Community treatment orders (CTOs) in England and Wales were introduced by 2007 amendments to the Mental Health Act 1983, and have been used since November 2008. The Code of Practice states the principle is to provide an alternative to ongoing treatment in hospital and to prevent relapse and the harm associated with it. 1 The purpose of CTOs is to provide support and treatment to patients who would otherwise refuse treatment and deteriorate and return to hospital as a result.
Community treatment orders allow specific conditions to be attached to community treatment that are felt necessary or appropriate to ensure that the patient receives medical treatment, or to prevent risk of harm to the patient's health or safety, or to protect other people. Community treatment orders can be considered for people with a mental disorder who are detained in hospital for treatment but for whom treatment can be provided without continued detention, provided the patient is deemed liable to be recalled to hospital to receive treatment if there is a risk of harm to the health or safety of the patient or other people if they were not recalled. The purpose of recall is to allow a period of assessment (up to 72 h) of whether the CTO can continue (including the appropriateness of voluntary admission) or whether compulsory admission is necessary. If the latter is the case, the CTO is revoked and the patient is treated under the original order.
Before this legislation, individuals could be placed under a supervised discharge order (Section 25a). This allowed for conveyance of a patient to a suitable place where a formal Mental Health Act assessment could be undertaken to determine suitability for detention in hospital. There was a 6-month period from November 2008 during which patients who had previously been subject to provisions of Section 25a could be placed on a CTO without having to be readmitted to hospital.
There was significant controversy among professional and patient groups concerning the introduction of CTOs. Reference Lawton-Smith, Dawson and Burns2 Earlier authors raised ethical and practical objections and suggested that the introduction of CTOs was likely to lead to undermining of constructive working relationships with patients and further alienation and stigmatisation. Reference Moncrieff and Smyth3 This was countered by others, who argued that CTOs could be used successfully in place of compulsory detention in hospital, be a vital element in keeping a small number of people well, and reduce the marginalisation that can come with repeated hospital admissions. Reference Burns4 Nationally, the initial uptake of CTOs has been higher than expected. The Department of Health estimated 200 patients would become subject to supervised community treatment in the first year, rising to about 2250 patients after 5 years; 5 after only 5 months, however, 2100 CTOs had been implemented. By the end of March 2011, this figure was 10 071, and only 41.2% of these orders had ended (via revocation or discharge), with 3025 recalls to hospital and 1940 subsequent revocations. 6 This suggests some people are being maintained on supervised community treatment for long periods of time. No data were published about the percentage of revocations that eventually led to further CTOs.
Data indicate that within Suffolk in 2009-2010 there were 199 formal admissions and 31 CTO initiations (15.6%); 7 in 2010-2011 these figures were 191 and 44 (23.0%) respectively. 6 From all National Health Service organisations with 100 or more formal admissions, these percentages were 14.2% in 2009-2010 7 and 13.4% in 2010-2011. 6 There are no similar comparisons available for 2008-2009.
This paper aims to identify patients in Suffolk placed under a CTO within the first 8 months of legislation and to explore outcomes over a 2-year period following implementation of the CTO.
Method
The study population consisted of individuals under the care of one English mental health service (Suffolk Mental Health Partnership NHS Trust) on whom a CTO was initiated between 3 November 2008 and 2 July 2009. The study was approved as clinical audit by the Trust's clinical governance department. Data on biological, psychosocial, risk, follow-up and support factors over 2 years following CTO were compared with data from the same period before CTO; each patient acted as his or her own control. The date of the CTO was the point of division for retrospective and prospective data. All patients were assigned a sheet designed for the study on which data were entered.
General data consisted of electronic patient record number, age, gender, relationship and employment status. Biological data consisted of primary psychiatric diagnosis, comorbid conditions, treatments, number of admissions, length of each stay and episodes of leave from hospital. Diagnoses were recorded in multi-axial DSM-IV format, and an ICD-10 code was given to Axis I and Axis II psychiatric disorders. Treatments involving psychotropic medications were recorded from the patients’ medication charts.
Clinical response to treatment, functionality, risks and insight were assessed and recorded using the Global Assessment of Functioning GAF (Axis V of DSM-IV) 8 and the Threshold Assessment Grid (TAG). Reference Slade, Powell, Rosen and Strathdee9 The GAF measures psychological, social and occupational functioning on a hypothetical continuum (0-100). The TAG considers severity of mental health problems across seven domains: the first four domains assess risk to self and others, and the last three domains assess survival and psychosocial risks; scores for each domain vary between 0 (none) to 3 (severe) for domains 2, 3, 6 and 7, and between 0 (none) and 4 (very severe) for domains 1, 4 and 5.
The GAF and TAG were measured at index admission, at commencement of CTO and at 2-year follow-up. Social circumstances were recorded in the form of type of accommodation and community support systems. We measured the following main outcome measures.
-
• Duration of time spent in the community (either discharged from hospital or on leave) and number of admissions to hospital. In England a CTO can be implemented only following formal admission, and so time spent within hospital in the index admission was excluded from the comparative analysis. Proportions of time spent in the community before and after the CTO were analysed (not absolute times, as the time period at risk varied from person to person, depending on the length of the index admission). Leave periods within the index admission were included, because before the 2007 amendments to the Mental Health Act it was not atypical for patients to spend significant periods on leave of absence from hospital, subject to conditions deemed necessary by the responsible medical officer (Section 17 leave). Similarly, the index admission was removed from the statistical analysis of numbers of admissions, which were studied per unit time before and after.
-
• Level of engagement with services: a discrete scale was devised to note this and used when reviewing each patient record:
-
0 = complete disengagement and non-adherent to treatment
-
1 = minor engagement (some appointments attended and doubtful adherence to medication)
-
2 = intermittent engagement (approximately 50% of appointments attended and mainly adherent to medication)
-
3 = good engagement (most appointments attended and generally adherent to treatment)
-
4 = excellent engagement (all appointments attended and completely adherent to treatment).
-
Where appropriate, we used paired t-tests to elucidate differences, or Wilcoxon matched-pairs signed-rank tests for differences not assumed to be normally distributed.
Results
Demographics
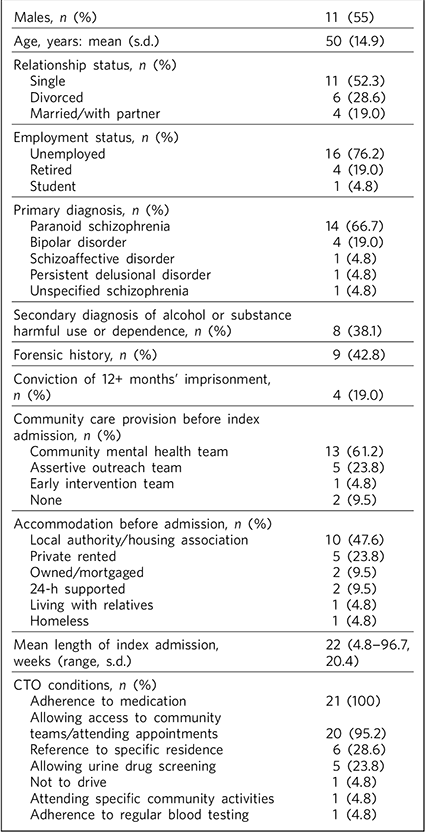
Within the first 8 months of legislation, 21 patients were placed on a CTO (including 1 patient whose status was changed from Section 25a to a CTO). All patients were White. The patients’ age, gender, employment status, relationship status, diagnosis, forensic history, prior community care provision, length of admission and subsequent CTO conditions are shown in Table 1.
TABLE 1 Demographic information of patients and community treatment order (CTO) conditions
| Males, n (%) | 11 (55) |
|---|---|
| Age, years: mean (s.d.) | 50 (14.9) |
| Relationship status, n (%) | |
| Single | 11 (52.3) |
| Divorced | 6 (28.6) |
| Married/with partner | 4 (19.0) |
| Employment status, n (%) | |
| Unemployed | 16 (76.2) |
| Retired | 4 (19.0) |
| Student | 1 (4.8) |
| Primary diagnosis, n (%) | |
| Paranoid schizophrenia | 14 (66.7) |
| Bipolar disorder | 4 (19.0) |
| Schizoaffective disorder | 1 (4.8) |
| Persistent delusional disorder | 1 (4.8) |
| Unspecified schizophrenia | 1 (4.8) |
| Secondary diagnosis of alcohol or substance harmful use or dependence, n (%) |
8 (38.1) |
| Forensic history, n (%) | 9 (42.8) |
| Conviction of 12+ months’ imprisonment, n (%) |
4 (19.0) |
| Community care provision before index admission, n (%) |
|
| Community mental health team | 13 (61.2) |
| Assertive outreach team | 5 (23.8) |
| Early intervention team | 1 (4.8) |
| None | 2 (9.5) |
| Accommodation before admission, n (%) | |
| Local authority/housing association | 10 (47.6) |
| Private rented | 5 (23.8) |
| Owned/mortgaged | 2 (9.5) |
| 24-h supported | 2 (9.5) |
| Living with relatives | 1 (4.8) |
| Homeless | 1 (4.8) |
| Mean length of index admission, weeks (range, s.d.) |
22 (4.8-96.7, 20.4) |
| CTO conditions, n (%) | |
| Adherence to medication | 21 (100) |
| Allowing access to community teams/attending appointments |
20 (95.2) |
| Reference to specific residence | 6 (28.6) |
| Allowing urine drug screening | 5 (23.8) |
| Not to drive | 1 (4.8) |
| Attending specific community activities | 1 (4.8) |
| Adherence to regular blood testing | 1 (4.8) |
Six patients changed accommodation to more supported arrangements before discharge from hospital, and one patient moved from a community mental health team to community forensic psychiatric services.
Measurements and follow-up
One patient died from a physical condition. Of the remaining 20 patients, 7 were still subject to a CTO after 2 years. Of the CTOs that ended, five were allowed to expire, three were discharged by a tribunal, and five were discharged by the responsible clinician. In the 2 years after a CTO initiation, the mean length of time a patient remained subject to it was 52.6 weeks (s.d. = 31.7 weeks).
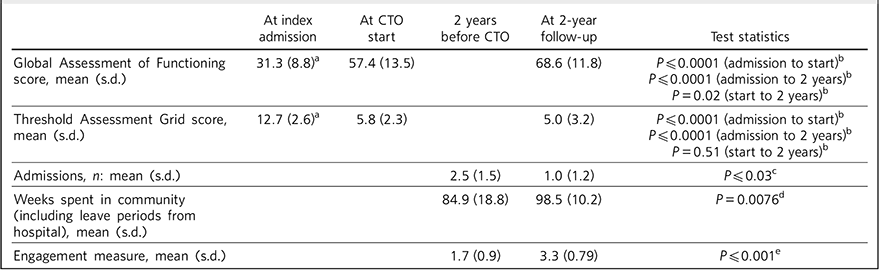
Table 2 illustrates GAF and TAG measurements at index admission, at the start of the CTO and at 2-year follow-up; the number of admissions; time spent in the community; and engagement level.
TABLE 2 Results
| At index admission |
At CTO start |
2years before CTO |
At 2-year follow-up |
Test statistics | |
|---|---|---|---|---|---|
| Global Assessment of Functioning score, mean (s.d.) |
31.3 (8.8)Footnote a | 57.4 (13.5) | 68.6 (11.8) |
P⩽0.0001 (admission to start)Footnote
b
P⩽0.0001 (admission to 2 years)Footnote b P=0.02 (start to 2 years)Footnote b |
|
| Threshold Assessment Grid score, mean (s.d.) |
12.7 (2.6)Footnote a | 5.8 (2.3) | 5.0 (3.2) |
P⩽0.0001 (admission to start)Footnote
b
P⩽0.0001 (admission to 2 years)Footnote b P =0.51(startto2years)Footnote b |
|
| Admissions, n: mean (s.d.) | 2.5 (1.5) | 1.0 (1.2) | P⩽0.03Footnote c | ||
| Weeks spent in community (including leave periods from hospital), mean (s.d.) |
84.9 (18.8) | 98.5 (10.2) | P = 0.0076Footnote d | ||
| Engagement measure, mean (s.d.) | 1.7 (0.9) | 3.3 (0.79) | P⩽0.001Footnote e |
CTO, community treatment order.
a Excluding one patient not admitted before CTO (converted from Section 25).
b Two-tailed t-test, paired observations.
c Wilcoxon matched pairs. Difference between admissions per unit time (excluding index admission).
d Two-tailed t-test, paired observations. Difference in proportion of time spent in community (statistical analysis excludes time spent in hospital on index admission).
e Wilcoxon matched pairs.
Fourteen patients were receiving depot medication at the start of the CTO. After 2 years these individuals had spent an average of 95.0 weeks in the community and had been admitted an average of 0.8 times; the average length of each admission was 5.2 weeks. This compared with 83.8 weeks in the community and 1.3 admissions, and an average length of admissions of 12.0 weeks for the seven individuals receiving only oral antipsychotic medication at the start of the CTO. This was a significant reduction in admissions (P = 0.0001). Medication was changed in six individuals (two commenced clozapine from a depot, two moved from depot to other oral medications, two started a depot). The confounding variables and lack of power in the study precluded further detailed statistical comparisons of this.
Discussion
There are obvious weaknesses in this study, including small numbers of patients, localised geographical area, lack of a control group over the same time period, and investigators being unmasked to any factors. Despite national guidelines, it has been demonstrated that there is variation in uptake of legislation; therefore, this is a pragmatic survey of outcomes and the method can be used by others to monitor use of supervised community treatment within their own services.
Numbers of recalls and revocations were not reported since the purpose of this study was to measure outcomes of CTOs with respect to the intention of the legislation – namely, to decrease time spent within hospital for a group of patients who have repeated admissions due to frequent relapses. Anecdotally, the severity of mental illness tolerated before recall to hospital varied considerably between teams, and further analysis or other research examining factors considered when patients are recalled may be beneficial.
Individuals within this group, from a population where 5.6% individuals are Black or minority ethnic, 10 were all White. There was an average age of 50 years and a similar proportion of males and females. A significant proportion of patients had a history or current use of alcohol or illicit substances, or had a forensic history; all had a major psychotic illness. This compares with a paper describing the first 6 months of CTO use in Birmingham, which showed CTOs were used in people who displayed a high recorded rate of violence and alcohol or substance misuse, and which was consistent with previous international studies demonstrating typical use in males aged around 40 years with a psychotic illness, with an overrepresentation of Black and minority ethnic groups. Reference Evans, Makala, Humphreys and Mohan11
Scotland has had CTOs since October 2005. Although such CTOs are applied only by a mental health tribunal after detention in hospital or as an alternative to a hospital order, it may be useful to compare their use. One study reported CTOs constituting about 30% of all long-term civil orders. From a review of almost 500 individuals in 2009, 81% had a diagnosis of schizophrenia, 57% were prescribed a depot, 63% were male, 63% lived alone, and 65% were viewed as posing a risk to others. Reference Taylor12
Two randomised controlled trials explored community orders in the USA more than 10 years ago. One trial reported no significant findings; Reference Steadman, Gounis, Dennis, Hopper, Roche and Swartz13 the other trial initially revealed no differences, but a post hoc analysis found that patients under a community order for more than 6 months with high levels of support had fewer admissions to hospital and spent less time in hospital. Reference Swartz, Swanson, Wagner, Burns, Hiday and Borum14 A Cochrane review of the US trials did not find evidence that CTOs decreased readmission or improved quality of life. Reference Kisely, Campbell and Preston15 The current study demonstrates significant positive group differences, revealing increased time spent in the community, decreased number of admissions, and improvement in functioning following implementation of a CTO. Only one patient spent less time in the community, and only three patients had more admissions to hospital.
Another review of international studies found no evidence to support CTOs decreasing relapse rates or improving adherence to treatment. Reference Churchill, Owen, Singh and Hotopf16 Measurement of adherence within our study was crude, subjective and not masked but showed improvements with treatment adherence and management. Some patients improved dramatically in these measurements, and it may be pertinent to perform a post hoc analysis to identify possible factors to be examined more closely in further studies (e.g. accommodation status, level of support given by treating team, amount of contact with professionals). Experientially there is no doubt that some patients benefit greatly from the use of CTOs, but factors contributing to this need to be identified clearly. A naturalistic study performed in Canada concluded that patients found CTOs provided structure in their lives and valued ongoing support. Reference O'Reilly, Keegan, Corring, Shrikhande and Natarajan17
Data from an Australian study showed that individuals subject to a CTO were more than three times as likely to be receiving depot medication. Reference Lambert, Singh and Patel18 Anecdotally within Suffolk, this perspective, along with the view that use of a depot with CTO is more beneficial than oral medication in effective monitoring, prevention of relapse and readmission, was believed but without evidence. Of the 21 patients, 14 were receiving depots at the start of the order, and crude analysis revealed this group had fewer and shorter admissions in the 2 years following the start of a CTO. Although the small number of patients studied makes the chance of false positive results a possibility, it could be a factor to consider when selecting types of patient who would benefit from the use of supervised community treatment.
Although measurements of functioning and risk using the GAF and TAG were taken at index admission, at initiation of CTO and at 2-year follow-up, no control group or comparison was available for the time before CTO. There was a significant decrease in TAG measurements from index admission to the start of the CTO (P⩽l0.0001), which was maintained after 2 years (P⩽l0.0001), but with no significant difference between the start of the CTO and at 2-year follow-up (P = 0.51). There was significant improvement in GAF scores, both between admission and the start of the CTO (P⩽l0.0001) and between the start of the CTO and 2-year follow-up (P = 0.02). The number of patients in this current study precluded the use of statistical analyses examining multiple specific factors associated with outcome (e.g. admissions, medication), but a post hoc analysis to consider the factors to be looked at in future studies may be worthwhile. It is heartening to note improvements, but the question remains – could this improvement be replicated by assertive follow-up from community teams without using legislation? This poses further questions: how can identification of individuals who would benefit from CTO be refined, and does a CTO provide simply more care rather than different care? It is hoped that the national multi-centre programme of prospective research Reference Burns, Rugkasa and Molodynski19 and other studies examining mandated community treatment (e.g. the MacArthur studies Reference Monahan, Needham, Nijman, Palmistierna, Almvik and Oud20 ) will provide more detail regarding the use and outcomes of supervised community treatment and contribute greatly to answering these questions.
Community treatment orders appear to be used as a relatively long-term commitment, and this study supports this finding in Suffolk. The study also demonstrates that in a significant minority of patients, the CTO was allowed to expire rather than being formally discharged (while others were discharged around the time renewal was due). Given that best practice is to ‘keep under review the appropriateness of using that power [to discharge patients]’, this needs to be examined further. 21 It may be that previously mentioned findings of some patients viewing these orders as protective could contribute to their length of use, although this may be at odds with Code of Practice guidance. This was essentially a study that collected data; one weakness was that the study did not directly ask patients, carers and professionals about the perceived usefulness of implementing this legislative order in their treatment. Any further examination would benefit greatly from the involvement and feedback of these groups of people, and it may be pertinent to refer to Care Quality Commission feedback on the use of CTOs to pilot any research in this area.
Acknowledgements
The authors would like to thank Chris Foy for statistical advice.







eLetters
No eLetters have been published for this article.