INTRODUCTION
Infection with Salmonella enterica is primarily foodborne and causes an estimated 1 million illnesses and 378 deaths annually in the USA [Reference Scallan1]. In 2006, among 40 888 laboratory-confirmed S. enterica cases reported to the Centers for Disease Control and Prevention (CDC), 6872 (16·9%) were serotype Typhimurium, making it the most common of over 2500 Salmonella serotypes [2]. Salmonella is found in the intestinal tract of animals, and subsequently outbreaks of Salmonella Typhimurium infections have been caused by foods of animal origin [3, 4] and animal contact [Reference Fuller5–Reference Lynch8], and also by contaminated raw produce items [Reference Horby9, Reference Brooks10]. In recent years, six large multistate salmonellosis outbreaks have been linked to contaminated tomatoes traced to growing areas in Eastern and Southeastern USA [11–Reference Cummings15].
Investigation of multistate outbreaks can be challenging requiring coordination of efforts across public health jurisdictions, and hypothesis generation can be particularly difficult. Sometimes, within a more widespread outbreak, clusters of cases associated with particular restaurants may aid hypothesis generation or even identify the food vehicle responsible for the larger outbreak. In our investigation of a multistate outbreak of S. Typhimurium infections in 2006, restaurant-associated clusters of cases in four states were identified. Although a single food vehicle was not initially identified in any one restaurant cluster, comparison of case exposures across all four restaurant-associated clusters was instrumental in rapidly identifying the cause of this large multistate outbreak. This report describes the 2006 outbreak investigation and summarizes the ongoing problem of tomato-associated outbreaks of salmonellosis in the USA.
METHODS
Outbreak detection, case finding, and hypothesis generation
On 3 October 2006, Vermont State Public Health Laboratory officials informed staff of PulseNet, the national molecular subtyping network for foodborne disease surveillance, of two S. Typhimurium isolates with an indistinguishable pulsed-field gel electrophoresis (PFGE) pattern (CDC XbaI pattern JPXX01.0604). During the last week of September 2006, officials from the Minnesota Department of Health (MDH) had identified four human case isolates of S. Typhimurium with indistinguishable PFGE patterns (pattern that matched that posted by Vermont) and on 4 October, MDH posted a message on the PulseNet web-board about their investigation. The same day, PulseNet identified 33 isolates of XbaI pattern JPXX01.0604 submitted to PulseNet from multiple states since 1 August 2006. During October of the four previous years, up to 30 isolates with this PFGE pattern were submitted to PulseNet each year. PulseNet staff notified all state public health laboratories of the increase in reports of this pattern. During the first 2 weeks of October, MDH and other state health departments began investigating S. Typhimurium cases with XbaI pattern JPXX01.0604. On 19 October, CDC began coordinating a multistate investigation.
For case-finding, a confirmed case was defined as a person with a culture-confirmed S. Typhimurium infection with the isolate demonstrating the out-break PFGE pattern (XbaI enzyme JPXX01.0604 and BlnI enzyme JPXA26.0174) with illness onset, or if unknown, specimen collection date, between 1 September and 20 October 2006.
A dynamic, iterative process of hypothesis generation was utilized in this investigation. For initial hypothesis generation, state and local health departments reported information from patients on exposure to food and beverage items as gathered in their state's routine case evaluation questionnaires, some of which included standardized hypothesis-generating interviews, that collected exposure information on >300 food and beverage items and other exposures including dining at restaurants. No common food item was identified in cases initially by routine case evaluation; however, focal restaurant clusters were identified. A restaurant cluster was defined as ⩾2 cases with exposure to the same restaurant in the week before illness began. To develop hypotheses of potential sources of S. Typhimurium infections, state health department officials from four states (Connecticut, Massachusetts, Michigan, Minnesota) identified restaurant clusters, conducted telephone interviews of patients, and collected additional information from restaurant managers regarding food served at each restaurant. Case-exposure rates to food items served in these four restaurant clusters were compared to identify high-exposure foods reported in cases in all restaurant clusters. After consultation via conference calls with health officials from involved states, standardized hypotheses-generation interviews were conducted among non-restaurant cases using a standardized case questionnaire that focused on the foods reported by cases in all the restaurant clusters and routine case interviews. Cases were asked if they ate, might have eaten, or did not eat selected produce items in the 7 days before illness onset. Cases were also asked about places where they purchased lettuce and tomatoes in the 7 days before illness onset, including patronage at restaurants. CDC contacted Canadian public health officials to inquire if case-patients had been identified in Canada.
Case-control studies
Two case-control studies were conducted to identify specific food exposures associated with infection; one study was conducted in nine states and one study was conducted in a single state, Minnesota. Study cases were defined as infections with the outbreak strain of S. Typhimurium in a person who had illness onset between 1 September and 20 October 2006.
In the multistate study, cases and controls were limited to persons aged 18–70 years, and controls were persons without diarrhoeal illness between 15 September and 20 October 2006 identified by use of a reverse telephone directory. We attempted to enrol one control for each interviewed case. This study focused on adults since the overall median case age was 37 years and enrolling adult controls would facilitate control recruitment. Cases previously interviewed during hypothesis generation were not excluded from the case-control study. Study questionnaires collected information on demographics, food sources including restaurants, >20 specific food items identified as possible vehicles by hypothesis generation, including a variety of produce items and cheeses as identified as high-exposure foods in cases in the four restaurant clusters and during hypothesis generation, and whether foods were prepared inside or outside of the home. Patients were asked about exposures in the 7 days before illness onset; controls were asked about exposures matching the corresponding case's exposure period.
In the Minnesota study, up to three controls per case were enrolled through sequential digit dialling anchored on the cases' telephone numbers. Controls were individuals that reported no diarrhoea or vomit-ing during the 2 weeks preceding the corresponding case-patient's onset date matched to cases by age group (0 to <6, 6 to <12, 12 to <18, 18 to <40, 40 to <60, >60 years). These study questionnaires collected information on demographics; travel; contact with pets; food sources, including restaurants; >40 specific food items; method of preparation; and where and when foods were prepared or consumed.
Statistical analyses
Matched statistical analyses were conducted using SAS v. 9.1 (SAS Institute, USA). Matched odds ratios (mOR) and 95% confidence intervals (CI) were calculated using logistic regression. Mid-P confidence intervals were used in the Minnesota case-control analysis [Reference Vollset16]. This P value is an exact likelihood ratio test-based P value as opposed to Fisher's exact test. The P value reported for the odds ratio (OR) is twice the one-sided tail area of a likelihood ratio test against the null hypothesis of the OR equalling 1.
Laboratory investigation
State public health laboratories serotyped Salmonella isolated from patients' specimens. Isolates of S. Typhimurium were subtyped by PFGE at state public health laboratories and results were electronically submitted to PulseNet [Reference Swaminathan17]. Outbreak isolates were tested for susceptibility to 15 antimicrobial agents by the National Antimicrobial Resistance Monitoring System (NARMS) Laboratory at CDC [18].
Traceback and environmental investigation
Traceback activities were initiated in states with restaurant clusters following identification of foods commonly reported by cases in restaurant clusters identified during hypothesis generation. Traceback investigations were narrowed once the results of the multistate case-control study implicated a food vehicle. Officials from the U.S. Food and Drug Administration (FDA), in conjunction with state and local authorities, conducted traceback investigations to determine the source of tomatoes from seven restaurants with confirmed cases. By the time the packing house was identified in November 2006, seasonal tomato production had ended, and the operator was not available. The fields used to grow tomatoes from implicated lots were also identified. As a result, FDA deferred the field investigation until the next growing season and completed the investigation in August 2007. The investigation involved observing practices in the tomato packing house, observing current practices in tomato fields, and assessing the fields used to grow implicated tomatoes in 2006. Environmental and water samples were also collected in 2007.
RESULTS
Outbreak detection, case-finding, and hypothesis generation
We identified 190 cases of S. Typhimurium with the outbreak pattern predominately in the Midwest and Northeastern USA and Canada; the 189 cases in the USA were reported from 21 states (Fig. 1). The single patient identified in Canada had travelled to the USA during their incubation period. Illness onset dates ranged from 2 September to 20 October 2006. The peak in illness onset dates occurred between 14 September and 1 October 2006; 91% of onsets occurred during this time period (Fig. 2). Patients ranged in age from 2 to 88 years (median 34 years); 58% were female. Of 109 patients for whom clinical data were reported, 24 (22%) were hospitalized; no deaths were reported.
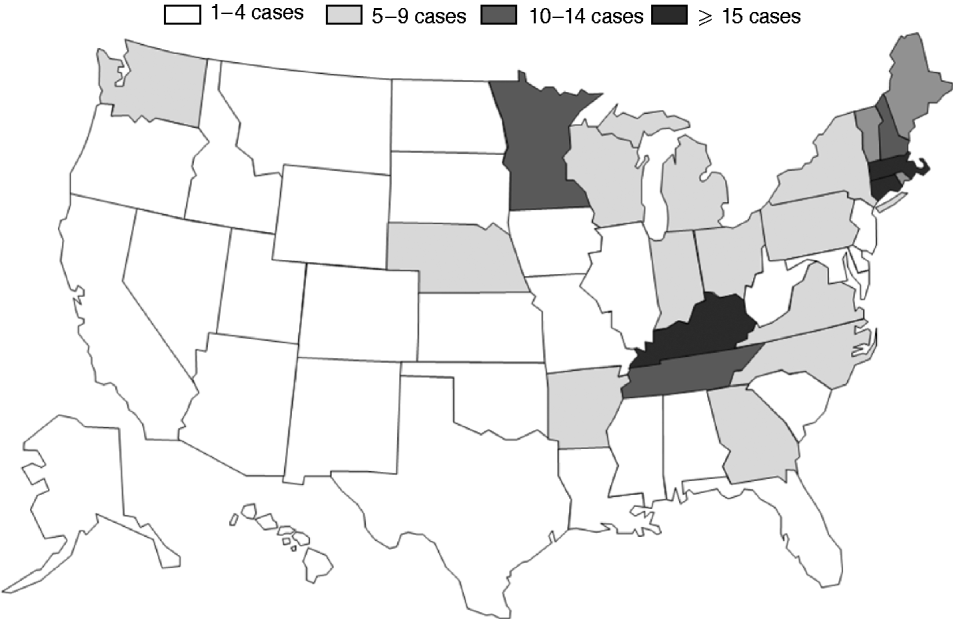
Fig. 1. Number of cases by state, multistate outbreak of Salmonella Typhimurium infections, USA, 2006 (n=190). There was one confirmed case in Canada.
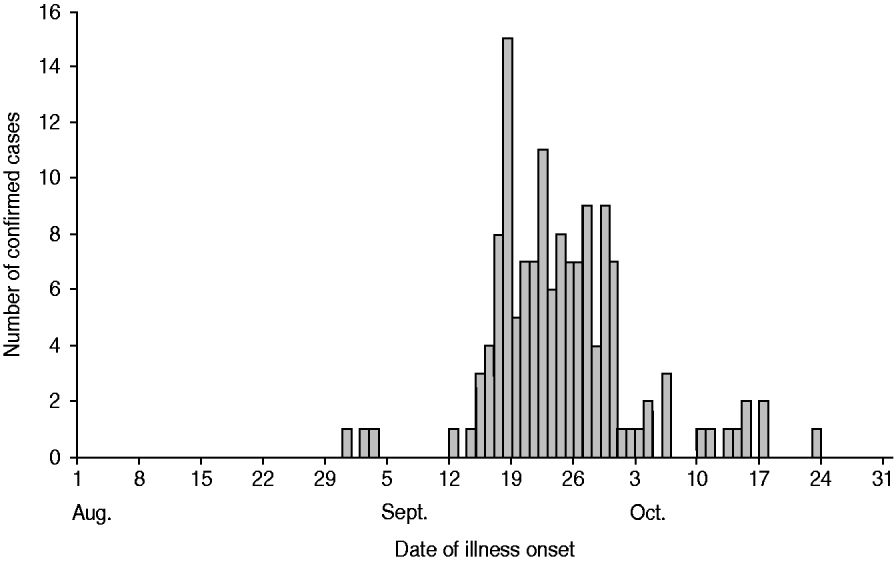
Fig. 2. Cases by date of illness onset, multistate outbreak of Salmonella Typhimurium infections, USA, 2006 (n=139). A case was defined as a person with a culture-confirmed S. Typhimurium infection with the isolate demonstrating the outbreak PFGE pattern (XbaI enzyme JPXX01.0604 and BlnI enzyme JPXA26.0174) with illness onset or, if unknown, specimen collection date, between 1 September and 20 October 2006.
For patients involved in the four restaurant clusters and patients not linked to individual restaurants, hypothesis-generation interviews identified lettuce and tomatoes as food exposures meriting evaluation in an analytical study. The four restaurants, located in Minnesota, Massachusetts, Connecticut, and Michigan, were of a variety of types including a fast-food burger establishment, a seasonal restaurant, a restaurant serving Mexican-style food, and a gourmet delicatessen. Interviews of the patients in the four restaurant clusters indicated that 29 (97%) of 30 patients consumed large, round tomatoes (Table 1). Lettuce types consumed by patients varied: 22/32 (69%) were iceberg; 7/32 (22%) were romaine, and 1/32 (3%) was mesclun (Table 1). Fewer patients (18/30, 60%) ate cheese of several different types. Furthermore, in hypothesis-generation interviews of 59 patients not associated with restaurant clusters, patients reported consuming tomatoes at a restaurant (n=33, 56%), large tomatoes at a restaurant (n=26, 44%), lettuce at a restaurant (n=33, 56%), and iceberg lettuce at a restaurant (n=17, 29%).
Table 1. Food histories for patients with laboratory-confirmed Salmonella Typhimurium infections with the outbreak strain in the four restaurant clusters by produce item and state
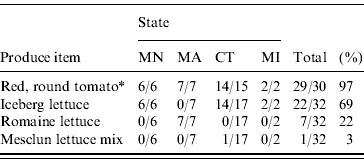
* No other tomato varieties used at the four restaurants.
Case-control studies
Among the 189 outbreak cases in the USA, 61 patients resided in the nine states that participated in the multistate study. Of these 61 cases, 59 (97%) cases and 59 geographically matched controls were enrolled in the multistate study. Ninteen cases included in the case-control study were also interviewed during hypothesis generation. The mean age of cases was 37 years (range 18–86 years) and of controls 49 years (range 18–70 years). Thirty-five (59%) of 59 patients and 23 (39%) of 59 controls were female. Symptoms reported by patients included: diarrhoea (92%), abdominal cramps (88%), fever (80%), bloody diarrhoea (58%), vomiting (45%), and nausea (27%). Sixty-eight percent of enrolled patients visited an emergency room and 27% were hospitalized. The mean duration of hospitalization for patients was 4 days (range 1–8 days).
Forty-four (81%) of 54 case-patients and 42 (78%) of 54 controls reported eating any tomatoes during the exposure period. Among 53 case-control pairs, cases (62%) were more likely than controls (30%) to eat tomatoes in a restaurant (mOR 3·5, 95% CI 1·5–8·2) or lettuce in a restaurant (69% cases vs. 45% controls; mOR 2·9, 95% CI 1·2–7·5) (Table 2). When analysed by produce type, illness was associated with eating raw, large, round tomatoes in restaurants (mOR 3·1, 95% CI 1·3–7·3). Patients ate multiple types of lettuce at restaurants, and illness was not associated with any single lettuce type. Illness was not associated with any other food item.
Table 2. Matched univariate analysis for multistateFootnote † case-control study of selected food exposures during the 7 days before illness onset for cases of Salmonella Typhimurium infection and controls
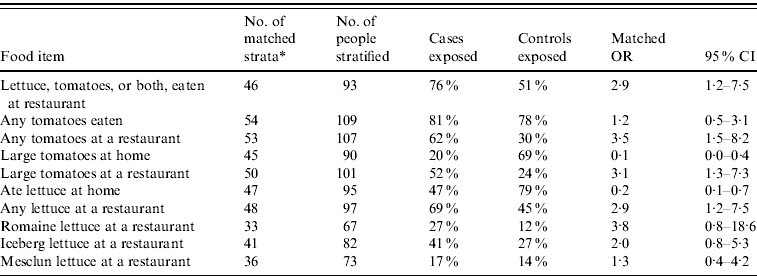
OR, Odds ratio; CI, confidence interval.
* Where response available from both case and matched control.
† Interviews conducted in Connecticut, Massachusetts, Maine, New Hampshire, Ohio, Rhode Island, Tennessee, Virginia, and Vermont.
Fifteen cases and 38 controls were included in the Minnesota case-control study. Univariate analysis found that eating at a single location of fast-food restaurant chain A (6/15 cases vs. 0/35 controls; OR undefined, 95% CI undefined, P<0·001) was associated with illness; however, eating at fast-food restaurant chain A was marginally significant (615 cases vs. 5/35 controls; OR 4·0, mid-P 95% CI 1·02–19·5, P=0·047). In analysis restricted to cases and controls that did not eat at any fast-food restaurant chain A, only eating tomatoes at a restaurant (6/8 cases vs. 9/28 controls; OR 6·3, mid-P 95% CI 1·05–50·44, P=0·046) was associated with illness.
Laboratory investigation
PulseNet PFGE pattern XbaI enzyme JPXX01.0604 was the tenth most common of 1490 S. Typhimurium patterns reported to PulseNet during 1998–2006. Three isolates were pansusceptible to the NARMS panel of 15 antimicrobial agents.
Traceback investigation
Tomatoes supplied to all four restaurants with ⩾2 cases were traced through multiple wholesalers and brokers to a single packing house in Ohio supplied by three tomato growers from 25 fields in three counties. Six environmental and four water samples were collected; two environmental samples, one from a creek used for irrigation and one from a ditch next to a tomato field, yielded Salmonella serotypes Newport and Give. Potential cross-connections were identified between creeks, wells and ditches for irrigation water.
DISCUSSION
In October 2006, we investigated a large, multi-state S. Typhimurium outbreak involving four restaurant-associated clusters. A single PFGE-defined strain of S. Typhimurium caused a multistate outbreak of diarrhoeal illness in 190 residents of 21 states and Canada. Because only an estimated 3% of Salmonella infections are laboratory-confirmed and reported to surveillance systems [Reference Voetsch19], the actual number of cases in this outbreak was likely to have been much larger than the 190 laboratory-confirmed cases identified. Cases were linked to the outbreak through molecular subtyping of patients' isolates and investigation involved the coordination of multiple state and local health and agriculture departments, laboratories, FDA, and CDC. The results of the epidemiological investigation, combined with the biological plausibility, frequency of exposure, information on restaurant clusters in four states, and traceback findings converging to one grower/packer in Ohio implicated large, round tomatoes eaten at restaurants as the outbreak vehicle. Additionally, the majority of affected states were in the Midwest and Northeastern USA. This geographical clustering of cases primarily in Eastern USA correlates with distribution of tomatoes produced in Ohio. Last, the findings in this investigation are consistent with previous multistate tomato outbreaks (n=11) reported to the CDC. Most of these outbreaks occurred over a 6- to 8-week period. Additionally patients were typically older with median age in the 30s and there were slightly more female patients than males (CDC, unpublished data).
At the conclusion of the case-control studies, the pattern of the epidemic curve indicated little evidence of ongoing transmission. Typically, under favourable conditions, the shelf-life of a tomato is about 30 days; however, shelf-life depends on the maturity at which the tomato is picked and the temperature at which it is held. By November 2006, contaminated tomatoes associated with this outbreak were likely to have been consumed or discarded. As a result, no recall was issued. In response to the outbreak, the grower/packer made improvements in good agricultural and manufacturing practices relating to the packing house and contracted a third-party auditor to improve food-safety practices based on customer request.
Since the advent of surveillance using molecular subtyping methods, identification of widespread multistate outbreaks is increasing. Hypothesis generation in these multistate outbreaks can be challenging. Hypothesis generation was conducted in a dynamic and iterative fashion. A limitation of this investigation is the inclusion of cases interviewed in hypothesis generation in the case-control study. However, it was necessary to use a compressed time-frame in order to expedite the investigation and rapidly identify the source of illnesses. This investigation demonstrates that information gathered during rapid evaluation of restaurant clusters can be critical in the investigation of a multistate outbreak, even if the source of the local cluster is not immediately clear. Raw produce items, such as tomatoes, that might be consumed in small quantities as ingredients of other dishes might not be remembered and can be difficult to implicate in epidemiological studies [Reference Mahon20].
Tomatoes are a well-documented vehicle for Salmonella outbreaks [11–Reference Cummings15, Reference Hedberg21–Reference Yuan24]. The outbreak Salmonella strain was isolated from tomatoes or their growing environment during three investigations [11, Reference Greene12, Reference Sandt22, Reference Kretsinger23], although finding a tomato contaminated with the outbreak strain during an active investigation has been a challenge. Due to the short shelf-life of tomatoes compared to the time required to complete an epidemiological study implicating tomatoes as an outbreak source and the associated traceback, there are usually no tomatoes left from the same contaminated lot for laboratory testing. A limitation of the environmental investigation was that tomato production had ended by the time the packing house was implicated in November 2006 which resulted in deferment of the environmental investigation until the next growing season in August 2007. Testing conducted as part of the FDA investigation did not yield the outbreak strain from the tomato-growing environment or packing house, but did identify two different Salmonella serotypes.
The tomato traceback implicating a single grower/packer in Ohio provided further support that tomatoes were the food vehicle responsible for this outbreak. No traceback was conducted on tomatoes consumed by controls; however, given the large number of tomato sources available the probability that the source of all four restaurants, unrelated by corporate affiliation, would have the same source of tomatoes is low. Even if there were only two sources of tomatoes, the simple binomial probability that all four restaurants would have the same source is 1/16. This is the first outbreak of human infections traced to tomatoes in the Ohio growing region of the USA. Tomato-associated outbreaks over the past 15 years have been traced to produce originating from several states in Eastern and Southeastern USA, including Virginia [Reference Greene12] Florida [11, Reference Gupta14, Reference Cummings15], and South Carolina [Reference Hedberg21]. One outbreak in 2005 was associated with tomatoes from California [Reference Yuan24]. These outbreaks, and this outbreak traced to a new growing region in Ohio suggest that the problem is not localized to one particular region.
Outbreaks of salmonellosis due to contaminated tomatoes have been widely dispersed, indicating that contamination is probably occurring early in the distribution chain, such as at the farm or packing house, rather than at the multiple restaurants or the kitchens of multiple patients. Indeed, the outbreak strain has been found in irrigation pond water from tomato farms on the eastern shore of Virginia during environmental investigations in response to outbreak investigations associated with S. Newport and in a sample of chopped tomatoes left over from a restaurant collected from the home of a case-patient [Reference Greene12]. Clusters of S. Newport PFGE pattern JJPX01.0061 have been detected every year since 2002; in 2002 and 2005 outbreaks were traced to tomatoes grown on the eastern shore of Virginia [Reference Greene12] suggesting that contamination of the growing environment may persist over time.
These recurrent multistate outbreaks indicate that the tomato-growing environment can be an ongoing source of contamination of tomatoes. Possible sources of environmental Salmonella contamination include faeces from domestic or wild animals including reptiles, amphibians, rodents, or birds, or of their habitat, such as ponds or drainage ditches in or near to tomato fields. The exact mechanism by which tomatoes become contaminated is unknown but several are suggested by experimental evidence. Tomatoes may internalize Salmonella when they are immersed in contaminated water with a temperature less than the tomatoes' temperature [Reference Guo25]. Tomatoes can become internally contaminated when tomato stems and flowers are inoculated with Salmonella [Reference Lin26], which could occur during growth if contaminated water is directly applied to plants. Contamination on the tomato surface can also be drawn into the interior of a tomato when it is cut. Once contaminated, cut tomatoes provide an excellent medium for bacterial amplification [Reference Lin26].
In recent years, 6/11 large multistate salmonellosis outbreaks have been linked to contaminated tomatoes served in restaurants similar to tomatoes in this investigation [11–Reference Cummings15, Reference Yuan24]. Tomatoes served in restaurants are of particular concern because restaurants may have different sources of produce compared to grocers and might store and handle tomatoes in ways that allow for amplification of bacteria [11, Reference Kirkland27]. Because Salmonella can rapidly replicate on the cut surface of contaminated tomatoes, the U.S. FDA Federal Food Code has been amended so that cut tomatoes (because they have a pH ⩾4·2 and water activity >0·99) are defined as a ‘time/temperature control for safety’ food, which requires refrigeration of cut, sliced, or processed tomatoes [28]. In addition, growers, harvesters, re-packers, retailers, and food-service employees should follow guidelines for good agricultural and manufacturing practices when handling tomatoes [11, Reference Greene12]. Restaurants should maintain adequate records to allow for traceback and trace-forward of food products implicated in outbreaks. Tomato growers, packers, re-packers, and processors should maintain adequate records to aid in traceback of products implicated in outbreaks. Because tomatoes are commonly eaten raw, prevention of tomato contamination should include interventions on the farm, during packing, and at restaurants. Re-staurant managers and restaurant staff should be educated on the safe handling of tomatoes in a restaurant setting. Additionally, consumers should be educated on the safe handling of tomatoes in the home.
The FDA launched a Tomato Safety Initiative during the summer of 2007 in response to recurring outbreaks of Salmonella infections associated with fresh and fresh cut tomatoes. This ongoing initiative is a collaborative effort between FDA and the state health and agriculture departments in Virginia and Florida, in cooperation with several universities and members of the produce industry, and CDC. The initiative is part of a risk-based strategy to reduce foodborne illness by focusing food-safety efforts on specific products, practices, and growing areas that have been found to be problematical in the past. Findings from assessments in this initiative will allow FDA to continue to improve its guidance and policy on tomato safety.
These large, recurrent multistate outbreaks indicate that raw tomatoes pose an ongoing threat for salmonellosis. Public health professionals should be aware that tomatoes are a possible vehicle when investigating outbreaks of Salmonella infections. If tomatoes are identified as an outbreak food vehicle, tracing implicated tomatoes to their source is critical to understanding the mechanism of contamination. Because tomatoes are often used as a raw ingredient, prevention of contamination is critical. To prevent future tomato-associated outbreaks, further research by industry, academia, and public health, agriculture, and regulatory agencies is necessary to determine the source and vectors of contamination, mechanisms by which pathogens contact and become internalized, the stages of development at which plants are most susceptible to contamination that persists, and procedures by which contamination can be reduced or eliminated.
ACKNOWLEDGEMENTS
We gratefully acknowledge the following: A. Sheth, MD, R.M. Hoekstra, PhD, Alyssa Wilkinson, DVM, Ian Williams, PhD, MS, Division of Foodborne, Waterborne and Environmental Diseases, CDC; Enteric Diseases Laboratory Branch, CDC; and Center for Food Safety and Applied Nutrition, FDA. We gratefully acknowledge the important contributions from public health, food regulatory, and laboratory personnel from the affected states and our FDA partners.
DECLARATION OF INTEREST
None.








