10 results
Inventory of Sources of Stress During Medical Education - Further Validation
- M. Carneiro, A. Macedo, E. Loureiro, M. Dias, F. Carvalho, D. Telles Correia, F. Novais, C. Barreto Carvalho, C. Cabacos, D. Pereira, P. Vitória, A. Araújo, A.T. Pereira
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S619
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The Inventory of Academic Sources of Stress in Medical Education (IASSME) evaluates the presence and intensity of the main sources of academic stress for Portuguese Medicine students in five dimensions: Course demands/CD, Human demands/HD, Lifestyle/LS, Academic competition/AC, and Academic adjustment/AA.
ObjectivesTo further validate the ISSME using Confirmatory Factor Analysis and to analyze[ATP1] the psychometric properties of a new version including additional sources of stress.
MethodsParticipants were 666 Portuguese medicine (82.6%) and dentistry (17.4%) students (81.8% girls); they answered an online survey including the ISSME and other validated questionnaires: Maslach Burnout Inventory – Students Survey (MBI-SS) and Depression Anxiety and Stress Scales (DASS).
ResultsConfirmatory Factor Analysis showed that the second order model composed of five factors (the original structure by Loureiro et al. 2008), but excluding item 11 (loading=.371), presented good fit indexes (χ2/df=3.274; RMSEA=.0581, p<.001; CFI=.917; TLI=.904, GFI=.919). The Cronbach’s alfas were α=.897 for the total and from α=.669 (F2-HD) to α=.859 (F1-CD) for the dimensions. The expanded version, including two additional items related to lack of interest in medicine/dentistry (F6, α=.543) and two additional COVID-19 stress-related-items (F7, α=.744) also showed acceptable fit indexes (χ2/df=3.513; RMSEA=.061, p<.001; CFI=.88.; TLI=.866, GFI=.892). This new version’s α was of .896. Pearson correlations between ISSME and the other measures were significant (p<.01) and high: >.55 with DASS and >.50 with MBI-SS. Girls presented significantly higher ISSME scores. F6 score was significantly higher in dentistry students.
ConclusionsThis further validation study underlines that IASSME presents good validity (construct and convergent) and reliability.
DisclosureNo significant relationships.
Inventory of Sources of Stress During Medical Education - Further Validation
- M. Carneiro, A. Macedo, E. Loureiro, M. Dias, F. Carvalho, D. Telles Correia, F. Novais, C. Barreto Carvalho, C. Cabacos, D. Pereira, P. Vitória, A. Araújo, A.T. Pereira
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S693
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The Inventory of Academic Sources of Stress in Medical Education (IASSME) evaluates the presence and intensity of the main sources of academic stress for Portuguese Medicine students in five dimensions: Course demands/CD, Human demands/HD, Lifestyle/LS, Academic competition/AC, and Academic adjustment/AA.
ObjectivesTo further validate the ISSME using Confirmatory Factor Analysis and to analyze the psychometric properties of a new version including additional sources of stress.
MethodsParticipants were 666 Portuguese medicine (82.6%) and dentistry (17.4%) students (81.8% girls); they answered an online survey including the ISSME and other validated questionnaires: Maslach Burnout Inventory – Students Survey (MBI-SS) and Depression Anxiety and Stress Scales (DASS).
ResultsConfirmatory Factor Analysis showed that the second order model composed of five factors (the original structure by Loureiro et al. 2008), but excluding item 11 (loading=.371), presented good fit indexes (χ2/df=3.274; RMSEA=.0581, p<.001; CFI=.917; TLI=.904, GFI=.919). The Cronbach’s alfas were α=.897 for the total and from α=.669 (F2-HD) to α=.859 (F1-CD) for the dimensions. The expanded version, including two additional items related to lack of interest in medicine/dentistry (F6, α=.543) and two additional COVID-19 stress-related-items (F7, α=.744) also showed acceptable fit indexes (χ2/df=3.513; RMSEA=.061, p<.001; CFI=.88.; TLI=.866, GFI=.892). This new version’s α was of .896. Pearson correlations between ISSME and the other measures were significant (p<.01) and high: >.55 with DASS and >.50 with MBI-SS. Girls presented significantly higher ISSME scores. F6 score was significantly higher in dentistry students.
ConclusionsThis further validation study underlines that IASSME presents good validity (construct and convergent) and reliability.
DisclosureNo significant relationships.
Laminar and turbulent plasmoid ejection in a laboratory Parker Spiral current sheet
- Ethan E. Peterson, Douglass A. Endrizzi, Michael Clark, Jan Egedal, Kenneth Flanagan, Nuno F. Loureiro, Jason Milhone, Joseph Olson, Carl R. Sovinec, John Wallace, Cary B. Forest
-
- Journal:
- Journal of Plasma Physics / Volume 87 / Issue 4 / August 2021
- Published online by Cambridge University Press:
- 05 August 2021, 905870410
-
- Article
- Export citation
-
Quasi-periodic plasmoid formation at the tip of magnetic streamer structures is observed to occur in experiments on the Big Red Ball as well as in simulations of these experiments performed with the extended magnetohydrodynamics code, NIMROD. This plasmoid formation is found to occur on a characteristic time scale dependent on pressure gradients and magnetic curvature in both experiment and simulation. Single mode, or laminar, plasmoids exist when the pressure gradient is modest, but give way to turbulent plasmoid ejection when the system drive is higher, which produces plasmoids of many sizes. However, a critical pressure gradient is also observed, below which plasmoids are never formed. A simple heuristic model of this plasmoid formation process is presented and suggested to be a consequence of a dynamic loss of equilibrium in the high-$\beta$
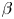 region of the helmet streamer. This model is capable of explaining the periodicity of plasmoids observed in the experiment and simulations, and produces plasmoid periods of 90 minutes when applied to two-dimensional models of solar streamers with a height of $3R_\odot$
region of the helmet streamer. This model is capable of explaining the periodicity of plasmoids observed in the experiment and simulations, and produces plasmoid periods of 90 minutes when applied to two-dimensional models of solar streamers with a height of $3R_\odot$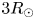 . This is consistent with the location and frequency at which periodic plasma blobs have been observed to form by Large Angle and Spectrometric Coronograph and Sun Earth Connection Coronal and Heliospheric Investigation instruments.
. This is consistent with the location and frequency at which periodic plasma blobs have been observed to form by Large Angle and Spectrometric Coronograph and Sun Earth Connection Coronal and Heliospheric Investigation instruments.
P0256 - Aripiprazole in schizophrenic patients
- A. Chinchilla, R. Gonzalez, I. Gobernado, M.F. Pando, A. Loureiro, E. Erausquin, M. Martín, M.D. Crespo, M. Vega
-
- Journal:
- European Psychiatry / Volume 23 / Issue S2 / April 2008
- Published online by Cambridge University Press:
- 16 April 2020, p. S156
-
- Article
-
- You have access Access
- Export citation
-
We worked with a group of 36 patients diagnosed with schizophrenia (DSM-IV-TR) who were in a chronic condition, with a predominance of negative and depressive-amotivational sympthomatology. They were on a long-term therapy with antipsychotic agents, achieving just a light improvement on the symptoms.
We switched to aripiprazole using a daily dosage of 15-30 mg. We evaluated the results on PANSS and ICG scales at the beginning of the treatment and after the first and third month, whilst paying special attention to the side-effects and adverse reactions that occurred. Concomitantly, we used benzodiacepines and hypnotics during the first two weeks, and antipakinsonism agents were not needed.
From an average initial PANSS score of 74 and ICG score of 3.6, after a month, PANSS average score lowered to 60 and ICG's came down to 3. After 3 months, PANSS average score was 45 and ICG'S was 2.5.
There was no need for discontinuing the treatment in 35 of the patients. One patient discontinued treatment and follow-up. Side-effects were Invaluable in general, though at the start insomia and light jitterness were observed in some of the patients.
We believe that aripiprazole is a very useful antipsychotic drug, not only for controlling acute episodes, but also on chronic patients for its effectiveness and good tolerability.
Dementia in acutely-ill medical elderly patients
- P. Sá Esteves, D. Loureiro, E. Albuquerque, F. Vieira, L. Lagarto, S. Neves, J. Cerejeira
-
- Journal:
- European Psychiatry / Volume 33 / Issue S1 / March 2016
- Published online by Cambridge University Press:
- 23 March 2020, p. S190
-
- Article
-
- You have access Access
- Export citation
-
Introduction
Dementia is one of the leading causes of disability and burden in Western countries. In Portugal, there is a lack of data regarding dementia prevalence in hospitalized elderly patients and factors associated with in-hospital adverse outcomes of these patients.
ObjectivesDetermine dementia prevalence in acutely-ill medical hospitalized elderly patients and its impact in health outcomes.
MethodsAll male patients (> 65 years) admitted to a medical ward (> 48 h) between 1.03.2015 to 31.08.2015 were included in the study. Patients were excluded if unable to be assessed due to sensorial deficits, communication problems or severity of the acute medical condition. Baseline evaluation included socio-demographic variables, RASS, NPI, Barthel Index and Confusion Assessment Method.
ResultsThe final sample consisted of 270 male subjects with a mean age of 80.9 years, 116 (43%) having prior dementia. Dementia patients were significantly older (83.5 vs 78.9; P < 0.001) and had lower values of Barthel Index (dementia: 34.8 vs non-dementia: 85.8; P < 0.001). Mortality rate (9,3%) and length of hospitalization (11.2 days) were similar between groups (12.1 vs 7.1; P = 0.204 and 11.9 vs 10.6; P = 0.218, respectively). Patients with dementia had higher rates of all neuropsychiatric symptoms except depression, anxiety and mood elation. The level of consciousness (measured by RASS) was impaired in 50% of patients with dementia, which was significantly higher than in non-demented subjects (12.3%; P < 0.001). Delirium rates were 29.5% in dementia compared with 7.1% in controls (P < 0.001).
ConclusionsThere is a high prevalence of dementia and an appreciable rate of delirium among these patients.
Disclosure of interestThe authors have not supplied their declaration of competing interest.
Risk Factors of Increased Mortality During Hospitalization in Acutely-ill Elderly Patients with Altered State of Consciousness
- P. Sá Esteves, D. Loureiro, E. Albuquerque, F. Vieira, L. Lagarto, S. Neves, J. Cerejeira
-
- Journal:
- European Psychiatry / Volume 41 / Issue S1 / April 2017
- Published online by Cambridge University Press:
- 23 March 2020, pp. S175-S176
-
- Article
-
- You have access Access
- Export citation
-
Introduction
A significant proportion of acutely ill hospitalised elderly patients have impaired consciousness and this has been associated with increased mortality. It remains unclear which factors underlie this relation. Identification of mortality predictors in this population is important to improve care.
ObjectivesDetermine if advanced age, cognitive impairment, high burden of comorbidities and poor functional status are predictors of increased mortality during hospitalisation in acutely-ill medical hospitalised elderly patients with altered state of consciousness.
MethodsAll male patients (> 65 years) admitted to a medical ward (> 48 h) between 01/03/2015 to 31/08/2015 with delirium or RASS lower than–2 were included in the study. Patients were excluded if unable to be assessed due to sensorial deficits, communication problems or medical condition precluding the evaluation. Baseline evaluation included socio-demographic variables, RASS, CAM, IQCODE-SF, DSM-IV-TR criteria for dementia, Charlson Comorbidity Index and Barthel Index. The variables were entered in a logistic regression model (significance level < 0.05).
ResultsThe final sample consisted of 75 male subjects with altered state of consciousness, 14 of them died during hospitalisation. Dementia and Barthel Index were significantly associated with mortality during hospitalisation (P = 0.01 and P < 0.01, respectively). On the other hand, age and Charlson Co-morbidity Index were not associated significantly with mortality during hospitalisation (P = 0.22 and P = 0.1, respectively).
ConclusionsAcutely ill elderly patients with altered state of consciousness at admission have higher risk of death during hospitalisation if they have prior dementia or poor functional status. Health care should be improved to provide better response to this type of patients.
Disclosure of interestThe authors have not supplied their declaration of competing interest.
Equivalency of the diagnostic accuracy of the PHQ-8 and PHQ-9: a systematic review and individual participant data meta-analysis – ERRATUM
- Yin Wu, Brooke Levis, Kira E. Riehm, Nazanin Saadat, Alexander W. Levis, Marleine Azar, Danielle B. Rice, Jill Boruff, Pim Cuijpers, Simon Gilbody, John P.A. Ioannidis, Lorie A. Kloda, Dean McMillan, Scott B. Patten, Ian Shrier, Roy C. Ziegelstein, Dickens H. Akena, Bruce Arroll, Liat Ayalon, Hamid R. Baradaran, Murray Baron, Charles H. Bombardier, Peter Butterworth, Gregory Carter, Marcos H. Chagas, Juliana C. N. Chan, Rushina Cholera, Yeates Conwell, Janneke M. de Manvan Ginkel, Jesse R. Fann, Felix H. Fischer, Daniel Fung, Bizu Gelaye, Felicity Goodyear-Smith, Catherine G. Greeno, Brian J. Hall, Patricia A. Harrison, Martin Härter, Ulrich Hegerl, Leanne Hides, Stevan E. Hobfoll, Marie Hudson, Thomas Hyphantis, Masatoshi Inagaki, Nathalie Jetté, Mohammad E. Khamseh, Kim M. Kiely, Yunxin Kwan, Femke Lamers, Shen-Ing Liu, Manote Lotrakul, Sonia R. Loureiro, Bernd Löwe, Anthony McGuire, Sherina Mohd-Sidik, Tiago N. Munhoz, Kumiko Muramatsu, Flávia L. Osório, Vikram Patel, Brian W. Pence, Philippe Persoons, Angelo Picardi, Katrin Reuter, Alasdair G. Rooney, Iná S. Santos, Juwita Shaaban, Abbey Sidebottom, Adam Simning, Lesley Stafford, Sharon Sung, Pei Lin Lynnette Tan, Alyna Turner, Henk C. van Weert, Jennifer White, Mary A. Whooley, Kirsty Winkley, Mitsuhiko Yamada, Andrea Benedetti, Brett D. Thombs
-
- Journal:
- Psychological Medicine / Volume 50 / Issue 16 / December 2020
- Published online by Cambridge University Press:
- 19 August 2019, p. 2816
-
- Article
-
- You have access Access
- HTML
- Export citation
Equivalency of the diagnostic accuracy of the PHQ-8 and PHQ-9: a systematic review and individual participant data meta-analysis
- Yin Wu, Brooke Levis, Kira E. Riehm, Nazanin Saadat, Alexander W. Levis, Marleine Azar, Danielle B. Rice, Jill Boruff, Pim Cuijpers, Simon Gilbody, John P.A. Ioannidis, Lorie A. Kloda, Dean McMillan, Scott B. Patten, Ian Shrier, Roy C. Ziegelstein, Dickens H. Akena, Bruce Arroll, Liat Ayalon, Hamid R. Baradaran, Murray Baron, Charles H. Bombardier, Peter Butterworth, Gregory Carter, Marcos H. Chagas, Juliana C. N. Chan, Rushina Cholera, Yeates Conwell, Janneke M. de Man-van Ginkel, Jesse R. Fann, Felix H. Fischer, Daniel Fung, Bizu Gelaye, Felicity Goodyear-Smith, Catherine G. Greeno, Brian J. Hall, Patricia A. Harrison, Martin Härter, Ulrich Hegerl, Leanne Hides, Stevan E. Hobfoll, Marie Hudson, Thomas Hyphantis, Masatoshi Inagaki, Nathalie Jetté, Mohammad E. Khamseh, Kim M. Kiely, Yunxin Kwan, Femke Lamers, Shen-Ing Liu, Manote Lotrakul, Sonia R. Loureiro, Bernd Löwe, Anthony McGuire, Sherina Mohd-Sidik, Tiago N. Munhoz, Kumiko Muramatsu, Flávia L. Osório, Vikram Patel, Brian W. Pence, Philippe Persoons, Angelo Picardi, Katrin Reuter, Alasdair G. Rooney, Iná S. Santos, Juwita Shaaban, Abbey Sidebottom, Adam Simning, Lesley Stafford, Sharon Sung, Pei Lin Lynnette Tan, Alyna Turner, Henk C. van Weert, Jennifer White, Mary A. Whooley, Kirsty Winkley, Mitsuhiko Yamada, Andrea Benedetti, Brett D. Thombs
-
- Journal:
- Psychological Medicine / Volume 50 / Issue 8 / June 2020
- Published online by Cambridge University Press:
- 12 July 2019, pp. 1368-1380
-
- Article
- Export citation
-
Background
Item 9 of the Patient Health Questionnaire-9 (PHQ-9) queries about thoughts of death and self-harm, but not suicidality. Although it is sometimes used to assess suicide risk, most positive responses are not associated with suicidality. The PHQ-8, which omits Item 9, is thus increasingly used in research. We assessed equivalency of total score correlations and the diagnostic accuracy to detect major depression of the PHQ-8 and PHQ-9.
MethodsWe conducted an individual patient data meta-analysis. We fit bivariate random-effects models to assess diagnostic accuracy.
Results16 742 participants (2097 major depression cases) from 54 studies were included. The correlation between PHQ-8 and PHQ-9 scores was 0.996 (95% confidence interval 0.996 to 0.996). The standard cutoff score of 10 for the PHQ-9 maximized sensitivity + specificity for the PHQ-8 among studies that used a semi-structured diagnostic interview reference standard (N = 27). At cutoff 10, the PHQ-8 was less sensitive by 0.02 (−0.06 to 0.00) and more specific by 0.01 (0.00 to 0.01) among those studies (N = 27), with similar results for studies that used other types of interviews (N = 27). For all 54 primary studies combined, across all cutoffs, the PHQ-8 was less sensitive than the PHQ-9 by 0.00 to 0.05 (0.03 at cutoff 10), and specificity was within 0.01 for all cutoffs (0.00 to 0.01).
ConclusionsPHQ-8 and PHQ-9 total scores were similar. Sensitivity may be minimally reduced with the PHQ-8, but specificity is similar.
Probability of major depression diagnostic classification using semi-structured versus fully structured diagnostic interviews
- Brooke Levis, Andrea Benedetti, Kira E. Riehm, Nazanin Saadat, Alexander W. Levis, Marleine Azar, Danielle B. Rice, Matthew J. Chiovitti, Tatiana A. Sanchez, Pim Cuijpers, Simon Gilbody, John P. A. Ioannidis, Lorie A. Kloda, Dean McMillan, Scott B. Patten, Ian Shrier, Russell J. Steele, Roy C. Ziegelstein, Dickens H. Akena, Bruce Arroll, Liat Ayalon, Hamid R. Baradaran, Murray Baron, Anna Beraldi, Charles H. Bombardier, Peter Butterworth, Gregory Carter, Marcos H. Chagas, Juliana C. N. Chan, Rushina Cholera, Neerja Chowdhary, Kerrie Clover, Yeates Conwell, Janneke M. de Man-van Ginkel, Jaime Delgadillo, Jesse R. Fann, Felix H. Fischer, Benjamin Fischler, Daniel Fung, Bizu Gelaye, Felicity Goodyear-Smith, Catherine G. Greeno, Brian J. Hall, John Hambridge, Patricia A. Harrison, Ulrich Hegerl, Leanne Hides, Stevan E. Hobfoll, Marie Hudson, Thomas Hyphantis, Masatoshi Inagaki, Khalida Ismail, Nathalie Jetté, Mohammad E. Khamseh, Kim M. Kiely, Femke Lamers, Shen-Ing Liu, Manote Lotrakul, Sonia R. Loureiro, Bernd Löwe, Laura Marsh, Anthony McGuire, Sherina Mohd Sidik, Tiago N. Munhoz, Kumiko Muramatsu, Flávia L. Osório, Vikram Patel, Brian W. Pence, Philippe Persoons, Angelo Picardi, Alasdair G. Rooney, Iná S. Santos, Juwita Shaaban, Abbey Sidebottom, Adam Simning, Lesley Stafford, Sharon Sung, Pei Lin Lynnette Tan, Alyna Turner, Christina M. van der Feltz-Cornelis, Henk C. van Weert, Paul A. Vöhringer, Jennifer White, Mary A. Whooley, Kirsty Winkley, Mitsuhiko Yamada, Yuying Zhang, Brett D. Thombs
-
- Journal:
- The British Journal of Psychiatry / Volume 212 / Issue 6 / June 2018
- Published online by Cambridge University Press:
- 02 May 2018, pp. 377-385
- Print publication:
- June 2018
-
- Article
-
- You have access Access
- HTML
- Export citation
-
Background
Different diagnostic interviews are used as reference standards for major depression classification in research. Semi-structured interviews involve clinical judgement, whereas fully structured interviews are completely scripted. The Mini International Neuropsychiatric Interview (MINI), a brief fully structured interview, is also sometimes used. It is not known whether interview method is associated with probability of major depression classification.
AimsTo evaluate the association between interview method and odds of major depression classification, controlling for depressive symptom scores and participant characteristics.
MethodData collected for an individual participant data meta-analysis of Patient Health Questionnaire-9 (PHQ-9) diagnostic accuracy were analysed and binomial generalised linear mixed models were fit.
ResultsA total of 17 158 participants (2287 with major depression) from 57 primary studies were analysed. Among fully structured interviews, odds of major depression were higher for the MINI compared with the Composite International Diagnostic Interview (CIDI) (odds ratio (OR) = 2.10; 95% CI = 1.15–3.87). Compared with semi-structured interviews, fully structured interviews (MINI excluded) were non-significantly more likely to classify participants with low-level depressive symptoms (PHQ-9 scores ≤6) as having major depression (OR = 3.13; 95% CI = 0.98–10.00), similarly likely for moderate-level symptoms (PHQ-9 scores 7–15) (OR = 0.96; 95% CI = 0.56–1.66) and significantly less likely for high-level symptoms (PHQ-9 scores ≥16) (OR = 0.50; 95% CI = 0.26–0.97).
ConclusionsThe MINI may identify more people as depressed than the CIDI, and semi-structured and fully structured interviews may not be interchangeable methods, but these results should be replicated.
Declaration of interestDrs Jetté and Patten declare that they received a grant, outside the submitted work, from the Hotchkiss Brain Institute, which was jointly funded by the Institute and Pfizer. Pfizer was the original sponsor of the development of the PHQ-9, which is now in the public domain. Dr Chan is a steering committee member or consultant of Astra Zeneca, Bayer, Lilly, MSD and Pfizer. She has received sponsorships and honorarium for giving lectures and providing consultancy and her affiliated institution has received research grants from these companies. Dr Hegerl declares that within the past 3 years, he was an advisory board member for Lundbeck, Servier and Otsuka Pharma; a consultant for Bayer Pharma; and a speaker for Medice Arzneimittel, Novartis, and Roche Pharma, all outside the submitted work. Dr Inagaki declares that he has received grants from Novartis Pharma, lecture fees from Pfizer, Mochida, Shionogi, Sumitomo Dainippon Pharma, Daiichi-Sankyo, Meiji Seika and Takeda, and royalties from Nippon Hyoron Sha, Nanzando, Seiwa Shoten, Igaku-shoin and Technomics, all outside of the submitted work. Dr Yamada reports personal fees from Meiji Seika Pharma Co., Ltd., MSD K.K., Asahi Kasei Pharma Corporation, Seishin Shobo, Seiwa Shoten Co., Ltd., Igaku-shoin Ltd., Chugai Igakusha and Sentan Igakusha, all outside the submitted work. All other authors declare no competing interests. No funder had any role in the design and conduct of the study; collection, management, analysis and interpretation of the data; preparation, review or approval of the manuscript; and decision to submit the manuscript for publication.
Longitudinal study of rotavirus infections among children from Belém, Brazil
- A. C. Linhares, Y. B. Gabbay, R. B. Freitas, E. S. Travassos da Rosa, J. D. P. Mascarenhas, E. C. B. Loureiro
-
- Journal:
- Epidemiology & Infection / Volume 102 / Issue 1 / February 1989
- Published online by Cambridge University Press:
- 15 May 2009, pp. 129-145
-
- Article
-
- You have access Access
- Export citation
-
From December 1982 to March 1986 a group of 80 children between 0 and 3 years old who lived in the peripheral area of Belém, Brazil, were followed up for episodes of diarrhoea. A total of 441 diarrhoeal episodes were recorded and 36 (8·2%) were associated with rotavirus. This agent was the only pathogen in 50% of rotavirus-related episodes of acute diarrhoea, and strains were characterized by analysis of RNA in polyacrylamide gels. Forty-one belonged to subgroup II (long pattern) and five to subgroup I. Reinfections by rotavirus were noted in 12 children involving either the same or different subgroups. Ten distinct electrophoretypes were detected in the study period and the predominant one had the ‘1N2L’ profile. The cumulative age-specific attack rate for diarrhoea reached 2–8 by the end of the first year of life; a frequency of 2–3 episodes of diarrhoea per child per year was observed throughout the complete investigation. In comparing the age-specific attack rates for diarrhoea between breast-fed and bottle-fed children, a peak at 6 months of age was noted in the former, and at 1 month in the latter. A comparison by Fischer's exact test (P = 0·21) provided no evidence for protection against clinical rotavirus disease by maternal milk. By the same test, however (P = 0·021), we found significant evidence that early rotavirus infections were more likely to be asymptomatic and that infections after 4 months were more likely to be symptomatic. The clinical picture in children with rotavirus-related diarrhoea was more severe than in those suffering from acute diarrhoea due to another agent.