Prion diseases are neurodegenerative illnesses caused by conversion of normal prion protein (PrPc) to misfolded abnormal prion (PrPSc) through an infection-like molecular templating process.Reference Geschwind1 They may be sporadic, genetic or acquired, with 85–95% of cases classified as sporadic Creutzfeldt-Jakob disease (CJD).Reference Geschwind1 The typical presentation of CJD is rapid cognitive decline with myoclonus, visual disturbances, cerebellar dysfunction, pyramidal/extrapyramidal symptoms, and/or cortical findings, and death typically occurs within 12 months.Reference Geschwind1 Although no disease-modifying therapy exists, accurate diagnosis remains paramount to ensure that another treatable condition is not missed. Data regarding the utility of cerebrospinal fluid (CSF) biomarkers to diagnose CJD (14-3-3, S100B, neuron-specific enolase and total tau) is conflicting, and they may be elevated in other dementing illnesses.Reference Geschwind1, Reference Forner, Takada and Bettcher2 Electroencephalography (EEG) characteristically shows periodic sharp-wave complexes (PSWCs), which were initially reported to have a sensitivity of 64% for CJDReference Steinhoff, Zerr, Glatting, Schulz-Schaeffer, Poser and Kretzschmar3; a more recent study, however, found a sensitivity of only 44%, and PSWCs may not be seen in the initial stages of the disease.Reference Geschwind1, Reference Hermann, Laux and Glatzel4 Brain magnetic resonance imaging (MRI) looking for cortical and basal ganglia diffusion restriction is a highly sensitive and specific diagnostic tool in CJD, but these abnormalities are frequently not reported or misinterpreted.Reference Forner, Takada and Bettcher2, Reference Vitali, Maccagnano and Caverzasi5, Reference Carswell, Thompson and Lukic6
A test using cyclic shaking of samples on the FLUOstar Omega plate reader to mimic the PrPc to PrPSc conversion process in an accelerated in vitro format, known as real-time quaking-induced conversion (RT-QuIC), has been touted as a prion-specific assay with a high sensitivity (about 90%) and near-perfect specificity (98–100%) in CJD.Reference Geschwind1, Reference McGuire, Peden and Orrú7 The Canadian National Microbiology Laboratory (NML) in Winnipeg, Manitoba now offers a similar test that instead uses Eppendorf ThermoMixer-aided shaking, called endpoint quaking-induced conversion (EP-QuIC).Reference Cheng, Vendramelli and Sloan8 In a retrospective case-control analysis comparing EP-QuIC to RT-QuIC, EP-QuIC was found to have a sensitivity and specificity of 98% and 91%, respectively, for the diagnosis of CJD, indicating a slightly lower specificity but higher sensitivity than RT-QuIC.Reference Cheng, Vendramelli and Sloan8 Importantly, while RT-QuIC has been shown to have a high negative predictive value (NPV) of 91% and excellent positive predictive value (PPV) of 100% in the diagnosis of CJD, a similar investigation into the predictive value of EP-QuIC has not been performed.Reference Franceschini, Baiardi and Hughson9 In particular, evaluation of the PPV of EP-QuIC is needed, since its potentially slightly lower specificity compared to RT-QuIC may translate to false-positives when tested in a low-prevalence population. We report an exploratory analysis of the NPV and PPV of EP-QuIC for CJD at London Health Science Centre (LHSC) in London, Ontario.
Patients were reviewed for study inclusion if they a) were assessed at LHSC for suspected CJD, b) had CSF sent to the NML for EP-QuIC testing from 2016 to –2018, and c) had EP-QuIC performed that was reported as positive or negative. In this study, patients who met neuropathologic criteria for definite CJD or University of California San Francisco (UCSF) 2007 criteria for probable CJD were classified as CJD, unless a more likely alternative diagnosis was identified clinically or pathologically resulting in a classification of non-CJD.Reference Geschwind1, Reference Geschwind, Josephs, Parisi and Keegan10 Remaining patients were otherwise classified as non-CJD, as long as a more likely diagnosis than CJD was identified clinically or pathologically.Reference Geschwind1, Reference Geschwind, Josephs, Parisi and Keegan10 Any patient who did not meet criteria for definite or probable CJD but who had no more likely alternative diagnosis identified was excluded from our analysis, given the level of diagnostic uncertainty. All clinical information, neuroimaging and EEG reports were reviewed by two authors (AB and RGT) to determine whether patients met criteria for definite/probable CJD. If there was a discrepancy between the reporting neuroradiologist and these two authors, then their images were reviewed by an independent senior neuroradiologist to determine whether the MRI findings were typical of CJD or not. Any patient with periodic discharges on EEG reportedly concerning for prion disease had their EEG reviewed by an electroencephalographer (JGB) to determine the presence or absence of PSWCs. Once all study patients were classified as CJD or non-CJD, the NPV and PPV of EP-QuIC for CJD was calculated.
A total of 22 patients who had CSF sent to the NML for EP-QuIC testing from 2016 to 2018 were identified and reviewed for study inclusion. Three patients did not meet inclusion criteria for our analysis (One bloody CSF sample precluding EP-QuIC testing; One indeterminate EP-QuIC result; One patient did not meet diagnostic criteria for definite or probable CJD, but no more likely alternative diagnosis was identified clinically and no autopsy was performed). There were 19 patients remaining that met inclusion criteria for our analysis. Five patients were classified as CJD, while the remaining fourteen patients were classified as non-CJD (see Table 1 for alternative diagnoses). Patient characteristics including age, sex, presence of MRI findings typical of CJD, presence of PSWCs on EEG, presence of elevated CSF biomarkers, and the presence of CSF pleocytosis or elevated protein can be found in Table 2. Brain MRI findings typical of CJD were seen in all CJD cases and not observed in any non-CJD cases. On EEG, however, PSWCs were not seen in any CJD cases. Regarding CSF biomarkers for CJD, a positive CSF 14-3-3 or positive CSF total tau was more common among CJD cases than non-CJD cases, but this difference did not reach statistical significance.
Table 1: Alternative diagnoses in patients classified as non-CJD

Table 2: Patient characteristics among those classified as CJD compared to non-CJD
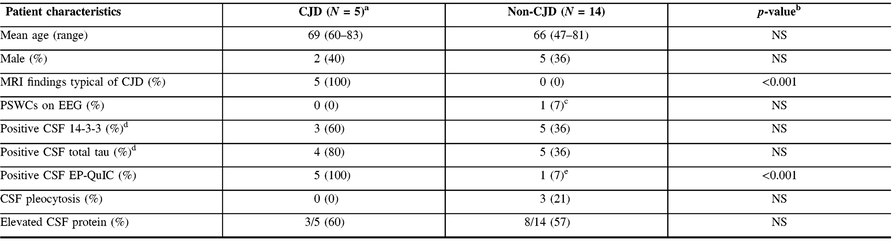
CJD = Creutzfeldt-Jakob disease; CSF = cerebrospinal fluid; EEG = electroencephalogram; EP-QuIC = endpoint quaking-induced conversion; MRI = magnetic resonance imaging; NML = National Microbiology Laboratory; NS = not significant; PRNP = prion protein gene; PSWCs = periodic sharp-wave complexes; WBC = white blood cell
a Of the five patients with CJD, four patients were considered to be sporadic and one patient was confirmed to have genetic CJD with a family history of CJD and a PRNP E200K mutation identified.
b Statistical significance set at p < 0.00625 using Bonferroni correction to account for multiple comparisons. P-value calculated using Student’s t-test or Fisher’s exact test, as appropriate.
c Generalized periodic discharges resembling PSWCs were seen in one non-CJD case. This patient had reversible MRI white matter changes and CSF pleocytosis most concerning for an inflammatory process, with superimposed sepsis with recurrent cellulitis. She recovered and lived for over 1 year before ultimately passing away due to sepsis from infected decubitus ulcers (no autopsy was performed as there was no ongoing concern of CJD).
d Positive CSF 14-3-3 or positive CSF total tau refers to a reported value above the cut-off set by the NML, which is 20,000 AU/mL for CSF 14-3-3 and 976 pg/mL for CSF total tau.
e Patient with false-positive EP-QuIC is described in manuscript. The CSF WBC count for this patient was 2 WBC/µL (normal 0–5 WBC/µL) and the CSF protein was 1057 mg/L (normal 200–400 mg/L). Elevations in CSF WBC or protein are not expected to result in a false-positive EP-QuIC.
In this study, 5/5 patients classified as CJD had a positive EP-QuIC result, compared to only 1/14 patients classified as non-CJD. The calculated NPV and PPV of EP-QuIC was 100% and 83%, respectively. Importantly, one patient had a positive EP-QuIC in April 2016 but a neuropathologically proven alternative diagnosis of amyloid beta-related angiitis. On retrospective review of this patient’s chart by AB and RGT, the pre-test probability of CJD at the time of EP-QuIC testing was deemed very low. The patient had prominent early seizures, leptomeningeal enhancement and new multifocal white matter T2-signal abnormalities on MRI, all of which are highly atypical of prion disease and concerning for an inflammatory disease etiology. In discussing this case with the NML, it was learned that the EP-QuIC protocol had been modified as of April 2017. When this patient’s sample was re-analyzed using this modified EP-QuIC protocol, which is currently used as standard of practice at the NML, it was reported as negative. Using this updated result led to a revised PPV of 100% for EP-QuIC in CJD.
In this first Canadian study investigating the predictive value of EP-QuIC for CJD, we found an NPV and PPV of 100% and 83%, respectively. The EP-QuIC test has, however, been optimized since its introduction, and as described above the modified EP-QuIC protocol currently in use at the NML would have eliminated the false-positive result we identified and resulted in a PPV of 100%. Of note, there are several limitations to our study. This is an exploratory single-centre review of a diagnostic test performed for a rare disease, and so the sample size is expectedly small. Due to its retrospective nature, there were no pre-defined criteria regarding who was selected for EP-QuIC testing. However, this is reflective of routine clinical practice, since clinicians frequently order this test on patients with a rapidly progressive neurologic syndrome of unclear cause. We did not have pathologic confirmation of diagnoses in the majority of cases, but fortunately the only case that was initially classified as a false-positive EP-QuIC had neuropathologic data confirming an alternative diagnosis.
Despite the limitations of our study, several conclusions can be drawn that are helpful to the practicing clinician. The NPV of EP-QuIC was 100%, and although our sample size is small this suggests that the diagnosis of prion disease should be critically re-evaluated in a patient with suspected CJD but a negative EP-QuIC result. Perhaps more importantly, even though the number of patients with a positive EP-QuIC in our study was small we still had one initial false-positive result. The potential consequences of false-positives are magnified by recently proposed criteria that allow for a diagnosis of probable CJD to be made with a positive RT-QuIC and only one clinical symptom.Reference Hermann, Laux and Glatzel4 The misdiagnosis of this invariably fatal disease is immensely distressing to patients and can hinder identification of a treatable condition, so every effort must be made to avoid false-positive results in suspected CJD. Canadian practitioners should be aware that although EP-QuIC is a highly useful clinical test, it has not yet been reported to have the near-perfect specificity of RT-QuIC.Reference McGuire, Peden and Orrú7, Reference Cheng, Vendramelli and Sloan8 Rectification of our false-positive result using the current modified EP-QuIC protocol is encouraging, but continued evaluation of test sensitivity, specificity, positive and negative predictive value is needed before it can be said with certainty that EP-QuIC may serve as a substitute for RT-QuIC in newly proposed diagnostic criteria for CJD.Reference Hermann, Laux and Glatzel4 Since no non-pathologic test for CJD can provide a definitive diagnosis, practitioners must consider all the available clinical and ancillary test information when evaluating suspected cases. Our study highlights that although EP-QuIC is a valuable diagnostic test in patients with suspected CJD, Canadian health care providers should use caution when interpreting a positive EP-QuIC result in a patient with clinical, radiographic or laboratory findings that are clearly atypical for prion disease.
Funding
Although not relevant to this manuscript, Dr. JGB discloses that he receives support from Western University through the Jack Cowin Chair in Epilepsy Research, research support from EpLink and the Ontario Brain Institute, and has received funding from Western University.
Conflict Of Interest
Drs. AB, RGT, JF, JDK, and SHP have no conflicts of interest to disclose.
Statement of authorship
Dr. AB participated in the study design, analyzed the data, reviewed the neuroimaging and drafted the manuscript. Dr. RGT participated in the study design, analyzed the data, reviewed the neuroimaging and edited the manuscript for intellectual content. Dr. JF aided in results interpretation and edited the manuscript for intellectual content. Dr. JGB reviewed the electroencephalography, aided in results interpretation and edited the manuscript for intellectual content. Dr. JDK aided in study design, results interpretation, and edited the manuscript for intellectual content. Dr. SHP aided in study design, results interpretation, and edited the manuscript for intellectual content.






