Introduction
Australia and Canada share many similarities including a federal system, a colonial past and a somewhat-national health insurance scheme called Medicare. Australia’s Medicare was modelled on Canada’s (Scotton and Macdonald, Reference Scotton and Macdonald1993), but with important modifications to take account of Australia’s contemporary health system, history and constitution.
In both countries, this universal health insurance system ensures that patients have access to hospitals without any financial barriers – in Australia this access is to ‘public hospitals’ which account for about two-thirds of all beds, and include the major academic medical centres – and access to medical services, which are generally provided by independent medical practitioners (not employed by government) who are primarily rewarded on a fee-for-service basis. Funding for these services comes from government. In Australia there is an identified ‘Medicare levy’, but this is not currently hypothecated to health care, although the 2017 Commonwealth budget provided that it would be allocated to a ‘Medicare Guarantee Fund’ (Duckett, Reference Duckett2017). Legislation to establish the Medicare Guarantee Fund had not been introduced into parliament at the date of writing (June 2017).
The two countries share a democratic, Westminster style of government, and are roughly comparable in terms of wealth (Canadian gross domestic product per capita in 2015 was $45,415 compared with Australia’s of $47,758; both in US$ purchasing power parity). Canada’s population in 2017 is somewhat larger than Australia’s (36 vs 23 million), and both are large geographically but with low average population density (Canada at 3.5 people/km2; Australia at 3.1 people/km2). The population of both, though, is concentrated: in Canada in the south of the country, in Australia along the Eastern seaboard and the south-west corner. The demography of Canada and Australia is similar, with both facing ageing populations and poorer health outcomes for Indigenous populations.
These similarities of history (majority), language and national wealth, and the similar Medicare arrangements mean that the health systems in the two countries are closer in structure than any other pairing for both Canada and Australia and have often led to the two nations being part of: comparative studies of aspects of system performance (Morgan et al., Reference Morgan, McMahon, Mitton, Roughead, Kirk, Kanavos and Menon2006; Clement et al., Reference Clement, Harris, Li, Yong, Lee and Manns2009; Tempier et al., Reference Tempier, Meadows, Vasiliadis, Mosier, Lesage, Stiller, Graham and Lepnurm2009; Coleman et al., Reference Coleman, Forman, Bryant, Butler, Rachet, Maringe, Nur, Tracey, Coory, Hatcher, McGahan, Turner, Marrett, Gjerstorff, Johannesen, Adolfsson, Lambe, Lawrence, Meechan, Morris, Middleton, Steward and Richards2011; Sunderland et al., Reference Sunderland, Harris, Johnstone, Del Fabbro and Kendall2015); system organisational arrangements (Philippon and Braithwaite, Reference Philippon and Braithwaite2008; Elson, Reference Elson2009; Suchowersky et al., Reference Suchowersky, Suchowersky and Duckett2012); contracting and accountability for Indigenous health care (Lavoie, Reference Lavoie2004; Lavoie et al., Reference Lavoie, Boulton and Dwyer2010; Dwyer et al., Reference Dwyer, Lavoie, O’Donnell, Marlina and Sullivan2011; Tenbensel et al., Reference Tenbensel, Dwyer and Lavoie2014); as well as a number of whole system comparative publications (Duckett, Reference Duckett1983; Crichton, Reference Crichton1995; Crichton, Reference Crichton1998; Duckett, Reference Duckett2015). Australia and Canada were two of the original five nations included in the Commonwealth Fund’s International Health Policy survey, the others being New Zealand, the United Kingdom and the United States (Donelan et al., Reference Donelan, Blendon, Schoen, Davis and Binns1999; Schoen et al., Reference Schoen, Davis, DesRoches, Donelan and Blendon2000), and Australia remains one of the 11 countries in the contemporary surveys (Osborn et al., Reference Osborn, Squires, Doty, Sarnak and Schneider2016).
This paper is the first to identify whole system lessons for Canada from the Australian health system.
Australia’s constitution gives the federal (‘Commonwealth’) government power to make laws about hospital and pharmaceutical benefits and, subject to certain constraints, medical services and for those laws to take precedence over state laws (McMillan, Reference McMillan1992; Wheelwright, Reference Wheelwright1995). It also gives the Commonwealth exclusive power to levy excise and effectively to crowd the states out of income taxation (Mathews and Jay, Reference Mathews and Jay1972). The term ‘states’ is used in this paper to refer to Australia’s six states and two mainland territories.
Responsibility for health care in Australia is shared between the Commonwealth government–responsible for subsidising medical services, pharmaceuticals, private health insurance and aged care – and the states which are responsible for public hospitals, although the Commonwealth provides grants to the states which cover about 40% of the costs of public hospitals (Duckett, Reference Duckett2014). The dual responsibility and the revenue squeeze on the states have resulted in regular and unedifying financial stoushes between the Commonwealth and state governments over the share of public hospital costs met by the Commonwealth government. These exchanges have dominated the Australian health care debate and led to cost and blame shifting (House of Representatives. Standing Committee on Health and Ageing, 2006), to the detriment of political accountability and resulting in a somewhat confusing system of gaps and overlaps in services (Swerissen and Duckett, Reference Swerissen and Duckett2007), which one commentator has dubbed ‘marble cake federalism’ (Wiltshire, Reference Wiltshire1992).
A distinguishing characteristic of Australian health care is the strong role played by the private sector in hospital provision (discussed below), with the business model of private hospitals underpinned by private health insurance, which is in turn subsidised by the Commonwealth government. About 47% of Australians have some form of private health insurance.
Out of this morass has emerged substantial innovation in health care delivery and funding, and a health system which has relatively good outcomes, at least as measured in terms of average life expectancy, and this has been achieved at an affordable cost (Duckett and Willcox, Reference Duckett, Breadon, Weidmann and Nicola2015). Health status for Australia’s Indigenous population is poor, and, although there are methodological difficulties in making comparisons (Australian Institute of Health and Welfare, 2011), probably relatively poorer than First Nations people in Canada (Anderson et al., Reference Anderson, Robson, Connolly, Al-Yaman, Bjertness, King, Tynan, Madden, Bang, Coimbra, Pesantes, Amigo, Andronov, Armien, Obando, Axelsson, Bhatti, Bhutta, Bjerregaard, Bjertness, Briceno-Leon, Broderstad, Bustos, Chongsuvivatwong, Chu, Deji, Gouda, Harikumar, Htay, Htet, Izugbara, Kamaka, King, Kodavanti, Lara, Laxmaiah, Lema, Taborda, Liabsuetrakul, Lobanov, Melhus, Meshram, Miranda, Mu, Nagalla, Nimmathota, Popov, Poveda, Ram, Reich, Santos, Sein, Shekhar, Sherpa, Skold, Tano, Tanywe, Ugwu, Ugwu, Vapattanawong, Wan, Welch, Yang, Yang and Yap2016). Consequently, lessons to be learned are probably from Canada to Australia rather than vice versa in this regard.
Typical criteria to evaluate health system performance include equity, quality, efficiency and acceptability (e.g. see Duckett and Willcox, Reference Duckett, Breadon, Weidmann and Nicola2015). Two of these criteria, equity and efficiency, have been used to select four areas where Canada can learn from Australia: the Pharmaceutical Benefits Scheme (PBS); innovations in care for people with chronic conditions; support for the frail elderly; and funding policy for hospital care. These developments have all been generally positive on the two criteria. Not so positive has been Australia’s experience with out-of-pocket costs for health care (failing significantly on the equity criterion) and the role of private insurance and private provision (failing on both criteria).
The PBS
The Australian PBS has positive lessons for Canada, as a relatively efficient way of providing access to pharmaceuticals. It was introduced on 1 July 1948 as part of post Second World War expansion of social provision. Relatively few prescriptions were provided under this scheme initially because of opposition from the medical profession. The Liberal (conservative) Government elected in 1949 altered the scheme, introducing a list of 139 ‘life saving and disease preventing drugs’ that were provided free of charge to the whole community (Sloan, Reference Sloan1995). Since then, the range of drugs covered by the PBS has expanded significantly with new drugs being added each year. In 2014–2015 government spending on the PBS totalled A$7.9 billion for 207 million subsidised prescriptions (PBS Information Management Section, 2016). This amounts to an annual government subsidy of A$332 per person, with the average person receiving 8.7 prescriptions each year.
The PBS incorporates defined mandatory co-payments with co-payments for each prescription for low income and social security beneficiaries set at A$6.30 (as at 1 January 2017), other people at A$38.80, and a ‘safety net’ under which high users pay either no co-payment or a reduced co-payment after meeting a specified threshold of prescriptions (or prescription co-payments) each year. These mandatory co-payments have equity implications, discussed in the section on co-payments below.
The decision to list an item on the PBS can lead to commitment of significant government expenditure. Australia pioneered the ‘fourth hurdle’ for listing new drugs, requiring demonstrable value for money supplementing the standard international expectations of quality, safety and efficacy (Mullins et al., Reference Mullins, Ndiritu, Yoder, Shaya and Taylor2003; Schwarzer et al., Reference Schwarzer, Rochau, Saverno, Jahn, Bornschein, Muehlberger, Flatscher-Thoeni, Schnell-Inderst, Sroczynski, Lackner, Schall, Hebborn, Pugner, Fehervary, Brixner and Siebert2015).
Under the PBS cost-effectiveness arrangements, which have prevailed since 1993, pharmaceutical manufacturers’ proposals for listing include cost-effectiveness data (Birkett et al., Reference Birkett, Mitchell and McManus2001; Bulfone et al., Reference Bulfone, Younie and Carter2009). Although there are no explicit thresholds used in decision-making (Bulfone et al., Reference Bulfone, Younie and Carter2009), a retrospective study of the decision-making process showed that in the early 1990s new pharmaceuticals costing more than $68,913 per life year saved were generally not listed on the PBS, while those costing less than $36,450 were listed (George et al., Reference George, Harris and Mitchell2001). No apparent decision rules have been found to apply to the intermediate zone.
The Australian government, through the PBS, is a near monopsonistic purchaser for out-of-hospital pharmaceuticals. It has used this power in recent years to drive the price of pharmaceuticals down to approximate international benchmark pricing (Duckett and Banerjee, Reference Duckett and Breadon2017). On average, Australian pharmaceutical prices appear to be about one-third of Canadian (Alberta and Ontario) prices (Duckett and Banerjee, Reference Duckett and Breadon2017). For example, the wholesale price for a packet of 3040 mg tablets for atorvastatin is A$12.97 in Canada and A$3.43 in Australia.
Canada is still struggling to introduce a universal pharmaceutical scheme (Gagnon, Reference Gagnon2010; Boothe, Reference Boothe2012; O’Brady et al., Reference O’Brady, Gagnon and Cassels2015; Morgan and Boothe, Reference Morgan and Boothe2016; Morgan et al., Reference Morgan, Gagnon, Mintzes and Lexchin2016) and could well draw on lessons from Australia about a scheme which provides universal coverage, at a reasonable cost, albeit with structured co-payments. The main lessons for Canada in the design of a new Pharmacare scheme are:
∙ The scheme should involve rigorous assessment of what is included in a national formulary, including assessing cost-effectiveness of listed drugs.
∙ Monoposonistic purchasing helps to depress prices.
∙ Strategies to ensure rational prescribing and avoid over-prescribing (described as ‘quality use of medicines’ in Australia) should be introduced (Smith and McGettigan, Reference Smith and McGettigan2000; Weekes et al., Reference Weekes, Mackson, Fitzgerald and Phillips2005; Beilby et al., Reference Beilby, Wutzke, Bowman, Mackson and Weekes2006); see also Rosen (Reference Rosen2018) on similar strategies in Israel.
Recognising Canada’s more decentralised health system, provincial variation could include provinces being able to set different incremental cost-effectiveness ratios for listed drugs, different co-payments and different payments to pharmacists.
Australia’s PBS provides negative lessons too. Mandatory co-payments can have equity and access implications (see discussion of out-of-pocket costs below) and so care would need to be taken if they are an integral part of the design. A new Canadian Pharmacare programme could improve on some of the identified weaknesses of the Australian PBS, particularly on pricing where Australian prices are higher than some other countries (UK, New Zealand), in addition to going further than Australia’s quite modest use of therapeutic equivalence or ‘reference’ pricing (Bulfone et al., Reference Bulfone, Younie and Carter2009; Acosta et al., Reference Acosta, Ciapponi, Aaserud, Vietto, Austvoll-Dahlgren, Kösters, Vacca, Machado, Diaz Ayala and Oxman2014; Duckett and Banerjee, Reference Duckett and Breadon2017).
Management of chronic conditions
In common with the situation in other countries, the health needs of the Australian population are changing as more people experience chronic disease. Three-quarters of Australians over the age of 65 now have one or more chronic disease and 90% of Australians die from chronic disease (Swerissen and Duckett, Reference Swerissen and Duckett2016). Australia has developed a series of initiatives to change the way family physicians work through targeted financial incentives, potentially providing lessons for Canada about improving efficiency in family practice in the way care for people with chronic illnesses is provided.
Australia’s Medicare Benefits Scheme (MBS) arrangements are still dominated by fee-for-service reimbursement, a system which ‘encourages reactive rather than systematic care’ (Harris and Zwar, Reference Harris and Zwar2007). However, the Commonwealth Government, responsible for the design and funding of the MBS, has recognised the importance of introducing other modes of payments for general practitioners to encourage different practice patterns, including introducing incentives for better management of chronic conditions. Until recently, the main relevant medical professional organisations, the Australian Medical Association and the Royal Australian College of General Practitioners, have been opposed to capitation payment as an alternative to fee-for-service (Hunter, Reference Hunter1980; Gillespie, Reference Gillespie1991; Royal Australian College of General Practitioners, 2015).
The government’s response to meeting chronic care needs has been a proliferation of new, largely item-based additions to the MBS, but no overarching strategic vision or end point for the future of general practice (Beilby, Reference Beilby2007). The Medicare payment rules for these items inhibit both innovation in the way practices manage chronic disease (Robson et al., Reference Robson, Hull, Mathur and Boomla2014) and ‘the links between different services at the local level’ (Fine, Reference Fine1999).
Even though this innovation has been a second-best solution because of the political difficulties of initiating wider capitation arrangements, each of these item-based additions is innovative. Table 1 identifies some of the major changes to the funding of general practice over the last two decades.
Table 1 Reforms to Medicare Benefits Scheme (MBS) items for general practice, Australia, 1998–2016
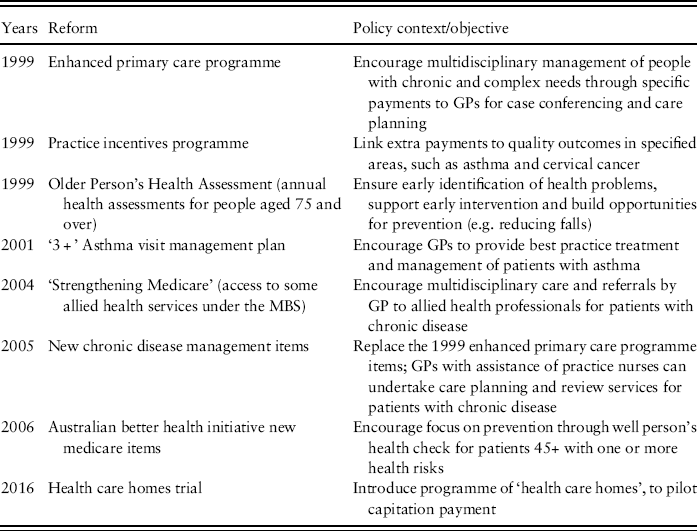
Source: Updated from Duckett and Willcox (2015).
These initiatives have rarely been evaluated in terms of their impact on outcomes, with evaluations often simply focussing on process measures such as provider acceptability (Blakeman et al., Reference Blakeman, Harris, Comino and Zwar2001; Harris et al., Reference Harris, Blakeman and Zwar2002; Zwar et al., Reference Zwar, Hermiz, Comino, Shortus, Burns and Harris2005; Rhee et al., Reference Rhee, Zwar and Kemp2012), uptake (Price et al., Reference Price, Beilby, McElroy, Wilkinson, Best, Morey and Mott2002; Wilkinson et al., Reference Wilkinson, McElroy, Beilby, Mott, Price, Morey and Best2002a; Wilkinson et al., Reference Wilkinson, McElroy, Beilby, Mott, Price, Morey and Best2002b, Reference Wilkinson, McElroy, Beilby, Mott, Price, Morey and Best2003; Hamirudin et al., Reference Hamirudin, Ghosh, Charlton, Bonney and Walton2015) and impact on allied health services (Cant and Aroni, Reference Cant and Aroni2007; Foster et al., Reference Foster, Mitchell, Haines, Tweedy, Cornwell and Fleming2008; Menz, Reference Menz2009; Haines et al., Reference Haines, Foster, Cornwell, Fleming, Tweedy, Hart and Mitchell2010). The few outcome evaluations have been mildly positive, showing that the introduction of the Enhanced Primary Care items was associated with improved diabetes care (Zwar et al., Reference Zwar, Comino, Hasan and Harris2007); that a 45+ health check was associated with change in patient exercise patterns but not clinical measures (Amoroso et al., Reference Amoroso, Harris, Ampt, Laws, McKenzie, Williams, Jayasinghe, Zwar and Davies2009); and that a falls prevention programme funded through use of the chronic disease management items reduced falls (Mackenzie and Clemson, Reference Mackenzie and Clemson2014).
The Practice Incentives Program introduced a pay-for-performance (P4P) element into primary medical care funding. More accurately described as ‘pay for process adherence’, as would be expected from the very mixed international evaluations of P4P (Tanenbaum, Reference Tanenbaum2009; Cromwell et al., Reference Cromwell, Trisolini, Pope, Mitchell and Greenwald2011; de Bruin et al., Reference de Bruin, Caroline and Struijs2011; Eijkenaar, Reference Eijkenaar2012; Eijkenaar et al., Reference Eijkenaar, Emmert, Scheppach and Schöffski2013), the Australian P4P experience in primary care is also mixed (Scott et al., Reference Scott, Schurer, Jensen and Sivey2009; Scott et al., Reference Scott, Sivey, Ouakrim, Willenberg, Naccarella, Furler and Young2011; Greene, Reference Greene2013).
One particularly important innovation was the 2004 initiative to provide coverage for allied health services, thus facilitating multidisciplinary care. The Medicare Chronic Disease Management items (Australia’s Medicare billing unit) allow GPs to refer selected patients to eligible allied health professionals, with patients able to claim Medicare rebates for a maximum of five allied health services annually. These services are only accessible for patients with a chronic disease whose GP has prepared a management plan and initiated team care arrangements. Allied health services can be provided by registered private practitioners who fall within one of the 14 classes of eligible allied health professionals.
In 2015–2016 over six million allied health services were provided under the chronic disease management MBS items at a cost to Medicare of about A$330 million (data extracted from http://medicarestatistics.humanservices.gov.au/statistics/mbs_item.jsp). About three-quarters of allied health services claimed under Medicare are for podiatry (45% of allied health services) and physiotherapy (31%). There is fairly limited use of most of the other 12 categories of allied health services eligible for Medicare funding.
In common with many other countries (Tsiachristas et al., Reference Tsiachristas, Dikkers, Boland and Rutten-van Mölken2013; Struckmann et al., Reference Struckmann, Quentin, Busse and van Ginneken2016), Australia’s main response to using financial incentives to improve care continuity has been a pay-for-coordination strategy. Despite this, care coordination remains a critical issue for the health care system, causing problems with consistency of information provision and quality of care (Schoen et al., Reference Schoen, Davis, DesRoches, Donelan and Blendon2011). In 2016, Australians with chronic conditions were more likely to have experienced problems with care coordination than their counterparts in comparable countries (the United Kingdom, United States, New Zealand, Canada, France, Germany, the Netherlands, Norway, Sweden and Switzerland); specifically Australians with chronic conditions were less likely to have discussed their main goals and care priorities with a health professional, and less likely to have discussed treatment options and side effects (Osborn et al., Reference Osborn, Squires, Doty, Sarnak and Schneider2016). More than $1 billion dollars a year is spent on pay-for-coordination or P4P payments but still a high proportion of patients with chronic disease do not receive recommended best practice care (Swerissen and Duckett, Reference Swerissen and Duckett2016).
The 2016–2017 ‘health care homes trial’ is the latest attempt to update the Medicare payment arrangements to encourage better care for people with chronic conditions (Dwyer and Duckett, Reference Dwyer and Duckett2016; Gunn, Reference Gunn2016). The trial is relatively small with only 65,000 patients across 200 practices (Department of Health, 2016) and is more designed as a minimalist toe-in-the-water rather than transformational change. It does not provide the essential foundations for the primary care reforms which are necessary (Swerissen and Duckett, Reference Swerissen and Duckett2017), nor address recognised problems of voluntary enrolment (Glazier et al., Reference Glazier, Kopp, Schultz, Kiran and Henry2012; Kiran et al., Reference Kiran, Kopp and Glazier2016). It involves voluntary enrolment of patients and capitation payments for these patients. Despite its limitations, it represents the beginning of a process of change which could provide a basis for more systemic change over time by allaying the medical profession’s fears of funding reform and aversion to capitation.
The lessons for Canada from Australia’s MBS system are mixed. A number of provinces have introduced ‘alternative payment plans’ for family physicians, and Canada has rightly been described as a leader in such developments (Wranik and Durier-Copp, Reference Wranik and Durier-Copp2009), with mixed results in terms of the benefit of the alternative models compared to fee-for-service (Hutchison and Glazier, Reference Hutchison and Glazier2013; Rudoler et al., Reference Rudoler, Deber, Barnsley, Glazier, Dass and Laporte2015; Howard et al., Reference Howard, Chalifoux and Tanuseputro2016; Lavergne et al., Reference Lavergne, Law, Peterson, Garrison, Hurley, Cheng and McGrail2016; Laberge et al., Reference Laberge, Wodchis, Barnsley and Laporte2017).
More change for primary care payment is on the way in Canada, at least in Ontario (Marchildon and Hutchison, Reference Marchildon and Hutchison2016), and Canadian provinces could perhaps learn from Australia’s blended payment model. In particular, grafting new incentives onto the fee-for-service system has been achieved with the medical profession’s support. However, these changes have been incremental, poorly planned and do not provide a coherent basis for a primary care system well adapted to emerging needs. Notwithstanding that, there is still potential to assess each of the innovations in terms of their ability to supplement existing Canadian approaches to addressing the challenges of the epidemiological transition to greater prevalence of chronic conditions. The first lesson is about the strategy of grafting new incentives onto a fee-for-service system, not the precise way Australia has implemented these changes. The second lesson is about how Australia has extended access to allied health services such as physical therapy – traditionally not part of Medicare in Canada – by means of integration into a Medicare framework.
Support for the elderly
Commonwealth support for aged care services, more recently reformulated as support for people in need (through direct grants which can then be used by recipients to purchase services from any provider) has a long tradition, commencing early in the 20th century and is associated with support for people in receipt of Commonwealth pensions. It was stimulated as part of post Second World War reconstruction, but was expanded through subsidies for church and charitable organisations to provide aged care accommodation by the Liberal (conservative) government in the mid-1950s (Kewley, Reference Kewley1973; Dixon, Reference Dixon1977; Jeon and Kendig, Reference Jeon and Kendig2017). Over the last 40 years, policy has shifted towards emphasising support to keep frail older people in the community rather than providing support to the service provider (Gibson, Reference Gibson1998, Reference Gibson1996; Australian Institute of Health and Welfare, 2014), with the most recent changes being the result of a comprehensive review of current and future challenges for the aged care system (Productivity Commission, 2011; Jeon and Kendig, Reference Jeon and Kendig2017). This is the area where Australia has lessons for Canada.
The Australian aged care arrangements are efficient (especially in terms of reducing demand for high cost residential care) and equitable (available to all people, but with greater support to those with fewer assets and lower income). The existing aged support arrangements involve a coordinated mix of residential support and support for home care services.
Community or home-based care
The basis for all aged care assistance is assessment of need. As part of the ‘My Aged Care’ portal, Commonwealth government-funded Regional Assessment Services assess the support needs of older people using standardised assessment instruments independently of service providers. If a person’s needs are able to be met in the home, the ‘Commonwealth Home Support Program’ provides assistance within three broad service sub-programmes:
∙ Community and home support provides entry-level services to support older people to live independently at home and in the community, for example, meals, domestic assistance and transport.
∙ Care relationships and carer support is available to support and maintain care relationships between older people and their carers.
∙ Assistance with care and housing supports vulnerable clients to remain in the community through accessing appropriate, sustainable and affordable housing and linking them to community care and other support services.
Funding under the Commonwealth Home Support Program is structured into ‘service groups’ which are designed to achieve common goals or outcomes: increased independence; nutrition; social participation; assistance at home; access to the community; and care relationships. Consumers have a choice of care providers – from providers participating in the scheme who have been allocated funding by the Commonwealth government – across all the relevant sub-programmes.
There is a standard national fee schedule, with consumers being expected to contribute a ‘basic daily fee of up to 17.5 per cent of the pension’, with an income-tested amount above that of up to A$25,000–A$40,000 depending on marital status and living arrangements (the range quoted is single compared with couple; see http://www.myagedcare.gov.au/costs/help-home-costs-explained, accessed 22 December 2016).
Residential and substitute care
Older people who require access to more intensive support than is available through the Commonwealth Home Support Program face further assessment to determine their eligibility to access either community-based or residential aged care services. Subject to this assessment, people who require a higher level of support than is available in the Commonwealth Home Support Programs, but do not need to move into a residential aged care facility, can be allocated a ‘home care package’. Packages range in value from a base subsidy of $22.04 per week to $133.09 per week, with supplements paid for some attributes of the patient (e.g. with dementia) or in rural and remote locations (see https://agedcare.health.gov.au/funding/aged-care-subsidies-and-supplements/schedule-of-subsidies-and-supplements, accessed 4 January 2017).
Since July 2012, all new Home Care Packages have been provided as ‘Consumer-directed Care’ packages which give consumers a personalised budget for them to purchase their desired mix of services. People in receipt of Home Care Packages pay the same fees as under the Commonwealth Home Support Program.
People with higher level needs are supported to live in residential aged care where they receive personal care. There are two major sources of funding to support people in residential facilities. These are:
∙ A Commonwealth subsidy, which varies with the resident’s dependency and need for care; and
∙ A resident payment, the latter in part recognising that residential facilities provide food and shelter that residents would need to pay for wherever they lived.
The care cost subsidies are based on the resident’s needs as measured using the Aged Care Funding Instrument which involves an appraisal of the resident’s ‘usual care needs’ across three domains: activities of daily living (such as mobility and continence); behaviour (such as cognitive skills and depression); and complex health care (including use of medication).
To encourage residential care facilities to give places to residents who cannot meet their own accommodation costs, the Commonwealth also pays supplements to facilities based on the share of concessional residents, although the level of the payment may be insufficient to ensure appropriate access (Gargett, Reference Gargett2010).
Lessons for Canada
As people age, they become frailer and their informal social supports (often through partners, husbands, wives) become more fragile. Care needs increase in fits and starts, often as a result of a slow continuous functional decline, sometimes because of acute events (strokes, falls). The pathways to care are quite different depending on the nature of the underlying disablement, with people with dementia or who have had a stroke having quite different patterns compared with people with other conditions (Karmel et al., Reference Karmel, Gibson, Anderson, Wells and Duckett2012). Design of aged care funding arrangements is complex, as it has to be designed with interactions with both income support policy and housing ownership in mind (Ong, Reference Ong2016).
The Australian system is strong on providing access, particularly to community-based care. Median waiting times between assessment and admission to care in 2014–2015 were 84 days for residential care and 73 days for home care. Further, one-quarter of people were admitted to residential care within 1 month, and a third accessed home care within that period [Steering Committee for the Review of Commonwealth/State Service Provision (SCRCSSP) , 2017], with some of the delay presumably to organise financing and other arrangements. However, regulation of quality of residential care has demonstrable weaknesses, and Canadian provinces could only learn from Australia’s failures in this area, not its success (Hamilton and Menezes, Reference Hamilton and Menezes2011; Baldwin et al., Reference Baldwin, Chenoweth and Rama2015a, Reference Baldwin, Chenoweth, Rama and Liu2015b).
In contrast to the comprehensiveness and universality of Australia’s aged care support, the Canadian service system, as currently structured, is poorly suited to respond, and is characterised by discontinuities: discontinuities between hospitals and services outside those walls, between home care and residential care, and between ‘health’ and ‘social’ care. These discontinuities impact on both individuals and the system as a whole. For the individual, they may not get the service that is most appropriate for them. For the system, it may lead to inefficiency in that people might remain in hospital, for example, when they would be better cared for in another location (Manzano-Santaella, Reference Manzano-Santaella2010a, Reference Manzano-Santaella2010b).
As Hirdes pointed out:
Canada’s universal, publicly funded health care system has not been designed in a way that established a uniform national approach to long-term care. Instead, the needs of the frail elderly are addressed through a policy mosaic that results in inequalities in access to services and differential burdens of care on family members. Moreover, the lack of a standardized health information system has made it difficult to compare the experiences of users of long-term care systems from province to province (Reference Hirdes2001).
This is in contrast to Australia where there is a universal, national programme for aged care, which emphasises home care and support. Expansion of home care in Canada was supported by the two national inquiries into health care conducted in the last 20 years [Senate. Standing Committee on Social Affairs Science Technology (Chair: Senator Michael Kirby), 2002; Commission on the Future of Health Care in Canada (Chair: Roy Romanow), 2002], with the Romanow Commission referring to home care as ‘the next essential service’ [Commission on the Future of Health Care in Canada (Chair: Roy Romanow), 2002: 171]. Australia can provide useful lessons on the means to organise such an expansion.
Hospital efficiency
Unlike Canada, Australia has a mixed system of hospital provision. All Australians are eligible to receive treatment in public hospitals – hospitals generally owned by state governments but operated by quasi-independent boards of directors appointed by the State government. Some states do not have independent boards of hospitals; there are also a handful of hospitals run by Roman Catholic organisations – formerly religious orders of nuns – which operate as public hospitals (Gleeson, Reference Gleeson1989). Public hospital funding is determined by state governments, with substantial subsidies (around 40% of funding) from the Commonwealth government, but paid via the states (Duckett, Reference Duckett2015). Private hospitals are owned by a mix of for profit and not-for-profit organisations, charging patients for accommodation (Duckett and Willcox, Reference Duckett, Breadon, Weidmann and Nicola2015).
Australia has been an international pioneer in driving efficiency in its hospital services, principally through the introduction of activity-based funding (or ‘casemix’ funding as it was originally termed). Victoria adopted activity-based funding as the basis of paying for public hospital inpatient services in 1993 (Duckett, Reference Duckett1995), and its scope has been expanded to other aspects of public hospital care since then. A 2011 national agreement has led to activity-based funding being adopted in larger states and nationally for determining adjustments to the flow of funds between the Commonwealth and states (Council of Australian Governments, 2016, 2011).
An important piece of national infrastructure is the Independent Hospital Pricing Authority, which is indeed independent as its name implies: the Commonwealth government chooses the Chair, the states and territories the Deputy Chair, and all other members are agreed through the Council of Australian Governments.
Typically, the key features characterising activity-based payment used by states in payment models for public hospitals have comprised the following:
∙ Standard prices: Most states have adopted the ‘National Efficient Price’ determined by the Independent Hospital Pricing Authority used for determining the Commonwealth payments to states (Independent Hospital Pricing Authority, 2015).
∙ Use of payment relativities (termed ‘payment weights’) to determine relative prices across diagnosis related groups (DRGs): Payment weights are calculated by the Independent Hospital Pricing Authority from cost data submitted by states.
∙ Capping of expenditure: Unlike the private sector, state government spending on public hospitals is capped, usually achieved either through explicit volume caps (no payment for services above a negotiated or target level) or by declining marginal payment for additional volume. Commonwealth government funding of the costs of activity growth is also capped at an arbitrary 6.5% per annum, although this cap is unlikely to be breached given recent levels of cost and activity growth.
Since 2014/2015 Commonwealth payments to states are adjusted in line with changes in activity and costs. Importantly, this activity adjustment is paid at the ‘National Efficient Price’ as determined by the Independent Hospital Pricing Authority.
The 2016 Agreement on hospital funding introduced a new element to the funding formula: payment for quality (Council of Australian Governments, 2016). The Independent Hospital Pricing Authority has been directed to incorporate consideration of specified adverse events (including a list of agreed hospital acquired conditions), ineffective interventions, and readmissions into their pricing structure. The Authority has advanced a number of ways in which that could be done for phased implementation from July 2017 (Independent Hospital Pricing Authority, 2016).
Australia’s hospital system is more efficient than Canada’s (Varabyova and Schreyögg, Reference Varabyova and Schreyögg2013) and there are two clear lessons for Canada in the Australian experience of driving improvements in hospital efficiency. First, there has been the very clear acceptance that there is room to improve the efficiency of hospital care, and that this is best done through paying hospitals on the basis of their activity, not their history, negotiated ‘global budgets’ or other methods (Duckett et al., Reference Duckett and Banerjee2014). Second, Australian governments have negotiated an agreement which means that the Commonwealth and states share the costs of growth in hospital demand, but the formula includes an incentive for efficiency, by only funding growth using an ‘efficient price’.
Cautionary tales: the problems of mixed public and private funding
All is not rosy in Australia, and there are cautionary tales about Australian health polices which can inform contemporary Canadian policy debates. In particular, the effects of Australia’s high level of private funding and provision can provide a warning signal to Canada about the potential consequences of increased private funding in the context of the current Charter challenge being litigated in the British Columbia Cambie case (Costain, Reference Costain2017).
Out-of-pocket costs
Compared with many countries, Australian consumers contribute a large proportion of health care costs through fees: almost one-fifth of all health care spending. Australia is ranked in the middle of the Organisation for Economic Co-Operation and Development for the proportion of health costs paid for with out-of-pocket fees. Compared with 17 other wealthy countries, however, Australia has the third highest reliance on these payments. Only Switzerland and Belgium outstrip Australia, and rates are far lower in the United Kingdom, Canada and New Zealand. The amount Australians pay as a proportion of their household expenditure is also relatively high (Duckett and Breadon, Reference Duckett and Willcox2014).
An Australian Bureau of Statistics survey found that almost one in 20 of people need to see a GP but do not go because of cost, with the rate higher for females (5.2%) than males (2.8%). The proportion is 8% for specialists and 19% for dentists (Australian Bureau of Statistics, 2016). According to data from the Commonwealth Fund’s international health policy survey, Australia (at 14%) and Canada (at 16%) had similar proportions of respondents reporting that they ‘had any cost-related access problem to medical care in past year’ (Osborn et al., Reference Osborn, Squires, Doty, Sarnak and Schneider2016).
Of the almost A$30 billion spent by households on health care in 2014–2015, about one-third was for medications not covered by the PBS (including vitamins and supplements), and 5% for PBS medications (Australian Institute of Health and Welfare, 2016b). Other large components were dental care (about 20% of household health care spending) and aids and appliances (about 10%). Poorer families spend a higher proportion of their income (but a lower absolute amount) than wealthier families.
Although only a small proportion of household health expenditure – around 2% – is for family physician visits, the distribution of this is uneven (e.g. higher co-payments in rural areas) and, as indicated above, these out-of-pocket costs create a barrier to access for some.
There is no regulation of patient fees in Australia, nor are doctors who ‘extra-bill’ required to opt-out of public funding. As a result, patient charges are at the whim of the individual practice with medical practitioners applying their own assessment of whether patients will be charged any fee and, if charged, what level of payment will be required. There is thus considerable variation in fees charged (Freed and Allen, Reference Freed and Allen2017; Hua et al., Reference Hua, Erreygers, Chalmers, Laba and Clarke2017; Johar et al., Reference Johar, Mu, Van Gool and Wong2017).
Australia’s high level of reliance on out-of-pocket payments is an area of weakness on the equity criterion. Out-of-pocket payments are thus one area where Canada can learn from Australia, but this is something that Canada should avoid rather than emulate.
Private hospital care and private health insurance
In addition to out-of-pocket contributions, there is a significant role for private funding in Australia – just under 9% of all health care funding is mediated through private health insurance (Australian Institute of Health and Welfare, 2016b). Private health insurance is heavily subsidised by the Commonwealth government through rebates to the insured population which cover about 25% of the cost of insurance policies, and insurance is further encouraged by a complex array of carrots and sticks (Hall et al., Reference Hall, De Abreu Lourenco and Viney1999; Palangkaraya and Yong, Reference Palangkaraya and Yong2005; Kay, Reference Kay2017; Kettlewell et al., Reference Kettlewell, Stavrunova and Yerokhin2018; McDonald and Duckett, Reference McDonald and Duckett2017). In Canada, private health insurance complements public provision in that there is no overlap in coverage. In contrast, private health insurance in Australia facilitates private hospital care (Eldridge et al., Reference Eldridge, Onur and Velamuri2017) and provides insurance for the same services which might also be provided, for most patients without charge, in public hospitals. In addition to covering private hospital care, private health insurance also provides rebates against dental fees and allied health services.
Almost half the population is covered by private health insurance, although most have products with high levels of deductibles and exclusion clauses. In addition to this private funding, Australia has a strong private hospital sector, with private health insurance responsible for almost half of that sector’s revenue and government subsidies through health insurance accounting for a further one-fifth of revenue (totalling 68% of private hospital revenue).
Private hospitals primarily specialise in elective procedures, which account for over 80% of their activity (Australian Institute of Health and Welfare, 2016a). Almost 60% of all elective admissions are admitted to private hospitals, in contrast only 8% of emergency admissions are admitted to private hospitals.
Private hospitals admit patients of lower levels of acuity (Table 2 shows data about orthopaedic procedures showing for both hip and knee replacements), as well as higher proportions of cases in the less complex Diagnosis-Related Group. They also tend to refer out more complex patients and receive referrals of less complex patients from public hospitals (Cheng et al., Reference Cheng and Vahid2015).
Table 2 Number and length of stay for selected diagnosis-related groups, Australia, 2010–2011

Note: CC=complications or comorbidities.
Source: Author’s analysis.
Table 2 shows that private hospitals admit proportionately more of the simpler elective hip and knee replacements (for hips, around 58% for the simpler around 67% for the simpler – without catastrophic complications or comorbidities; around 42% for more complex) than expected given the prevalence of private health insurance in Australia (around 47%). In contrast, for three of the four arthroplasty groups, private hospitals admit a much smaller proportion of emergency admissions. Patients in private hospitals tend to stay longer than patients in public hospitals, suggesting they may be less efficient (all differences for arthroplasty groups are statistically significant).
Medical practitioners are able to work in both the public and private sectors, with most working in both (Cheng et al., Reference Cheng, Joyce and Scott2013). A key determinant of whether medical practitioners choose to work in the public or private sectors is remuneration. In Australia, remuneration per hour is greater in the private sector than it is in the public sector. This differential remuneration creates a theoretical incentive to work in the private sector, and this is borne out empirically: Cheng and Vahid (Reference Cheng, Haisken-DeNew and Yong2011) have shown that an increase in private earnings is more than offset by any reduction in earnings from the public sector.
It is possible that one consequence of this combination of incentives, insofar as it promotes private activity over public activity, is greater waiting times in the public system. Some supporting evidence for this hypothesis can be seen in that median waiting times for procedures are lower when the public patient share of activity for that specialty is greater (Duckett, Reference Duckett2005).
However, attributing causation to this result is problematic, in part because it is difficult to determine the direction of causation. There are two competing hypotheses. One suggests that doctors create waiting lists in the public sector to increase demand for their work in the private sector, for which they earn more. The other suggests that the supply imbalance in the public sector has its root in under-resourcing of the sector, which drives activity towards the private sector. There is no substantial empirical evidence that sheds light on which of these hypotheses is more credible. Evidence of the impact of private vs public sector earnings on waiting times is therefore inconclusive.
Private provision may not undermine Canada’s Medicare if the provision is under subcontract to the public funder as a complement and is not an alternative. For example, a number of Canadian provinces have experience with both not-for-profit hospitals (especially run by Roman Catholic religious groups) and for-profit specialist providers functioning within the Medicare framework. In contrast, private funding certainly has its dangers. As the Australian experience shows, private funding brings the risk of potential cream-skimming and differential access, and does little to reduce pressure on waiting times. There is also little evidence that private provision improves efficiency through competitive pressure, and may lead to increased prices (Buckley et al., Reference Buckley, Cuff, Hurley, McLeod, Mestelman and Cameron2012).
Conclusion
Australia’s mixed public–private, Commonwealth-state health system has both positive and negative lessons for Canada. The common heritage of the dominant culture has led to many similarities in system design (Crichton, Reference Crichton1998); but it is the differences which can lead to lessons from one country to the other. First, Australia has expanded provision in two key areas where there is quite inadequate provision across Canada: access to pharmaceuticals and programmes to support older people in need of home-based or residential care. Australia’s pharmaceutical strategy has resulted in lower prices being paid for medications compared with Canada and may provide evidence to those who claim a Canadian ‘Pharmacare’ may be able to be at least partly funded by better drug prices.
Australia might also provide lessons about driving efficiency in hospital provision and in adapting a fee-for-service system to meet the needs of people with chronic conditions.
There are also lessons about what to avoid. Australia’s high level of out-of-pocket costs and mixed private funding arrangements are associated with both differential access and barriers to seeking care.
Acknowledgement
Valuable comments were received from reviewers and participants in the AMS 80th Anniversary Symposium. Remaining errors are the author’s.