6 results
Implementing nasal povidone-iodine decolonization to reduce infections in hemodialysis units: a qualitative assessment
- Kimberly C. Dukes, Stacey Hockett Sherlock, AM Racila, Loreen A. Herwaldt, Jesse Jacob, Anitha Vijayan, Joseph Kellogg, David Pegues, Pam C. Tolomeo, Jason Cobb, Mony Fraer, Susan C. Bleasdale, Melissa A. Ward, Brenna Lindsey, Marin L. Schweizer
-
- Journal:
- Infection Control & Hospital Epidemiology , First View
- Published online by Cambridge University Press:
- 23 May 2024, pp. 1-6
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background:
A substantial proportion of patients undergoing hemodialysis carry Staphylococcus aureus in their noses, and carriers are at increased risk of S. aureus bloodstream infections. Our pragmatic clinical trial implemented nasal povidone-iodine (PVI) decolonization for the prevention of bloodstream infections in the novel setting of hemodialysis units.
Objective:We aimed to identify pragmatic strategies for implementing PVI decolonization among patients in outpatient hemodialysis units.
Design:Qualitative descriptive study.
Setting:Outpatient hemodialysis units affiliated with five US academic medical centers. Units varied in size, patient demographics, and geographic location.
Interviewees:Sixty-six interviewees including nurses, hemodialysis technicians, research coordinators, and other personnel.
Methods:We conducted interviews with personnel affiliated with all five academic medical centers and conducted thematic analysis of transcripts.
Results:Hemodialysis units had varied success with patient recruitment, but interviewees reported that patients and healthcare personnel (HCP) found PVI decolonization acceptable and feasible. Leadership support, HCP engagement, and tailored patient-focused tools or strategies facilitated patient engagement and PVI implementation. Interviewees reported both patients and HCP sometimes underestimated patients’ infection risks and experienced infection-prevention fatigue. Other HCP barriers included limited staffing and poor staff engagement. Patient barriers included high health burdens, language barriers, memory issues, and lack of social support.
Conclusion:Our qualitative study suggests that PVI decolonization would be acceptable to patients and clinical personnel, and implementation is feasible for outpatient hemodialysis units. Hemodialysis units could facilitate implementation by engaging unit leaders, patients and personnel, and developing education for patients about their infection risk.
Which nursing home workers were at highest risk for SARS-CoV-2 infection during the November 2020–February 2021 winter surge of COVID-1?
- Joseph Kellogg, William Dube, Carly Adams, Matthew Collins, Theodore Lopman, Theodore Johnson, Avnika Amin, Joshua Weitz, Scott Fridkin
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, p. s7
-
- Article
-
- You have access Access
- Open access
- Export citation
-
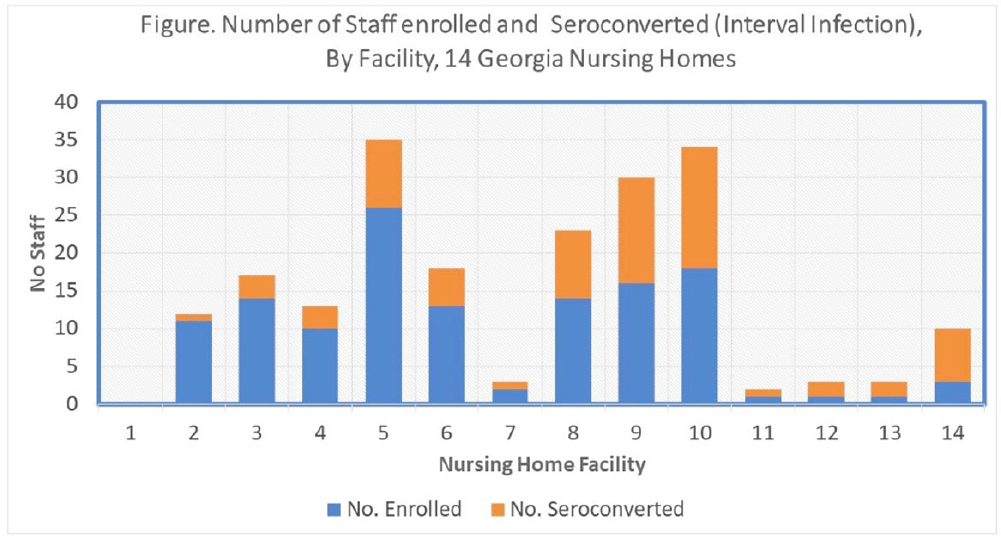
Background: Nursing home (NH) residents and staff were at high risk for COVID-19 early in the pandemic; several studies estimated seroprevalence of infection in NH staff to be 3-fold higher among CNAs and nurses compared to other staff. Risk mitigation added in Fall 2020 included systematic testing of residents and staff (and furlough if positive) to reduce transmission risk. We estimated risks for SARS-CoV-2 infection among NH staff during the first winter surge before widespread vaccination. Methods: Between February and May 2021, voluntary serologic testing was performed on NH staff who were seronegative for SARS-CoV-2 in late Fall 2020 (during a previous serology study at 14 Georgia NHs). An exposure assessment at the second time point covered prior 3 months of job activities, community exposures, and self-reported COVID-19 vaccination, including very recent vaccination (≤4 weeks). Risk factors for seroconversion were estimated by job type using multivariable logistic regression, accounting for interval community-incidence and interval change in resident infections per bed. Results: Among 203 eligible staff, 72 (35.5%) had evidence of interval seroconversion (Fig. 1). Among 80 unvaccinated staff, interval infection was significantly higher among CNAs and nurses (aOR, 4.9; 95% CI, 1.4–20.7) than other staff, after adjusting for race and interval community incidence and facility infections. This risk persisted but was attenuated when utilizing the full study cohort including those with very recent vaccination (aOR, 1.8; 95% CI, 0.9–3.7). Conclusions: Midway through the first year of the pandemic, NH staff with close or common resident contact continued to be at increased risk for infection despite enhanced infection prevention efforts. Mitigation strategies, prior to vaccination, did not eliminate occupational risk for infection. Vaccine utilization is critical to eliminate occupational risk among frontline healthcare providers.
Funding: None
Disclosures: None
Risk factors for severe acute respiratory coronavirus virus 2 (SARS-CoV-2) seropositivity among nursing home staff
- Avnika B. Amin, Joseph T. Kellogg, Carly Adams, William C. Dube, Matthew H. Collins, Benjamin A. Lopman, Theodore M. Johnson II, Joshua Weitz, Scott K. Fridkin
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue 1 / 2021
- Published online by Cambridge University Press:
- 28 October 2021, e35
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Objectives:
To estimate prior severe acute respiratory coronavirus virus 2 (SARS-CoV-2) infection among skilled nursing facility (SNF) staff in the state of Georgia and to identify risk factors for seropositivity as of fall 2020.
Design:Baseline survey and seroprevalence of the ongoing longitudinal Coronavirus 2019 (COVID-19) Prevention in Nursing Homes study.
Setting:The study included 14 SNFs in the state of Georgia.
Participants:In total, 792 SNF staff employed or contracted with participating SNFs were included in this study. The analysis included 749 participants with SARS-CoV-2 serostatus results who provided age, sex, and complete survey information.
Methods:We estimated unadjusted odds ratios (ORs) and 95% confidence intervals (95% CIs) for potential risk factors and SARS-CoV-2 serostatus. We estimated adjusted ORs using a logistic regression model including age, sex, community case rate, SNF resident infection rate, working at other facilities, and job role.
Results:Staff working in high-infection SNFs were twice as likely (unadjusted OR, 2.08; 95% CI, 1.45–3.00) to be seropositive as those in low-infection SNFs. Certified nursing assistants and nurses were 3 times more likely to be seropositive than administrative, pharmacy, or nonresident care staff: unadjusted OR, 2.93 (95% CI, 1.58–5.78) and unadjusted OR, 3.08 (95% CI, 1.66–6.07). Logistic regression yielded similar adjusted ORs.
Conclusions:Working at high-infection SNFs was a risk factor for SARS-CoV-2 seropositivity. Even after accounting for resident infections, certified nursing assistants and nurses had a 3-fold higher risk of SARS-CoV-2 seropositivity than nonclinical staff. This knowledge can guide prioritized implementation of safer ways for caregivers to provide necessary care to SNF residents.
Evaluation of Care Interactions Between Healthcare Personnel and Residents in Nursing Homes Across the United States
- Nai-Chung Chang, Karim Khader, Molly Leecaster, Lindsay Visnovsky, Scott Fridkin, Morgan Katz, Philip Polgreen, Mary-Claire Roghmann, Candace Haroldsen, Diane Mulvey, Kristina Stratford, Lauren Dempsey, William Dube, Ghinwa Dumyati, Linda Frank, Deborah Godine, Siyeh Gretzinger, Trupti Hatwar, Marion Kainer, Joseph Kellogg, Sarah Kuchman, Laura LaLonde, Giancarlo Licitra, Ruth Lynfield, J.P. Mahoehney, Joelle Nadle, Sujan Reddy, Nicola Thompson, Rebecca Tsay, Lucy Wilson, Alexia Zhang, Matthew Samore
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s36-s38
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Certain nursing home (NH) resident care tasks have a higher risk for multidrug-resistant organisms (MDRO) transfer to healthcare personnel (HCP), which can result in transmission to residents if HCPs fail to perform recommended infection prevention practices. However, data on HCP-resident interactions are limited and do not account for intrafacility practice variation. Understanding differences in interactions, by HCP role and unit, is important for informing MDRO prevention strategies in NHs. Methods: In 2019, we conducted serial intercept interviews; each HCP was interviewed 6–7 times for the duration of a unit’s dayshift at 20 NHs in 7 states. The next day, staff on a second unit within the facility were interviewed during the dayshift. HCP on 38 units were interviewed to identify healthcare personnel (HCP)–resident care patterns. All unit staff were eligible for interviews, including certified nursing assistants (CNAs), nurses, physical or occupational therapists, physicians, midlevel practitioners, and respiratory therapists. HCP were asked to list which residents they had cared for (within resident rooms or common areas) since the prior interview. Respondents selected from 14 care tasks. We classified units into 1 of 4 types: long-term, mixed, short stay or rehabilitation, or ventilator or skilled nursing. Interactions were classified based on the risk of HCP contamination after task performance. We compared proportions of interactions associated with each HCP role and performed clustered linear regression to determine the effect of unit type and HCP role on the number of unique task types performed per interaction. Results: Intercept-interviews described 7,050 interactions and 13,843 care tasks. Except in ventilator or skilled nursing units, CNAs have the greatest proportion of care interactions (interfacility range, 50%–60%) (Fig. 1). In ventilator and skilled nursing units, interactions are evenly shared between CNAs and nurses (43% and 47%, respectively). On average, CNAs in ventilator and skilled nursing units perform the most unique task types (2.5 task types per interaction, Fig. 2) compared to other unit types (P < .05). Compared to CNAs, most other HCP types had significantly fewer task types (0.6–1.4 task types per interaction, P < .001). Across all facilities, 45.6% of interactions included tasks that were higher-risk for HCP contamination (eg, transferring, wound and device care, Fig. 3). Conclusions: Focusing infection prevention education efforts on CNAs may be most efficient for preventing MDRO transmission within NH because CNAs have the most HCP–resident interactions and complete more tasks per visit. Studies of HCP-resident interactions are critical to improving understanding of transmission mechanisms as well as target MDRO prevention interventions.
Funding: Centers for Disease Control and Prevention (grant no. U01CK000555-01-00)
Disclosures: Scott Fridkin, consulting fee, vaccine industry (spouse)
The Last Interglacial Ocean
- Rose Marie L. Cline, James D. Hays, Warren L. Prell, William F. Ruddiman, Ted C. Moore, Nilva G. Kipp, Barbara E. Molfino, George H. Denton, Terence J. Hughes, William L. Balsam, Charlotte A. Brunner, Jean-Claude Duplessy, Ann G. Esmay, James L. Fastook, John Imbrie, Lloyd D. Keigwin, Thomas B. Kellogg, Andrew McIntyre, Robley K. Matthews, Alan C. Mix, Joseph J. Morley, Nicholas J. Shackleton, S. Stephen Streeter, Peter R. Thompson
-
- Journal:
- Quaternary Research / Volume 21 / Issue 2 / February 1984
- Published online by Cambridge University Press:
- 20 January 2017, pp. 123-224
-
- Article
- Export citation
-
The final effort of the CLIMAP project was a study of the last interglaciation, a time of minimum ice volume some 122,000 yr ago coincident with the Substage 5e oxygen isotopic minimum. Based on detailed oxygen isotope analyses and biotic census counts in 52 cores across the world ocean, last interglacial sea-surface temperatures (SST) were compared with those today. There are small SST departures in the mid-latitude North Atlantic (warmer) and the Gulf of Mexico (cooler). The eastern boundary currents of the South Atlantic and Pacific oceans are marked by large SST anomalies in individual cores, but their interpretations are precluded by no-analog problems and by discordancies among estimates from different biotic groups. In general, the last interglacial ocean was not significantly different from the modern ocean. The relative sequencing of ice decay versus oceanic warming on the Stage 6/5 oxygen isotopic transition and of ice growth versus oceanic cooling on the Stage 5e/5d transition was also studied. In most of the Southern Hemisphere, the oceanic response marked by the biotic census counts preceded (led) the global ice-volume response marked by the oxygen-isotope signal by several thousand years. The reverse pattern is evident in the North Atlantic Ocean and the Gulf of Mexico, where the oceanic response lagged that of global ice volume by several thousand years. As a result, the very warm temperatures associated with the last interglaciation were regionally diachronous by several thousand years. These regional lead-lag relationships agree with those observed on other transitions and in long-term phase relationships; they cannot be explained simply as artifacts of bioturbational translations of the original signals.
Preparing Emergency Physicians for Acute Disaster Response: A Review of Current Training Opportunities in the US
- Bhakti Hansoti, Dylan S. Kellogg, Sara J. Aberle, Morgan C. Broccoli, Jeffrey Feden, Arthur French, Charles M. Little, Brooks Moore, Joseph Sabato, Jr., Tara Sheets, R. Weinberg, Pat Elmes, Christopher Kang
-
- Journal:
- Prehospital and Disaster Medicine / Volume 31 / Issue 6 / December 2016
- Published online by Cambridge University Press:
- 19 September 2016, pp. 643-647
- Print publication:
- December 2016
-
- Article
- Export citation
-
Study Objective
This study aimed to review available disaster training options for health care providers, and to provide specific recommendations for developing and delivering a disaster-response-training program for non-disaster-trained emergency physicians, residents, and trainees prior to acute deployment.
MethodsA comprehensive review of the peer-reviewed and grey literature of the existing training options for health care providers was conducted to provide specific recommendations.
ResultsA comprehensive search of the Pubmed, Embase, Web of Science, Scopus, and Cochrane databases was performed to identify publications related to courses for disaster preparedness and response training for health care professionals. This search revealed 7,681 unique titles, of which 53 articles were included in the full review. A total of 384 courses were found through the grey literature search, and many of these were available online for no charge and could be completed in less than six hours. The majority of courses focused on management and disaster planning; few focused on clinical care and acute response.
ConclusionThere is need for a course that is targeted toward emergency physicians and trainees without formal disaster training. This course should be available online and should utilize a mix of educational modalities, including lectures, scenarios, and virtual simulations. An ideal course should focus on disaster preparedness, and the clinical and non-clinical aspects of response, with a focus on an all-hazards approach, including both terrorism-related and environmental disasters.
Hansoti B Kellogg DS Aberle SJ Broccoli MC Feden J French A Little CM Moore B Sabato J Jr. Sheets T Weinberg R Elmes P Kang C Preparing Emergency Physicians for Acute Disaster Response: A Review of Current Training Opportunities in the US . Prehosp Disaster Med.2016 ;31 (6 ):643 –647 .




