Obsessive–compulsive disorder (OCD) commonly arises in childhood and adolescence (Reference Heyman, Fombonne and SimmonsHeyman et al, 2001). Young people with the disorder perceive their symptoms as embarrassing and do not disclose them unless specifically asked. Therefore, OCD in this age group often remains unrecognised and untreated. The associated distress and developmental handicap are avoidable as effective treatments are available, namely cognitive–behavioural therapy with or without serotonin reuptake inhibiting medication (Reference Heyman, Mataix-Cols and FinebergHeyman et al, 2006). There is evidence that early detection and intervention improve outcome (Reference Stewart, Geller and JenikeStewart et al, 2004). The National Institute for Health and Clinical Excellence (NICE) guidance on the assessment and treatment of OCD recommends routine screening of young people at risk in general practice or other settings where they may present for help (National Collaborating Centre for Mental Health, 2005). Such screening requires short, easy-to-use and widely available measures. We report on the development, validation and dissemination of such a self-report tool, the Short OCD Screener (SOCS).
METHOD
The questionnaire was developed from the five most discriminant items of the 44-item child version of the Leyton Obsessional Inventory (Reference Berg, Rapoport and FlamentBerg et al, 1986). These items enquire about common symptoms including checking, touching, cleanliness/washing, repeating and exactness. Two further questions were designed to gauge the associated impairment and resistance. A three-option response format (‘no’, ‘a bit’, or ‘a lot’) was used throughout. A SOCS score is calculated by summing the scores for all seven items (‘no’, 0, ‘a bit’, 1; ‘a lot’, 2).
We administered the SOCS to 127 individuals aged 11–15 years consecutively referred to the Clinic for Obsessive–Compulsive and Related Disorders at the Michael Rutter Centre, Maudsley Hospital, London. Of the 127 referred individuals, 114 met ICD–10 diagnostic criteria for OCD (World Health Organization, 1992), established by a comprehensive psychiatric assessment and the structured Child Yale–Brown Obsessive–Compulsive Scale (CY–BOCS; Reference Scahill, Riddle and McSwiggin-HardinScahill et al, 1997). The remaining 13 individuals received other ICD–10 diagnoses, including anxiety disorder (n=7), conduct disorder (n=4), hyperactivity (n=3) and depression (n=3). All participants completed the SOCS prior to clinical assessment.
We further administered the SOCS to a community sample of 203 children aged 11–15 years as a part of the British nationwide pilot survey of child and adolescent mental health (Reference GoodmanGoodman, 1999). Diagnoses of ICD–10 psychiatric disorders in the community sample were established using the Development and Well-Being Assessment (Reference Goodman, Ford and RichardsGoodman et al, 2000). Two of the individuals in this sample met diagnostic criteria for OCD and 20 had other ICD–10 diagnoses including conduct disorder (n=12), anxiety disorders (n=6), hyperkinetic disorder (n=3) and depression (n=2). The clinic and community samples were combined to obtain a group of 116 cases of OCD, including 72 boys and 44 girls with mean age 13.3 years (s.d.=1.3, range 11–15), mean duration of illness 3.3 years (s.d.=2.2, range 0.5–10) and mean total CY–BOCS impairment score 23.1 (s.d.= 5.0, range 15–40).
Three overlapping control groups were used. The first comparison group comprised the 181 individuals without any psychiatric diagnosis from the community sample, constituting the ‘pure healthy control’ group (mean age 13.0 years, s.d.= 1.4; 98 boys). This group was used to obtain estimates of how well the SOCS can discriminate OCD cases from healthy individuals. The second control group was also drawn from the community sample and consisted of healthy individuals and those with non-OCD psychiatric diagnoses, forming a ‘mixed community control’ group of 201 with a proportion of individuals with other psychiatric diagnoses representative of the general population (mean age 13.0 years, s.d.=1.4; 111 boys). This group was used to provide more realistic estimates of discrimination in a community setting. The third control group is a ‘psychiatric control’ group, included 33 individuals with a psychiatric diagnosis other than OCD from both the community and the clinic samples (mean age 13.1 years, s.d.=1.3; 20 boys); this group was used to explore whether the SOCS could discriminate OCD from other psychiatric disorders in clinical samples.
We used receiver operating characteristics analysis to establish optimal cut-offs for screening (Reference FombonneFombonne, 1991). The 95% confidence intervals for proportions were calculated using the efficient score method (Reference NewcombeNewcombe, 1998).
RESULTS
The mean total SOCS scores were 9.7 (s.d.=2.2) for the OCD group, 3.0 (s.d.=2.3) for the healthy control group, 3.3 (s.d.=2.5) for the mixed community control group and 5.8 (s.d.=2.8) for the psychiatric control group. Thus an average OCD case scored 3 standard deviations above the healthy population mean and 1.5 standard deviations above the mean of psychiatric controls.
Internal consistency of the SOCS was good, with Cronbach's α=0.85. Item-total correlations were all above 0.4. A principal axis factor analysis clearly indicated unidimensionality dimensionality with a single latent factor explaining 53% of variance and all item loadings >0.4.
A SOCS score of 6 or more differentiated OCD cases with a sensitivity of 0.97 (95% CI 0.91–0.99). The specificity was 0.88 (95% CI 0.82–0.92) for differentiation from the healthy control group, 0.84 (95% CI 0.78–0.89) for the mixed community control group, and 0.52 (95% CI 0.34–0.69) for the psychiatric control group. Thus the screener identifies almost all true cases of OCD, approximately one in ten healthy adolescents and one in two of those with other psychiatric disorders (Table 1). In the composite sample of OCD cases and mixed community controls, the positive predictive value was 0.78 (95% CI 0.70–0.84) and the negative predictive value was 0.98 (95% CI 0.94–0.99).
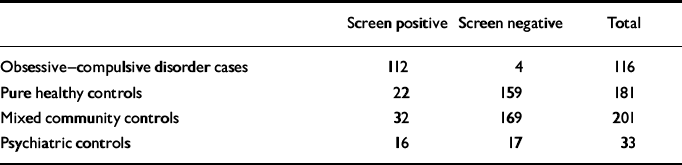
Table 1 Numbers of true and false positives/negatives using the cut-off score of 6 or more on the Short OCD Screener
| Screen positive | Screen negative | Total | |
|---|---|---|---|
| Obsessive—compulsive disorder cases | 112 | 4 | 116 |
| Pure healthy controls | 22 | 159 | 181 |
| Mixed community controls | 32 | 169 | 201 |
| Psychiatric controls | 16 | 17 | 33 |
DISCUSSION
The SOCS is shorter than other self-report tools (Reference Bamber, Tamplin and ParkBamber et al, 2002; Reference Hudziak, Althoff and StangerHudziak et al, 2006) and has comparable or better discriminant characteristics. The high sensitivity and negative predictive value make the SOCS an adequate screening tool for settings such as general practice, educational psychology, paediatric services or dermatology clinics. Because of its moderate specificity the SOCS cannot be recommended for making diagnoses in psychiatric samples.
The use of a composite sample from the general population and from referred patients allowed collection of a large sample of young people with OCD. However, this enriched sample differed from the population encountered in community practice. Obsessive–compulsive disorder was more prevalent in the study sample and more severe forms of the disorder might be over-represented. A study of young people attending primary care will be needed to establish more accurate estimates of discriminatory characteristics for this setting.
The questionnaire is available online at http://ocdyouth.iop.kcl.ac.uk/downloads/socs.pdf. We hope that this simple tool will help to implement the NICE guideline recommendation to increase the awareness and detection of OCD in young people (National Collaborating Centre for Mental Health, 2005). It is potentially suitable for use in primary care, community child health services, educational psychology or specialist medical settings where OCD is common, such as dermatology clinics (Reference Fineberg, O'Doherty and RajagopalFineberg et al, 2003). A negative result (SOCS score 5 or lower) means that OCD is unlikely. A positive result does not mean that the young person has OCD but should serve as a basis for discussion with the young person and parents, and diagnostic assessment. In our experience, young people find that completing this measure helps them with the initial stages of treatment, as it provides them with a vocabulary to use with their therapist.






eLetters
No eLetters have been published for this article.