Mental capacity is a multidimensional construct that is a central determinant of an individual's ability to make autonomous decisions. Its assessment has become increasingly important with the move away from the paternalistic role of healthcare professionals towards a greater emphasis on an individual's own treatment decisions (Reference SchneiderSchneider, 1998). The American Psychiatric Association has developed a model statute which uses a mental capacity test (Reference Stromberg and StoneStromberg & Stone, 1983). In many other jurisdictions mental capacity and mental health legislation have developed along different lines to deal with the specific needs of different groups of patients. In both England and Scotland, mental capacity legislation has developed with the aim of providing a framework for people with either severe communication difficulties or cognitive problems (intellectual disability, dementia and other organic brain syndromes). In contrast, mental health legislation has developed with the needs of patients with psychiatric disorders – in particular, although not exclusively, psychotic disorders – in mind. Mental health legislation that does not use capacity tests generally applies a ‘status’ approach, whereby a wide range of treatments can be given to the patient on the basis of certain general conditions being met (e.g. the presence of a mental disorder, or the presence of perceived risk to the patient or others).
The use of status approaches has numerous implications. Under mental capacity legislation treatments are only provided in the patient's best interests (with particular attention paid to previously expressed wishes, including advance directives, which have legal weight), whereas under mental health legislation best interests do not have to be considered, although in practice many psychiatrists effectively apply a best interests test (Reference PeayPeay, 2003). Further, the use of a ‘status’ approach means that the patient can be given a range of treatments, even if he or she might have capacity to refuse one or more of these. This has led some to suggest that current status-based approaches are anachronistic and unethical (Reference Szmukler and HollowaySzmukler & Holloway, 1998) and that mental capacity and mental health legislation could be fused (Reference Dawson and SzmuklerDawson & Szmukler, 2006).
A review of emergent case law literature in the USA (Reference Grisso, Applebaum and Hill-FotouhiGrisso et al, 1997) has resulted in a ‘four abilities’ model, namely the ability to express a choice about treatment; the ability to understand information relevant to the treatment decision; the ability to appreciate the significance of that treatment information for one's own situation; and the ability to reason with relevant information so as to engage in a logical process of weighing treatment options. Despite the influential work of the MacArthur Foundation (Grisso & Appelbaum, Reference Grisso and Appelbaum1995a ,Reference Grisso and Appelbaum b ; Reference Grisso, Appelbaum and MulveyGrisso et al, 1995), concern exists regarding the reliability of capacity assessments in individuals with a mental disorder, and the extent to which legislation that uses a capacity test covers the same or different groups of patients as mental health legislation which uses a status approach. Some have pointed to particular areas of perceived difficulty such as the area to appreciation, which may be difficult to operationalise (Reference Saks, Dunn and MarshallSaks et al, 2002; Reference Breden and VollmannBreden & Vollmann, 2004).
Our aim was to make a systematic review of empirical, quantitative studies of mental capacity in order to answer the following three questions:
-
(a) Can the mental capacity of a patient be reliably assessed by two or more raters?
-
(b) What is the proportion of patients with psychiatric disorders in in-patient settings who are judged to lack capacity?
-
(c) What factors are associated with lack of capacity in individuals with psychiatric disorders?
METHOD
We aimed to identify all studies relevant to the aims of this review. Inclusion criteria were that the papers should be in the English language, describe defined populations of patients with psychiatric disorders; report quantitative research (i.e. research that produces numerical summaries of results, as opposed to qualitative research), and describe how the assessment of mental capacity was performed; capacity had to be assessed in relation to a current treatment decision, as opposed to capacity to make advance directives, capacity to participate in research, testamentary capacity or capacity to stand trial. Studies were excluded if they were conducted on children or young people less than 18 years old; exclusively concerned organic psychiatric disorders (dementia or delirium) or intellectual disability; were case reports, commentaries or review articles; or were retrospective case-note reviews.
Search strategy
Relevant research articles were identified from a systematic search of electronic data-bases. These comprised PsycInfo (1967 to July 2006), Medline (1996 to July 2006) and EMBASE (1980 to July 2006). The electronic database search terms were divided into three sets: mental health legislation terms (e.g. Mental Health Act, coercion, patients’ rights), disorder terms (e.g. schizophrenia) and capacity terms (e.g. incompetence, capacity, autonomy). The titles and abstracts of all articles generated were examined on the above inclusion and exclusion criteria. If the reviewer was uncertain as to whether an article fulfilled these criteria, the full paper was requested. The main reviewer was D.O. and his decision to include or exclude studies was reviewed for 100 abstracts by G.O. There were disagreements in 10 papers but further examination indicated none would have been eligible for the final review. The interrater reliability of reviewers was good (κ=0.72). These searches were augmented by personal correspondence with experts on mental capacity research. Experts were identified from the investigators’ prior knowledge and a delegate list from a recent UK seminar which had advertised for researchers working on this area and included several international speakers. The International Journal of Law and Psychiatry was hand-searched from the first to the most recent issue. Finally, the bibliographies of retrieved articles were used to identify further articles.
Data analysis
Articles were categorised and data extracted corresponding to our three main questions. We extracted data from the full-length articles using forms to ensure the process was standardised. D.O. performed the data extraction but all studies were checked independently by M.H. As the papers were heterogeneous a formal meta-analysis was not attempted. Where possible we present median values and interquartile ranges. Where the data provided were sufficient to calculate a kappa value, we did so in order to provide a uniform measure of interrater reliability.
RESULTS
The searches identified 15 490 references, which were scanned by abstract and title. On the basis of the abstract or title, 367 papers were retrieved; 316 did not meet the inclusion criteria, leaving 51 identified from the electronic search, many of which were known to us already. The original review was broader than the aims of the present paper (including mental capacity in individuals with medical illness or dementia) and we finally identified 37 papers relevant to this review (see data supplement to the online version of this paper).
Capacity assessments
The included articles reported many different methods for assessing capacity. Three used vignettes (Reference Grisso and AppelbaumGrisso & Appelbaum, 1995b ; Reference Grisso, Appelbaum and MulveyGrisso et al, 1995; Reference Vellinga, Smit and van LeeuwenVellinga et al, 2004), which present the participant with a hypothetical patient facing a treatment dilemma, about which the participant is then asked a series of questions. Fourteen devised assessments of capacity for a specific procedure, for instance capacity to consent to electroconvulsive therapy, having a blood test or admission to a psychiatric ward (Appelbaum et al, Reference Appelbaum, Mirkin and Bateman1981, Reference Appelbaum, Appelbaum and Grisso1998; Reference Roth, Lidz and MeiselRoth et al, 1982; Reference Norko, Billick and McCarrickNorko et al, 1990; Reference Grisso and AppelbaumGrisso & Appelbaum, 1991; Reference Janofsky, McCarthy and FolsteinJanofsky et al, 1992; Bean et al, Reference Bean, Nishisato and Rector1994, Reference Bean, Nishisato and Rector1996; Reference Poythress, Cascardi and RitterbandPoythress et al, 1996; Reference Tomoda, Yasumiya and SumiyamaTomoda et al, 1997; Reference Paul and OyebodePaul & Oyebode, 1999; Wong et al, Reference Wong, Clare and Holland2000, Reference Wong, Cheung and Chen2005; Reference Vollmann, Bauer and Danker-HopfeVollmann et al, 2003). Sixteen (Reference Hoffman and SrinivasanHoffman & Srinivasan, 1992; Reference Grisso, Applebaum and Hill-FotouhiGrisso et al, 1997; Reference Melamed, Kimchi and ShnitMelamed et al, 1997; Reference Tomoda, Yasumiya and SumiyamaTomoda et al, 1997; Reference Kitamura, Tomoda and TsukadaKitamura et al, 1998; Reference Palmer, Nayak and DunnPalmer et al, 2002; Bellhouse et al, Reference Bellhouse, Holland and Clare2003a ,Reference Bellhouse, Holland and Clare b ; Reference Lapid, Rummans and PooleLapid et al, 2003; Reference Vollmann, Bauer and Danker-HopfeVollmann et al, 2003; Cairns et al, Reference Cairns, Maddock and Buchanan2005a ,Reference Cairns, Maddock and Buchanan b ; Reference Howe, Foister and JenkinsHowe et al, 2005; Reference Jacob, Clare and HollandJacob et al, 2005; Reference Koren, Poyurovsky and SeidmanKoren et al, 2005; Reference Beckett and ChaplinBeckett & Chaplin, 2006) used more flexible assessment methods, designed for use with any treatment decision. Studies generally framed capacity either in binary terms (i.e. present or absent for a specific decision) or as a continuous variable measured on a dimensional scale. A third approach adopted by some (Reference Kitamura, Tomoda and TsukadaKitamura et al, 1998; Reference Paul and OyebodePaul & Oyebode, 1999) was to describe the participant's ability to meet increasingly stringent (binary) tests of capacity. Such studies combined aspects of both the multidimensional and binary approaches.
Reliability of capacity assessments
Seventeen studies reported interrater reliability of competency assessments. These had a median sample size of 56 participants (interquartile range 14–62). These studies could be categorised under three broad themes:
-
(a) binary decisions (capacity present or absent) using the same assessment tool and two or more raters;
-
(b) binary decisions comparing a clinician's assessment with an assessment made by a clinical researcher using a mental capacity tool;
-
(c) score on an individual dimension of capacity measured on an assessment tool.
Where available, we report agreement using Cohen's kappa, which is used as a measure of reliability taking into consideration the level of agreement expected by chance. Kappa takes a value between –1 and 1, and we define kappa scores as follows (Reference Landis and KochLandis & Koch, 1977): <0, poor; 0–0.2, slight; 0.2–0.4, fair; 0.4–0.6, moderate; 0.6–0.8, substantial; 0.8–1, almost perfect.
Reliability of binary assessment of mental capacity using interviews
Five studies (Table 1) assessed mental capacity using two or more raters administering the same structured or semi-structured interview (Reference Roth, Lidz and MeiselRoth et al, 1982; Reference Wong, Clare and HollandWong et al, 2000; Bellhouse et al, Reference Bellhouse, Holland and Clare2003a ,Reference Beckett and Chaplin b ; Reference Cairns, Maddock and BuchananCairns et al, 2005b ). Methods mainly involved raters assessing the same videotaped or transcribed interview performed by a single interviewer, although one paper described the results of two interviews performed by separate interviewers (Reference Cairns, Maddock and BuchananCairns et al, 2005b ). Assessments used a variety of methods: one (Reference Roth, Lidz and MeiselRoth et al, 1982) used a derivative of a 15-item questionnaire (Reference Roth, Meisel and LidzRoth et al, 1977); one used the MacArthur Competence Assessment Tool for Treatment (MacCAT–T) (Reference Cairns, Maddock and BuchananCairns et al, 2005b ) and one used a semi-structured interview adapted from the MacCAT–T (Reference Wong, Clare and HollandWong et al, 2000). Two papers described interrater reliability on two different decisions (admission and treatment) in similar samples (Bellhouse et al, Reference Bellhouse, Holland and Clare2003a ,Reference Bellhouse, Holland and Clare b ), using a checklist derived from English legal definitions. Kappa values ranged from ‘moderate’ to ‘almost perfect’ (median κ=0.81 IQR 0.75–0.82). These results suggest that when a consistent approach is taken to the assessment of mental capacity, two or more raters can make a binary assessment with a high level of agreement.
Table 1 Interrater reliability of mental capacity assessments using same assessment

| Study | κ |
|---|---|
| Bellhouse et al (Reference Bellhouse, Holland and Clare2003a ) | 0.74 |
| Bellhouse et al (Reference Bellhouse, Holland and Clare2003b ) | 0.75 |
| Roth et al (Reference Roth, Lidz and Meisel1982) | 0.81 |
| Cairns et al (Reference Cairns, Maddock and Buchanan2005a ) | 0.82 |
| Wong et al (Reference Wong, Clare and Holland2000) | 0.87 |
Binary decisions comparing a clinician's assessment and that made by a clinical researcher using a mental capacity tool
Six studies (Reference Bean, Nishisato and RectorBean et al, 1996; Reference Tomoda, Yasumiya and SumiyamaTomoda et al, 1997; Reference Vollmann, Bauer and Danker-HopfeVollmann et al, 2003; Reference Vellinga, Smit and van LeeuwenVellinga et al, 2004; Reference Cairns, Maddock and BuchananCairns et al, 2005b ; Reference Beckett and ChaplinBeckett & Chaplin, 2006) assessed agreement between an interviewer performing a structured or semi-structured mental capacity assessment and a clinician's view of the patient's mental capacity. The kappa values ranged from ‘slight’ to ‘substantial’, (median κ=0.45, IQR 0.39–0.66). This suggests that when formal assessments are compared with clinical impressions, agreement is well above chance, but not as high as when two raters are using the same assessment tool. Clinicians universally reported fewer patients lacking mental capacity than did researchers.
Other studies comparing agreement using dimensional scales
Eleven studies addressed interrater agreement on dimensional scales (Reference Norko, Billick and McCarrickNorko et al, 1990; Reference Grisso and AppelbaumGrisso & Appelbaum, 1991; Reference Janofsky, McCarthy and FolsteinJanofsky et al, 1992; Reference Bean, Nishisato and RectorBean et al, 1994; Grisso et al, Reference Grisso, Appelbaum and Mulvey1995, Reference Grisso, Applebaum and Hill-Fotouhi1997; Reference Palmer, Nayak and DunnPalmer et al, 2002; Reference Vollmann, Bauer and Danker-HopfeVollmann et al, 2003; Reference Cairns, Maddock and BuchananCairns et al, 2005b ; Reference Wong, Cheung and ChenWong et al, 2005; Reference Appelbaum and RedlichAppelbaum & Redlich, 2006). These studies are difficult to summarise, since they tend to present correlation coefficients between raters on dimensional scales, or give kappa values for sub-scales of multidimensional scales. Deserving particular mention are the studies of Grisso and Appelbaum on the development of the MacCAT–T and related measures (Grisso et al, Reference Grisso, Appelbaum and Mulvey1995, Reference Grisso, Applebaum and Hill-Fotouhi1997), which present detailed analyses of interrater agreement for each of the dimensions of the MacCAT–T and show that high interrater correlations are the rule. Reliability indices were generally similar for each sub-scale of the MacCAT–T, suggesting that there is no single particularly hard-to-measure dimension (Reference Grisso, Applebaum and Hill-FotouhiGrisso et al, 1997; Reference Palmer, Nayak and DunnPalmer et al, 2002; Reference Vollmann, Bauer and Danker-HopfeVollmann et al, 2003; Reference Cairns, Maddock and BuchananCairns et al, 2005b ).
Frequency of mental incapacity in psychiatric patients
Admission to psychiatric units
We identified five studies that assessed mental capacity in relation to admission to a psychiatric unit (Appelbaum et al, Reference Appelbaum, Mirkin and Bateman1981, Reference Appelbaum, Appelbaum and Grisso1998; Reference Norko, Billick and McCarrickNorko et al, 1990; Reference Poythress, Cascardi and RitterbandPoythress et al, 1996; Reference Bellhouse, Holland and ClareBellhouse et al, 2003a ). One British study (Reference Bellhouse, Holland and ClareBellhouse et al, 2003a ), described a mixed clinical population of patients and found that 67% had mental capacity to make the decision. Three studies (Appelbaum et al, Reference Appelbaum, Mirkin and Bateman1981, Reference Appelbaum, Appelbaum and Grisso1998; Reference Norko, Billick and McCarrickNorko et al, 1990) described capacity to make this decision among voluntary patients admitted to psychiatric hospital. It is difficult to summarise the results of these studies since each presents more than one measure of incapacity; however, approximately 30–50% of participants scored in a range that suggests they were competent to make decisions, a sizeable minority scored in an intermediate range, and as many as 50% (Reference Norko, Billick and McCarrickNorko et al, 1990) had significant impairments of mental capacity despite accepting voluntary admission. One study (Reference Poythress, Cascardi and RitterbandPoythress et al, 1996) described patients who were brought to hospital on a court order (of whom half subsequently accepted informal admission), and found that 55% had an impairment of capacity on a stringent definition and 35% had impairment on a less stringent definition.
Psychiatric in-patients: other treatments
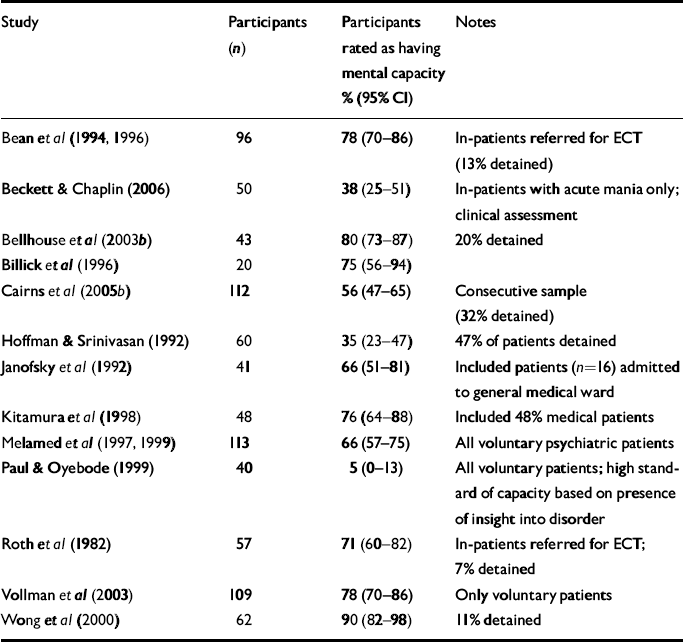
Of the remaining studies of psychiatric patients, most described treatment for diverse interventions (Reference Grisso and AppelbaumGrisso & Appelbaum, 1991; Reference Hoffman and SrinivasanHoffman & Srinivasan, 1992; Reference Janofsky, McCarthy and FolsteinJanofsky et al, 1992; Grisso et al, Reference Grisso, Appelbaum and Mulvey1995, Reference Grisso, Applebaum and Hill-Fotouhi1997; Reference Billick, Naylor and MajeskeBillick et al, 1996; Reference Melamed, Kimchi and ShnitMelamed et al, 1997; Reference Tomoda, Yasumiya and SumiyamaTomoda et al, 1997; Reference Kitamura, Tomoda and TsukadaKitamura et al, 1998; Reference Melamed, Kimchi and ShnitMelamed et al, 1999; Reference Bellhouse, Holland and ClareBellhouse et al, 2003b ; Reference Vollmann, Bauer and Danker-HopfeVollmann et al, 2003; Reference Vellinga, Smit and van LeeuwenVellinga et al, 2004; Reference Cairns, Maddock and BuchananCairns et al, 2005b ; Reference Jacob, Clare and HollandJacob et al, 2005; Reference Beckett and ChaplinBeckett & Chaplin, 2006), whereas a few focused on either antipsychotic medication (Reference Paul and OyebodePaul & Oyebode, 1999; Reference Wong, Cheung and ChenWong et al, 2005) or electroconvulsive therapy (Reference Roth, Lidz and MeiselRoth et al, 1982; Reference Bean, Nishisato and RectorBean et al, 1996). In some studies the population was well defined, and a true cross-sectional study of consecutive patients had been performed. In others the population under study was much less well characterised, and convenience samples were used. For those 12 studies that provided a binary (present/absent) rating of mental capacity in the various psychiatric in-patient groups, estimates ranged from 10% to 95% of the participants lacking capacity (Table 2). However, all but two studies estimated that less than half of psychiatric in-patients lacked capacity, and the median value was 29% (IQR 22–44).
Table 2 Frequency of mental capacity among psychiatric in-patients
| Study | Participants (n) | Participants rated as having mental capacity % (95% CI) | Notes |
|---|---|---|---|
| Bean et al (Reference Bean, Nishisato and Rector1994, Reference Bean, Nishisato and Rector1996) | 96 | 78 (70-86) | In-patients referred for ECT (13% detained) |
| Beckett & Chaplin (Reference Beckett and Chaplin2006) | 50 | 38 (25-51) | In-patients with acute mania only; clinical assessment |
| Bellhouse et al (Reference Bellhouse, Holland and Clare2003b ) | 43 | 80 (73-87) | 20% detained |
| Billick et al (Reference Billick, Naylor and Majeske1996) | 20 | 75 (56-94) | |
| Cairns et al (Reference Cairns, Maddock and Buchanan2005b ) | 112 | 56 (47-65) | Consecutive sample (32% detained) |
| Hoffman & Srinivasan (Reference Hoffman and Srinivasan1992) | 60 | 35 (23-47) | 47% of patients detained |
| Janofsky et al (Reference Janofsky, McCarthy and Folstein1992) | 41 | 66 (51-81) | Included patients (n=16) admitted to general medical ward |
| Kitamura et al (Reference Kitamura, Tomoda and Tsukada1998) | 48 | 76 (64-88) | Included 48% medical patients |
| Melamed et al (Reference Melamed, Kimchi and Shnit1997, Reference Melamed, Kimchi and Shnit1999) | 113 | 66 (57-75) | All voluntary psychiatric patients |
| Paul & Oyebode (Reference Paul and Oyebode1999) | 40 | 5 (0-13) | All voluntary patients; high standard of capacity based on presence of insight into disorder |
| Roth et al (Reference Roth, Lidz and Meisel1982) | 57 | 71 (60-82) | In-patients referred for ECT; 7% detained |
| Vollman et al (2003) | 109 | 78 (70-86) | Only voluntary patients |
| Wong et al (Reference Wong, Clare and Holland2000) | 62 | 90 (82-98) | 11% detained |
Specific psychiatric diagnoses
Four studies (Reference Grisso and AppelbaumGrisso & Appelbaum, 1995c ; Reference Grisso, Applebaum and Hill-FotouhiGrisso et al, 1997; Reference Vollmann, Bauer and Danker-HopfeVollmann et al, 2003; Reference Appelbaum and RedlichAppelbaum & Redlich, 2006) presented the results of capacity assessments for patients with psychiatric diagnoses separately. Three used the MacCAT–T, and compared participants with schizophrenia or depression, all finding that impairments in mental capacity were much more common in the schizophrenia group. The MacArthur study (Reference Grisso, Applebaum and Hill-FotouhiGrisso et al, 1997) found that 52% of patients with schizophrenia had impaired capacity, as opposed to 24% of those with depression. This study gave a further detailed breakdown of areas of difficulty, indicating that when individuals with schizophrenia had difficulties in decision-making, their appreciation, understanding and reasoning could all be affected. In contrast, decision-making difficulties in depression were mainly related to difficulties in appreciation. The third study (Reference Vollmann, Bauer and Danker-HopfeVollmann et al, 2003) reported a remarkably consistent result: 53% of in-patients with schizophrenia were judged to lack capacity, as opposed to 20% of those with depression.
Associations of mental incapacity in psychiatric patients
Twenty-seven studies described associations of mental incapacity in psychiatric in-patients. These papers presented a range of variables, including socio-demographic factors (such as age, gender, educational level and ethnicity) as well as patient variables (such as cognitive abilities and whether the person was accepting or refusing treatment).
Socio-demographic variables
Fourteen studies (Appelbaum et al, Reference Appelbaum, Mirkin and Bateman1981, Reference Appelbaum, Appelbaum and Grisso1998; Reference Norko, Billick and McCarrickNorko et al, 1990; Reference Hoffman and SrinivasanHoffman & Srinivasan, 1992; Reference Bean, Nishisato and RectorBean et al, 1996; Reference Billick, Naylor and MajeskeBillick et al, 1996; Reference Grisso, Applebaum and Hill-FotouhiGrisso et al, 1997; Reference Melamed, Kimchi and ShnitMelamed et al, 1997; Reference Paul and OyebodePaul & Oyebode, 1999; Reference Palmer, Dunn and AppelbaumPalmer et al, 2004; Reference Cairns, Maddock and BuchananCairns et al, 2005a ; Reference Jacob, Clare and HollandJacob et al, 2005; Reference Wong, Cheung and ChenWong et al, 2005; Reference Beckett and ChaplinBeckett & Chaplin, 2006) presented results on gender, and none of these indicated an association. Thirteen studies presented results on age, with ten (Reference Appelbaum, Mirkin and BatemanAppelbaum et al, 1981; Reference Billick, Naylor and MajeskeBillick et al, 1996; Reference Grisso, Applebaum and Hill-FotouhiGrisso et al, 1997; Reference Melamed, Kimchi and ShnitMelamed et al, 1997; Reference Palmer, Dunn and AppelbaumPalmer et al, 2004; Reference Appelbaum and RedlichAppelbaum & Redlich, 2006; Reference Beckett and ChaplinBeckett & Chaplin, 2006; Reference Cairns, Maddock and BuchananCairns et al, 2005a ; Reference Jacob, Clare and HollandJacob et al, 2005; Reference Wong, Cheung and ChenWong et al, 2005) describing no association and three (Reference Roth, Lidz and MeiselRoth et al, 1982; Reference Norko, Billick and McCarrickNorko et al, 1990; Reference Appelbaum, Appelbaum and GrissoAppelbaum et al, 1998) describing an association with increasing age and mental incapacity. Results on socio-economic status were scarce, but of the four studies presenting associations, two described an association between mental incapacity and lower socio-economic status (Reference Grisso and AppelbaumGrisso & Appelbaum, 1995b ; Reference Roth, Lidz and MeiselRoth et al, 1982), and two described no such association (Reference Billick, Naylor and MajeskeBillick et al, 1996; Reference Grisso, Applebaum and Hill-FotouhiGrisso et al, 1997). For educational attainment, two studies showed an association between incapacity and lower educational status (Reference Roth, Lidz and MeiselRoth et al, 1982; Reference Wong, Cheung and ChenWong et al, 2005) whereas the remaining eight showed no association (Reference Grisso and AppelbaumGrisso & Appelbaum, 1991; Reference Billick, Naylor and MajeskeBillick et al, 1996; Reference Kitamura, Tomoda and TsukadaKitamura et al, 1998; Reference Paul and OyebodePaul & Oyebode, 1999; Reference Palmer, Dunn and AppelbaumPalmer et al, 2004; Reference Cairns, Maddock and BuchananCairns et al, 2005a ; Reference Appelbaum and RedlichAppelbaum & Redlich, 2006; Reference Beckett and ChaplinBeckett & Chaplin, 2006). Seven studies assessed ethnic group, with six finding no association (Reference Norko, Billick and McCarrickNorko et al, 1990; Reference Billick, Naylor and MajeskeBillick et al, 1996; Reference Grisso, Applebaum and Hill-FotouhiGrisso et al, 1997; Reference Appelbaum, Appelbaum and GrissoAppelbaum et al, 1998; Reference Paul and OyebodePaul & Oyebode, 1999; Reference Jacob, Clare and HollandJacob et al, 2005). The one exception (Reference Cairns, Maddock and BuchananCairns et al, 2005a ) showed an association between Black and minority ethnic group and mental incapacity, but the Black and minority ethnic group consisted of more individuals with psychotic illness and once this was controlled for the effect of ethnicity was lost.
Clinical variables
The other main variables to have been examined in the psychiatric studies were broadly clinical. When groups of patients with mixed diagnoses were examined, it was almost universally shown that capacity was more often impaired in individuals with psychotic illness than in individuals with non-psychotic illness (usually depressive disorder) (Reference Grisso and AppelbaumGrisso & Appelbaum, 1995c ; Reference Bean, Nishisato and RectorBean et al, 1996; Reference Poythress, Cascardi and RitterbandPoythress et al, 1996; Reference Bellhouse, Holland and ClareBellhouse et al, 2003a ; Reference Vollmann, Bauer and Danker-HopfeVollmann et al, 2003; Reference Appelbaum and RedlichAppelbaum & Redlich, 2006). Most studies (Reference Grisso and AppelbaumGrisso & Appelbaum, 1995b ; Reference Billick, Naylor and MajeskeBillick et al, 1996; Reference Grisso, Applebaum and Hill-FotouhiGrisso et al, 1997; Reference Cairns, Maddock and BuchananCairns et al, 2005a ; Reference Howe, Foister and JenkinsHowe et al, 2005; Reference Jacob, Clare and HollandJacob et al, 2005; Reference Wong, Cheung and ChenWong et al, 2005; Reference Beckett and ChaplinBeckett & Chaplin, 2006) although not all (Reference Paul and OyebodePaul & Oyebode, 1999) – showed that severity of psychopathology was also associated with loss of capacity. Perhaps unsurprisingly, individuals who refused treatment were more often considered to be lacking capacity compared with those who accepted it (Reference Roth, Lidz and MeiselRoth et al, 1982; Reference Bean, Nishisato and RectorBean et al, 1996; Reference Melamed, Kimchi and ShnitMelamed et al, 1997; Reference Jacob, Clare and HollandJacob et al, 2005; Reference Wong, Cheung and ChenWong et al, 2005) and a corresponding feature is that patients admitted involuntarily were more likely to lack capacity (Reference Hoffman and SrinivasanHoffman & Srinivasan, 1992; Reference Bean, Nishisato and RectorBean et al, 1996; Reference Poythress, Cascardi and RitterbandPoythress et al, 1996; Reference Melamed, Kimchi and ShnitMelamed et al, 1997; Reference Appelbaum, Appelbaum and GrissoAppelbaum et al, 1998; Reference Cairns, Maddock and BuchananCairns et al, 2005a ). Few studies of psychiatric patients have assessed the cognitive underpinnings of mental incapacity, but one intriguing study (Reference Koren, Poyurovsky and SeidmanKoren et al, 2005) showed that although problems with capacity were weakly related to performance on the Wisconsin Card Sorting Test (a measure of executive function), performance on a ‘metacognitive’ scoring system was much more closely related. The meta-cognitive scoring system emphasised the level of confidence patients had about their performance, and the degree to which this was at odds with actual performance was predictive of poor performance on the MacCAT–T.
DISCUSSION
We identified a number of studies that have used a systematic approach to measure mental capacity in individuals with psychiatric disorders. Although the methods used to measure capacity varied considerably, we have been able to address the three aims of this review. Our first aim was to determine whether mental capacity could be assessed in a reliable manner. The answer to this question depends upon the study design. Studies that used a standardised assessment reported very high interrater reliabilities, with a median kappa of 0.81. Despite capacity being a complex, value-laden, multidimensional construct, this finding suggests that it can be assessed with greater reliability than cardiologists interpreting exercise electrocardiograms, radiologists interpreting mammograms or haematologists reading peripheral blood films (Reference Sackett, Haynes and GuyattSackett et al, 1991). When interrater reliability of single dimensions of capacity such as understanding is measured, results again suggest that these measures are highly reproducible. It is noteworthy that even dimensions such as reasoning and appreciation, which are hard to operationalise, are assessed with good interrater reliability. However, interviewers using standardised assessments agreed much less frequently with the clinicians who had been treating the study participants, and although this difference may be artefactual (under certain circumstances kappa values may be low despite good agreement) we think that it is probable that reliability is generally lower when a researcher's assessment is pitted against that of a clinician. In general, clinicians were much less likely to judge a patient to lack capacity, and it may be that if a patient is prepared to accept the treatment proposed the issue of incapacity does not arise – the clinician presumes it is present. Clinicians might have a tendency to equate treatment refusal with incapacity and treatment acceptance with capacity. Alternatively, it might be that clinicians lack training or the time in which to perform careful assessments. Finally, although there is no gold standard criterion of capacity, it may be that formal assessments, although reliable, lack specificity and tend to ‘overdiagnose’ incapacity compared with the clinicians’ assessments.
The second question related to the frequency of incapacity to make key treatment decisions among patients with psychiatric disorders. Taking the median values as an approximate estimate, the results of the reviewed studies indicate that of in-patients with psychiatric disorders, a sizeable proportion – usually the majority – are capable of making treatment decisions. Indeed, the frequency of incapacity in psychiatric in-patients found in the reviewed studies did not differ greatly from that in general hospital in-patients (Reference Raymont, Bingley and BuchananRaymont et al, 2004). The consistency of estimates of incapacity in psychiatric in-patients is striking, given the diverse nature of the populations studied. Half the studies estimated the frequency of participants’ lack of capacity to be within the range 22–44%. Similarly, the two studies to report on rates of incapacity in schizophrenia and depression found almost exactly the same rates, despite one being conducted in the USA and the other in Germany, where differences in healthcare systems might have led to differences in patient characteristics. This suggests that although diverse measures of mental capacity have been used, they are capable of making fairly consistent estimates.
The frequency of incapacity in voluntary patients when consenting to admission was remarkably high. This leads to a potential dilemma, as individuals lacking capacity may acquiesce to admission, but may lack protections that an admission under a legal framework would afford. Such patients may, to some extent, feel coerced into accepting admission, presumably since they felt that if they did not agree to an admission they would be detained anyway. Finally, the British studies of mental capacity (Reference Bellhouse, Holland and ClareBellhouse et al, 2003a ; Reference Cairns, Maddock and BuchananCairns et al, 2005a ) in those detained under the Mental Health Act 1983 indicated that a sizeable proportion have capacity to accept or refuse admission to hospital. Further work needs to be done to understand the implications of capacity-based mental health legislation for these individuals.
Mental capacity is not associated with any individual socio-demographic variable apart from advancing age. It is unclear why this should be, but it may be driven by cognitive decline or increased negative symptoms in older patients with psychotic illness. Given that mental capacity assessments are value-laden, it is reassuring that neither gender nor ethnic group has an effect; associations with educational level and social class are inconsistent. The clinical and legal variables associated with mental incapacity in the psychiatric groups should come as no surprise – psychosis, illness severity, involuntary admission and treatment refusal are all consistently reported as risk factors.
Limitations of our review
The most serious problem of a summary of capacity is that it is by nature a functional definition and to describe the frequency in a specific treatment setting is to ignore the fact that patients may have capacity for some decisions and not for others. It is likely that the variation in the results presented here stems from the heterogeneity of the patient groups, the range of capacity assessment tools used, the different legal standards for capacity assessment and the differences in treatment choices presented to participants. Furthermore, frequency of capacity in some of the primary research was not the main aim of the study and was reported as an incidental finding. Studies were often small, and many were not truly cross-sectional in that they did not define a clear population and sample from it, but instead used convenience samples. Participation rates were frequently unreported, and when they were, were often low. Little information was given about non-participants to allow inferences to be made about non-participation bias.
The primary studies are – with some notable exceptions – particularly weak in their reporting of data on associations. Similar difficulties have been observed in other systematic reviews of descriptive studies (Reference Altman, Egger, Davey Smith and AltmanAltman, 2000). We suspect that many of the studies emphasise ‘positive’ associations and fail to report ‘negative’ ones. This might lead to a bias, which would mean that conclusions would be more conservative than possibly indicated here. Many studies are statistically under-powered and report negative findings without any consideration of the possibility that a genuine difference was not detected because the sample size was too small. Nevertheless, the generally consistent negative findings in relation to demographic variables probably do reflect a true lack of association.
There are potential limitations of the review methods presented here. This review represents a novel use of systematic review methods, akin to recent developments in summarising information in diagnostics (Reference StrausStraus, 2006). There is a less well-trodden methodology for such reviews compared with reviews of randomised controlled trials. We excluded non-English language papers, and despite considerable effort might have missed relevant eligible papers owing to the diverse language used to describe mental capacity. We did not apply a pre-defined assessment of quality, as we reasoned that the primary studies were too heterogeneous in their designs to do this in a meaningful way.
Implications
A number of implications arise from this body of research. First, we have found that most studies report that most psychiatric in-patients are capable of making key treatment decisions; given that as many as a third of general medical patients lack mental capacity (Reference Raymont, Bingley and BuchananRaymont et al, 2004), this should remind clinicians, policy makers and the general public that patients with psychiatric disorders are not intrinsically different and this may be important in campaigns against stigma. Equally important is the finding that many in-patients with psychiatric disorder lack capacity and there is a tendency for clinicians to underestimate this (especially when patients are accepting treatment) relative to research estimates. This underestimate may have the effect of underestimating clinical and social need. Second, studies are consistent in showing the reliability of mental capacity assessments, and these measurements are correlated with indicators of clinical severity but not with demographic differences. This indicates that mental capacity can be reliably measured, and also that it has some criterion validity. These characteristics mean that it can, we believe, be researched in a useful manner. Third, there is little information on the points where mental capacity and mental health legislation do not overlap. The information from informal admissions suggests that a high proportion of patients may lack capacity – the question then is whether their treatment in an in-patient psychiatric setting is acceptable. A recent ruling by the European Court (HL v. United Kingdom, 2005) that the informal hospitalisation of an incompetent patient with intellectual disability was unlawful as he was deprived of his liberty in the absence of required safe-guards (the Bournewood case) suggests that mental health providers – in Europe at least – will have to consider much more carefully the legal structures used in healthcare settings which may be judged to deprive individuals of liberty. Much less information exists on patients who have been detained under mental health legislation but are thought to retain capacity; more information is required on the nature of this group, the complexities of capacity assessment within it and the consequences of overriding capable decisions regarding treatment.
Acknowledgements
The study was funded by the Department of Health. The authors are grateful to Professor Genevra Richardson and Professor George Szmukler for their comments on an earlier draft.







eLetters
No eLetters have been published for this article.