In the USA, immigrant groups are the fastest-growing population segment, comprising 13 % of the total population, with 53 % from Latin America, 28 % from Asia and 4 % from Africa( Reference Gambino, Trevelyan and Fitzwater 1 , 2 ). Immigrant communities are disproportionately confronted with health disparities including childhood obesity and obesity-related chronic diseases( Reference Camerota 3 – Reference Walker and Barnett 5 ). According to national data, Hispanic youth have higher rates of overweight or obesity than their White counterparts( Reference Flegal, Kruszon-Moran and Carroll 6 ). Similarly, 16·7 % of 2–5-year-old Latino children are obese compared with 3·5 % of Whites( Reference Spencer, Thanh and Louise 7 ). In Minnesota the rate of overweight/obesity is also higher among Latino, Somali and Hmong adolescents compared with Whites( Reference Arcan, Larson and Bauer 8 ).
Although newly arrived immigrants in the USA are healthier and have better weight status than their US-born counterparts( Reference Dey and Lucas 9 ), their risk for obesity( Reference Goel, McCarthy and Phillips 10 ) and other chronic diseases( Reference Koya and Egede 11 – Reference Lear, Humphries and Hage-Moussa 13 ) increases with longer time in the USA. Immigrant families face stressors stemming from resettlement and adjustment in the host country( Reference Perera, Gavian and Frazier 14 ), including financial realities, language differences, time constraints( Reference Lytle, Hearst and Fulkerson 15 , Reference Fulkerson, Kubik and Story 16 ), structural issues such as neighbourhood safety( Reference Brewer and Kimbro 17 ), as well as new weather patterns( Reference Gordon-Larsen, McMurray and Popkin 18 – Reference Perez, Slymen and Sallis 20 ). Indeed, several studies of immigrants’ health have shown that changes in lifestyle behaviours, such as change in diet quality and physical activity (PA), may be contributing to increase in weight, increase in incidence of chronic diseases and decrease in immigrants’ perception of their health status( Reference Acevedo-Garcia, Bates and Osypuk 21 – Reference Akresh 23 ).
Families are essential agents of change providing a home environment that supports behaviours that influence weight( Reference Patrick and Nicklas 24 – Reference Kral and Rauh 27 ). Important aspects of the home food environment, such as home food availability, family meal frequency, food preparation, parent role modelling and parent’s encouragement for healthy eating, have been associated with weight-related dietary behaviours among youth( Reference Arcan, Neumark-Sztainer and Hannan 28 , Reference Savage, Fisher and Birch 29 ). Most of the research exploring the home food environment in immigrant families has involved Hispanics/Latinos( Reference Crawford, Gosliner and Anderson 30 – Reference Pham, Harrison and Kagawa-Singer 32 ), with a paucity of data for other immigrant groups, such as Hmong and Somali( Reference Wieland, Weis and Palmer 33 – Reference Tiedje, Wieland and Meiers 37 ). However, there are limited data among immigrant families with younger-age children, including Latinos( Reference Crawford, Gosliner and Anderson 30 – Reference Pham, Harrison and Kagawa-Singer 32 , Reference Wieland, Tiedje and Meiers 34 , Reference Bayles 38 – Reference Ayala, Ibarra and Binggeli-Vallarta 40 ). With the continuous arrival of immigrant groups and the ongoing changes in previously arrived people, further studies are needed to understand commonalities as well as differences in lifestyle behaviours of immigrant families with children. These identified issues could then inform programmes to support practices for healthy-weight children in immigrant populations.
According to the National Institutes of Health’s Summit on The Science of Eliminating Health Disparities, health disparities research should build on strong community collaborations that promote community engagement( Reference Dankwa-Mullan, Rhee and Williams 41 ). Community-based participatory research (CBPR) is particularly appropriate for immigrant populations that are not routinely included in national studies, since it engages community partners as active participants in building knowledge in their unique communities( Reference Panapasa, Jackson and Caldwell 42 – Reference Israel, Schulz and Parker 45 ).
Following a CBPR approach, in the present study researchers and Somali, Latino and Hmong (SLH) community members sought to identify parents’ perceptions of childhood body weight and obesity, barriers to and enablers of families’ dietary and PA approaches, and suggestions for food and activity programmes that could support parents’ efforts to raise healthy children. The long-term goal of the study was to inform the development of culturally appropriate programmes that would prevent obesity in SLH children.
Methods
The current CBPR study involved an academic–community partnership that included one academic researcher and eight community researchers (two clinic staff and six community members; two Somali, two Latino, two Hmong) with SoLaHmo Partnership for Health and Wellness (SoLaHmo), which is a community-participatory research programme of West Side Community Health Services, Inc. (West Side), in the Twin Cities, Minnesota, USA. All community members had CBPR and qualitative research training and experience and were involved in all phases of the project, including conception of the study, development of questions, administration, transcription, translation and analysis of focus groups, and interpretation of study findings.
Study design and procedures
Ten focus groups (three Somali, four Latino, three Hmong), were conducted with sixty-seven adults (n 28 Somali, n 19 Latino, n 20 Hmong; 81 % women) who were primary caregivers of at least one child aged 3–12 years (Table 1). With the exception of one participant, all others were born outside the USA; the number of years since their arrival to the USA differed for each ethnic community (Somalis: 1–12 years; Latinos: 2–20 years; Hmong: 6–26 years). Participants were recruited through telephoning patients at West Side and advertising at community centres and housing projects. (Note: we have used the word ‘parents’ throughout to designate all caregivers.)
Table 1 Demographic characteristics of Somali, Latino and Hmong participants in the Twin Cities, Minnesota, USA, September 2011 through August 2012
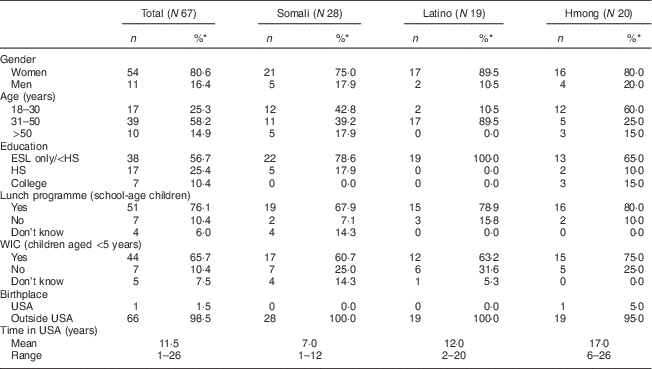
ESL, English as a second language; HS, high school; WIC, Special Supplemental Nutrition Program for Women, Infants, and Children.
*The values might not add up to 100 % due to incidental missing data.
The focus group questions were collectively developed by the entire group following extensive review of prior qualitative studies among immigrant populations. The focus groups lasted 1·5–2 h and took place at West Side, community centres or housing projects. They were conducted in a semi-structured manner in participants’ native language or English by a trained native-speaking SoLaHmo community researcher and were supported by the academic researcher and two community researchers (one clinic staff and one native-speaking note taker). After the third focus group for each community, the research team decided a fourth group was necessary for the Latino community in order to obtain saturation; general focus group guidelines support aiming for saturation of ideas, which usually occurs with two to five groups per category of participants( Reference Carlsen and Glenton 46 ). Prior to focus groups a brief demographic survey was completed by participants about their age, gender, education, birthplace, years lived in the USA, and their children’s participation in the free or reduced-price school lunch and WIC (Special Supplemental Nutrition Program for Women, Infants, and Children) programmes.
The focus group questions elicited parents’ views about healthy weight-children, causes of childhood obesity, barriers to and enablers of children eating and being physically active, aspects of their culture about healthy eating and being active that they wished to pass on to their children, and elements of potential programmes for children to achieve or maintain a healthy weight. Participants received $US 20 for their participation. The study was approved by the Institutional Review Board of the University of Minnesota.
Data coding and analysis
A thematic analysis approach was utilized to analyse the transcripts with the full team, following CBPR principles( Reference Jackson 47 ). Initially, each community research team independently coded one transcript of its community’s focus group, and then the entire research group met to identify a common coding tree. Guided by the common coding tree, each community team coded all of its community’s focus group transcripts. In a reiterative fashion, the entire group met again to adjust the coding tree, and each team completed its focus group coding. Once all transcripts were coded, the entire group met again to identify themes and sub-themes( Reference Morgan and Krueger 48 , Reference Vaismoradi, Turunen and Bondas 49 ). The derived themes were then discussed and interpreted by each community, based on its cultural norms and beliefs. Similarities and differences among the three ethnic communities were collectively determined by all members.
Results
The overarching theme for all three cultural groups was ‘parents’ challenges in raising healthy-weight children in the USA’. SLH parents are trying to raise healthy-weight children based on their understanding of children’s health, contributors to obesity, and importance of diet and PA, while dealing with social, economic and environmental challenges and trying to maintain their cultural identity and traditions. As there were more similarities than differences across the three ethnic groups, the common themes and sub-themes are presented first and any ethnic differences are subsequently specified. Tables 2–5 display quotes that represent the larger set of participants’ quotes (Table 2: parents’ perceptions of healthy weight and causes of childhood obesity; Table 3: parents’ goals, challenges and approaches for children to eat healthy foods; Table 4: parents’ goals, challenges and strategies for children to be physically active; Table 5: parents’ programmatic suggestions)
Table 2 Somali (S), Latino (L) and Hmong (H) parents’ perceptions of healthy weight and causes of childhood obesity, the Twin Cities, Minnesota, USA, September 2011 through August 2012
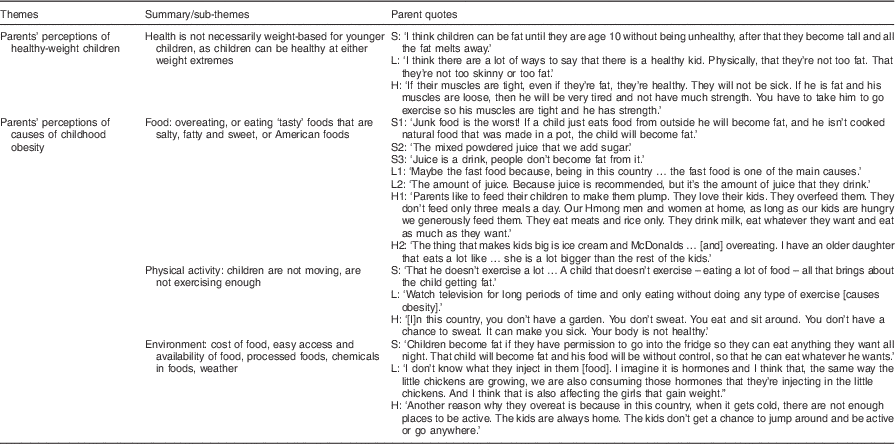
Table 3 Somali (S), Latino (L) and Hmong (H) parents’ goals, challenges and approaches for children to eat healthy foods, the Twin Cities, Minnesota, USA, September 2011 through August 2012

WIC, Special Supplemental Nutrition Program for Women, Infants, and Children.
Table 4 Somali (S), Latino (L) and Hmong (H) parents’ goals, challenges and strategies for children to be physically active, the Twin Cities, Minnesota, USA, September 2011 through August 2012

Table 5 Somali (S), Latino (L) and Hmong (H) parents’ programmatic suggestions, the Twin Cities, Minnesota, USA, September 2011 through August 2012

Parents’ perceptions of healthy weight and causes of childhood obesity
Parent’s perceptions of healthy-weight children
In general, parents from SLH communities stated that healthy children are happy and active, they sleep well and are not frequently sick. They described healthy children as having good appetites, high energy levels, colour in their faces or lips, and good muscle tone. In contrast, parents characterized unhealthy children as weak, becoming sick more often, not sleeping well, having poor appetites, pale faces, low energy levels and poor muscle tone, and perhaps being sad, lazy or depressed. Participants discussed that health is not necessarily weight-based, as children can be healthy at any weight, including weight extremes. Some Hmong and Somali parents said children in the middle of the weight range are likely to be healthier and stronger, with heavy and skinny children likely to be unhealthier and weaker, while a few Hmong parents said that fat children are healthy (Table 2).
Causes of childhood obesity
Participants from all three communities shared similar ideas about causes of childhood obesity. They stated that obese children in the USA are eating too much, or eating ‘bad’ foods (which they described as ‘tasty’, including salty, fatty and sweet foods) or eating ‘American’ foods (pizza, hamburgers, fast foods and junk food). Regarding PA, participants stated that obese children are not moving, are not exercising enough and are engaging in too many sedentary activities (i.e. watching too much television and playing too many video games). Participants also mentioned multiple environmental factors contributing to obesity, such as the low cost of unhealthy foods and the high cost of healthy foods, easy access to and availability of unhealthy foods, processed foods and chemicals (like pesticides) in foods. Finally, a few participants described a variety of biological factors that could contribute to children’s obesity, such as genetics (parents are fat so children are fat), metabolism (some children eat less and still get fat), digestion (some children digest more or less of the foods they eat) and body composition (some bodies are just fat).
Parents’ goals, challenges and approaches to healthy foods and physical activity
Parents’ perceptions of food and physical activity
Tables 3 and 4 list the parents’ perceptions, goals, challenges and approaches. All three groups noted that their everyday traditional foods are healthy, their ceremonial traditional foods are unhealthy if eaten daily and ‘American’ foods are unhealthy. The traditional daily foods that parents considered healthy were fresh organic vegetables, milk, goat meat and wheat for Somalis; rice and beans for Latinos; and boiled rice, organic vegetables and boiled meat for Hmong. Traditional celebratory foods were generally identified as less healthy, such as Latino tamales, Hmong pig soup, and Somali halwa (dessert) and meat. For Somalis, healthy foods include foods that are purchased, prepared and consumed the same day. The general consensus was that there are important cultural foods that they wish to maintain. However, in their native countries some ceremonial traditional foods were available only at certain times of the year, while they are more readily available and more frequently consumed in the USA.
Parents recognized that PA is important for their children’s health, stating that healthy children are inherently physically active and interactive with other people and their environment, while unhealthy children are slow, lazy, weak and inactive. However, the importance of regimented activity differed by community. Somali parents believed that young children are naturally active so do not need organized exercise routines and that older children exercise at school so do not need after-school activities. Latino parents viewed children’s physical ‘mischief’ as normal and establishing an exercise routine (such as after-school play time) and having family-oriented PA were essential. Hmong parents viewed high levels of children’s activity to the point of being naughty as expected and healthy; they also identified the importance of a routine, stating that children are not as naughty when they are consistently active, and stressed the need to guide young children before they make decisions on their own.
Parents’ goals for children’s eating and physical activity
Parents from all three communities shared a main goal about feeding that was to provide healthy food so their children were healthy. They also had two other goals: keep their children happy about food so they would eat and not be malnourished, which might include feeding and eating unhealthy ‘American’ foods; and teach their children to prepare traditional foods to be self-sufficient and maintain their cultural identity (Somali and Hmong). Aiming to keep their children happy, parents experienced a conflict between wanting to offer healthy foods (which children may not want) and buying more unhealthy foods (which children may want), such as ‘American’ commercial foods and school lunches. Hmong families emphasized teaching boys and girls to cook so that they could be functioning mature adults, while Somalis focused on teaching cooking skills to girls.
Similarly, parents from all three communities shared the same goal of supporting PA for their children so they would be healthy and happy, while ensuring their safety during PA. However, many recognized that purposeful exercise done to promote physical health was not supported by their traditional cultures. Hmong and Somali parents particularly stressed the importance of sweating in being healthy and noted a marked decrease in sweating in the USA from their home countries because of differences in lifestyle and occupational requirements (e.g. walking to the market or farming in their home country).
Parents’ challenges to meeting healthy food and physical activity goals
Parents reported facing similar challenges in their efforts to help their children eat healthy foods and be physically active. Overall, SLH parents tried to achieve a balance between cost, convenience, time, nutritional benefits and family eating habits. The challenges reported by parents included children’s desire for ‘tasty’ foods (salty, fatty and sweet foods), foods that many parents consider ‘unhealthy’ (American foods like pizzas and hamburgers or traditional ceremonial foods) and a narrow range of specific foods (‘picky eaters’). According to a few Hmong parents, their foreign-born children were more receptive to everyday traditional foods compared with their US-born children.
Parents also reported uncertainties about what foods and cooking techniques are healthy and unhealthy – for both traditional and American foods. They also cited structural and environmental factors that influenced their purchasing, preparing and serving healthy foods, such as cost of food, time constraints to prepare food, transportation costs to obtain food, lack of traditional food availability, ease of obtaining and abundance of prepared foods, school food and advertising of unhealthy foods. Somali parents expressed concern about advertisements that expose children to unhealthy American foods, while both Hmong and Latino parents reported concerns about the negative influence of school lunches and the school food environment on their children. In addition, Latino and Hmong parents expressed disappointment with their (or other adult family members’) behaviours of not being the best ‘role models’.
Similarly, SLH parents faced challenges in achieving balance for PA, including cost, convenience, time, transportation and family habits. Some expressed common concerns with children’s preferences for sedentary activities (e.g. watching television or playing video games) which, when coupled with children’s resistance to PA, were difficult for parents to overcome. They also expressed struggles, including uncertainties about how to support children’s exercise, given their own lack of personal exercise, their lack of knowledge about exercise programmes and organizations, their busy lives and key structural constraints. Parents struggled to find time for regular family exercise, given work, school or day care schedules, being tired after work and school, and having to attend to extended family needs especially on the weekends. They also cited significant structural and environmental issues as obstacles to exercising, including neighbourhood safety, winter weather causing discomfort and illness, and playing inside in small homes because of space constraints, leading to noise and possible eviction notices. Challenges in accessing community organizations with exercise programmes because of high cost, distance and language barriers were also reported. In addition, Somali parents found most PA programmes unacceptable because of women’s revealing clothing and not being separated by gender. Latino parents had experiences with feeling unwelcomed and even discriminated against at fitness centres.
Parents’ approaches to overcoming challenges
Parents utilized various approaches to ensure their children ate healthy foods and were physically active. Generally, all parents purchased and prepared foods they considered healthy and avoided foods they considered unhealthy. In addition to cultural variations about which foods or approaches were considered healthy, a few Somali parents mentioned trying to cook traditional foods in healthy ways; Latino parents emphasized the importance of having regular family meals; and Hmong parents stressed serving a variety of foods and colours, as well as valuing the knowledge they gained from doctors (e.g. eat lean meats and avoid fatty pork; boil rather than fry foods). Overall, parents described striving to serve healthy, traditional foods cooked in a variety of ways that their children would enjoy.
To accommodate their children’s food preferences, parents described two distinct parenting approaches: they either (i) prepared multiple meals to satisfy individual preferences to ensure their children were not hungry or (ii) prepared one meal for everyone in the family. Most Hmong parents mentioned catering to their children’s desires including purchasing a variety of foods and/or cooking foods multiple ways (e.g. an American meal for children and a Hmong meal for adults); Somali and Latino families reported using either approach.
Parents from each community used various feeding practices and food-related messages to encourage their children to eat, such as setting expectations and limits, although different approaches were emphasized across ethnic groups. Somali parents described encouraging their children to finish their food by telling them that the last piece of the food has the ‘most reward’, referring to religious context of being rewarded for cleaning one’s plate. Latino parents stressed the importance of trying new foods, giving warnings that overeating will lead to obesity and avoiding offering food as a reward for good behaviours. Hmong parents commonly told their children to eat until they are ‘stuffed’; however, some Hmong parents also set limits on ‘bad’ foods.
Parents stressed the importance of being good role models for preparing and eating healthy foods and setting food schedules, although they had different emphases. Latino and Hmong parents wanted their children to eat scheduled meals and not snack repeatedly throughout the day. Latino and Somali parents particularly stressed the importance of family meals because it reinforces the meaning of family. In addition, parents acknowledged their role modelling as a strategy to help their children eat healthily and be physically active, although they recognized the challenges and limitations of being effective role models, given their own behaviours.
Regarding their children’s PA, parents had similar strategies with slight differences across the three communities. They mentioned the importance role modelling PA and the role of others (e.g. extended family members) who are often involved in raising their children and their influence on their children’s behaviours. Given limited indoor space and severe winter weather in Minnesota, parents from different ethnic groups creatively made do with what they had: walking up and down hallways and stairways in apartment buildings, setting up space in basements, buying interactive video games, and dancing to videos and music. While the summer provided more opportunities for low-cost activities like outdoor play, parents expressed their desire to know more about non-expensive places for children’s activities during the winter, such as low-priced neighbourhood programmes and local gymnasiums. They were generally hopeful about schools providing exercise for their children, with Somalis assuming that schools do so during the school day, while Latinos were critical of schools for not supporting after-school activities. Hmong and Latino parents expressed valuing and enjoying activities with their children and some Somali parents seemed to like the idea of exercising at a gender-divided gym while their children are occupied.
Parents’ programmatic suggestions
Table 5 describes the parents’ suggestions for programmes to help them improve their families’ healthful eating and PA. Parents across all three communities voiced an interest in cooking classes for adults and children to gain new knowledge about identifying and cooking healthy foods, learning about which American foods are healthy/unhealthy and shopping for healthy foods on a budget. Participants wanted programmes that are free, easy to access (or with free transportation), provide childcare or children’s programming, and are offered at convenient times to accommodate family schedules. Latino and Hmong parents wanted programmes to incorporate recipes for quick, tasty and healthy meals, and healthy portion sizes. Latino parents were also interested in learning more about food preservation and meal planning, age-appropriate healthy body size, and becoming knowledgeable about and involved in improving the quality of school food programmes. Hmong parents were interested in learning about age-appropriate healthy food choices for children, identifying healthy options at fast-food restaurants, and understanding the medical risks of unhealthy diets for both obesity and eating disorder prevention. Somali parents specified that religious requirements (e.g. no pork) needed to be observed in any programme.
Participants from all three ethnic communities wanted convenient access to open spaces for exercise, particularly large indoor spaces in which their children could run and play. Hmong and Latino parents welcomed family-based exercise activities, while Somali participants desired separate exercise spaces for men and women. Latino parents wanted more information about local free or low-cost programmes, particularly where families could exercise together and where peers could motivate children to be physically active. All parents wanted to stay warm in the winter, with Latinos expressing some desire to be active outside in the winter, including participating in winter sports. Hmong parents mentioned the possibility of combining cooking and exercising programmes. While not a requirement, Somali and Hmong parents preferred an exercise instructor of their ethnicity; for Somalis, this could be combined with teaching traditional cultural activities such as dances, storytelling and games.
Discussion
The current CBPR qualitative study identified SLH parents’ perceptions about children’s weight, causes of childhood obesity, parent’s goals to raising healthy-weight children, challenges to dietary and PA goals, and approaches to addressing these challenges. The findings indicate that immigrant parents aim to raise healthy and happy children in the USA by balancing their understanding of obesity, eating and PA with their economic and social challenges, while attempting to maintain their cultural identity. Overall, there were more similarities than differences in SLH parents’ experiences of feeding their children and supporting their PA, which emphasizes the common social, environmental, structural and economic factors of living in the USA( Reference Tiedje, Wieland and Meiers 37 ). Similar results as in our study emerged in previous qualitative studies conducted with immigrant populations (e.g. Somali, Mexican and Cambodian)( Reference Wieland, Tiedje and Meiers 34 , Reference Tiedje, Wieland and Meiers 37 ). The similarities shared by these communities about raising healthy children around their dietary intake and PA indicate that a core intervention programme designed for immigrant parents could be relevant to multiple ethnic groups, with adaptations for language and culture.
Although the majority of SLH parents reported that a child’s weight is not necessarily health-based and children can be healthy at both ends of the weight range, the majority of participants indicated that being in the middle of the weight range is likely to be healthier. This finding is consistent with other qualitative studies among immigrant groups that found a child’s health is defined not by weight but by appearance such as energy level, skin and hair appearance, and emotional health, such as happiness( Reference Crawford, Gosliner and Anderson 30 , Reference Pham, Harrison and Kagawa-Singer 32 ). These parents were generally more concerned about their children not becoming malnourished than not becoming obese. Thus, the parents were willing to fulfil their children’s preference for ‘unhealthy American’ foods, contrary to parents’ desire to feed them their everyday traditional foods. In a recent study of parent feeding styles among low-income first-generation Hispanic mothers, compared with USA-born mothers, immigrant mothers more frequently pressured their children to eat, used food as a reward and limited intake of non-healthy foods( Reference Power, O’Connor and Orlet Fisher 50 ). Similarly in a previous study, Somali parents favoured large portion sizes and a larger body size as a sign of better health( Reference Tiedje, Wieland and Meiers 37 ). Variation in feeding styles and concern about child malnutrition may reflect cultural norms and past experiences around food, especially food insecurity and immigration status, which may have been true for some participants in the present study( Reference Peterman, Wilde and Liang 51 ). However, our study did not assess the participants’ resettlement process prior to arrival in the USA. Since past food experiences may be integral factors in shaping immigrant families’ behaviours about feeding children, future studies should explore and address these factors.
The challenges reported by these parents present opportunities for interventions to improve families’ dietary and PA behaviours. One of the identified challenges was the generational differences in food preference, as older family members prefer more traditional foods than younger members, and as some (perhaps foreign-born) children prefer traditional foods compared with other (particularly American-born) children. The diverse eating patterns among family members may reflect the interplay of multiple factors, including structural issues, desire for cultural preservation, school food, the local food environment and the media( Reference Franzen and Smith 52 , Reference Mulasi-Pokhriyal and Smith 53 ). According to findings of other qualitative studies with immigrant populations, the preference for ‘American’ foods by children and adolescents may be the result of the children’s reactions to their families’ desire and control to maintain traditional food ways( Reference Tiedje, Wieland and Meiers 37 ). Future studies should assess intergenerational dynamics with respect to eating and PA, and future healthy-weight programmes for immigrant communities should include intergenerational communication and interaction as an integral component( Reference Rhodes, Chan and Prichard 54 ).
Other challenges reported by SLH parents that were found in other qualitative studies were lack of knowledge about what constitutes healthy foods( Reference Head, Barr and Baker 55 ), especially American foods preferred by their children( Reference Tiedje, Wieland and Meiers 37 , Reference Franzen and Smith 52 ), unfamiliarity with certain local fruits and vegetables and ways to prepare them, and lack of control of children’s eating habits. Overall, parents expressed limited knowledge of the local food environment, their belief that American foods are unhealthy and traditional foods are healthy, and their desire to pass on traditional foods and eating habits to their children. Our findings suggest that many immigrant families have had limited exposure to American foods, therefore they may be unaware of a range of ‘healthy’ American foods. A study by Arcan et al. found that Somali adolescents consumed fast food almost daily( Reference Arcan, Larson and Bauer 8 ). Fast-food and other low-cost food consumption is often linked to lower socio-economic status and overall neighbourhood food availability( Reference Watts, Mason and Loth 56 – Reference Cook, Tseng and Tam 59 ), and in our study cost of foods was reported as one of the challenges preventing parents from feeding their families healthier foods. When immigrant families first arrive to the USA, their limited financial resources and lack of familiarity with local healthy foods may prohibit them from purchasing healthy options, thus exposing them predominantly to the taste and familiarity of convenient foods. As Lee et al. posited, a longer stay in the USA was strongly correlated with negative dietary changes among adult immigrants. Further, both length of stay and dietary changes were strong predictors of negative self-reported health status, indicating the decline of diet quality may be a factor in the pathway towards declining health( Reference Lee, O’Neill and Ihara 22 ). Collectively, these findings present a great opportunity for nutrition education, especially soon after arrival to the USA, to introduce immigrant families to healthy American foods and ways to obtain and prepare them on a limited budget.
To maintain their cultural identity and feel connected with their past while in the host country, immigrant families participate in ethnic social occasions that involve sharing food, especially ‘ceremonial foods’ that may be high in energy, fats and refined carbohydrates. The parents recognized that these foods, which were previously consumed only on special occasions, are now more readily available in the USA and are increasingly becoming a part of everyday diet( Reference Azar, Chen and Holland 60 ). A previous focus group study among Somali parents indicated lower intakes of fruits and vegetables and higher intakes of meat and pasta, reflecting their perception that meat consumption was associated with higher social status( Reference McEwen, Straus and Croker 61 ). Recognizing the need for social connectedness and the increasing role of ceremonial foods in immigrant diets, nutrition interventions can incorporate tips on healthful choices and cooking methods of these foods.
The need for social connectedness among immigrant groups was also expressed when SLH parents recommended that future programmes promoting PA are family- and community-focused. Although all participants agreed that PA was important in achieving and maintaining health, they cited challenges to PA that are common to other immigrant groups, including socio-economic position and environmental and structural factors( Reference Wieland, Weis and Palmer 33 , Reference Wieland, Tiedje and Meiers 34 , Reference Gidlow, Johnston and Crone 62 ). Moreover, the way PA was conceptualized and practised by some immigrant groups might pose an additional challenge to being physically active in the host country( Reference Wieland, Tiedje and Meiers 34 , Reference Rothe, Holt and Kuhn 63 ). As physical labour and sweating were an integral part of their daily work routines, many immigrant groups are not accustomed to recreational exercise and do not feel as if they are physically active without sweating( Reference Wieland, Tiedje and Meiers 34 ). In addition, as expressed by Somali participants, moral and cultural norms about gender differences in PA practices and prohibitions against exercising in public should be addressed in order to increase participation and ensure sustainability of behaviours( Reference Devlin, Dhalac and Suldan 64 ). An example of a culturally tailored programme that respected gender differences was the development of a swimming programme for Somali women in Seattle( Reference Moore, Ali and Graham 65 ).
Study limitations include the convenience sample of focus group participants that limits the generalizability of the findings; the qualitative design that prevents quantification of differences across ethnic groups; and lack of measurement of acculturation that prevents discussion about the families’ acculturative change. Lastly, although the inclusion of immigrant participants from three distinct ethnic communities makes the sample heterogeneous, the findings of the study may not be generalizable as they reflect the influence of the social norms of the local environment on the participants’ food- and PA-related attitudes and behaviours that may be different for people living in different geographic areas.
Conclusions and implications
The study’s findings indicate that immigrant parents aim to raise healthy-weight children by providing healthy foods and PA for their children. However, they face multiple challenges that require parents’ adjustment and negotiation between the push of dominant culture, new familial and generational dynamics, and preservation or development of their ethnic community identity. These study results will guide the design of programmatic interventions with strong community participation, following the principles of CBPR, in order to maximize the programme’s effectiveness. Future programmes should elicit participants’ goals, build upon common goals, acknowledge and attempt to address the challenges that impair parents’ abilities to meet their goals, and focus on building parents’ knowledge, skills and strategies needed to address the challenges. Future qualitative research should extensively measure level of acculturation for each ethnic community to address the participants’ specific needs more effectively. While logistical issues of language, location, food preferences and activity preferences have to be addressed, programmes that draw people from different ethnic groups together could allow for successful learning and sharing between groups, strengthen relationships between people, and empower them to form alliances that could address larger societal issues, such as safe neighbourhoods.
Acknowledgements
Acknowledgements: The authors extend their appreciation to all community members who participated in the focus groups. They extend special appreciation to Hodan Dualeh, Warda Geele, Luis E. Ortega, Mai See Thao and Charles Vang, SoLaHmo members, for their participation in all phases of the project. Financial support: This work was supported by the UCare Foundation (grant number 2011-09R). The UCare Foundation had no role in the design, analysis or writing of this article. Conflict of interest: None. Authorship: At the time of the study, C.A. was a Research Associate at the Division of Epidemiology and Community Health, School of Public Health, University of Minnesota, Minneapolis. C.A. was the lead author and participated in the study development, analysis and interpretation of the results. K.A.C.-P. participated in the study development, analysis and interpretation of the results, and critically reviewed and edited the manuscript. S.P. advised on the CBPR approach, participated in the study development, analysis and interpretation of the results and critically reviewed and edited the manuscript. M.R.-L. conducted, transcribed and translated the focus groups, participated in data analysis and interpretation of the results, and reviewed the manuscript. M.B.X. conducted, transcribed and translated the focus groups, participated in data analysis and interpretation of the results, and reviewed the manuscript. Ethics of human subject participation: This study was conducted according to the guidelines laid down in the Declaration of Helsinki and all procedures involving human subjects/patients were approved by the Institutional Review Board of the University of Minnesota. Written informed consent was obtained from all subjects.










