92 results
Lost in translation? Deciphering the role of language differences in the excess risk of psychosis among migrant groups
- Kelly K. Anderson, Jahin Ali Khan, Jordan Edwards, Britney Le, Giuseppe Longobardi, Ivan Witt, María Francisca Alonso-Sánchez, Lena Palaniyappan
-
- Journal:
- Psychological Medicine , First View
- Published online by Cambridge University Press:
- 22 May 2024, pp. 1-8
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
Migration is a well-established risk factor for psychotic disorders, and migrant language has been proposed as a novel factor that may improve our understanding of this relationship. Our objective was to explore the association between indicators of linguistic distance and the risk of psychotic disorders among first-generation migrant groups.
MethodsUsing linked health administrative data, we constructed a retrospective cohort of first-generation migrants to Ontario over a 20-year period (1992–2011). Linguistic distance of the first language was categorized using several approaches, including language family classifications, estimated acquisition time, syntax-based distance scores, and lexical-based distance scores. Incident cases of non-affective psychotic disorder were identified over a 5- to 25-year period. We used Poisson regression to estimate incidence rate ratios (IRR) for each language variable, after adjustment for knowledge of English at arrival and other factors.
ResultsOur cohort included 1 863 803 first-generation migrants. Migrants whose first language was in a different language family than English had higher rates of psychotic disorders (IRR = 1.08, 95% CI 1.01–1.16), relative to those whose first language was English. Similarly, migrants in the highest quintile of linguistic distance based on lexical similarity had an elevated risk of psychotic disorder (IRR = 1.15, 95% CI 1.06–1.24). Adjustment for knowledge of English at arrival had minimal effect on observed estimates.
ConclusionWe found some evidence that linguistic factors that impair comprehension may play a role in the excess risk of psychosis among migrant groups; however, the magnitude of effect is small and unlikely to fully explain the elevated rates of psychotic disorder across migrant groups.
P119: The Valladolid Multicenter Study: The Use of Benzodiacepines in the Elderly and Falls Reported By a Liaison Psychiatry Units
- Mª Desamparados D. Perez Lopez, Elena Alonso, Alejandro Compared Sanchez, Eduardo Delgado Parada, Miguel Alonso Sánchez, Leire Narvaiza Grau, Monica Prat Galbany, Andrea Santoro, Maria Iglesias Gonzalez, Cristina Pujol Riera, Eduardo Fuster Nacher
-
- Journal:
- International Psychogeriatrics / Volume 35 / Issue S1 / December 2023
- Published online by Cambridge University Press:
- 02 February 2024, pp. 172-173
-
- Article
-
- You have access Access
- Export citation
-
Objective:
The objective of this study is to describe the prevalence of benzodiazepine in a sample of patients (≥65 years) attended by liaison psychiatry units (LPU) in Spain and its possible relation to falls.
Methods:This is an observational., cross-sectional, multicenter study. We obtained data from a sample of 165 patients (≥65 years) admitted to 7 general hospitals in Spain referred from different departments to each liaison psychiatry unit. Data was collected for a month and a half period. Psychiatric evaluations were performed while the patients were on wards.
Results:We obtained a sample of 165 patients (78 women, 88 men) with a mean age of 76,03 years old (42.10% <75 years, 57,83% ≥ 75 years). Most of them were married and they lived accompanied (67,27%). Only 5,45% lived in a nursing home. 65,45% of patients had prescribed at least one psychotropic drug before LPU intervention; mainly (50,9%) benzodiazepines (60%women/40%men). 70,9% of these group of patients had more than one psychotropic drug prescribed before LPU. After LPU intervention in 39,39% at least one drug was withdrawn (in 50,81 % of cases benzodiazepines). Falls in the past 6 months were reported in 24.8% of total patients. Patients under benzodiazepine treatment had fallen in 29% of cases. After LPU intervention benzodiazepines were withdrawn in 56,25% % of them.
Conclusions:Benzodiazepines are widely used in our sample and frequently is associated with polypharmacy. LPU intervention might be a useful tool to reduce the use of them, specially for those who reported falls.
Longitudinal studies might be carried out to study these factors and their possible relationship with falls, given that Benzodiazepines are consistently associated with a higher risk of falls. It is unclear whether specific subgroups such as short-acting benzodiazepines and selective serotonin reuptake inhibitors are safer in terms of fall risk. Ppropriate prescription of medications such as BZDs is an important public health issue.
P112: Valladolid Multicenter Study: Diagnostic agreement between physicians and liaison psychiatry units in an elderly population in 7 hospitals in Spain.
- Leire Narvaiza, Monica Prat Galbany, Ferran Vilalta, Andrea Santoro, Maria Iglesias Gonzalez, Cristina Pujol Riera, Eduardo Fuster Nacher, Mª Desamparados Perez Lopez, Eduardo Delgado Parada, Miguel Alonso Sánchez
-
- Journal:
- International Psychogeriatrics / Volume 35 / Issue S1 / December 2023
- Published online by Cambridge University Press:
- 02 February 2024, pp. 212-213
-
- Article
-
- You have access Access
- Export citation
-
Objective:
The objective of this study is to describe the diagnostic agreement between physicians and liaison psychiatry units (LPU) in 7 general hospitals of Spain for elderly patients and to analyze possible factors related to it.
Methods:This is an observational., cross-sectional, multicenter study. We obtained data from a sample of 165 patients (≥65 years) admitted to 7 general hospitals in Spain referred from different departments to each liaison psychiatry unit. Data was collected for a month and a half period. Psychiatric evaluations were performed while the patients were on wards.
Results:We obtained a sample of 165 patients (78 women, 88 men) with a mean age of 76,03 years old (42.10% <75 years, 57,83% ≥ 75 years). Most of them were married and they lived accompanied (67,27%). Only 5,45% lived in a nursing home.
In 55.15% the main reason to referral was anxiety/depression symptoms. 42,42% had no psychiatry medical background. After LPU visit a new diagnosis was done in 56.96%. Main diagnoses were adjustments disorders (26,66%), delirium (20,6%) and no psychiatric pathology (14,54%)
Cohen’s kappa statistics were used to estimate the agreement between the diagnoses made by LPU and the diagnoses considered by the referring doctors. We obtained a moderate global agreement (kappa= 0,4971) between observers (0,424 for <75 years, 0,557 for ≥65 years) Moderate agreement was found for alcohol or substance abuse (kappa= 0,41) and low agreement was found for affective disorders (kappa= 0,3278) and delirium/ psychological and behavioral symptoms in dementia (Kappa= 0,2341).
We analyzed factors which might affect de agreement between physicians and LPU such is group of age, functional impairment, comorbidity by Charlson index and previous diagnosis of dementia.
Conclusions:Further longitudinal studies might help in the future to analyze the factors related to agreement between doctors and might help to establish educational programs
P54: The Valladolid Multicentre Study: Clinical Difference Between Age Groups in a Sample of Geriatiric Patiants Referred to 7 Liaison Psychiatrics
- Eduardo Fuster Nacher, Mª Desamparados D. Perez Lopez, Miguel Alonso-Sánchez, Eduardo Delgado Parada, Leire Narvaiza Grau, Monica Prat Galbany, Maria Iglesias Gonzalez, Cristina Pujol Riera
-
- Journal:
- International Psychogeriatrics / Volume 35 / Issue S1 / December 2023
- Published online by Cambridge University Press:
- 02 February 2024, pp. 242-243
-
- Article
-
- You have access Access
- Export citation
-
Introduction and Objectives:
It is well known that geriatric patients are at increased risk of developing comorbid medical and psychiatric conditions, and a large proportion of them are admitted to psychiatric liaison units (LPUs). The aim of this study is to determine which clinical differences between age groups (65- 74 years and ≥75 years) are statistically significant to potentially warrant special attention when referring to an LPU.
Methods:This is an observational, cross-sectional and comparative multicentre study. We collected data from 165 patients (≥65 years) admitted to 7 Spanish general hospitals and referred to each LPU from different departments. Data were collected over a period of one and a half months. Psychiatric examinations were performed during the patients' stay in the wards. The sample was divided into two age groups of patients and a comparative analysis was done.
Results:We obtained a sample of 165 patients with a mean age of 76.03 years (42.10% < 75 years, 57.83% ≥ 75 years). We analysed several variables between two age groups: the youngest (65- 74 years) and the oldest (≥75 years). In the younger group (mean age 69.87 years), the mean Barthel index before admission was 93.23 (52.1% with independent ambulation) and at the time of our first assessment was 54.62, before 82.71 of the older group (mean age 80.63). The mean Lawton index was 4.44 (6.35 for the older group) and the Charlson index was 6.38 (5.6 for the older group). 21.11% reported falls in the last 6 months, compared to 27.6% in the older group. The most common reason for referral was anxiety/depression symptoms in both groups (52.12% and 56.53%) and agitation (24.46% in the older group). After the LPU visit, the main diagnoses were adjustment disorder in both groups (25.3% and 25.53%) and delirium in the older group (23.4%). Antidepressants and benzodiazepines were the most common psychotropic drugs prescribed before the LPU visit, and benzodiazepines were the most common drugs discontinued after the LPU visit in both groups.
Conclusions:Clinical differences were found between two age groups (65-74 years and ≥75 years) at LPU, which could allow professionals to improve their attention and interventions.
P41: Valladolid Multicenter Study: Factors related to time to referral and length of hospital stay in old psychiatry patients in seven general hospitals in Spain
- Cristina Pujol Riera, Anna Barnés Andreu, Eduardo Fuster Nacher, Mª Desamparados Perez Lopez, Miguel Alonso Sánchez, Eduardo Delgado Parada, Leira Narvaiza Grau, Monica Prat Galbany, Andrea Santora, Maria Iglesias Gonzalez
-
- Journal:
- International Psychogeriatrics / Volume 35 / Issue S1 / December 2023
- Published online by Cambridge University Press:
- 02 February 2024, p. 201
-
- Article
-
- You have access Access
- Export citation
-
Objective:
Older patients (≥65yo) admitted to general hospitals have increased in the past years. This resulted in an increase in hospitalization periods, health costs, and morbi-mortality rates in this group of patients.
Previous evidence points that the reduced time to referral (TTR) to Consultation-Liaison Psychiatry Units (CLP) leads to a reduced length of stay (LOS) in GH improving long-term prognosis of medical conditions.
This study aims to explore whether a prior disability in older patients leads to delay the search for psychiatric help. And to explore whether early referral to CLP is associated with reduced LOS in general hospitals.
Methodology:This is an observational, cross-sectional, multicentre study. We obtained a complete data set from a sample of 152 patients (≥65 years old) admitted to 7 general hospitals in Spain referred to CLP unit for 1,5 months.
Results:Mean age of the sample was 76.3 (±6.4). TTR was 14.5 (±18.0) days. LOS was 26.7 (±22.4) days, and length of stay after consultation was 12.3 (±10.3) days. Barthel Index before admission was 87.3 (±18.0) and Lawton&Brody Index before admission was 5.3 (2.7). We found a significant positive association of Barthel Index (r=0.17, p=0.042) and Lawton&Brody Index (r=0.20, p=0.014) before admission with TTR, which indicates that patients with a worse clinical status were attended earlier. Similarly, antecedents of both falling episodes (r=-0.2, p= 0.013) and walking difficulties (r=-0.24, p= 0.003) were associated with shorter TTR. TTR in Medical Departments was 11.7 (±15.0) days and in Surgical Departments was 24.0 (±22.8) days (t=-3.5, p= 0.001). TTR showed a highly significant positive correlation with LOS (r=0.89, p<0.0001) and a more discrete positive correlation with length of stay after consultation (r=0.20, p=0.016).
Conclusion:We confirm that a shorter TTR to CLP was related to a shorter LOS. Also, patients in medical wards had shorter TTR. In contrast to our hypothesis, we found that a higher disability prior to hospitalization led to earlier referral to CLP, meaning that these patients were assessed and treated earlier leading to better long- term prognosis and lower health costs.
FC6: The Valladolid Multicenter Study: ¿Is there ageism in liaison psychiatry? Referrals of patients over 65 years to 7 Liaison Psychiatric Units (LPU) in Spain
- Miguel Alonso Sanchez, Eduardo Delgado Parada, Leire Narvaiza Grau, Monica Prat Galbany, Andrea Santoro, Maria Iglesias Gonzalez, Cristina Pujol Riera, Eduardo Fuster Nacher, Mª Desamparados Perez Lopez
-
- Journal:
- International Psychogeriatrics / Volume 35 / Issue S1 / December 2023
- Published online by Cambridge University Press:
- 02 February 2024, p. 69
-
- Article
-
- You have access Access
- Export citation
-
Introduction and objective:
Ageism is defined by the World Health Organization as stereotypes, prejudice, and discrimination towards others or oneself based on age. Ageism is thought to pose a risk to the physical and mental health of older adults, but little is known about how to measure it in LPUs. We propose that a form of ageism can be detected by comparing the referrals made by liaison psychiatry services among patients over age 65 at discharge with functional status and medical comorbidity. Our hypothesis is that the worse the functional index and medical comorbidity, the fewer referrals to psychiatric services and the more referrals to primary care physicians.
Methods:This is an observational, cross-sectional, multicenter study. We obtained data from a sample of 165 patients (≥65 years) admitted to seven general hospitals in Spain referred from different departments to each LPU. Data was collected over a period of one and a half months. Psychiatric evaluations were performed while the patients were in the wards. Sociodemographic, clinical, and care variables were collected. Functional status was measured with the Barthel and Lawton index and comorbidity with the Charlson index.
Results:We obtained a sample of 165 patients with a mean age of 76,03 years old. The mean Barthel index was 87,18 previous admission and 61,15 at the time of our first visit. The mean Lawton index was 5,266667 and the Charlson index was 6,03. The different options for referral were primary care physician, psychiatric facilities, nursing homes, substance use centers, or exitus. Statistical analysis was performed using the nonparametric Kruskal-Wallis test to determine if there were significant differences (p < 0,05) between the indices and referrals. Contrary to our hypothesis, statistical significance was observed only for the Lawton index, but with more referrals to psychiatric facilities among patients with the worst functional scores. No other statistical significance was observed.
Conclusions:Functional status and medical comorbidity did not play a role in the referral of inpatients managed by LPUs. Further studies are needed to clarify whether there is any form of ageism in the referral of elderly inpatients attended by Psychiatric Liaison Units.
Coronavirus disease 2019 is associated with long-term depressive symptoms in Spanish older adults with overweight/obesity and metabolic syndrome
- Sangeetha Shyam, Carlos Gómez-Martínez, Indira Paz-Graniel, José J. Gaforio, Miguel Ángel Martínez-González, Dolores Corella, Montserrat Fitó, J. Alfredo Martínez, Ángel M. Alonso-Gómez, Julia Wärnberg, Jesús Vioque, Dora Romaguera, José López-Miranda, Ramon Estruch, Francisco J. Tinahones, José Manuel Santos-Lozano, J. Luís Serra-Majem, Aurora Bueno-Cavanillas, Josep A. Tur, Vicente Martín Sánchez, Xavier Pintó, María Ortiz Ramos, Josep Vidal, Maria Mar Alcarria, Lidia Daimiel, Emilio Ros, Fernando Fernandez-Aranda, Stephanie K. Nishi, Oscar García Regata, Estefania Toledo, Jose V. Sorli, Olga Castañer, Antonio Garcia-Rios, Rafael Valls-Enguix, Napoleon Perez-Farinos, M. Angeles Zulet, Elena Rayó-Gago, Rosa Casas, Mario Rivera-Izquierdo, Lucas Tojal-Sierra, Miguel Damas-Fuentes, Pilar Buil-Cosiales, Rebeca Fernández-Carrion, Albert Goday, Patricia J. Peña-Orihuela, Laura Compañ-Gabucio, Javier Diez-Espino, Susanna Tello, Ana González-Pinto, Víctor de la O, Miguel Delgado-Rodríguez, Nancy Babio, Jordi Salas-Salvadó
-
- Journal:
- Psychological Medicine / Volume 54 / Issue 3 / February 2024
- Published online by Cambridge University Press:
- 05 September 2023, pp. 620-630
-
- Article
- Export citation
-
Background
The coronavirus disease 2019 (COVID-19) has serious physiological and psychological consequences. The long-term (>12 weeks post-infection) impact of COVID-19 on mental health, specifically in older adults, is unclear. We longitudinally assessed the association of COVID-19 with depression symptomatology in community-dwelling older adults with metabolic syndrome within the framework of the PREDIMED-Plus cohort.
MethodsParticipants (n = 5486) aged 55–75 years were included in this longitudinal cohort. COVID-19 status (positive/negative) determined by tests (e.g. polymerase chain reaction severe acute respiratory syndrome coronavirus 2, IgG) was confirmed via event adjudication (410 cases). Pre- and post-COVID-19 depressive symptomatology was ascertained from annual assessments conducted using a validated 21-item Spanish Beck Depression Inventory-II (BDI-II). Multivariable linear and logistic regression models assessed the association between COVID-19 and depression symptomatology.
ResultsCOVID-19 in older adults was associated with higher post-COVID-19 BDI-II scores measured at a median (interquartile range) of 29 (15–40) weeks post-infection [fully adjusted β = 0.65 points, 95% confidence interval (CI) 0.15–1.15; p = 0.011]. This association was particularly prominent in women (β = 1.38 points, 95% CI 0.44–2.33, p = 0.004). COVID-19 was associated with 62% increased odds of elevated depression risk (BDI-II ≥ 14) post-COVID-19 when adjusted for confounders (odds ratio; 95% CI 1.13–2.30, p = 0.008).
ConclusionsCOVID-19 was associated with long-term depression risk in older adults with overweight/obesity and metabolic syndrome, particularly in women. Thus, long-term evaluations of the impact of COVID-19 on mental health and preventive public health initiatives are warranted in older adults.
Predictors of transition from paliperidone palmitate 1 and 3 months (PP1M & PPP3M) to paliperidone palmitate 6 months (PP6M)
- P. J. Escobedo-Aedo, J. Merayo-Cano, S. Sánchez Alonso, S. Ovejero, L. Muñoz Lorenzo, L. Mata Iturralde
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S438
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Schizophrenia is a severe, chronic, mental disease. Its stability relies upon a multidisciplinary treatment, where pharmacological treatment is a key aspect. Long-acting injectable antipsychotics (LAIs) have proved efficacy in improving adherence, reducing hospitalizations and relapses, compared with oral treatment[1,2]. Paliperidone palmitate is a long-acting antipsychotic, approved by FDA in 2009 for acute and chronic treatment in schizophrenia. To date, long evidence exists regarding treatment efficacy of paliperidone palmitate 1 month (PP1M) and paliperidone palmitate 3 month (PP3M)[3]. In September 2021 a new long-acting medication was approved for schizophrenia treatment, that is, paliperidone palmitate 6 months (PP6M). This is the first LAI with 6 months duration of treatment, which means, only 2 administrations per year.
We here analyzed the factors explaining transitioning from PP1M and PP3M to PP6M treatment in a population previously described somewhere else[4].
ObjectivesTo identify the variables explaining the transition from other long-acting formulations (PP1M and PP3M) to the new biannual formulation (PP6M) in our clinical practice.
Methods123 patients, previously diagnosed with psychotic disorders, in follow-up in our clinical center Fundación Jiménez Díaz Hospital, was analyzed. Sociodemographic factors and clinical evolution were compared in order to identify factors predicting transitioning from PP1M and PP3M to PP6M.
ResultsIn the PP1M group, patients transitioning to PP6M had more than 6 years of evolution of disease ans active consummation of drugs, compared with patients who stayed on PP1M. Other sociodemographic were similar in both groups. Only 1 patient was readmitted in hospital since transition to PP6M and no emergency visits were accounted for people transitioned.
In the PP3M group, the majority of people transitioning to PP6M were under polypharmacy of which, 42% were on clozapine treatment. The percentage of people with schizophrenia diagnosis was significantly less than in the no transitioning group, though it remained the principal diagnosis. No other significant difference was found with regard to sociodemographic variables. Additionally, no emergency visits nor readmissions to hospital were accounted in this group.
Finally, the PP3M transitioned to PP6M significantly more than PP1M group. Although no clear variable explained this situation.
ConclusionsWith these results, we conclude that chronicity and drugs consummation were the main variables explaining transitioning from PP1M to PP6M. In the other hand, the main variable explaining transitioning from PP3M to PP6M was polypharmacy.
These results are preliminary and, therefore, should be taken cautiously. We will probably dilucidated future tendency in these treatment use in the upcoming months.
Disclosure of InterestNone Declared
Smoking treatments for patients with mental illness: case presentation and a brief literature review
- F. Garcia Sanchez, M. Gutierrez Rodriguez, C. Moreno Menguiano, M. A. Corral Alonso, J. J. Vazquez Vazquez, S. M. Bañon Gonzalez, V. Voces Domingo, J. A. Casado de la Hera
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S756
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Smoking prevalence in patients with mental illness ranges between two to 4 times higher than general population. This higher prevalence has a multifactorial origin, and some of the possible causes are still unknown.
They have a higher prevalence of tobacco-associated diseases and higher mortality.
Additionally, these patients have greater difficulty in treating and quitting smoking.
A relationship has been found between severity of mental illness and smoking. Risk of suicide seems to be higher in patients with higher tobacco consumption. Schizophrenia is the mental illness that has been most closely related to smoking, with a prevalence close to 90%.
ObjectivesThe aim of this work is reviewing the current bibliography referring to smoking treatments for patients with mental illness
MethodsA literature search using electronic manuscripts available in PubMed database published during the last ten years and further description and discussion of a single-patient clinical case
ResultsThe treatment of tobacco dependence in patients with mental illnesses is sometimes waited until there is psychiatric stability, which can take a long time in those cases with more severe mental disorders, which can have negative physical and psychiatric consequences.
The combined treatment of cognitive behavioral therapy and pharmacological treatment is the most effective approach. Nicotine replacement therapy can be useful, while combined use of antidepressants or anxiolytics is also recommended.
Bupropion has shown efficacy. In patients with schizophrenia it does not seem to worsen positive symptomatology, but improving the negative one. It should not be used in patients with bipolar disorder or bulimia.
Varenicline has shown efficacy in the general population, but limitations were established in patients with mental illness, although it is the drug that has shown greater efficacy. However, is not currently available in our country.
Cytisine is a drug with limited number of studies in the psychiatric population but it may be a reasonable treatment alternative.
ConclusionsThe prevalence of tobacco use in patients with mental illness is higher than the general population, especially in paranoid schizophrenia. The consequences on physical health and the evolution of psychiatric illness are very relevant. Based on above, a multidisciplinary and coordinated management involving psychiatrists and other specialists in the treatment of these patients should be desirable.
Disclosure of InterestNone Declared
Acute mutism in a young female. A case report of a 20-year-old female who presents a 3-month mutism
- A. Gonzalez-Mota, A. Gonzalez-Gil, C. Martin-Gomez, J. A. Benito-Sanchez, I. M. Peso-Navarro, L. Fernandez-Alonso
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S177-S178
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
A 20-year-old female presents with a progressive 3-month mutism, hyporexia (20kg weight loss), abulia, anhedonia, apathy, social isolation,seeking company of her parents even at night, bradypsychia, sialorrhea, psychomotor slowdown and hypomimia. She is hospitalized in the Psychiatric Brief Hospitalization Unit (PBHU).Her parents relate the beginning of this symptomatology to a breakup and gender violence,which the patient confirms during the interview by eye/cephalic movements and single words jotted down.
ObjectivesThe objective of this study is to describe the evolution of the patient during her hospitalization in the PBHU of Salamanca and to look into the available bibliography about mutism related to stress and sialorrhea.
MethodsWe carried out a follow-up of the hospitalization of the patient and a structured search in PubMed with the keywords “mutism”,“sialorrhea” and “stress” in the last 10 years in English,Spanish and French.
ResultsFew or no articles where found.Therefore, the articles about mutism and stress were analyzed, which focused mostly in selective mutism. Regarding fear,the response to cope with the threat(fight, flight, freeze) is mediated by the autonomic system. The “Polyvagal Theory” speaks about the vagus nerve participating in emotion regulation (social communication and mobilization). Dissociation, in this context,has adaptive and defensive purposes and its threshold can be reduced by repeated stress situations.Long-term alteration of the autonomic nervous system has been described in selective mutism.This malfunction can be related to an elevated production of saliva due to the activation of the parasympathetic in the salivary glands, causing sialorrhea in our patient.
The patient began treatment with sertraline 100mg and risperidone 2mg with the aim of its antidepressive and major tranquilizer effects, she also began individual and family psychotherapy, we assured her sleep and intakes and she began to progressively recover her speech and mobility,identifying a possible trigger for the symptomatology: a physical beating of gender violence after her breakup.
ConclusionsDissociation and “freeze” response can be a maladaptative mechanism to fear.The malfunction of the autonomic nervous system can explain the disconnection,poor gaze,low facial and body expression and inability to speak.
Disclosure of InterestNone Declared
What do we know about lithium associated hypercalcemia?
- N. Laherrán Cantera, R. Palacios - Garrán, A. Sanchez-Guerra Alonso, C. Gutiérrez Santaló, L. I. Muñoz-Manchado
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S577
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Lithium associated with hypercalcemia may mimic a psychiatric condition and be confused for a relapse of bipolar disorder. The etiology seems to be due to a reduced sensitivity of the parathyroid cells to calcium, altering the parathyroid hormone (PTH) response. Lithium as an essential monovalent cation has some structural similarity to calcium (Ca) and can interact with protein receptors. This leads to changes in the inhibitory configuration of PTH and increased serum calcium concentrations, rising the threshold necessary to suppress hormone secretion.
Lithium-induced hyperparathyroidism (HIL) is the main cause of hypercalcemia in these patients.
ObjectivesBased on a clinical case of lithium-associated hypercalcemia in a patient with bipolar disorder, review the existing literature and state the needs for periodic monitoring protocols.
MethodsCase report and bibliographical review.
ResultsA 38-year-old woman, diagnosed with bipolar affective disorder at the age of 18, has been treated with lithium during which she developed secondary tubulointerstitial nephropathy as an adverse effect. Recently, she requested medical evaluation for constitutional syndrome associated with deterioration of general condition with loss of strength and difficulty in walking. Analytically, mild hypercalcemia was detected, and the study was extended to include Ca and PTH.
Chronic lithium therapy often develops mild hypercalcemia (approximately 10 to 20 percent of patients taking lithium), most likely due to increased secretion of PTH. Lithium can also unmask previously unrecognized mild hyperparathyroidism in patients with adenomas within a few years of starting therapy or induce parathyroid hyperplasia with a chronic use.
The hypercalcemia usually, but not always, subsides when the lithium is stopped. Normalization of serum calcium is more likely to occur one to four weeks post-lithium withdrawal in patients with a relatively short duration of lithium use. It is less likely in patients receiving lithium for more than 10 years.
Regarding the case to be presented, a review of the literature is carried out and the need to propose periodic calcium monitoring protocols is exposed.
ConclusionsRecommendations include determination of serum calcium every 6 months, urinary calcium and creatinine every 12 months, and bone mineral density monitoring every 1 to 3 years. Regular analytical monitoring including total calcium, PTH and vitamin D, would identify patients with a tendency to hypercalcemia so that appropriate measures could be taken. So as chronic treatment with lithium can develop mild hypercalcemia, I consider it necessary to develop periodic monitoring protocols for this adverse effect.
Disclosure of InterestNone Declared
Exploring the concept and management of post ictal psychosis through a clinical case and review
- A. Compaired Sánchez, B. Lázaro Alonso, J. Gómez-Arnau Ramírez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S765-S766
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Postictal Psychosis of Epilepsy (PIPE), part of the group collectively known as Psychosis of Epilepsy, is characterized by an onset of confusion or psychotic symptoms within one week of apparent normal mental function. PIPE has been argued to be underdiagnosed in the clinical population, perhaps due to a failure to recognize the temporal relation between the seizure and the psychotic episode.
ObjectivesTo explore the concept and management of post ictal psychosis.
MethodsWe present a clinical case and a review of the literature concerning post ictal psychosis.
ResultsWe report the case of a 36 year old woman with focal refractory epilepsy after a likely episode of limbic encephalitis in 2015. Cognitive and psychiatric sequelae in the form of depressive symptoms, in treatment with neurology and psychiatry since 2021. One previous episode of psychotic symptoms during seizures. Worsening of seizure frequency since march of 2022 with apparent normalization (absence of seizures after dose reduction of eslicarbamazepine and introduction oflamotrigine) for about four days before being hospitalized in the neurology unit due tobehavioral abnormalities. During psychiatric exploration, the patient showed signs of partial clouding of consciousness with manierisms, ecopraxias and ecolalias; verbigerance in the form of the neurologist’s name and bizarre movements like looking behind suggestive of sensoroperceptive disturbances. The symptomatology resolved itself during the following week after treatment with diazepam.
Finally, a narrative review concerning the case was also performed; with particular emphasis on antipsychotic drugs with low risk of lowering seizure threshold (such as risperidone or aripiprazole) as the recommended treatment.
ConclusionsOur findings point to the relevance of Postictal Psychosis of Epilepsy as a clinical entity. Further studies on pathogenic mechanisms and therapeutic management are required.
Disclosure of InterestNone Declared
Visual hallucinations and age-related macular degeneration: case presentation and a brief literature review
- M. M. Gutiérrez Rodríguez, F. García Sánchez, M. Á. Corral Alonso, J. J. Vázquez Vázquez, C. Moreno Menguiano
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S936-S937
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
age-related macular degeneration (AMD) is an ocular disease involving central vision. It is one of the mainreasons of vision loss in people over 50. Seeing non-existing faces or shapes are described in AMD. Symtoms of visualhallucinations that occur as a result of vision loss is known as Charles Bonnet syndrome (CBS). These patients haveintact cognition, do not have hallucinations in any other sensory modalities, and retain insight into the unreal nature oftheir hallucinations.
Objectivesthe aim of this work is analizing ethiology, demographic characteristics, clinica features and treatment inpatients with AMD and visual hallucinations
Methodsa literature search using electronic manuscripts available in PubMed database published during the last ten years with further description and discussion of a single-patient clinical case.
Resultsin different studies in patients diagnosed with AMD, the reported prevalence ranges between 15 up to 39percent. Patients with more significant vision loss may be more likely to experience visual hallucinations. In large caseseries, mean age is 70 to 85 years. Hallucinations can last few minutes or several hours. On average, people experiencethese hallucinations on and off for about 3 years. Those who experience hallucinations tend to see multiple types ofimages, particularly people and faces.The diagnosis of CBS is made when visual hallucinations occur in patients withvision loss in the absence of psychosis, delirium, or other causes.
There is no specific treatment for CBS: optimal ocular care, education and differents techniques to manage hallucinations(changing your lighting conditions and environment, blinking frequently or moving your eyes side-to-side rapidly whilekeeping your head still…). Antidepressants, anticonvulsants, anxiolytics and low-dose of antipsychotics have been used for CBS with positiveeffects in previous reports, but the efficacy of these drugs in the treatment is somewhat questionable and should bereserved for those who exhibit high levels of distress and have not responded to conventional intervention.
Case report: 80-years old woman who presented with a 4 month history of hallucinations and legally blind from AMD. Aworkup for other pathological causes of visual hallucinations was negative.
ConclusionsCBS is an under-recognized and under-reported disorder that involves visual hallucinations in visuallyimpaired individuals. It requires a multidisciplinary approach from neurologists, psychiatrists, general practitioners andophthalmologists. New studies are needed in order to understand its clinical presentation and to improve its management.
Disclosure of InterestNone Declared
Building bridges between body and mind: liaison psychiatry
- S. Bravo Herrero, I. Moreno Alonso, M.J. Sánchez Artero, A.M. Matas Ochoa
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S472-S473
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
As liaison psychiatrists, it is very important to mantein a good relationship with other medical specialties in order to obtain the best result for our patients. Most of the times, the somatic process affects direct or indirectly to mental healt and vice versa, so our cooperation is extremely important for the patient’s welbeing.
ObjectivesWith this study we try to find special considerations and necesities of every specialty that count on us in our hospital. We have design this batebase with the aim of discovering which are the main problems that suffer the admitted patients, which doubts face our colleagues when evaluate mental health patients, etc. Thus, our team could help other physicians properly or so we could stablish a proper liaison in order to make things easier.
MethodsA database has been created with all the patients evaluated by our liaison psychiatry team during half a year. We have taken into account sex, age, referral specialist, mental health diagnosis (after our evaluation), previous mental health follow-up, if they are on psycopharmacology treatment, if they requiere psycopharmacology treatment and if they requiere follow-up once discharged.
Results22,9% were kid/adolescent patients. 25,8% were elderly people (>70 yo). 47% were men (of which, 6% were trans men), 53% were women. 22,9% suffered from adjustment disorder, 14,1% had no acute mental health problem, 11,76% presented substance abuse. Main petitions were made from Internal Medicine (30%)
ConclusionsWith this information we can explore other specialists’ and admitted patients’ needs and concerns and focus our effort in solving them.
DisclosureNo significant relationships.
Differences of use between paliperidone palmitate 3 month and paliperidone palmitate 1 month in real practice, with psychotic patients
- P. Escobedo-Aedo, J. Merayo-Cano, L. Mata Iturralde, L. Muñoz Lorenzo, S. Ovejero, S. Sánchez Alonso
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S730-S731
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Paliperidone palmitate 1-month (PP1M) is a Long-acting injectable antipsychotic formulation, approved for the treatment of schizophrenia and schizoaffective disorder. Recently, paliperidone palmitate 3-months (PP3M) formulation was introduced, which maintains stability while offering a longer dosing interval for the maintenance treatment in patients previously treated with PP1M. Despite of this, many patients are treated with PP1M without transition to PP3M.
ObjectivesTo identify variables explaining maintenance of PP1M treatment instead of going to PP3M. We hypothesize that more severe patients are delayed in transition to PP3M because of expectation to complete stabilization.
MethodsA descriptive analysis of 123 patients, diagnosed with psychotic disorders, on treatment with paliperidone palmitate 1 month or 3 months, was performed. Age, sex, type of paliperidone treatment, hospitalizations after the initiaton of treatment, years since diagnosis, polytherapy and toxic habits were some of the variables measured and compared between both groups (PP1M and PP3M).
ResultsMost of patients (63,41%) were on PP3M. Both groups shared characteristics like male sex predominance, schizophrenia as the most common diagnosis, having a recent onset diagnosis, same frequency of polypharmacy and same pattern of drug consumption. There was a slight difference between both groups regarding severity. PP1M and PP3M showed respectively 33% and 16,7% of admissions after initiation.
ConclusionsNo clear pattern determines less transition to PP3M from PP1M. No statistical difference was found except form the difference found in admission after change of treatment (to PP1M or PP3M), which could reflect influence of severity in treatment. Future research is needed in order to better elucidate this association.
DisclosureNo significant relationships.
Relationship between cannabis use and schizophrenia
- J.J. Vazquez Vazquez, M.M. Gutiérrez Rodríguez, M.D.L.A. Corral Y Alonso, C. Moreno Menguiano, F. Garcia Sánchez
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S469
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Numerous studies have shown evidence that cannabis use increases the appearance of psychotic symptoms and disorders, and worsens the course of the disease in those with schizophrenia. However, a causal relationship between cannabis and schizophrenia has not been well established yet.
ObjectivesIn this presentation we try to review the relationship between cannabis use and prevalence of schizophrenia.
MethodsWe performed a search of Medline looking for systematic reviews and methodologically robust studies in the field published in English in the last 5 years.
ResultsA number of studies, both cross-sectional and prospective, find a prevalence of schizophrenia several times higher among cannabis users than in non-users. This association becomes stronger the lower the age of cannabis use onset, the higher the amount consumed and the higher the THC concentration are. Half of the patients with a cannabis-induced psychotic disorder turn into a diagnosis of schizophrenia within a few years. So far, it has not been possible to demonstrate a global increased prevalence of schizophrenia in relation to the increase of cannabis use in the population in recent decades.
ConclusionsCannabis and schizophrenia have a complex relationship model; we still cannot clearly establish whether it is causal or the first works as a trigger for pathology in vulnerable subjects.
DisclosureNo significant relationships.
Antidepressants in epilepsy
- M.M. Gutiérrez Rodríguez, M.D.L.A. Corral Y Alonso, C. Moreno Menguiano, F. Garcia Sánchez, J.J. Vazquez Vazquez, S.M. Bañón González
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S298
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Depressive disorders are one of the most frequent psychiatric comorbidity in epilepsy and they have a negative impact on the quality of life. Depression often requires antidepressant treatment. However, it is often left untreated in people with epilepsy, in part due to fear that antidepressants could cause seizures.
ObjectivesThe goal of this study was to do a review and describe the evidence of the efficacy and safety of pharmacological treatment for depression in epilepsy.
MethodsReview of literature sources were obtained through electronic search in PubMed database with special focus in papers published in the last 5 years.
ResultsThe existing evidence of the effectiveness of antidepressants in treating depressive symptoms associated with epilepsy is still limited and response rate was highly variable. It is essential first to optimize seizure control and minimize unwanted antiepileptic drug-related side effects. As the first line of treatment you should consider the use of SSRI or IRSN. The improvement in depressive symptoms ranged from 25% to 82% according to the different studies and depending on the antidepressant administered. A review of the literature indicates that the risk of antidepressant-associated seizures is low although some antidepressants such as amoxapine or bupropion are not recommended.
ConclusionsThere are few comparative data to support the choice of antidepressant drug or drug class in terms of efficacy or safety for the treatment of people with epilepsy and depression. It would be important to design controlled trials of antidepressants in large cohorts of participants with epilepsy and clinically significant depression.
DisclosureNo significant relationships.
Clinical predictors of hepatic complications in Anorexia Nervosa
- S. Villa, I. Sánchez, F. Fernandez-Aranda, N. Custal, J. Menchón, P. Alonso
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S386
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Hepatic ones are some of the most described somatic complications in anorexia nervosa (AN) affected patients. They can be due to malnutrition, which is the more usual thing, or due to re-feeding. The first one can lead to more marked elevations of the hepatic enzymes, especially alanine-aminotransferase (ALT). It’s been also described the relation between a sharply decreased body mass index (BMI) and this kind of complications, but there are still to determine more predictors.
ObjectivesIdentifying clinical predictors of hepatic complications in AN.
MethodsWe analysed data from 71 AN affected patients hospitalized at Bellvitge Hospital from January 2016 to October 2021. We used IBM SPSS Statistics 22 to do all the statistics in this work.
ResultsThe medium age of the sample was 27.66 years with 10.8 years of evolution of AN. The medium BMI was 13.88. 33.80% of them had some sort of hepatic enzymes elevation, two of them a several one. AST, ALT and ALP were significantly more elevated in those patients with lower BMI. GGT was significantly more elevated in patients with more years of disorder development. We didn’t identify correlation between any purgative method and hepatic alterations.
ConclusionsThe elevation of ALT, AST and ALP seems to be related with the BMI of the patients, while the elevation of the GGT turns out to be related to the time of evolution of the eating disorder. Purgative methods don’t seem to be related to the development of hepatic alterations in AN.
DisclosureNo significant relationships.
What we know about Auditory Charles Bonnet Syndrome?
- C. Moreno Menguiano, F. Garcia Sánchez, J.J. Vazquez Vazquez, M.M. Gutiérrez Rodríguez, M.D.L.A. Corral Y Alonso
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S655
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Charles Bonnet syndrome (CBS) is defined like visual hallucinations found in individuals who are not necessarily mentally ill, who have visual impairment and no cognitive deficits. Although CBS make reference to visual hallucinations, in this case we are going to deal about Auditory Charles Bonnet Syndrome (aCBS), a very infrequent condition that consists in the presentation of musical hallucinations in patients with sensorineural hearing loss and which etiology is not clearly due to a psychiatric condition.
ObjectivesReview the scientific literature available on aCBS to see how much we know about this syndrome.
MethodsReview of available literature sources were obtained through electronic search in PubMed database.
ResultsMusical hallucination is a complex form of auditory hallucinations. The most common of these are idiopathic and they present in elderly patients with deafness or impaired audition, which suggests a deterioration of cerebral function. The pathophysiologic mechanism is not understood. These patients tend to have intact reality tests. The time course is variable. In those cases in which it is possible, treating the hearing loss can lead to a significant improvement of the symptom. However, when every this strategies are insufficient, pharmacological treatments can be considered.
Conclusions- aCBS is an uncommon condition characterized by the presence of complex auditory hallucinations that mainly affect elderly patients with hearing loss. - In most cases there is no previous psychiatric history. - The etiology and pathophysioplogic are not well defined. - There is no etiological treatment. We can use pharmacological and no pharmacological methods of treatment.
DisclosureNo significant relationships.
E-health treatments for Dual Disorders on pregnancy
- R. Carmona Camacho, N. Lopez Carpintero, I. Caro-Cañizares, L. Albarracin García, E. Baca Garcia, M. Sanchez Alonso
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S92-S93
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Dual pathology during pregnancy, described as the co-occurrence of substance use and mental health problems, is one of the leading preventable causes of maternal and perinatal mortality and morbidity; however, effective and accessible treatments are lacking.
ObjectivesAs part of the WOMAP(Woman Mental Health and Addictions on Pregnancy) initiative, our study aimed to evaluate the effectiveness of an e-health-based psychotherapeutic program compared to enhanced usual care.
MethodsThis effectiveness clinical trial was conducted between 2016-2020 in 5 hospitals in the Madrid (Spain) metropolitan area. 2014 pregnant women under 26 weeks of pregnancy were screened. Eligible participants(n=120) were those who screened positive for co-occurring symptoms (AC-OK screener) and were not receiving specialized behavioral treatment. Participants were assessed in depth at baseline, 2,4,8 and 12 months(PHQ-9;GAD-7;PCL-5;AUDIT;DAST;Fagerström) and randomized to the usual care control group(n=38) or to two groups of a 10-session pregnancy-adapted psychotherapeutic program, one delivered by App/internet(n=41) and one by telephone(n=41). Intent-to-treat analyses assessed effectiveness.
ResultsStatistically significant effects of the intervention were found for mental health symptoms in the telephone group as compared to the control and App/internet groups, with an improvement effect starting earlier (2 months) and lasting longer (figures 1-3). Regarding substance use, due to the lack of other substances consumption, only smoking and alcohol cessation rates were analyzed. Patients in the App/internet and telephone groups discontinued significantly more, earlier and for a longer period compared to the control group(figures 4-5).
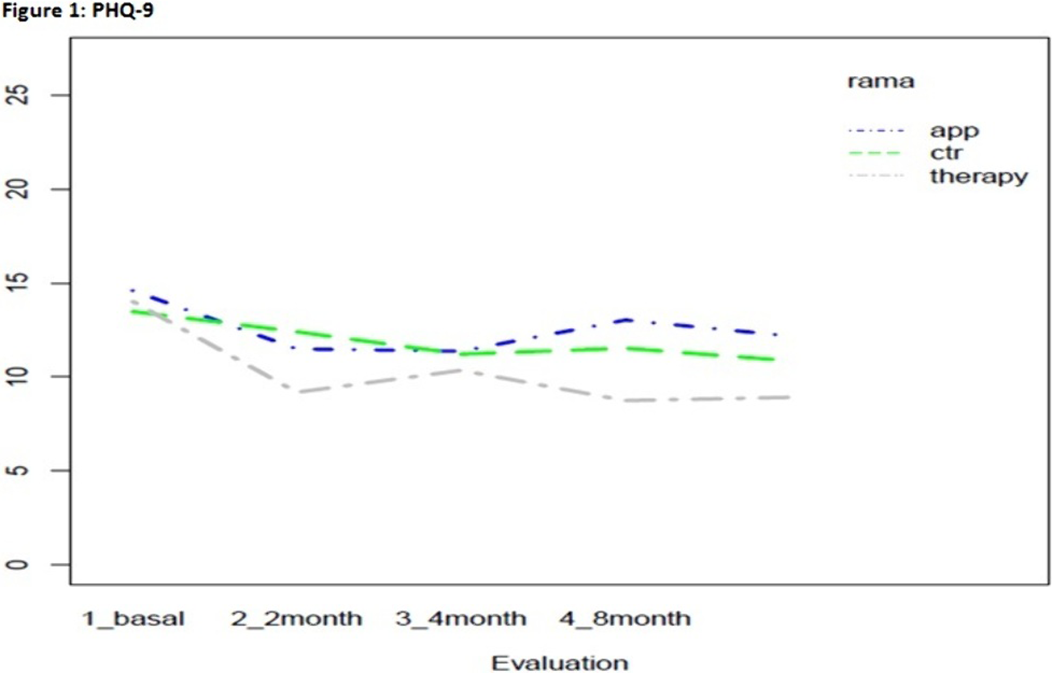
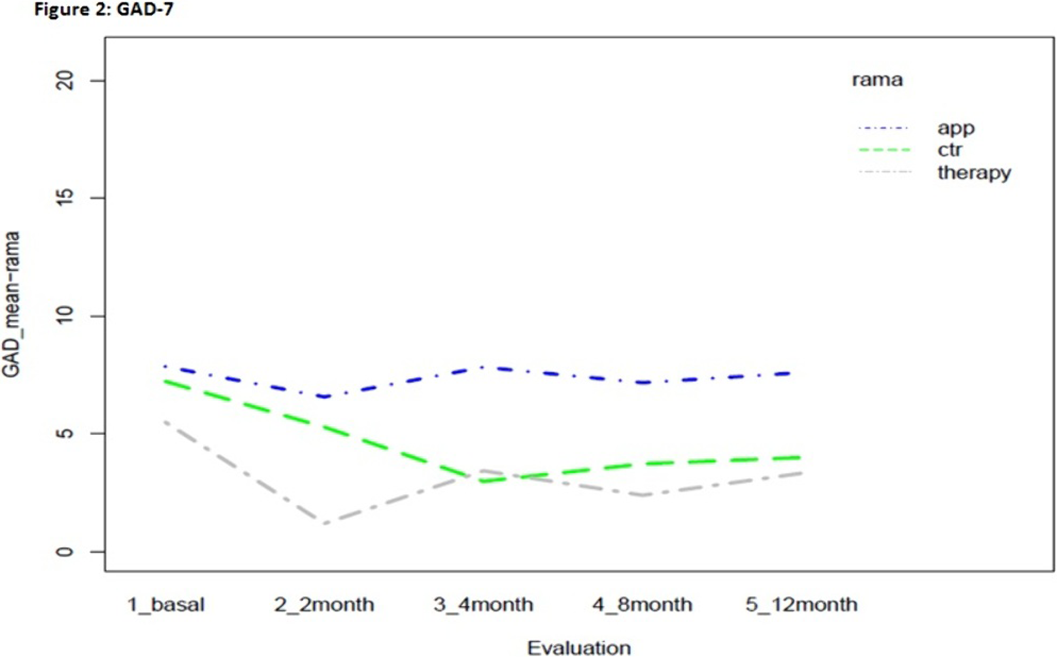
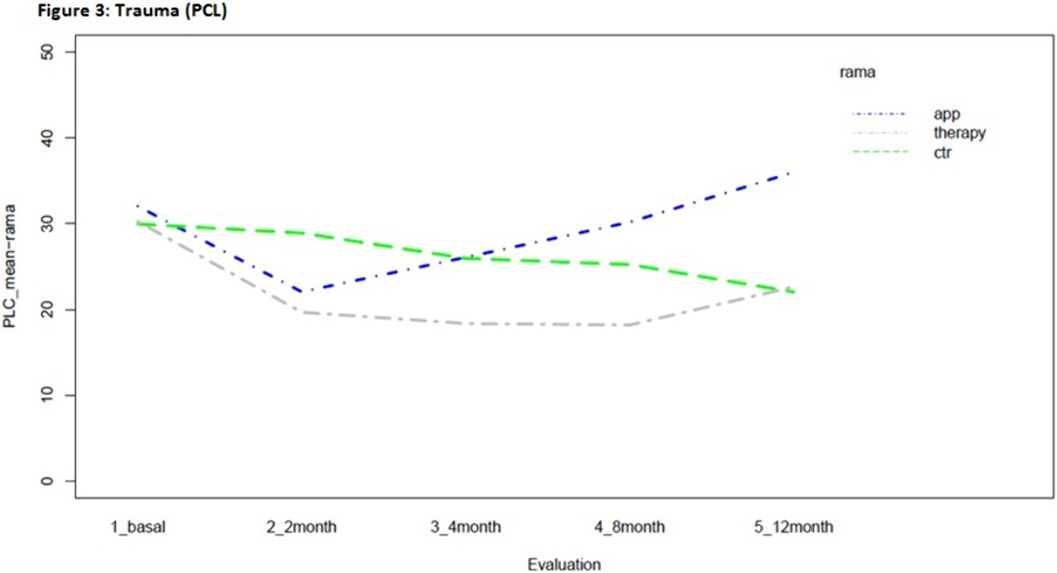
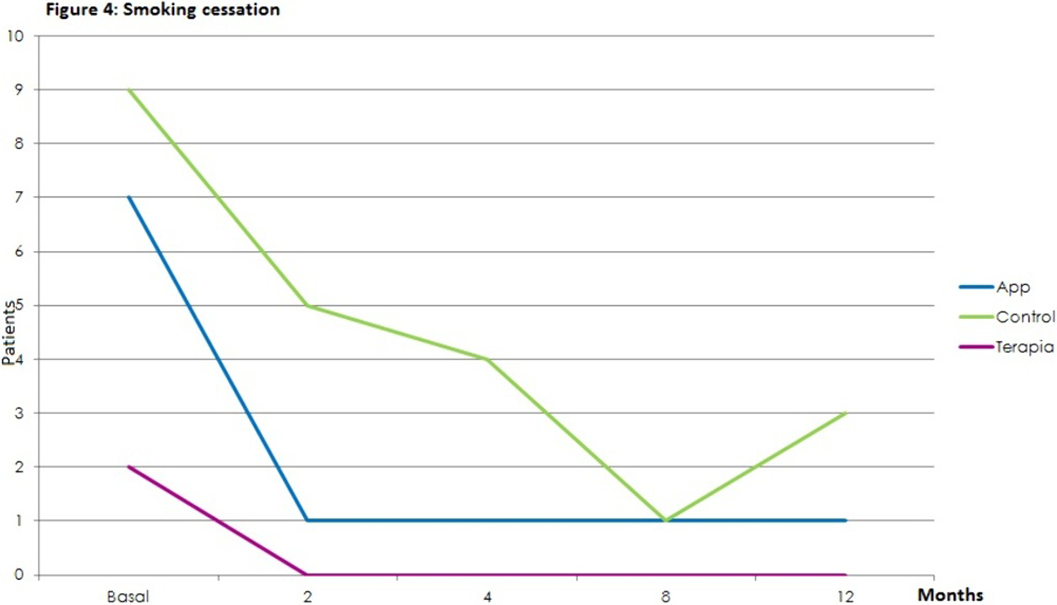
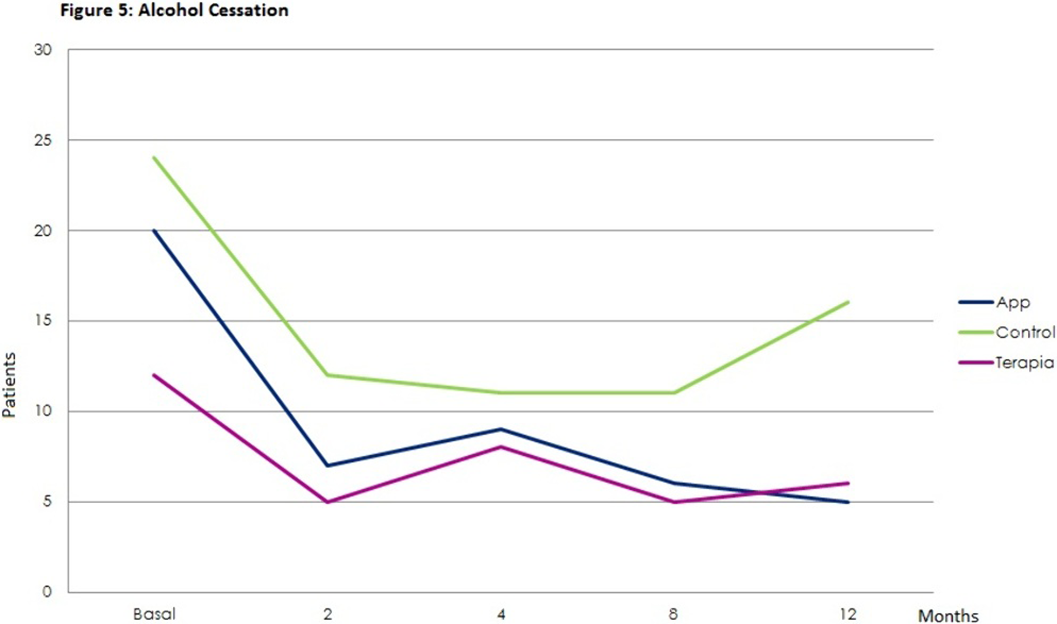 Conclusions
ConclusionsE-health psychotherapeutic programs could benefit pregnant women with dual disorders. An App/internet implementation could only be useful if focused solely on substances.
DisclosureNo significant relationships.








