INTRODUCTION
Diabetes mellitus is a complex and progressive metabolic disorder that is characterised by persistent hyperglycaemia caused by insulin deficiency and/or insulin resistance. It has been estimated that in 2003 nearly 190 million people worldwide had diabetes. By 2025, that figure is predicted to increase by 72% to 324 million. Studies in the USA have found rates of known diabetes in the general population of between 1.2% and 6.3% depending upon age and ethnicity. In the UK, 1.4 million people are known to have diabetes; another 1 million are thought to have undiagnosed diabetes. The prevalence of impaired glucose tolerance, a pre-diabetic state of impaired glucose metabolism, may be 2–3 times higher than that of diabetes.
Type 2 diabetes, the most common form of diabetes, results from an interaction between a genetic predisposition and environmental factors such as a poor diet and a sedentary lifestyle. Early detection and treatment of type 2 diabetes is essential to prevent the long-term complications. It is thought that the pathological process that leads to the development of type 2 diabetes starts on average 10–15 years before diagnosis. Since type 2 diabetes is generally asymptomatic, the emphasis must be on effective screening programmes, especially in high-risk groups.
The interaction between diabetes and schizophrenia is complex. Many people with schizophrenia have multiple risk factors for type 2 diabetes, such as a family history of diabetes, higher-risk ethnic origin, obesity, sedentary lifestyle and smoking. It has also been suggested that the condition itself might be an additional risk factor for diabetes, as may antipsychotic treatment. Consequently, people with schizophrenia may represent an independent high-risk group for diabetes.
Much conflicting data have been published on the relationship between schizophrenia, antipsychotics and diabetes, resulting in a lack of consensus on the issue. Little has been done to propose a pragmatic pathway for managing diabetes risks in people with mental illness. For these reasons, an international group of experts in psychiatry and diabetic medicine was convened in order to review the evidence to date and answer the following questions.
-
(a) What is the effect of schizophrenia on glucose metabolism?
-
(b) What is the effect of antipsychotics on glucose metabolism?
-
(c) How should diabetes risks be managed in people with schizophrenia?
-
(d) What research questions need to be addressed?
This document summarises the group's collective view on these issues. It is hoped that by clarifying some of the controversial areas, the quality of care available to people with schizophrenia will be improved in the future.
WHAT IS THE EFFECT OF SCHIZOPHRENIA ON GLUCOSE METABOLISM?
The prevalence of type 2 diabetes in people with schizophrenia can be 2–4 times higher than in the general population. The precise prevalence can be reasonably estimated to be approximately 15–18%. The prevalence of impaired glucose tolerance in people with schizophrenia may be as high as 30%, depending upon age. A high prevalence of diabetes and impaired glucose tolerance is also seen in other severe mental illnesses such as bipolar disorder. The prevalence of type 2 diabetes in people with bipolar disorder can be 2–3 times that in the general population.
As many as two-thirds of cases of diabetes and impaired glucose tolerance may currently go unidentified in people with schizophrenia, as screening is not undertaken routinely.
Type 2 diabetes and impaired glucose tolerance may be present in people with schizophrenia prior to their exposure to any antipsychotic drug treatment. An association between severe mental illnesses and impaired glucose metabolism was identified many decades before the introduction of antipsychotic medications. In one of the most recent studies, impaired fasting glycaemia was reported in young, first-episode, drug-naïve schizophrenia patients.
The relationship between schizophrenia and diabetes is not fully understood. An association between the two conditions was recognised in the pre-antipsychotic era. Schizophrenia and diabetes may share a common aetiology and/or pathogenic mechanisms. Many people with schizophrenia have a diet high in saturated fat and sugar and low in fibre (which is known to precipitate many of the conditions associated with the metabolic syndrome), smoke and take little exercise. They are also up to three times more likely to have a family history of type 2 diabetes than the general population. It seems likely therefore that type 2 diabetes develops as a result of environmental and lifestyle factors in people who are genetically predisposed to disease.
There is cumulative evidence that schizophrenia is an independent risk factor for diabetes.
WHAT IS THE EFFECT OF ANTIPSYCHOTICS ON GLUCOSE METABOLISM?
Antipsychotic treatment is essential for the well-being of people with schizophrenia. Effectiveness should be the most important consideration when selecting antipsychotic treatment.
Idiosyncratic cases of diabetic ketoacidosis have been reported with both typical and atypical antipsychotics. Case reports can be found even with the latest atypical agents in spite of their relatively small usage.
All atypical antipsychotics have been associated with impaired glucose metabolism. Published evidence to date shows no convincing difference between agents, and impaired glucose metabolism is now considered to be a class effect.
Atypical antipsychotics, especially clozapine, may have a stronger association with impaired glucose metabolism than typical antipsychotics. However, this difference may be due to the fact that patients taking atypical drugs are screened much more frequently than patients taking typical antipsychotics.
Other factors such as severe mental illness and associated lifestyle issues may be contributing more to the high prevalence of impaired glucose metabolism seen in people with schizophrenia than drug treatment.
The mechanisms by which antipsychotics may influence glucose metabolism are unknown. In published studies, albeit short-term ones, no association has been found between treatment-related weight gain and diabetes. However, since obesity is a risk factor for diabetes, weight management and a healthy lifestyle should be encouraged in all patients at risk of developing diabetes, including those with schizophrenia.
The available evidence supports an association between antipsychotics and impaired glucose metabolism but does not establish causality. Most studies to date have been retrospective, and these have a number of limitations, including detection and selection bias and an inability to control for confounding risk factors. Prospective, randomised trials allow more accurate between-treatment comparisons. Long-term prospective studies need to be undertaken in order to provide definitive answers.
HOW SHOULD DIABETES RISKS BE MANAGED IN PEOPLE WITH SCHIZOPHRENIA?
Health care professionals should be aware that people with severe mental illness such as schizophrenia are a high-risk group for developing diabetes.
Timely screening and effective management of risk factors are vital for the early detection of impaired glucose tolerance and diabetes and for the reduction of disease progression and development of complications.
Mental health teams should take on some responsibility for managing general health issues in their patients, e.g. providing education about healthy living, ensuring that screening for diabetes is done and that other services are involved when necessary.
Mental health teams should be aware of local guidelines for the screening and management of diabetes. If screening programmes do not exist, they should consider establishing their own programmes in consultation with primary care teams and diabetes specialist services.
Well-defined responsibilities and good communication between mental health teams, primary care teams and diabetes specialist services will be critical to reducing the burden of diabetes in people with schizophrenia.
Proposed pragmatic pathways for managing diabetes risks in people with schizophrenia
-
(a) Drug-naïve patients starting an antipsychotic treatment OR drug-treated patients switched to another antipsychotic:
-
(i) baseline random (or fasting) plasma glucose and glycosylated haemoglobin (HbA1c) test;
-
(ii) repeat 4 months after initiating or changing an antipsychotic;
-
(iii) if normal, repeat random (or fasting) glucose annually;
-
(iv) if abnormal, refer to pathway (d) below;
-
(v) communicate results between services.
-
-
(b) Non-diabetic patients established on medication:
-
(i) ask about symptoms of hyperglycaemia;
-
(ii) test random (or fasting) plasma glucose levels annually;
-
(iii) communicate results between services.
-
-
(c) Diabetic patients established on antipsychotic medication:
-
(i) general practitioner (GP) or diabetes specialist services to continue to manage the diabetes;
-
(ii) mental health teams to continue to manage the mental illness;
-
(iii) patient to continue with home blood glucose monitoring as usual;
-
(iv) communicate any issues between services.
-
-
(d) Patients whose test results suggest impaired glucose tolerance or diabetes:
-
(i) refer the patient to GP/diabetes specialist services for proper diagnosis;
-
(ii) if diagnosis is positive, GP/diabetes specialist services to coordinate the future management of diabetes/impaired glucose tolerance and to make sure that the patient is part of their diabetes follow-up service, including the annual review process;
-
(iii) a multidisciplinary clinical decision may be required regarding the future use of an antipsychotic; a change in antipsychotic medication will usually be unnecessary.
-
WHAT RESEARCH QUESTIONS NEED TO BE ADDRESSED?
Prospective, active comparator studies with a long-term follow-up are needed to elucidate the relationship between antipsychotics and diabetes.
In particular, long-term prospective comparator studies in drug-naïve patients with schizophrenia would help to establish the metabolic status of patients prior to starting antipsychotics and oversee any changes that time, lifestyle and drug treatment would have on the emergence of various cardiovascular factors.
Other studies suggested by the group included the following.
-
(a) Studies of diabetes incidence and prevalence comparing African Americans with native Africans, Chinese Americans with native Chinese, etc. Existing databases could be used in order to minimise the amount of de novo research required in this area. These studies would lead to better understanding of the impact of ethnicity v. lifestyle.
-
(b) Studies of lifestyle interventions in schizophrenia: these would help to establish which interventions are most effective in preventing diabetes and/or improving glucose control.
It was recommended that a process should be in place to determine the effectiveness and impact of any diabetes management guidelines for patients with schizophrenia or other mental health conditions.
APPENDIX 1
Common symptoms of diabetes
-
• Polyuria
-
• Polydipsia
-
• Nocturia
-
• Unexplained weight loss
-
• Loss of energy
-
• Recurrent infections, e.g. candidiasis (‘thrush’)
-
• Blurred vision.
APPENDIX 2
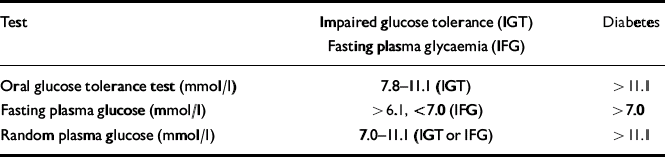
Making a diagnosis of diabetes
| Test | Impaired glucose tolerance (IGT) Fasting plasma glycaemia (IFG) | Diabetes |
|---|---|---|
| Oral glucose tolerance test (mmol/l) | 7.8-11.1 (IGT) | >11.1 |
| Fasting plasma glucose (mmol/l) | >6.1, <7.0 (IFG) | >7.0 |
| Random plasma glucose (mmol/l) | 7.0-11.1 (IGT or IFG) | >11.1 |
APPENDIX 3
Simple lifestyle adjustments to decrease the risk of diabetes
-
• Decrease calorific and fat content of food and increase fibre intake
-
• Increase intake of fruit and vegetables
-
• Eat complex rather than simple carbohydrates, e.g. wholewheat bread rather than refined white bread
-
• Avoid sugary drinks
-
• Exercise for at least 10–15 min per day.

| Chairman | |
| Professor Ted Dinan | Professor of Psychopharmacology, Cork University Hospital, Cork, Ireland |
| Speakers | |
| Dr Richard Holt | Senior Lecturer in Endocrinology and Metabolism, University of Southampton, Southampton; UK Vice Chair of the Science and Research Group of the Professional Advisory Council, Diabetes UK |
| Professor Dora Kohen | Professor of Clinical Psychiatry/Consultant Psychiatrist, Lancashire Postgraduate School of Medicine, Leigh, UK |
| Dr Jogin Thakore | Senior Lecturer/Consultant Psychiatrist, St Vincent's Hospital, Dublin, Ireland |
| Dr Peter Haddad | Consultant Psychiatrist/Honorary Lecturer, Salford, UK |
| Dr Robert Baker | Associate Medical Director, Lilly US Neuroscience, Indianapolis, USA |
| Professor Malcolm Peet | Consultant Psychiatrist, Rotherham Mental Health Services, Swallownest, UK |
| Dr Stephen Gough | Reader in Diabetic Medicine, University of Birmingham, Birmingham Heartlands Hospital, UK |
| Discussants | |
| Professor Brian Leonard | Emeritus Professor of Psychiatry, National University of Ireland, Galway, Ireland; President-elect CINP (Collegium Internationale Neuro-Psychopharmacologicum) |
| Professor Jack McIntyre | Vice-President for Behavioural Health and Chair, Department of Psychiatry and Behavioural Health, Unity Health System, Rochester, NY, USA; Past President of the American Psychiatric Association |
| Carol Paton | Chief Pharmacist, Oxleas National Health Service Trust, Bexley, UK |
| Professor Robert Peveler | Professor of Psychiatry, University of Southampton, Southampton, UK |






eLetters
No eLetters have been published for this article.