2 results
Bloodstream infection burden among cancer clinic patients with PICC Lines: A prospective, observational study
- Jessica Bethlahmy, Hiroki Saito, Bardia Bahadori, Thomas Tjoa, Shereen Nourollahi, Mohamad Alsharif, Justin Chang, Linda Armendariz, Vincent Torres, Sandra Masson, Edward Nelson, Richard Van Etten, Syma Rashid, Raheeb Saavedra, Raveena D. Singh, Shruti Gohil
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, p. s49
-
- Article
-
- You have access Access
- Open access
- Export citation
-
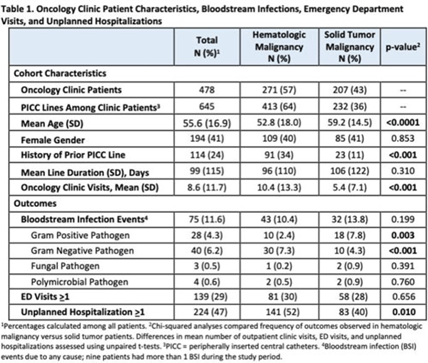
Background: Oncology patients are at high risk for bloodstream infection (BSI) due to immunosuppression and frequent use of central venous catheters. Surveillance in this population is largely relegated to inpatient settings and limited data are available describing community burden. We evaluated rates of BSI, clinic or emergency department (ED) visits, and hospitalizations in a large cohort of oncology outpatients with peripherally inserted central catheters (PICCs). Methods: In this prospective, observational study, we followed a convenience sample of adults (age>18) with PICCs at a large academic outpatient oncology clinic for 35 months between July 2015 and November 2018. We assessed demographics, malignancy type, PICC insertion and removal dates, history of prior PICC, and line duration. Outcomes included BSI events (defined as >1 positive blood cultures or >2 positive blood cultures if coagulase-negative Staphylococcus), ED visits (without hospitalization), and unplanned hospitalizations (excluding scheduled chemotherapy hospitalizations). We used χ2 analyses to compare the frequency of categorical outcomes, and we used unpaired t tests to assess differences in means of continuous variable in hematologic versus solid-tumor malignancy patients. We used generalized linear mixed-effects models to assess differences in BSI (clustered by patient) separately for gram-positive and gram-negative BSI outcomes. Results: Among 478 patients with 658 unique PICC lines and 64,190 line days, 271 patients (413 lines) had hematologic malignancy and 207 patients (232 lines) had solid-tumor malignancy. Cohort characteristics and outcomes stratified by malignancy type are shown in Table 1. Compared to those with hematologic malignancy, solid-tumor patients were older, had 47% fewer clinic visits, and had 32% lower frequency of prior PICC lines. Overall, there were 75 BSI events (12%; 1.2 per 1,000 catheter days). We detected no significant difference in BSI rates when comparing solid-tumor versus hematologic malignancies (P = 0.20); BSIs with gram-positive pathogen were 69% higher in patients with solid tumors. Gram-negative BSIs were 41% higher in patients with hematologic malignancy. Solid-tumor malignancy was associated with 4.5-fold higher odds of developing BSI with gram-positive pathogen (OR, 4.48; 95% CI, 1.60–12.60; P = .005) compared to those with hematologic malignancy, after adjusting for age, sex, history of prior PICC, and line duration. Differences in gram-negative BSI were not significant on multivariate analysis. Conclusions: The burden of all-cause BSIs in cancer clinic adults with PICC lines was 12% or 1.2 per 1,000 catheter days, as high as nationally reported inpatient BSI rates. Higher risk of gram-positive BSIs in solid-tumor patients suggests the need for targeted infection prevention activities in this population, such as improvements in central-line monitoring, outpatient care, and maintenance of lines and/or dressings, as well as chlorhexidine bathing to reduce skin bioburden.
Disclosures: None
Impact of a Central-Line Insertion Site Assessment (CLISA) score on localized insertion site infection to prevent central-line–associated bloodstream infection (CLABSI)
- Shruti K. Gohil, Jennifer Yim, Kathleen Quan, Maurice Espinoza, Deborah J. Thompson, Allen P. Kong, Bardia Bahadori, Tom Tjoa, Chris Paiji, Scott Rudkin, Syma Rashid, Suzie S. Hong, Linda Dickey, Mohamad N. Alsharif, William C. Wilson, Alpesh N. Amin, Justin Chang, Usme Khusbu, Susan S. Huang
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue 1 / January 2020
- Published online by Cambridge University Press:
- 08 November 2019, pp. 59-66
- Print publication:
- January 2020
-
- Article
- Export citation
-
Objective:
To assess the impact of a newly developed Central-Line Insertion Site Assessment (CLISA) score on the incidence of local inflammation or infection for CLABSI prevention.
Design:A pre- and postintervention, quasi-experimental quality improvement study.
Setting and participants:Adult inpatients with central venous catheters (CVCs) hospitalized in an intensive care unit or oncology ward at a large academic medical center.
Methods:We evaluated CLISA score impact on insertion site inflammation and infection (CLISA score of 2 or 3) incidence in the baseline period (June 2014–January 2015) and the intervention period (April 2015–October 2017) using interrupted times series and generalized linear mixed-effects multivariable analyses. These were run separately for days-to-line removal from identification of a CLISA score of 2 or 3. CLISA score interrater reliability and photo quiz results were evaluated.
Results:Among 6,957 CVCs assessed 40,846 times, percentage of lines with CLISA score of 2 or 3 in the baseline and intervention periods decreased by 78.2% (from 22.0% to 4.7%), with a significant immediate decrease in the time-series analysis (P < .001). According to the multivariable regression, the intervention was associated with lower percentage of lines with a CLISA score of 2 or 3, after adjusting for age, gender, CVC body location, and hospital unit (odds ratio, 0.15; 95% confidence interval, 0.06–0.34; P < .001). According to the multivariate regression, days to removal of lines with CLISA score of 2 or 3 was 3.19 days faster after the intervention (P < .001). Also, line dwell time decreased 37.1% from a mean of 14 days (standard deviation [SD], 10.6) to 8.8 days (SD, 9.0) (P < .001). Device utilization ratios decreased 9% from 0.64 (SD, 0.08) to 0.58 (SD, 0.06) (P = .039).
Conclusions:The CLISA score creates a common language for assessing line infection risk and successfully promotes high compliance with best practices in timely line removal.




