103 results
F.1 Oscillatory network markers of subcallosal cingulate deep brain stimulation for depression
- IE Harmsen, M Scherer, N Samuel, GJ Elias, J Germann, A Boutet, P Giacobbe, NC Rowland, L Milosevic, AM Lozano
-
- Journal:
- Canadian Journal of Neurological Sciences / Volume 51 / Issue s1 / June 2024
- Published online by Cambridge University Press:
- 24 May 2024, p. S12
-
- Article
-
- You have access Access
- Export citation
-
Background: Identifying functional biomarkers related to treatment success can aid in optimizing therapy and provide a better understanding of the neural mechanisms of treatment-resistant depression (TRD) and subcallosal cingulate deep brain stimulation (SCC-DBS). Methods: Magnetoencephalography data were obtained from 16 individuals with SCC-DBS for TRD and 25 healthy subjects. We identified region-specific oscillatory modulations that both (i) discriminate individuals with TRD (SCC-DBS OFF) from healthy controls and (ii) discriminate responders from non-responders (SCC-DBS ON). The effects of stimulation intensity and frequency were also explored. Results: Discriminative regions that differentiated responders from non-responders based on modulations of increased alpha (8-12 Hz) and decreased gamma (32-116 Hz) power included nodes of the default mode, central executive, and somatomotor networks, Broca’s area, and lingual gyrus. Furthermore, low stimulation frequency had stronger effects on oscillatory modulation. Conclusions: The identified functional biomarkers implicate modulations of TRD-related activity in brain regions involved in emotional control/processing, motor control, and interactions between speech, vision, and memory – all implicated in depression. These electrophysiological biomarkers have the potential to be used as functional proxies for therapy optimization. Additional stimulation parameter analyses revealed that oscillatory modulations are strengthened by increasing stimulation intensity or reducing frequency, which may benefit SCC-DBS non-responders.
E.3 fMRI correlates of symptom-specific improvement in STN deep brain stimulation
- B Santyr, A Loh, J Germann, A Boutet, A Ajala, J Qiu, M Abbass, A Fasano, A Lozano
-
- Journal:
- Canadian Journal of Neurological Sciences / Volume 51 / Issue s1 / June 2024
- Published online by Cambridge University Press:
- 24 May 2024, p. S11
-
- Article
-
- You have access Access
- Export citation
-
Background: Subthalamic nucleus (STN) deep brain stimulation (DBS) improves the cardinal symptoms of Parkinson’s disease (PD). However, the therapeutic mechanisms are incompletely understood. By leveraging patient-specific brain responses to DBS using functional magnetic resonance imaging (fMRI) acquired during stimulation, we identify and validate symptom-specific networks associated with clinical improvement. Methods: Forty PD patients with STN-DBS were enrolled for fMRI using a 30-sec DBS-ON/OFF cycling paradigm. The four cardinal motor outcomes of PD were chosen a priori and measured using the Movement Disorder Society-Sponsored Revision of the Unified Parkinson’s Disease Rating Scale, part III (MDS-UPDRSIII): axial instability, tremor, rigidity, bradykinesia. Stimulation-dependent changes in blood oxygen level-dependent (BOLD) signal were correlated with each symptom. Results: The relationship between BOLD response and outcomes revealed significant networks of clinical response (p<0.001). Using BOLD responses from the network hubs, each symptom-specific model was significantly predictive of actual improvement: axial instability (R2=0.38, p=0.000026), bradykinesia (R2=0.29, p=0.00033), rigidity (R2=0.40, p=0.000013), tremor (R2=0.26, p=0.00073). Conclusions: Using patient-specific imaging, we provide evidence of an association between DBS-evoked fMRI response and individual symptom improvement. Brain networks associated with clinical improvement were different depending on the PD symptom examined, suggesting the presence of symptom-specific networks of efficacy which may allow personalization of DBS therapy.
P.078 fMRI-based deep brain stimulation programming: a blinded, crossover clinical trial
- B Santyr, A Ajala, I Alhashyan, J Germann, J Qiu, A Boutet, A Fasano, A Lozano
-
- Journal:
- Canadian Journal of Neurological Sciences / Volume 51 / Issue s1 / June 2024
- Published online by Cambridge University Press:
- 24 May 2024, pp. S37-S38
-
- Article
-
- You have access Access
- Export citation
-
Background: Success of deep brain stimulation (DBS) in Parkinson’s disease (PD) relies on time-consuming trial-and-error testing of stimulation settings. Here, we prospectively compared an fMRI-based stimulation optimization algorithm with >1 year of standard-of-care (SoC) programming in a double-blind, crossover, non-inferiority trial. Methods: Twenty-seven PD-DBS patients were prospectively enrolled for fMRI using a 30-sec DBS-ON/OFF cycling paradigm. Optimal settings were identified using our published classification algorithm. Subjects then underwent >1 year of SoC programming. Clinical improvement was assessed, after an overnight medication washout period, under SoC and fMRI-determined stimulation conditions. A predefined non-inferiority margin was -5 points on the Unified Parkinson’s Disease Rating Scale (UPDRSIII). Results: UPDRSIII improved from 45.3 (SD=14.6) at baseline to 24.9 (SD=10.9) and 24.1 (SD=10.9) during SoC and fMRI-determined stimulation, respectively. The mean difference in scores was 0.8 (SD=8.5; 95% CI -4.5 to 6.2). The non-inferiority margin was not contained within the 95% confidence interval, establishing non-inferiority (p=0.013). Conclusions: This is the first prospective evaluation of an algorithm able to suggest stimulation parameters solely from the fMRI response to stimulation. It suggests equivalent outcomes may be achieved in 3 hours of fMRI scanning immediately after surgery compared to SoC requiring 6 or more in-person clinic visits throughout >1 year.
Evidence-based recruitment strategies for clinical research: Study personnel’s and research participants’ perceptions about successful methods of outreach for a U.S. Autism-Research Cohort
- Robin P. Goin-Kochel, Ivana Lozano, Gabrielle Duhon, Gabriela Marzano, Amy Daniels, J. Kiely Law, Katharine Diehl, LeeAnne Green Snyder, Pamela Feliciano, Wendy K. Chung, SPARK Consortium
-
- Journal:
- Journal of Clinical and Translational Science / Volume 8 / Issue 1 / 2024
- Published online by Cambridge University Press:
- 02 April 2024, e65
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Introduction:
Under enrollment of participants in clinical research is costly and delays study completion to impact public health. Given that research personnel make decisions about which strategies to pursue and participants are the recipients of these efforts, we surveyed research staff (n = 52) and participants (n = 4,144) affiliated with SPARK (Simons Foundation Powering Autism for Knowledge) – the largest study of autism in the U.S. – to understand their perceptions of effective recruitment strategies.
Methods:In Study 1, research personnel were asked to report recruitment strategies that they tried for SPARK and to indicate which ones they would and would not repeat/recommend. In Study 2, SPARK participants were asked to indicate all the ways they heard about the study prior to enrollment and which one was most influential in their decisions to enroll.
Results:Staff rated speaking with a SPARK-study-team member (36.5%), speaking with a medical provider (19.2%), word of mouth (11.5%), and a live TV news story (11.5%) as the most successful strategies. Participants most often heard about SPARK via social media (47.0%), speaking with a medical provider (23.1%), and an online search (20.1%). Research personnel’s and participants’ views on effective recruitment strategies often differed, with the exception of speaking with a medical provider.
Conclusion:Results suggest that a combination of strategies is likely to be most effective in reaching diverse audiences. Findings have implications for the selection of strategies that meet a study’s specific needs, as well as recruitment-strategy “combinations” that may enhance the influence of outreach efforts.
22 Cordoba Naming Test Performance and Acculturation in a Geriatric Population
- Isabel C.D. Muñoz, Krissy E. Smith, Santiago I. Espinoza, Diana M. R. Maqueda, Adriana C. Cuello, Ana Paula Pena, Carolina Garza, Raymundo Cervantes, Jill Razani, Tara L. Victor, David J. Hardy, Alberto L. Fernandez, Natalia Lozano Acosta, Daniel W. Lopez-Hernandez
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 335-336
-
- Article
-
- You have access Access
- Export citation
-
Objective:
A commonly used confrontation naming task used in the United States is The Boston Naming Test (BNT). Performance differences has been found in Caucasian and ethnic minorities on the BNT. The Cordoba Naming Test (CNT) is a 30-item confrontation naming task developed in Argentina. Past research has shown acculturation levels can influence cognitive performance. Furthermore, one study evaluated geriatric gender differences on CNT performance in Spanish. Researchers reported that older male participants outperformed female participants on the CNT. To our knowledge, researchers have not evaluated ethnic differences on the CNT using a geriatric sample. The purpose of the present study was to examined CNT performance and acculturation in a Latinx and Caucasian geriatric sample. It was predicted the Caucasian group would outperform the Latinx group on the CNT. Moreover, the Caucasian group would report higher acculturation levels on the Abbreviated Multidimensional Acculturation Scale (AMAS) compared to the Latinx group.
Participants and Methods:The sample consisted of 9 Latinx and 11 Caucasian participants with a mean age of 66.80 (SD =6.10), with an average of 14.30 (SD = 2.00) years of education. All participants were neurologically and psychologically healthy and completed the CNT and the AMAS in English. Acculturation was measured via the AMAS English subscales (i.e., English Language, United States. Identity, United States, Competency). A series of ANCOVAs, controlling for years of education completed and gender, was used to evaluate CNT performance and acculturation.
Results:The ethnic groups were not well demographically matched (i.e., years of education and gender).We found that the Caucasian group outperformed the Latinx group on CNT performance p = .012, ηp 2 = .34. Furthermore, the Caucasian group reported higher acculturation levels (i.e., English Language, United States, Identity, United States, Competency) compared to the Latinx group p’s < .05, ηps2 = .42-.64.
Conclusions:To our knowledge, this is the first study to evaluate CNT performance between ethnic groups with a geriatric sample. As expected the Caucasian group outperformed the Latinx group on the CNT. Also, as expected the Caucasian group reported higher English acculturation levels compared to the Latinx group. Our findings are consistent with past studies showing ethnic differences on confrontational naming performance (i.e., The Boston Naming Test), favoring Caucasians. A possible explanation for group differences could have been linguistic factors (e.g., speaking multiple languages) in our Latinx group. Therefore, since our Latinx group reported lower levels of English Language, United States identity, and United States competency the Latinx group assimilation towards United States culture might of influence their CNT performance. Future studies with different ethnic groups (e.g., African-Americans) and a larger sample size should examine if ethnic differences continue to cross-validate in a geriatric sample.
30 Analyzing Spanish Speakers Cordoba Naming Test Performance
- Raymundo Cervantes, Isabel D.C. Munoz, Estefania J. Aguirre, Natalia Lozano Acosta, Mariam Gomez, Adriana C. Cuello, Krissy E. Smith, Diana I. Palacios Mata, Krithika Sivaramakrishnan, Yvette De Jesus, Santiago I. Espinoza, Diana M. R. Maqueda, David J. Hardy, Tara L. Victor, Alberto L. Fernandez, Daniel W. Lopez-Hernandez
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 443-444
-
- Article
-
- You have access Access
- Export citation
-
Objective:
A 30-item confrontation naming test was developed in Argentina for Spanish speakers, The Cordoba Naming Test (CNT). The Boston Naming Test is an established confrontation naming task in the United States. Researchers have used the Boston Naming Test to identify individuals with different clinical pathologies (e.g., Alzheimer’s disease). The current literature on how Spanish speakers across various countries perform on confrontational naming tasks is limited. To our knowledge, one study investigated CNT performance across three Spanish-speaking countries (i.e., Argentina, Mexico, and Guatemala). Investigators found that the Guatemalan group underperformed on the CNT compared to the Argentine and Mexican groups. The purpose of this study was to extend the current literature and investigate CNT performance across five Spanish-speaking countries (i.e., Argentina, Mexico, Guatemala, Colombia, United States). We predicted that the Argentine group would outperform the other Spanish-speaking countries.
Participants and Methods:The present study sample consisted of 502 neurologically and psychologically healthy participants with a mean age of 29.06 (SD = 13.41) with 14.75 years of education completed (SD = 3.01). Participants were divided into five different groups based on their country of birth and current country residency (i.e., United States, Mexico, Guatemala, Argentina, & Colombia). All participants consented to voluntary participation and completed the CNT and a comprehensive background questionnaire in Spanish. The CNT consisted of 30 black and white line drawings, ranging from easy to hard in difficulty. An ANCOVA, controlling for gender, education, and age, was used to evaluate CNT performance between the five Spanish-speaking country groups. Meanwhile, a Bonferroni post-hoc test was utilized to evaluate the significant differences between Spanish-speaking groups. We used a threshold of p < .05 for statistical significance.
Results:Results revealed significant group differences between the five Spanish speaking groups on the CNT, p = .000, np2 = .48. Bonferroni post-hoc test revealed that the United States group significantly underperformed on the CNT compared to all the Spanish-speaking groups. Next, we found the Guatemalan group underperformed on the CNT compared to the Argentinian, Mexican, and Colombian groups. Additionally, we found the Argentinian group outperformed the Mexican, Guatemalan, and United States groups on the CNT. No significant differences were found between the Argentinian group and Colombian group or the Mexican group and Colombian group on the CNT.
Conclusions:As predicted, the Argentinian group outperformed all the Spanish-speaking groups on the CNT except the Colombian group. Additionally, we found that the United States group underperformed on the CNT compared to all the Spanish-speaking groups. A possible explanation is that Spanish is not the official language in the United States compared to the rest of the Spanish-speaking groups. Meanwhile, a possible reason why the Argentinian and Colombian groups demonstrated better CNT performances might have been that it was less culturally sensitive than the United States, Mexican, and Guatemalan groups. Further analysis is needed with bigger sample sizes across other Spanish-speaking countries (e.g., Costa Rica, Chile) to evaluate what variables, if any, are influencing CNT performance.
Impact of Hurricanes Irma and Maria on Asthma, Hypertension, and Depression in a Sample of the Puerto Rico Population
- Marijulie Martínez-Lozano, Frank Fraticelli, Jessica Irizarry, Israel Almodóvar-Rivera, Martha Nunn, Kaumudi J. Joshipura
-
- Journal:
- Disaster Medicine and Public Health Preparedness / Volume 17 / 2023
- Published online by Cambridge University Press:
- 13 October 2023, e508
-
- Article
- Export citation
-
Objective:
To evaluate the impact of Hurricanes Irma and Maria on 3 major chronic diseases in Puerto Rico.
Methods:San Juan Overweight Adults Longitudinal study participants were re-evaluated after Hurricanes Irma and Maria (May 2019–July 2020) for the Preparedness to Reduce Exposures and Diseases Post-hurricanes and Augment Resilience study. This study compared the prevalence and incidence of asthma, depression, and hypertension within the same 364 individuals over time.
Results:Asthma and depression prevalence and incidence did not change significantly after the hurricanes. The prevalence of hypertension increased significantly after the hurricanes (OR = 2.2, 95% CI: 1.2, 3.9). The incidence of hypertension after the hurricanes (IR = 9.0, 95% CI: 6.5, 12.4) increased significantly compared to before the hurricanes (IR = 6.1, 95% CI: 4.5, 8.0) (age-adjusted incidence rate ratio [aIRR] = 1.4, 95% CI: 4.5, 8.0) for similar time periods.
Conclusion:Hurricanes Irma and Maria were associated with a significant increase in the prevalence and incidence of hypertension in this study population. Contrary to expectations, no significant increases were observed in depression and asthma prevalence after the hurricanes. Results from this study can inform better strategies to prevent and manage hypertension in the population affected by a hurricane.
Coronavirus disease 2019 is associated with long-term depressive symptoms in Spanish older adults with overweight/obesity and metabolic syndrome
- Sangeetha Shyam, Carlos Gómez-Martínez, Indira Paz-Graniel, José J. Gaforio, Miguel Ángel Martínez-González, Dolores Corella, Montserrat Fitó, J. Alfredo Martínez, Ángel M. Alonso-Gómez, Julia Wärnberg, Jesús Vioque, Dora Romaguera, José López-Miranda, Ramon Estruch, Francisco J. Tinahones, José Manuel Santos-Lozano, J. Luís Serra-Majem, Aurora Bueno-Cavanillas, Josep A. Tur, Vicente Martín Sánchez, Xavier Pintó, María Ortiz Ramos, Josep Vidal, Maria Mar Alcarria, Lidia Daimiel, Emilio Ros, Fernando Fernandez-Aranda, Stephanie K. Nishi, Oscar García Regata, Estefania Toledo, Jose V. Sorli, Olga Castañer, Antonio Garcia-Rios, Rafael Valls-Enguix, Napoleon Perez-Farinos, M. Angeles Zulet, Elena Rayó-Gago, Rosa Casas, Mario Rivera-Izquierdo, Lucas Tojal-Sierra, Miguel Damas-Fuentes, Pilar Buil-Cosiales, Rebeca Fernández-Carrion, Albert Goday, Patricia J. Peña-Orihuela, Laura Compañ-Gabucio, Javier Diez-Espino, Susanna Tello, Ana González-Pinto, Víctor de la O, Miguel Delgado-Rodríguez, Nancy Babio, Jordi Salas-Salvadó
-
- Journal:
- Psychological Medicine / Volume 54 / Issue 3 / February 2024
- Published online by Cambridge University Press:
- 05 September 2023, pp. 620-630
-
- Article
- Export citation
-
Background
The coronavirus disease 2019 (COVID-19) has serious physiological and psychological consequences. The long-term (>12 weeks post-infection) impact of COVID-19 on mental health, specifically in older adults, is unclear. We longitudinally assessed the association of COVID-19 with depression symptomatology in community-dwelling older adults with metabolic syndrome within the framework of the PREDIMED-Plus cohort.
MethodsParticipants (n = 5486) aged 55–75 years were included in this longitudinal cohort. COVID-19 status (positive/negative) determined by tests (e.g. polymerase chain reaction severe acute respiratory syndrome coronavirus 2, IgG) was confirmed via event adjudication (410 cases). Pre- and post-COVID-19 depressive symptomatology was ascertained from annual assessments conducted using a validated 21-item Spanish Beck Depression Inventory-II (BDI-II). Multivariable linear and logistic regression models assessed the association between COVID-19 and depression symptomatology.
ResultsCOVID-19 in older adults was associated with higher post-COVID-19 BDI-II scores measured at a median (interquartile range) of 29 (15–40) weeks post-infection [fully adjusted β = 0.65 points, 95% confidence interval (CI) 0.15–1.15; p = 0.011]. This association was particularly prominent in women (β = 1.38 points, 95% CI 0.44–2.33, p = 0.004). COVID-19 was associated with 62% increased odds of elevated depression risk (BDI-II ≥ 14) post-COVID-19 when adjusted for confounders (odds ratio; 95% CI 1.13–2.30, p = 0.008).
ConclusionsCOVID-19 was associated with long-term depression risk in older adults with overweight/obesity and metabolic syndrome, particularly in women. Thus, long-term evaluations of the impact of COVID-19 on mental health and preventive public health initiatives are warranted in older adults.
Group psychotherapy for patients with first-episode psychosis: Effect on the clinical status and use of resources
- P. Herrero Ortega, A. Oliva Lozano, J. Garde González, C. Bayón-Pérez, R. Mediavilla, M. P. Vidal-Villegas, B. Rodríguez-Vega, S. Cebolla, E. Román, E. V. Pérez Pérez, M. F. Bravo-Ortiz, O. B. O. AGES-Mind Group
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S635-S636
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Psychotic disorders carry several economical, psychological and social consequences, both at individual and community levels. Early intervention programs after first-episode psychosis which combine pharmacological and psychosocial strategies are aimed at reducing symptoms, lowering costs in the use of health and non-health care resources and improving overall functioning. AGES-Mind study is based on manualized psychotherapeutic interventions for people with first-psychosis episodes.
ObjectivesThe aim of the study was to evaluate the effect of a group psychotherapeutic intervention on the clinical status and use of clinical resources in a sample of patients with first-episode psychosis at 12 and 24 months after the beginning of the intervention. This cohort will be compared to patients with first-psychosis episodes without group psychotherapeutic intervention.
MethodsLongitudinal, observational, retrospective study on a cohort of N=46 patients with first-episode psychosis within the last 5 years. Two groups of 23 patients each were formed. The participants of one of those groups received group psychotherapy in the context of the AGES-Mind study and the other group received treatment as usual without group intervention. Non-exposed patients were matched by age, gender and time elapsed since first-episode psychosis with those exposed to the intervention. Sociodemographic data, clinical status and use of clinical resources outcome variables were assessed.
ResultsNo significant differences were found in clinical status and use of resources between participants and non-participants in the psychotherapeutic group intervention after 12 and 24 months.
ConclusionsAfter controlling for potentially confounding variables as sociodemographic, age and time since first-episode, participating in a group psychotherapeutic program does not seem to improve clinical variables or use of resources. Further studies with larger samples would be necessary to explore other variables, such as symptoms, satisfaction with the intervention or social functioning.
Disclosure of InterestNone Declared
AGESMind clinical trial: SocialMIND® results at 16 weeks
- M. P. Vidal-Villegas, A. Abad Pérez, P. Herrero Ortega, A. Oliva Lozano, J. Garde González, J. Andreo-Jover, A. Muñoz-Sanjosé, R. Mediavilla, B. Rodríguez-Vega, G. Lahera, Á. Palao-Tarrero, C. Bayón-Pérez, M. F. Bravo-Ortiz
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S480-S481
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Early intervention on a first psychotic episode is fundamental for a more favorable prognosis, and it usually combines pharmacological treatment, which mainly affects positive psychotic symptoms, with interventions that can improve the rest of the symptoms and associated problems such as deterioration in social functioning (Harvey & Penn, 2010; Fusar-Poli, McGorry & Kane, 2017). While Mindfulness is gaining more and more prominence in the field of psychotherapy (Chan et al., 2019; Cillesen et al., 2019), social cognition and social functioning are being researched as key targets on which to intervene after a first psychotic episode (Green, Horan & Lee, 2015).
SocialMIND® is a mindfulness-based social cognition training tailor-made to improve social functioning in people who have suffered a first psychotic episode within the last five years. It is currently being compared with a group Psychoeducational Multicomponent Intervention (PMI) in a Randomized Controlled Trial (RCT) (Mediavilla et al., 2019). Both group psychotherapies include 17 sessions delivered over a 9 month period: 8 weekly sessions, 4 biweekly sessions and 5 monthly sessions.
The results of SocialMIND® at 8 weeks showed improvements in social cognition and social functioning, specifically on affective social cognition and self-care (Mediavilla et al., 2021).
ObjectivesTo evaluate the efficacy of SocialMIND® in improving social functioning, measured by the Personal and Social Functioning (PSP) scale 16 weeks after starting the intervention, in people who have suffered a first psychotic episode in the last 5 years.
MethodsRandomized, controlled pilot trial (use of a psychoeducational multicomponent intervention or PMI as active comparator) of two parallel groups (SocialMIND® and PMI) with a 1:1 ratio using a blind evaluator.
ResultsNo statistically significant differences were found in the social functioning variable between the two treatment arms. Intragroup differences are observed in other secondary variables studied (social cognition) 16 weeks after starting the interventions.
ConclusionsSocialMIND® has not been shown to be more effective than a PMI in improving social functioning at 16 weeks after starting the intervention in people who have suffered a first psychotic episode in the five years prior to being included in the study.
Disclosure of InterestNone Declared
Differential diagnosis of late onset psychotic symptoms. A case report.
- J. Sánchez Rodríguez, S. Puyal González, M. Paz Otero, E. Lozano Bori, A. García Recio
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1063
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We present the case of a sixty-seven-year-old woman who is examined for the first time in the emergency room because of a nine-month clinical picture that involves psychotic symptoms. The patient exhibits persecutory delusions that started after she shared some private information on social media. These symptoms also entail emotional distress and behavioral disturbances. She has never experienced hallucinations, but she does present delusional interpretations of the environment. Her clinical history reveals abnormalities of premorbid personality, including paranoid and immature features.
Objectives(1) We will be carrying out a differential diagnosis of late onset psychotic symptoms. We will as well be exploring the concept of Paraphrenia and analyzing its differential features in order to stablish the most suitable diagnosis for the case.
(2) The relationship between abnormalities in premorbid personality and psychotic symptoms will be covered, reviewing the available literature on this matter, and relating it to the patient’s symptomatology.
MethodsA review of the patient’s clinical history will be carried out, considering her biography, the testimony of her family and the complementary tests performed during the hospitalization period.
A bibliographic review of the available scientific literature will also be developed involving disorders that could explain psychotic symptoms in the elderly, as well as the term Paraphrenia, which describes specific features in a psychotic episode but is not included in the diagnostic manuals.
Results(1) The symptomatology that our patient exhibits may be considered atypical given the late stage of its onset and its specific features.
(2) The case could be explained under the category of Delusional Disorder. From a psychopathological point or view, it could also fit under de diagnosis of Paraphrenia as described by Ravindran et al.
(3) Pathological personality traits were assessed in premorbid personality which included paranoid and immature features.
ConclusionsIt could be useful to review the concept of the “paranoid spectrum” as proposed by some authors regarding some patient’s psychotic symptoms that don’t exactly fit any of the nowadays diagnostic categories. “Paraphrenia” could be understood as a distinct clinical entity for patients who show psychotic disorders but keep affective warmth and lack though deterioration and grossly disorganized behavior.
Most patients with late life paranoid psychoses have abnormal premorbid personalities, most usually of schizoid or paranoid type. There’s a decent amount of consensus in viewing the premorbid personality as having been abnormal as an early marker of impending psychosis.
Reformulating the way we approach diagnosis of psychotic symptoms of late onset could help us identify vulnerable patients on a premorbid stage and better classify and understand atypical entities.
Disclosure of InterestNone Declared
Superior mesenteric artery syndrome: when vomiting are not voluntary
- M. A. Morillas Romerosa, A. Oliva Lozano, P. Herrero Ortega, J. Garde Gonzalez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S851
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Superior mesenteric artery syndrome is a gastro-vascular disorder in which the third and final portion of the duodenum is compressed between the abdominal aorta and the overlying superior mesenteric artery. This rare, potentially life-threatening syndrome is typically caused by an angle of 6°–25° between the abdominal aorta and the superior mesenteric artery, in comparison to the normal range of 38°–56°, due to a lack of retroperitoneal and visceral fat (mesenteric fat). In addition, the aortomesenteric distance is 2–8 millimeters, as opposed to the typical 10–20. However, a narrow superior mesenteric artery angle alone is not enough to make a diagnosis with no symptoms.
Symptoms are fullness and epigastric tightness after meals, nausea and vomiting (often bilious) and pain in the middle of the abdomen that improves with the prone or knees flexed to the chest. The diagnosis is supported by imaging tests (esophagogastroduodenal transit or CT) showing dilation and stasis proximal to AMS in the third duodenal portion.
Relief from vomiting with feeding through a enteral probe placed beyond the obstruction to the proximal jejunum supports diagnosis.
Precipitating factors should be corrected first, whenever possible. Acute symptoms can be resolved with gastric decompression and intravenous fluids. Therefore, surgical correction should only be done in well-studied patients with chronic recurrent episodes of AMS syndrome. The most recommended surgical technique is a laparoscopic proximal duodenojejunostomy
ObjectivesTo describe a case of superior mesenteric artery syndrome and review in literature the organic complications and associated psychopathology of this disorder
MethodsClinical case report and brief review of literatura
Results17-year-old woman with a diagnosis of anorexia nervosa. Admitted for behavioral disorder, repeated self-harm and low mood. Presents a BMI of 16.6. Irregular rules. Progressive diet is started to which nutritional supplements are added with good initial tolerance. It presents a loss of 2kg and begins with nausea, vomiting and postprandial epigastralgia. Oral panendoscopy and abdominal ultrasound are performed showing possible mesenteric aortic clamp so naso-jejunal probe and exclusive enteral feeding is prescribed. She received enteral jejunal nutrition progressively with feedback syndrome prophylaxis that included parenteral vitamin B1. After a few days, oral supplementation began. He remained hemodynamically stable, with no signs of heart failure. It gained 3kg of weight up to 43.2kg, starting before discharge from the hospital successfully oral tolerance.
ConclusionsSuperior mesenteric artery syndrome is a serious complication in anorexia nervosa with a low incidence and an estimated mortality of 33%. A multidisplinar approach that addresses both the medical and psychological needs of these patients throughout their hospital stay is necessary.
Disclosure of InterestNone Declared
Efficacy of maintenance electroconvulsive therapy in recurrent depression: a case series
- G. Guerra Valera, Ó. Martín Santiago, M. Esperesate Pajares, Q. D. L. de la Viuda, A. A. Gonzaga Ramírez, C. Vallecillo Adame, C. de Andrés Lobo, T. Jiménez Aparicio, N. Navarro Barriga, B. Rodríguez Rodríguez, M. Fernández Lozano, M. J. Mateos Sexmero, A. Aparicio Parras, M. Calvo Valcárcel, M. A. Andreo Vidal, P. Martínez Gimeno, M. P. Pando Fernández, M. D. L. Á. Guillén Soto
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S832
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Maintenance electroconvulsive therapy (mECT) is an option in the treatment of affective disorders which progress is not satisfactory. It is certainly neglected and underused during the clinical practice.
ObjectivesTo evaluate the efficacy of mECT in reducing recurrence and relapse in recurrent depression within a sample of three patients.
MethodsWe followed up these patients among two years since they received the first set of electroconvulsive sessions. We applied the Beck Depression Inventory (BDI) in the succesives consultations for evaluating the progress.
ResultsThe three patients were diagnosed with Recurrent Depressive Disorder (RDD). One of them is a 60 year old man that received initially a cycle of 12 sessions; since then he received 10 maintenance sessions. Other one is a 70 year old woman that received initially a cycle of 10 sessions; since then she received 6 maintenance sessions. The last one is a 55 year old woman that received initially a cycle of 14 sessions; since then she received 20 maintenance sessions.
All of them showed a significant reduction in depressive symptoms evaluated through BDI and clinical examination. In the first case, we found a reduction in the BDI from the first consultation to the last that goes from 60 to 12 points; in the second case, from 58 to 8 points; and in the last case, from 55 to 10 points. The main sections that improved were emotional, physical and delusional.
As side-effects of the treatment, we found anterograde amnesia, lack of concentration and loss of focus at all of them.
ConclusionsWe find mECT as a very useful treatment for resistant cases of affective disorders like RDD.
It should be considered as a real therapeutic option when the first option drugs have been proved without success.
Disclosure of InterestNone Declared
“Social functioning and use of rehabilitation resources in a group of people who experienced a first episode of psychosis and participated in a psychotherapeutic group program versus a control group”
- A. Oliva Lozano, J. Garde Gonzalez, P. Herrero Ortega, A. Muñoz-Sanjosé, Á. Palao-Tarrero, M. P. Vidal-Villegas, R. Mediavilla, P. Tarín Garrón, J. M. Pastor-Haro, Á. De Diego Gómez-Cornejo, M. F. Bravo-Ortiz, O. B. O. A.-M. Group
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S185
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Psychotic disorders have a huge impact on social functioning, which is the ability to stablish and maintain social activities such as interpersonal relationships and self-care activities of daily living. Research data support that the early intervention in people who have experienced a first episode of psychosis (FEP) -based on a multidisciplinary treatment including both psychopharmacological and psychosocial treatments-, has a relevant role in a favorable evolution. AGES-Mind study is based on manualized psychotherapeutic interventions for people with first-psychosis episodes.
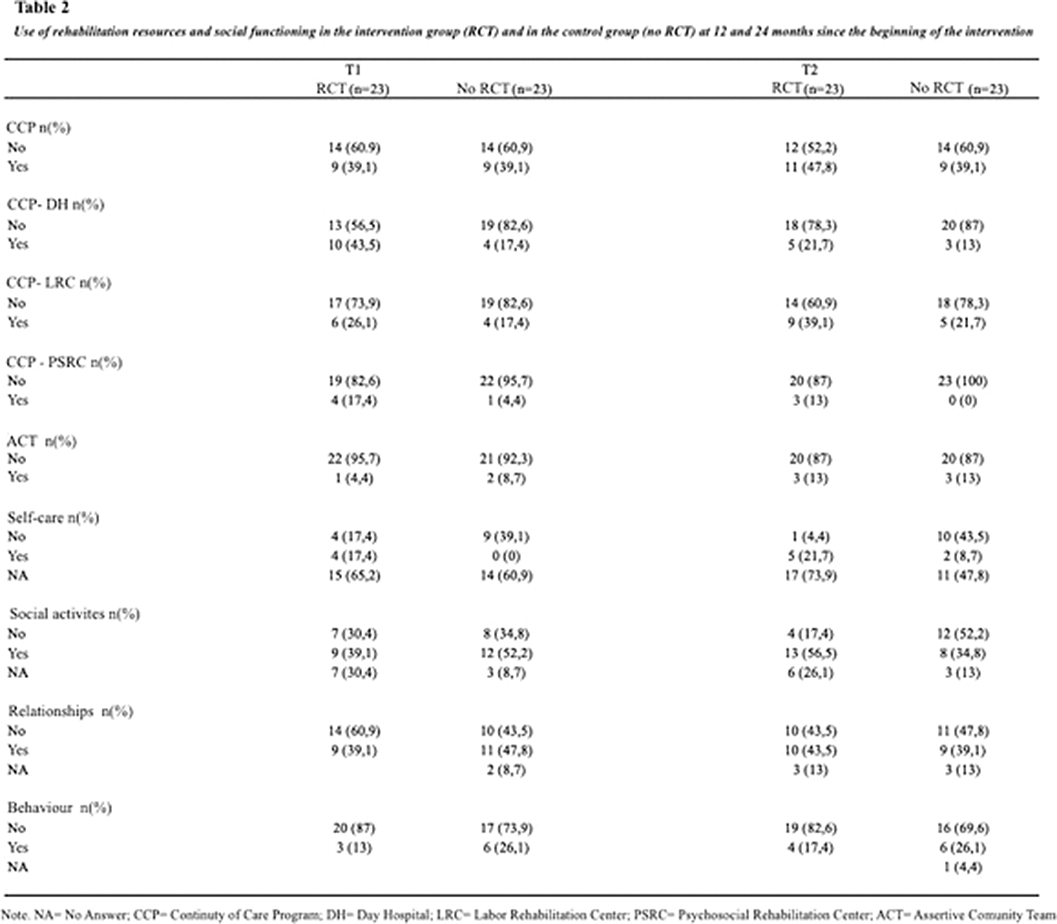
ObjectivesTo describe the use of rehabilitation resources and social functioning in a group of people with FEP who were included in a psychotherapeutic group program versus a control group, at 12 and 24 months since the beginning of the intervention.
MethodsLongitudinal, analytical, observational, retrospective study on a cohort of 46 patients with first-episode psychosis within the last 5 years. 23 patients received group psychotherapy in the context of the AGES-Mind study and they were compared with 23 control patients who did not receive a group intervention (treatment as usual). Controls were matched by age, gender and time elapsed since the first episode of psychosis with those exposed to the intervention. Sociodemographic data, social functioning (self-care, social activities, social relationships, and behavior) and use of rehabilitation resources outcome variables were assessed.
ResultsSignificant differences were found regarding participation in social activities in the intervention group versus control group at 24 months. No significant differences were found in other dimensions of social functioning or in the use of rehabilitation resources.
Image:
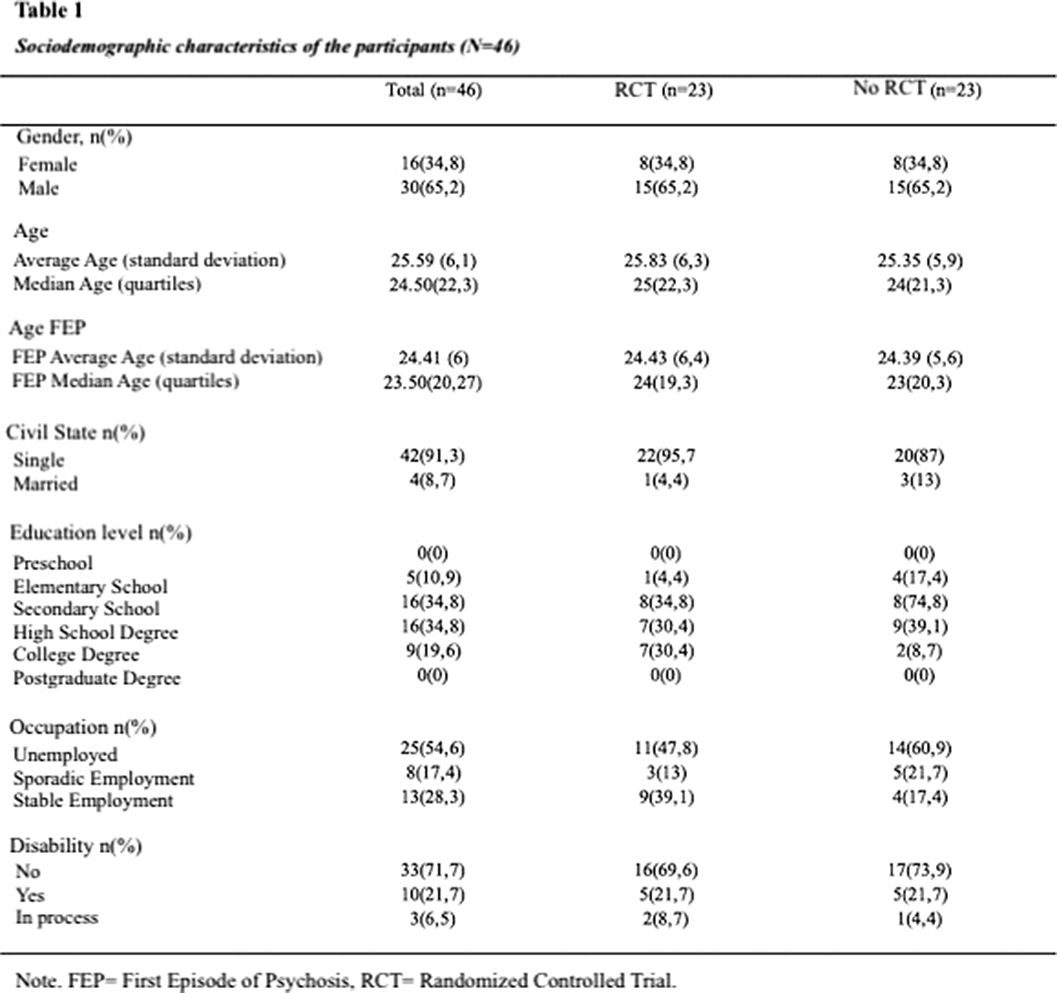
Image 2:
 Conclusions
ConclusionsFurther studies with larger sample sizes are needed in order to determine if the participation in group therapy leads to an improvement in social functioning and use of rehabilitation resources for people who have experienced a first episode of psychosis.
Disclosure of InterestNone Declared
“Unspecified organic personality and behavioral disorder due to brain damage from HHV-6 encephalitis in child. case report and literature review”
- A. Oliva Lozano, M. A. Morillas Romerosa, P. Herrero Ortega, J. Garde Gonzalez, B. Orgaz Álvarez, J. Curto Ramos, M. Alcamí Pertejo
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S143-S144
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We present a case of a 15 year-old boy diagnosed with Unspecified Personality and Beheavioral Disorder Due to Brain Damage from a Human Herpes Virus-6 Encephalitis.
ObjectivesTo describe a case of an Unspecified Organic Personality and Behavioral Disorder secondary to brain damage from Human Herpes Virus-6 (HHV-6) Encephalitis in an 11 year-old childand to review recent literature, in order to improve clinical practice.
MethodsClinical case report and brief review of literature. A bibliographic research was made in the database PubMed, using the terms “Viral Encephalitis” AND “Neuropsychiatric symptoms”; “Viral Encephalitis” AND “Behavioral Disorder”; “Long-Term Neurological Morbidity” AND “Viral Encephalitis”.
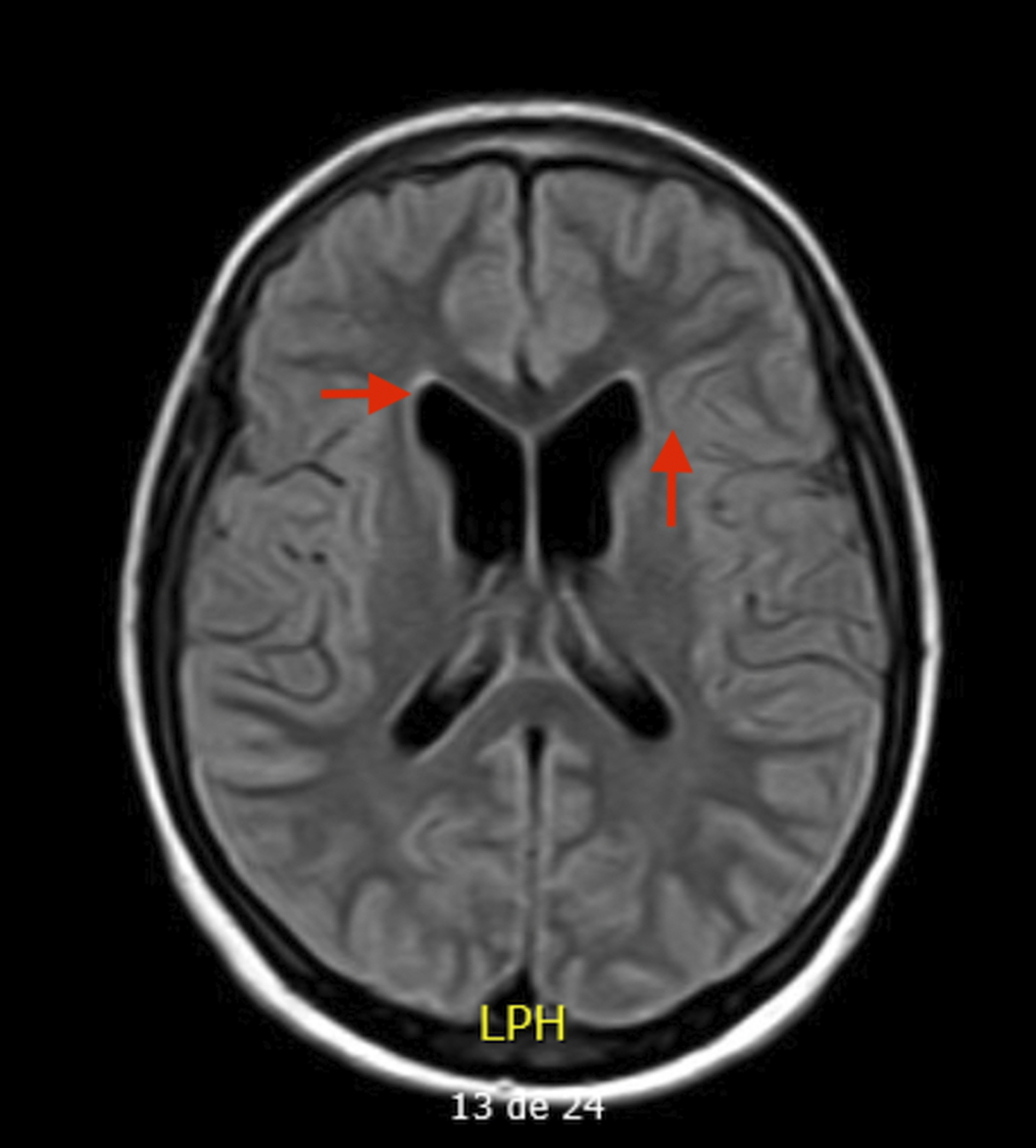
Results15 year-old boy diagnosed with Unspecified Personality and Beheavioral Disorder Due to Brain Damage from a Human Herpes Virus-6 Encephalitis, secondary to immunosupression in the context of haematopoietic progenitor transplantation (HPT) at 11 years old. MRI showed supratentorial ventriculomegaly, atrophic changes in encephalon and right hippocampus with subcortical retraction secondary to previous encephalitis. Clinically, main changes appeared in behavior, presenting a serious frontal syndrome with high disinhibition, what implied severe social and academic difficulties. During the outpatient follow-up, the behavioural disorder is being pharmacologically treated with Risperidone 1,5mg per day with a partially favorable evolution. The patient presented intolerance to olanzapine, with an episode of low level of conciuosness after taking it.
Bibliographic research results indicate that the gold standard treatment for behavioral disturbances are antipsychotics. Risperdidone is proven save for treatment in children. Results point out also the importance of an early multidisciplinar intervention, involving family training, rehabilitation resources and curricular adaptations.
Image:
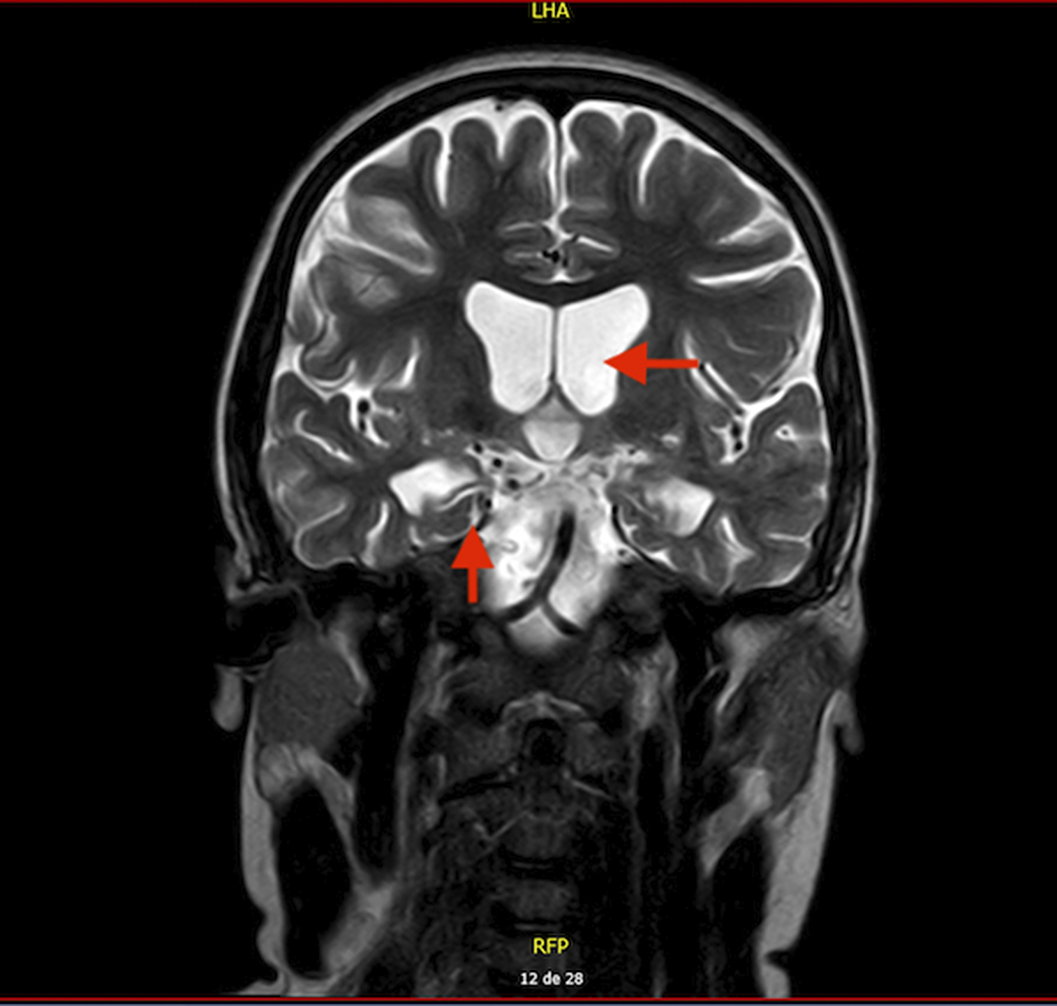
Image 2:
 Conclusions
ConclusionsViral encephalitis may have serious neuropsychiatric consequences, especially during childhood while the brain development is not finished. When the neurological damage affects the frontal lobes of the brain, behavioural and personality disturbances are expected and an early multidisciplinar intervention should be considered. Antypsichotics are the gold standard pharmacological treatment for behavioural disturbances. During the scholar period, special curricular adaptations should be done in order to reduce study-related stress.
Disclosure of InterestNone Declared
UNTIL IT BURSTS OR ALL OF US BURST. A SCHIZOTYPICAL CASE.
- B. Rodríguez Rodríguez, N. Navarro Barriga, M. Fernández Lozano, M. J. Mateos Sexmero, M. A. Andreo Vidal, M. Calvo Valcárcel, P. Martínez Gimeno, M. P. Pando Fernández, A. Aparicio Parras, M. D. L. Á. Guillén Soto, T. Jiménez Aparicio, M. D. C. Vallecillo Adame, C. de Andrés Lobo, A. A. Gonzaga Ramírez, G. Guerra Valera, M. Queipo de Llano de la Viuda, M. Esperesate Pajares
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S967
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Schizotypal disorder is conceptualized as a stable personality pathology (Cluster A) and as a latent manifestation of schizophrenia. It can be understood as an attenuated form of psychosis or high-risk mental state, which may precede the onset of schizophrenia or represent a more stable form of psychopathology that doesn’t necessarily progress to psychosis.
ObjectivesTo exemplify the continuum of psychosis
MethodsReview of scientific literature based on a relevant clinical case.
Results39-year-old male living with his parents. He started studying philosophy. He is a regular cannabis user and has an aunt with schizophrenia. He’s admitted to psychiatry for behavioral disturbance in public. He refers to having been hearing a beeping noise in his street for months, what he interprets as a possible way of being watched due to his past ideology. Without specifying who and why, he sometimes shouts “until it bursts” to stop the noise and he thinks that his neighbours alerted the police about his behavior. During the interview he alludes to Milgram’s experiment, saying that throughout history there have been crimes against humanity and those who pointed them out were labeled “crazy”. His father refers that he has always been “strange” and with certain extravagant revolutionary ideas and thoughts. He doesn’t maintain social relationships and dedicates himself to reading and writing.
ConclusionsIt’s important to understand psychosis as a continuum to advance the understanding of etiology, pathophysiology and resilience of psychotic disorders and to develop strategies for prevention and early intervention
Disclosure of InterestNone Declared
The RNA editing patterns are different in blood of euthymic and depressed bipolar patients
- M. Hayashi, N. Salvetat, C. Cayzac, F. J. Checa-Robles, C. Lozano, J.-D. Abraham, B. Dubuc, S. Mereuze, J. V. Nani, F. Molina, E. Brietske, D. Weissmann
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S573
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Bipolar disorder (BD) is a severe mental disorder associated with functional impairment, high disability and premature mortality. Modifications of editing in mRNA of serotonin receptor subtype 2C (5-HTR2c) was reported by us in depressed suicide decedents. We have also identified a panel of RNA editing-based blood biomarkers for the diagnosis of BD, which also allowed to discriminate unipolar depression from BD with high sensivity and specificity.
ObjectivesHerein, aiming to confirm the diagnostic value of this panel, a new cohort of BD patients was recruited in Brazil.
MethodsThis study is based on the analysis of 47 control patients (CTRL) compared to 40 patients with bipolar disorder (BD). BD patients (BP) were classified into 4 subgroups: euthymic (BP_EUT, n = 17), depressive (BP_DEP, n = 11), manic/hypomanic (BP_HM, n = 7) and mixed (BP_MIX, n = 5). The diagnostic value of a panel of RNA editing-based blood biomarkers for the diagnosis of BD, which includes a set of eight genes, namely PDE8A, CAMK1D (calcium/calmodulin-dependent protein kinase type 1D); GAB2 (growth factor receptor bound protein 2-associated protein 2); IFNAR1 (interferon alpha/beta receptor 1); KCNJ15 (ATP-sensitive inward rectifier potassium channel 15); LYN (tyrosine-protein kinase Lyn); MDM2 (E3 ubiquitin-protein ligase Mdm2); PRKCB (protein kinase C beta type), which was able to discriminate unipolar depression from BD with high sensivity and specificity, was confirmed here by testing an independent cohort of patients suffering from BD recruited in a well-known genetic admixed ancestry population, which is typical in South America, more specifically in Brazil.
ResultsWe identified new combinations allowing a clear discrimination of euthymic versus depressed bipolar patients, and euthymic versus healthy controls, confirming that RNA editing is a key mechanism in the physiopathology of mental disorders, in particular in BD.
ConclusionsIn conclusion of this study, we confirm that RNA editing is a key mechanism in the physiopathology of mental disorders in general, and in BD in particular, and that measuring changes in this mechanism at the peripheral level allowed us to stratify BD patients not only with respect to their symptomatology, but also with respect to the pathophysiology, thus paving the way for personalised medicine in psychiatry.
Disclosure of InterestNone Declared
Delirious episode secondary to rotigotine: the psychotic patch
- M. A. Andreo Vidal, M. Calvo Valcárcel, P. Martínez Gimeno, P. Pando Fernández, B. Rodríguez Rodríguez, N. Navarro Barriga, M. Fernández Lozano, M. J. Mateos Sexmero, T. Jiménez Aparicio, M. D. C. Valdecillo Adame, C. de Andrés Lobo, G. Guerra Valera, M. Queipo de Llano de la Viuda, A. A. Gonzaga Ramirez, M. D. L. Á. Guillén Soto, A. Aparicio Parras, M. Esperesate Pajares
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S626
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
There is a fine line separating psychiatry and neurology. Most movement disorders can have psychiatric symptoms, not only those caused by the disease itself, but also those induced by the drugs used to treat them.
ObjectivesPresentation of a clinical case about a patient diagnosed with Parkinson’s disease presenting a several-month-long delirious episode due to dopaminergic drugs.
MethodsLiterature review on drug-induced psychosis episodes in Parkinson’s disease.
ResultsA 57-year-old patient with diagnosis of Parkinson’s disease for six years, who went to the emergency room accompanied by his wife due to delirious ideation. He was being treated with levodopa, carbidopa and rasagiline for years, and rotigotine patches whose dosage was being increased over the last few months.
His wife reported celotypical clinical manifestations and multiple interpretations of different circumstances occurring around her. He chased her on the street, had downloaded an app to look for a second cell phone because he believed she was cheating on him, and was obsessed with sex. He had no psychiatric background. It was decided to prescribe quetiapine.
The following day, he returned because he refused to take the medication since he thought he was going to be put to sleep or poisoned. It was decided to admit him to Psychiatry.
During the stay, rasagiline and rotigotine were suspended. Olanzapine and clozapine were introduced, with behavioral improvement and distancing from the psychotic symptoms which motivated the admission. The patient was also motorically stable. Although levodopa is best known for causing psychotic episodes, the symptons were attributed to rotigotine patches for temporally overlapping the dose increase.
ConclusionsPsychiatric symptoms are the third most frequent group of complications in Parkinson’s disease after gastrointestinal complications and abnormal movements. All medication used to control motor disorders can lead to psychosis, not only dopaminergics, but also selegiline, amantadine and anticholinergics.
Excessive stimulation of mesocortical and mesolimbic dopaminergic pathways can lead to psychosis, which is the most common psychiatric problem related to dopaminergic treatment.
In the face of a psychotic episode, antiparkinsonian drugs which are not strictly necessary for motor control should be withdrawn. If this is not sufficient, levodopa dose should be reduced, considering the side effects that may occur. When the adjustment of antiparkinsonian treatment is not effective, neuroleptics, especially quetiapine or clozapine, should be administered. In a recent study, pimavanserin, a serotonin 5-HT2 antagonist, was associated with approximately 35% lower mortality than atypical antipsychotic use during the first 180 days of treatment in community-dwelling patients.
Medication should always be tailor-made to suit each patient and we usually have to resort to lowering or withdrawing the dopaminergic medication.
Disclosure of InterestNone Declared
Bipolar disorder and substance use: Risk factors and prognosis
- M. Fernández Lozano, B. Rodríguez Rodríguez, M. J. Mateos Sexmero, N. Navarro Barriga, C. Vallecillo Adame, C. de Andrés Lobo, T. Jimenez Aparicio, M. Queipo de Llano de la Viuda, G. Guerra Valera, A. A. Gonzaga Ramírez, M. P. Pando Fernández, M. Calvo Valcárcel, M. A. Andreo Vidal, P. Martínez Gimeno
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S704
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Bipolar disorder comorbidity rates are the highest among the major mental disorders. In addition to other intoxicants, alcohol is the most abused substance because it is socially accepted and can be legally bought and consumed. Estimates are between 40-70% with male predominance, which further influences the severity with a more complicated course of both disorders.
ObjectivesThe objective of this article is to highlight the impact of substance use on the course and prognosis of bipolar disorder, as well as to make a differential diagnosis of a manic episode in this context.
MethodsBibliographic review of scientific literature based on a relevant clinical case.
ResultsWe present the case of a 45-year-old male patient. Single with no children. Unemployed. History of drug use since he was young: alcohol, cannabis and amphetamines. Diagnosed with bipolar disorder in 2012 after a manic episode that required hospital admission. During his evolution he presented two depressive episodes that required psychopharmacological treatment and follow-up by his psychiatrist of reference. Since then, he has been consuming alcohol and amphetamines occasionally, with a gradual increase until it became daily in the last month. He went to the emergency department for psychomotor agitation after being found in the street. He reported feeling threatened by a racial group presenting accelerated speech, insomnia and increased activity.
ConclusionsThe presence of substance abuse complicates the clinical presentation, treatment and development of bipolar disorder. It is associated with a worse prognosis with multiple negative consequences including worsening symptom severity, increased risk of suicide and hospitalization, increased medical morbidity and complication of social problems. In addition, this comorbidity delays both the diagnosis and treatment, by masking the symptoms, and making more difficult an adequate differential diagnosis.
Disclosure of InterestNone Declared
I don’t know where I’m going or where I come from. Self-disorders in schizophrenia.
- M. D. C. Vallecillo Adame, L. Rodríguez Andrés, C. de Andrés Lobo, T. Jimenez Aparicio, M. Queipo de Llano de la Viuda, G. Guerra Valera, A. A. Gonzaga Ramirez, M. Fernández Lozano, M. J. Mateos Sexmero, N. Navarro Barriga, B. Rodríguez Rodríguez, M. P. Pando Fernández, M. Calvo Valcárcel, P. Martínez Gimeno, M. A. Andreo Vidal, I. D. L. M. Santos Carrasco
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1069-S1070
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
In the early stages of schizophrenia the person experiences feelings of strangeness about themselves, difficulty in making sense of things and difficulty in interacting with their environment. Based on this, self-disorder assessment instruments have been developed and empirical studies have been conducted to assess people at risk of developing a schizophrenia spectrum disorder. These studies show that self-disorders are found in pre-psychotic stages and that their manifestation can predict the transition to schizophrenia spectrum disorders.
ObjectivesWe present the case of a patient with multiple diagnoses and mainly dissociative symptoms who, after years of evolution, was diagnosed with schizophrenia.
MethodsBibliographic review including the latest articles in Pubmed about self-disorders and schizophrenia.
ResultsWe present the clinical case of a 51-year-old woman with a long history of follow-up in mental health consultations and with multiple hospital admissions to the psychiatric unit, with several diagnoses including: dissociative disorder, histrionic personality disorder, adaptive disorder unspecified psychotic disorder and, finally, schizophrenia. The patient during the first hospital admissions showed a clinical picture of intense anxiety, disorientation and claiming to be a different person. The patient related these episodes to stressors she had experienced, and they improved markedly after a short period of hospital admission. Later, psychotic symptoms appeared in the form of auditory and visual hallucinations and delusional ideation, mainly of harm, so that after several years of follow-up and study in mental health consultations and in the psychiatric day hospital, she was diagnosed with schizophrenia and treatment with antipsychotics was introduced, with a marked clinical improvement being observed.
ConclusionsIt is important to take into account this type of symptoms (self-disorders), as they allow the identification of individuals in the early stages of the disorder and create the opportunity for early therapeutic interventions.
Disclosure of InterestNone Declared







