2 results
Assessment of COVID-19 Infection Prevention and Control Capabilities in 39 Haitian Hospitals
- Afeke Kambui, Mentor Lucien, Catherine Emilien, Francois Staco, Ymeline Pateau St Vil, Pierre Philippe Wilson Registe, Mackenley Brice, Dassaëve Brice, Nathan Zephirin, Sandra Benjamin, Martha Murdock
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue S1 / July 2021
- Published online by Cambridge University Press:
- 29 July 2021, p. s66
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Infection prevention and control (IPC) is key (1) to keeping health workers and patients safe from contracting infections during care, (2) to enabling continuity of essential health services, and (3) to pandemic preparedness and response. Frontline health workers are at 3-fold increased risk for COVID-19 (Lancet 2020) and account for 6% of COVID-19 hospitalizations (CDC 2020). With the support of the US Agency for International Development Bureau of Humanitarian Assistance (USAID/BHA) and collaboration of the Haitian Ministry of Health (MSPP), MSH’s Rapid Support to COVID-19 Response in Haiti project (RSCR Haiti) developed an instrument to assess select public hospitals and identify IPC gaps that informed COVID-19 response and system strengthening measures for increasing patient and provider safety. Methods: The IPC tool contains 13 IPC domains and 80 questions, for a total of 600 points. It was developed based on the World Health Organization IPC Assessment Framework for Health Facilities (2018) and US Centers for Disease Control Facility Readiness Assessment for COVID-19 (2020). In total, 39 health facilities chosen by the MSPP across all 10 departments of Haiti were evaluated in October 2020. Data were analyzed in Microsoft Excel by category, site, and IPC capabilities then classified as inadequate, basic, intermediate or advanced. Results: IPC capabilities scored as inadequate in 18% and basic in 67% of hospitals (Graph 1). No institution was advanced. Among health facilities, IPC programs existed in only 18%; IPC guidelines or procedures were present in 38%; staff were trained regularly in 12%; and healthcare-associated infection surveillance was performed in 19%. Systems for COVID-19 triage existed in 56%; 39% had IPC commodity management systems; 45% provided COVID-19 training; 26% practiced monitoring of staff and patients for COVID-19; 36% had protocols for an influx of COVID-19 cases; and 72% practiced risk communication (Table 1). Conclusions: No health facility was sufficiently equipped to implement adequate COVID-19 IPC measures, and all needed strengthening, even in the highest-scoring IPC areas. Through RSCR Haiti, MSH and MSPP were able to identify and address priorities in hospitals: establishing hospital IPC programs; training staff; monitoring health workers and patients; and implementing guidance, triage, and commodity-management systems. This study demonstrates that it is possible to do a quick yet thorough assessment to rapidly identify IPC needs and opportunities, using the results to rapidly build response capacity. Haiti’s experience of integrating locally contextualized global IPC tools to inform systemic COVID-19 response measures can benefit other experts globally.
Funding: United States Agency for International Development Bureau of Humanitarian Assistance (USAID/BHA)
Disclosures: None
Figure 1.
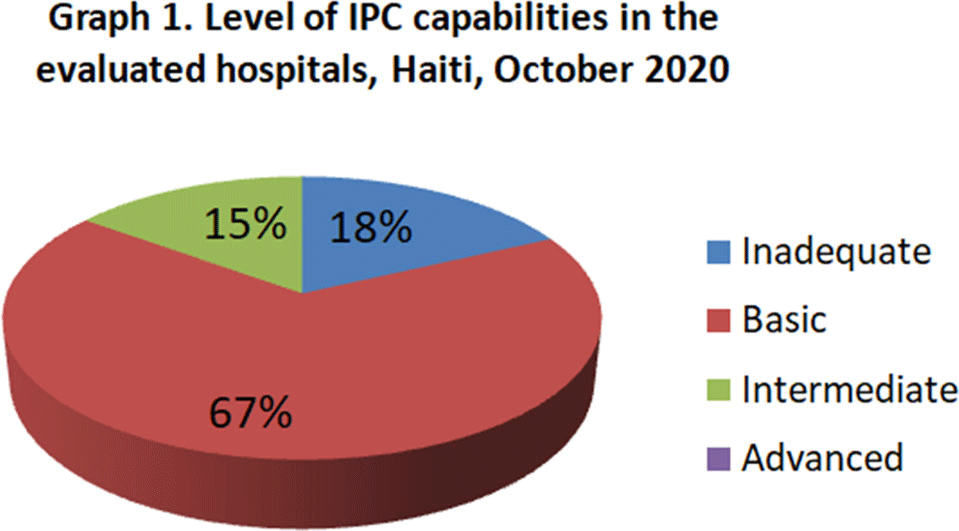
Table 1. 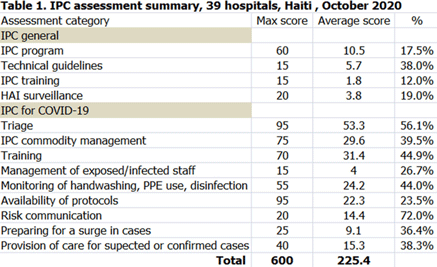
A Multicenter Point-Prevalence Survey of Antibiotic Use in Haiti, June–August 2019: Findings and Implications
- Hatim Sati, Mentor Ali Ber Lucien, Jenny Hsieh, Jean-Baptiste Theodule, Mauricio Cerpa, Nienke Bruinsma, Gerard Joseph, Patrick Dely, Jacques Boncy, Maria del Pilar Ramon-Pardo
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s20-s21
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Inappropriate use of antibiotics in hospitalized settings contributes to the selection and emergence of antimicrobial-resistant pathogens. This trend is particularly challenging in resource-constrained settings where the high burden of infectious diseases, combined with suboptimal infection prevention and control measures, are further complicated by limited access to reliable microbiological services to inform antimicrobial prescription at the patient level. In this study, we describe the use of antibiotics in selected Haitian hospitals; we aimed to create a baseline to inform antimicrobial stewardship interventions. Methods: WHO/PAHO Hospital Antibiotic Use Point Prevalence Survey (HAMU-PPS) were conducted in 6 acute-care Haitian hospitals: La-Paix and Hospital-Albert (June 2019) and Hospital-Universitaire-Justinien, Hospital-Bienfaisance-de-Pignon, Hospital-Sacre-Coeur-de-Milot, and Hospital Immaculee-Conception-des-Cayes (July-August 2019) in 6 different cities. Trained data collectors completed electronic forms using REDCap software including data related to antibiotic use, indications, and utilization of laboratory services from medical records of all inpatients meeting study inclusion criteria. Analyses were done using Microsoft Excel software (v2016). Results: In total, 510 inpatients records were surveyed. Patients ages ranged from 0 to 92, with median age of 27 years (IQR, 4–47); 269 were women (57.7%) and 239 were men (46.9%). The prevalence of antibiotic use was 73% (95% CI, 68.2%–81.8 %); this prevalence was 74.5% among men (178 of 239) and 70.6% among women (190 of 269). The highest antibiotic use was observed among children aged <1 year (98 of 108, 90.7%). Of the patients on antibiotics, 63% were treated with >1 antibiotic. In addition, 384 indications for antibiotic prescription were reported. Of the indications for antibiotics therapy, 49.7% (191 of 384) were for treatment, and 49% (188 of 384) were for prophylaxis. Of the treatments, 92% were empiric with 6% reported as targeted. Only 13% (50 of 370) of the patient records indicated that samples were taken for microbiological identification. Of those, 9 had results for culture, and 1 had results for drug susceptibility. The most commonly reported antibiotic was ceftriaxone (n = 110, 23%) followed by ampicillin (n = 153, 21.4%) and metronidazole (n = 135, 20%). Conclusions: This study shows high use of antibiotics among hospitalized patients in Haitian hospitals, especially in children aged <1 year. Almost all the antibiotics were prescribed as either empiric or prophylaxis therapy, with very few microbiology samples collected. These results suggest limited laboratory corroboration across hospitals to inform antibiotic use. Implementation of antimicrobial stewardship interventions is recommended to optimize antibiotic therapy and to mitigate antimicrobial resistance in hospital care settings, but adaptation of the methodology should be done in settings with limited laboratory capacity.
Funding: None
Disclosures: None





