2 results
General intelligence in adult patients with early- and adult-onset schizophrenia
- T. Calkova, L. Mørch-Johnsen, R. Elle Smelror, K. Nordbø Jørgensen, S. Cervenka, K. Collste, A. Vaskinn, A. Margrethe Myhre, O. A. Andreassen, T. Ueland, I. Agartz, D. Andreou
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S490-S491
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Early-onset schizophrenia (EOS) is a relatively uncommon disorder with psychotic symptoms emerging before 18 years of age. Although still under debate, EOS may be a more severe disorder relative to adult-onset schizophrenia (AOS), with worse prognosis. Cognitive deficits are a core feature of schizophrenia, accounting for a large part of the detrimental effect of the disorder and may reflect underlying neurodevelopmental disturbances. Some but not all previous studies show that the magnitude of cognitive deficits, including intelligence quotient (IQ), in patients with schizophrenia is dependent on the age of onset.
ObjectivesWe aimed to assess IQ in adult patients with EOS and AOS, and healthy controls. We hypothesized that patients with EOS would show lower IQ than those with AOS, and both patient groups lower IQ than HC.
MethodsWe included 136 adult patients with EOS (mean age: 24.7 (7.7) years, mean duration of illness: 9.3 (8.5) years, 50% women), 382 patients with AOS (mean age: 32.4 (9.5) years, mean duration of illness: 5.7 (6.6) years, 40.1% women) and 896 adult healthy controls (mean age: 33.2 (9.2) years, 47.1% women). We assessed current IQ with the Wechsler Abbreviated Scale of Intelligence (WASI) which yielded verbal (VIQ), performance (PIQ) and full-scale IQ (FIQ) scores. In a post-hoc analysis, we estimated premorbid IQ using the National Adult Reading Test (NART). We applied analyses of covariance (ANCOVAs) to investigate the putative differences in IQ scores and IQ change between patients with EOS, patients with AOS and healthy controls.
ResultsIn sex-, and age-adjusted models, FIQ and PIQ, but not VIQ, were significantly lower in EOS than in AOS (p=0.03, p<0.001 and p=0.428, respectively) (Image). Patients with EOS had fewer years of education than patients with AOS (p<0.001); the PIQ but not the FIQ difference between EOS and AOS remained significant after adjustment for education years (p=0.016 and p=0.333, respectively). Both patient groups had significantly lower IQ scores than healthy controls (Image). Further, patients with EOS and patients with AOS did not significantly differ in estimated premorbid IQ (109 and 110 units, respectively, p=0.092), whereas patients with EOS had a significantly larger estimated IQ decline after the disease onset compared to patients with AOS (12 and 9 units decline, respectively, p=0.015).
Image:
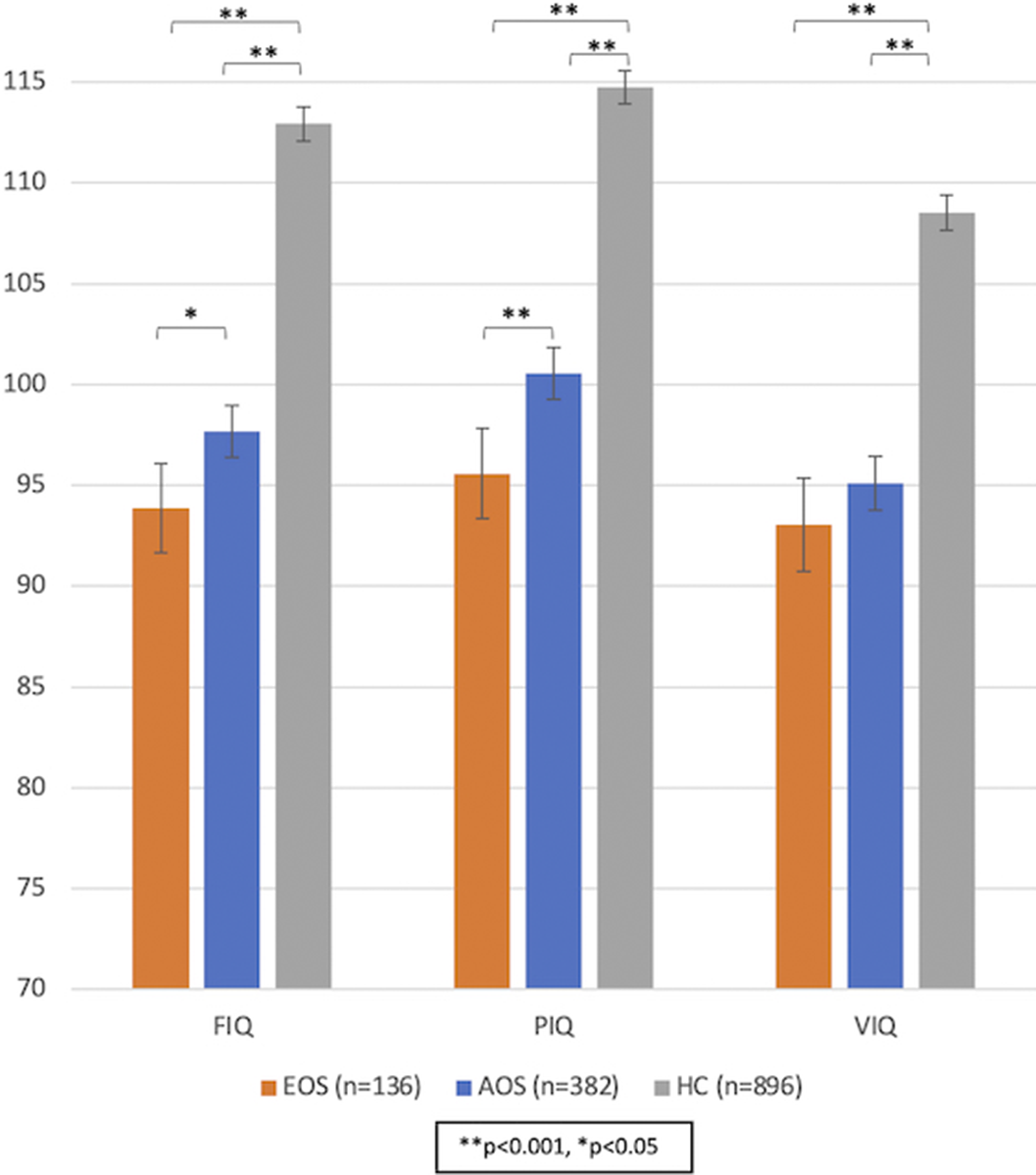 Conclusions
ConclusionsOur findings show that adult patients with EOS have significantly lower PIQ and FIQ scores, and significantly larger IQ decline after the disease onset, but not lower premorbid IQ, compared to patients with AOS. The adolescent onset of psychotic symptoms is linked, as expected, to fewer total years of education, which appears to explain the lower FIQ but only partially the lower PIQ in EOS, which may thereby be linked to the disorder per se.
Disclosure of InterestT. Calkova: None Declared, L. Mørch-Johnsen: None Declared, R. Elle Smelror: None Declared, K. Nordbø Jørgensen: None Declared, S. Cervenka: None Declared, K. Collste: None Declared, A. Vaskinn: None Declared, A. Margrethe Myhre: None Declared, O. A. Andreassen Consultant of: HealthLytix, Speakers bureau of: Lundbeck and Sunovion, T. Ueland: None Declared, I. Agartz: None Declared, D. Andreou: None Declared
Lower circulating neuron-specific enolase concentrations in adults and adolescents with severe mental illness
- Dimitrios Andreou, Nils Eiel Steen, Kjetil Nordbø Jørgensen, Runar Elle Smelror, Kirsten Wedervang-Resell, Stener Nerland, Lars T. Westlye, Terje Nærland, Anne Margrethe Myhre, Inge Joa, Solveig Merete Klæbo Reitan, Arne Vaaler, Gunnar Morken, Erlend Bøen, Torbjørn Elvsåshagen, Birgitte Boye, Ulrik Fredrik Malt, Pål Aukrust, Silje Skrede, Rune Andreas Kroken, Erik Johnsen, Srdjan Djurovic, Ole A. Andreassen, Thor Ueland, Ingrid Agartz
-
- Journal:
- Psychological Medicine / Volume 53 / Issue 4 / March 2023
- Published online by Cambridge University Press:
- 11 August 2021, pp. 1479-1488
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
Both neurodegenerative and neurodevelopmental abnormalities have been suggested to be part of the etiopathology of severe mental illness (SMI). Neuron-specific enolase (NSE), mainly located in the neuronal cytoplasm, may indicate the process as it is upregulated after neuronal injury while a switch from non-neuronal enolase to NSE occurs during neuronal maturation.
MethodsWe included 1132 adult patients with SMI [schizophrenia (SZ) or bipolar spectrum disorders], 903 adult healthy controls (HC), 32 adolescent patients with SMI and 67 adolescent HC. Plasma NSE concentrations were measured by enzyme immunoassay. For 842 adults and 85 adolescents, we used total grey matter volume (TGMV) based on T1-weighted magnetic resonance images processed in FreeSurfer v6.0. We explored NSE case-control differences in adults and adolescents separately. To investigate whether putative case-control differences in NSE were TGMV-dependent we controlled for TGMV.
ResultsWe found significantly lower NSE concentrations in both adult (p < 0.001) and adolescent patients with SMI (p = 0.007) compared to HC. The results remained significant after controlling for TGMV. Among adults, both patients with SZ spectrum (p < 0.001) and bipolar spectrum disorders (p = 0.005) had lower NSE than HC. In both patient subgroups, lower NSE levels were associated with increased symptom severity. Among adults (p < 0.001) and adolescents (p = 0.040), females had lower NSE concentrations than males.
ConclusionWe found lower NSE concentrations in adult and adolescent patients with SMI compared to HC. The results suggest the lack of progressive neuronal injury, and may reflect abnormal neuronal maturation. This provides further support of a neurodevelopmental rather than a neurodegenerative mechanism in SMI.




