260 results
Treatment Interruptions and Mortality among Puerto Rican Women with Gynecologic Cancers in Puerto Rico after Hurricanes Irma and María: A Retrospective Cohort Study
- Fabiola A. Rivera-Gastón, Sharee Umpierre-Catinchi, Jeslie M. Ramos-Cartagena, Karen J. Ortiz-Ortiz, Carlos R. Torres-Cintrón, Sandra I. García-Camacho, William A. Calo, Guillermo Tortolero-Luna, Liz M. Martínez Ocasio, Ana P. Ortiz
-
- Journal:
- Disaster Medicine and Public Health Preparedness / Accepted manuscript
- Published online by Cambridge University Press:
- 21 May 2024, pp. 1-12
-
- Article
- Export citation
-
Objective:
Cancer patients are among the most vulnerable populations during and after a disaster. We evaluated the impact of treatment interruption on the survival of women with gynecologic cancer in Puerto Rico following hurricanes Irma and María.
Methods:Retrospective cohort study among a clinic-based sample of women diagnosed between January 2016-September 2017 (n=112). Women were followed up from their diagnosis until December 2019, to assess vital status. Kaplan-Meier survival curves and Cox proportional hazards models were performed.
Results:Mean age was 56 (±12.3) years; corpus uteri (58.9%) was the most common gynecologic cancer. Predominant treatments were surgery (91.1%) and chemotherapy (44.6%). Overall, 75.9% were receiving treatment before the hurricanes, 16.1% experienced treatment interruptions and 8.9% died during the follow-up period. Factors associated with treatment interruption in bivariate analysis included younger age (≤55 years), having regional/distant disease, and receiving >1 cancer treatment (p<0.05). Crude analysis revealed an increased risk of death among women with treatment interruption (HR: 3.88, 95% CI=1.09-13.77), persisting after adjusting for age and cancer stage (HR: 2.49, 95% CI= 0.69-9.01).
Conclusions:Findings underscore the detrimental impact of treatment interruption on cancer survival in the aftermath of hurricanes, emphasizing the need for emergency response plans for this vulnerable population.
Evaluating the effectiveness of a Mexican strain of Duddingtonia flagrans as a biological control agent against gastrointestinal nematodes in goat faeces
- N.F. Ojeda-Robertos, P. Mendoza-de Gives, J.F.J. Torres-Acosta, R.I. Rodríguez-Vivas, A.J. Aguilar-Caballero
-
- Journal:
- Journal of Helminthology / Volume 79 / Issue 2 / June 2005
- Published online by Cambridge University Press:
- 12 April 2024, pp. 151-157
-
- Article
- Export citation
-
The use of Duddingtonia flagrans in the control of goat nematodes was investigated. Initially, the time of passage of chlamydospores through the digestive tract of goats was evaluated. Two groups of seven parasite-free kids were formed. Group A received a single dose of 3.5×106 D. flagrans chlamydospores (FTHO-8 strain) per kg of live weight. Group B did not receive any chlamydospores. Faeces were obtained from each kid daily from day 4 prior to inoculation until day 5 post-inoculation (PI) and were placed in Petri dishes containing water agar. Gastrointestinal nematode infective larvae were added to each Petri dish and incubated at 25°C for 7 days. Petri dishes were examined to detect the fungus and trapped nematodes. A second trial evaluated the effect of D. flagrans on the number of gastrointestinal nematode larvae harvested from goat faecal cultures in naturally infected goats. Two groups of seven goats were formed. The treated group received a single dose of 3.5×106 D. flagrans chlamydospores per kg of liveweight. The control group did not receive any chlamydospores. Faeces were obtained twice daily from each kid. Two faecal cultures were made for each kid. One was incubated for 7 days and the other for 14 days. Gastrointestinal nematode larvae were recovered from each culture and counted. Percentage of larval development reduction was determined using a ratio of larvae/eggs deposited in the control and treated groups. Duddingtonia flagrans survived the digestive process of goats, and maintained its predatory activity, being observed from 21 to 81 h PI (3 to 4 days). A reduction in the infective larvae population in the treated group compared to the non-treated group was observed in both incubation periods (7 days: 5.3–36.0%; 14 days: 0–52.8%, P>0.05). Although a single inoculation of D. flagrans can induce a reduction of infective larvae collected from faeces, a different scheme of dosing may be needed to enhance the efficacy of D. flagrans in goats.
Incidence of mental health diagnoses during the COVID-19 pandemic: a multinational network study
- Yi Chai, Kenneth K. C. Man, Hao Luo, Carmen Olga Torre, Yun Kwok Wing, Joseph F. Hayes, David P. J. Osborn, Wing Chung Chang, Xiaoyu Lin, Can Yin, Esther W. Chan, Ivan C. H. Lam, Stephen Fortin, David M. Kern, Dong Yun Lee, Rae Woong Park, Jae-Won Jang, Jing Li, Sarah Seager, Wallis C. Y. Lau, Ian C. K. Wong
-
- Journal:
- Epidemiology and Psychiatric Sciences / Volume 33 / 2024
- Published online by Cambridge University Press:
- 04 March 2024, e9
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Aims
Population-wide restrictions during the COVID-19 pandemic may create barriers to mental health diagnosis. This study aims to examine changes in the number of incident cases and the incidence rates of mental health diagnoses during the COVID-19 pandemic.
MethodsBy using electronic health records from France, Germany, Italy, South Korea and the UK and claims data from the US, this study conducted interrupted time-series analyses to compare the monthly incident cases and the incidence of depressive disorders, anxiety disorders, alcohol misuse or dependence, substance misuse or dependence, bipolar disorders, personality disorders and psychoses diagnoses before (January 2017 to February 2020) and after (April 2020 to the latest available date of each database [up to November 2021]) the introduction of COVID-related restrictions.
ResultsA total of 629,712,954 individuals were enrolled across nine databases. Following the introduction of restrictions, an immediate decline was observed in the number of incident cases of all mental health diagnoses in the US (rate ratios (RRs) ranged from 0.005 to 0.677) and in the incidence of all conditions in France, Germany, Italy and the US (RRs ranged from 0.002 to 0.422). In the UK, significant reductions were only observed in common mental illnesses. The number of incident cases and the incidence began to return to or exceed pre-pandemic levels in most countries from mid-2020 through 2021.
ConclusionsHealthcare providers should be prepared to deliver service adaptations to mitigate burdens directly or indirectly caused by delays in the diagnosis and treatment of mental health conditions.
High touch surface bioburden associated with the use of disinfectants with and without continuously active disinfection in ambulatory care settings
- Heidi M. Torres, Jamie Marino, Matthew S. Simon, Harjot K. Singh, Lars F. Westblade, David P. Calfee
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 45 / Issue 6 / June 2024
- Published online by Cambridge University Press:
- 20 February 2024, pp. 790-792
- Print publication:
- June 2024
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
A quaternary ammonium and alcohol-based disinfectant with reported continuous activity demonstrated reduced microbial buildup on surfaces over time compared to routine disinfectants without continuous activity in in vitro and hospital studies. We compared these disinfectants in ambulatory settings and found no difference in bioburden on high-touch surfaces over time.
Night-time/daytime Protein S100B serum levels in paranoid schizophrenic patients
- E. Diaz-Mesa, A. Morera-Fumero, L. Torres-Tejera, A. Crisostomo-Siverio, P. Abreu-Gonzalez, R. Zuñiga-Costa, S. Yelmo-Cruz, R. Cejas-Mendez, C. Rodriguez-Jimenez, L. Fernandez-Lopez, M. Henry-Benitez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S445-S446
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
S100B is a calcium-binding astrocyte-specific cytokine, that is considered a biomarker of neurodegeneration; which may be involved in the imbalance of the inflammatory response observed in several brain disorders, including major depression and schizophrenia. Two meta-analyses have reported higher serum levels of S100B in patients with schizophrenia respect to healthy controls.
Different studies have described circadian and seasonal variations of biological variables, such as melatonin or cortisol. It has been reported that there is not circadian rhythm of S100B blood levels in healthy subjects. However, it is not known whether there are circadian oscillations in S100B blood concentrations in patients with schizophrenia.
ObjectivesThe aim of this study is to describe S100B serum levels in patients with schizophrenia and to analyse whether they follow a circadian rhythm.
MethodsOur sample consists in 47 patients in acute phase and stabilized status. Blood samples were collected at 12:00 and 00:00 hours by venipuncture. Serum levels of Protein S100B were measured three times: at admission, discharge and three months after discharge. Protein S100B was measured by means of ELISA (Enzyme-linked immunosorbent assay) techniques.
Results12:00 24:00 P ADMISSION 132,95±199,27 85,85±121,44 0,004 DISCHARGE 73,65±71,744 75,80±123,628 0,070 CONTROL 43,49±34,60 40,14±23,08 0,47 P global P Admission Vs. Discharge P Admission Vs. Control P Discharge Vs. Control 0,97 There is a significance difference between 12:00 and 24:00 at admission for the Protein S100B.However, these difference did not occur at discharge and at three months after discharge.It can be interpreted as there is a circadian rhythm of Protein S100B when the patient has got a psychotic outbreak and disappears at discharge and when is psychopathologically stable.
ConclusionsWith respect to our results we can hypothesize that schizophrenic patients in acute relapse present circadian S100B rhythm that is not present when the patients are clinically stable.Furthermore, the decrease of serum protein S100B levels at discharge is indicative of a reduction of the cerebral inflammation, thus it can be a biomarker of cerebral inflammation and this reduction can be the effect of the treatment. Finally, its circadianity could be a guide of this process and clinical improvement.
Disclosure of InterestNone Declared
Assessment of executive functions through a virtual reality task in euthymic patients with bipolar disorder and influence in psychosocial functioning
- J. Andreu Martínez, D. Beltrán Cristancho, P. Navalón, P. Sierra San Miguel, A. García Blanco, A. Chicchi Glioli, S. Cervera Torres, M. Alcañiz Raya, Y. Cañada Pérez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S700
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Previous research has shown that neurocognitive deficits, especially deficits in executive functions, may persist during euthymia in in patients with bipolar disorder (BD) and that those are associated with an impairment of psychosocial functioning. The assessment of executive functions (EFs) is normally carried out using laboratory tests. Novel methodologies such as virtual reality (VR) allow the creation of immersive environments, to evaluate executive performance with greater potential for ecological validity than evaluations with standard tasks.
ObjectivesThe objectives of this project are to evaluate executive performance in euthymic patients with BD with a novel virtual reality task compared to standard computerized tasks, and to find predictors of functioning associated with cognitive performance.
MethodsThis is a cross sectional study in which 46 euthymic patients with BD treated at La Fe University and Polytechnic Hospital were assessed with a battery of standard computerized tasks (ST) (TMT/Stroop,/Go-No-Go/TOL/DOT) and with the Cooking Task virtual reality task. The Cooking Task presents 4 tasks of increasing difficulty in which you must cook food in a specific time. It records total time to complete the task, whether food is cooled or burned, the simultaneous use of two fires, the proper use of seasonings and the time to set the table.
Functioning was assessed with the Functioning Assessment Short Test (FAST) that evaluates the overall functioning of patients with a mental illness in 6 subscales.
Correlation analyses between cognitive performance variables and clinical variables were done. Multiple linear regression was performed with the FAST score as a dependent variable and cognitive performance variables and relevant clinical variables to executive functioning (months of euthymia, age, and number of total episodes) were included as independent variables.
ResultsA worse psychosocial functioning was significantly associated with a worse performance in standard tasks (TMTA, TMTB, STROOP, and TOL) and cooking task (total time spent on task 2, burning time and total time spent on task 3, and total time spent on task 4). In the regression analysis, the correct simultaneous use of the two fires was the best predictor of a better psychosocial functioning in BD patient. This implies the preserved ability of planning and performing dual tasks.
ConclusionsOur findings suggest that euthymic patients with BD present deficits in executive functions related with a worse psychosocial functioning. Among the tasks, the cooking task may have a greater sensitivity than standards task to predict real functioning. This in an opportunity to design virtual applications for diagnostic and therapeutic purposes.
Disclosure of InterestNone Declared
Use of Caripracina in a case of manic episode with psychotic symptoms difficult to treat due to side effects with the use of psychotropic medication. A case report
- P. Casado De La Torre
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S708-S709
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
There are manic episodes to involve a challenge in treatment due to finding resistance or secondary effects with the drugs of choice, this situation oblige forcing us to seek alternatives in the data sheet.
ObjectivesTo describe the complicated evolution of a case of acute mania difficult to threat with stabilizer drugs and antipsychotics of choice. We discuss the psychopharmacological approach.
MethodsCase summary. We have conduced a systematic review of the descriptions published to date, regarding this case.We presented a case, in a 48-year-old female, admitted to our hospital due to psychopathological descompensation of bipolar affective disorder, where we observed manic and psychotic symtoms.
ResultsIn the first instance, we started treatment with Lithium and Olanzapine, in increasing doses, along with benzodiazepine support.
During more than four months of follow-up , multiple drugs have been tested sequentially: olanzapine, aripiprazole and quetiapine. We observed a good response but low tolerance issue to secondary effects consisting of severe akathisia, in progressive stiffness (spasticity) and hands tremor, it was very disabling problem for patient, even though the use of biperiden.
This situation forced us to search another option of treatment, different from non-pharmacological therapies (ECT). After checking the literature and publications about it, we decided to start treatment with Caripracine 3mg/24h, for which the therapeutic indication is the treatment of manic with mixed symtoms.
ConclusionsWe propose, through a clinical case, the use of cariprazine as a first choice in the acute decompensation of bipolar affective disorder, without symptoms of mixed mania.
During the treatment, the patient presente multiple difficulties and finally, a good response is was obtained with the use of Cariprazine, althought this patient continued showing slight akathisia well tolerated, she was able to leave after four months of hospitalization in the acude mental health unit.
Disclosure of InterestNone Declared
Does intensive home treatment change treatment trajectories of psychiatric disorders?
- A. Martín-Blanco, A. González-Fernández, A. Farré, S. Vieira, P. Alvaro, C. Isern, D. Giménez, C. Torres, V. de la Cruz, C. Martín, N. Moll, O. Castro, M. Sagué-Vilavella
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S167-S168
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Intensive home treatment (IHT) for people experiencing a mental health crisis has been progressively established in many western countries as an alternative to in-ward admission. But is this a real alternative? We previously reported that patients treated in our IHT unit only differ from those voluntarily admitted to hospital in suicidal risk and severe behaviour disorders (not in other factors such as clinical severity) (Martín-Blanco et al., Rev Psiquiatr Salud Ment 2022;15:213-5). Now we are interested in disentangle if those patients who used to require inward management can be successfully treated at home.
ObjectivesTo describe subsequent treatment trajectories of the first 1000 admissions to our IHT unit and to compare clinical characteristics among the different groups of trajectories.
MethodsRetrospective cohort study. Subsequent treatment trajectories were collected from December 2016 to October 2022 and classified: absence, hospital, IHT, and mixed (hospital and IHT). Statistical significance was tested by means of ANOVA or Kruskal-Wallis test for quantitative variables (corrected for multiple comparisons) and chi-square tests for qualitative variables.
ResultsTables 1 shows the characteristics of the whole sample. Of the 1000 IHT admissions, 12.1% needed subsequent hospital admission(s), 12.7% IHT admission(s), and 9.3% mixed admission(s). There were no differences among these groups in median severity at IHT admission, but there were differences in the number of previous admissions (p=0.0001): the group with no subsequent admissions had less previous admissions than the other groups (pBonf<0.0001), and the group with subsequent IHT admissions had less than the group with mixed admissions (pBonf=0.0123). There were differences between groups regarding distribution of diagnoses (p<0.0001) (Fig. 1). When considering subsequent admissions by diagnosis, there were differences in severity at IHT admission (p=0.0068) and in number of previous hospitalizations (p<0.0001) (Fig. 2).
Table 1. Clinical characteristics of the whole sample (N=1000) mean SD Age (years) 47.07 17.02 CGI-s at admission * 5 4-5 N % Sex (female) 548 54.8% Psychotic disorders 463 46.3% Affective disorder 257 25.7% Bipolar disorder 128 12.8% Other disorders 152 15.2% Hospital admission in the previous 5 years 313 31.3% CGI-s: clinical global impression - severity. * median and IQR
Image:
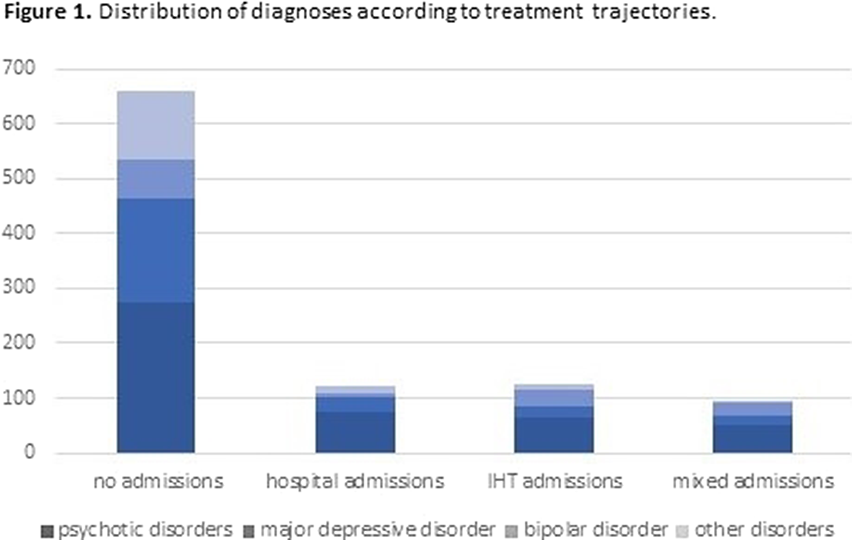
Image 2:
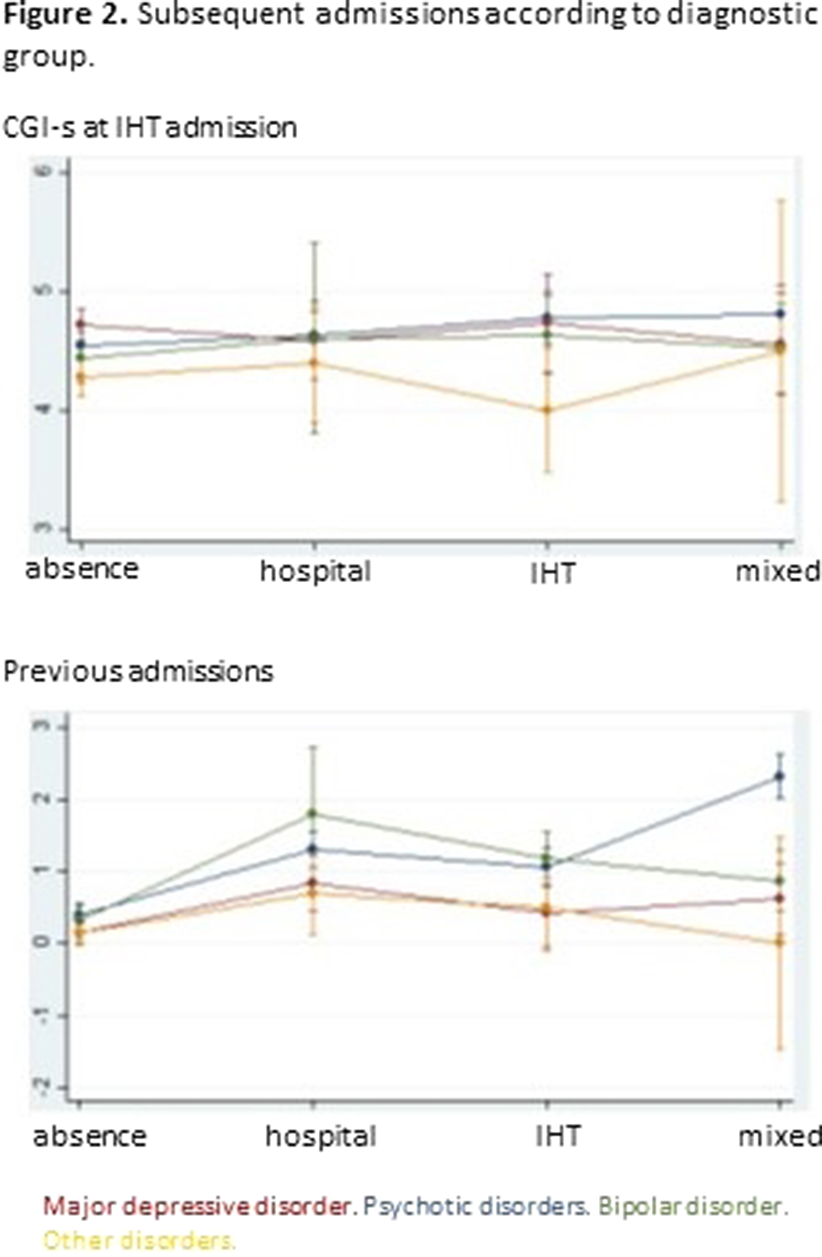 Conclusions
ConclusionsPatients that used to require inward management can now be treated at home when suffering an acute episode. Therefore, IHT has changed treatment trajectories for some patients with psychiatric disorders.
Disclosure of InterestNone Declared
Memory deficits in children and adolescents with psychotic disorders: A systematic review and meta-analysis
- E. Rodríguez Toscano, P. Díaz-Carracedo, P. de la Higuera-González, G. Padilla, A. de la Torre-Luque
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S332
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Cognitive symptoms in psychosis represent a major unmet clinical need (Acuna-Vargas et al. Cog in Psych 2019; 21(3), 223–224). Deficit in memory has been largely described in first episode early onset psychosis (Mayoral et al. Eur Psych 2008; 23(5), 375-383) and has been associated to a worse functionality (Øie et al. Neuropsychology 2011; 25(1), 25–35). However, results from existing studies are quite mixed on memory deficits of early psychosis patients, particularly in terms of memory contents and storage resources.
ObjectivesThe aims of this study were 1) to examine the nature and extent of cognitive impairment in early-onset psychosis and 2) to analyze which type of memory (verbal and visual) is more affected in the disorder.
MethodsThe present systematic review and meta-analysis was conducted according to the PRISMA criteria (Moher et al. Systematic Reviews 2015; 4(1), 1 - 9). A systematic search of CINAHL, PsycInfo, PubMed, Redalyc, SCOPUS and Web of Science (published from 2000 to 2020) identified case-control studies of early onset psychotic disorder (under 18 years old). Those studies focused on both verbal and visual memory performance.
ResultsTwenty articles were included in the review. A deficit in memory in child and adolescent psychotic disorders was obtained displaying a large effect size in memory tasks (g = -0.83). Also, a medium effect size was found in visual memory tasks (g = - 0.61) and a large effect size was found in verbal memory tasks (g = -1.00).
ConclusionsIt was observed a strong memory deficit on early psychotic disorders already present at the onset of the illness. This deficit was stronger when verbal memory tasks were used compared to the effect found with visual memory tasks. Based on previous literature (García-Nieto et al. Jou Cli Child & Ado Psych 2011; 40(2), 266-280; Lepage et al. Eur Psych 2008; 23(5):368- 74; Hui et al. Psych Med 2016; 46(11):2435-44), these results contribute to describe and characterize the cognitive symptoms in the first-episode psychosis in a youth population.
Disclosure of InterestNone Declared
Gastric bezoar in a patient hospitalized in an eating disorder unit. Case report
- J. Torres Cortés, I. Esteban Avendaño, J. B. González del Valle, R. González Lucas, J. J. Padín Calo, J. P. Morillo González
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S850-S851
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
It is well known that eating disorders are related to comorbidity. At least, half of these patients have other mental disorders and, in addition to it, the presence of physical comorbidity (cardiovascular, kidney, nervous system, digestive tract, metabolic or endocrine disorders) comes with a decline in life expectancy.
ObjectivesDescription of a patient with a diagnosis of anorexia nervosa (AN) who developed a gastric bezoar during hospitalization.
MethodsCase treated in a specific Eating Disorder Unit in a Third-Level Hospital.
Results26 years old woman with a diagnosis of AN hospitalized in General Psychiatric Unit with BMI of 11,78 kg/m2. Nasogastric tube was necessary and, after 1 month with a progressive weight recovery (BMI 13,84 kg/m2), the patient was transferred to the Eating Disorder Unit in order to follow specific psychological therapy. No incidence related to physical exploration or clinical analyses happened during this month apart from pancytopenia due to malnutrition.
However, 8 days after, patient developed nausea and had 3 vomit episodes, constant abdominal pain at hipogastrium (moderate intensity), dizziness, instability and constipation. The patient refused possibility of pregnancy. The physical exam showed bowel sounds augmented but no mass or peritoneal irritation appeared. Blood test results were normal. Abdominal X-Ray showed gastric dilatation with small bowel faeces sign, which suggested diagnosis of gastric bezoar.
The treatment was the dissolution of the bezoar by Coca-Cola, solving the symptoms completely.
The patient refused having eaten hair or any other kind of object or indigestible material but admitted to be following a strict vegan diet. Finally, after an endoscopy was done, the patient was diagnosed of phytobezoar.
ConclusionsBased on literature, bezoars are rare in AN, being phytobezoars the most common between the types of bezoars. Nevertheless, there are some risk factors, such as delayed gastric emptying, dehydration or, in the case of phytobezoar, ingestion of food containing high amount of cellulose, hemi-cellulose, lignin, and tannins (celery, pumpkin, grape skins, prunes, raisins and, in particular, persimmons). Some of the symptoms caused by phytobezoar can be similar to those of the AN (abdominal pain, intestinal obstruction, poor appetite, vomiting, malnutrition, weight loss). Therefore, gastric bezoar could be an underdiagnosed or even undiagnosed disease in this group of patients. Taking this into account could reduce time until diagnosis and treatment, decreasing the risks associated.
Disclosure of InterestNone Declared
Healthy mental higher education students’: Presentation of a project
- A. Torres, J. Costa, P. Carvalho, M. Loureiro
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S985-S986
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The prevalence of mental disorders in Higher Education Students (HES) is high and has shown a worrying growth. However, only a small percentage of HES in need of psychological support request it, due to the stigma related to mental illness, requesting informal help from friends and family. Training and increasing Mental Health Literacy (MHL) have been stated as appropriate strategies to reduce stigma and increase the demand for professional psychological support. However, with the increase in the demand for help, the difficulty of providing an adequate response from psychological support of HE services also increases. Therefore, procedures that develop socio-emotional skills in the HES and strategies that enhance the responsiveness of these services are necessary.
ObjectivesTaking in consideration the literature review in this field, we develop a project to improve the mental health of HES. The project objectives’: a) the reduction of stigma related to mental disorders through the promotion of MHL in the academic community; b) the promotion of mental health and socio-emotional skills of HES; c) increasing detection and active search for professional mental health support, and d) the implementation of psychological intervention based on a stepped care model that provides an adequate response to most of the students’ mental health needs, according to individual needs.
MethodsThe project proposes to perform the following methods: a) training in mental health open to the academic community, which will aim to train volunteers to be Gatekeepers, in order to promote awareness, detection and referral of students in need of professional psychological support; b) implementation of a Student Observatory, with tracking of psychopathological symptoms, supported on the Web; c) implementation of a psychological intervention program based on a stepped care model, which will include the following progressive phases by severity: 1) digital self-help manual; 2) web-based self-help groups; 3) psychological intervention groups supported by the Web; 4) face-to-face intervention groups and 5) individual psychological intervention.
Students will be assessed before and after each step of care, with the following psychological instruments: Mental Health Inventory (MHI); Patient Health Questionnaire (PHQ-9) and Generalized Anxiety Disorder (GAD-7).
ResultsThe implementation of the presented methods expect to achieve improvements on HES’ mental health, namely improvement of MHI, reduction of PHQ-9 and GAD-7 after each step of the psychological care.
ConclusionsThe project presented encloses evidence-based interventions, with inspiration on psychoeducation and cognitive behavioral approaches, and it is expected to contribute to the improvement of mental health of HES. The results will be collected and disseminated. We encourage other researcher and clinicians to perform studies about the mental health of HES.
Disclosure of InterestNone Declared
Antiandrogenic treatment of obsessive compulsive neurosis: A case review
- L. Huerga García, I. Careno Baez, G. Oropeza Hernández, A. Marcos Rodrigo, C. Delgado Torres, G. Garriga Rocío, P. Gómez Pérez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S927
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Obsessive-compulsive disorder (OCD) is a mental disorder in which patients who suffer from it have repetitive and undesirable thoughts, feelings, ideas, sensations (obsessions) and behaviors that drive them to do something over and over again (compulsions).
Often the person tries to get rid of the obsessive thoughts through compulsions, but this only provides short-term relief. Not carrying out the obsessive rituals can cause enormous anxiety and suffering.
ObjectivesTo describe a 23-year-old male patient, who suffers from anxiety and mood symptoms, reacts to ego-dystonic obsessive ideas and sexual content, of months of evolution, and who manages to calm down through compulsive masturbation or watching sexual videos on the internet. All this clinic negatively interferes with their quality of life, asking the patient for medical help to calm these ideas.
MethodsWe carried out a review in Pubmed with the terms Antiandrogens and TOC, in order to make a better description of the clinical case.
ResultsAfter several treatment attempts (Sertraline, Paroxetine, Clomipramine, Clomipramine + SSRI), reaching maximum doses according to clinical guidelines, and with poor therapeutic response, it was decided to discuss the case with the endocrinology department of our hospital, deciding to start treatment with antiandrogens, in order to alleviate the persistent intrusive ideas of a sexual nature. The administration of antiandrogens in men can cause a decrease or increase in the development or involution of secondary sexual characteristics in men, reducing the activity or function of accessory sexual organs, and hyposexuality, with decreased sexual desire or libido.
After several weeks, there was improvement in the obsessive symptoms with a decrease in compulsive rituals. However, after the 3rd mo, some symptoms reappeared, but not with the same severity and intensity as before treatment. In addition, we cannot ignore the adverse effects that have occurred, such as involution of secondary sexual characteristics. However, and taking into account the negative repercussion that this clinic had on the patient’s quality of life, the benefit obtained exceeded the risk, having noted clear improvement with this therapy, and maintaining evolutionary controls by both psychiatry and endocrinology.
ConclusionsPatients suffering from obsessive-compulsive disorder can be effectively treated with anti-androgenic pharmacological agents with various modes of action. The most effective group of such agents is the long-acting analogues of the gonadotropin-releasing hormone. The objective of this review is to elucidate the possibility of using such powerful anti-androgenic agents in the treatment of obsessive-compulsive disorder.
Disclosure of InterestNone Declared
Comorbid Obsessive-Compulsive Symptoms in Schizophrenia - Diagnostic and Treatment Challenges
- J. A. Leal, J. C. Moura, T. C. Rocha, J. F. Cunha, S. P. Torres, D. Seabra, I. M. Lopes, M. E. Carneiro, S. M. Esteves, R. Cajão, G. Lima
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1061
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The comorbidity between Schizophrenia and Obsessive-Compulsive Symptoms represents almost 25% of schizophrenic patients and it is believed that almost 12% match the diagnostic criteria for Obsessive-Compulsive Disorder. Some second-generation antipsychotics may worsen or even induce those symptoms, which makes the treatment of this patients a difficult challenge.
ObjectivesTo assess the link between Schizophrenia and Obsessive-Compulsive Symptoms, to discuss the diagnostic challenges and treatment options. To present a clinical case report of a schizophrenic patient with Obsessive-Compulsive Symptoms, which improved with proper treatment.
MethodsWe performed a non-systematic review of the existent literature with the keywords “Schizophrenia” and “Obsessive-Compulsive Symptoms”. Description of a clinical case report.
ResultsWe present the case report of a male, 21 years old, single, diagnosed with Schizophrenia. In the past year, he was admitted twice in a psychiatric ward for persecutory and mystic delusions, which lead him to erratic behaviour. Since his adolescence he manifested repeated washing and compulsive cleaning associated with the fear of being contaminated with multiple diseases. Those compulsions worsened when he started being treated with antipsychotics. However, with therapeutic adjustments and with the introduction of an antidepressant we were able to control those symptoms.
ConclusionsSome antipsychotics may induce or even aggravate Obsessive-Compulsive Symptoms in psychotic patients. It is of extreme relevance to differentiate those symptoms as comorbid in Schizophrenia or if they existed prior to the first positive symptoms, since they can be representative of an Obsessive-Compulsive Disorder. Understanding this diagnostic and treatment complexity enables us to be more familiar with the development of Obsessive-Compulsive Symptoms in schizophrenic patients.
Disclosure of InterestNone Declared
Catatonia in a case of major depression resistant to pharmacotherapy. A case report
- C. M. Gil Sánchez, P. Casado de la Torre, M. V. Taillefer Aguanell
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S827
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Catatonia is a clinical syndrome characterized by behavioral alterations, which may include motor immobility or excitation. As a symptom, catatonia may be present in several mental disorders, primarily schizophrenia and mood disorders. Symptoms can be severe and can lead to dangerous and lethal conditions if not diagnosed and treated properly.
ObjectivesTo describe the complicated evolution of a case of major depression with psychotic symptoms, which developed catatonic status. We discuss the psychopharmacological approach and non-pharmacological therapies (ECT).
MethodsCase summary. We have conducted a systematic review of the descriptions published to date, regarding this case.
ResultsWe present a case of extreme severity, in a 55-year-old male, with a broad differential diagnosis with organic pathology, which required multidisciplinary management in conjunction with other specialties and multiple complementary tests.
Eventually diagnosed with major depression with psychotic symptoms evolving into a catatonic state. During more than one year of follow-up, multiple drugs have been tested sequentially: SSRI antidepressants, dual action, low-dose antipsychotics (caripracin, lurasidone, aripiprazole, olanzapine).
Finally, a good response was obtained in the treatment with lorazepam 1mg /6h and 12 sessions of ECT administered concomitantly.
In this case, the patient presented a refusal to eat and weight loss with a BMI of malnutrition. We had to be coordinated with the endocrinology service for a nutritional restitution strategy through dietary supplements. Once nutritional restitution was achieved, we started treatment with clomipramine, with good results on affective symptoms.
ConclusionsNowadays, the origin and treatment of catatonia are still unclear.
We present the case of a man with melancholic depression with psychotic symptoms, who evolved into a catatonic syndrome. A good response was achieved with the combination of ECT and benzodiazepines.
We want to highlight nutritional recovery as an important point to achieve good absorption of antidepressant drugs. Once achieved, we started treatment with clomipramine with good results.
During the treatment, he has presented multiple difficulties and finally, he was able to leave after five months of hospitalization in the acute mental health unit.
Disclosure of InterestNone Declared
Psychiatric comorbidity profiles among suicidal attempters: A cohort study
- Y. Sanchez-Carro, M. Diaz-Marsa, V. Fernandez-Rodrigues, W. Ayad-Ahmed, A. Pemau, I. Perez-Diaz, A. Galvez-Merlin, P. de la Higuera-Gonzalez, V. Perez-Sola, P. Saiz, I. Grande, A. Cebria, J. Andreo-Jover, P. Lopez-Peña, M. Ruiz-Veguilla, A. de la Torre-Luque
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S318-S319
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
More than 700,000 people die by suicide in 2019 globally (World Health Organitation 2021). Mental health problems constitute a risk factor for suicidal behavior and death by suicide (Hoertel et al. Mol Psychiatry 2015; 20 718–726). Different mental disorders have been related to different forms of suicidal ideation and behavior (Conejero et al. Curr Psychiatry Rep 2018; 20, 33) (Quevedo et al. Compr Psychiatry 2020; 102 152194). However, little is known on comorbidity profiles among suicide attempters.
ObjectivesThe aim of our work was to identify the psychiatric comorbidity profiles of individuals who were admitted a hospital emergency department due to a suicide attempt. Moreover, it intended to know their clinical characteristics according to comorbidity profile.
MethodsA sample of 683 attempters (71.30% female; M age= 40.85, SD= 15.48) from the SURVIVE study was used. Patients were assessed within the 15 days after emergency department admission. Sociodemographic (i.e., sex, age, marital status and employment status) and clinical data were collected. The International Neuropsychiatric Interview (MINI) was used to assess DSM-V Axis 1 mental health diagnoses and the Columbia Suicide Rating Scale (C-SSRS) to assess suicidal ideation and behavior. The Acquired Capacity for Suicide-Fear of Death Scale (ACSS-FAD), the Patient Health Questionnaire (PHQ-9) to assess the frequency of depressive symptoms during the past 2 weeks, and the General Anxiety Disorder-7 (GAD-7) scale to assess symptoms of worry and anxiety were also conducted. For the identification of comorbidity profiles, latent class analysis framework was followed considering diagnosis to each individual disorder as clustering variables. On the other hand, binary logistic regression was used to study the relationship between comorbidity profile membership and clinical factors.
ResultsTwo classes were found (Class I= mild symptomatology class, mainly featured by emotional disorder endorsement; and Class II= high comorbidity class, featured by a wide amount of endorsed diagnoses) (see figure 1). Individuals from the High comorbidity class were more likely to be female (OR= 0.98, p<.05), younger in age (OR= 0.52, p< .01), with more depressive symptoms (OR=1.09, p<.001) and have greater impulsivity (OR= 1.01, p<.05).
Image:
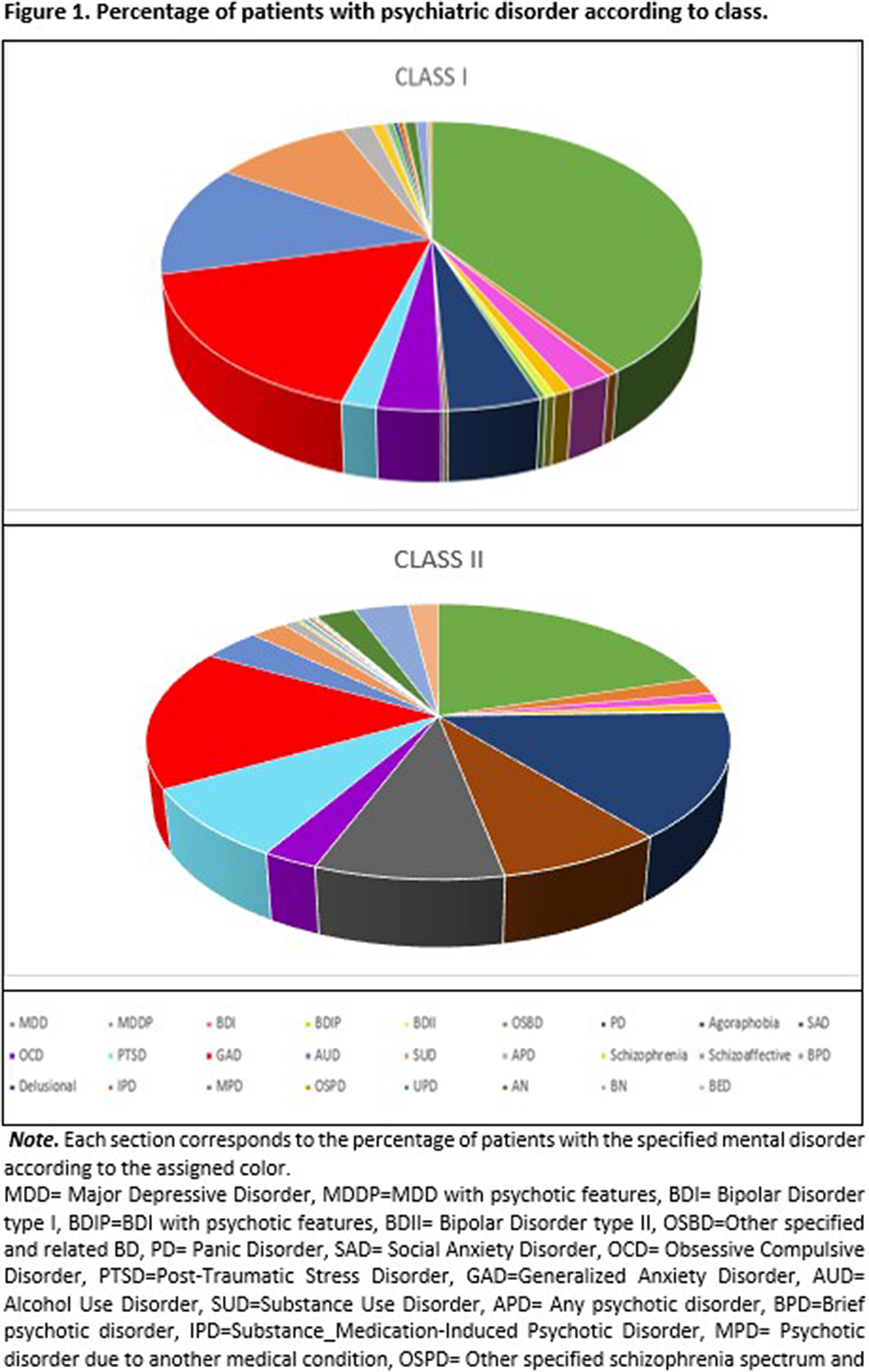 Conclusions
ConclusionsWe found two profiles of people with suicidal behavior based on the presence of mental disorders. Each of the suicidal subtypes had different associated risk factors. They also had a different profile of suicidal behavior.
Disclosure of InterestNone Declared
Possible psychotic episode after repeated ayahuasca intake: a case report
- E. Prades Marin, A. Martínez Torres, P. Sánchez Díez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S753
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Ayahuasca is a traditional brew containing the psychedelic 5-DMT (a tryptamine that acts as a 5HT2A-R agonist) used to achieve non-ordinary states of consciousness, with a long tradition among various cultures in ritual and therapeutic contexts. Ayahuasca is being studied as potential treatment in Mental Health, which has led to non-controlled and recreational use. This has led to a rise in the description of side effects, such as substance-induced psychosis.
ObjectivesTo describe a case of a possible psychotic episode related to the intake of ayahuasca brew in a ritual context.
MethodsClinical assesment and bibliographic review of pertinent literature.
ResultsWe will present the case of a 43 year old woman, who participated in three ayahuasca sessions in three consecutive months. Two days after the last session, she suffered and episode of loss of consciousness, convulsions, loss of streng and paraesthesia in right forearm and righr side of the face and head; and apparition of perceptual alterations and delusions that she did not experience during the trip. Such alterations included the perception of electromagnetic fields (EMF) robbing her of her vital energy and lifeforce. She required ICU treatment for four days, after which se was hospitalized in Internal Medicine Unit and was assessed by Mental Health team. Though the symptoms were coherent with the previous beliefs of the patient, they were clearly exacerbated and interfered with her normal and previous functioning. She was treated with risperidone 1,5 mg, with complete symptom remission.
ConclusionsThe case presented is consistent with other reports of ayahuasca-induced psychotic symptoms, though with less intensity and duration. We discuss prevalence and repercussions of the rising use of this powerful substance; that must be taken into consideration by clinicians worldwide.
Disclosure of InterestNone Declared
Psychopathological symptoms as clinical phenotypes in suicide attempters: relation in terms of suicidal ideation, suicidal related behaviors and medical damage of the attempt
- D. Saiz-Gonzalez, P. Diaz-Carracedo, A. Pemau, W. Ayad-Ahmed, F.-R. Veronica, M. Navas Tejedor, A. de la Torre-Luque, M. Diaz-Marsa
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S560-S561
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Suicide behaviour is a complex and multifactor concept that includes different risk factors. According with literature a dimensional concept of illness could help to understand this complexity and clarify clinical aspects of suicide risk.
ObjectivesThe aim of this study is to identify different profiles of symptoms in a sample of suicide attempters and the relationship between this profiles and suicide behaviour in terms of outcome: presence and intensity of suicidal ideation, presence and number of attempts and severity of the medical damage in the current attempt.
Methods634 patients were recruited at the psychiatry emergency of eight public general hospitals in Spain between November 2020 until February 2022 in the SURVIVE protocol. The patients were assessed in 15 days using a battery of clinical tools that includes Brief Symptom Inventory, a sociodemographic interview, Mini Clinical Interview and C-SSRS, ACSS and BIS-11 scales. Latent profile analysis was applied to obtain profile symptoms. Logistic and multivariant regression was used to obtain data about outcome.
ResultsThree clinical profiles of psychiatric symptoms were described in suicide attempters (p < 0.01): high symptoms (HS) (45.02%), moderate symptoms (MS) (42.5 %) and low symptoms (LS) (12.48%). Significant differences were found between classes in four symptom domains (Figure 1): anxiety, obsessive-compulsive, sensitivity, and somatization (p < 0.01). Participants of the HS class showed higher values in relation with the BSI summary indexes, and more diagnoses, higher levels of suicidal ideation and suicidal related behaviour as well as higher acquired capability for suicide. Participants of the LS class were more likely to be women, older and unemployed and was related, according the analysis, with severe medical damage when compared with other groups (P< 0.01).
Image:
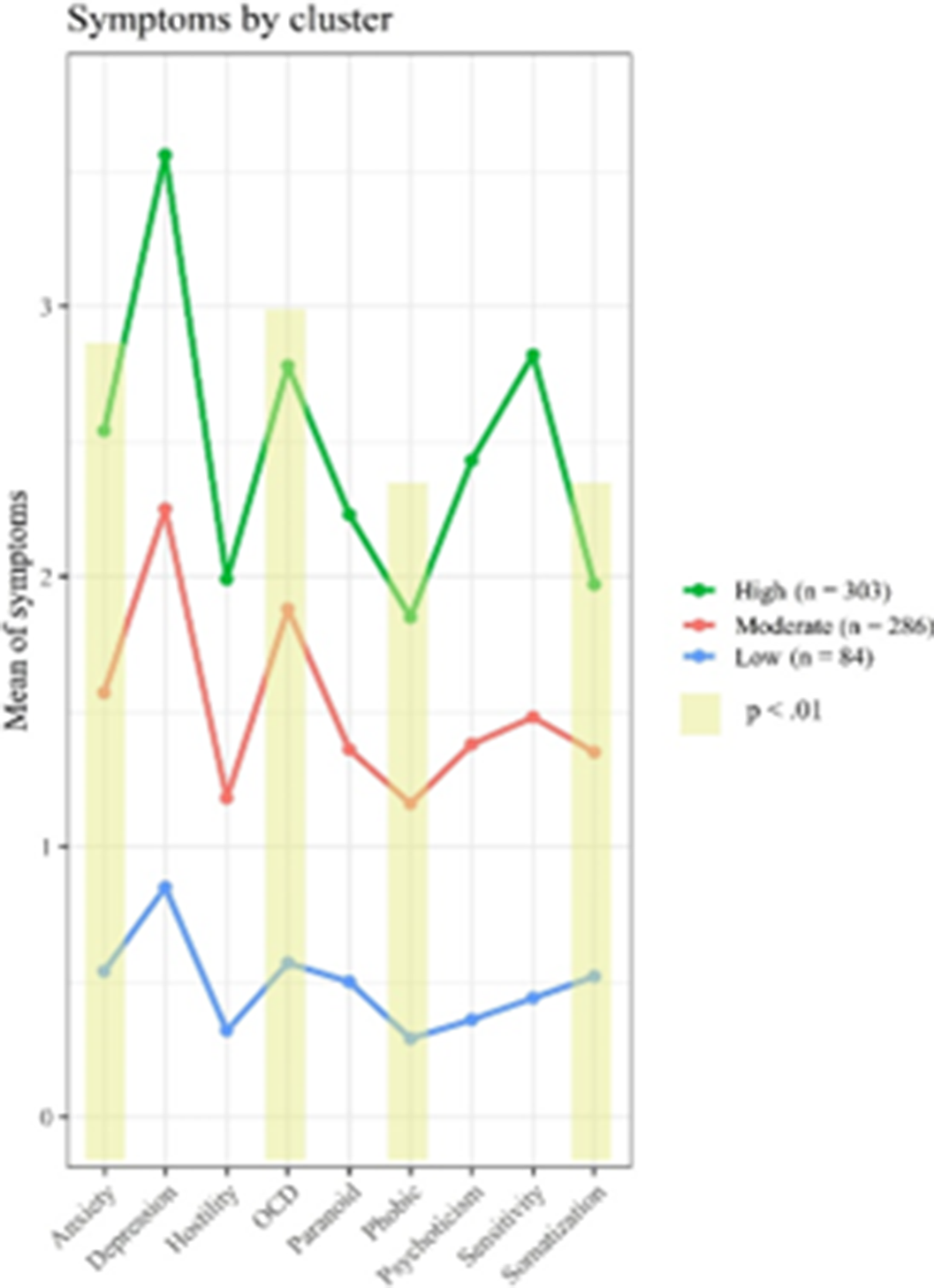 Conclusions
ConclusionsAccording with the predictive model the study suggests different symptom-frequency clusters related with suicide attempt outcomes. Suicide ideation presence and intensity is related with HS class and acquired capability of suicide. Suicide ideation intensity is also related with number of diagnosis and number of previous attempts. Suicide behaviours presence is associated with being student and number with HS profile. Both presence and number were related with number of diagnosis as well as number of previous attempts (the higher all these clinical factors, the more intense of ideation in the last month). Finally, the severity of medical damage was related with LS profile and unemployed/retired work status. The dimensional symptom profile could be useful to predict suicide attempt outcome. Further study is needed to clarify this relation.
Disclosure of InterestNone Declared
Study of mentalizing ability in borderline personality disorder: relationship with impulsivity
- A. Galvez-Merlin, P. de la Higuera-Gonzalez, J. M. Lopez-Villatoro, A. de la Torre-Luque, M. Diaz-Marsa, J. L. Carrasco
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S114
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Borderline personality disorder (BPD) is a severe mental disorder characterized by affective, behavioral and relational instability, along with interpersonal hypersensitivity and unstable affective relationships (APA 2013). Poor interpersonal functioning could be associated with critical deficits in the ability to mentalize in these patients, together with high levels of impulsivity. Although most studies have described hypermentalization deficits among BPD patients (Bora Psychol Med 2021;51 2541-2551), existing literature is still scarce on this aspect, as well as its relationship with the impulsive behavior.
Objectives1) to assess specific mentalizing deficits in BPD compared to healthy controls in a complex ecological mentalization task; 2) evaluate the relationship between mentalization and impulsivity in BPD.
Methods63 patients diagnosed with borderline personality disorder and 31 control subjects were studied using the Movie for the Assessment of Social Cognition -MASC- (Dziobeck et al. J Autism Dev Disord 2006; 36 623-636) and the Barratt Impulsivity Scale -BIS-11- (Patton et al. J Clin Psychol 1995; 51 768-774), as well as other sociodemographic and clinical factors. The clinical research study was approved by the Clinical Research Ethics Committee of the Hospital Clínico San Carlos (Madrid, Spain).
ResultsThe results showed significant differences in the scores related to correct mentalization, hypomentalization, and non-mentalizing responses between patients and controls, with BPD patients showing worse performance. A significant negative relationship was also observed between impulsivity scores and correct mentalizing responses in BPD patients.
ConclusionsThe results showed a deficit in the ability to mentalize in BPD patients, compared to control subjects, characterized by a hypomentalization and an absence of mentalization. Likewise, this deficit in mentalization ability was related to greater impulsive behavior in patients. These results would be consistent with the hyperarousal hypothesis in BPD, which would reduce inhibitory control, causing mentalization deficits (Euler et al. J Pers Disord. 2021; 35 177-193). Future studies will try to associate specific impulsive behaviors associated with the characteristics of hypomentalization and absence of mentalization observed in our results.
Disclosure of InterestNone Declared
Assessment of Theory of Mind in Psychopathology: a Scoping Review
- P. de la Higuera-Gonzalez, A. Galvez-Merlin, E. Rodríguez-Toscano, J. Andreo-Jover, T. Lopez-Soto, A. de la Torre-Luque
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1001-S1002
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Theory of Mind (ToM) is defined as the cognitive ability that infers other’s mental states (Premack & Woodruff. J Behav Brain Sci 1978; 1 515-526).The interest in the study of ToM distinguishing its affective and cognitive components has been growing. Its study in psychopathology has been evolved from its original studies in autism spectrum disorders (ASD), schizophrenia (SCZ) and, borderline personality disorder (BPD), to other mental disorders like major depressive disorder (MDD), bipolar disorder (BP), anorexia nervosa (AN) and social anxiety disorder (SAD).
Objectives1) review the most commonly used instruments for ToM assessment; 2) to compile the evidence on ToM deficits across mental disorders. For both objectives, target disorders are previously mentioned.
MethodsThe search was carried out on the PubMed, PsycInfo and Scopus databases, using the terms “Theory of mind”, “Mentalization” and the previously mentioned mental disorders and pertinent thesaurus. Articles in English, published since 2010 were considered. A 2-step strategy (first, article screening and full reading) was followed to select articles of interest.
ResultsReading the Mind in the Eyes (Baron-Cohen et al., J Child Psychol Psychiatry 2001; 42 241-251) and Movie for the Assessment of Social Cognition (Dziobeck et al. J Autism Dev Disord 2006; 36 623-636) were the most commonly used tasks to assess ToM. Regarding mental disorders, studies showed deficits in cognitive and affective ToM skills in ASD, SCZ, BPD, MDD and BP. Hypomentalization was mainly observed in ASD and MDD, while BPD and SCZ were featured by errors associated with hypermentalization. Studies in AN and SAD are scarce, but they mainly highlight a cognitive ToM deficit, with hypomentalization in AN and hypermentalization in ASD. In all of them, depressive symptomatology seems to be a critical moderator of ToM performance.
ConclusionsAlthough ToM impairments are well described for some mental disorders, more research is needed to reach solid conclusions for others. The use of different and heterogeneous ToM assessment instruments can strongly influence the results of studies. The study of ToM is essential to gain a better understanding of the diseases and to develop effective treatments targeting specific ToM deficits.
Disclosure of InterestNone Declared
Assessment of unconsciousness during carbon dioxide stunning in pigs
- P Rodríguez, A Dalmau, JL Ruiz-de-la-Torre, X Manteca, EW Jensen, B Rodríguez, H Litvan, A Velarde
-
- Journal:
- Animal Welfare / Volume 17 / Issue 4 / November 2008
- Published online by Cambridge University Press:
- 11 January 2023, pp. 341-349
-
- Article
- Export citation
-
The aim of this study was to assess unconsciousness in pigs during exposure to CO2 through changes in the middle latency auditory evoke potentials (MLAEP) of the central nervous system (CNS), blood parameters (pH, carbon dioxide partial pressure [pCO2], oxygen partial pressure [pO2], oxygen saturation [SatO2] and bicarbonate [HCO−3]), behaviour and the corneal reflex. The MLEAP did not decrease significantly until after 60 s exposure to CO2. The blood parameters (decreased pH, pO2 and SatO2 and increased pCO2 and HCO3) changed 53 s after the onset of immersion. The burst suppression index (BS%) and the A-line ARX index (AAI) from the MLEAP recovered basal levels at 136 and 249 s, respectively. The first blood parameter to return to basal levels was HCO−3 at 76 s of exposure, followed by SatO2 at 180 s, pH and pO2 at 210 s and pCO2 at 240 s. During exposure to the gas, pigs exhibited lateral head movements and sneezing (10.3 s), gasping (23.5 s) and vocalisation (26.1 s). Furthermore, all pigs demonstrated muscular excitation after between 19 and 39 s exposure, when the AAI and BS% values were not significantly different from basal values. It was suggested, therefore, that these excitatory movements represent conscious movement, indicative of aversion to the gas. According to our results, loss of consciousness began, on average, after 60 s inhalation of 90% CO2. During exposure to the gas, decreased brain activity was seen, immediately following the changes in blood parameters. Following exposure, the restoration of blood parameters to basal levels allows a return to normal brain activity.







