36741 results in European Psychiatry & past titles
Diphenhydramine-induced delirium on top of HIV-associated neurocognitive disorder
- R. T. E. Sollano
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S399
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
HIV-associated neurocognitive disorder has been less frequent in recent years due to the availability of anti-retrovials. However, in the Philippines, persons with HIV are diagnosed late resulting to cases of HIV-associated neurocognitive disorder. With higher incidence of depression and anxiety in this population, difficulty sleeping becomes a prominent symptom and diphenhydramine is a common non-prescription nighttime sleep aid being given.
ObjectivesTo present a case of diphenhydramine-induced delirium after a patient with HIV-associated neurocognitive disorder.
MethodsThis a case report.
ResultsMr. JR., a 38-year-old person living with HIV and no past psychiatric history, presents with acute onset altered mental status, suicidal attempt, and jerking movements of the neck and extremities. He has been having bouts of diarrhea, fatigue, weight loss, and forgetfulness for a year before he was diagnosed with HIV-AIDS with CD4 count of 59 cells/mm3. At this time, he already had blurring of vision, poor sleep, weakness, poor concentration, and increasing severity of forgetfulness. He also started to have depressed mood and anhedonia but no suicidal ideations. He was eventually started on antiretroviral (ARVs) which are lamivudine, tenofovir, dolutegravir and antibiotics targeting opportunistic bacteria – Isoniazid, Moxifloxacin and Clindamycin. A few days after, he started to have jerking movements of the neck and extremities contributing further to poor sleep. Upon consult with a local clinic to address his sleep, he was prescribed with Diphenhydramine and after taking 50mg dose that evening, he started to have disorientation, paranoia, command auditory hallucinations resulting to a suicidal attempt, on top of the jerking movements, which prompted consult to the emergency room and subsequent admission. Initially assessed as central nervous system infection and focal seizure, CSF fluids studies and EEG were done showing normal findings. Started on Sodium Valproate + Valproic acid 500mg IV twice daily and Olanzapine 2.5mg twice a day, on top of his previously mentioned ARVs and antibiotics, the disorientation, auditory hallucinations, and myoclonic jerks mood resolved after five days. Five months on ARVs, he has no recurrence of myoclonic jerks, disorientation or psychosis, with memory and concentration improved, euthymic mood, and was able to resume work as an engineer.
ConclusionsDiphenhydramine is a common nighttime sleep aid. Due to its anticholinergic effect, cases of delirium were reported for doses 300mg to 1,000mg per day. For Mr. JR, the mere 50mg dose of diphenhydramine caused disorientation and psychosis as his co-occurring HIV-associated neurocognitive disorder made his brain “delirium-ready”. Diphenhydramine is a relatively safe drug however not getting a thorough medical history may inadvertently cause harm to patients who are medically ill and frail.
Disclosure of InterestNone Declared
Sex differences for antipsychotic dosing and how to guide therapy
- G. Schoretsanitis
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S31
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Abstract
Over the past decades the role of sex in the antipsychotic treatment type and dose selection has been virtually overseen. In fact, medication approval trials barely stratify for sex differences. Emerging hints from different types of data highlight the need for antipsychotic treatment personalization within the context of sex differences. Varying bioavaibility patterns of the prescribed antipsychotics between female and male patients may be easy to capture measuring plasma or serum levels of the antipsychotics ultimately guiding dose selection in clinical routine. Here we will discuss pitfalls and current evidence regarding sex affecting dose selection to enhance safety and effectiveness outcomes of antipsychotic treatment.
Disclosure of InterestG. Schoretsanitis Consultant of: HLS Therapeutics and ThermoFisher
Effects of intrahipocampal nmda on re-extinction of an aversive emotional memory task in rats
- E. P. Ruiz Gonzalez, D. M. Gómez Ordoñez, L. F. Cárdenas, M. N. Muñoz Argel
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S613
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
N-Methyl-D-aspartate (NMDA) receptors are involved in learning and memory. It is known that ventral hippocampus is a crucial structure involved in emotional memory formation mainly for fear and anxiety situations. The aim of this research is to identify the effect of the stimulation of ventral hipocampal NMDA receptors on the reextinction of an aversive emotional memory task. NMDA (0.2 ug/μl; 0.2 μl) or saline (0.9 %; 0.2 μl) was bilateral and locally administered in the ventral hippocampus of male Wistar rats, before the re-instatement trial.
The experimental group consisted of 10 animals and the control group by 9 subjects. The results suggest that the activation of ventral hipocampal NMDA receptors induces an increase in the time needed to re-extinguish the conditioned fear, suggesting a possible potentiating effect on re-installation.
ObjectivesTo evaluate the effect of NMDA at the intrahippocampal level, on the reinstatement and re extinction of a conditioned fear response in male Wistar rats.
MethodsThis study is experimental, where two groups of adult male Wistar rats were used. The bilateral cannulas was implanted, the animals were injected intraperitoneally with a mixture of ketamine (Rotexmédica) and xylacin (Bayer; 75 mg/Kg and 5 mg/Kg), respectively, then the animals were placed in a stereotaxic apparatus (Narishige) and injected with veterinary antibiotic.The (21G) caliber cannulas were bilaterally implanted in HPv at the following coordinates: AP = -5.2 mm relative to Bregma; ML = ± 5 mm in relation to the midline and DV = 5.1 mm in relation to the skull and according to the atlas (Paxinos & Watson, 1985).
ResultsIt was observed that in the first phase of extinction there were no statistically significant differences between the two groups, experimental and control, as in the second phase of extinction. The results obtained for the re-extinction phase 1 and 2 showed that there were significant statistical differences between the groups. This difference was only evident in the first three minutes in the two phases of re-extinction.
Image 2:
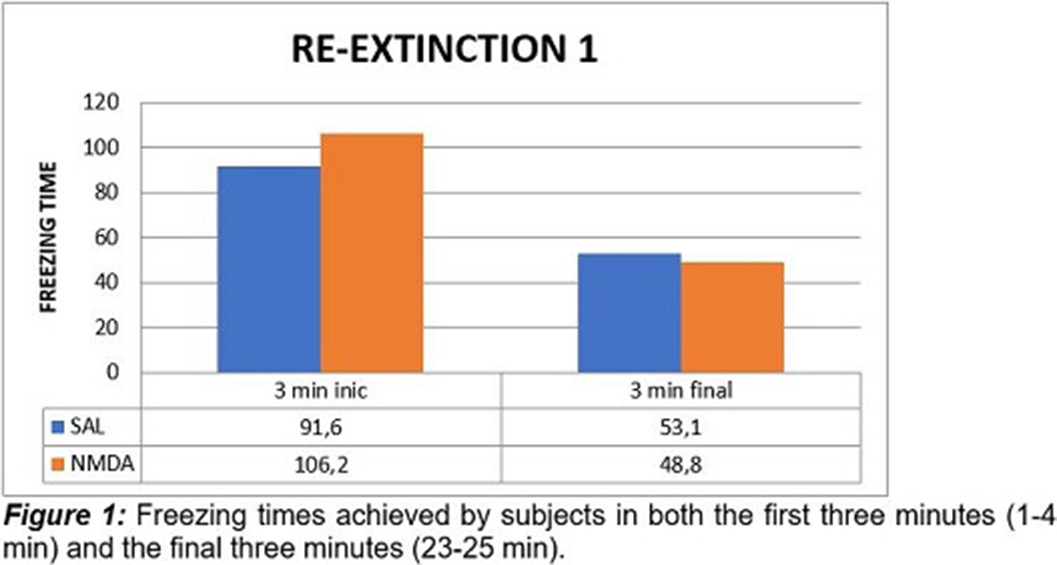
Image 3:
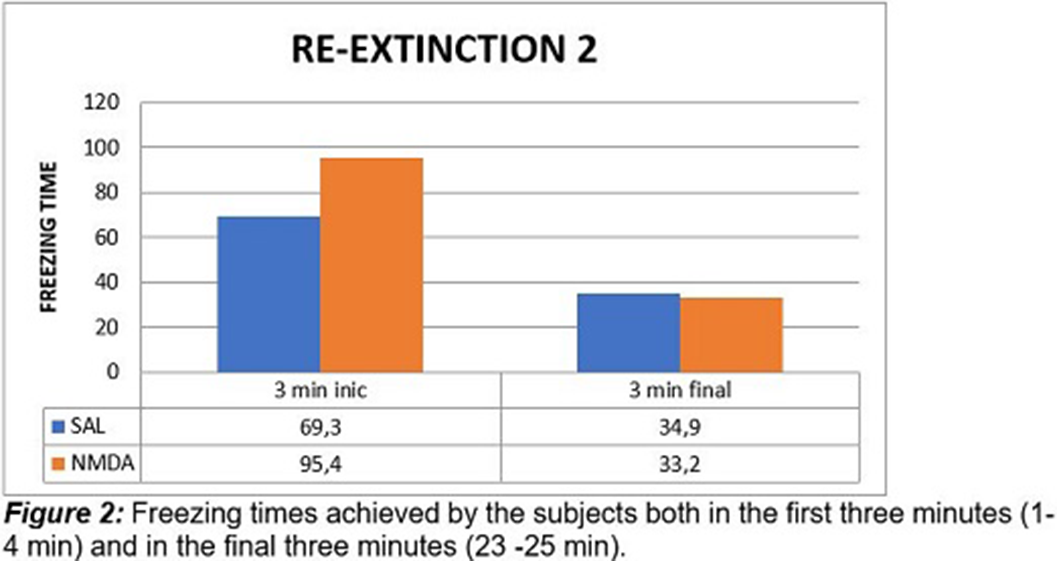 Conclusions
ConclusionsStatistically significant differences were observed between the two groups, in the phases of re-extinction, seeing a longer time of the freezing response in the experimental group, as an effect of the application of NMDA in the ventral hippocampus (HPv), which suggests that this substance has a memory-enhancing effect, and therefore contributes to increasing the permanence of the fear response. It should be noted that this difference was only evident in the first three minutes in the two re-extinction phases. These results may be related to other studies where it has been shown that LTP is dependent on the N-methyl-D-aspartate receptor in the CA1 region in vivo (Zhong, Cherry, Bies, Florence, & Gerges, 2009)
Disclosure of InterestNone Declared
The use of a Subjective wellbeing scale as predictor of adherence to neuroleptic treatment to determine poor prognostic factor in African population with Schizophrenia
- J. J. Boshe, D. Stein, M. Campbell
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S156
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Subjective well-being when on neuroleptic treatment (SWBN), has been established as a good predictor of adherence, early response and prognosis in patients with schizophrenia. The 20-item subjective well-being under neuroleptic treatment scale (SWN-K 20) is a self-rating scale that has been validated to measure SWBN. However the SWN-K20 has not been previously used to explore psychosocial and clinical factors influencing a low SWN-K20 score in an African population. This study uses the the SWN-K 20 scale among Xhosa speaking African patients with Schizophrenia to determine factors associated with SWBN in this population
ObjectivesTo investigate and identify demographic and clinical predictors of subjective well-being in a sample of Xhosa people with schizophrenia on neuroleptic treatment.
MethodsAs a part of a large genetic study, 244 study participants with a confirmed diagnosis of schizophrenia completed the translated SWN-K 20 scale. Internal consistency analysis was performed, and convergent analysis and exploratory analysis were conducted using Principal Component Analysis (PCA). Linear regression methods were used to determine predictors of SWBN in the sample population.
ResultsWhen translated into isiXhosa, the sasubscales of SWN-K 20 on their own were observed to be less reliable when compared to the scale in its entirety,internal consistency of 0.86 vs0. 59-0.47. The subscales were therefore noted to be not meaningful in measuring specific constructs but the full scale could be used to determine a single construct of general wellbeing.The validity of the SWN-K20 was further confirmed by moderate correlation scores with Global Assesment functioning scores (GAF), 0.44.There was a significant correlation between overall subjective well-being score with higher education level, and increased illness severity and GAF scores.
ConclusionsPatients’ perception of well-being while on neuroleptic treatment is an essential area of focus when aiming at improving patient centred treatment, compliance and overall treatment outcome. Treating individuals with SMI is difficult and made more complex when patient’s treatment experience and expectations are not elicited. Having a self-reported measurement like the SWN-K 20 available in a validated Xhosa language version provides helpful, possibly broad insights into the subjective well-being experiences of this patient group. Future studies should explore specific symptoms domains that are associated with a change in subjective wellbeing instead of general illness severity.
Disclosure of InterestNone Declared
Do we have an “anti-stigmotic”? – Addressing Mental-Illness Related Stigma as the main issue
- C. Cabaços, J. Andrade, F. Pocinho, M. Carneiro, G. Santos, D. Loureiro, A. Macedo
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1031
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
For people with mental illness, internalized stigma, also referred to as self-stigma, is characterized by a subjective perception of devaluation, marginalization, secrecy, shame, and withdrawal. It has many adverse effects on individual’s psychological well-being and clinical outcomes. The iatrogenic effects it has during psychotherapeutic treatment can significantly reduce utilization of mental health care services, reduce quality of life and increase avoidant coping. Overall, internalized stigma is considered a risk factor for poorer mental health prognosis. Although some interventions have recently been developed to specifically intervene on this target as part of psychological recovery goals over the course of treatment, most clinicians are not yet aware or empowered to correctly address this.
ObjectivesDescription of a clinical case illustrating the relevance on addressing internalized mental illness related stigma during the recovery process.
MethodsClinical case report and review of the literature on the subject.
ResultsWe present the case of a 47-year-old female patient, C.S., single, graduated in social work (currently unemployed), who was admitted at the Psychiatry Day Hospital, where she was referred by her Psychiatry Assistant because of abulia, social withdrawal and isolation, depressed mood, thoughts of shame, guilt and self-devaluation and work incapacity. She had been admitted in the Psychiatry ward one year earlier for a first psychotic breakthrough, presenting persecutory and grandiose delusions and auditory hallucinations. After three weeks of inpatient treatment with antipsychotics, a full remission of the symptoms was achieved, without any posterior relapse. Before that first psychotic episode, the patient had been taking anti-depressive medication (escitalopram 20 mg id) for many years, prescribed by her General Practitioner, for mild to moderate depressive symptoms. After being discharged from the Psychiatry ward, C. kept following an outpatient treatment with anti-depressives and behavioural activation-based psychotherapy. She started to believe she was mentally ill and therefore weak, uncapable, and less deserving than her peers or her previous self. These self-stigmatizing ideas were enhanced by the lack of family support and the beliefs that were fostered by her mother, with whom she started to live after the hospitalization. These factors led to a dysfunctional internalization of an illness behaviour, jeopardizing the patient’s ability to reach full recovery.
ConclusionsThis case reinforces the importance of targeting mental illness related stigma during the recovery process. Also, involving the family is of extreme importance to achieve support and address shared beliefs and the interchange between social and internalized stigma.
Disclosure of InterestNone Declared
A Case Report of Complex Clozapine Initiation Despite Contraindications
- G. Dumais-Lévesque, L. Béchard, E. Malenfant, M.-F. Demers, A.-P. Bouffard
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1057-S1058
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Clozapine is well known for its unique efficacy in treatment-resistant schizophrenia and to reduce violent behaviour. Unfortunately, life-threatening adverse reactions including ileus, myocarditis and agranulocytosis can hinder its use. In this context, some clinicians may be reluctant to initiate clozapine in patients who are prone to these adverse drug reactions.
ObjectivesTo describe a complex clozapine initiation despite the presence of serious adverse effects and contraindications. The management of these adverse events, using effective multidisciplinary team leadership strategies, will also be described.
MethodsA case report will be presented. The challenges faced while using clozapine and strategies implemented to pursue the use of this medication will be described.
ResultsA young black man with severe first episode psychosis was admitted to the early intervention outpatient clinic in Québec, Canada. Multiple aggression and critically disorganized behaviour prompted patient transfer to a specialized long-term care unit. Given the severity of the resistant disease and after a shared decision-making process with the family, clozapine was introduced despite ethnic neutropenia (down to 0,2 X 109/L) and idiopathic cerebral lesions. Both gave rise to multiple concerns. A specific hematological surveillance protocol was designed. Facing multiple severe neutropenia episodes, the use of prophylactic granulocyte colony-stimulating factor (300 mcg SC weekly) was added after literature review and a favourable consult of both pharmacist and hematologist. Cardiac enzyme elevation also requested specialized investigation and follow-up. Specialized educators, social workers, and nursing all needed to be deeply involved in the treatment process and team coordination requested strong team building capacities. After 6 months, the patient is now taking clozapine 325 mg daily and his symptomatology has sufficiently reduced to allow hospital leave. The patient is now engaged in his recovery process.
ConclusionsUsing an evidence-based approach, promoting expertise from multiple healthcare professionals, and allowing a substantial amount of time to develop team cohesion were all crucial elements of this success story.
Disclosure of InterestNone Declared
Amantadine augmentation in electroconvulsive therapy-resistant catatonia: a case report.
- L. Bueno Sanya, H. Andreu Gracia, O. De Juan Viladegut, L. Olivier Mayorga
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1066-S1067
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Catatonia is a syndrome characterized by physical symptoms ranging from immobility to excessive motor activity. Besides being historically associated mainly with schizophrenia, it is widely known that it can be the expression of different psychiatric, neurological or medical conditions. The treatment of choice is benzodiazepines, indicating electroconvulsive therapy in refractory cases. Amantadine is considered a second-line therapy in setting when electroconvulsive therapy is not available.
ObjectivesTo describe the case of a patient with treatment-resistant catatonic schizophrenia. Not having responded to benzodiazepines or electroconvulsive therapy, potentiation with amantadine was subsequently started.
MethodsOur patient presented at a psychopathological level; psychomotor inhibition, a perplexing attitude, and mute speech. At the motor level; ambitendency, indecision, automatic obedience, motor stereotypes, and facial grimaces. He did not present other alterations at the neurological level. Regarding complementary explorations, we performed neuroimaging and blood tests, which resulted all anodyne. With an alternative diagnosis, we considered that sequelae of a neuroleptic malignant syndrome could have produced the symptoms that he had suffered. Due to the persistence of the symptoms and their typical characteristics, catatonia was our first diagnostical impression. As treatment with benzodiazepines was ineffective, electroconvulsive therapy was started. No clinical improvement was observed. Given the refractoriness of the case, a review of the existing literature was carried out. We found reports of a good response to amantadine in similar cases. Amantadine was introduced up to a dose of 200mg.
ResultsAfter four weeks of treatment with amantadine at a dose of 200mg, the patient showed meager improvement at both psychopathological and motor level.
ConclusionsWe find the case of a patient with long-term schizophrenia who is nowadays dependent on all daily living activities and requires sustained care.
Disclosure of InterestNone Declared
Correlations of thought disorders with attenuated positive symptoms at clinical high-risk state for psychosis
- V. Kaleda, M. Omelchenko, E. Arutyunova
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S277-S278
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
One of the methods for early diagnosis in individuals at clinical high-risk state for psychosis could be the identifying specific symptoms, such as thought disorders. Thought disorders may be a separate symptom, unrelated to attenuated positive symptoms (APS) with an independent predictive value.
ObjectivesCorrelation analysis of thought disorders and APS in patients at clinical high-risk state for psychosis.
MethodsThe study included 30 young men (mean age 19.2±2.1 years) hospitalized at the clinic of the FSBSI “Mental Health Research Centre” with the APS in the first depressive episode (F32.1, F32.2, F32.28, F32.8) which is considered as clinical high-risk state for psychosis. The severity of thought impairment was assessed using the Thought, Language and Communication Scale (TLC). Subsequently was performed the search for correlations of scores on the TLC and the severity of “prodromal” symptoms, according to The Scale of Prodromal Symptoms (SOPS).
ResultsThe median value of the total score on the TLC was 20 [17.25;23.5]. The most important finding is the discovery of only minor correlations of thought disorder with “prodromal” symptoms. Indeed, the total score on the TLC correlated only with the total score on the SOPS at admission (r=0.370, p<0.05). Such symptoms of the TLC scale as «Derailment», «Incoherence», «Perseveration» did not find any correlation with prodromal symptoms (p>0.05).
ConclusionsThe obtained data indicates the independent nature of thought disorder in patients at clinical high-risk state for schizophrenia, which leads the need to determine its own prognostic value.
Disclosure of InterestNone Declared
Gambling Disorder and suicide risk – a clinical case
- P. Tirlea, R. Tipa, I. Luciana
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S566
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Pathological gambling is an addictive disorder and a current important issue with substantial social and personal costs. It is associated with impaired functioning, criminal record, bankruptcy and mental health problems. There is a significant comorbidity between gambling disorder, mood disorders and other addictive behaviors like alcohol use. Suicidality is common, impulsivity being a major risk factor for suicidal acts.
ObjectivesCase presentation of gambling disorder associated with a suicide attempt
MethodsReview of the clinical file of a patient diagnosed with gambling disorder and non-systematic review on the topic on PubMed
ResultsA 35 old male patient is brought to our psychiatrical emergency unit by means of ambulance as he attempted to commit suicide by inflicting multiple deep cuts on his forearms. He has a positive history of gambling disorder, no prior suicide attempt, or criminal record. He has a precarious economic status, the trigger for his acts being the loss of a substantial financial amount. The risk factors in his case were a positive familial history of addictive disorders (his father was diagnosed with alcohol use disorder), aversive childhood events, comorbid depression, alcohol misuse and low income. The patient resumed his gambling behavior 7 months prior to admission, after a 5 year abstinence, motivated by the desire to rapidly pay a loan he recently took. The addictive behavior worsened after his wife experienced a miscarriage. He started borrowing money, engaging in antisocial acts like stealing money from his wife’s bank account, neglecting his job and ending up in financial debt. He experienced feelings of alienation and isolation from his social network and family, unable to verbalize his burden. He also feared a divorce. Psychological coping strategies such as thought and emotional suppression were present and also an important tendency to minimize the severity of the events. Cluster B traits were present but not clinically significant. The suicide attempt is described by the pacient as being impulsive, with no prior planning, as a mean of problem solving for his desperate situation of high financial and social burden.
In the hospital setting, pharmacological treatment with SSRI Escitalopram and opiate antagonist Naltrexone was initiated. The patient was referred to psychological counseling during hospitalisation and to CBT after he left the hospital. He had excellent social support.
ConclusionsAlthough suicide is initially seen as an impulsive act, in fact it includes a constellation of thoughts, emotions and behaviors which lead to the hopelessness and desperation preceding the suicidal attempt. Gambling disorder tends to have a chronic evolution, impacting many important life domains, complex management such as pharmacotherapy, psychological interventions and social support being necessary for a favorable outcome.
Disclosure of InterestNone Declared
Mental health evaluation in senior year medical students
- M. A. Ghrab, I. Sellami, A. Haddar, M. Hajjaji, K. Jmal Hammami, M. L. Masmoudi
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S905
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Medical studies are known for being difficult and hard. They require a lot of dedication and hard work from students. This takes a toll on their mental health over the years.
ObjectivesDetect signs of anxiety, depression, and stress levels in 5th-year medical students.
MethodsThis study was cross-sectional through a self-administered pre-established questionnaire for medical students during September and October 2022. We used the General Anxiety Disorder-7 (GAD-7) questionnaire, the Patient Health Questionnaire-9 (PHQ-9) and the Perceived Stress Scale-10 (PSS-10). The satisfaction level with the choice of the medical field as a career was assessed on a scale ranging from 1 to 10.
ResultsOur population consisted of 54 5th-year medical students. The average age was 22.94±0.78 and 64.8% were female. All our population were singles. Active smokers represented 9.3% and alcohol consumption was reported by 9.3% of the participants. More than half of the population (51.9%) had a regular leisure activity. Most of the students had no medical history (72.2%) or psychiatric history (94.4%). The mean satisfaction level from choosing the medical field was 7.43±1.84. The mean GAD-7 and PHQ-9 scores were respectively 3.50±3.80 and 4.70±4.42. The PSS-10 score had a mean of 14.07±5.29. Five students (7.4%) presented self-harm thoughts. Students who were less satisfied with their choice of the medical field as a career had significantly higher scores of PHQ-9 (p<0.001), GAD-7 (p=0.004) and PSS-10 (p=.042).
ConclusionsMedical studies are the first step for these young doctors in their professional careers, which presents further psychological stressors. More attention towards the mental health of this population is needed to properly prepare them for their future.
Disclosure of InterestNone Declared
Identification of anxiety-depressive disorders in paramedics working shift work
- D. Brahim, N. Mechergui, I. Youssef, W. Ayed, M. Mersni, S. Ernez, N. Ladhari
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S473
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Shift work can lead to mental health problems evolving into real anxiety disorders with significant socio-professional repercussions.
ObjectivesThe purpose of our work was to screen paramedics with shift work for anxiety disorders.
MethodsCross-sectional study carried out among the paramedical staff of a Tunisian university hospital. The data was collected from a pre-established record sheet. Screening for anxiety-depressive disorders was done using the HAD scale
ResultsThe study included 158 paramedics. The average age was 36.48 years with female predominance at 70.9%. The average working time was 11.1 8.9 years and the average working time in shift work was 10.27 9.2 years. Of the 13 departments with non-standard hours of work, the main departments represented were resuscitation (n=24; 15.2%), emergencies (n=18; 11.4%) and radiology (n=17; 10.8%). Nurses accounted for 46.2%, manual workers for 23.4% and senior technicians for 19%.Certain anxiety symptomatology was found in 53.2% (n=84) and doubtful symptomatology in 29.1% (n=46) of the general population. Certain depressive symptomatology was noted in 17.1% (n=27) and doubtful symptomatology in 30.4% (n=48) of the general population. Occupational seniority and seniority in shift work were statistically significantly associated with both anxiety (p=0.04/p=0.05) and depression (p=0.05/p=0.006) symptomatology. ). Similarly, this anxiety-depressive symptomatology was associated with the position occupied (p=0.02 / p=0.04) and the assignment department (p=0.008 / p=0.01).
ConclusionsAnxiety-depressive disorders are common among paramedics working shift work in hospitals. Screening consultations in occupational medicine are necessary to detect these disorders early.
Disclosure of InterestNone Declared
The psychodynamic role of the displacement defense mechanism in people with obesity and anorexia nervosa
- F. Mustač, M. Matovinović, D. Marčinko
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S849
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Feeding plays a very important role in our lives. First of all survival, but in general it has a much wider and important social role. Through feeding, in addition to satisfying life’s needs and basic instincts, we experience a sense of satisfaction through the investment of libido. Anorexia nervosa and obesity as the two extremes of eating disorders can be considered as a disturbed experience of the satisfaction of eating, and in the background there is usually a very weak, fragile personality structure. A fragile personality structure tends to use primitive defense mechanisms, but the use of healthier, neurotic defense mechanisms in people with eating disorders should not be neglected.
ObjectivesTo investigate the role of the psychological defense mechanism of displacement in people with obesity and anorexia nervosa.
MethodsSearch of contemporary professional and scientific literature in the field of psychodynamics of eating disorders.
ResultsDisplacement is a defense mechanism in which, when faced with a problem, the problem is not solved with the initial object of aggression, but the problem is moved to another object or situation that the individual perceives as less dangerous. Thus, when faced with a stressful situation or sadness, obese people may have a need for emotional eating, which can be interpreted as displacement of the problem, which is temporarily “solved” by satisfying the basic instinct, but later the person becomes overwhelmed by internal and external shame. Equally so, a traumatic upbringing and disturbed interpersonal family dynamics, which are often present in people with anorexia nervosa, can cause anxiety drives that are displaced in the form of the need for a strong restriction of food intake.
ConclusionsIn people with obesity and anorexia nervosa, the use of the defense mechanism of displacement is pointed out. Through psychodynamic psychotherapy it can be very useful to recognize and interpert the use of displacement and, thus to enable reaching a neurotic and healthier level of functioning in people with the aforementioned eating disorders.
Disclosure of InterestNone Declared
Nanopore sequencing as a novel approach to transcend into the deep universe of schizophrenia
- I. B. Nita, O. D. Ilie, A. S. Ciobica, L. D. Hritcu, R. Popescu, R. P. Dobrin
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S439
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Schizophrenia (SCZ) is a chronic neuropsychiatric disorder possessing a multifactorial nature and dual facets of symptoms with a core underlying genetic mechanism that is still obscure. Lately, genomic studies revealed numerous single nucleotide polymorphisms (SNPs) that are non-coding and influence ribonucleic acid (RNA) expression, particularly its splicing.
ObjectivesConsidering that next-generation sequencing (NGS) protocols focus upon long-read sequencing as opposed to conventional RNA sequencing methodologies once with the advent of Oxford Nanopore Technologies’ (ONT) MinION, we primarily aimed to gather and review all evidence into how this approach may deepen and further offer insight into SCZ still undiscovered domain.
MethodsThe relevant literature searches were performed using distinct combinations of keywords including “schizophrenia” alongside „Nanopore”, “MinION”, and “Oxford Nanopore Technologies” on four databases (PubMed/Medline, ISI Web of Knowledge, Scopus, and ScienceDirect). We implied the entries to strictly “research articles” written in English as inclusion criteria.
ResultsBy restricting the returned results starting with the year when the platform was officially launched, a total of n = 69 studies were displayed between the pre-established interval (2014 – 2022). If taken per database, n = 2 were identified in PubMed/Medline, n = 7 in ISI Web of Knowledge, n = 4 in Scopus, and n = 56 in ScienceDirect. In chronological order, n = 0 were published in 2014, n = 3 in 2015, n = 7 in 2016, n = 7 in 2017, n = 9 in 2018, n = 3 in 2019, n = 7 in 2020, n = 19 in 2021 and n = 14 in 2022. Finally, per the strategy applied, n = 49 were returned for “schizophrenia” + “Nanopore” from which n = 2 in PubMed/Medline, n = 5 in ISI Web of Knowledge, n = 4 in Scopus, and n = 38 in ScienceDirect. For “schizophrenia” + “MinION, there was a cumulative number of n = 5, from which we had n = 0 in PubMed/Medline, n = 0 in ISI Web of Knowledge, n = 0 in Scopus, and n = 5 in ScienceDirect. Finally, for “schizophrenia” + “Oxford Nanopore Technologies” were displayed n = 15, and the situation was n = 0 in PubMed/Medline, n = 2 in ISI Web of Knowledge, n = 0 in Scopus, and n = 13 in ScienceDirect.
ConclusionsWe presently assist to a fulminant ascension in the literature, with applicability in other fields. Perhaps as cornerstone stands a recent publication in which the authors reveal the risk of the Calcium Voltage-Gated Channel Subunit Alpha1 C (CACNA1C) gene involved, being identified thirty-eight novel exons and two hundred and forty-one novel transcripts following RNA purification from six regions (cerebellum, striatum, and dorsolateral prefrontal cortex) among which targeted were cingulate, occipital and parietal cortexes.
Disclosure of InterestNone Declared
Role of Folic acid as adjuvant treatment in Schizophrenia: A randomized controlled trial
- P. Saxena, S. Kumar, K. Vaibhav
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S634-S635
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Schizophrenia is a chronic psychiatric illness with symptoms in positive, negative and cognitive domain.The interplay of dietary folic acid intake with common genetic variants that influence folate metabolism, has potential implications for Schizophrenia pathogenesis and treatment.Therefore, it’s deficiency has been identified as a risk factor for Schizophrenia through epidemiologic, biochemical and gene association studies.
Objectives1-To assess the efficacy of folic acid supplementation on severity of symptoms and overall functional status of patients
2-To assess the correlation of serum folate levels with symptom severity and overall functional status of patients
MethodsA randomized control trial study was carried out in the inpatient department of a psychiatric tertiary care centre on 40 participants (29 males and 11 females)who were between the ages of 18 – 55 years,met diagnostic criteria for Schizophrenia (ICD 10) and had at least 2 years of illness duration while those with a co-morbid psychiatric illness, medical illness and substance abuse were excluded. The participants were then randomly allocated into two groups (experimental Group A which received 5mg folic/day along with anti psychotic drugs and control Group B which received only anti psychotic drugs) and followed up for 3 months. Blood sample for measuring serum folate level was obtained from the experimental group at the beginning and at the end of the study period. Scales applied were Positive and Negative Syndrome Scale(PANSS) for symptom severity and Global Assessment of Functioning scale(GAF) for overall functional status.
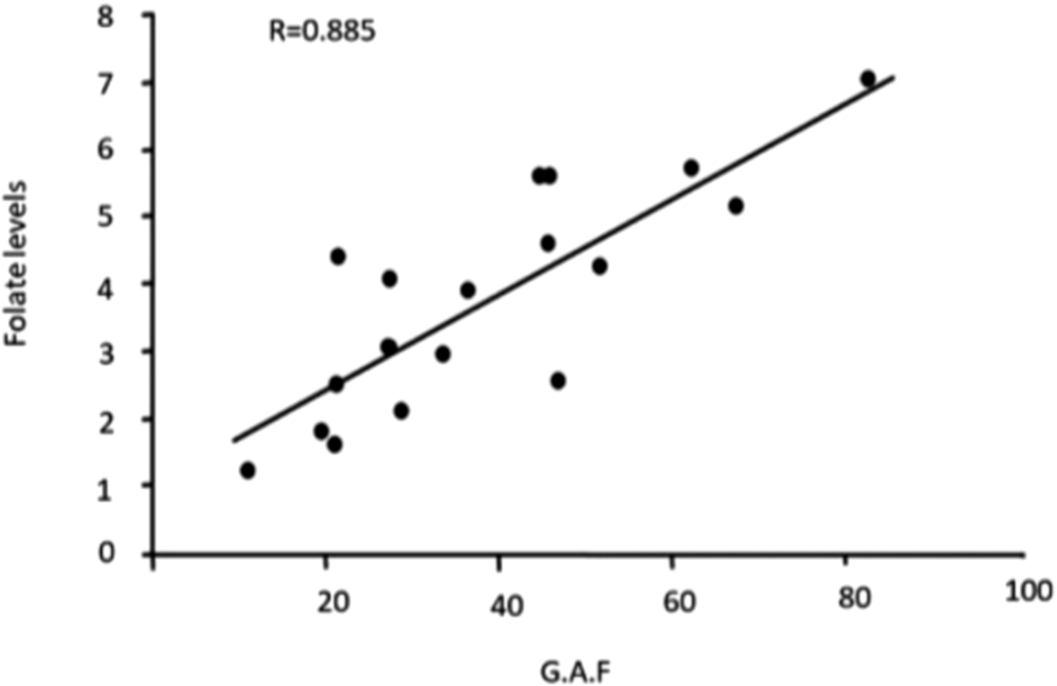
ResultsA significant difference (p value< 0.05) was observed in PANSS scores at the end of the study between experimental group and control group( table 1) and also in GAF scores between both the groups after 3 months(table 2). At the end of the study period,a strong negative correlation(r= -0.9) was found between serum folate level and total PANSS score in the experimental group (figure 1) while the correlation between GAF score and serum folate level was strongly positive (r= 0.8) (figure 2).
Table 1 PANSS (3 Month) Group A(n=20) Group B (n=20) P value Positive 16.8±2.80 22.9±3.37 0.036 Negative 14.3±3.32 15.1±2.61 0.18 General 17.95±2.52 21.85±3.18 0.0001 Total 45.95±3.41 58±3.49 0.00249 Table 2 GAF Group A(n=20) Group B (n=20) P value 0 MONTH 23.25±3.43 22.7±2.90 0.3 3 MONTH 65.75±4.22 44.9±7.09 0.0256 Image:
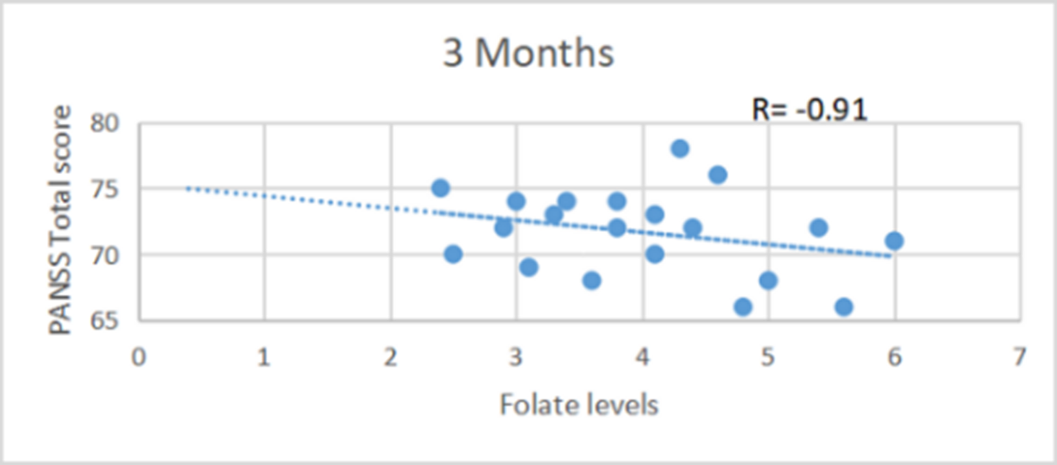
Image 2:
 Conclusions
ConclusionsOur study is among the few to use a randomized controlled study design for assessing the effect of folic acid supplementation on severity of symptoms and global functioning in Schizophrenia,strongly suggesting the use of folic acid as an adjuvant treatment for Schizophrenia.
Disclosure of InterestNone Declared
Health and care system assessment aimed at cultural adaptation of MhGAP modules
- E. Dozio, L. Caron
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S155
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
As part of the Global Mental Health (GMH) movement, WHO launched the Mental Health Gap Action Program (mhGAP). One of the key initiatives of the MhGAP is to train lay health professionals to meet the mental health needs of populations, particularly in low- and middle-income countries (LMICs) where the need far exceeds the availability and quality of services. Training modules are standardized and designed for use in many countries and settings. In practice, there is often a stereotyped reproduction of modules without consideration of specific cultural adaptation needs.
ObjectivesAs part of a psychosocial support program in two provinces of the eastern Democratic Republic of Congo (Ituri and North Kivu), the NGO Action contre la Faim proposed a health and care system assessment aimed at adapting MhGAP modules for health center staff. The objective was to know the local practices in terms of psychic care as well as to identify the competences already existing to reinforce them, but also to contextualize the tools and the contents of the trainings.
MethodsThe methodology used was mixed.
A questionnaire based on the WHO situation analysis tools was revised, simplified and adapted to the zone, allowing us to obtain quantitative data on the health centers, the care provided, referrals and supervision. Health care workers were interviewed using the questionnaire from ACF’s “Strengthening the Health Care System” guide, focusing on care methods, knowledge of mental health and the most frequently encountered symptoms. Focus Group Discussions with the Community Relais in the area allowed for the collection of information on the level of knowledge of the population in terms of mental health, their awareness on this subject, their cultural vision and the means of care.
ResultsThe data collected from 9 health centers in the two provinces allowed us to learn about:
- Poor knowledge of mental health and school readiness
- Identification of barriers to access to care
- Beliefs around mental health, mental suffering and care
- Details about the different pathologies and symptoms as well as the issues related to the therapeutic framework.
ConclusionsThe evaluation was fundamental to have a better knowledge of the context, which made it possible to adapt the content of the MhGap training modules les, to design tools more adherent to reality. The data collected may also be the subject of advocacy aimed at mobilizing the country’s policies in terms of mental health, as well as raising awareness in the international community.
Disclosure of InterestNone Declared
Cognitive effects after ECT: how to treat them?
- E. Verwijk
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S25
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Abstract
How far have we progressed in the field of treating cognitive side effects? Six months after the last ECT treatment, about 15% of patients still have such symptoms, limiting daily life. So far, studies in the field of cognitive training for ECT-related cognitive side effects show few positive effects. Nevertheless, these patients seem to help well. Because they have no structural damage to their brain, training with long-term effectiveness may be available for them. Amsterdam University Medical Centers started the CONNECT clinic (Cognitive and Neuropsychological Aftercare ECT) in early 2022 for diagnosis and treatment of patients with long-term cognitive complaints (longer than six months) that hamper their daily functioning. After the intake and neuropsychological diagnostics, treatment starts if there is an indication. Patients are then offered ’cognitive strategy training’ in an individual course. Developed in the field of neuropsychological rehabilitation, these help to get a grip on cognitive complaints by improving memory or executive functioning with learning strategies. Our initial experiences with patients show that patients master these strategies very well and quickly. We present a pilot project from the Amsterdam UMC where an individualized treatment-programme for long-term cognitive complaints after ECT is being implemented and evaluated.
Disclosure of InterestNone Declared
Thyroid Stimulating Hormone circadian variations in paranoid schizophrenic psychosis between acute and stable phases. A comparative study.
- A. Marcos-Rodrigo, A. L. Morera-Fumero, P. Abreu-Gonzalez, E. Diaz-Mesa, L. Fernandez-Lopez, J. J. Tascon-Cervera
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S186
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Day-night changes in several molecules are studied as biomarkers of circadian rhytms (Morera-Fumero, A. L. et al. Progress in Neuro-Psychopharmacology and Biological Psychiatry 2017; 75 207-212). Circadian rhythmicity of the pituitary-thyroid axis has been proven in healthy individuals, with a Thyroid Stimulating Hormone (TSH) peak in serum around midnight and peaks during day hours (Bellastella, G. et al. Life 2021; 11(5), 426). A recent meta-analysis has reported differences in serum TSH levels between first-episode psychosis and multiple-episode schizophrenia (Misiak, B. et al. Progress in Neuro-Psychopharmacology and Biological Psychiatry 2021; 111, 110402). However, studies assessing quantitative circadian variations on TSH serum in schizophrenic patients are scant.
ObjectivesComparing serum TSH levels at two different times of the day (12:00 and 24:00 hours) and the differences between the acute (hospital admission) and recovered phase (hospital discharge) of the disease.
MethodsFourteen male patients (age 26,8±9,3 years) with the diagnosis of paranoid schizophrenia psychosis according to the DSM-IV partake in the study. Patients were admitted to the University Hospital of the Canary Islands psychiatric room because of acute relapse. Blood samples were taken in the first 24 h of admission and at 24 h. before discharge. All patients gave written consent to participate in the research study. Serum TSH was determined by ELISA methods. Paired sample t-tests were performed between TSH serum levels at admission and discharge at 12:00 and 24:00 hours. Statistical analyses were performed using IBM® SPSS® Statistics 25 software for MAC (IBM Corporation 1989, 2017).
ResultsThere were statistical differences between the 12:00 h and the 24:00 h of the TSH serum levels at admission (12:00: 145,856±156,961vs. 00:00: 192,006± 122,757, p = 0.04); TSH discharge, (12:00: 134,483±72,882vs 00:00: 244,214±148,697, p = 0.002). There were no statistical differences between the 12:00 TSH levels at admission and discharge (145,856±156,961 vs. 134,483± 72,882, p = 0.66). The 24:00 h comparison of TSH levels neither elicited significant results (admission: 192,006±122,757 vs. discharge: 244,214± 148,697, p = 0.15).
ConclusionsSchizophrenic patients undergo TSH serum changes in a circadian pattern during the acute and stable phases of the disease; nevertheless, they experience smaller deviations during the acute phase. Higher levels of TSH were observed around midnight, as it happens in healthy individuals, with higher peaks during the stable phase compared to the acute one.
Disclosure of InterestNone Declared
Adjunctive short- and long-term combination treatment of esketamine and VNS in difficult to treat depression (DTD)
- E. Kavakbasi, B. T. Baune
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S249-S250
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
NMDA-Receptor antagonists have rapid antidepressant and antisuicidal properties. However, the antidepressant effect is short lasting raising the question of best maintenance strategy, which is unanswered so far. Invasive vagus nerve stimulation (VNS) as a treatment option for refractory and chronic major depression was shown to reduce the need of maintenance treatment sessions in electroconvulsive therapy (ECT) patients.
ObjectivesThere are no published data on the combination of VNS and esketamine. To determine the impact of the combination of VNS and esketamine in DTD.
MethodsIn this naturalistic observational study, we investigated the short- and long-term impact of combination of VNS and esketamine in n=8 patients with difficult-to-treat depression (DTD). Follow-up evaluations were scheduled prospectively pre-surgery at baseline and every 3 months after VNS-implantation (follow-up period 12-24 months, mean 17).
ResultsThe mean age of patients was 50,8 years. 50 % of patients (n=4) were female. All patients suffered from severe DTD (mean MADRS at baseline 30,9). Mean number of hospitalizations per months decreased from 0.17 to 0.11 after VNS implantation. 6 of 8 patients were offered maintenance esketamine treatment. Mean MADRS at 12-months was 19 (38.5 % MADRS reduction). The need of mean esketamine treatment sessions decreased from 2.3 at 6-months visit (V6) to 1.37 at V9 and 0.96 at V12 respectively. Termination of maintenance esketamine was possible in 4 cases after a mean of 11.5 months.
ConclusionsCombination of esketamine and VNS is a safe and effective treatment option in severely ill DTD patients to relieve disease severity and reduce hospitalizations. Need of esketamine treatment sessions decreases 6 months after VNS implantation.
Disclosure of InterestNone Declared
Exploring the attitudes of non- psychiatric healthcare workers towards patients with alcohol use disorder in a tertiary hospital
- H. T. Tan
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S379
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
There are serious adverse effects on the physical and mental wellbeing of patients with alcohol use disorders.
It is important to screen and provide brief intervention for these group of patients during their inpatient admission.
Prompt identification and treatment of patients with alcohol use disorders are contingent on the attitudes of healthcare workers towards them.
Non-psychiatric doctors and nurses might respond inadequately due to negative attitudes and beliefs.
ObjectivesWe examined the attitudes of non-psychiatric workers in the medical and surgical wards.
MethodsThe Alcohol & Alcohol-Problems Perceptions Questionnaire (AAPPQ) was administered to 128 doctors and 785 nurses from the medical and surgical disciplines in a tertiary hospital.
Results75.5% of doctors and 51.9% of nurses endorsed the domain of role legitimacy in the AAPPQ.
However both groups reported low-levels of role-adequacy (combined: 41.2%), role-support (combined: 36.9%), motivation (combined: 36.5%), task-specific self-esteem (combined: 25.1) and work satisfaction (combined: 20.5%) in the AAPPQ.
ConclusionsWhile non-psychiatric healthcare workers acknowledged the importance to initiating intervention for patients with alcohol-use disorder in daily work, there were low levels of therapeutic commitments towards patients with problematic alcohol-use.
It is vital to introduce in-house programmes to educate, empower and emphasise the importance of therapeutic contact with patients for alcohol intervention.
Disclosure of InterestNone Declared
Psychedelics for depression: from neurobiology to treatment
- K. P. Kuypers
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S18
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Abstract
Decades ago, the classical psychedelics psilocybin and LSD entered the therapeutic setting and already then showed their therapeutic potential in the treatment of psychiatric disorders. For thousands of years another psychedelic, ayahuasca, is being used by tribes in western Amazonia for healing and divination, and in recent years its use has expanded worldwide.
Research into the therapeutic potential of these substances has re-emerged and (preliminary) findings are promising, showing that after one or two administrations remission is reached in depressed patients that were labeled as treatment-resistant. This is a remarkable finding as the therapeutic effects of treatment with conventional pharmacological agents like SSRIs take longer to lead to remission, with one-third of the patients failing to reach this stage.
The fast onset of positive therapeutic effects by psychedelics increases the interest to discover the mechanism of action behind this. There is a debate about the importance of the psychological experience caused by these agents in the therapeutic outcome, while science also tries to understand the neurobiological correlates. The latter will be addressed in my talk and I will link it to psychedelics’ therapeutic effects.
Disclosure of InterestNone Declared







