11 results
Implementing nasal povidone-iodine decolonization to reduce infections in hemodialysis units: a qualitative assessment
- Kimberly C. Dukes, Stacey Hockett Sherlock, AM Racila, Loreen A. Herwaldt, Jesse Jacob, Anitha Vijayan, Joseph Kellogg, David Pegues, Pam C. Tolomeo, Jason Cobb, Mony Fraer, Susan C. Bleasdale, Melissa A. Ward, Brenna Lindsey, Marin L. Schweizer
-
- Journal:
- Infection Control & Hospital Epidemiology , First View
- Published online by Cambridge University Press:
- 23 May 2024, pp. 1-6
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background:
A substantial proportion of patients undergoing hemodialysis carry Staphylococcus aureus in their noses, and carriers are at increased risk of S. aureus bloodstream infections. Our pragmatic clinical trial implemented nasal povidone-iodine (PVI) decolonization for the prevention of bloodstream infections in the novel setting of hemodialysis units.
Objective:We aimed to identify pragmatic strategies for implementing PVI decolonization among patients in outpatient hemodialysis units.
Design:Qualitative descriptive study.
Setting:Outpatient hemodialysis units affiliated with five US academic medical centers. Units varied in size, patient demographics, and geographic location.
Interviewees:Sixty-six interviewees including nurses, hemodialysis technicians, research coordinators, and other personnel.
Methods:We conducted interviews with personnel affiliated with all five academic medical centers and conducted thematic analysis of transcripts.
Results:Hemodialysis units had varied success with patient recruitment, but interviewees reported that patients and healthcare personnel (HCP) found PVI decolonization acceptable and feasible. Leadership support, HCP engagement, and tailored patient-focused tools or strategies facilitated patient engagement and PVI implementation. Interviewees reported both patients and HCP sometimes underestimated patients’ infection risks and experienced infection-prevention fatigue. Other HCP barriers included limited staffing and poor staff engagement. Patient barriers included high health burdens, language barriers, memory issues, and lack of social support.
Conclusion:Our qualitative study suggests that PVI decolonization would be acceptable to patients and clinical personnel, and implementation is feasible for outpatient hemodialysis units. Hemodialysis units could facilitate implementation by engaging unit leaders, patients and personnel, and developing education for patients about their infection risk.
Examining barriers to implementing a surgical-site infection bundle
- Kimberly C. Dukes, Heather Schacht Reisinger, Marin Schweizer, Melissa A. Ward, Laura Chapin, Timothy C. Ryken, Trish M. Perl, Loreen A. Herwaldt
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 45 / Issue 1 / January 2024
- Published online by Cambridge University Press:
- 26 July 2023, pp. 13-20
- Print publication:
- January 2024
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background:
Surgical-site infections (SSIs) can be catastrophic. Bundles of evidence-based practices can reduce SSIs but can be difficult to implement and sustain.
Objective:We sought to understand the implementation of SSI prevention bundles in 6 US hospitals.
Design:Qualitative study.
Methods:We conducted in-depth semistructured interviews with personnel involved in bundle implementation and conducted a thematic analysis of the transcripts.
Setting:The study was conducted in 6 US hospitals: 2 academic tertiary-care hospitals, 3 academic-affiliated community hospitals, 1 unaffiliated community hospital.
Participants:In total, 30 hospital personnel participated. Participants included surgeons, laboratory directors, clinical personnel, and infection preventionists.
Results:Bundle complexity impeded implementation. Other barriers varied across services, even within the same hospital. Multiple strategies were needed, and successful strategies in one service did not always apply in other areas. However, early and sustained interprofessional collaboration facilitated implementation.
Conclusions:The evidence-based SSI bundle is complicated and can be difficult to implement. One implementation process probably will not work for all settings. Multiple strategies were needed to overcome contextual and implementation barriers that varied by setting and implementation climate. Appropriate adaptations for specific settings and populations may improve bundle adoption, fidelity, acceptability, and sustainability.
162 Building a Pandemic-Responsive, Community-Engaged Research Program to Advance Health Equity for Persons with Diabetes
- Part of
- Carolina Gonzalez Bravo, Aneli Villa, Aloha Wilks, Di Daniels, Emilia Marroquin, Kimberly Dukes, Bailey Goodman, Shakoora Sabree
-
- Journal:
- Journal of Clinical and Translational Science / Volume 7 / Issue s1 / April 2023
- Published online by Cambridge University Press:
- 24 April 2023, p. 50
-
- Article
-
- You have access Access
- Open access
- Export citation
-
OBJECTIVES/GOALS: Diabetes mellitus and COVID-19 have converged to form a syndemic. Our team sought to identify and respond to the evolving needs of patients and communities affected by diabetes amid the COVID-19 pandemic and to engage community partners and student leaders in the advancement of health equity research and practice in the state of Iowa. METHODS/STUDY POPULATION: A team of faculty, staff, students, and community partners was assembled to facilitate, design, and implement mixed methods research related to diabetes care in collaboration with more than five sites in Eastern and Western Iowa during the pandemic, with a focus on potentially preventable complications such as diabetes-related foot ulcers and amputations in adult patients. Attention was directed towards the experiences of rural residents, persons working in frontline occupations during the pandemic, persons from minoritized racial or ethnic groups, and persons who speak Spanish. RESULTS/ANTICIPATED RESULTS: A semi-structured interview study about diabetes care revealed themes in the experiences of persons with diabetes during the pandemic. A pilot study of an educational tool called the Foot Book among patients and providers demonstrated the potential for use of this tool in health care and community settings to reduce gaps in diabetes foot care. All study materials and activities were offered in English and Spanish. Study results were combined with input from community partners to develop ongoing interventions to improve care in Iowa communities. DISCUSSION/SIGNIFICANCE: Amid the syndemic of COVID-19 and diabetes, urgent action is needed to mitigate health inequities and prevent further acceleration of these inequities. Our team developed a community-engaged, patient-centered, and student-led research program that can respond to the needs of patients and communities in the pandemic era.
Unfamiliar personal protective equipment: The role of routine practice and other factors affecting healthcare personnel doffing strategies
- Emily E. Chasco, Jaqueline Pereira da Silva, Kimberly Dukes, Jure Baloh, Melissa Ward, Hugh P. Salehi, Heather Schacht Reisinger, Priyadarshini R. Pennathur, Loreen Herwaldt
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 12 / December 2023
- Published online by Cambridge University Press:
- 12 April 2023, pp. 1979-1986
- Print publication:
- December 2023
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background:
Healthcare personnel (HCP) may encounter unfamiliar personal protective equipment (PPE) during clinical duties, yet we know little about their doffing strategies in such situations.
Objective:To better understand how HCP navigate encounters with unfamiliar PPE and the factors that influence their doffing strategies.
Setting:The study was conducted at 2 Midwestern academic hospitals.
Participants:The study included 70 HCP: 24 physicians and resident physicians, 31 nurses, 5 medical or nursing students, and 10 other staff. Among them, 20 had special isolation unit training.
Methods:Participants completed 1 of 4 doffing simulation scenarios involving 3 mask designs, 2 gown designs, 2 glove designs, and a full PPE ensemble. Doffing simulations were video-recorded and reviewed with participants during think-aloud interviews. Interviews were audio-recorded and analyzed using thematic analysis.
Results:Participants identified familiarity with PPE items and designs as an important factor in doffing. When encountering unfamiliar PPE, participants cited aspects of their routine practices such as designs typically used, donning and doffing frequency, and design cues, and their training as impacting their doffing strategies. Furthermore, they identified nonintuitive design and lack of training as barriers to doffing unfamiliar PPE appropriately.
Conclusion:PPE designs may not be interchangeable, and their use may not be intuitive. HCP drew on routine practices, experiences with familiar PPE, and training to adapt doffing strategies for unfamiliar PPE. In doing so, HCP sometimes deviated from best practices meant to prevent self-contamination. Hospital policies and procedures should include ongoing and/or just-in-time training to ensure HCP are equipped to doff different PPE designs encountered during clinical care.
Chronic Antibiotic Suppression for Nonstaphylococcal Prosthetic Joint Infections Treated with Debridement or Implant Retention
- Poorani Sekar, Rajeshwari Nair, Brice Beck, Bruce Alexander, Kelly Miell, Aaron Tande, Kimberly Dukes, Julia Friberg, Marin Schweizer, Andrew Pugely
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue S1 / July 2021
- Published online by Cambridge University Press:
- 29 July 2021, pp. s3-s4
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Early postoperative and acute prosthetic joint infection (PJI) may be managed with debridement, antibiotics, and implant retention (DAIR). Among patients with nonstaphylococcal PJI, an initial 4–6-week course of intravenous or highly bioavailable oral antibiotics is recommended in the Infectious Diseases Society of America (IDSA) guidelines, with disagreement among committee members on the need for subsequent chronic oral antimicrobial suppression (CAS). We aimed to characterize patients with nonstaphylococcal PJI who received CAS and to compare them to those who did not receive CAS. Methods: This retrospective cohort study included patients admitted to Veterans’ Affairs (VA) hospitals from 2003 to 2017 who had a PJI caused by nonstaphylococcal bacteria, underwent DAIR, and received 4–6 weeks of antimicrobial treatment. PJI was defined by Musculoskeletal Infection Society (MSIS) 2011 criteria. CAS was defined as at least 6 months of oral antibiotics following initial treatment of the PJI. Patients were followed for 5 years after debridement. We used χ2 tests and t tests were used to compare patients who received CAS with those who did not receive CAS. Results: Overall, 561 patients had a nonstaphylococcal PJI treated with DAIR, and 80.6% of patients received CAS. The most common organisms causing PJI were streptococci. We detected no significant differences between patients who received CAS and those who did not receive CAS, except that modified Acute Physiology and Chronic Health Evaluation (mAPACHE) scores were higher among patients who did not receive CAS (Table 1). Conclusion: Patients not on CAS were more severely ill (by mAPACHE) than those on CAS. Otherwise, the 2 groups were not different. This finding was contrary to our hypothesis that patients with multiple comorbidities or higher mAPACHE scores would be more likely to get CAS. A future analysis will be conducted to assess treatment failure in both groups. We hope to find a specific cohort who may benefit from CAS and hope to deimplement CAS in others who may not benefit from it.
Funding: No
Disclosures: None
Table 1. 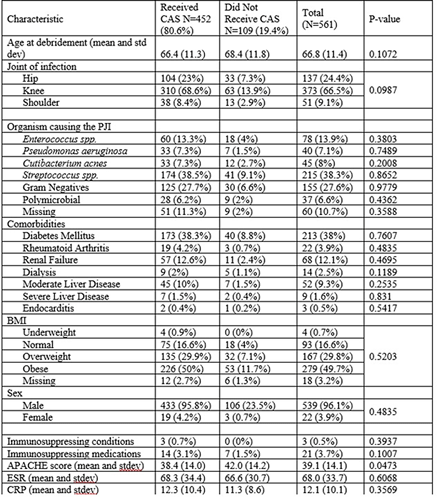
Fostering innovation at Academic Medical Centers: The Case of University of Colorado Anschutz Medical Campus
- Cigdem H. Benam, Gali Baler, Richard Duke, Demetria M. McNeal, Kimberly A. Muller, Cathy Bodine, Elaine H. Morrato, Ronald J. Sokol
-
- Journal:
- Journal of Clinical and Translational Science / Volume 5 / Issue 1 / 2021
- Published online by Cambridge University Press:
- 17 May 2021, e148
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Commercializing biomedical discoveries is a challenging process for many reasons. However, Academic Medical Centers (AMC) that have teaching, patient care, research, and service engrained in their mission are well poised to host these discoveries. These academic discoveries can lead to improvement in patient health and economic development if supported to cross the “valley of death” through institutional assistance, by providing guidance, gap funding and product development expertise. Colorado has a vibrant local startup ecosystem, state support for commercialization and entrepreneurship as well as critical mass of product development expertise. University of Colorado Anschutz Medical Campus, as a major AMC, is an engine for growth for the region. This article discusses innovation efforts at the University of Colorado Anschutz Medical Campus as a case study, which is built around two major efforts: the CCTSI and CU Innovations. I-Corps at CCTSI and the SPARK|REACH program of CU Innovations have been instrumental in fostering innovation, commercialization, and entrepreneurship on the campus.
The Role of Routine Practice in Healthcare Worker Strategies when Doffing Unfamiliar Personal Protective Equipment
- Emily Chasco, Jaqueline Pereira da Silva, Kimberly Dukes, Jure Baloh, Melissa Ward, Hugh Salehi, Heather Reisinger, Priyadarshini Pennathur, Loreen Herwaldt Abbott
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, p. s410
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Appropriate doffing of personal protective equipment (PPE) prevents healthcare worker (HCW) self-contamination and spread of pathogens. HCWs may encounter an array of PPE types (eg, gloves, gowns, masks) and designs (eg, masks with elastic ear loops vs ties) during their duties, some of which may be unfamiliar. We know little about how HCWs strategize when doffing unfamiliar PPE. As part of a larger study examining the doffing process and the risk of self-contamination, we used qualitative methods to explore factors influencing HCW PPE doffing strategies. Methods: In total, 70 HCW participants from 2 Midwestern academic hospitals were assigned to 1 of 4 doffing simulation scenarios. In the first 3 scenarios, participants were asked to doff 3 mask designs (n = 10), 2 gown designs (n = 10), or 2 glove designs (n = 10). In the fourth scenario, HCWs with different levels of training (n = 40) participated in 2 doffing simulations randomized per participant: a distraction simulation and a nondistraction simulation (using identical PPE types and designs). In all scenarios, participants were instructed to doff in their usual manner. Doffing performances were video-recorded. Participants then reviewed the recordings and took part in short semistructured interviews about their performance. Interviews were audio-recorded, transcribed, and analyzed using thematic analysis. Results: When faced with unfamiliar PPE during the simulations, participants were required to problem solve. In so doing, participants reported drawing on their day-to-day routine practices with familiar PPE to inform their doffing strategies. Aspects of routine practice identified as influential included PPE types typically worn, PPE donning and doffing order, doffing frequency, familiar PPE design cues, and experience tailoring strategies to specific patient care contexts. Participants frequently reported the desire to avoid self-contamination as driving doffing strategies and problem solving, but they also noted unique patient care demands related to their specific roles when they explained their doffing decisions. At the same time, HCWs identified lack of familiarity, lack of training, and nonintuitive design as barriers to doffing appropriately when encountering unfamiliar PPE. Conclusions: Different PPE designs may not be interchangeable, and proper doffing techniques may not be intuitive. The previous experiences of HCWs informed their strategies when doffing unfamiliar PPE. However, this practice sometimes caused them to use inappropriate doffing techniques and resulted in self-contamination. This finding has important implications for hospital policies and procedures regarding the introduction of new PPE and indicates that HCWs need training when new items are introduced.
Funding: None
Disclosures: None
Self-Contamination While Doffing Personal Protective Equipment
- Jaqueline Pereira da Silva, Priyadarshini Pennathur, Hugh Salehi, Emily Chasco, Jure Baloh, Kimberly Dukes, Melissa Ward, Heather Reisinger, Loreen Herwaldt Abbott
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s385-s386
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Personal protective equipment (PPE) effectiveness can be undermined by inappropriate doffing methods. Objective: We used human factors engineering methods to evaluate self-contamination during PPE doffing. Methods: In this study, 30 participants at a Midwestern academic hospital (A) donned and doffed 3 mask styles (n = 10), 2 gown styles (n = 10), and 2 glove styles (n = 10; the Doffy glove has a tab to facilitate doffing). Also, 30 additional participants at hospital A (residents or fellows, nurses, special isolation trained staff [SITS]) and 10 SITS at academic hospital B doffed a surgical mask, a breakaway neck gown, and exam gloves (PPE ensemble) twice: once while distracted with conversation and once when not distracted. We randomized the order in which participants used different PPE styles or they did the doffing scenario. We collected demographic data. We applied Glo Germ Mist (1.5 dilution in water) with a mucosal atomizer to participants’ PPE before they doffed. We video-recorded participants as they doffed, and we photographed their scrubs and exposed skin before and after each donning and doffing episode. We reviewed videos for doffing errors and photographs for fluorescent spots. We counted fluorescent spots and noted their locations. Results: Overall, 45 (64.3%) participants were women, 31 (44.3%) were nurses, 24 (34.3%) were physicians. Among the participants, 25 (35.7%) had >15 years of experience and 61 (87.1%) had some training in doffing. Participants frequently contaminated their skin or clothing while doffing (Table 1). For all scenarios, hands followed by the torso were contaminated most frequently. Analysis of the videos found that touching the gown front with bare hands was the most common doffing error. Fewer participants self-contaminated when using the Doffy glove without training than when using the standard exam glove. Although most participants in the glove trial indicated that they did not need to watch the Doffy glove training video again, most had difficulty doffing the Doffy glove with the beak method. Many participants stopped doffing to answer questions when they doffed the PPE ensemble during the interruption scenario. Conclusions: Self-contamination was very common with all PPE styles and during all scenarios. Distraction did not increase the risk of contamination. However, participants often stopped doffing to answer questions, which they rarely do in practice. Watching a video was inadequate training for the beak glove-doffing method. The Doffy glove, which decreased contamination compared with the standard glove in the untrained scenario, may have advantages over standard exam gloves and should be evaluated further.
Funding: None
Disclosures: None
2234 Developing the future translational science workforce at the University of Iowa
- James Torner, Beth R. Knudson, Kimberly Dukes
-
- Journal:
- Journal of Clinical and Translational Science / Volume 2 / Issue S1 / June 2018
- Published online by Cambridge University Press:
- 21 November 2018, pp. 53-54
-
- Article
-
- You have access Access
- Open access
- Export citation
-
OBJECTIVES/SPECIFIC AIMS: To evaluate the extent to which the curriculum delivered via an innovative program, the Early Scholars Certificate in Clinical and Translational Science (CCTS) at the University of Iowa (UI), develops a translational science workforce pipeline by increasing awareness of and interest in translational science as a career goal for highly prepared undergraduates. METHODS/STUDY POPULATION: The CCTS’s objective is to increase the awareness of the philosophy and tools of translational science and to incorporate critical evaluation and self-appraisal of the translational aspects of a scholar’s own research. CCTS is a 16-semester-hour (sh) academic certificate program introducing translational science concepts and careers to undergraduate students. The CCTS is a selective program with requirements including a minimum GPA, minimum sh completed, completion of course prerequisites, and already engaged and supported by mentored research. The curriculum includes electives in the area of their research interests (6 sh); graduate level Epidemiology (3 sh); Biostatistics (3 sh); and 2 core Translational Research courses (4 sh total). The first core course, an Introduction to Translational Research, is a survey course providing students the opportunity to learn how translational research is conceived and developed. It is designed to instruct the student how to interpret their research in a translational T1 to T4 paradigm. The program’s capstone course, Practicum in Translational Research, provides undergraduate students the opportunity to address how their research experience translates into clinical practice. Student’s spend the majority of this course’s contact hours in a shadowing experience with a clinician in the area of their research. Students reflect on this shadowing experience and its relevance to their academic and professional goals. The students also spend time developing skills in peer review—not only learning to provide constructive feedback to other research professionals, but also how to receive and integrate the feedback. The course includes a mock research fair where both UI faculty and classmates provide feedback that is later integrated into their capstone projects—a poster presentation at the UI Carver College of Medicine Research Fair as well as a final translational paper. As part of the ongoing evaluation of the program and graduates, we examined the participant data, the course satisfaction with content, the change in understanding of translational science, and the intention to incorporate translational science into research and career goals. We also conducted course evaluation surveys and qualitative analysis of a focus group and interviews. RESULTS/ANTICIPATED RESULTS: Since 2015, the CCTS program has introduced translational science curriculum to 20 undergraduate participants (men/woman 40%/60%; 5% Hispanic or Latino; 15% Center for Diversity and Enrichment Eligible). Areas of academic interest include: biology, genetics, engineering, bioinformatics, biochemistry, neuroscience, psychology, and microbiology. Graduates of the Certificate and degree program to date (n=8) have gone onto: Fullbright awards (1), medical school/Masters in public health (1), combined MD/PhD programs (2), biomedical PhD program (1), or currently work in translational science positions in industry (2). In questionnaire and focus group results, we found that in general, students reported increased understanding of the translational spectrum and felt the certificate program helped them clarify their educational or career goals. Data from both the focus group and the questionnaire demonstrate that students are strongly positive about the program in general, including its quality, faculty and guest speakers, structure, goals, opportunities, personality, and personnel. All students highly valued many elements of the program and each course, and particularly the opportunity for clinical shadowing. Among the questionnaire findings for 2016–17, all students (100%) rated program quality “excellent,” and 7 of 8 (87.5%) “strongly agreed” that they better understood translational science, that they saw themselves continuing in translational science research after graduation, and they were better able to communicate how their lab research fits within the translational spectrum. In each case 1 of 8 “agreed.” Participants also generally felt that their career goals had been affirmed or realigned, and that they were better able to communicate the meaning of translational science to multiple audiences. Responses on changes to career aspirations and plans were mixed, and are ambiguous. Questionnaire Item 4, “My UI curricular and/or co-curricular plans changed as a result of the CCTS program,” which had mixed responses, asked specifically about the CCTS program as a reason for change, but it is not clear if, whether, or how the program specifically wants to change curricular plans. In the focus group, students reported using their individual shadowing and lab experience in determining preferences and intentions about future career choices (e.g., whether or not to apply to medical school and/or pursue basic science research). Participants perceived the shadowing experience, complementing or contrasting their lab research, as particularly relevant in deciding about their future careers. Other themes that emerged from the focus group and/or open section of the questionnaire demonstrate the impact of various course elements on participants’ understanding of translational science and potential careers, including: quality of instruction, program and course content (including guest speakers, the shadowing experience, and the poster development process); the exposure to a range of possibilities along the translational spectrum and the expansion of ideas about what research could look like; the value of connections (to faculty, researchers and clinicians, and other CCTS students and alumni); the attributes of the cohort; and the “personality” of the program and personnel. DISCUSSION/SIGNIFICANCE OF IMPACT: Developing a pipeline for translational science workforce development has been problematic because a lack of the understanding of the need of translational research and a structuring a time efficient program for early career clinical and basic scholars. Undergraduates making critical decisions about educational paths and career goals and plans may not be aware of opportunities in translational science or the type of choices they need to make to prepare for such opportunities. Our data demonstrates that CCTS was an effective way of introducing translational science concepts and career paths to undergraduate students and potentially a powerful way to encourage them to consider these career paths. Participants in our program improved their knowledge of the field and expressed interest and intention to incorporate translational science training into their career plans. However, improvements can be made in the CCTS program. Additionally, CTSAs should consider ways to incorporate findings like these into a wider sphere of training to help develop and strengthen a translational science workforce for the future. The exposure to a variety of translational science career possibilities and specialties was important to students. Based on both focus group discussion and questionnaire data, a few students did expand slightly their sense of career possibilities, but the larger benefit may be their concrete experiences that validate or solidify their interests, making them more skilled at talking about and supporting their career goals on applications and in interviews. Shadowing did not always encourage students to go into clinical medicine, but often solidified interests or leanings students already had, giving them a more grounded basis for refining their decisions. For some students, shadowing a clinician confirmed ideas of being a physician; for others, it steered them away from it. Some now found ethical challenges, bureaucracy, or emotional challenges daunting or newly necessary to consider before focusing on clinical careers. This may be just what students need at this point, and emphasizes for them the relation between different kinds of research and application within translational science. Our evaluation suggests that CCTS contributes to academic choices for career development and additionally can help attract highly skilled students into TS research, including students of color. Future work to evaluate CCTS impact on graduates’ career outcomes will inform the translational research direction and content. In terms of program design, it could be useful to build in multiple opportunities for students to understand the diversity of translational science careers and provide students more exposure to different possibilities in clinical and translational work.
Research Agenda for Microbiome Based Research for Multidrug-resistant Organism Prevention in the Veterans Health Administration System
- Part of
- Ashley E. Kates, Jessica S. Tischendorf, Marin Schweizer, Loreen Herwaldt, Matthew Samore, Kimberly C. Dukes, Dale N. Gerding, Daniel J. Diekema, Nasia Safdar
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 39 / Issue 2 / February 2018
- Published online by Cambridge University Press:
- 08 February 2018, pp. 202-209
- Print publication:
- February 2018
-
- Article
-
- You have access Access
- HTML
- Export citation
Effectiveness of Measures to Eradicate Staphylococcus aureus Carriage in Patients with Community-Associated Skin and Soft-Tissue Infections: A Randomized Trial
- Stephanie A. Fritz, Bernard C. Camins, Kimberly A. Eisenstein, Joseph M. Fritz, Emma K. Epplin, Carey-Ann Burnham, Jonathan Dukes, Gregory A. Storch
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 32 / Issue 9 / September 2011
- Published online by Cambridge University Press:
- 02 January 2015, pp. 872-880
- Print publication:
- September 2011
-
- Article
- Export citation
-
Background.
Despite a paucity of evidence, decolonization measures are prescribed for outpatients with recurrent Staphylococcus aureus skin and soft-tissue infection (SSTI).
Objective.Compare the effectiveness of 4 regimens for eradicating S. aureus carriage.
Design.Open-label, randomized controlled trial. Colonization status and recurrent SSTI were ascertained at 1 and 4 months.
Setting.Barnes-Jewish and St. Louis Children's Hospitals, St. Louis, Missouri, 2007–2009.
Participants.Three hundred patients with community-onset SSTI and S. aureus colonization in the nares, axilla, or inguinal folds.
Interventions.Participants were randomized to receive no therapeutic intervention (control subjects) or one of three 5-day regimens: 2% mupirocin ointment applied to the nares twice daily, intranasal mupirocin plus daily 4% chlorhexidine body washes, or intranasal mupirocin plus daily dilute bleach water baths.
Results.Among 244 participants with 1-month colonization data, modified intention-to-treat analysis revealed S. aureus eradication in 38% of participants in the education only (control) group, 56% of those in the mupirocin group (P = .03 vs controls), 55% of those in the mupirocin and chlorhexidine group (P = .05), and 63% off those in the mupirocin and bleach group (P = .006). Of 229 participants with 4-month colonization data, eradication rates were 48% in the control group, 56% in the mupirocin only group (P = .40 vs controls), 54% in the mupirocin and chlorhexidine group (P = .51), and 71% in the mupirocin and bleach group (P = .02). At 1 and 4 months, recurrent SSTIs were reported by 20% and 36% of participants, respectively.
Conclusions.An inexpensive regimen of dilute bleach baths, intranasal mupirocin, and hygiene education effectively eradicated S. aureus over a 4-month period. High rates of recurrent SSTI suggest that factors other than endogenous colonization are important determinants of infection.
Trial Registration.ClinicalTrials.gov identifier: NCT00513799.




