8 results
Association between adverse childhood experiences and the number of suicide attempts in lifetime
- J. Andreo-Jover, E. Fernandez-Jimenez, J. Curto-Ramos, N. Angarita-Osorio, N. Roberto, A. De la Torre-Luque, A. Cebria, M. Diaz-Marsa, M. Ruiz-Veguillla, J. B. Bobes Garcia, M. Fe Bravo Ortiz, V. Perez Solá
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S561-S562
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Adverse childhood experiences (ACEs), defined as abuse, neglect, or a dysfunctional household in childhood, have been associated with suicidality (Fjeldsted et al., 2020). Every type of ACE has a direct impact on suicide ideation, self-harm and/or suicide attempt (Angelakis et al., 2019).
ObjectivesWe aim to quantify the association between types of ACEs (including emotional, physical, sexual abuse, and emotional and physical neglect) and the number of suicide attempts in lifetime.
MethodsWe included 748 patients who attempted suicide at least once. They were asked to complete the Columbia-Suicide Severity Rating Scale (CSSRS), and the Childhood Trauma Questionnaire-Short Form (CTQ-SF). Logistic regression models were run to assess the association between each ACE type and the number of suicide attempts.
ResultsPoisson univariate regression analyses show a linear trend in the relationship between having a higher number of suicide attempts and having suffered every ACE type in childhood (p<0.05). Our results show a lower percentage of previous suicide attempts among participants without ACEs, and an increasing tendency among patients with various types of ACEs. The rate of ACEs types is significantly higher in the group with previous suicide attempts than in the first-attempt group (p=0.000).
Image:
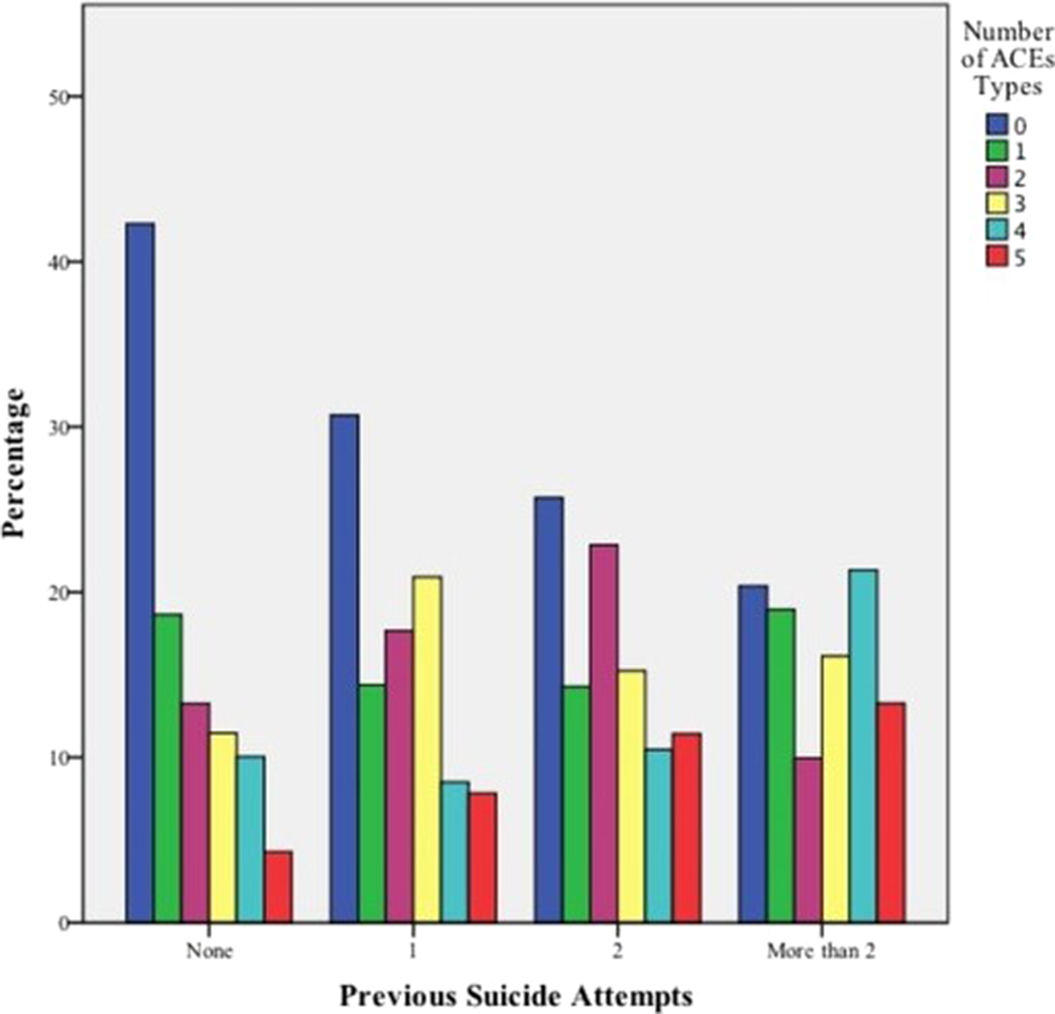
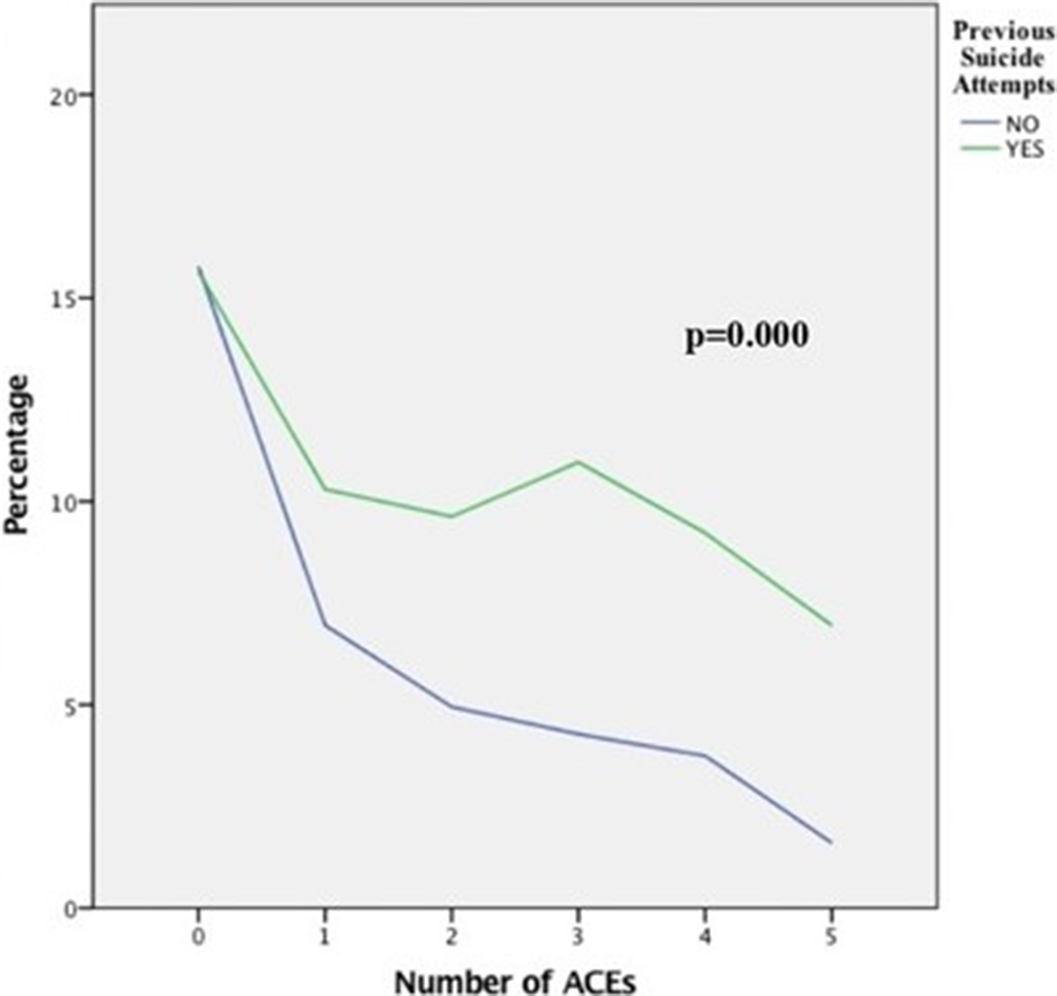
Image 2:
ConclusionsThis study contributes to clarify the role of childhood trauma in the number of suicide attempts in lifetime. This has important implications for reducing suicide rates, and preventing future re-attempts. Further studies analysing every construct of childhood trauma may contribute to the detection of suicidal behaviour.
FundingsThis work was supported by the Instituto de Salud Carlos III (grant number: PI19/00941 SURVIVE) and co-funded by the European Union (grant numbers: COV20/00988, PI17/00768), the European Union’s Horizon 2020 research and innovation programme Societal Challenges (grant number: 101016127), and the Fundación Española de Psiquiatría y Salud Mental
AcknowledgementsSURVIVE project (PI19/00941)
KeywordsSuicide attempt, Adverse Childhood Experiences
ReferencesAngelakis, I., Gillespie, E. L., & Panagioti, M. (2019). Childhood maltreatment and adult suicidality: A comprehensive systematic review with meta-analysis. Psychological Medicine, 49(7), 1057-1078. https://doi.org/10.1017/S0033291718003823
Fjeldsted, R., Teasdale, T. W., & Bach, B. (2020). Childhood trauma, stressful life events, and suicidality in Danish psychiatric outpatients. Nordic Journal of Psychiatry, 74(4), 280-286. https://doi.org/10.1080/08039488.2019.1702096
Disclosure of InterestNone Declared
AGESMind clinical trial: SocialMIND® results at 16 weeks
- M. P. Vidal-Villegas, A. Abad Pérez, P. Herrero Ortega, A. Oliva Lozano, J. Garde González, J. Andreo-Jover, A. Muñoz-Sanjosé, R. Mediavilla, B. Rodríguez-Vega, G. Lahera, Á. Palao-Tarrero, C. Bayón-Pérez, M. F. Bravo-Ortiz
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S480-S481
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Early intervention on a first psychotic episode is fundamental for a more favorable prognosis, and it usually combines pharmacological treatment, which mainly affects positive psychotic symptoms, with interventions that can improve the rest of the symptoms and associated problems such as deterioration in social functioning (Harvey & Penn, 2010; Fusar-Poli, McGorry & Kane, 2017). While Mindfulness is gaining more and more prominence in the field of psychotherapy (Chan et al., 2019; Cillesen et al., 2019), social cognition and social functioning are being researched as key targets on which to intervene after a first psychotic episode (Green, Horan & Lee, 2015).
SocialMIND® is a mindfulness-based social cognition training tailor-made to improve social functioning in people who have suffered a first psychotic episode within the last five years. It is currently being compared with a group Psychoeducational Multicomponent Intervention (PMI) in a Randomized Controlled Trial (RCT) (Mediavilla et al., 2019). Both group psychotherapies include 17 sessions delivered over a 9 month period: 8 weekly sessions, 4 biweekly sessions and 5 monthly sessions.
The results of SocialMIND® at 8 weeks showed improvements in social cognition and social functioning, specifically on affective social cognition and self-care (Mediavilla et al., 2021).
ObjectivesTo evaluate the efficacy of SocialMIND® in improving social functioning, measured by the Personal and Social Functioning (PSP) scale 16 weeks after starting the intervention, in people who have suffered a first psychotic episode in the last 5 years.
MethodsRandomized, controlled pilot trial (use of a psychoeducational multicomponent intervention or PMI as active comparator) of two parallel groups (SocialMIND® and PMI) with a 1:1 ratio using a blind evaluator.
ResultsNo statistically significant differences were found in the social functioning variable between the two treatment arms. Intragroup differences are observed in other secondary variables studied (social cognition) 16 weeks after starting the interventions.
ConclusionsSocialMIND® has not been shown to be more effective than a PMI in improving social functioning at 16 weeks after starting the intervention in people who have suffered a first psychotic episode in the five years prior to being included in the study.
Disclosure of InterestNone Declared
Psychiatric comorbidity profiles among suicidal attempters: A cohort study
- Y. Sanchez-Carro, M. Diaz-Marsa, V. Fernandez-Rodrigues, W. Ayad-Ahmed, A. Pemau, I. Perez-Diaz, A. Galvez-Merlin, P. de la Higuera-Gonzalez, V. Perez-Sola, P. Saiz, I. Grande, A. Cebria, J. Andreo-Jover, P. Lopez-Peña, M. Ruiz-Veguilla, A. de la Torre-Luque
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S318-S319
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
More than 700,000 people die by suicide in 2019 globally (World Health Organitation 2021). Mental health problems constitute a risk factor for suicidal behavior and death by suicide (Hoertel et al. Mol Psychiatry 2015; 20 718–726). Different mental disorders have been related to different forms of suicidal ideation and behavior (Conejero et al. Curr Psychiatry Rep 2018; 20, 33) (Quevedo et al. Compr Psychiatry 2020; 102 152194). However, little is known on comorbidity profiles among suicide attempters.
ObjectivesThe aim of our work was to identify the psychiatric comorbidity profiles of individuals who were admitted a hospital emergency department due to a suicide attempt. Moreover, it intended to know their clinical characteristics according to comorbidity profile.
MethodsA sample of 683 attempters (71.30% female; M age= 40.85, SD= 15.48) from the SURVIVE study was used. Patients were assessed within the 15 days after emergency department admission. Sociodemographic (i.e., sex, age, marital status and employment status) and clinical data were collected. The International Neuropsychiatric Interview (MINI) was used to assess DSM-V Axis 1 mental health diagnoses and the Columbia Suicide Rating Scale (C-SSRS) to assess suicidal ideation and behavior. The Acquired Capacity for Suicide-Fear of Death Scale (ACSS-FAD), the Patient Health Questionnaire (PHQ-9) to assess the frequency of depressive symptoms during the past 2 weeks, and the General Anxiety Disorder-7 (GAD-7) scale to assess symptoms of worry and anxiety were also conducted. For the identification of comorbidity profiles, latent class analysis framework was followed considering diagnosis to each individual disorder as clustering variables. On the other hand, binary logistic regression was used to study the relationship between comorbidity profile membership and clinical factors.
ResultsTwo classes were found (Class I= mild symptomatology class, mainly featured by emotional disorder endorsement; and Class II= high comorbidity class, featured by a wide amount of endorsed diagnoses) (see figure 1). Individuals from the High comorbidity class were more likely to be female (OR= 0.98, p<.05), younger in age (OR= 0.52, p< .01), with more depressive symptoms (OR=1.09, p<.001) and have greater impulsivity (OR= 1.01, p<.05).
Image:
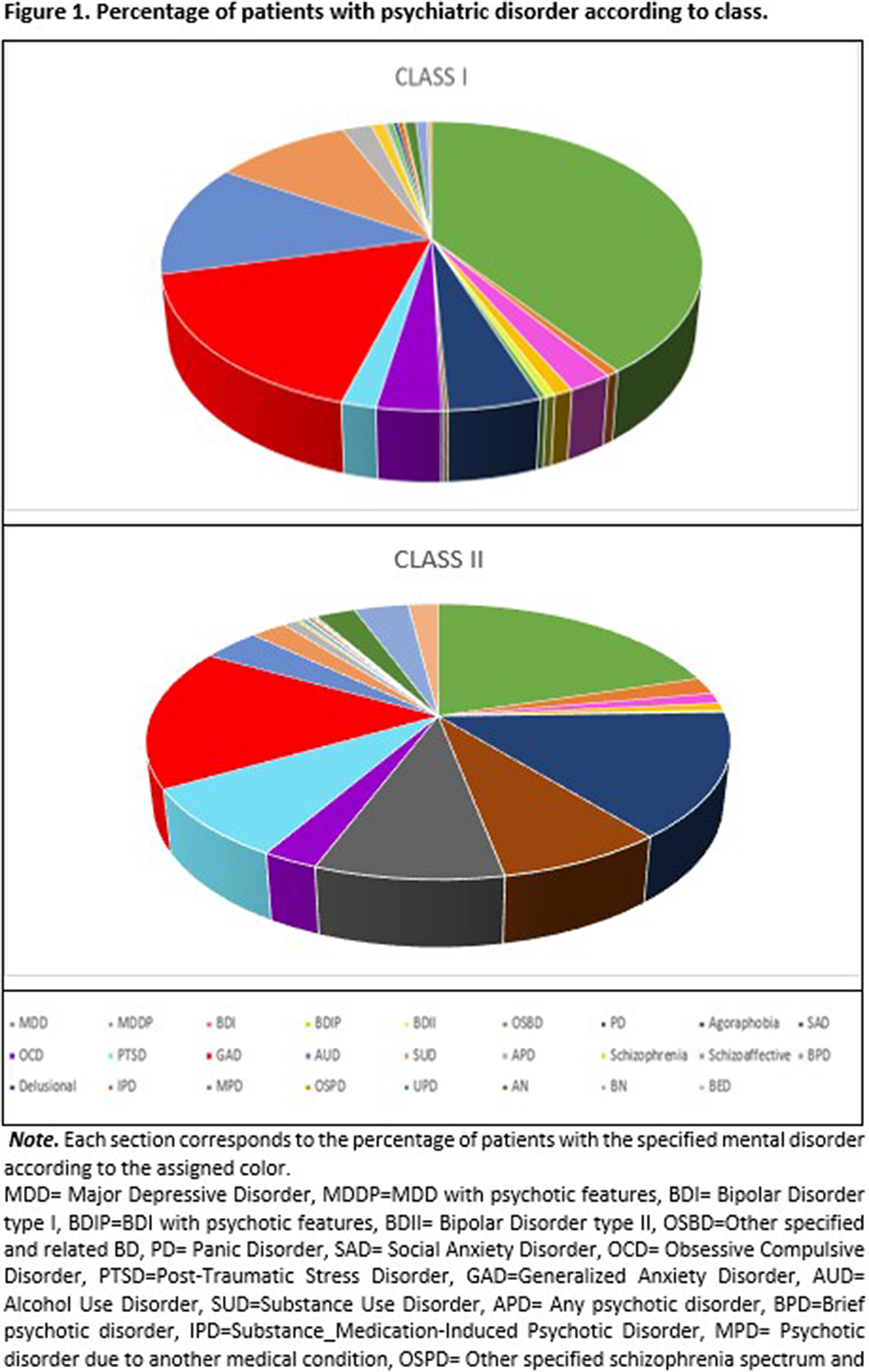 Conclusions
ConclusionsWe found two profiles of people with suicidal behavior based on the presence of mental disorders. Each of the suicidal subtypes had different associated risk factors. They also had a different profile of suicidal behavior.
Disclosure of InterestNone Declared
Changes in the characteristics of Suicide Attempts during COVID-19 pandemic
- J. Curto Ramos, N. Kishanchandani Chandiramani, M. Torrijos, J. Andreo-Jover, B. Orgaz-Alvarez, M. Velasco, D. García Martínez, G. Juárez, S. Cebolla, P. Aguirre, B. Rodríguez Vega
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S405
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Different studies indicate high prevalence’s of suicidal behaviour, anxiety, depression, insomnia, and PTSD associated with the COVID-19 pandemic. There is currently not enough scientific evidence available to analyze the impact that the COVID-19 pandemic has had on the rate of suicide attempts and their characteristics.
ObjectivesTo analyze and compare the characteristics of suicidal behavior (in terms of method, severity, medical damage produced and need for hospitalization) of patients attended during the COVID-19 pandemic compared to previous years.
MethodsA retrospective study was performed based on a standardized data collection of patients attending the University Hospital La Paz between April 2018 and November 2021. 581 patients who attempted suicide at least once were included in this study. We compared the severity using the Beck Suicide Intent Scale. Chi-square ant Student’s t were used to compare clinical characteristics such as medical damage, method of suicide attempt and indication for admission after the attempt, between suicide attempts during the COVID-19 pandemic and previous years.
ResultsOur results suggest that during the COVID-19 pandemic suicide attempts caused more medical damage (p<0.001), had higher severity (p<0.000), and required more admission in Intensive Care Units, General Internal Medicine and Psychiatry compared with pre-Covid years (p<0.000).
ConclusionsThis is the first study in Spain analysing the changes in characteristics of suicide attempts during the COVID-19 pandemic. This has important implications for reducing suicide rates, preventing future attempts, and enabling us to design specific treatments of Suicidal Behaviour.
Disclosure of InterestNone Declared
Assessment of Theory of Mind in Psychopathology: a Scoping Review
- P. de la Higuera-Gonzalez, A. Galvez-Merlin, E. Rodríguez-Toscano, J. Andreo-Jover, T. Lopez-Soto, A. de la Torre-Luque
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1001-S1002
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Theory of Mind (ToM) is defined as the cognitive ability that infers other’s mental states (Premack & Woodruff. J Behav Brain Sci 1978; 1 515-526).The interest in the study of ToM distinguishing its affective and cognitive components has been growing. Its study in psychopathology has been evolved from its original studies in autism spectrum disorders (ASD), schizophrenia (SCZ) and, borderline personality disorder (BPD), to other mental disorders like major depressive disorder (MDD), bipolar disorder (BP), anorexia nervosa (AN) and social anxiety disorder (SAD).
Objectives1) review the most commonly used instruments for ToM assessment; 2) to compile the evidence on ToM deficits across mental disorders. For both objectives, target disorders are previously mentioned.
MethodsThe search was carried out on the PubMed, PsycInfo and Scopus databases, using the terms “Theory of mind”, “Mentalization” and the previously mentioned mental disorders and pertinent thesaurus. Articles in English, published since 2010 were considered. A 2-step strategy (first, article screening and full reading) was followed to select articles of interest.
ResultsReading the Mind in the Eyes (Baron-Cohen et al., J Child Psychol Psychiatry 2001; 42 241-251) and Movie for the Assessment of Social Cognition (Dziobeck et al. J Autism Dev Disord 2006; 36 623-636) were the most commonly used tasks to assess ToM. Regarding mental disorders, studies showed deficits in cognitive and affective ToM skills in ASD, SCZ, BPD, MDD and BP. Hypomentalization was mainly observed in ASD and MDD, while BPD and SCZ were featured by errors associated with hypermentalization. Studies in AN and SAD are scarce, but they mainly highlight a cognitive ToM deficit, with hypomentalization in AN and hypermentalization in ASD. In all of them, depressive symptomatology seems to be a critical moderator of ToM performance.
ConclusionsAlthough ToM impairments are well described for some mental disorders, more research is needed to reach solid conclusions for others. The use of different and heterogeneous ToM assessment instruments can strongly influence the results of studies. The study of ToM is essential to gain a better understanding of the diseases and to develop effective treatments targeting specific ToM deficits.
Disclosure of InterestNone Declared
Mental health service requirements after hospitalization due to COVID-19: a 1- year follow-up study
- J. Andreo Jover, M.P. Vidal-Villegas, R. Mediavilla, I. Louzao Rojas, S. Cebolla Lorenzo, E. Fernández Jiménez, A. Muñoz-Sanjosé, M.F. Bravo-Ortiz, G. Martinez-Ales, C. Bayón-Pérez
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S381
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Long-term COVID-19 effects has been recently described as persistent and prolonged symptoms after an acute and severe SARS-COV-2 (1). An important concern is that the sequelae of severe COVID-19 may suppose a substantial outpatient 's burden for the specialized services in reopening pandemic phase (2).
ObjectivesTo describe the frequency of mental health service use in COVID-19 hospitalized patients after discharge and to estimate the costs associated to the post- discharge consultations.
MethodsWe used a 1-year follow-up cohort of 1455 COVID-19 inpatients hospitalized in La Paz University Hospital of Madrid, Spain between March 16th and April 15th, 2020. Data were retrieved from Psychiatry Service (PS) electronic health records and we described the frequency of mental health reason for consultation. We used information published by the Madrid health Office to estimate the cost of initial and following appointments.
ResultsOur sample consisted of 1,455 patients admitted with a COVID-19 diagnosis between March 16th and April 15th, 2020, and then discharged. Roughly half of them were men (776, 53%), 238 (16%) had a prior history of mental health problems, and 44 (3%) died. 193 participants (13%) visited the mental health department after being discharged. The total cost was estimated in 103,581 USD, of which two-thirds corresponded to patients with prior history of mental health problems.
ConclusionsOur results indicate that the mental health burden of severe COVID-19 inpatient s after discharge was substantial during the first year of follow-up. This generate important economic impact to mental health providers and society at large.
DisclosureNo significant relationships.
Paralization and online adaptation of an ongoing clinical trial in La Paz University Hospital (Madrid, Spain) during the COVID-19 worldwide pandemic
- M.P. Vidal-Villegas, J. Andreo Jover, R. Mediavilla, A. Muñoz-Sanjosé, B. Rodríguez-Vega, C. Bayón-Pérez, Á. Palao Tarrero, M.F. Bravo-Ortiz
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S617-S618
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Spain went into lockdown in March of 2020 due to the COVID-19 outbreak. We had to stop the third randomization of our ongoing clinical trial (Mediavilla et al., 2019), pausing weekly group psychotherapy for 12 people with a first episode of psychosis. Only 5 weekly sessions had been delivered, thus many were just starting to form a therapeutic link with the group. In a public health emergency context, psychotherapeutic groups are considered avoidable gatherings. However, stopping psychological therapy abruptly can make participants more vulnerable. The intervention groups were launched in an online format because we could not let anyone go without psychological support in such a difficult time.
ObjectivesCommunicate how we adapted an ongoing clinical trial to an online format during the lockdown in Spain.
MethodsIn light of our participants’ needs and their acute deterioration the first two weeks of lockdown, we adapted our intervention. First, both arms (mindfulness-based v. psychoeducational multicomponent intervention) began online adaptations of the interventions. Second, a research assistant made weekly phone calls to provide basic psychosocial support, assure participants groups would continue, and later remind them of each online session. Third and last, the phoneline was accessible 24/7 (WhatsApp).
ResultsThe third randomization concluded in December. Six participants were lost in the transition to online groups. However, adherence was comparable to the previous two randomizations (4/12 completed the intervention).
ConclusionsOnline psychotherapy may be used in emergencies such as a lockdown. However, the psychological mid- and long-term effects of a lockdown and online group therapy remain unknown.
DisclosureNo significant relationships.
Child psychiatric emergency visits during the COVID-19 pandemic
- J. Andreo Jover, D. Hernandez Calle, J. Curto-Ramos, L. Vicente Valor, D. García Martínez, G. Juárez, M. Alcamí, A. Ortiz, N. Iglesias, M.F. Bravo-Ortiz, G. Martinez-Ales, B. Rodríguez-Vega
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S510-S511
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Paediatric and adult psychiatric emergency department (ED) visits decreased during the initial COVID-19 pandemic outbreak. Long-term consequences of the pandemic will include increases in mental healthcare needs especially among especially vulnerable groups such as children and adolescents.
ObjectivesThis study examined changes in the number of overall and diagnosis-specific mental health ED visits among patients aged <18 years following onset of the COVID-19 pandemic in Madrid, Spain.
MethodsWe used electronic health records to extract the monthly numbers of total and diagnosis-specific mental health ED visits among patients aged <18 years, between October 2018 and April 2021, to La Paz University Hospital. We conducted interrupted time-series analyses and compared trends before and after the day of the first ED COVID-19 case (1st March 2020).
ResultsIn March 2020, there was a marked initial decrease of -12.8 (95%CI -21.9, -7.9) less monthly mental health ED visits. After April 2020, there was a subsequent increasing trend of 3.4 (95%CI 2.6, 4.2) additional monthly mental health ED visits.
ConclusionsAfter onset of the COVID-19 pandemic, there was an increase in paediatric psychiatric ED visits, especially due to suicide-related reasons. These data reinforce the crucial role of the ED in the management of acute mental health problems among youth and highlight the need for renovated efforts to enhance access to care outside of and during acute crises during the pandemic and its aftermath.
DisclosureNo significant relationships.






