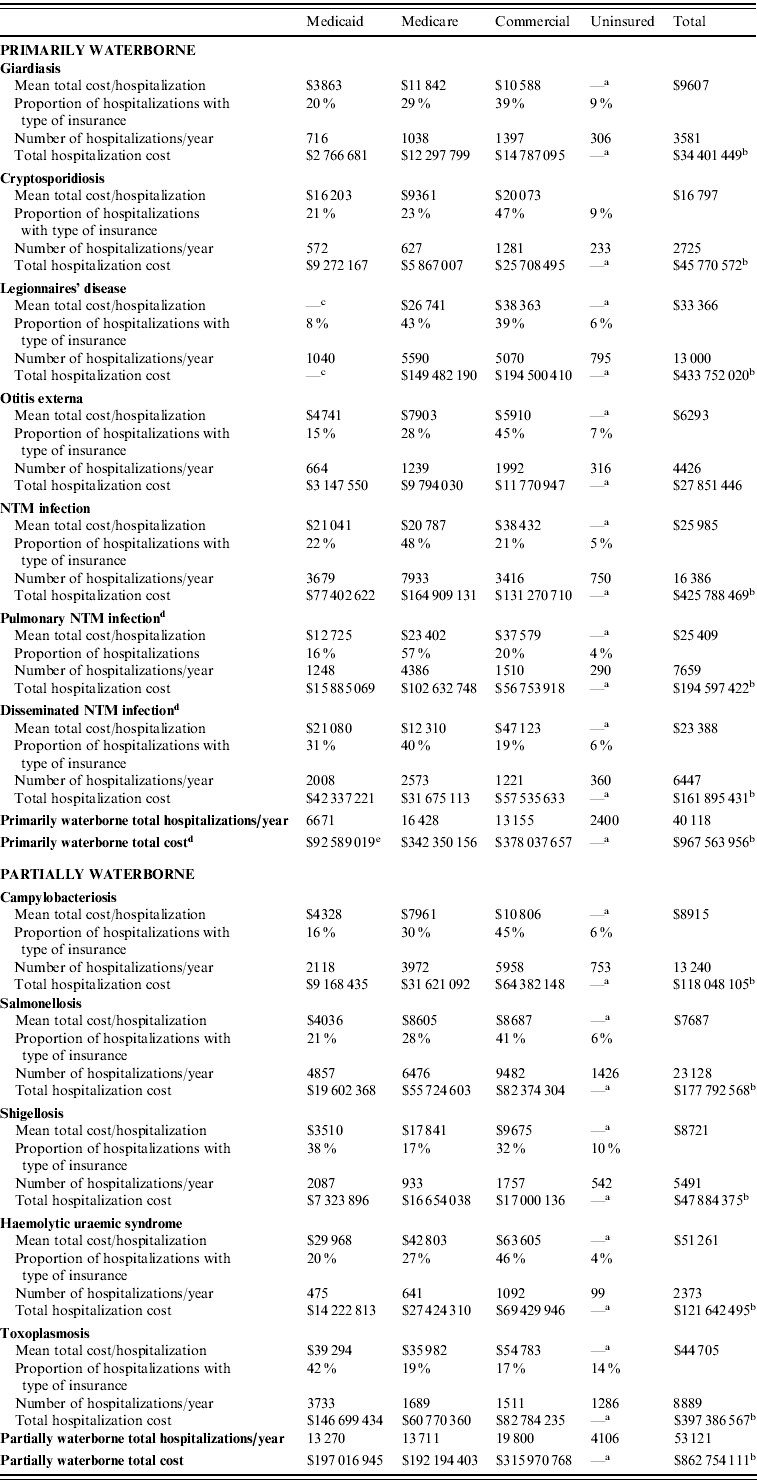
NTM, Non-tuberculous mycobacteria.
Data sources: 2006–2007 Nationwide Inpatient Sample; Marketscan 2004–2005 Multistate Medicaid and 2006–2007 Medicare Supplemental and Commercial Claims databases. All costs in 2007 US dollars.
a Costs for uninsured patients could not be estimated from the insurance claims-based Marketscan databases.
b Totals are higher than the sum of Medicaid, Medicare, and Commercial columns because the total includes the uninsured and other insurance sources (e.g. Tricare).
c The number of cases of Legionnaires' disease in the Marketscan Medicaid database was too small (<5 cases) to calculate cost estimates.
d Pulmonary and disseminated NTM infections were a subset of all NTM infections and are not included in total cost calculations.
e Not including Legionnaires' disease costs.
Over 40 000 hospitalizations for Legionnaires' disease, otitis externa, and NTM infection, diseases entirely or primarily transmitted by water, were estimated to occur each year and cost $970 million annually, including at least $430 million in costs for Medicare and Medicaid patients (because of small numbers of patients in the database, costs for Medicaid patients with Legionnaires' disease could not be calculated). An additional 50 000 hospitalizations for campylobacteriosis, salmonellosis, shigellosis, HUS, and toxoplasmosis cost $860 million annually ($390 million in payments for Medicaid and Medicare patients), an unknown portion of which can be assumed to be due to waterborne transmission.
DISCUSSION
Waterborne disease in the USA involves a complex mixture of pathogens, transmission routes, and water uses. The five primarily waterborne diseases in this analysis were responsible for over 40 000 hospitalizations at a cost of $970 million per year, and included at least $430 million in hospitalization costs for Medicaid and Medicare patients. These costs probably represent only a fraction of the overall cost of US waterborne disease and underscore the need for further investment in waterborne disease monitoring, economic analyses, and burden estimates.
Average costs for outpatient visits were also reported in this analysis. Although annual national costs for outpatient visits were desired, no nationally representative outpatient visit data source evaluated contained the pathogen-specific diagnosis codes used in this analysis, perhaps because the diagnoses reflect laboratory testing completed after the visit records are submitted to the outpatient databases. An exception is otitis externa, which is frequently readily apparent without diagnostic testing.
In the USA, there were 2·4 million ambulatory care visits for otitis externa in 2007 [15], and a UK report estimated the prevalence of otitis externa in general practice patients to be more than 1·2% in a 12-month period [Reference Rowlands16]. The average cost per otitis externa visit in this analysis was $192, implying that outpatient visits might add an additional $0·5 billion to the cost of this preventable waterborne disease.
A complete estimate of the true cost of waterborne illness would also include the cost of mortality and disability, work and time loss, and chronic sequelae, which could be substantial. As an example, salmonellosis was estimated to cost $2·5 billion per year in 2007 US dollars when productivity loss and mortality (but not chronic sequelae, childcare or travel expenses) were accounted for [17].
The near-universal exposure to drinking water can lead to extraordinary costs in a community-wide outbreak. The massive 1993 outbreak of cryptosporidiosis in Milwaukee sickened 400 000 and was estimated to cost $96·2 million in medical costs and lost productivity [Reference Corso18]. For illness associated with recreational water, the popularity of swimming implies a large population of exposed people and a high potential economic cost of illness or beach closure. Dwight et al. estimated that nearly 75 000 excess cases of illness were due to water pollution at just two beaches in Orange County, California [Reference Dwight19], while an economic analysis of closures at a single Lake Michigan beach found a net economic loss of $1274–37 030 per day (depending on the method used to assign values for health and recreation costs) [Reference Rabinovici20].
Previous publications have estimated healthcare costs for some of the diseases included in this analysis. A study by Ballarino and co-workers [Reference Ballarino21] of 27 hospitalized pulmonary NTM patients reported a median cost of $19 876 (range $398–70 917), slightly lower than the mean cost of $25 409 for the 366 episodes observed this analysis. In an analysis by the Economic Research Service of the US Department of Agriculture, salmonellosis was estimated to cost $512 per outpatient visit and $10 412 per hospitalization (2007 US dollars), similar to the $418 (outpatient visit) and $7687 (hospitalization) observed in this analysis [17, Reference Frenzen22]. A study that addressed salmonellosis in California between 1990 and 1999 estimated an average cost of $9054 per hospitalized case, similar to the $7687 observed in this analysis [Reference Trevejo23].
A limitation of these estimates is their reliance on ICD-9 codes from billing records. Because a conservative estimate was desired, no adjustments for under-diagnosis were made. In particular, the estimates of hospitalization derived from the NIS instead of literature estimates (NTMs, HUS and otitis externa) are almost certainly lower than the actual number of hospitalizations because patients could have been hospitalized and treated for their symptoms without receiving a pathogen-specific diagnosis. The otitis externa total might also be lower since only hospitalized patients with a primary diagnosis of otitis externa and no concurrent diagnosis of otitis media were included.
A second limitation of this analysis in estimating the true cost of waterborne disease is the unknown proportion of disease transmission that is waterborne. Legionnaires' disease [Reference Lau and Ashbolt24], NTM infection [Reference Vaerewijck25], and otitis externa [Reference Mena and Gerba26–Reference van Asperen28] are believed to be almost entirely transmitted by water, while water is thought to be the primary vehicle for transmission of giardiasis [Reference Gagnon29] and cryptosporidiosis [Reference Roy30, Reference Majowicz31]. Campylobacteriosis, salmonellosis, shigellosis, HUS, and toxoplasmosis are transmitted via multiple routes (foodborne, waterborne, person-to-person, and zoonotic transmission have all been documented) with non-water-related routes thought to be the primary mode of transmission. The fraction of cases acquired through water has not been precisely quantified, although some attempts at describing transmission sources have been made [Reference Scallan12, Reference Mead32–Reference Hennessy39]. Denno et al. [Reference Denno33] reported that recreational water exposure was responsible for 44% of E. coli O157 infections (the primary infectious agent of HUS) and 23% of campylobacteriosis cases in children, while 17% of salmonellosis cases were associated with septic tank use and 11% with well water use, but risk factors could differ for adult cases. Scallan et al. [Reference Scallan12] estimated the foodborne percentage for campylobacteriosis (80%), salmonellosis (94%), shigellosis (31%), Shiga-toxin producing E. coli O157 (68%), and toxoplasmosis (50%). The proportions of these diseases that are transmitted via person-to-person, zoonotic or other routes have also not been fully quantified, further obscuring the overall attribution picture.
Future studies are needed to more fully describe the burden of waterborne disease in the USA beyond the costs of hospitalizations. The national hospitalization cost estimates reported here represent nearly a billion dollars or more in healthcare costs for preventable waterborne diseases. However, these are underestimates since they do not include the substantial cost of outpatient care, work and time losses, and mortality associated with waterborne infections (e.g. Legionella, NTM infections). With millions of waterborne infections estimated to occur each year, the large healthcare expenditures for hospitalizations reported here underscore the likelihood of a large and hidden toll of waterborne disease and demonstrate a need for investment in future waterborne disease surveillance and prevention programmes.
ACKNOWLEDGEMENTS
The findings and conclusions in this report are those of the authors and do not necessarily represent the official position of the Centers for Disease Control and Prevention.
DECLARATION OF INTEREST
None.






