A recent meta-analysis reported robust evidence linking longer duration of untreated psychosis (DUP) with poorer recovery at 12 and 24 months (Reference Marshall, Lewis and LockwoodMarshall et al, 2005). The UK Department of Health targets a median DUP of 3 months with no one waiting longer than 6 months (Department of Health, 2002). This target necessitates a greater understanding of the factors influencing DUP in the UK.
It has been suggested that DUP is not a unitary variable but is composed of distinct intervals. In France, Cougnard et al (Reference Cougnard, Kalmi and Desage2004) reported a median delay of 9 weeks between the first psychotic symptom and the first helping contact. A Canadian study (Reference Norman, Malla and VerdiNorman et al, 2004) reported a comparable delay component with a median duration of 5.1 weeks and a mean of 25.1 weeks. Norman et al (Reference Norman, Malla and Verdi2004) reported a second component reflecting the delay between help-seeking commencement and antipsychotic medication, with a median duration of 5.1 weeks and a mean of 44.6 weeks. However, this second component included both delays in the referral pathway to secondary services and delays within secondary services themselves.
The present study investigates the duration of all three components (delays in help-seeking, referral pathways and mental health services) in a geographically defined inner-city area not yet supported by an early intervention service.
Method
Sampling
Participants were recruited from eastern inner-city Birmingham (population 160 000, mean Jarman index +25; Office for National Statistics, 2001). Between November 2001 and November 2002 all new referrals to mental health services were screened for individuals aged between 14 and 35 years, meeting broad diagnostic criteria for psychosis in the absence of a primary mood disorder (ICD-10 categories F20, F22, F23, F25; World Health Organization, 1992).
Procedure
Weekly contact with admission units, home treatment teams and out-patient clinics were established to proactively screen all new cases using the World Health Organization (1992) checklist. In addition, all letters to general practitioners (GPs) from consultants were screened.
Individuals meeting the inclusion criteria were invited to take part during recovery from their first episode. Details of symptom onset and development, pathways to care, medication and treatment adherence were collected from mental health records. Semi-structured interviews were conducted with clients and with key relatives where possible. Pathways to care were recorded using an adapted version of the Pathways Encounter Form (Reference Gater, Sousa and BarrientosGater et al, 1991).
Definitions
‘Onset of non-specific symptoms’ was defined in accordance with symptoms listed by Beiser et al (Reference Beiser, Erickson and Fleming1993).
‘Onset of psychosis’ followed the definition used by Larsen et al (Reference Larsen, McGlashan and Moe1996) and required either one symptom from the positive scale of the Positive and Negative Syndrome Scale (Reference Kay, Fiszbein and OplerKay et al, 1987) at a level of 4 or above in the context of a manifestation of psychotic symptoms; or a cluster of these symptoms including either delusions, conceptual disorganisation or hallucinatory behaviour and reaching a total rating of 7 or more (excluding ‘absent’ ratings). Symptoms had to be present for a minimum of 2 weeks unless remission was due to treatment.
‘First help-seeking contact’ on the pathway to care including any individual other than friends or family.
‘Onset of criteria treatment’ required antipsychotic treatment either: at dosage levels recommended by the British National Formulary (for example 2 mg risperidone; British Medical Association & Royal Pharmaceutical Society of Great Britain, 2001) with participants taking medication regularly for 1 month after commencement; or leading to a significant reduction in symptoms.
The lead researcher (K.B.) conducted all calculations of treatment delays and pathways to care.
Results
There were 80 individuals who fulfilled the study criteria, 25 (31%) of whom were not interviewed because they declined to take part (n=18; 23%), they presented significant safety risks (n=3; 4%), suitable interpreters were unavailable (n=2; 3%), or service inception had occurred out of the area (n=2; 3%). A key relative was interviewed to provide additional information in 34 (62%) of the remaining 55 cases. Demographic characteristics did not differ between participants and non-participants.
Participants were predominantly male (73%), single (75%) and living with parents or guardians (62%). Ages ranged between 14 and 35 years, with a mean age of 23 years at the onset of psychosis. The majority did not hold educational qualifications above the General Certificate of Education or National Vocational Qualification level 1 (66%), and were unemployed (64%). Participants were of South Asian (48%), White (38%), Black (6%) and dual (7%) ethnicity.
Components of treatment delay
Thirteen (24%) participants sought help during the prepsychotic period. Table 1 presents data for the three components of DUP, each of which included extreme values and demonstrated high levels of variability. This was particularly true of the delay in the commencement of help-seeking. Treatment delay components were unrelated to socio-demographic variables, including ethnicity.
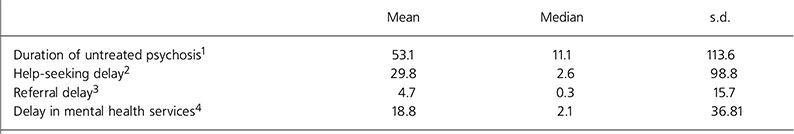
Table 1. Components of treatment delay (weeks) for the 55 participants
| Mean | Median | s.d. | |
|---|---|---|---|
| Duration of untreated psychosis1 | 53.1 | 11.1 | 113.6 |
| Help-seeking delay2 | 29.8 | 2.6 | 98.8 |
| Referral delay3 | 4.7 | 0.3 | 15.7 |
| Delay in mental health services4 | 18.8 | 2.1 | 36.81 |
Most notable was the major contribution of delays within mental health services, having a median over seven times longer than the median referral delay. Mean delay in mental health services accounted for 35% of overall DUP.
Discussion
In line with the literature (Reference Marshall, Lewis and LockwoodMarshall et al, 2005), overall DUP was lengthy, with a mean of approximately 1 year. Nevertheless, the median delay of only 11 weeks suggests that the majority of individuals experienced delays within Department of Health guidelines of 3 months. The delay within mental health services was a major contributor, with a median of 2.1 weeks and a mean of 19 weeks, accounting for 35% of overall DUP. This is a surprising finding and to our knowledge the first documentation of this component of delay. Although community education has been found to contribute to the reduction of DUP (Reference Melle, Larsen and HaahrMelle et al, 2004), these findings highlight barriers within specialist services as highly significant, at least in the UK.
Qualitative information from the Pathways Encounter Form indicated a number of potential contributors to delays in mental health services. Overwhelming service pressures often led to long waiting lists for initial appointments, a delay compounded when individuals failing to attend three appointments were automatically discharged and underwent a lengthy re-referral process. Delays also occurred where ambiguous presentations led to diagnostic uncertainty and a course of non-antipsychotic intervention before psychosis was identified. In some cases this was avoided through periods of drug-free assessment, thus postponing ‘criteria treatment’. Finally, once a thorough assessment had been completed and psychosis identified, some individuals elected not to take antipsychotic medication.
These observations warrant further investigation both locally and nationally to inform the development of appropriate strategies for early intervention service teams. Organisational changes may enable more prompt assessments, and more assertive approaches could avoid premature discharge where clients are unable or unwilling to attend out-patient appointments. Clearer protocols for the definition and treatment of first episodes, and specialist training within secondary services might also accelerate identification and treatment. Finally, a drive to improve initial service engagement might reduce treatment delay.
These observations are congruent with the guidance for early intervention services outlined in the Mental Health Policy Implementation Guide (Department of Health, 2001); it might be anticipated that the introduction of these early intervention services would directly influence these care pathways in mental health services.
We would caution that the onset of psychotic symptoms and onset of criteria treatment remain arbitrary time-points. Our definition of criteria treatment is certainly not intended to discourage drug-free assessment or to imply that pharmacological treatment is the only intervention considered adequate. Indeed one study has reported an association between longer delay in intensive psychosocial intervention and poorer prognosis (Reference De Haan, Linszen and Leniorde Haan et al, 2003). Nevertheless, here we apply a consistent definition and the relative contribution of delays in mental health services is apparent.
The combined delay in referral and within services (mean=23.5 weeks) was shorter than that reported in Canada (44.6 weeks; Reference Norman, Malla and VerdiNorman et al, 2004). However, as mean DUP is commonly affected by extreme values a meaningful comparison would require median values of referral delay and delays in mental health services. Mean help-seeking delay (29.8 weeks) was comparable to Norman et al's report of 25.1 weeks; however, the median help-seeking delay in Birmingham (2.6 weeks) was shorter than that reported either in Canada (5.1 weeks; Reference Norman, Malla and VerdiNorman et al, 2004) or in France (9 weeks; Reference Cougnard, Kalmi and DesageCougnard et al, 2004). Therefore it appears that although a number of individuals experienced very long delays in this inner-city UK cohort, the majority sought help quickly in comparison with their counterparts in Canada or France. These findings were independent of ethnicity and echo the recent findings of Morgan et al (Reference Morgan, Fearon and Hutchinson2006); however, in the present sample there were more Asian and few Black participants.
Duration of untreated psychosis among patients declining to take part in studies may be longer than DUP among participants (Reference Friis, Melle and LarsenFriis et al, 2004). It may therefore be that DUP and its components were underestimated in the present study, although it remains unknown which components of DUP might vary according to willingness to participate. These results are also specific to individuals aged between 14 and 35, in line with Department of Health guidelines for early intervention service development (Department of Health, 2001).
Conclusions
The association of shorter DUP and improved outcome makes DUP of interest to both scientific enquiry and policy development. The reduction of DUP requires interventions that focus on all components. First, community educational interventions may promote help-seeking by young people and relatives. Second, as help-seeking occurs predominantly through primary care in the UK, education of related professionals is also crucial (Reference Tait, Lester and BirchwoodTait et al, 2005). Finally, this study emphasises the necessity to focus training on the definition, recognition and treatment of first-episode psychosis in mental health services. These illnesses do not present in ‘neat parcels’ and often present with diagnostic uncertainty (Reference McGorry, Edwards and MihalopoulosMcGorry et al, 1996). The introduction of early intervention services should include an explicit focus on the care pathways within secondary care, as early intervention services often sit behind front-line services such as community mental health and home treatment teams.
Declaration of interest
None.






eLetters
No eLetters have been published for this article.