The Traumatic Stress Service (TSS) at the Maudsley Hospital is a multidisciplinary tertiary specialist out-patient unit providing assessment and treatment for traumatised individuals. The service has a commitment to offering treatment to those with a history of chronic and/or multiple traumas in adulthood (for example warfare, torture, domestic violence) and/or childhood (for example sexual abuse) and who therefore typically present with complex trauma reactions (Reference van der Kolk, Roth and PelcovitzVan der Kolk et al, 2005). Consequently, although all patients taken on for treatment suffer from post-traumatic stress disorder (PTSD) and, invariably, depression, the majority also present with further complications probably familiar to those working in community mental health teams (CMHTs). Typically, these are personality disorders, substance misuse, significant risk of suicide and/or violence to others, enduring personality change, self-harm, psychiatric histories pre-dating the index trauma, significant social problems and the need for interpreters.
The National Institute for Health and Clinical Excellence (NICE) guidelines (National Collaborating Centre for Mental Health, 2005) indicate that the first-line treatment for PTSD is trauma-focused cognitive-behavioural therapy (CBT; for example Reference Ehlers and ClarkEhlers & Clark, 2000) or eye movement desensitization and reprocessing (EMDR; Reference ShapiroShapiro, 1995). Such approaches are both trauma-focused in that they involve some degree of retelling the traumatic story to process disturbing memories of the event, among other goals. These NICE recommendations are based on favourable results from the meta-analysis of numerous clinical trials. It is worth noting, however, that for understandable methodological reasons, the majority of the 30 studies reviewed in the meta-analysis tended to exclude patients in their samples if they presented with the above-mentioned complications (the few exceptions to this include Reference Paunovic and OstPaunovic & Ost, 2001; Reference Resnick, Nishith and WeaverResnick et al, 2002; Reference Kubany, Hill and OwensKubany et al, 2004). Furthermore, only one of the studies (Reference Paunovic and OstPaunovic & Ost, 2001) is concerned with the treatment of refugees, which make up an important proportion of trauma victims presenting to NHS clinics.
Within the TSS, CBT and EMDR are routinely used for the treatment of PTSD symptoms. However, the aforementioned complications have dictated a more flexible approach, and the treatment offered has therefore evolved and adapted to take them into account.
In general, the concept of complex PTSD (Herman,Reference Herman1992a ,Reference Herman b ) or disorders of extreme stress not otherwise specified (DESNOS; Reference Pelcovitz, van der Kolk and RothPelcovitz et al, 1997; Reference van der Kolk, Roth and PelcovitzVan der Kolk et al, 2005) is often used as an overarching framework for guiding treatment at the TSS. The syndrome encompasses the psychological sequelae resulting from more prolonged trauma such as torture, sexual and domestic abuse, as opposed to a single event. In addition to the symptoms of PTSD (intrusive experiences, arousal and avoidance), complex PTSD encompasses dissociation, relationship difficulties, revictimisation, somatisation, affect dysregulation and disruptions in identity (Reference HermanHerman, 1992a ).
Interventions at the TSS are typically informed by Herman's (Reference Herman1992b ) and Bloom's (Reference Bloom1997) treatment approach for complex PTSD and from an attachment disorder perspective (Reference HenryHenry, 1997; Reference WangWang, 1997; de Zulueta, Reference De Zulueta2002, Reference De Zulueta2006a ,Reference De Zulueta b ; Reference Ruiz, Bland and EdmondRuiz et al, 2005). Anecdotally, most patients have responded well to the treatment at the TSS. However, it is important to evaluate more systematically its effectiveness. The main aim of this study was therefore to investigate this by comparing pre- and post-treatment symptom measures. A further aim was to explore in more detail what team members perceive to be the additional complexities of the client group and how they have, as a result, adapted their approach to trauma work.
Method
Data collection
Data were collected on the patients who were offered assessment appointments over two financial years. Demographic information was collected as well as scores from self-report measures at assessment and end of treatment. The measures used were the Post-traumatic Diagnostic Scale (PDS; Reference Foa, Cashman and JaycoxFoa et al, 1997), the Beck Depression Inventory (BDI; Reference Beck and SteerBeck & Steer, 1987) and the Work and Social Adjustment Scale (WSAS; Reference Mundt, Marks and ShearMundt et al, 2002) for level of social impairment.
Data were also gathered on the problems in addition to PTSD that team members believed they had to address in interventions and the corresponding modifications they made to standard treatment approaches for PTSD. This was achieved by distributing the Adaptations to Trauma Work questionnaire survey, which asked team members to rate how often (i.e. never, sometimes, frequently) they had to focus on various other problems during their work in addition to PTSD (for example asylum issues, self-harm). The survey also included a list of possible interventions in addition to trauma-focused therapy and/or adaptations to trauma-focused work. Team members were asked to rate how often they used these approaches (never, sometimes, frequently).
Data analysis
The scores for each of the patients who completed the BDI, PDS and WSAS both at assessment and end of treatment were analysed using paired-sample t-tests. The data from the Adaptations to Trauma Work questionnaire were analysed by collating which items the majority of staff endorsed as ‘never’, ‘sometimes’ or ‘frequently’.
Results
Demographics
In total 354 patients were offered assessment appointments between the 1 April 2002 to 31 March 2004; 193 (60%) were male; 248 (70%) were neither employed nor studying; 184 (52%) were asylum seekers/refugees, and of these, 131 (71%) were still in the process of applying for asylum at the time of the assessment; 201 (57%) of all the patients offered assessments (i.e. not just asylum seekers/refugees) did not have English as their first language, and an interpreter was used for 120 of the patients (34% of the whole sample). These latter two figures are not equal because some patients’ level of English was sufficient for an interpreter not to be needed and because some team members speak other languages.
Outcome of assessment
Of the 354 patients who were offered an assessment appointment 84 (21%) did not attend. Of those 270 who came for the first appointment, 156 (58%) were offered treatment and 79 (29%) were not suitable for treatment and/or were referred elsewhere. Unsuitability for treatment at the TSS was occasionally based on the fact that the primary diagnosis was of another Axis I disorder other than PTSD, such as obsessive-compulsive disorder or schizophrenia. This was not often the case however, as individuals with other diagnoses hypothesised as having a traumatic origin (for example dissociative disorders or somataform disorders) were not excluded. The main reasons for unsuitability for treatment were: the patient was misusing drugs to the extent that they were intoxicated during the assessment, homelessness, the patient was about to be dispersed out of the catchment area, being in an ongoing abusive relationship and being at too high a risk of harming others to be managed on an out-patient basis. Sixteen patients (6%) were seen for a second opinion only and 20 (7%) dropped out at the assessment stage.
Treatment offered
Patients at the TSS are seen by team members for a modified psychiatric assessment (lasting 1-3 sessions), which can involve family members as well as professionals from other psychiatric teams. The findings are presented in the weekly team meeting where decisions are taken regarding the modality of treatment best suited to both the individual and social needs of the patient.
All 156 patients who were offered therapy were allocated to therapists trained in either EMDR or CBT for trauma-focused work. However, allocation was also based on what other problems they presented with. There were 90 patients (58%) with severe interpersonal difficulties/borderline features who were offered therapy with a professional trained in attachment-based psychotherapy or cognitive analytic therapy. Forty-seven (30%) had significant family/couple difficulties and were seen by a therapist with a systemic training. Nineteen (12%) were offered a structured psychotherapy group for survivors of childhood sexual abuse.
Of the 156 who were offered therapy, 112 (72%) completed treatment, 36 (23%) dropped out and 8 (5%) were either deported or moved out of area in the middle of treatment. The mean number of therapy sessions was 29 (s.d.=18) and the range was 4-77 sessions.
In addition to psychological therapy the vast majority of patients were being prescribed medication as per the NICE guidelines for PTSD. This was typically a selective serotonin reuptake inhibitor (SSRI); 125 patients entering treatment (80%) were already stable on such medication, previously prescribed by their CMHT or general practitioner (GP) for example. Twenty-three patients (15%) either had their existing medication changed or were started on medication for the first time as per NICE guidelines. Only 8 (5%) were not on any medication. Some patients with psychotic symptoms or very severe dissociative phenomena were also prescribed antipsychotic medication such as risperidone or olanzapine in low doses.
Effectiveness of treatment: comparison of measures pre- and post-treatment
Of those 112 patients who completed therapy, 48 (43%) completed the PDS and BDI both pre-treatment and at the end of treatment; 43 (38%) completed the WSAS pre- and post-treatment. There were a number of reasons why this figure was below 100%; for example, for non-English-speaking patients, the length of time needed to fill in these questionnaires via an interpreter (up to an hour) meant that some therapists did not prioritise completing the measures or it was unfeasible. Also many patients were not willing to fill in the questionnaires.
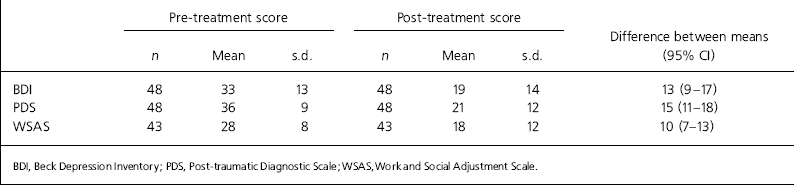
Mean scores pre- and post-treatment for each measure were all normally distributed and lower at the end of treatment than pre-treatment (Table 1). Paired-sample t-tests were performed for each measure and showed that these reductions were significant for the BDI (t=6.8, P<0.001) the PDS (t=8.7, P<0.001) and the WSAS (t=6.2, P<0.001). Furthermore, the mean scores for each measure shifted by one or more severity rating from pre-treatment to post-treatment.
Table 1. Comparison of measures pre- and post-treatment
| Pre-treatment score | Post-treatment score | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| n | Mean | s.d. | n | Mean | s.d. | Difference between means (95% CI) | |||||
| BDI | 48 | 33 | 13 | 48 | 19 | 14 | 13 (9–17) | ||||
| PDS | 48 | 36 | 9 | 48 | 21 | 12 | 15 (11–18) | ||||
| WSAS | 43 | 28 | 8 | 43 | 18 | 12 | 10 (7–13) | ||||
BDI, Beck Depression Inventory; PDS, Post-traumatic Diagnostic Scale; WSAS, Work and Social Adjustment Scale
Box 1. Problems in addition to post-traumatic stress disorder
Frequently occurring
Mental/physical health problems
-
• Severe depression with serious risk of suicide
-
• Severe interpersonal difficulties (e.g. violent anger out-bursts)
-
• Somatic/physical complaints (e.g. severe headaches, disability as a result of torture)
-
• Significant levels of dissociation
-
• Problems in keeping safe (e.g. patients repeatedly find themselves in abusive relationships)
Social/cultural issues
-
• Unsafe/unstable social situation (e.g. in contact with the perpetrator, becoming homeless)
-
• Difficulties working with interpreters
-
• Ongoing immigration/asylum issues (e.g. threat of deportation, court appearances)
-
• Significant social isolation (e.g. being only family member still alive)
-
• Complications arising from cultural factors (e.g. threat of ‘honour killings’ from husbands of rape victims)
-
• Legal problems that interfere with therapy (e.g. ongoing compensation case)
Occasionally occurring
Mental/physical health problems
-
• Self-harming behaviour (e.g. cutting)
-
• Substance misuse (mainly of alcohol)
-
• Psychotic symptoms (mainly hallucinations)
Adaptations to trauma work
Ten (83%) team members completed the Adaptations to Trauma Work questionnaire. In terms of presenting problems in addition to PTSD, the majority of therapists rated the difficulties shown in Box 1 as frequently prevalent during the course of therapy. A smaller number of problems were also rated by the majority of therapists as occasionally present; these problems were grouped under either mental/physical health problems or social/cultural issues.
In terms of adaptations to trauma-focused work all therapists reported that they often used the other approaches listed in the questionnaire. These are grouped in Box 2 under three categories.
Box 2. Adaptations to trauma-focused work
Therapeutic approach used
-
• Addressing dynamics in therapy resulting from childhood trauma (e.g. abuse/loss/neglect)
-
• Supportive/‘holding’ therapy (in times of crises)
-
• Being very flexible with the model of intervention
-
• Basic couple/family work
-
• Active risk management (e.g. instigating an in-patient admission)
-
• Prescribing medication
Additional techniques used
-
• Working with somatic complaints (e.g. using imagery, psycho-education)
-
• Teaching affect regulation (e.g. mindfulness, safe place/relaxation exercises)
-
• Anger/conflict management
-
• Addressing dissociation (e.g. using grounding techniques, identifying its triggers)
-
• Addressing self-harm (e.g. understanding its ‘function’, finding better coping mechanisms)
-
• Addressing substance misuse (e.g. looking at alternative coping strategies)
Liaison work
-
• Facilitating social integration/support (e.g. linking asylum seekers with appropriate voluntary organisations)
-
• Writing psychiatric reports for legal matters (for immigration or compensation purposes)
-
• Liaison with non-mental health workers (e.g. hostel workers, voluntary workers, solicitors)
Discussion
Service evaluation
The reductions in scores for those patients who completed the measures between assessment and post-therapy provide some evidence that the treatment approach being utilised at the TSS is effective. As well as showing statistically significant reductions in the scores, the shift in severity category for each measure indicates clinically significant improvements in levels of PTSD, depression and social functioning. However, much caution must be exercised in interpreting these findings, because a high proportion of patients did not complete pre- and post-measures. One cannot therefore assume that the findings of symptom improvement are representative of all the patients who received treatment at the TSS. This is particularly pertinent bearing in mind that the treatment completers would probably have shown more improvements compared with those that did not complete therapy. Furthermore, there was no control group so it is possible that the symptom reductions shown would have occurred spontaneously over time with no treatment, although this is unlikely in light of how chronic most patients’ problems already were by the time they were treated at the TSS.
In terms of the complexities of the client group, results from the staff questionnaire highlight the range of problems patients have in addition to PTSD. Many of these are psychological/psychiatric, such as dissociation, self-harm, severe depression and extreme somatisation. Many also reflect the complex social situations that the patients find themselves in (particularly asylum seekers), such as social isolation, the threat of deportation, unstable accommodation and cross-cultural family dynamics. Perhaps as a result of these complexities, comparison with the NICE studies also reveals how the severity of PTSD and depression of TSS patients at assessment (as measured by the PDS and BDI) is higher than in all but two (Reference Devilly and SpenceDevilly & Spence, 1999; Reference Paunovic and OstPaunovic & Ost, 2001) of the NICE studies that use these measures, although no statistical analyses were used to look for significant differences. Interestingly, the mean BDI score for TSS patients is more comparable with scores in outcome studies for major depression (Reference Fennell and TeasdaleFennell & Teasdale, 1982; Reference Hollon, Shelton and LoosenHollon et al, 1991).
Adaptation to trauma-focused work and models of treatment for complex PTSD
Staff at the TSS described various additional approaches in their interventions. First, working with patients from diverse cultures has meant being flexible with Western-based treatment models, for example integrating certain belief systems (e.g. religious) in order to find a shared meaning. Physical expression of psychic distress may be more common in some cultures, and therapists have to be creative in how they formulate this with their patients. Furthermore, taking into account the importance of the family and intervening at this level may also be vital before any change can occur.
Social interventions can also be crucial, particularly for asylum seekers, who may benefit most from support with housing, education, asylum applications and linking them with community groups. Liaison work and writing letters may be most appropriate in the early stages of treatment. Attention to these external factors also addresses the social attachment needs of these patients.
While the above ‘additional’ approaches to the trauma work are responses by therapists to each patient's particular problems rather than coming from a specific therapeutic orientation, at the TSS the complex-PTSD model referred to earlier is seen to be helpful in providing a guiding framework for the therapeutic work within which these specific techniques are used. Ford et al (Reference Ford, Courtois and Steel2005) describe a phased approach for working with complex trauma where phase 1 is ‘alliance and stabilisation’, phase 2 is ‘trauma processing’ and phase 3 is ‘functional reintegration’.
At the TSS the first phase - provision of safety (i.e. a secure base) - is seen as a crucial focus of the treatment programme and can take much time for severely traumatised and unstable patients. This is achieved through psychoeducation, affect regulation, medication, the establishment of a cohesive support network and the building up of a good therapeutic alliance, for example by helping with housing and immigration matters (for asylum seekers). This stage is where generic rather than specialised skills can be the most appropriate.
The next step, which involves remembering and/or processing and grieving while learning how to modulate feelings (without dissociating), is where CBT and EMDR techniques for processing traumatic memories are instrumental, although other models such as a narrative (Reference Schauer, Neuner and ElbertSchauer et al, 2005) or psychoanalytic approach (Reference GarlandGarland, 1998) are used. It should be noted that not all patients wish to embark on this stage for various reasons and it is not something that should be forced onto them, however much the therapist believes it is what they need to move on.
The final stage of reintegration is where the patient reconnects with ‘normal life’, engaging in previously excluded activities, examining the changes they have made in therapy and reconnecting with others.
Conclusion
The majority of patients referred to the Traumatic Stress Service present with complex problems, both social and psychological. The therapy models advocated within the NICE guidelines are often not sufficient for the treatment of such patients, who typically need more stabilisation before trauma-focused work can take place if at all. In this paper other approaches and ideas that fall within the complex-PTSD framework and can be used in the treatment of severely traumatised patients have been illustrated and some evidence for their effectiveness shown.
Further research needs to be carried out on what treatments work for ‘real-world’ trauma patients in order to aid clinicians working in this field. Future service evaluations could address the gaps in this study, for example investigating comorbidity more systematically (using diagnostics rather than therapist reports), teasing out which specific interventions are most effective and for which specific problems, including a control group and using other outcome measures to look at factors such as dissociation and interpersonal problems.
Declaration of interest
None.




eLetters
No eLetters have been published for this article.