Article contents
Effect of behavior therapy for Tourette's disorder on psychiatric symptoms and functioning in adults
Published online by Cambridge University Press: 27 August 2019
Abstract
Although behavior therapy reduces tic severity, it is unknown whether it improves co-occurring psychiatric symptoms and functional outcomes for adults with Tourette's disorder (TD). This information is essential for effective treatment planning. This study examined the effects of behavior therapy on psychiatric symptoms and functional outcomes in older adolescents and adults with TD.
A total of 122 individuals with TD or a chronic tic disorder participated in a clinical trial comparing behavior therapy to psychoeducation and supportive therapy. At baseline, posttreatment, and follow-up visits, participants completed assessments of tic severity, co-occurring symptoms (inattention, impulsiveness, hyperactivity, anger, anxiety, depression, obsessions, and compulsions), and psychosocial functioning. We compared changes in tic severity, psychiatric symptoms, and functional outcomes using repeated measure and one-way analysis of variance.
At posttreatment, participants receiving behavior therapy reported greater reductions in obsessions compared to participants in supportive therapy (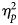 $\eta _p^2 $ = 0.04, p = 0.04). Across treatments, a positive treatment response on the Clinical Global Impression of Improvement scale was associated with a reduced disruption in family life (
$\eta _p^2 $ = 0.04, p = 0.04). Across treatments, a positive treatment response on the Clinical Global Impression of Improvement scale was associated with a reduced disruption in family life (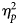 $\eta _p^2 $ = 0.05, p = 0.02) and improved functioning in a parental role (
$\eta _p^2 $ = 0.05, p = 0.02) and improved functioning in a parental role (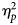 $\eta _p^2 $ = 0.37, p = 0.02). Participants who responded positively to eight sessions of behavior therapy had an improvement in tic severity (
$\eta _p^2 $ = 0.37, p = 0.02). Participants who responded positively to eight sessions of behavior therapy had an improvement in tic severity (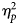 $\eta _p^2 $ = 0.75, p < 0.001), inattention (
$\eta _p^2 $ = 0.75, p < 0.001), inattention (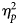 $\eta _p^2 $ = 0.48, p < 0.02), and functioning (
$\eta _p^2 $ = 0.48, p < 0.02), and functioning (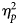 $\eta _p^2 $ = 0.39–0.42, p < 0.03–0.04) at the 6-month follow-up.
$\eta _p^2 $ = 0.39–0.42, p < 0.03–0.04) at the 6-month follow-up.
Behavior therapy has a therapeutic benefit for co-occurring obsessive symptoms in the short-term, and reduces tic severity and disability in adults with TD over time. Additional treatments may be necessary to address co-occurring symptoms and improve functional outcomes.
Keywords
- Type
- Original Articles
- Information
- Copyright
- Copyright © Cambridge University Press 2019
References
- 16
- Cited by




