Vitamin D insufficiency (<50 nmol/l) is highly prevalent worldwide( Reference van Schoor and Lips 1 ) and has been associated in observational studies with an increased risk of a wide range of chronic diseases, including osteoporosis, cancer, CVD, diabetes, multiple sclerosis and infectious diseases( Reference Holick 2 ), albeit evidence from randomised controlled trials is required to confirm direction of causality.
The economic burden of vitamin D deficiency is potentially phenomenal. In 2009 Grant et al. calculated a projected saving of €187 billion per year if all Western Europeans had a serum 25-hydroxyvitamin D (25(OH)D) concentration of 40 ng/ml (100 nmol/l)( Reference Grant, Cross and Garland 3 ), making reduction of vitamin D deficiency a high public health priority. Note that this is high target for vitamin D status (most guidelines( 4 , 5 ) recommend 25 or 50 nmol/l as a definition of vitamin D sufficiency), but the Grant et al. paper illustrates the point that vitamin D deficiency is costly to society.
Recent studies have highlighted high rates of vitamin D deficiency (<50 nmol/l) in Western-dwelling South Asians in North America( Reference Xiao, Wood and Swist 6 – Reference Sham, Yeh and Magalhaes 8 ), Europe( Reference Darling, Hart and Macdonald 9 – Reference Holvik, Meyer and Haug 18 ) and Australasia( Reference von Hurst, Stonehouse and Coad 19 ). This is likely to be underpinned in large part by darker skin pigmentation( Reference Libon, Cavalier and Nikkels 20 ), low sun exposure of the skin due to dress coverage and sun avoidance behaviour( Reference Kift, Berry and Vail 21 , Reference Kotta, Gadhvi and Jakeways 22 ), low dietary exposure to foods containing vitamin D( Reference Darling, Hart and Macdonald 9 , Reference Donin, Nightingale and Owen 23 ) and high prevalence of overweight/obesity (BMI≥25 kg/m2)( Reference Lyratzopoulos, McElduff and Heller 24 ). Improvement in vitamin D status is likely to help reduce the incidence of a variety of chronic diseases common in Western-dwelling South Asians, such as type 2 diabetes and CVD( Reference Barnett, Dixon and Bellary 25 ).
To tackle the problem of vitamin D deficiency (<50 nmol/l) in Europe, the European Food Safety Authority recommended an intake of 15 µg/d (600 IU/d) for all adults( 5 ). In the UK, the Scientific Advisory Committee on Nutrition (SACN) recently advised a Recommended Nutrient Intake for vitamin D of 10 µg/d for the whole UK population aged 4 years or over( 4 ). However, the UK diet is low in vitamin D, with the National Diet and Nutrition Survey (NDNS) reporting intakes of 1·8–3·2 µg/d in males and 1·8–2·3 µg/d in females, depending on survey year and age group( Reference Whitton, Nicholson and Roberts 26 ). Therefore, in practice the European Food Safety Authority and SACN advice translates into using a vitamin D supplement of cholecalciferol or ergocalciferol of up to 10–15 µg/d for most people who do not have a daily intake of at least one 100–150 g portion oily fish (e.g. 100 g of farm-raised salmon=10 µg of vitamin D( Reference Lu, Chen and Zhang 27 )) or substantial summer sun exposure. Other dietary sources of vitamin D (e.g. eggs, fortified breakfast cereal, cereals, fortified spreads) can also contribute to getting an intake of 10 µg/d but are available only in smaller amounts in the diet (e.g. 1 egg contains 1 µg of vitamin D).
In the SACN deliberations, there was a considerable lack of evidence regarding vitamin D status in South Asians to justify a separate recommendation for South Asians in the UK( 4 ). However, it is certainly plausible that such a recommendation be necessary considering South Asians’ higher vitamin D risk factors than other UK ethnic groups. The SACN report( 4 ) called for more information regarding the vitamin D requirements in South Asians and there is a clear need for specific insights into the demographic, dietary and lifestyle factors associated with supplement usage in UK South Asians.
To our knowledge, there are no studies that have reported on the use of vitamin D supplementation and its predictors among UK or other Western-dwelling South Asian adults specifically. Moreover, data on vitamin D intakes in different UK-based South Asian groups are extremely limited. One study found a vitamin D intake of 1·4 µg/d in South Asian boys, with no difference between those of Bangladeshi, Indian or Pakistani ethnicity( Reference Donin, Nightingale and Owen 23 ). Intakes of vitamin D in South Asian women have been estimated to be 1·2–2·2 µg/d( Reference Darling, Hart and Macdonald 9 , Reference Kift, Berry and Vail 21 ) depending on study and season.
In the present study our objective was twofold: first, using data from the UK Biobank cohort (8024 South Asians) to quantify dietary intakes of vitamin D and assess the occurrence of vitamin-D-containing supplement use among three different South Asian population groups (Bangladeshi, Indian and Pakistani); and second, to assess how demographic, dietary and lifestyle factors are associated with vitamin-D-containing supplement use among these populations. We hypothesised that vitamin D intakes would be lower in the Indian group than in the Bangladeshi and Pakistani groups due to the common consumption of vegetarian and vegan diets in Indian populations. Based upon known predictors of vitamin D supplement users in other ethnic groups( Reference Black, Jacoby and Nowson 28 , Reference Greene-Finestone, Langlois and Whiting 29 ), we hypothesised that women, and those of higher socio-economic status, would be more likely to use a vitamin D supplement than men, and those of a lower socio-economic status.
Methods
UK Biobank cohort
Briefly, the UK Biobank (www.ukbiobank.ac.uk/) is a large ongoing UK-wide cohort of over 500 000 individuals aiming to investigate exposures which impact on health outcomes in middle and older life( Reference Sudlow, Gallacher and Allen 30 ). The data collection has included a wide range of exposures and outcomes including demographic, dietary and lifestyle factors as well as genetic and biochemical markers. The participants were aged 40–69 years at the baseline visit and were recruited during the period 2006–2010 via central National Health Service (NHS) registers( Reference Sudlow, Gallacher and Allen 30 ). In the current cross-sectional analysis, all UK Biobank participants were eligible for inclusion if they self-reported as of ‘Bangladeshi’, ‘Indian’ or ‘Pakistani’ ethnicity, giving 8024 South Asians (3730 women, 4294 men) of whom 236 were Bangladeshi, 5951 were Indian and 1837 were Pakistani. No other inclusion or exclusion criteria were used. See Fig. 1 for illustration of the numbers of participants entering the current analysis from the whole UK Biobank cohort.

Fig. 1 Flowchart of UK Biobank participants: numbers of participants in the analyses as compared with the whole cohort (n 8024)
Dietary questionnaires
24 h dietary recall questionnaire
Baseline vitamin D intake in the UK Biobank was estimated from a participant-completed 24 h recall questionnaire which measured the frequency of foods consumed the previous day. The questionnaire covered the following food groups: Hot and cold beverages; Alcoholic beverages; Cereal; Milk, eggs and cheese; Bread, pasta and rice; Soups, snacks and pastries; Meat and fish; Vegetarian alternatives; Spreads, sauces and cooking oils; and Fruit and vegetables( 31 ). Therefore, the main food groups that contain vitamin D were included. The nutrient intake was calculated by multiplying the weight of food consumed (grams) by the vitamin D content per gram as defined by the 5th edition of McCance and Widdowson’s The Composition of Foods ( Reference Liu, Young and Crowe 32 , Reference Holland, Welch and Unwin 33 ). This questionnaire has previously been validated against other 24 h recall methods and compares well for the estimation of most nutrients (10 % difference or less between the methods)( Reference Liu, Young and Crowe 32 ). As vitamin D is likely to be poorly estimated based on one 24 h dietary recall, we decided to use the median vitamin D intake calculated for each participant across all dietary recalls completed.
This questionnaire included questions about how frequently the participant had consumed 200 foods and drinks (e.g. ‘Did you eat any bread or crackers yesterday?’). The questionnaire also asked about supplement use but these data were not included in the calculation of the nutrient intake. We did not include this in our calculation of how many people were on supplements because only one person who had not originally answered the touchscreen question (with a valid response) on supplement use answered this question (so it did not add anything to the analysis). The last 70 000 participants completed this questionnaire at the baseline visit using the touchscreen computer, and all participants who had provided the investigators with email addresses were invited to complete the same questionnaire from their home computer on four subsequent occasions from February 2011 to April 2012( 31 ), meaning that the maximum number of completions was five times. Invites were timed to ensure different days of the week were targeted on each occasion.
Food frequency (touchscreen) questionnaire
Frequency of consumption of different food groups was recorded via the Oxford WebQ FFQ( 34 ) on the touchscreen computer at the baseline visit. This was used only to code participants as vegetarian or not, and for estimation of oily fish intake for the logistic regression modelling. For the purposes of the current analysis, we defined individuals as vegetarian (no consumption of meat or fish) based on them having answered ‘never consumes’ to all of the following food categories on the touchscreen questionnaire: oily fish, non-oily fish, processed meat, poultry, pork, beef, lamb and mutton. This was because these questions were completed by 7296 South Asians, whereas only 571 South Asians completed the question on special diets which had been part of the 24 h recall questionnaire, making use of the food categories from the touchscreen questionnaire a more reliable source for determining meat- and fish-eating status.
Statistical analysis
Within-cohort supplement use prevalence and vitamin D intake
Figures were created using GraphPad Prism version 7.02. All statistical analyses were conducted using the statistical software package IBM SPSS Statistics version 21, with independent t tests (for sex) or one-way ANOVA (for ethnicity), to assess group differences, unless otherwise stated. The χ 2 test was used to test for associations between usage of vitamin-D-containing supplements by sex and ethnicity. For vitamin D intake, we used non-parametric tests instead of log-transformed data due to potential loss of data from participants who had zero values, a valid intake for vitamin D. All other continuous variables were normally distributed and so did not require log transformation prior to parametric statistical analysis.
Previous studies have defined ‘vitamin-D-containing supplements’ as any supplement containing vitamin D, including combined calcium and vitamin D and multivitamin and mineral( Reference Black, Jacoby and Nowson 28 , Reference Black, Walton and Flynn 35 ), some also including fish-body oils and fish-liver oils( Reference Black, Walton and Flynn 35 ). However, due to the nature of the data available in the UK Biobank we did not include fish-body or fish-liver oil, and defined ‘vitamin-D-containing supplements’ as just multivitamin and mineral supplements and all single vitamin D supplements, assuming all multivitamin and mineral supplements to contain vitamin D. We did not include mineral-only supplements as these rarely contain vitamin D. See the online supplementary material, Supplemental File 1, for further information regarding the rationale for this decision.
Variables associated with supplement use
Logistic regression analysis was used to examine the association of sex, ethnicity and age with supplement usage (binary coded as vitamin-D-containing supplement user v. non-user; model 1). Next, BMI category was added to the model (model 2), followed by socio-economic factors (gross annual household income and geographical region) in model 3. Finally, in model 4, dietary variables were added (oily fish consumption and vegetarianism). As this was an exploratory analysis, model variables were chosen based on a confirmed difference between vitamin-D-containing supplement users and non-users, after Bonferroni adjustment for multiple testing (α=0·005; online supplementary material, Supplemental Table 1). See Supplemental File 1 for details of how categorical variables were recoded from those of the original Biobank data and how continuous variables were converted to categorical variables.
Due to the relatively large sample sizes, and the subsequent risk of the analyses being statistically overpowered, confidence intervals rather than P values were used wherever possible to assess statistical significance in the logistic regression models. It was planned that sub-analyses would be conducted for single vitamin D supplements and multivitamin and mineral supplements separately to see if the variables associated with usage varied by supplement sub-type.
Results
Participant characteristics
Mean age and BMI were similar in males and females (see online supplementary material, Supplemental Table 2), with both sexes on average being classified as overweight. South Asian-specific waist-to-hip ratio cut-off points (0·8 cm for women and 0·9 cm for men)( Reference Alberti, Zimmet and Shaw 36 ) classified both sexes as centrally obese. The three ethnic groups were similar in age, BMI and waist-to-hip ratio (Table 1), with all groups being obese on average (South Asian BMI cut-off used for obesity: ≥25 kg/m2)( Reference Bodicoat, Gray and Henson 37 ) and having a waist-to-hip ratio indicating central obesity. The following percentages of females and males respectively had a BMI of 26–29 kg/m2 (34 %, 41 %) or of ≥30 kg/m2 (30 %, 24 %). The following percentages of Bangladeshis, Indian and Pakistanis respectively had a BMI of 26–29 kg/m2 (39 %, 37 %, 39 %) or of ≥30 kg/m2 (19 %, 24 %, 35 %).
Table 1 Characteristics of 8024 South Asian UK Biobank participants by ethnic group: continuous data split by ethnic sub-group (Bangladeshi, Indian, Pakistani)
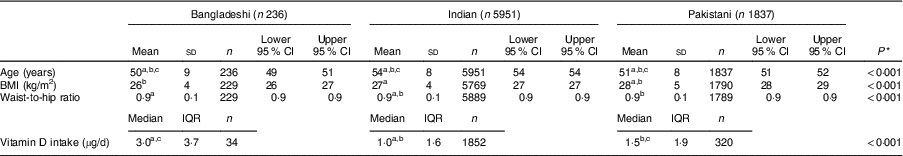
a,b,cValues within rows with like superscript letters were significantly different in post hoc tests (P<0·05).
* One-way ANOVA, except Kruskal–Wallis test (with Dunn’s multiple-comparison post hoc tests) for vitamin D intake.
See the online supplementary material, Supplemental File 2, for further details of participant characteristics by sex and ethnicity.
Characteristics by sex
Our analyses showed an association between sex and oily fish intake, with women being 1·5 times more likely to ‘never eat oily fish’ and half as likely to eat oily fish once or more daily than were men (P<0·001; online supplementary material, Supplemental Table 3). Women were also nearly twice as likely to be vegetarian (P<0·001). See the online supplementary material, Supplemental File 2, for further details of other participant characteristics by sex.
Characteristics by ethnicity
There was a higher proportion of females in the Indian group (49 %) than in the Bangladeshi (31 %) and Pakistani (39 %) groups (Table 2), which is important to bear in mind when interpreting the results between ethnic groups. Oily fish intake varied among the three ethnic groups (P<0·001), with 10 % of Bangladeshis (n 23) consuming oily fish daily compared with <1 % of Indians (n 17) and <1 % of Pakistanis (n 6). A higher proportion of Indians were vegetarians (30 %) compared with Bangladeshis and Pakistanis (<1 % vegetarian; P<0·001).
Table 2 Characteristics of 8024 South Asian UK Biobank participants by ethnic group: categorical data, split by ethnic subgroup (Bangladeshi, Indian, Pakistani)

* Based on χ 2 test.
Vitamin D intake and supplement use
There was little difference in vitamin D intake by sex, with a median (interquartile range) of 1·0 (1·6) and 1·2 (2·0) µg/d in females and males, respectively (Mann–Whitney U test, P=0·002, n 2206). However, vitamin D intake differed between the three ethnic groups (Kruskal–Wallis test, P<0·001, n 2206), with a median (interquartile range) of 3·0 (3·7), 1·0 (1·6) and 1·9 (2·0) µg/d in the Bangladeshi, Indian and Pakistani groups, respectively, and Dunn’s post hoc tests showing differences between all three groups (Table 1).
A χ 2 analysis showed that women were more likely to use a vitamin-D-containing supplement than were men (39 % usage in women v. 23 % usage in men; P<0·001, n 7553, Fig. 2). Persons of Indian ethnicity were more likely to use a vitamin-D-containing supplement than those of Bangladeshi and Pakistani ethnicity (P<0·001, n 7553, Fig. 2). Specifically, 22 % of Bangladeshi, 32 % of Indian and 25 % of Pakistani participants used a supplement containing vitamin D.

Fig. 2 Vitamin-D-containing supplement usage (![]() , vitamin D and multivitamin;
, vitamin D and multivitamin; ![]() , multivitamin;
, multivitamin; ![]() , single vitamin D supplement;
, single vitamin D supplement; ![]() , neither) by sex and ethnic group among 8024 South Asian UK Biobank participants. Women, and persons of Indian ethnicity, were more likely to use a vitamin-D-containing supplement than were men, and persons Bangladeshi and Pakistani ethnicity, respectively (χ
2 test, both P<0·001)
, neither) by sex and ethnic group among 8024 South Asian UK Biobank participants. Women, and persons of Indian ethnicity, were more likely to use a vitamin-D-containing supplement than were men, and persons Bangladeshi and Pakistani ethnicity, respectively (χ
2 test, both P<0·001)
Demographic, dietary and lifestyle factors associated with vitamin D containing supplement use
In our first model, which included sex, ethnicity and age variables (Table 3), sex had the strongest association with supplement use, with a 2·13 (95 % CI 1·93, 2·36) times higher odds in women than in men (reference category). Younger persons (40–59 years) had odds of supplement use of only 0·79 (95 % CI 0·71, 0·88) compared with those aged ≥60 years (reference category). Pakistanis (OR=0·77; 95 % CI 0·68, 0·87), but not Bangladeshis (OR=0·73; 95 % CI 0·52, 1·01), had lower supplement use than did Indians (reference category). When BMI was added to the model (model 2), BMI≤25·4 kg/m2 was associated with an increased odds of supplement use (1·25; 95 % CI 1·10, 1·43) compared with BMI>29.4 kg/m2 (reference category) and the odds for Pakistani (compared with Indian) was reduced in size (OR=0·80; 95 % CI 0·70, 0·90).
Table 3 Baseline odds of being a vitamin D supplement user (single vitamin D supplement, as part of multivitamin and mineral supplement, or both) among 8024 South Asian UK Biobank participants by demographic, dietary and anthropometric characteristics: logistic regression models 1 and 2
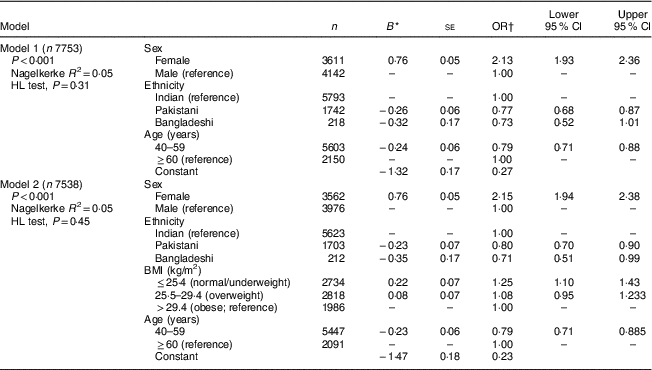
HL test, Hosmer–Lemeshow test for fit of data for model (null hypothesis=satisfactory fit).
* B=unstandardised coefficient.
† OR=odds of being a supplement user (v. non-supplement user, OR=1·00).
For model 3, when gross annual household income and region were added to model 2, sex and age were still associated variables, but the lower limit of the 95 % CI for BMI<25·4 kg/m2 (1·03) was now very close to the null (1·00) and Pakistani ethnicity did not now differ from Indian ethnicity (OR=0·95; 95 % CI 0·81, 1·11; Table 4). An income of <£18 000 per year was associated with a reduced odds of supplement use (OR=0·80; 95 % CI 0·67, 0·94) as compared with ≥£52000 (reference category). All geographical regions were associated with supplement use, having a lower odds of supplement use ranging from OR=0·52 (95 % CI 0·30, 0·90) to OR=0·76 (95 % CI 0·65, 0·89) compared with Greater London (reference category).
Table 4 Baseline odds of being a vitamin D supplement user (single vitamin D supplement, as part of multivitamin and mineral supplement, or both) among 8024 South Asian UK Biobank participants by demographic, dietary and anthropometric characteristics: logistic regression models 3 and 4

HL test, Hosmer–Lemeshow test for fit of data for model (null hypothesis=satisfactory fit).
* B=unstandardised coefficient.
† OR=odds of being a supplement user (v. non-supplement user, OR=1·00).
For model 4, vegetarianism and oily fish consumption were trialled, but the data fit was better with just oily fish consumption in the model (see online supplementary material, Supplemental File 2, for full details). Sex, region, household income and age had similar effect sizes to that previously, and oily fish consumption of less than once per week was associated with reduced odds of supplement use (OR=0·78; 95 % CI 0·63, 0·96) as compared with two or more times per week (reference), but the upper limit of the 95 % CI (0·96) was close to the null. See online supplementary material, Supplemental File 2, for further information on the final model as well as for the results of sub-analyses by vitamin-D-containing supplement type (Supplemental Table 4).
Discussion
There is currently little, if indeed any data on vitamin-D-containing supplement use and associated demographic, dietary and lifestyle factors in Western-dwelling South Asian populations. Our findings from this large research population of UK South Asians suggest that female sex, being over 60 years old and living in Greater London were associated with increased odds of using a supplement containing vitamin D. We also found borderline trends for a lower BMI, higher oily fish intake and higher household income being associated with higher likelihood of vitamin-D-containing supplement use.
Our findings support previous research in white Caucasian groups, showing female and older age being associated with supplement use( Reference Kofoed, Christensen and Dragsted 38 , Reference Li, Kaaks and Linseisen 39 ). These sex and age differences are perhaps not surprising considering vitamin D and calcium have been historically promoted more intensively to women than men, due to increased osteoporosis risk in women, and older age may intensify personal perception of increased osteoporosis or disease risk per se ( Reference Cline and Worley 40 ) relative to middle-aged persons.
Our finding that the majority of South Asians in the UK Biobank cohort do not use vitamin-D-containing supplements also supports previous studies in South Asians in other Western countries which have looked at cod-liver oil supplement use. For example, a study of Norway-dwelling South Asians by Holvik et al. found that 15 % of men and 15 % of women used cod-liver oil daily, with 58 % of men and 60 % of women not using cod-liver oil supplements( Reference Holvik, Meyer and Haug 18 ). Similarly, a study of Sri Lankans living in Norway found that 20 % took a cod-liver oil supplement daily( Reference Meyer, Holvik and Lofthus 41 ). A UK study which recorded vitamin D supplement use in South Asians (but did not assess predictors of usage) found that only 2–6 % of South Asian women used a vitamin D supplement at baseline( Reference Kift, Berry and Vail 21 ). In contrast, one study in Canada( Reference Ginter, Krithika and Gozdzik 42 ) found that only 17 % of South Asians did not take vitamin-D-containing supplements. The discrepancy between the latter study’s finding and that of our own, the other UK study and the two Norwegian studies is not easy to explain but could be due to the older age in the Canadian study (60–90 years)( Reference Ginter, Krithika and Gozdzik 42 ) compared with 30–60 years( Reference Holvik, Meyer and Haug 18 , Reference Meyer, Holvik and Lofthus 41 ) in the two Norwegian studies, 20–60 years in the other UK study( Reference Kift, Berry and Vail 21 ) and 40–69 years in the current study (UK Biobank).
Surprisingly, in the current study, South Asians in Greater London had a higher prevalence of vitamin-D-containing supplement use (35 %) than those in the other regions (18–28 %), who had lower odds of use by 28–54 %. This was despite the model controlling for sex, ethnicity, BMI, age, gross annual household income and oily fish consumption, which warrants further investigation.
We found a slightly higher usage of vitamin-D-containing supplements in Indians compared with Bangladeshis and Pakistanis. However, this association disappeared when controlling for sex and age in the regression models. On the other hand, there were clear differences in vitamin D intake by ethnicity, with Bangladeshis having on average a higher vitamin D intake (3·0 µg/d) than Indians (1·0 µg/d) and Pakistanis (1·5 µg/d). South Asians are particularly under-represented in UK-wide diet surveys so there is no national data with which to compare our findings, but our findings concur with a smaller UK cohort study reporting that South Asian women consume 1·6–2·2 µg of vitamin D daily( Reference Darling, Hart and Macdonald 9 ) from their diet (excluding supplements). These estimates are slightly lower than the NDNS average intake of 1·8–3·2 µg/d, based mainly on data from white Caucasians( Reference Whitton, Nicholson and Roberts 26 ).
The higher vitamin D intake in Bangladeshis is likely due to increased oily fish consumption relative to the other groups. Equally, the poor vitamin D intake in Indians is likely due to the high prevalence of vegetarianism in this group. Eggs, cereals and fortified spreads are other sources of vitamin D that may be relevant in this group, but these sources are lower in vitamin D content than oily fish. The numbers are generally too small in the Bangladeshi group to make definitive inferences, but it is noteworthy that only 10 % (n 22) of the Bangladeshi group ate oily fish daily. It is widely thought that this group is less vulnerable to vitamin D deficiency based on its traditional consumption of large amounts of oily fish. However, our findings support that of another UK research study which found that when food intake over the last 7 d was assessed, traditional dishes containing oily fish were consumed by only 7–50 % of Bangladeshi households( Reference Kassam-Khamis, Judd and Homas 43 ).
Importantly, the dietary vitamin D intakes of all three ethnic groups are very low and not sufficient to meet the SACN recommendation of 10 µg of vitamin D daily( 4 ). Therefore, there is a very urgent public health need to promote the use of vitamin-D-containing foods as well as supplements in South Asian populations.
To our knowledge, the present study is the first one ever to assess the demographic, dietary and lifestyle factors associated with vitamin D supplementation use among UK South Asians. In terms of internal validity, completion of the supplement use question was excellent with a 97 % completion rate in the 8024 South Asians, which supports the representativeness of our findings within the UK Biobank cohort.
We undertook a retrospective power calculation for our main predictive factor on supplement use: sex (exposure=sex, outcome=supplement use). We had 80 % power to observe an OR of 2·2, as 41 % of controls (non-supplement users) and 60 % of cases (supplement users) were female (exposed), and there was a ratio of controls to cases of 3·3. We had sufficient power as no OR for sex was larger than 2·2, except for the supplementary analysis for single vitamin D supplementation (excluding multivitamins) as seen in the online supplementary material, Supplemental Table 4.
Nevertheless, the study has a number of limitations which may affect its internal validity and warrant further discussion. First, due the wording of the supplement questions, we were not able to assess dosage or supplement brand, or season of supplement usage. The amount of vitamin D in both multivitamin and single vitamin supplements varies depending on brand used. For these reasons we were not able to assess the actual amount of vitamin D obtained from supplements in the current analysis. The 24 h dietary recall estimate did not include use of supplements, so actual vitamin D intakes were from diet only. Also, 24 h recall is not an ideal method for assessing vitamin D intake as many rich sources of vitamin D are often consumed only a few times per week (e.g. oily fish, eggs) and so may be missed if not consumed on the day of the recall.
Second, in terms of frequency of completion, only 18 % of the South Asian participants completed a 24 h dietary recall at least once, and thus had an estimate for vitamin D intake, with only 9 % completing a 24 h dietary recall more than once. This could be a source of bias as those who completed a higher number of recalls are likely to produce a more accurate estimate of vitamin D intake. Many participants did not have data for certain questions, excluding them from the modelling (see online supplementary material, Supplemental File 3, for details). Also, the questionnaire was designed for assessing a variety of nutrients, so may not give as accurate or valid estimate of vitamin D intake as would a questionnaire specific for vitamin D.
Third, not being able to include cod-liver oil consumption in the analysis, due to the relevant question only assessing fish oils in total (including n-3 supplements), may have led to a slight underestimation of vitamin-D-containing supplement use. Indeed, 13 % of the South Asians who said that they were not taking a single vitamin D supplement or multivitamin supplement reported that they used fish oils. It is unclear as to how many of these participants consumed cod-liver oil (containing vitamin D) and how many consumed other fish oil (e.g. n-3; not containing vitamin D). Similarly, 2 % of those who said they were not taking a single vitamin D supplement or multivitamin supplement reported that they took prescription medicines containing vitamin D. Therefore, actual vitamin-D-containing supplement use may be slightly underestimated in our analysis.
Fourth, due to a small sample size relative to the other ethnic groups, the results for the Bangladeshis (n 236) may lack robustness, particularly for vitamin D intake, whereby the number of Bangladeshis who completed at least one dietary recall was low (n 34; i.e. 14 % of original sample) compared with that of the Indians (31 %) and Pakistanis (17 %). Finally, some UK-wide representativeness may be lost due to the fact that about two-thirds of the South Asians came from four UK Biobank assessment centres (Leeds, Hounslow, Croydon and Birmingham).
Despite these limitations which may affect internal validity of the present study, it is still the largest analysis of its kind to date, providing us with the most comprehensive examination of vitamin D exposure through either dietary intake or vitamin-D-containing supplement usage in Western-dwelling South Asian populations. Importantly, 37 % of South Asians in our study live in areas below the UK census (2001) median Townsend Deprivation Index and 22 % live in the lowest (most deprived) quartile (http://census.ukdataservice.ac.uk/get-data/related/deprivation). This means that our study is likely to be more representative of the UK South Asian population, and have stronger external validity, than is the case in some other nutritional research and surveys in this population, which tend to include mostly South Asians of higher socio-economic status. However, as with all studies, external validity is still slightly limited by the fact that, as research participants, they may differ in some factors (e.g. health-consciousness) than the general South Asian population, and these data cannot be used to estimate formal prevalence rates of vitamin-D-containing supplement use. Further work is now planned to link the vitamin D intakes and supplement usage with measurements of 25(OH)D, which were not available at the time of the current analysis, in the South Asian subset of the UK Biobank cohort.
Conclusion
We have shown that vitamin D intakes in the UK Biobank South Asians were generally low but variable among South Asian sub-population groups, 1·0 to 3·0 µg/d, and not affected by sex. We have also demonstrated that being of female sex was associated with increased odds of vitamin-D-containing supplement use, as was being of younger age and living in Greater London. We found borderline trends for lower BMI, higher household income and higher oily fish consumption being associated with increased odds of using a supplement containing vitamin D.
These findings suggest that even in a research population, which is likely to be more health-conscious than the general population, current levels of vitamin-D-containing supplement use are very low and absolutely unlikely to be sufficient to ensure vitamin D sufficiency (≥50 nmol/l). There is a real need for development and implementation of public health strategies to promote the use of vitamin-D-containing foods as well as supplements among UK-dwelling South Asian populations, particularly in the light of the newly published UK vitamin D requirements( 4 ).
Acknowledgements
Acknowledgements: This research has been conducted using the UK Biobank Resource under application number 15168. Financial support: This work was supported by in-house funds from the University of Surrey for payment of the UK Biobank access fee. The UK Biobank was established by the Wellcome Trust medical charity, Medical Research Council, Department of Health, Scottish Government and Northwest Regional Development Agency. It has also had funding from the Welsh Assembly Government and the British Heart Foundation. UK Biobank is hosted by the University of Manchester and supported by the National Health Service (NHS). All the above funders had no role in the design, analysis or writing of the present article. Conflict of interest: S.A.L.-N. discloses that she is Research Director of D3-TEX Limited which holds the UK patent for the use of UVB-transparent clothing to prevent vitamin D deficiency, with a Gulf Corporation Council (GCC) patent pending. S.A.L.-N.’s husband, William Lanham-New, is Managing Director of D3-TEX Limited. S.A.L.-N. has received grants from: (i) the UK Biotechnology and Biological Sciences Research Council (BBSRC) (Project: Ergocalciferol (D2) v. Cholecalciferol (D3) Food Fortification: Comparative Efficiency in Raising 25OHD Status & Mechanisms of Action (D2-D3 Study), BB/I006192/1, £516823); (ii) the UK Food Standards Agency (Project: Vitamin D, Food Intake, Nutrition and Exposure to Sunlight in Southern England (D-FINES) Study, N05064, £600000); (iii) the European Union (Project: Food Based Solutions for Optimal Vitamin D Nutrition and Health Through the Life Cycle, Lead Work Package 4: Nutritional requirements for vitamin D during pregnancy, childhood and adolescence using RCTs, FP7-613977-ODIN, €6·2 million); and (iv) the UK Ministry of Defence (MoD, £2·4 million). S.A.L.-N. is a current member of SACN and a member of the panel that was responsible for the most recent revision of vitamin D recommended nutritional intake guidelines in the UK. She is a board member for the UK National Osteoporosis Society and the British Nutrition Foundation. She is Secretary of the Nutrition Society as well as Editor-in-Chief of the Nutrition Society textbook series. All other authors have no conflict of interest. Authorship: Author contributions were as follows. Formulating the research question(s): A.L.D., D.J.B., K.R.A., S.A.L.-N. Designing the study: A.L.D., D.J.B., K.R.A., S.A.L.-N. Data collection: not applicable. Analysing the data: A.L.D., D.J.B., K.R.A., S.A.L-.N. Writing the article: A.L.D., D.J.B., K.R.A., S.A.L.-N. Ethics of human subject participations: The UK Biobank study is conducted according to the guidelines laid down in the Declaration of Helsinki and all procedures involving human subjects were approved by the UK North West Multi-centre Research Ethics Committee (MREC) (application 11/NW/0382). Written informed consent was obtained from all subjects.
Supplementary material
To view supplementary material for this article, please visit https://doi.org/10.1017/S1368980018001404








