Rates of recruitment into psychiatry have been critically low in recent years, and in some parts of the UK mental health services are redesigning themselves for a future where they function with vastly fewer psychiatrists. In any other field of industry or human endeavour this situation would not be tolerated. If recruitment rates remained at such consistently abysmal levels in a large company, those employed to advertise and market the product would be sacked and a different approach adopted. If things persisted, those in charge on the board of the company would ultimately be fired. Why is the situation any different for psychiatry as a profession?
When we have attempted to re-market ourselves in recent years it has been psychiatrists who have designed strategies. The art and science of advertising, branding and marketing are not routinely covered in medical school and postgraduate curriculums. We have therefore no experience and expertise in these areas. Is it therefore any surprise that our attempts have floundered?
Almost every choice we make throughout the day, right down to the brand of laptop the reader might be viewing this article on, as well as the coffee they are sipping has been overtly or covertly influenced by professionals working in these fields. If we have not recognised this influence, then it merely serves to highlight the skill and effectiveness of those involved. Furthermore, as psychiatrists we take great pride in changing the thought patterns and behaviours of the patients we serve on an individual basis. Why would we not wish to learn and adopt techniques from fields that have expertise at doing this on a population level?
We have looked outside the worlds of psychiatry and academia for inspiration and to the worlds of advertising, branding and marketing. Some of the world's biggest companies from Coca-Cola to Apple have for decades been using a range of techniques to help them build brands that are loved and cherished by consumers. We need to apply the very same thinking to the challenges we face.
Reframing our objectives: knowing our audience
We know the undergraduate years are where negative attitudes and beliefs towards psychiatry take hold, 49% are favourable towards psychiatry as a career on entry, Reference Maidment, Livingstone, Katona, Whitaker and Katona1 whereas only 3% consider it on graduating. Reference Rajagopal, Redhill and Godfrey2 In marketing terms we therefore have a beautifully defined window of opportunity, and a captive audience to sell our discipline to. Therefore, getting an effective message across about psychiatry cannot happen early enough at medical school. The question is, even if we could reach new students, what positive ideas about psychiatry should we communicate? If we wish to counteract the powerfully corrosive bad mouthing that students hear about us from other disciplines, Reference Eagles, Wilson, Murdoch and Brown3 what should we say? This is where we need a strong brand.
Building a brand architecture
A brand is made up of many components, its attributes, audience, essence, etc (see Appendix). It is important to understand each of these elements and how they align in order to create a powerful brand that is meaningful for people and communicates confidently.
Developing a coherent brand that potential recruits can identify with might appear challenging. There are positive associations about psychiatry, however, even these can seem wildly disparate and contradictory, how can reassuringly scientific activities such as reading brain scans and intriguingly creative pursuits such as interpreting dreams possibly fall within the same specialty? However, we would argue that we should embrace these differences and incorporate them within our brand. We need to be clear that we are interested in the small number of doctors who can embrace the fields of science and the arts and also be confident enough to handle uncertainty and ambiguity. This of course does not appeal to the medical masses, however, it can also be a selling point. Niche brands such as Marmite have famously maximised their market share through making a virtue out of proudly advertising that they are not for everyone. Reference Mahdawi4
Bringing our brand to life
How we conduct ourselves in communicating our brand is a critically important starting point. We know that psychiatrists are victims of stigma, Reference Gaebel, Zäske, Zielasek, Cleveland, Samjeske and Stuart5 and having internalised this we may be part of the problem. Nothing sells like confidence. We need to inject confidence about what psychiatry is and does in everything we do.
We also know that we do not need to appeal to each and every medical undergraduate. We only need to increase our recruitment from 4 to 8% of medical graduates for all training places in the UK to be filled. Reference Davies6 This means that we can build a strategy around being selective. To date we have tended to try and sell ourselves as being ‘just as good’ as other medical specialties. This is a nonsensical way to market anything. (Did you choose your last holiday destination because it advertised itself as being just as good as some other place you had visited?) Instead we should be proudly elitist. Developing an air of exclusivity makes a product more desirable. Reference Mittone and Savadori7 Telling people they cannot have something makes them want it more. In recent years The Royal Marines have developed a highly successful recruitment drive based on this approach. Reference Jones8
We should be proud of and advertise the feet that we need the brightest and best doctors to enter psychiatry. The challenges involved in the job are vast (you know this), and a large number of doctors simply do not possess the mental agility to jump from biological to psychological to social paradigms within a single consultation. We should be telling students that we need the most special of them to come into our profession so that we can help develop them into a rare and exciting breed of doctor.
In recent years our approach has been to try and convince potential recruits and our colleagues from other disciplines that psychiatry is a ‘proper’ medical specialty and ‘just as scientific’ as others. As mentioned above, being ‘just as good’ would never be accepted as a marketing strategy in any other field. We should celebrate the phenomenal progress that has been made to date in understanding the mind, however, at the same time we should be clear that the frustrating limits of our knowledge is another thing that makes psychiatry uniquely attractive, that we are a discipline for pioneers and explorers.
Negative beliefs about the untreatability of psychiatric disorders can be challenged and turned into a selling point. Dare we communicate that neurology might be considered like understanding the electrical wiring to a light bulb in your house, whereas psychiatry in comparison is like building and flying a rocket to rescue a soul lost in the uncharted reaches of outer space? Such a ‘competitive’ approach between disciplines may seem initially unpalatable; however, it is worth remembering that Steve Jobs did not market Apple computers as being ‘just as scientific’ as Microsoft. Instead, this much smaller brand achieved a global identity and unprecedented success through a campaign of attracting those who wished to act and ‘think differently’. Reference Paris9
Such an approach also allows us to embrace our rich and controversial heritage and use this as a means of engagement rather than something to be nervously skirted around. If a student knows one thing about psychiatry it will be this, and it will be this they want to talk about (which reader has not been asked about One Flew Over the Cuckoo's Nest?). Can we not recognise that although R. D. Laing's mission was ultimately flawed, he did attempt to rescue those suffering and lost in psychic space using the best science available at the time; while still emphasising the lessons for today, namely that there is a need for a robust mission control to bring those doing ground-breaking work safely back to earth.
Ultimately though, the psychiatrist reading this piece is the media through which the brand is created, advertised and marketed. There will be no multi-million pound ad campaign. We need every person involved in the profession to live and breathe our brand and bring it to life every day and every time they come into contact with colleagues and students. Here are practical things you can do to promote a new brand of psychiatry.
-
(a) Be unashamedly confident and proudly elitist when talking about psychiatry. Psychiatry is not, and should not be for every doctor. Most doctors cannot handle the challenges, complexities, contradictions and uncertainties of the discipline. As a practising psychiatrist you can, so walk tall. Carry this into each and every interaction with students and with your medical colleagues from other disciplines.
-
(b) Have a ready explanation prepared for when someone asks you what a psychiatrist is, and does. If you are not comfortable with our suggested mantra (see below), develop your own based on the brand architecture model.
-
(c) Celebrate the achievements of psychiatry. Know of three psychiatrists whose work you admire and who have been influential and a force for good on a global scale. Tell others about them. (If you are stuck, shame on you, go Wikipedia Carl Jung, Karl Friston, Kenneth Kendler and Eric Kandel.)
-
(d) Think about and prepare answers for questions on our rich and controversial heritage: Bedlam, lobotomies, electroconvulsive therapy, LSD (lysergic acid diethylamide), anti-psychiatry, etc (you will be asked at the next dinner party you go to anyway). Be able to explain that the psychiatrist's role as a pioneer who searches out new ways to alleviate the suffering of those they serve was not, and still is not, without risk.
-
(e) Know of at least three celebrities who have had a positive experience of mental healthcare that you can tell others about (the British Royal Family have recently given you a head start).
-
(f) Think about and be prepared to tell others about cultural mega trends that link into psychiatry and that illustrate that we are the specialty of the moment, for the moment. Have at least two to hand (dementia, mindfulness etc.).
-
(g) Survey your local core trainees to identify the most engaging and charismatic teachers in each hospital. Incentivise these teachers to have as much exposure to medical undergraduates as early in the preclinical curriculum as possible.
-
(h) Communicate the key messages about ‘brand psychiatry’ to medical students as early as possible in the undergraduate years. These messages should be emphasised at the start and the end of every psychiatry block (to utilise the primacy and recency effect).
Fundamentally, we all are ‘brand psychiatry’ and this should be our mantra:
‘Psychiatrists are doctors who feel with their mind and think with their soul. They are just as comfortable with poetry as pathology. They see the person as whole. Psychiatrists understand the connection between the mind, the body and the soul. They are doctors who want to make a radical and transformational difference to the whole life of their patients. Psychiatrists are people who have the rare ability to treat the person, not the problem. Psychiatrists save lives.’
Appendix Brand architecture model
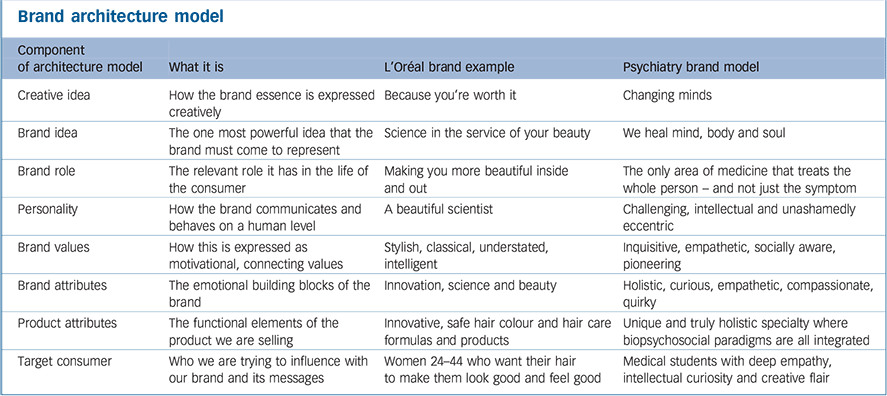
| Component of architecture model |
What it is | L'Oréal brand example | Psychiatry brand model |
|---|---|---|---|
| Creative idea | How the brand essence is expressed creatively |
Because you're worth it | Changing minds |
| Brand idea | The one most powerful idea that the brand must come to represent |
Science in the service of your beauty | We heal mind, body and soul |
| Brand role | The relevant role it has in the life of the consumer |
Making you more beautiful inside and out |
The only area of medicine that treats the whole person – and not just the symptom |
| Personality | How the brand communicates and behaves on a human level |
A beautiful scientist | Challenging, intellectual and unashamedly eccentric |
| Brand values | How this is expressed as motivational, connecting values |
Stylish, classical, understated, intelligent |
Inquisitive, empathetic, socially aware, pioneering |
| Brand attributes | The emotional building blocks of the brand |
Innovation, science and beauty | Holistic, curious, empathetic, compassionate, quirky |
| Product attributes | The functional elements of the product we are selling |
Innovative, safe hair colour and hair care formulas and products |
Unique and truly holistic specialty where biopsychosocial paradigms are all integrated |
| Target consumer | Who we are trying to influence with our brand and its messages |
Women 24–44 who want their hair to make them look good and feel good |
Medical students with deep empathy, intellectual curiosity and creative flair |





eLetters
No eLetters have been published for this article.