Poster Presentation - Poster Presentation
Diagnostic/Microbiology
Assessment of endotracheal aspirate culture appropriateness among adult ICU patients at an academic medical center
- Michael Chambers, Romney Humphries, Bryan Harris, Tom Talbot
-
- Published online by Cambridge University Press:
- 29 September 2023, p. s63
-
- Article
-
- You have access Access
- Open access
- Export citation
-
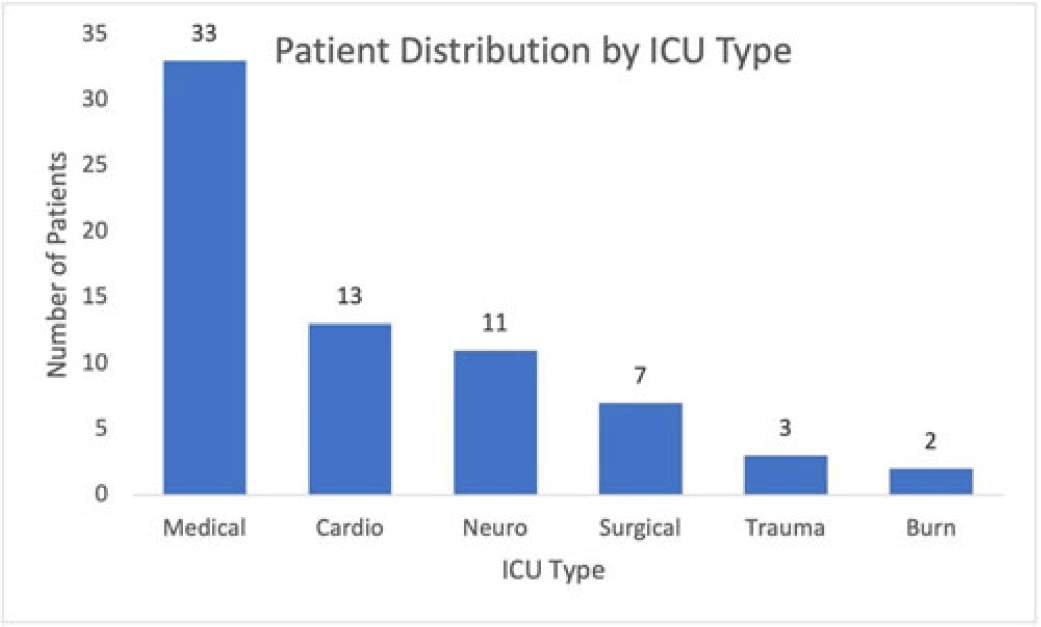
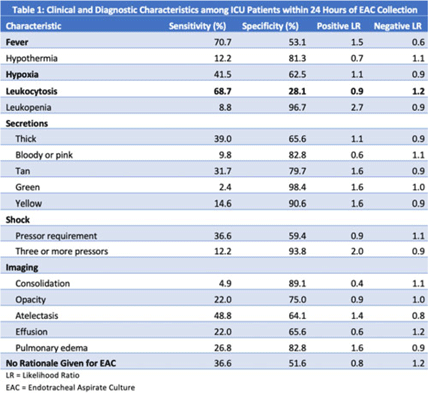
Background: Ventilator-associated pneumonia (VAP) is a significant cause of mortality in intensive care units (ICUs), but minimal research exists regarding the appropriateness of ordering endotracheal aspirate cultures (EACs). We evaluated the diagnostic utility of rationales given for EAC collection in ICUs at an academic medical center to assess potentially inappropriate EAC ordering. Methods: The study population comprised all adult patients admitted to an ICU in 2019 who underwent EAC collection. A random 10% sample from this population, stratified by ICU type, was selected. Clinical and diagnostic characteristics within 24 hours of EAC collection were identified by chart review. Clinical documentation was reviewed to identify ICU provider rationales for ordering EAC. Results: In total, 749 patients underwent EAC collection. Among them, 75 patients comprised the random sample, of whom 7 (9.3%) were excluded due to extubation before culture collection. Figure 1 shows patient distribution by ICU type. From these 68 patients, 105 EACs were collected. Of these, 41 (39%) were positive for potential pathogens, and 59 (56.2%) had explicit rationales for EAC collection, including fever (44.1%), hypoxia (18.6%), leukocytosis (16.9%), secretions (11.9%), shock (10.2%), and radiologic findings (8.5%). Also, 43.8% of EACs had no explicit rationale for collection. Table 1 shows sensitivities, specificities, positive likelihood ratios (LRs), and negative LRs for these rationales and related characteristics. Conclusions: EACs were commonly ordered without clear clinical indications. Of the noted rationales for EAC collections, most performed poorly at predicting positive cultures, which challenged common rationales for ordering EAC. This study could serve as a foundation for diagnostic stewardship interventions for EAC, potentially decreasing unnecessary cultures.
Disclosures: None
Dialysis
Developing a statewide infection prevention program assessment service for dialysis settings using a six-sigma framework
- Chelsea Ludington, Renee Brum
-
- Published online by Cambridge University Press:
- 29 September 2023, pp. s63-s64
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Due to the need for recurrent and direct access to the bloodstream, patients who require hemodialysis are at higher risk of developing healthcare-associated infections. Failure to assess gaps in systems and processes impedes the implementation of quality and performance improvement initiatives. In Michigan, there is no consultative service offered to dialysis units to assist with infection prevention practices, and no statewide dialysis data are being utilized. The Michigan Department of Health and Human Services developed a consultative, nonregulatory service dedicated to providing a comprehensive assessment of dialysis-based infection prevention programs. Methods: A multidisciplinary team created an infection prevention dialysis evaluation program using the six-sigma define–measure–analyze–design–verify model. These elements included content within the dialysis-specific Infection Control Assessment and Response (ICAR) Tool from the CDC with supporting program assessment items. From August 2021 through August 2022, the team completed 17 inpatient dialysis assessments within our cohort’s 17 hospitals. Data were analyzed using descriptive statistical analysis, and the final analysis included 1,086 observations from the developed assessment tool. Observations were grouped into 7 infection prevention categories: appropriate use of single and multiuse devices and supplies, aseptic technique, bloodborne pathogen prevention, cleaning and disinfection, hand hygiene, personal protection equipment (PPE) use, and storage of devices and supplies. Detailed summary reports were provided to the participating facilities after each site visit that included identified gaps, recommendations for improvement, and evidence-based resources. Results: Deficiencies were grouped into 7 major infection prevention categories among the 17 assessments, including cleaning and disinfection (n = 17, 100%), hand hygiene (n = 9, 53%), PPE use (n = 9, 53%), appropriate use of single and multiuse devices and supplies (n = 6, 35%), bloodborne pathogen prevention measures (n = 6, 35%), aseptic technique (n = 5, 29%), and storage of devices and supplies (n = 4, 24%). Conclusions: Our program’s prototype has been successful at detecting gaps in dialysis-based IP programs. By conducting data analyses of assessment findings, we have been able to assist the organization in establishing priorities for quality and performance improvement. Based on the results, comprehensive and robust systems to assess infection prevention programs, including those in dialysis settings, are necessary to enhance infection prevention operations across the continuum of care.
Disclosures: None
Characterization of negative health outcomes for dialysis events by vascular access type—Tennessee, 2015–2019
- Tara Suhs, Alex Kurutz, Christopher Wilson
-
- Published online by Cambridge University Press:
- 29 September 2023, p. s64
-
- Article
-
- You have access Access
- Open access
- Export citation
-
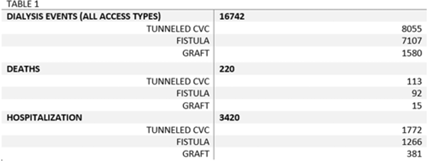
Background: The dialysis patient population is at a higher risk for nosocomial infections as well as related negative consequences including hospitalization and death. The CMS and the state of Tennessee mandate reporting of 3 types of dialysis events: positive blood culture, intravenous antimicrobial starts, and pus, redness, or increased swelling at the access site. We explored hospitalization and death outcomes by vascular access types for dialysis events reported to the NHSN for licensed outpatient hemodialysis clinics in Tennessee from 2015 to 2019. Methods: We looked at the frequency of hospitalization and death among those who experienced a dialysis event for 3 types of vascular access: arteriovenous fistula, arteriovenous graft, and tunneled central venous catheter (CVC). Other vascular-access types were excluded due to low usage rates. Odds ratios and confidence intervals were used to quantify the relationship between access type and hospitalization, and access type and death. Pooled analysis was used due to the stable rates of death and hospitalization among access types from 2015 to 2019. Results: From 2015 to 2019, 16,742 dialysis events were reported for the 3 access types: 8,055 dialysis events (48.1%) occurred among those with tunneled CVCs, 7,107 (42.5%) occurred among those with fistulas, and 1,580 (9.4%) occurred among those with grafts. Of the 16,742 dialysis events, 3,420 patients (20.4%) were hospitalized either due or related to their dialysis event; 220 (1.3%) deaths occurred either due to or related to the patient’s dialysis event. The odds of being hospitalized was 1.47 (95% CI, 1.29–1.67) times greater in those with grafts compared to those with fistulas. Patients with tunneled CVCs were 1.30 (95% CI, 1.20–1.41) times greater to be hospitalized compared to those with fistulas. The odds of death was 1.09 (95% CI, 0.9–2.5) times greater in those patient with tunneled CVCs compared to those with fistulas, whereas the odds of death among patients with grafts was 0.73 (95% CI, 0.82–1.43) times the odds of death compared to patients with fistulas. Conclusions: Overall, our findings conclude hemodialysis patients with tunneled CVCs have an increased risk for the negative health outcomes of hospitalization and death when compared to the other access types, supporting previous studies. Additionally, grafts had a higher risk of hospitalization compared to fistulas, but patients with grafts had lower odds of death than those with fistulas. Further investigation is needed to study how the COVID-19 pandemic may have affected the trends of negative health outcomes related to dialysis events.

Disclosures: None
Disinfection/Sterilization
Measuring the efficacy of routine disinfection methods on frequently used physical therapy equipment
- Aaron Barrett, Amanda Graves, Elaine De Jesus, Jennifer Edelschick, Diandrea McCotter, Deverick Anderson, Nicholas Turner, Bobby Warren
-
- Published online by Cambridge University Press:
- 29 September 2023, pp. s64-s65
-
- Article
-
- You have access Access
- Open access
- Export citation
-
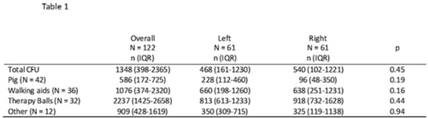
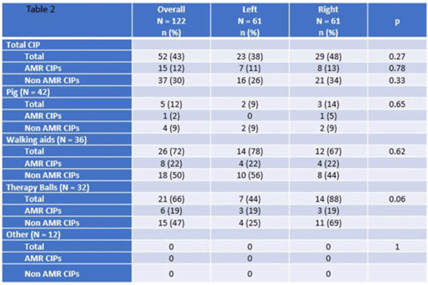
Background: Frequently used physical therapy (PT) equipment is notably difficult to disinfect due to equipment material and shape, however, the efficacy of standard disinfection of PT equipment is poorly understood. Methods: We completed a prospective observational microbiological analysis of fomites used in adult or pediatric PT at Duke University Health System, Durham, North Carolina, from September to December 2022. Predetermined study fomites were obtained after being used during a clinical shift and standard disinfection had been completed by clinical service staff. Fomites were split into 2 halves, left and right, for sampling. Samples were taken with premoistened cellulose sponges processed using the stomacher technique and were incubated on appropriate selective and general medias. We defined antimicrobial-resistant, clinically important pathogens (AMR-CIP) as MRSA, VRE, and MDR-gram-negative isolates, and non–AMR-CIP as MSSA, VSE, and gram-negative species. Study fomites were grouped as follows: (1) pediatric pig toy, (2) walking aids (walkers or canes), (3) balls (medicine, dodge, etc), and (4) other (foam roller, sliding board, etc). Results: In total, 47 patients, 61 fomites, and 122 were analyzed. Of the study patients, 24 (51%) were female, 13 (27%) had active infections, and 15 (32%) were on contact precautions. Because fomites were split in half, patients in the left and right study arms were identical. Overall, the median total colony-forming-units (CFU) of study fomites was 1,348 (IQR, 398–2,365): 468 (IQR, 161–1,230) for the left side study arm and 540 (IQR, 102–1,221) for the right study arm (P = .45). At the sample level, 52 (43%), 15 (12%), and 37 (30%) of 122 samples harbored any CIPs, AMR CIPs, or non-AMR CIPs, respectively. At the fomite level, 27 (44%), 5 (8%), 15(25%), and 7 (11%) of 61 fomites harbored any CIPs, only AMR-CIPs, only non-AMR CIPs, or both AMR and non-AMR CIPs, respectively. Generally, therapy balls were the most contaminated study fomites (n = 2,237; IQR, 1,425–2,658), and walking aids were most frequently contaminated with any CIPs (n = 26, 72%), AMR CIPs (n = 8, 22%), and non-AMR CIPs (n = 15, 47%). Discussion: Following routine disinfection, frequently used PT equipment remained heavily contaminated and harbored AMR and non-AMR CIPs, supporting the notion that PT equipment is difficult to disinfect via standard disinfection. Additionally, left-, and right-side fomite divisions had similar pathogens, suggesting that this sampling model of intrapatient comparisons may be helpful for resolving case-mix issues in future studies. Future work should focus on PT-specific enhanced disinfection strategies to improve the disinfection of PT equipment.
Financial support: This study was funded by PURioLABS.
Disclosures: None
Decontamination of bedding reduces the risk for contamination of personnel changing bedding: A simulation study
- Jennifer Cadnum, Andrew Osborne, Samir Memic, Curtis Donskey, Maria Torres-Teran
-
- Published online by Cambridge University Press:
- 29 September 2023, p. s65
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: The recent worldwide outbreak of Mpox virus infections has raised concern about the potential for nosocomial acquisition during handling of contaminated bedding or clothing. We conducted simulations to test the hypothesis that decontamination of bedding prior to handling could reduce the risk for contamination of personnel. Methods: We conducted a crossover trial to test the effectiveness of spraying contaminated bedding with a hydrogen peroxide disinfectant in reducing contamination of personnel during handling of the contaminated bedding. Bedding was contaminated on top and bottom surfaces with aerosolized bacteriophage MS2. Personnel (N = 10) wearing a cover gown and gloves removed the bedding from a patient bed and placed it into a hamper both with and without prior hydrogen peroxide spray decontamination. After handling the bedding, samples were collected to assess viral contamination of gloves, cover gown, neck or chest, and hands or wrists. Results: Contamination of the gloves and cover gown of personnel occurred frequently during handling of bedding and 20% of participants had contamination of their hands or wrists and neck after the simulation (Fig.). Decontamination of the bedding reduced contamination of the gloves and eliminated contamination of the cover gown, hands or wrists, or neck. Conclusion: Decontamination of bedding prior to handling could be an effective strategy to reduce the risk for nosocomial acquisition of Mpox by healthcare personnel.
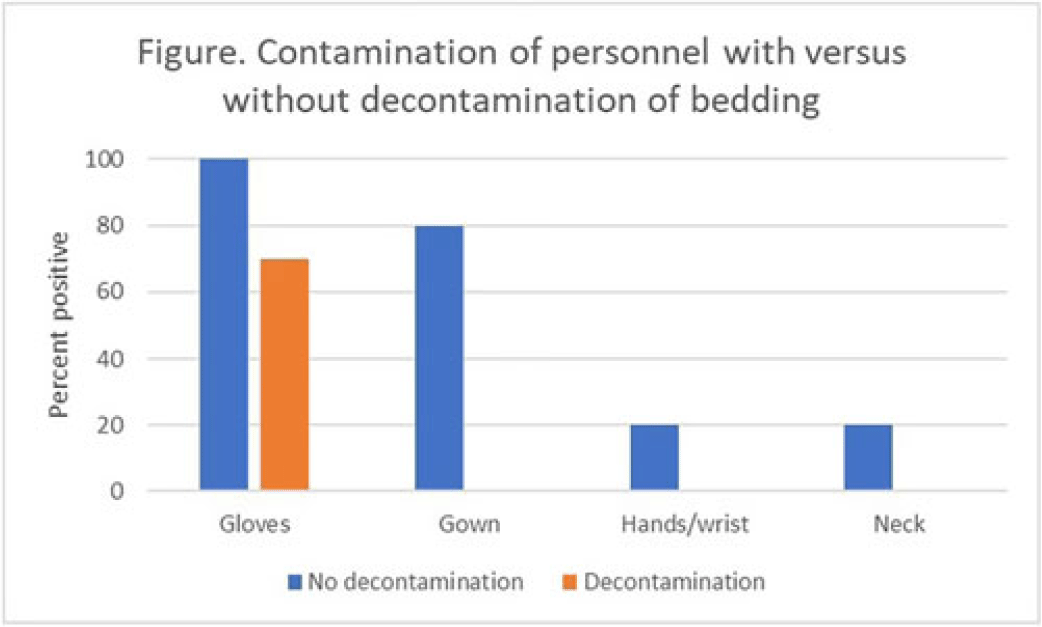
Disclosures: None
Emerging Pathogens
Healthcare personnel with laboratory-confirmed mpox in California
- Allison Bailey, Jane Siegel, Shua Chai, David Bui, Robert Snyder, Linda Lewis, Kayla Saadeh, J.B. Bertumen, Erin Epson
-
- Published online by Cambridge University Press:
- 29 September 2023, pp. s65-s66
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Objectives: Few reports have been published about the transmission of mpox in healthcare settings. During the 2022 multinational outbreak, the California Department of Public Health (CDPH) conducted a systematic review of healthcare personnel (HCP) with mpox, including their community and occupational exposures, to understand the transmission risk in healthcare settings. We also sought to inform return-to-work protocols by describing the frequency of HCP working while symptomatic for mpox and identifying occurrences of secondary transmission from infected HCP to patients. Methods: We analyzed surveillance data for laboratory-confirmed mpox cases in California with symptom onset from May 17 to September 30, 2022, collected by investigators at local health departments and reported to the CDPH. The reported data were supplemented by review of free-text variables, interview notes, and other files uploaded to state and county disease surveillance data registries. We identified HCP as all persons working in healthcare settings with potential for direct or indirect exposure to patients or infectious materials, including clinical and nonclinical staff but excluding remote workers. Results: The CDPH received reports of 3,176 mpox cases during the study period: 109 were HCP. Of the 109 HCP identified from 19 counties, 78 (72%) were aged 30–49 years, 102 (94%) were male, and 43 (39%) were Hispanic or Latino. Also, 29 HCP (27%) had received at least 1 dose of the JYNNEOS vaccine. Occupations requiring frequent physical interactions with patients were reported for 66 individuals (61%). During interviews with local health department investigators, nearly all HCP (n = 98, 90%) reported potential or confirmed sources of community exposure; 1 had confirmed occupational exposure with symptom onset 9 days after a sharps injury acquired during collection of an mpox specimen for testing. Of the 60 HCP who provided information about the days they worked, 35 (58%) worked while symptomatic, for a mean of 3.14 days (median, 2; IQR, 3). Also, 2 HCP worked for 12 days after symptom onset. No secondary cases of mpox were associated with HCP reported to the CDPH. Conclusions: This analysis suggests that HCP are more likely to be exposed to mpox in community settings than healthcare settings. The findings support recommendations against sharps use for mpox specimen collection. Although transmission between symptomatic HCP and patients was not reported, HCP can decrease opportunities for mpox transmission by closely monitoring themselves for symptoms after potential exposures and staying home from work if symptoms develop.
Disclosures: None
Genetic relatedness among Neisseria gonorrhoeae isolates in southeastern Michigan
- Anita Shallal, Robert Tibbets, Katherine Gurdziel, Dora Vager, Marcus Zervos, Geehan Suleyman
-
- Published online by Cambridge University Press:
- 29 September 2023, pp. s66-s67
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Antimicrobial resistance (AMR) in Neisseria gonorrhoeae (NG) is an emerging public health crisis. Whole-genome sequencing (WGS) is an efficient way of predicting AMR determinants and their spread in the population. In a previous study, genotype–phenotype correlation analyses among NG isolates to determine antimicrobial resistance revealed discordance for azithromycin (AZM) and ceftriaxone (CRO) compared to other antibiotics. We investigated the evolutionary relatedness of NG isolated from patients with sexually transmitted infection (STI) using WGS in southeastern Michigan. Methods: Isolates, corresponding demographic data, and minimum inhibitory concentrations (MIC) via E-test (CRO) and broth microdilution (AZM) were obtained from the Michigan Department of Health and Human Services. Whole-genome libraries were prepared using the QIAseq FX kit followed by sequencing on a NovaSeq6000 (>200X Coverage); samples were aligned to NG reference strain TUM19854 (NZ_AP023069.1) using Snippy before phylogenetic tree generation using Neighbor-joining clustering on the core.aln files. Phylogenetic trees were visualized using ATGC:PRESTO. Results: In total, 38 isolates were analyzed. Demographic data and susceptibility testing results are noted in Table 1. Most isolates were from males (63%), Blacks (44.7%), individuals living in Detroit City proper (47.3%), and those with unknown HIV status (55.2%). More than one-third had prior STI, including NG. All isolates were susceptible to CRO (CLSI susceptible breakpoint MIC, 1). Within the phylogenetic tree, 8 main branches were identified (Fig. 1). Moreover, 1 branch contained a cluster with 12 closely related isolates, which included the 9 isolates with nonsusceptible AZM. Nearly all isolates in that cluster had been collected from Detroit City proper and Wayne County, suggesting epidemiological overlap and potential spread of resistant strains in those counties.
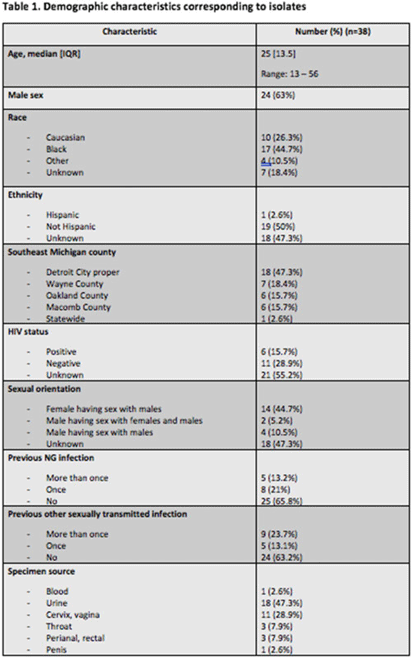
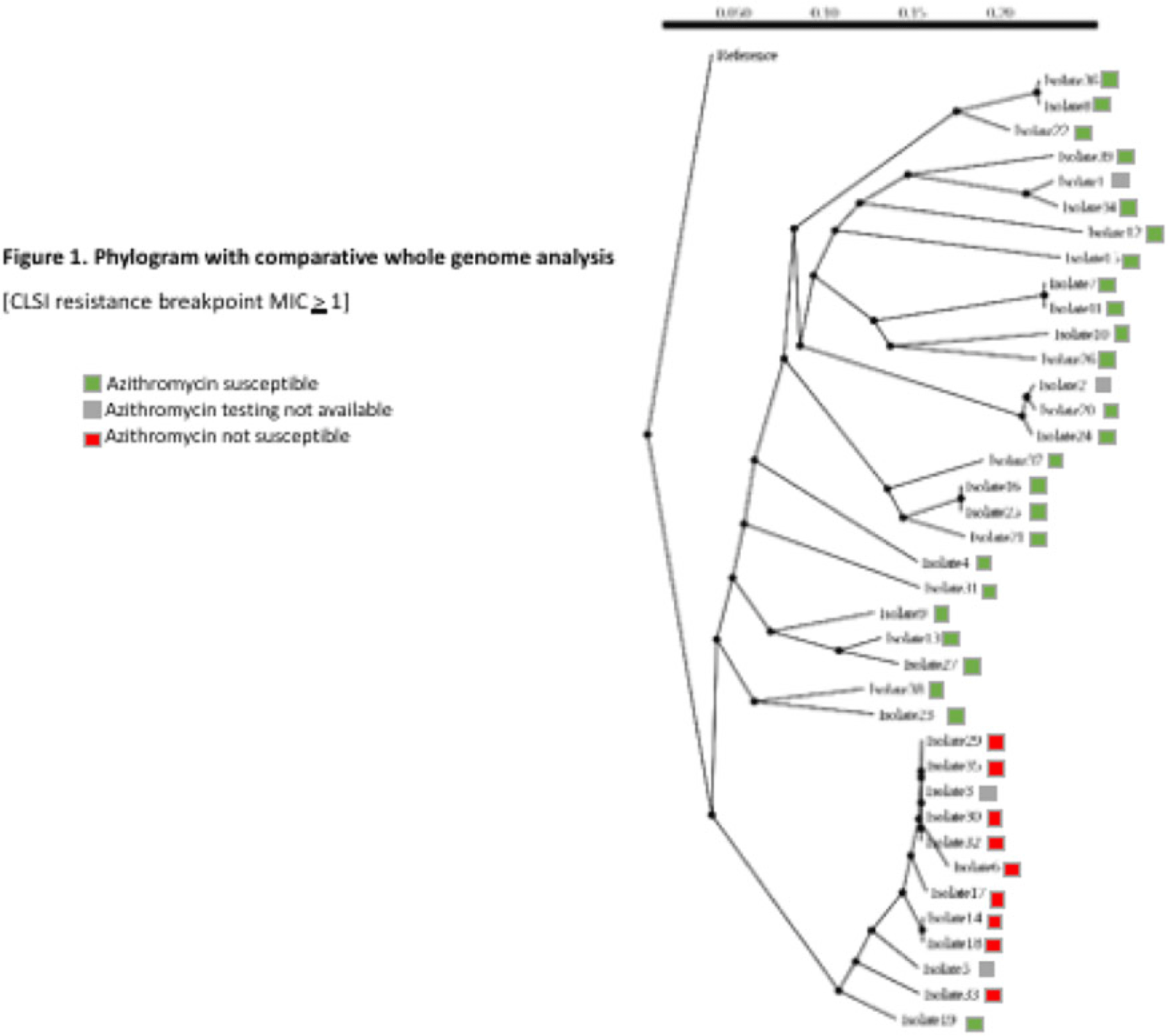 Conclusions: Comparative whole-genome and phylogenetic analyses among a subset of NG isolates revealed clustering of AZM resistance strains, suggesting a genomic component to AMR. Further studies are needed to determine the utility of WGS in diagnosis, outbreak investigations, and management of NG infections.
Conclusions: Comparative whole-genome and phylogenetic analyses among a subset of NG isolates revealed clustering of AZM resistance strains, suggesting a genomic component to AMR. Further studies are needed to determine the utility of WGS in diagnosis, outbreak investigations, and management of NG infections.Disclosures: None
Mpox exposure on a congregate inpatient psychiatry unit: Description of the investigation and outcomes—New York City, 2022
- Waleed Malik, Justin Chan, Simon Dosovitz, Clyde Gilmore, Jeanne Cosico
-
- Published online by Cambridge University Press:
- 29 September 2023, p. s67
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: In May 2022, New York City (NYC) experienced a large outbreak of human mpox (clade IIb). Data on mpox transmission following exposure in healthcare facilities in nonendemic settings are limited. Because mpox was previously not seen in NYC, our healthcare staff may not always recognize a suspected case and therefore may neglect to implement timely infection prevention and control measures, leading to infectious exposures. The risk of transmission from unrecognized mpox may be higher in inpatient psychiatric units where direct physical contact is more common in the setting of common spaces for patients. In July 2022, a patient was admitted to NYC Health + Hospitals–Bellevue (Bellevue) psychiatry with signs and symptoms of mpox that were not recognized for 4 days, at which point the patient was tested for mpox and was isolated. We describe the investigation of staff and patients exposed during the 4 days prior to diagnosis and isolation of the index patient, and we report on the outcome mpox infection among those exposed. Methods: This study was a retrospective chart review of adult patients admitted to and staff working on an inpatient psychiatric unit where the patient with mpox was admitted to Bellevue, the largest municipal hospital in NYC. Each individual was classified regarding degree of exposure, based on criteria from the CDC, and was offered postexposure mpox vaccination where indicated. We describe the nature of contact with the patient for those with high-risk exposures. The outcome of interest was development of mpox infection during 21 days after last exposure. Results: In total, 29 patients and 84 staff members were identified to have been on the psychiatric unit prior to isolation of the index case of mpox. All exposed individuals were monitored for signs and symptoms of mpox for 21 days after last exposure. The exposed and unexposed patients were kept apart in the psychiatric unit. All patients who had contact were classified as having a low-to-intermediate risk exposure. Among 23 staff members exposed, 8 had high-risk exposures, 4 had intermediate-risk exposures, and 11 had low-risk exposures. Those with high-risk exposures were offered Jynneos as postexposure vaccination, but they declined. None of the exposed staff or patients developed mpox during the follow-up period. Conclusions: Mpox transmission was not observed despite several exposures in a congregate psychiatry unit. Given limited data, further studies are needed to better understand transmission risk in congregate healthcare settings.
Disclosures: None
Environmental Cleaning
Effect of dry hydrogen peroxide on Candida auris environmental contamination
- Jennifer Sanguinet, Gerard Marshall, Julia Moody, Kenneth Sands
-
- Published online by Cambridge University Press:
- 29 September 2023, pp. s67-s68
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Candida auris is an emerging pathogen that exhibits broad antimicrobial resistance and causes highly morbid infections. Prolonged survival on surfaces has been demonstrated, and standard disinfectants may not achieve adequate disinfection. Persistent patient colonization and constant environmental recontamination poses an infection risk that may be mitigated by no touch disinfection systems. We evaluated the efficacy of continuous dry hydrogen peroxide (DHP) exposure on C. auris environmental contamination. Methods: The study was conducted in a large tertiary-care center where multiple patients were identified as either infected or colonized with C. auris. DHP-emitting systems were installed in the ventilation systems dedicated to the adult burn intensive care and children’s cardiac intensive care units. Composite surface samples were collected in a sample of patient rooms and shared clinical workspaces among units with current C. auris patients, before and after installation of the DHP system, and from areas with and without exposure to DHP. The samples included “high touch” surfaces near the patient, the general area of the patient room, shared medical equipment for the unit, shared staff work areas, and equipment dedicated to individual staff members (Table 1). Presence of C. auris was determined by polymerase chain reaction (PCR). Association between DHP exposure and C. auris contamination was determined using the Fisher exact test. Results: In the presence of C. auris patients, 5 baseline samples per unit were taken before DHP was installed, and then 5 samples per unit were taken on days 7, 14, and 28 after installation. Prior to initiation of DHP, 7 (70%) of 10 samples were PCR positive for C. auris. After DHP installation, a statistically significant decrease to 5 (16.7%) of 30 samples (P <.05) was observed. In total, 20 samples (5 before installation and 15 after installation) were collected from units without DHP on the same days. At baseline, 2 (40%) of 5 samples were PCR positive for C. auris. During subsequent periods, 4 (27%) 15 samples were positive (P = .66). No adverse effects were reported by patients, visitors, or personnel in association with the operation of the DHP systems. Conclusions: These findings suggest that DHP is effective in reducing surface C. auris contamination in a variety of patient and healthcare worker surfaces.
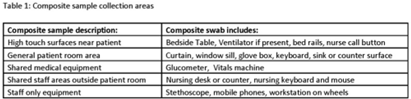
Disclosures: None
Environmental cleaning in operating rooms: A systematic review from the human factors engineering perspective
- Anping Xie, Hugo Sax, Oluseyi Daodu, Lamia Alam, Marium Sultan, Clare Rock, Shawna Perry, Ayse Gurses
-
- Published online by Cambridge University Press:
- 29 September 2023, pp. s68-s70
-
- Article
-
- You have access Access
- Open access
- Export citation
-
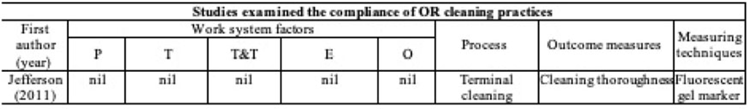
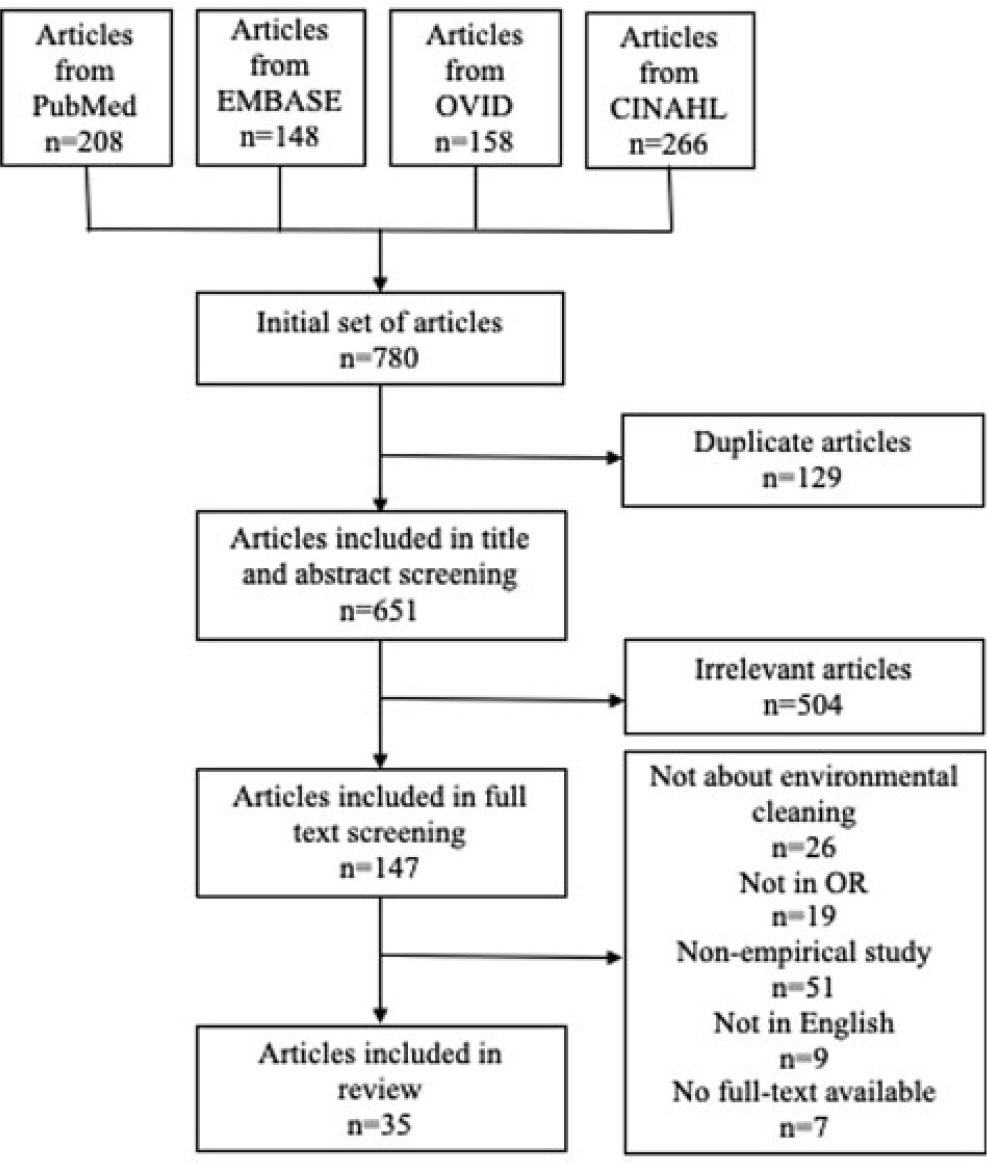
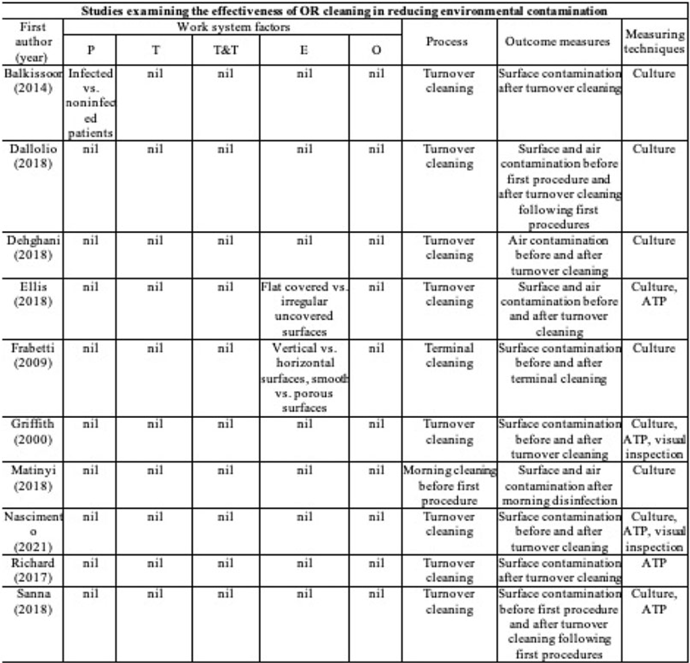
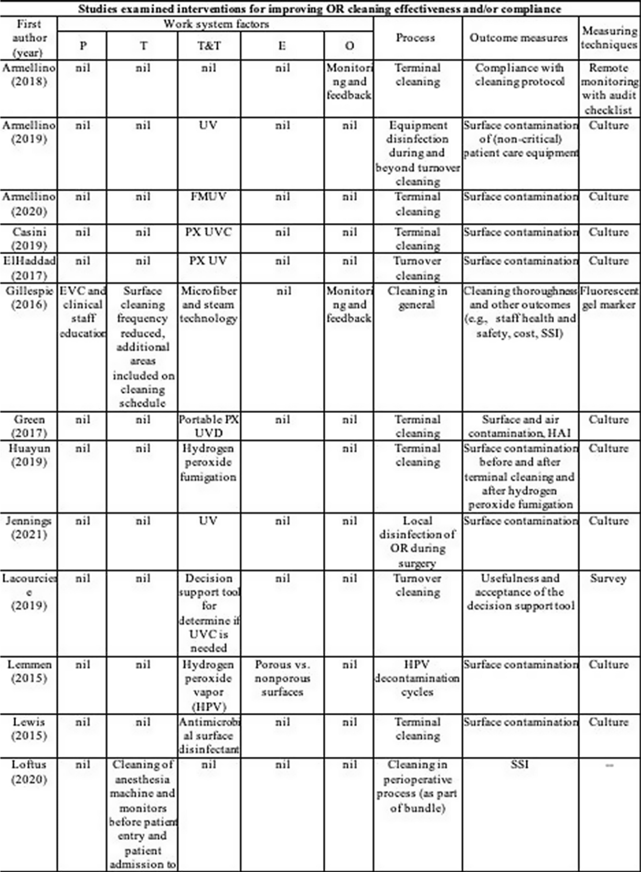
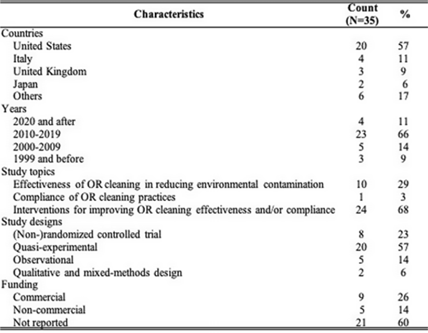
Background: Environmental cleaning is critical in preventing pathogen transmission and potential consecutive healthcare-acquired infections. In operating rooms (ORs), multiple invasive procedures increase the infectious risk for patients, making proper cleaning and disinfection of environmental surfaces of paramount importance. A human-factors engineering (HFE) approach emphasizing the impact of the entire work system on care processes and outcomes has been proposed to improve environmental cleaning. Using the lens of this HFE approach, we conducted a systematic review to synthesize existing evidence and identify gaps in the literature on OR cleaning. Methods: The systematic review was guided by the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines and limited to English-written, peer-reviewed journal articles reporting empirical studies on OR cleaning. Figure 1 shows the flowchart of study search and screening. The following data were extracted from each included article: (1) general information of the article (eg, first author, title, journal, year of publication) and (2) characteristics of the study (eg, country, objectives, design, outcome measures and measuring techniques, findings, funding source). In addition, work-system elements (eg, people, tasks, tools and technologies, physical environment, organizational conditions) and cleaning processes (eg, turnover cleaning, terminal cleaning) addressed in each included studywere coded based on the Systems Engineering Initiative for Patient Safety (SEIPS) model. The methodological quality of included studies using a (non)randomized controlled design was assessed using the version 2 of the Cochrane risk-of-bias tool for randomized trials. Results: In total, 35 studies were included in this review, among which 10 examined the effectiveness of OR cleaning in reducing environmental contamination (Fig. 2), 1 examined the compliance of OR cleaning practices (Fig. 3), and 24 examined interventions for improving OR cleaning effectiveness and/or compliance (Fig. 4). Figure 5 summarizes the characteristics of the included studies. Conclusions: In this review, OR cleaning was inconsistently performed in practice, and mixed findings were reported regarding the effectiveness of OR cleaning in reducing environmental contamination. No study has systematically examined work-system factors influencing OR cleaning. Efforts to improve OR cleaning focused on cleaning tools and technologies (eg, ultraviolet light) and staff monitoring and training. Interventions targeting the broader work system influencing the cleaning processes are lacking. The scientific rigor of the included studies was modest. Most studies were either commercially funded or did not reveal their funding sources, which might introduce a desirability bias.
Financial support: This study was funded by the Centers for Disease Control and Prevention.

Disclosures: None
Some like it hot: Variable impact of a tailpiece heating device on different gram-negative bacteria
- Stacy Park, Shireen Kotay, Katie Barry, Joanne Carroll, April Attai, William Guilford, Amy Mathers
-
- Published online by Cambridge University Press:
- 29 September 2023, p. s70
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Transmission of multidrug-resistant bacteria to patients from colonized hospital sink drains has prompted attempts to interrupt transmission through a variety of interventions directed at the wastewater environment. We previously found that use of a heating device designed to disrupt biofilm formation between the P trap and the sink drain, which is the major point of dispersal of bacteria to the patient-care environment, was associated with reduced risk of detectable gram-negative organisms on hospital sink drains. However, there was no observed effect on some important pathogens, including Pseudomonas aeruginosa and Stenotrophomonas maltophilia. We hypothesized that heating to a higher temperature would provide additional efficacy in preventing drain colonization. Methods: As part of a previous randomized study, 54 tailpiece heaters were installed in 3 intensive care units in an academic hospital and 2 acute-care units in an associated regional hospital; half of these devices were shams (ie, no heat). The devices were programmed to heat for 1 hour every fourth hour. Prior to this study, a device update increased the heating temperature (during the previous study the median heated temperature was 65.9°C). Sink drains and P traps were sampled monthly. Samples were assessed for semiquantitative growth of gram-negative bacteria on MacConkey agar, looking especially for P. aeruginosa and S. maltophilia. Frontline personnel were blinded to device assignment. Results: The mean heated temperature reached was 74.4°C. Based on proportional odds logistic regression (wherein the odds ratio reflects the likelihood of a given sample falling in a lower microbiologic burden level versus the levels above it), the heating device was associated with increased likelihood of lower microbiologic burden at the drain level for general growth on MacConkey agar (OR, 2.47; 95% CI, 1.11–5.51) and for growth of S. maltophilia (OR, 5.39; 95% CI, 2.20–13.18). The device did not have an effect on burden of Enterobacterales (OR, 1.38; 95% CI, 0.58–3.24). For P. aeruginosa, there was a trend toward decreased likelihood of lower microbiologic burden (OR, 0.41; 95% CI, 0.18–1.07) that did not reach statistical significance at the drain level, and the heating device was associated with decreased likelihood of lower microbiologic burden of P. aeruginosa at the P-trap level (OR, 0.20; 95% CI, 0.10–0.39). Conclusions: Heat disruption of biofilm between the P trap and sink may be a promising strategy for prevention of hospital sink drain colonization; however, the impact is variable across different bacterial species. Further understanding of the dynamics of the microbiome within wastewater is needed.
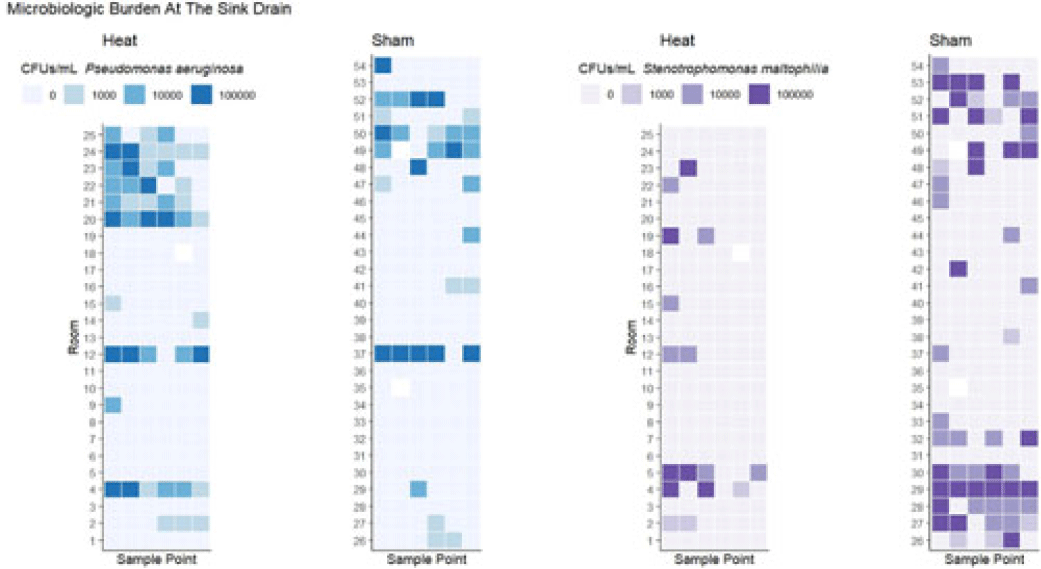
Disclosures: None
Hand Hygiene
Measuring hand hygiene opportunities per hour across two neonatal intensive care units
- Eugene Lee, Souad Al-Muthree, Paige Reason, Meghan Donohue, Michael Dunn, Meghan Statchuk, Sarah Khan, Shikha Gupta-Bhatnagar, Salhab El-Helou, Jerome Leis, Dominik Mertz
-
- Published online by Cambridge University Press:
- 29 September 2023, pp. s70-s71
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: To estimate hand hygiene compliance using electronic hand hygiene monitoring, the number of hand hygiene opportunities (HHOs) per period must be known in a given setting. Data on the number of HHOs in a neonatal ICU (NICU) are limited. We measured HHOs per hour and identified factors that may influence the number of HHOs per hour to calibrate compliance estimates for electronic hand hygiene monitoring. Methods: The study was conducted in 2 large NICUs in Ontario, Canada (72 and 42 beds, respectively). We centrally trained observers to identify HHOs using the Ontario-based “Four Moments of Hand Hygiene,” which is similar to combining moments 4 and 5 of the WHO “Five Moments of Hand Hygiene.” To apply the moments of hand hygiene to the NICU setting, the following modifications were made: moment 1 was entering the incubator or contact with anything within the ‘baby space’ directly around the incubator, and moment 4 was when hands exited the incubator and, as such, the ‘baby space.’ Using a standardized tool, the investigators conducted direct observation of HHOs during randomized observation periods from July 1, 2022, to January 9, 2023. In addition to HHOs, data on covariables potentially associated with the frequency of HHOs were collected: time and day of the week, acuity, additional precautions, corrected gestational age, and private versus multibed room or open pod. Results: We audited HHOs for 146 hours including 26 at site A and 120 at site B. Overall, 804 HHOs (69.2%) occurred during weekdays and 739 (63.6%) occurred during day shifts from 7:00 a.m. to7:00 p.m. The most frequent moments of hand hygiene were moment 1 (47.8%, before contact) and moment 4 (36.8%, after contact). The average numbers of HHOs were 7.8 per hour overall, 7.6 per hour on weekdays, 7.7 per hour on weekends, 8.8 per hour on day shifts, and 6.8 per hour on night shifts. The breakdown of HHOs by profession was 92.8% nurses, 0.6% physicians, 4.5% allied health, and 2.1% for others. Discussion: The rate of HHOs in NICU varied over a 24-hour period and was similar between 2 different NICUs. Evenings and weekends had considerably fewer average HHOs, and peaks were observed following nursing shift changes. The rate of HHOs may be influenced by other factors including unit design, patient acuity, and use of transmission-based precautions. Further analysis using a Poisson regression model will help to explore these factors and to calibrate electronic monitoring for this population.
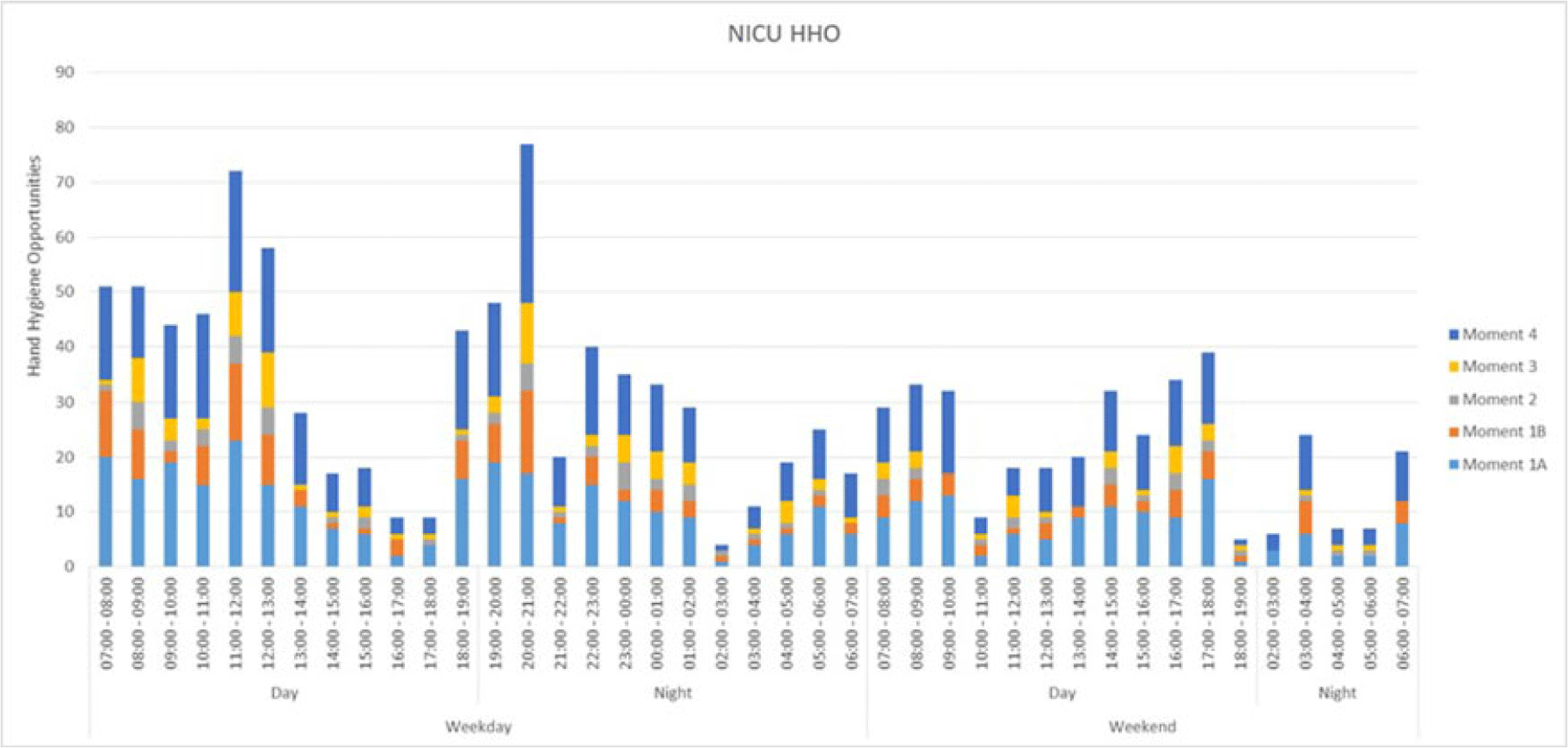
Disclosures: None
Functional dependence as a contributing factor for patient hand contamination by multidrug-resistant organisms in acute care
- Trenton Behunin, Julia Mantey, Marco Cassone, Lona Mody
-
- Published online by Cambridge University Press:
- 29 September 2023, pp. s71-s72
-
- Article
-
- You have access Access
- Open access
- Export citation
-
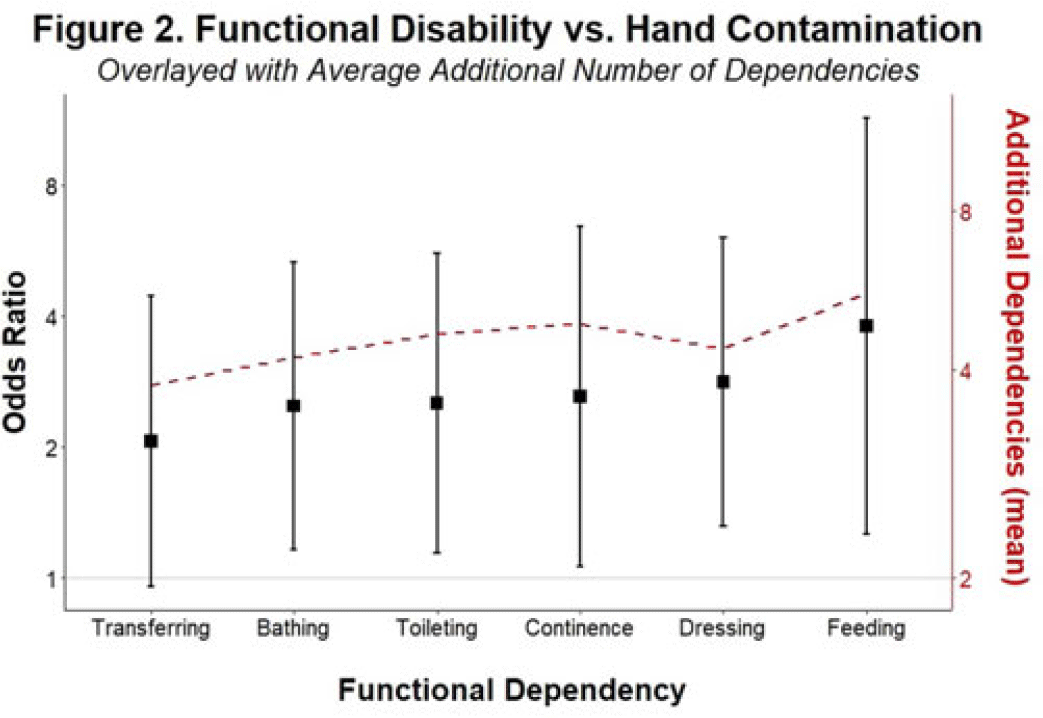
Background and objectives: Patients with functional disabilities are at higher risk of adverse outcomes, including infections. Although healthcare worker hand contamination has long been recognized as an important source of pathogen acquisition, the role of patient hands has been less clearly defined. We sought to determine whether the presence of functional disabilities is correlated with patient hand contamination by multidrug-resistant organisms (MDROs) and thus a potential target for patient hand hygiene (PHH) interventions. Methods: Case–control study of hand contamination with methicillin-resistant S. aureus, vancomycin-resistant enterococci, and gram-negative bacilli resistant to cephalosporins, fluoroquinolones, and/or carbapenems in 2 acute-care hospitals in southeastern Michigan. Cases (n = 40) and controls (n = 359) were defined as patients with or without hand contamination by MDROs, respectively. We assigned 3 exposure categories based on Katz activities of daily living scores: no functional disabilities (independent, reference group), 1–3 functional disabilities (partially dependent), and 4+ functional disabilities (dependent). We used stepwise logistic regression to identify confounding variables. Logistic regression was then used to establish the relationship between a patient’s functional dependence level and their hand contamination by MDROs. Results: The distribution of hand contamination of each target MDRO by level of patient dependence is shown in the Table. Overall, methicillin-resistant Staphylococcus aureus (MRSA) was the most represented, followed by resistant gram-negatives and vancomycin-resistant enterococci (VRE). Hospital site, sex, and history of MDROs were included in the model based on stepwise regression. The odds ratio (OR) of MRSA hand contamination in the dependent category was 3.19 (95% CI, 1.18–5.54) compared to the independent category, and for any MDRO the OR was 2.77 (95% CI, 1.22–6.32) (Fig. 1). The OR of MRSA hand contamination in the partially dependent category was 1.38 (95% CI, 0.27–7.07) compared to the independent group, and for any MDRO the OR was 0.86 (95% CI, 0.24–3.10) (Fig. 1). Feeding dependence had the highest single association with hand contamination (OR, 3.79, 95% CI, 1.26–11.43), with dressing dependence having the second highest association with hand contamination (OR, 2.82; 95% CI, 1.31–6.05) (Fig. 2). Conclusions: Patients with more functional dependencies were more likely to have MDRO hand contamination. This finding suggests a need for targeted PHH interventions in patients with functional disabilities to help prevent the spread of MDROs in the acute-care setting.
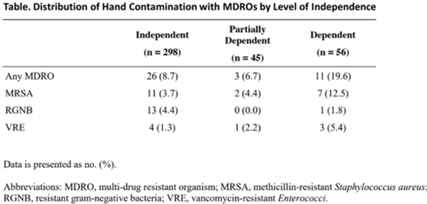
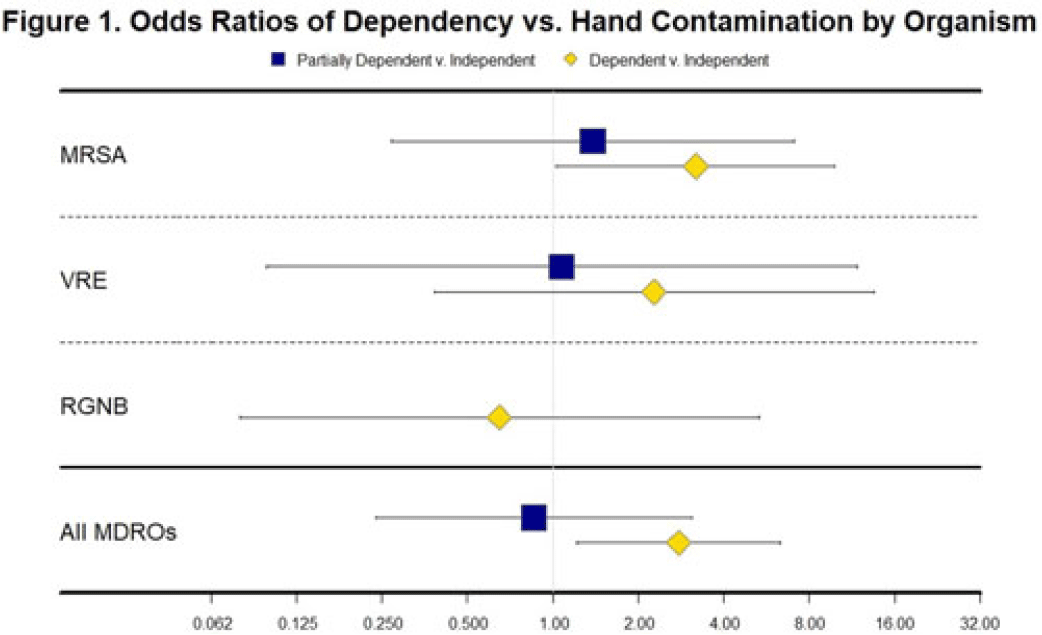
Disclosures: None
Addressing frontline healthcare worker perspectives on hand-hygiene monitoring badges
- Tucker Smith, Olivia Hess, Rachel Pryor, Michelle Doll, Gonzalo Bearman
-
- Published online by Cambridge University Press:
- 29 September 2023, p. s72
-
- Article
-
- You have access Access
- Open access
- Export citation
-
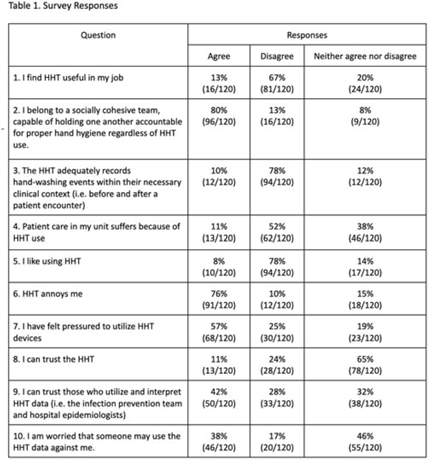
Background: Hand-hygiene technology (HHT) intends to monitor and promote hand washing by healthcare workers, a critical measure of infection control. Healthcare worker noncompliance with HHT is a major limitation to its implementation and utility in clinical settings. We assessed perspectives on HHT in an academic hospital system. Methods: Hand-hygiene team members created an anonymous, 37-question, Likert-scale survey to assess healthcare worker attitudes toward HHT. Surveys targeted nursing staff, advanced practice providers, care partners, and internal medicine physicians. Clinical coordinators from 5 distinct nursing units and 1 physician department emailed surveys to eligible employees. Research coordinators and clinical coordinators also posted a QR code for survey fliers at nursing stations. Results: Overall, 120 surveys were completed. Most surveys were completed by nurses and physicians (66.4% and 14.0%). Most respondents (67.5%) do not find HHT useful. Additionally, 78.3% of respondents believe that HHT does not accurately record hand-washing events. Most (78.3%) do not like using HHT, and 75.8% find it annoying. Only 10.8% believe that patient care suffers because of HHT. Conclusions: Most healthcare workers dislike the HHT badges, primarily due to perceived inaccuracies, lack of utility, burden of use, and pressure to comply. Distrust and effect on patient care do not appear to be substantial factors contributing to negative perceptions of HHT. Weaknesses of the study include overrepresentation of nursing staff and potential bias because respondents may have provided exceptionally negative responses believing it could lead to the removal of HHT.
Disclosures: None
Longitudinal effects of direct observation of hand hygiene practices and monitoring of alcohol-based handrub consumption
- Retsu Fujita, Rika Yoshida, Satoshi Hori
-
- Published online by Cambridge University Press:
- 29 September 2023, pp. s72-s73
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: In healthcare facilities, hand hygiene is important for infection control. The WHO recommends monitoring the consumption of alcohol-based handrub (ABHR) and direct observation of hand hygiene practices to ensure compliance with hand hygiene practices. Monitoring of ABHR is widely used, but direct observation is not widely performed, particularly in small facilities and non–acute-care facilities. We evaluated the effects of direct observation of hand hygiene practices and monitoring of ABHR consumption, with feedback to staff, on ABHR consumption and hand hygiene compliance. Methods: We conducted a prospective intervention study over a 4-year period. Monitoring of ABHR consumption and direct observation of hand hygiene practices, with periodic feedback to staff, was implemented in 17 facilities of varying types: 5 large-scale acute-care facilities, 6 middle-to-small-scale acute-care facilities, and 6 non–acute-care facilities. Statistics for ABHR consumption were calculated before and after the implementation of direct observation of hand hygiene practices, and the change in ABHR consumption was calculated. The paired t test was used to assess the statistical significance of changes. A generalized linear mixed model analysis was performed to assess factors associated with ABHR consumption. Results: The total observation time was 1,225 months (625 months before direct observation, 600 months after direct observation), and the average observation time per facility was 36.0 months (± 27.5). All facilities implemented ABHR consumption monitoring within 1 month of starting the study. However, the mean time required to implement direct observation of hand hygiene practices was 24.7 (±19.1) months. There was a significant increase in ABHR consumption in large and middle-to-small-scale acute-care facilities (P < .0001) after implementing the direct observation. However, there was not a significant increase for ABHR consumption in non–acute-care facilities (P = .14). Multivariable regression analysis showed that the hospital ward type, duration of ABHR consumption monitoring, and duration of direct observation of hand hygiene practices were independently associated with ABHR consumption. Conclusions: ABHR consumption increased in all facilities that implemented direct observation, but the change was not statistically significant in non–acute-care facilities. The generalized linear mixed model analysis showed significant associations between ABHR consumption and hospital ward type and time to monitoring of ABHR consumption and direct observation of hand hygiene practices. Direct observation of hand hygiene practices should be implemented more widely. The effect of intervention intensity should be evaluated in future studies.
Disclosures: None
Implementation Science
Factors associated with high influenza vaccination among healthcare workers in Tennessee acute-care hospitals, 2014–2022
- Ashley Gambrell, Raquel Villegas, Christopher Wilson, Simone Godwin
-
- Published online by Cambridge University Press:
- 29 September 2023, p. s73
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Healthcare workers (HCWs) are at increased risk of influenza exposure and represent a potential transmission source. The Department of Health and Human Services (HHS) set a goal for 2020 to have 90% of all HCWs in acute-care hospitals (ACHs) vaccinated. Vaccination against influenza decreases symptomatic illness and absenteeism and protects HCWs and their contacts. We assessed characteristics of facility intervention programs based on their success in meeting this benchmark. Methods: Data from the NHSN were utilized, including answers to the Annual Flu Survey for 2014–2022 and the rate of vaccine compliance by facility. Flu surveys detail facility-specific programs implemented for each influenza season, from October to March. We used SAS version 9.4 software for univariate analyses to determine factors significantly associated with meeting the HHS benchmark target of ≥90% vaccination among all HCWs, split into categories for employees, students or volunteers, and licensed independent practitioners. Facilities were excluded if they were not ACHs or Critical Access Hospitals (CAH), did not complete the Annual Flu Survey for at least 1 year, or required vaccination as a condition of employment. Results: From 2014 to 2022, 745 surveys were completed. Overall, 48.58% of respondents succeeded in meeting the HHS benchmark. Also, 306 surveys completed noted that their facility did not require influenza vaccination. Among those, only 19.93% respondents succeeded. Moreover, 80.33% of successful respondents for all HCWs required personal protective equipment (PPE) upon vaccination refusal compared to 34.29% of unsuccessful respondents (P < .0001). Furthermore, 98.36% successful respondents required documentation of offsite vaccination, compared to 89.39% of unsuccessful respondents (P = .027). For employees, 64.56% of successful respondents tracked vaccination rates in some or all units compared to 45.81% of unsuccessful respondents (P = .004). Also, 63.29% successful respondents had visible vaccination of leadership, compared to 43.61% of unsuccessful respondents (P = .003). Furthermore, 86.08% of successful respondents had mobile vaccination carts, compared to 73.57% unsuccessful respondents (P = .023). For the student- or volunteer-specific benchmark, 24.59% of successful respondents provided vaccination incentives compared to 14.63% of unsuccessful respondents (P = .035). Conclusions: Facilities with ≥90% vaccination among HCWs were more likely to require PPE after vaccination refusal and documentation for offsite vaccination. Other strategies for vaccination were differentially associated by employee type for Tennessee facilities. For future outreach, a multipronged approach is more likely to be successful in addressing vaccine uptake among employees with lagging rates. Strategies for influenza vaccine uptake could also improve other occupational vaccinations. More research is needed on the barriers to vaccination among HCWs specifically.
Disclosures: None
Exploring the relationship between the reduction of floor microbial burden and the impact on healthcare-associated infections
- Caitlin Crews-Stowe, Elizabeth Lambert, Lori Berthelot, Katherine Baumgarten
-
- Published online by Cambridge University Press:
- 29 September 2023, pp. s73-s74
-
- Article
-
- You have access Access
- Open access
- Export citation
-
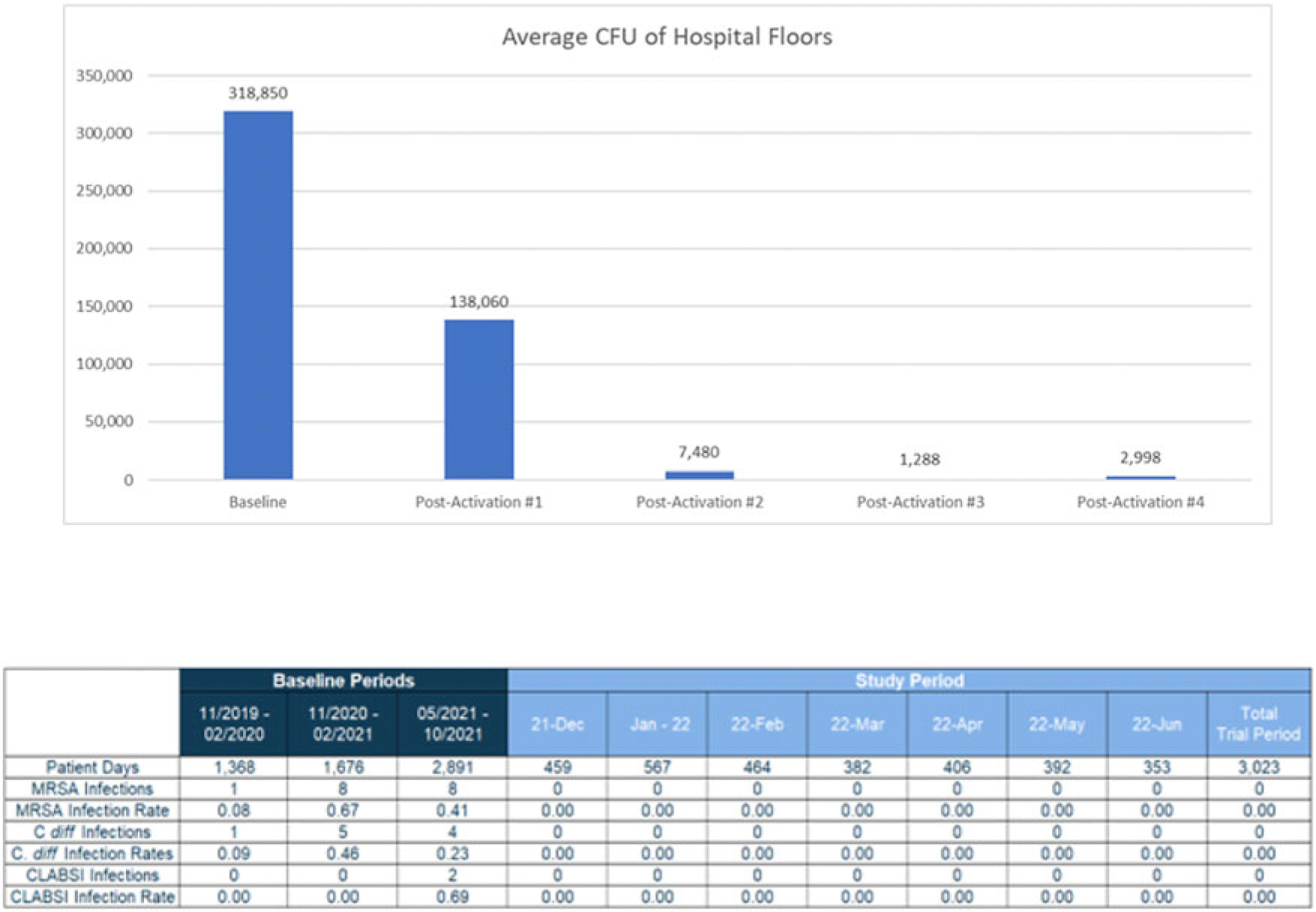
Background: Healthcare floors are a vehicle and/or source for potential pathogens that cause healthcare associated infections, and hospital floors are often heavily contaminated with pathogens such as Clostridioides difficile and methicillin-resistant Staphylococcus aureus. However, definitive research linking reductions in floor burden to reductions in HAIs has not yet been established. We sought to evaluate emerging technology for continuous disinfection and its potential impact on HAIs. This study was designed to explore the potential relationship between the reduction of microbial burden of floors and healthcare associated infections. Methods: A prospective study was conducted in a 22-bed medical-surgical intensive care unit in a 180-bed suburban hospital near New Orleans, Louisiana, from November 2021 to June 2022. Using sterile, premoistened sponges, samples were collected from the floors of 10 areas throughout the unit including 2 nurses’ stations, the physician charting area, and 7 patient rooms. The advanced photocatalytic oxidation (aPCO) equipment was then installed in the HVAC ductwork throughout the ICU and activated. Environmental surface sampling of the same floor surfaces was then repeated every 4 weeks for the first 5 months of the study. HAIs were also tracked throughout the entire study period. The facility’s normal cleaning floor protocols using a neutralizing floor cleaner were unchanged and followed during the study. Changes in surface burden were calculated using a repeated-methods ANOVA with post hoc analyses as appropriate. Rates of healthcare associated infections were compared using χ2 analyses. Results: Overall, there was a 99.6% statistically significant decrease in floor environmental surface burden from the baseline to the final postactivation test (Fig. 1). The average colony forming unit count (CFU) decreased from 318,850 CFU per 100 cm2 to just 2,988 CFU per 100 cm2. The unit also saw a statistically significant decrease in publicly reported healthcare associated infections (HO-MRSA, CLABSI, HO-CDI) during the study period compared to the same period a year prior and in the 6 months immediately prior to the beginning of the study (Fig. 2). Conclusions: Advanced photocatalytic oxidation technology resulted in a reduction of microbial burden on the floors of a high-traffic intensive care unit. Statistically significant decreases in healthcare-associated infections was also seen. This study highlights a novel aPCO technology and its efficacy at reducing microbial burden and healthcare-associated infections despite no change in practice.
Disclosures: None
Comparison of a standard environmental surface sampling method and a composite approach for select healthcare pathogens
- Monica Chan, Judith Noble-Wang, Laura Rose
-
- Published online by Cambridge University Press:
- 29 September 2023, p. s74
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Hospital surfaces are known to contribute to the spread of healthcare-associated infections (HAIs). Environmental sampling is often performed to locate a reservoir or to evaluate intervention strategies in healthcare facilities. Composite sampling is commonly practiced in other fields of environmental sampling and involves collection of multiple samples combined entirely or partially to form a new sample. We compared a standard CDC surface whole-tool sampling method with a composite sampling approach. Methods: Acinetobacter baumannii (AB), Klebsiella pneumoniae that produce K. pneumoniae carbapenemase (KPC), vancomycin-resistant Enterococcus faecalis (VRE), methicillin-resistant Staphylococcus aureus (MRSA), and Clostridioides difficile spores were suspended in an artificial soil and deposited as 40 µL droplets (~104 CFU total) onto steel coupons of surface areas 323 cm2, 645 cm2, or 1,290 cm2 and dried for 2 hours. The surfaces were sampled with a single pass of a cellulose sponge— either the larger side of the sponge (face) or the smaller side of the sponge (edge)—and the optimal surface area was determined. Recovery from the optimal surface area with a single pass sampling was compared to the recovery using a standard CDC method in which all sides were used (ie, whole-tool method) to sample a standard area (645 cm2). Recovery was determined by culture and total CFU were determined for each optimal surface area. Theoretical composites were constructed using the mean total CFU of optimal surface area; 2×((face) + (edge)). Significance was set at P ≤ .05. Results: Total CFU recovery using the whole-tool method was significantly greater than the single pass sample recovery for MRSA (18,300 vs 16,600 CFU) and VRE (27,600 vs 26,400 CFU) (P < .05). When comparing the theoretical composite method to the standard whole-tool area (625 cm2), the theoretical composite total CFU was significantly greater than the whole-tool method for all organisms. For example, VRE recovery with the standard CDC whole-tool method was 27,600 CFU from 625 cm2, yet a theoretical composite approach recovered 79,800 CFU from an area of 1,290 cm2. Conclusions: Many factors influence recovery when sampling the environment, and composite sampling is a promising approach when sampling large surface areas. Using a theoretical composite of single-pass samples, the potential for improved detection with composite sampling was demonstrated. A composite sampling approach will reduce time and resources for sampling and sample processing, allowing larger surface areas to be investigated which will improve infection control strategies.
Disclosures: None
Infection Control in Low and Middle-Income Countries
Infection prevention and control perspective and practices among healthcare workers in Bangladesh: A multicenter cross section
- Md. Golam Dostogir Harun, Shariful Amin Sumon, Aninda Rahman, Md Mahabub Ul Anwar, Md. Saiful Islam
-
- Published online by Cambridge University Press:
- 29 September 2023, pp. s74-s75
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Infection prevention and control (IPC) is a critical feature of preventing the spread of healthcare-associated infections (HAIs) in hospitals. IPC practices are particularly important in resource-constrained and crowded hospital settings. The successful implementation of infection prevention measures depends on healthcare worker (HCW) knowledge of, attitude toward, and practice (KAP) of IPC. In this project, we assessed the KAP of HCWs and identified factors associated with IPC compliance at tertiary-care hospitals in Bangladesh. Methods: From September 2020 to January 2021, we conducted this hospital-based cross-sectional assessment at 11 tertiary-care hospitals. A semistructured questionnaire was used to conduct face-to-face interviews with physicians, nurses, and cleaning staff who were directly involved in patient care. Based on >75% of the total score, each KAP component was divided into adequate knowledge, favorable attitude, and safe practice. We performed descriptive analysis and multivariate logistic regression to determine the KAP score and associated factors influencing IPC compliance in hospital settings. Results: In total, 1,728 HCWs were interviewed; 76.8% of the participants had adequate knowledge on IPC and 54.6% reported safe practices. However, only 16.2% of HCWs had a favorable attitude toward IPC. Among the 3 HCW groups, nurses had the highest KAP scores (76.07±12.7) followed by physicians (69.8±16.2), and cleaning staff (34.4±27.3). Only 29.2% of HCWs reported having received IPC training, and they cited heavy workload as a barrier to IPC guideline adherence. HCWs having adequate knowledge showed 9 times higher odds of safe IPC practice (AOR, 9.36; 95% CI, 5.47–16.04). HCWs who had a favorable attitude toward IPC were 16 times as likely to perform safe practice toward IPC activities (AOR, 15.5; 95% CI, 10.27–23.42). Conclusions: Knowledge of safe practices and having a favorable attitude toward IPC are key components of a successful IPC program. Significant improvements are required among all levels of HCWs in Bangladesh tertiary-care hospitals, especially cleaning staff. Educational interventions to train on IPC guidelines, plus monitoring, could improve HCW safe practices.
Disclosures: None
Infection Control in Low- and Middle-Income Countries
Healthcare worker perceptions about infection prevention and control processes and practices in Latin America
- Valeria Fabre, Pilar Beccar-Varela, Carolyn Herzig, Guadalupe Reyes-Morales, Clare Rock, Rodolfo Quiros
-
- Published online by Cambridge University Press:
- 29 September 2023, p. s75
-
- Article
-
- You have access Access
- Open access
- Export citation
-
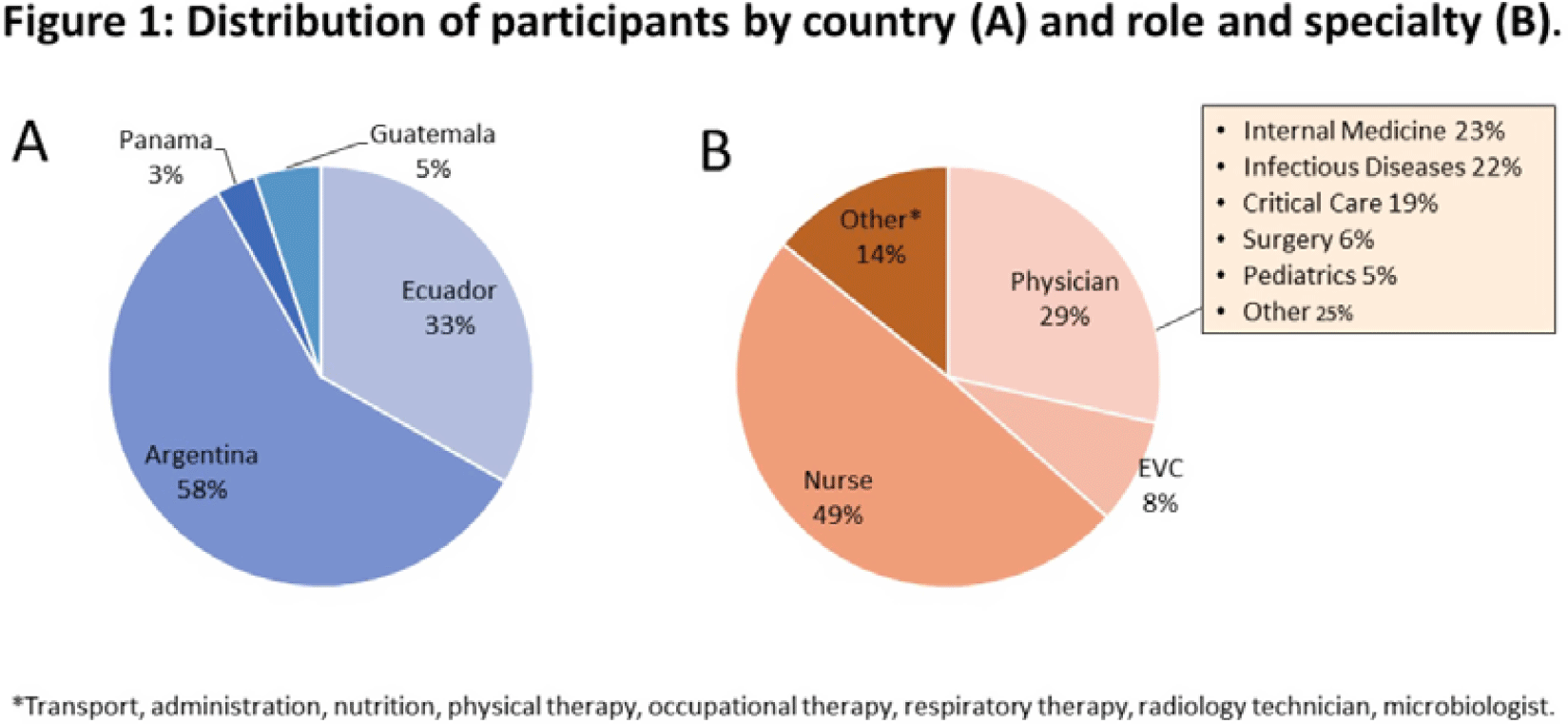
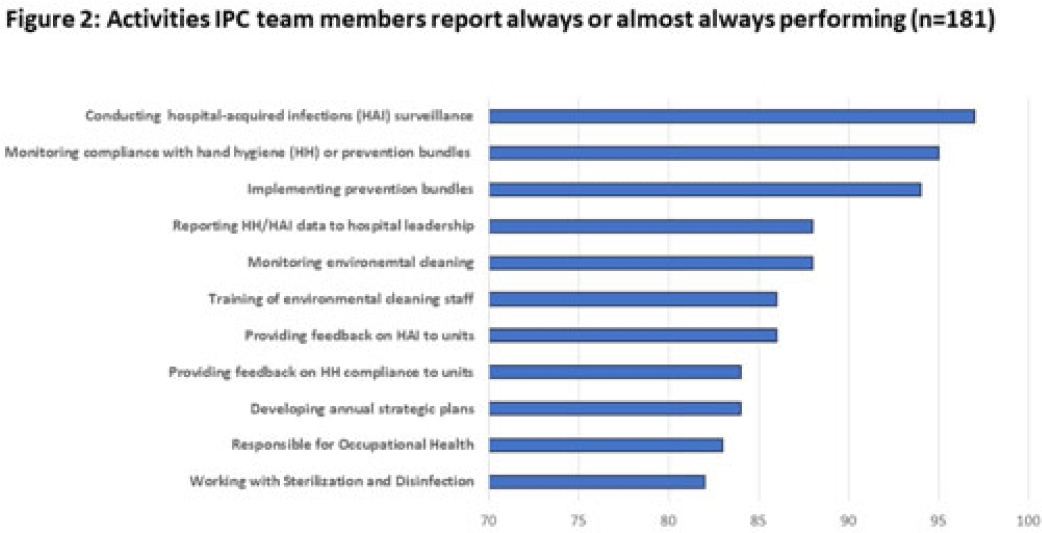
Background: The burden of hospital-associated infections (HAIs) and antimicrobial resistance (AMR) in Latin America is high. Improving engagement by healthcare workers (HCWs) in infection prevention and control (IPC) may lead to better patient outcomes; however, little is known about HCW perceptions of IPC in the region. We sought to understand HCW perceptions of IPC processes and practices. Methods: During August–September 2022, HCWs from 30 hospitals with IPC programs in 4 Latin American countries (Panama, Guatemala, Ecuador, and Argentina) were invited to participate in an electronic, voluntary, anonymous survey about their perceptions of IPC at their hospitals. Physicians, nurses, and environmental care (EVC) personnel were prioritized for recruitment. All respondents were asked 18 questions; IPC team members were asked 5 additional questions about specific activities implemented by IPC programs, how data are used, and how IPC could be improved. Answers with 5-point Likert scale responses were categorized into 2 groups (eg, strongly agree or agree vs neutral, disagree, or strongly disagree) for analysis. Results: Of 1,252 HCWs who completed the survey, 181 (14%) were IPC team members, 1,095 (87%) had direct patient contact, and 1,156 (92%) worked >20 hours per week. Figure 1 shows participant characteristics. Most participants (56%) rated their IPC program as very good, 38% rated it as good, and 6% rated it as bad. Physicians were less likely to give a favorable rating. Compliance with prevention bundles and hand hygiene (HH) by colleagues was rated as poor by 28% and 22% of HCWs, respectively; however, only 11% and 5% indicated that their own compliance was poor, respectively. Also, 25% of participants reported not receiving or only occasionally receiving HH compliance data. Similarly, 41% of participants reported not receiving HAI data on a regular basis, and 19% of IPC nurses reported not receiving data despite being responsible for conducting surveillance. Furthermore, 41% of respondents indicated not receiving or only occasionally receiving IPC training or education relevant to their role. When asked about the safety climate, 16% of participants reported not feeling appreciated. In addition, 22% of IPC nurses and 37% of individuals in the “other” category (eg, health technicians and therapists) were more likely to report this. When IPC team members were asked how frequently specific activities were conducted (Fig. 2), several opportunities for improvement were identified, including improving HCW access to HH data and development of strategic plans. Conclusions: Improving HCW access to training on IPC and to data on HAI burden and compliance with HH and prevention bundles should be emphasized in Latin American hospitals.
Disclosures: None

























